AMLALL BY BRITTNI MCCLELLAN CLASSIFICATIONS Acute Myelogenous Leukemia

AML/ALL BY: BRITTNI MCCLELLAN
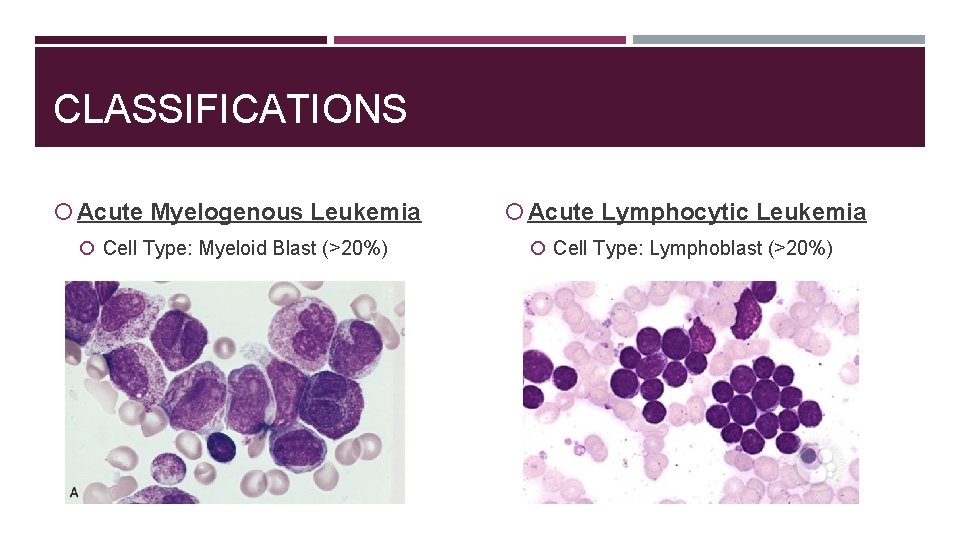
CLASSIFICATIONS Acute Myelogenous Leukemia Acute Lymphocytic Leukemia Cell Type: Myeloid Blast (>20%) Cell Type: Lymphoblast (>20%)
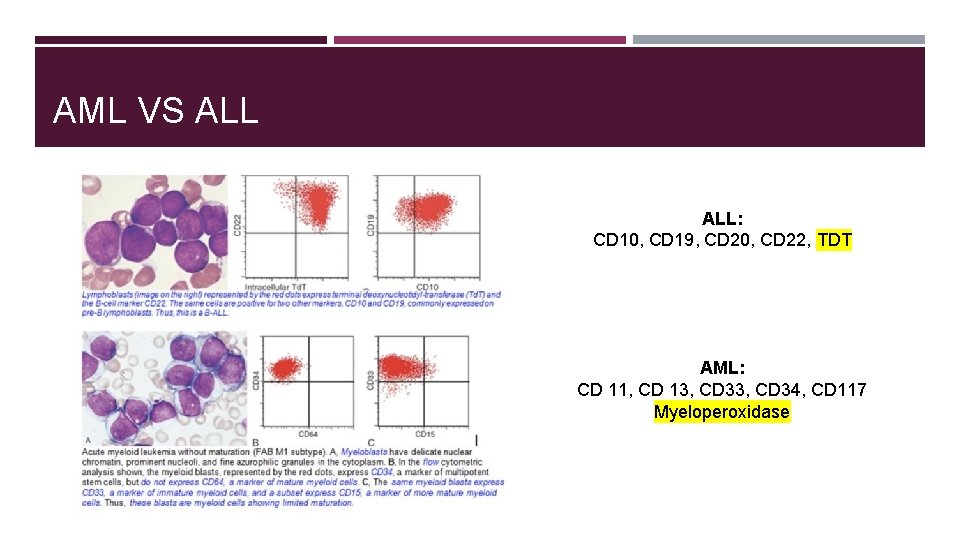
AML VS ALL: CD 10, CD 19, CD 20, CD 22, TDT AML: CD 11, CD 13, CD 34, CD 117 Myeloperoxidase
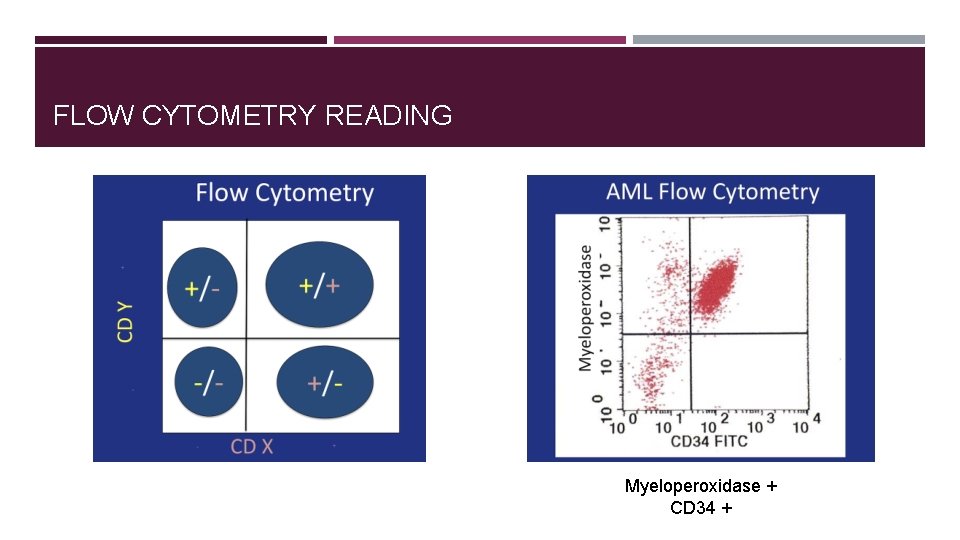
FLOW CYTOMETRY READING Myeloperoxidase + CD 34 +
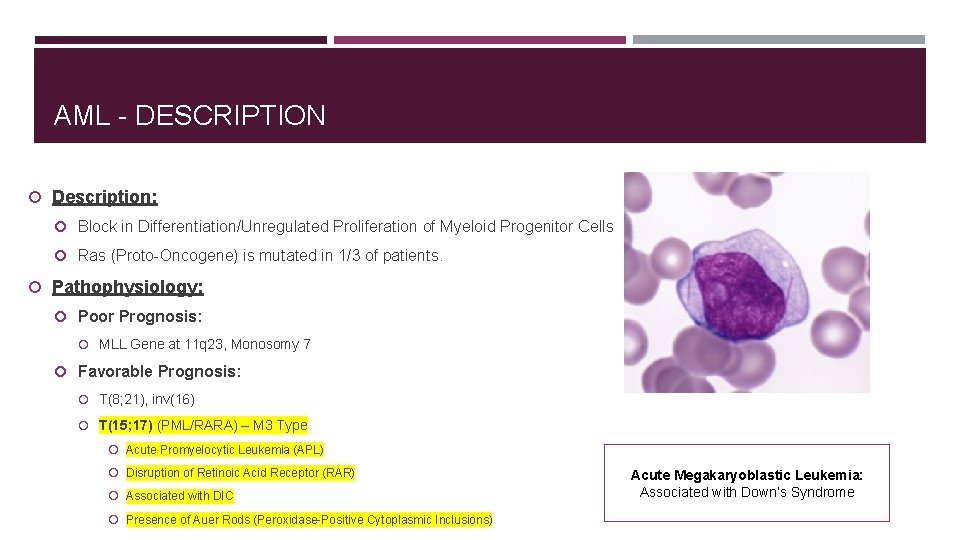
AML - DESCRIPTION Description: Block in Differentiation/Unregulated Proliferation of Myeloid Progenitor Cells Ras (Proto-Oncogene) is mutated in 1/3 of patients. Pathophysiology: Poor Prognosis: MLL Gene at 11 q 23, Monosomy 7 Favorable Prognosis: T(8; 21), inv(16) T(15; 17) (PML/RARA) – M 3 Type Acute Promyelocytic Leukemia (APL) Disruption of Retinoic Acid Receptor (RAR) Associated with DIC Presence of Auer Rods (Peroxidase-Positive Cytoplasmic Inclusions) Acute Megakaryoblastic Leukemia: Associated with Down’s Syndrome
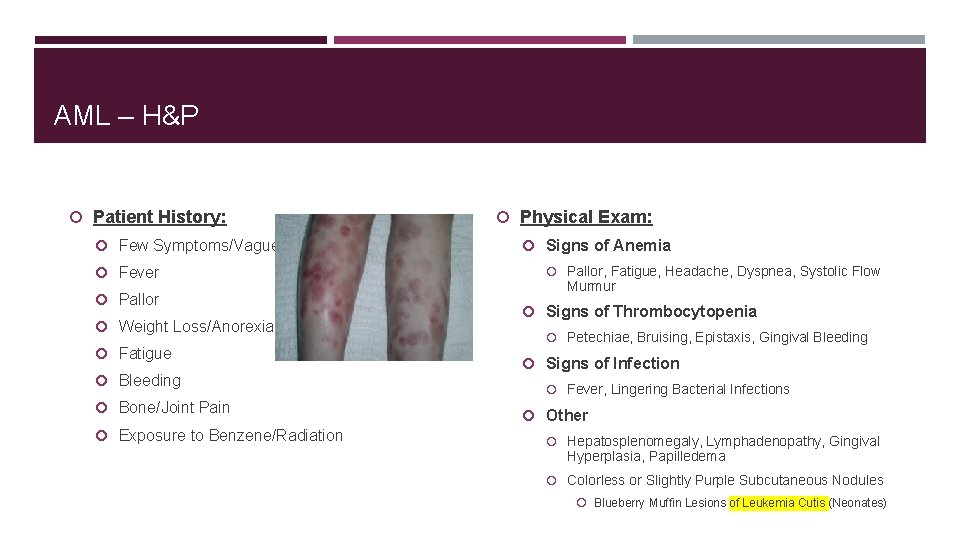
AML – H&P Patient History: Few Symptoms/Vague Fever Pallor Weight Loss/Anorexia Fatigue Bleeding Bone/Joint Pain Exposure to Benzene/Radiation Physical Exam: Signs of Anemia Pallor, Fatigue, Headache, Dyspnea, Systolic Flow Murmur Signs of Thrombocytopenia Petechiae, Bruising, Epistaxis, Gingival Bleeding Signs of Infection Fever, Lingering Bacterial Infections Other Hepatosplenomegaly, Lymphadenopathy, Gingival Hyperplasia, Papilledema Colorless or Slightly Purple Subcutaneous Nodules Blueberry Muffin Lesions of Leukemia Cutis (Neonates)

AML - DIAGNOSIS Diagnosis: CBC: Diagnostic Procedures: Southern Blotting ↓ Hemoglobin/Hematocrit (Anemia) Reverse Transcriptase-PCR Thrombocytopenia Fluorescence in Situ Hybridization ↓ WBC Peripheral Smear Bone Marrow Aspirate: ↑ PT/PTT Electrolytes: Hyperkalemia Hypocalcemia Hyperphosphatemia Hyperuricemia >20% Leukemic Myeloblasts Immunophenotyping: Myeloid Blast +: 90% of Cases CD 11 b, CD 13, CD 14, CD 15, CD 33, CD 36 Myeloperoxidase Lymphoid Markers: 30 -60% of Cases Megakaryocytic: CD 41, CD 42, CD 61

AML – MORPHOLOGY AND CYTOCHEMISTRY Diagnosis: Morphology: Large Blasts with Low Nuclear/Cytoplasmic Radio Multiple Nucleoli and Cytoplasmic Granules Auer Rods Cytochemistry: Myeloperoxidase + Sudan Black + Sudan Black Stain

AML – TREATMENT Medication: 6 -9 Months Intensive Chemotherapy in Cycles Anthracylines Doxorubicin Daunomycin Mitoxantrone Adjuncts Etoposide, Gemtuzumab, Dexamethasone, L-Asparaginase, 6 -Thioguanine M 3 Variant: High Rate of Remission Induction with all Trans-Retinoic Acid in APL. 85% of Cases Achieve Remission
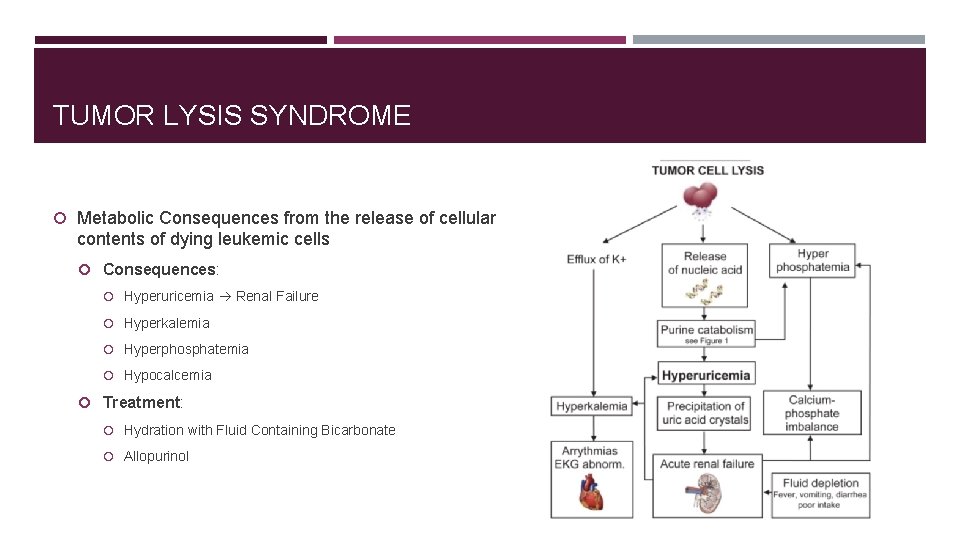
TUMOR LYSIS SYNDROME Metabolic Consequences from the release of cellular contents of dying leukemic cells Consequences: Hyperuricemia Renal Failure Hyperkalemia Hyperphosphatemia Hypocalcemia Treatment: Hydration with Fluid Containing Bicarbonate Allopurinol
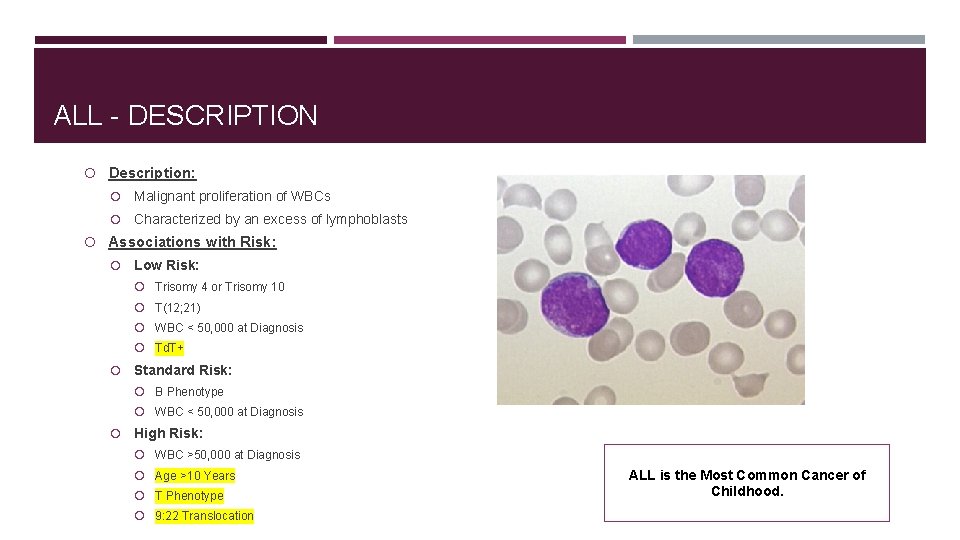
ALL - DESCRIPTION Description: Malignant proliferation of WBCs Characterized by an excess of lymphoblasts Associations with Risk: Low Risk: Trisomy 4 or Trisomy 10 T(12; 21) WBC < 50, 000 at Diagnosis Td. T+ Standard Risk: B Phenotype WBC < 50, 000 at Diagnosis High Risk: WBC >50, 000 at Diagnosis Age >10 Years T Phenotype 9: 22 Translocation ALL is the Most Common Cancer of Childhood.

ALL - PATHOPHYSIOLOGY • • Multiple Genetic Mutations Rapid Clonal Proliferation Lack of Cell Maturation Resistance to Apoptosis Crowding of Normal Bone Marrow Precursors Ineffective Hematopoiesis Associated Conditions: • • • Trisomy 21 Li-Fraumeni Syndrome Neurofibromatosis Type 1 Ataxia Telangiectasia Bloom Syndrome Immunodeficiencies

ALL – H&P Patient History: Few Symptoms/Vague Bone Pain, Limp, Refusal to Bear Weight Infiltrative Disease of Marrow Pathological Fractures Pallor Weight Loss/Anorexia Fatigue, Headache Bleeding//Easy Bruising/Epistaxis Signs of Anemia Pallor, Fatigue, Headache, Dyspnea, Systolic Flow Murmur Signs of Thrombocytopenia Petechiae, Bruising, Epistaxis, Gingival Bleeding Signs of Infection Fever, Lingering Bacterial Infections Other Hepatosplenomegaly, Lymphadenopathy, Bone Tenderness, Hypopyon (Layering of Leukemia Cells in the Anterior Chamber of the Eye), Painless Testicular Enlargement, Swelling of the Face (Superior Vena Cava Syndrome). Colorless or Slightly Purple Subcutaneous Nodules Blueberry Muffin Lesions of Leukemia Cutis (Neonates) Physical Exam:
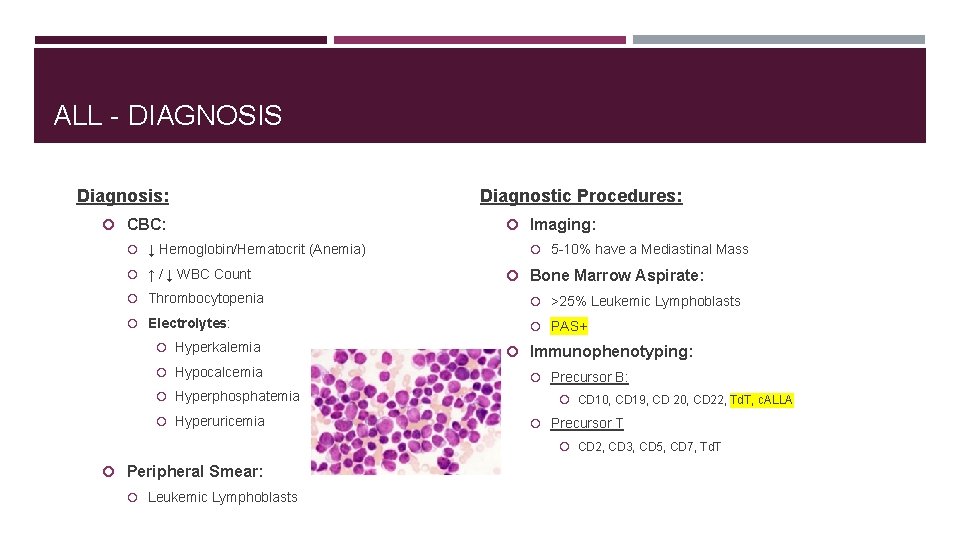
ALL - DIAGNOSIS Diagnosis: CBC: ↓ Hemoglobin/Hematocrit (Anemia) ↑ / ↓ WBC Count Diagnostic Procedures: Imaging: 5 -10% have a Mediastinal Mass Bone Marrow Aspirate: Thrombocytopenia >25% Leukemic Lymphoblasts Electrolytes: PAS+ Hyperkalemia Hypocalcemia Hyperphosphatemia Hyperuricemia Immunophenotyping: Precursor B: CD 10, CD 19, CD 20, CD 22, Td. T, c. ALLA Precursor T CD 2, CD 3, CD 5, CD 7, Td. T Peripheral Smear: Leukemic Lymphoblasts

ALL – TREATMENT Medication: Remission Induction Vincristine Adjuncts Prednisone/Dexamethasone, L-Asparaginase, Anthracycline Maintenance: Low Risk: Vincristine + Methotrexate Weekly (Oral) High Risk: Cyclophosphamide + Cytarabine + Methotrexate + Vincristine + Asparginase CNS Prophylaxis: Cytarabine (Ara. C)

QUESTION 1 A four-year-old girl is being evaluated for anemia. She originally presented to her pediatrician with her father who stated that she "hadn't seemed herself. " She was becoming easily fatigued and uncharacteristically cranky. He also thought she seemed to be bruising from only minor trauma. Her exam reveals cervical and axillary lymphadenopathy. A complete blood count revealed a hemoglobin of 7. 1 g/d. L, platelets of 50, 000, and a white blood cell count of 3, 000. Which of the following is most likely to be seen on peripheral blood smear? a) Myeloblasts with Auer rods b) Large, closely apposed blast cells with minimal cytoplasm intermixed with white spaces filled with debris c) Stacks of red blood cells d) Lymphoblasts with cytoplasmic aggregates of PAS positive material e) A microcytic anemia with target cells and hypochromic pencil-shaped cells c) Lymphoblasts with cytoplasmic aggregates of PAS positive material

QUESTION 2 A 55 -year-old male with fever, fatigue, generalized weakness, and bleeding gums for the past 3 weeks presents to his family physician. On exam, he has bilateral submandibular lymphadenopathy and hepatosplenomegaly. CBC demonstrates decreased RBCs and mature WBCs. The patient is referred to an oncologist, and a bone marrow aspiration is performed, demonstrating >20% myeloblasts with Auer rods that are myeloperoxidase positive. What is the most likely chromosomal translocation that is responsible for this patient's clinical presentation and lab results? a) 15; 17 b) 29; 22 c) 314; 18 d) 411; 14 e) 58; 14 a) 15; 17

QUESTION 3 A 13 -year-old male presents to clinic with fatigue a) The 9: 22 translocation denotes a better prognosis and fever. He has been spiking fevers for the b) Terminal deoxynucleotidyl past several weeks. He has no significant past transferase staining is likely positive medical history and has been growing and on the abnormal cells developing well. His vital signs are stable with the exception of a temperature of 38. 1 C. c) The 12: 21 translocation denotes a Physical examination is notable for pallor and poor prognosis hepatosplenomegaly. A complete blood count d) This patient's age is a good returns with leukocytosis of 110, 000. prognostic factor Subsequently, a bone marrow biopsy reveals 30% lymphoblasts. Which of the following is true e) B-cell phenotype decreases the risk regarding his illness? of CNS involvement b) Terminal deoxynucleotidyl transferase staining is likely positive on the abnormal cells
- Slides: 18