Amphotericin B Dr Pippa Newton Infectious Diseases Consultant

Amphotericin B Dr Pippa Newton, Infectious Diseases Consultant, Manchester University NHS Foundation Trust

Intended learning outcome To understand the mechanism of action of amphotericin B To be aware of the spectrum of activity of amphotericin B To understand the pharmacokinetics of amphotericin B To be aware of the clinical indication and dosages of amphotericin B To be aware of the adverse events associated with amphotericin B therapy

Introduction Amphoterin B, the first systemic antifungal, was introduced in 1958 It’s a natural product from the actinomycete Streptomyces nodosus It offers potent, broad-spectrum antifungal activity against yeasts, moulds and the dimorphic fungi It’s a large molecule with both hydrophobic and hydrophilic portions (amphiphatic) It has a molecular weight of 924 g/mol
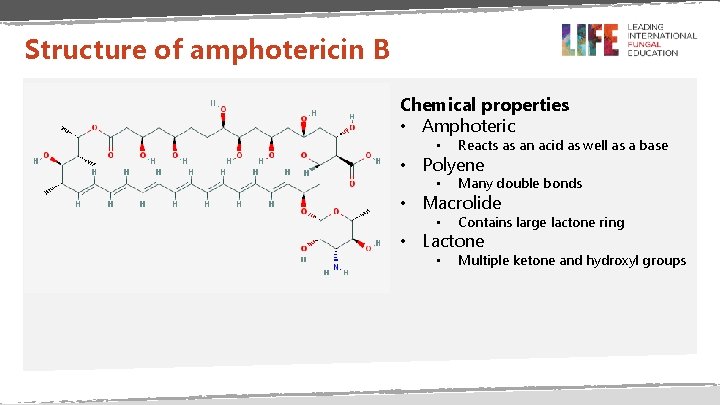
Structure of amphotericin B Chemical properties • Amphoteric • Reacts as an acid as well as a base • Many double bonds • Contains large lactone ring • Multiple ketone and hydroxyl groups • Polyene • Macrolide • Lactone
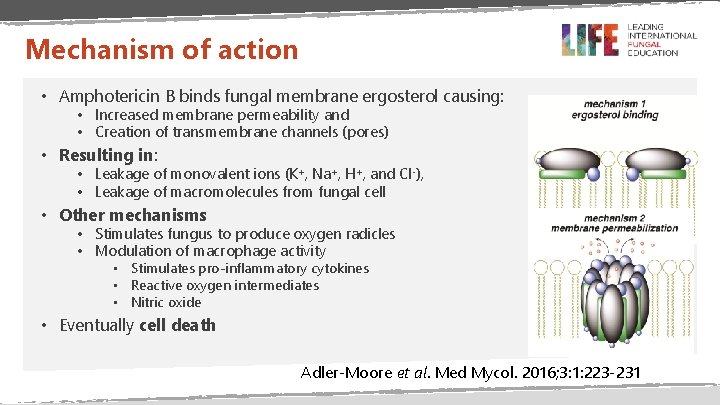
Mechanism of action • Amphotericin B binds fungal membrane ergosterol causing: • Increased membrane permeability and • Creation of transmembrane channels (pores) • Resulting in: • Leakage of monovalent ions (K+, Na+, H+, and Cl-), • Leakage of macromolecules from fungal cell • Other mechanisms • Stimulates fungus to produce oxygen radicles • Modulation of macrophage activity • Stimulates pro-inflammatory cytokines • Reactive oxygen intermediates • Nitric oxide • Eventually cell death Adler-Moore et al. Med Mycol. 2016; 3: 1: 223 -231

Amphotericin B formulations • “Conventional” • Amphotericin B deoxycholate (Am. B-d) • Newer (lipid-based) formulations • Liposomal amphotericin B (L-Am. B) • Amphotericin B lipid complex (ABLC) • Amphotericin B colloidal dispersion (ABCD) • Many others
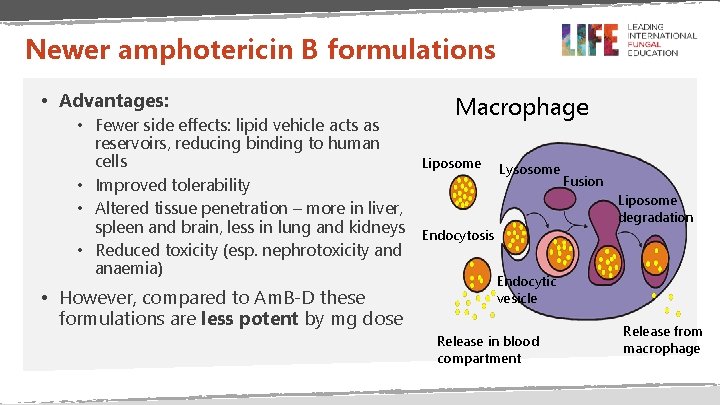
Newer amphotericin B formulations • Advantages: • Fewer side effects: lipid vehicle acts as reservoirs, reducing binding to human cells • Improved tolerability • Altered tissue penetration – more in liver, spleen and brain, less in lung and kidneys • Reduced toxicity (esp. nephrotoxicity and anaemia) • However, compared to Am. B-D these formulations are less potent by mg dose Macrophage Liposome Lysosome Fusion Liposome degradation Endocytosis Endocytic vesicle Release in blood compartment Release from macrophage
Spectrum of activity • Amphotericin B is one of the most potent antifungal agents, demonstrating activity against: Moulds Yeasts Dimorphic fungi
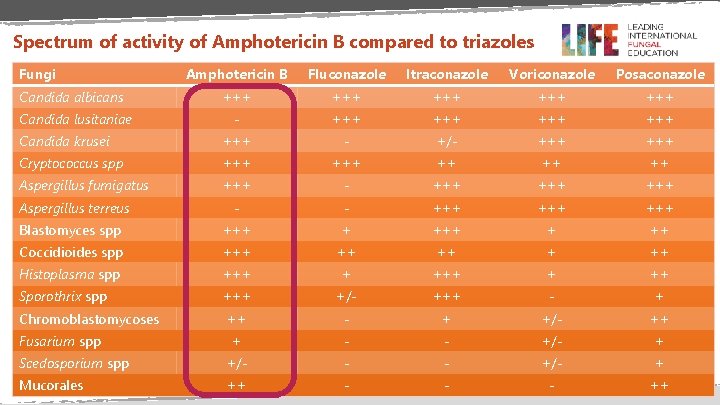
Spectrum of activity of Amphotericin B compared to triazoles Fungi Amphotericin B Fluconazole Itraconazole Voriconazole Posaconazole +++ +++ +++ - +++ +++ Candida krusei +++ - +/- +++ Cryptococcus spp +++ ++ Aspergillus fumigatus +++ - +++ +++ - - +++ +++ Blastomyces spp +++ + ++ Coccidioides spp +++ ++ ++ Histoplasma spp +++ + ++ Sporothrix spp +++ +/- +++ - + +/- ++ + - - +/- + Scedosporium spp +/- - - +/- + Mucorales ++ - - - ++ Candida albicans Candida lusitaniae Aspergillus terreus Chromoblastomycoses Fusarium spp

Resistance Intrinsic resistance • • Aspergillus terreus Aspergillus nidulans Candida lusitaniae Scedosporium spp. Acquired resistance • Very rare Higher MICs to: • • • Aspergillus flavus Fusarium spp. Scedosporium spp. Candida krusei Paecilomyces lilanicus

Resistance q Aspergillus flavus q Fusarium spp. q Scedosporium spp. q Candida krusei q Paecilomyces lilanicus Higher MICs Intrinsic resistance Acquired resistance q. Very rare q. Aspergillus terreus q. Aspergillus nidulans q. Candida lusitaniae q. Scedosporium spp.
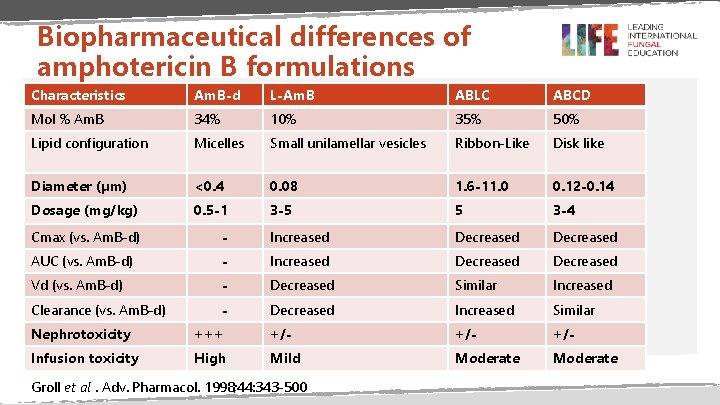
Biopharmaceutical differences of amphotericin B formulations Characteristics Am. B-d L-Am. B ABLC ABCD Mol % Am. B 34% 10% 35% 50% Lipid configuration Micelles Small unilamellar vesicles Ribbon-Like Disk like Diameter (µm) <0. 4 0. 08 1. 6 -11. 0 0. 12 -0. 14 Dosage (mg/kg) 0. 5 -1 3 -5 5 3 -4 Cmax (vs. Am. B-d) - Increased Decreased AUC (vs. Am. B-d) - Increased Decreased Vd (vs. Am. B-d) - Decreased Similar Increased Clearance (vs. Am. B-d) - Decreased Increased Similar Nephrotoxicity +++ +/- +/- Infusion toxicity High Mild Moderate Groll et al. Adv. Pharmacol. 1998; 44: 343 -500
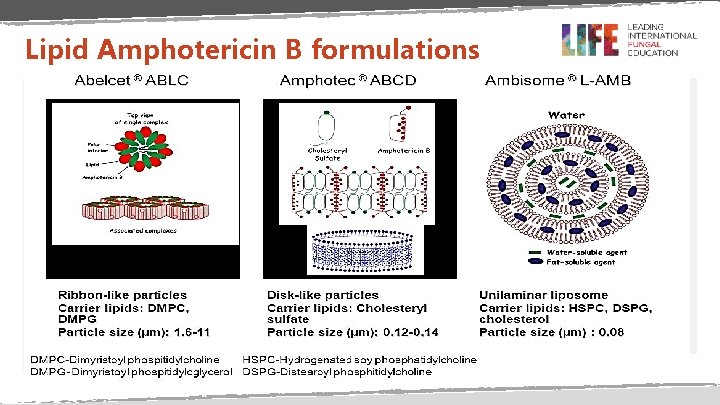
Lipid Amphotericin B formulations

Pharmacokinetics • Bioavailability: All formulations are parental • Distribution: Well distributed in most body compartments CNS penetration ~0% • Metabolism: t 1/2: ~15 days (detectable in urine for at least 7 weeks after last dose) Protein binging > 90% and is poorly dialyzable • Elimination: Excreted unchanged in urine (21%) and faeces (43%) Bellmann & Smuszkiewicz: Infections. 2017. pp 1 -43

Clinical indications First-line indications • Cryptococcal meningitis • Histoplasmosis • Mucormycosis • Penicilliosis (Talaromyces marneffei • Other indications infection) • Leishmaniasis Nett & Andes. Infect Dis Clin N Am. 2016; 30 51 -83 • Invasive aspergillosis • Invasive candidiasis • Candidaemia Coccidioidomycosis Blastomycosis Phaeohyphomycosis Sporotrichosis (disseminated) • Oesophageal candidiasis • •

Dosages Amphotericin B deoxycholate • Adults: 0. 7 -1 mg/kg/day • Paediatrics: 0. 7 -1 mg/kg/day Amphotericin B Liposomal • Adults: • Empiric therapy in neutropenia: 3 mg/kg/day • Systemic infections: 3 -5 mg/kg/day • Cryptococcal meningitis: 6 mg/kg/day • Paediatrics: same weight-based dosing

Adverse events • Acute infusion-related reactions • Nausea, vomiting, rigors , fever, hyper/hypotension, and hypoxia • Caused by the effects of amphotericin B on pro-inflammatory cytokine production • Nephrotoxicity • 34 -60% of patients • Due to: • Vasoconstriction • Direct damage to the distal tubule cell membranes • Results: • Loss of electrolytes • Impaired urinary acidification and concentration • Renal tubular acidosis Loo et al. Expert Opin Drug Saf. 2013; 12: 881 -895 Groll et al. Adv Pharmacol. 1998; 44; 343 -500

Other adverse events Common (≥ 1/100 to <1/10) Very common ( ≥ 1/10) • Anaemia • Nausea, vomiting • Hypomagnesemia • Hypotension • Headache • Hypokalaemia • Transient renal function test abnormalities (azotemia, hyposthenuria, renal tubular acidosis and nephrocalcinosis ) • Chills Rare ( ~ 1/1000) • Anaphylaxis Fungizone SPC: emc last updated 29 -Nov-2016 • Diarrhoea • Liver function test abnormalities • Injection site pain (with or without phlebitis or thrombophlebitis) • Acute renal failure • Bone or other pain (Am. Bisome)

Contraindication • Known hypersensitivity to amphotericin B • Unstable/moderately renal dysfunction, unless unavoidable.

Tips on administering amphotericin B • Use a central line if possible for Am. B-D, as phlebitis common – not so important for lipid-Am. B. • Set the infusion up and run in about 10 ml, and then stop for 15 -20 mins to check for anaphylaxis – a ‘test dose’ unnecessary and delays therapy. • Slower infusions reduce acute infusion-related side effects (> 2 hours for lipid formulations, > 4 hours for Am. B-d) • Pre-loading with N/saline (500 -1, 000 m. L) reduces renal dysfunction • Check renal function daily for first 4 -5 days then, 3 x weekly • Avoid other nephrotoxic drugs, especially aminoglycosides and frusemide • Check K+ at least 2 x/week and mg++ weekly, if possible. • Amiloride 5 mg daily, may reduce K+ loss. • Check Hb at 7, 14 and 21 days – may need transfusion • Avoid giving hydrocortisone for infusion-related side effects, if possible. Use acetaminophen/paracetamol, or low dose opiate. Khoo et al. J Antimicrob Chemother. 1994; 33: 203 -213

Conclusion • Amphoterin B, the first systemic antifungal, was introduced in 1958 • It offers potent, broad-spectrum antifungal activity but is associated with significant renal toxicity and infusion reactions • Lipid-based amphotericin B formulations were introduced in the 1990 s and maintain the potent, broad-spectrum activity of the deoxycholate formulation with less toxicity • Drug of choice for the vast majority of life-threatening systemic fungal infections • Treatment of mycoses in pregnant women as triazole class are considered teratogenic
- Slides: 21