Amebiasis Amebic Dysentery Dr M H ANVARI Amebiasis


Amebiasis (Amebic Dysentery) Dr. M. H. ANVARI

Amebiasis (Amebic Dysentery) Causal agent: Entamoeba histolytica is well recognized as a pathogenic amoeba. History: Loosh was first described in 1875 Geographic Distribution: Worldwide, with higher incidence of amebiasis in developing countries. In industrialized countries, risk groups include male homosexuals, travelers and recent immigrants, and institutionalized populations.
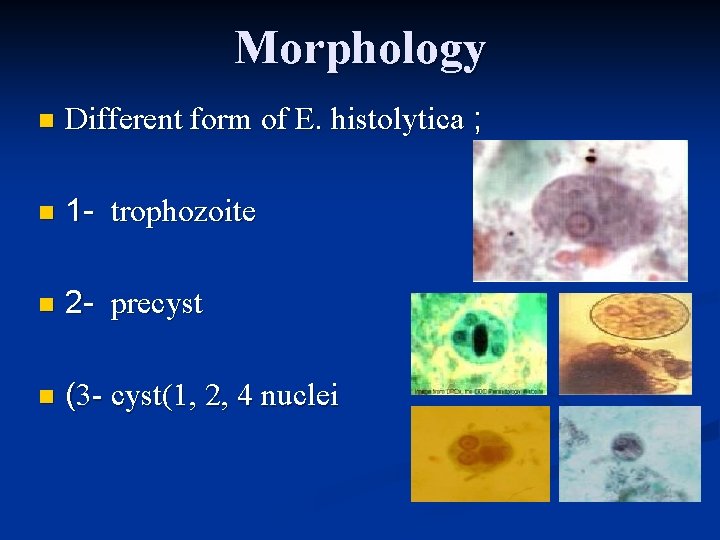
Morphology n Different form of E. histolytica ; n 1 - trophozoite n 2 - precyst n (3 - cyst(1, 2, 4 nuclei
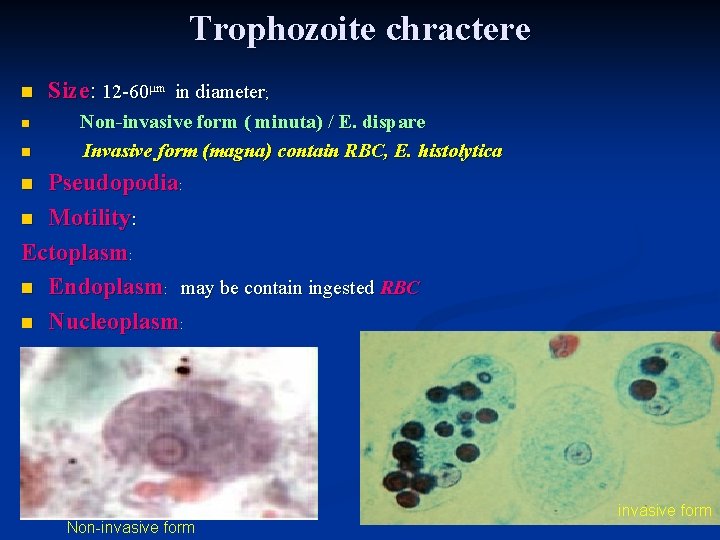
Trophozoite chractere n Size: 12 -60μm in diameter; n Non-invasive form ( minuta) / E. dispare n Invasive form (magna) contain RBC, E. histolytica Pseudopodia: n Motility: Ectoplasm: n Endoplasm: may be contain ingested RBC n Nucleoplasm: n Non-invasive form
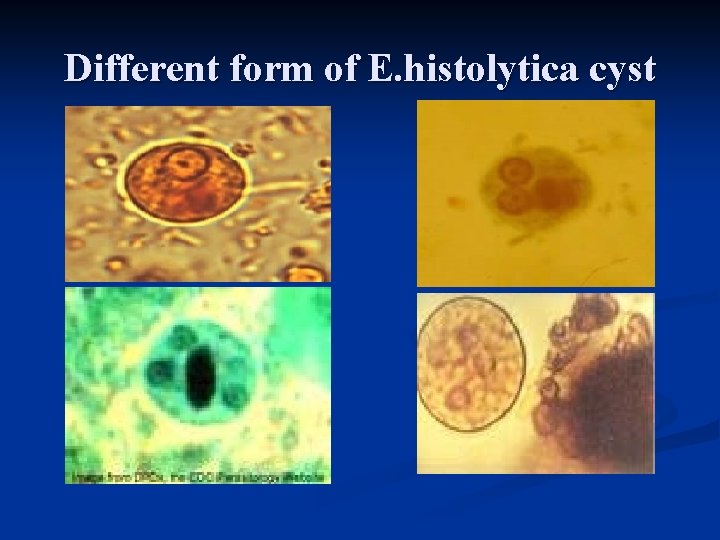
Different form of E. histolytica cyst
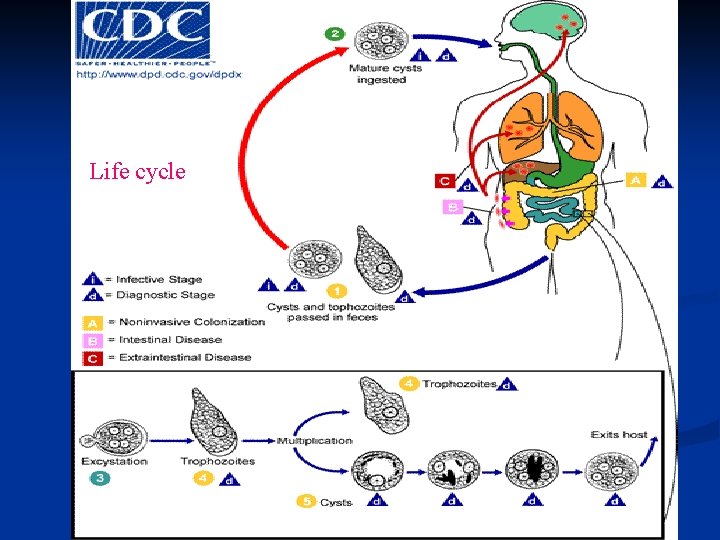
Life cycle

Epidemiology n Prevalence of amebic infection varies with level of sanitation and generally higher in tropics and subtropics than in tempearate climates. n *Worldwide prevalence is about 10% to 50% *Cyst passers are important source of infection n The true estimated prevalence of E. histolytica is close to 1% worldwide. Entamoeba histolytica is the second leading cause of mortality due to parasitic disease in humans. (The first being malaria). Amebiasis is the cause of an estimated 50, 000100, 000 deaths each year.

Transmission n n 1 -driect contact of person to person( fecal-oral) 2 - Veneral transmission among homosexual males( oral-anal 3 - Food or drink contaminated with feces containing the E. his. cyst 4 - Use of human feces (night soil) for soil fertilizer 5 - contamination of foodstuffs by flies, and possibly cockroaches

Pathogenesis n Effective factores: 1 - strain virulence: n - classic strain - non-classic strain; Laredo , Huff, …. - pathogen zymodemes n 2 - susceptibility of the host; nutrition status, immune-sys. n 3 - breakdown of immunologic barrier (tissue invasion)

Pathogenicity mechanisms 1 - secreting proteolytic enzymes( histolysine ) and cytotoxic substances. n 2 - contact-dependent cell killing n 3 – cytophagocytosis n n Amebic killing target cell: n 1 - receptore-mediated adherence of amebae to target cell ( adherence lectin) 2 - amebic cytolysis of target cell 3 - amebic phagocytosis of killed target cell n n
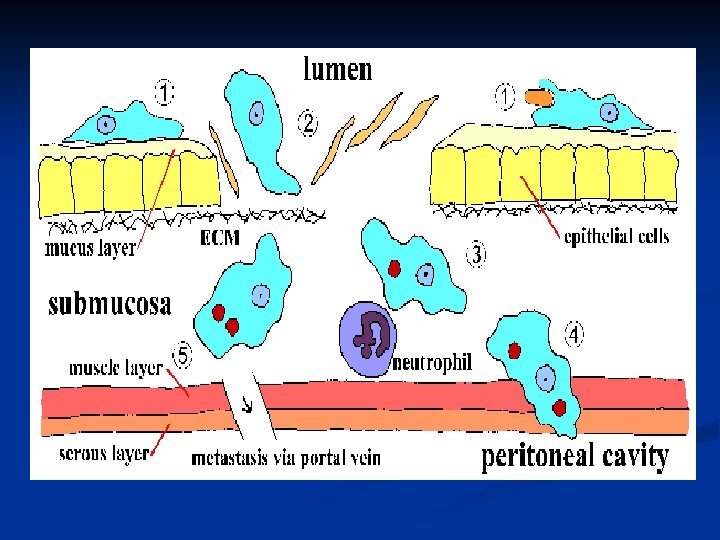
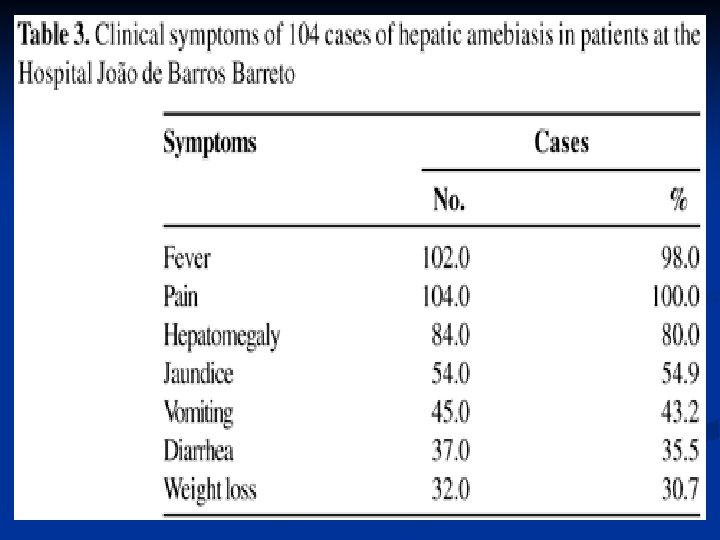
Clinical symptoms Asymptomatic infection Symptomatic infection Intestinal Amebiasis Extraintestinal Amebiasis Dysenteric Non-Dysenteric colitis Hepatic Pulmonary The extra foci Liver abscces Acut nonsupprative Intestinal Amebiasis symptoms: Diarrhea or dysentery, abdominal pain, cramping , anorexia, weight loss, chronic fatigue
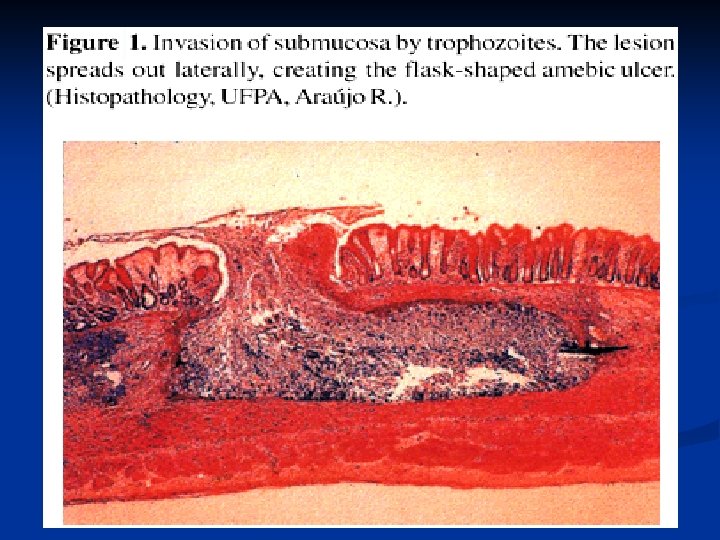
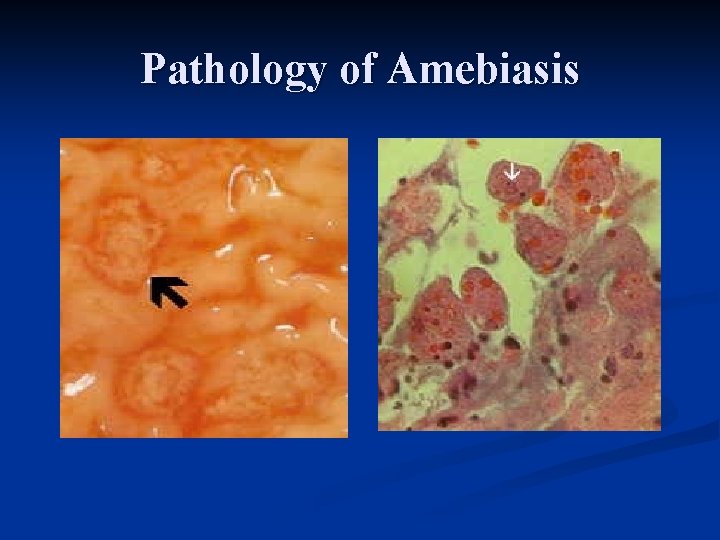
Pathology of Amebiasis
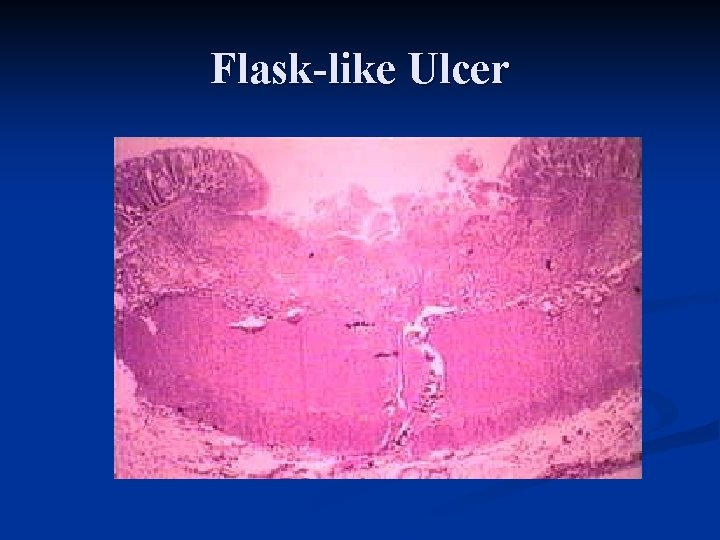
Flask-like Ulcer
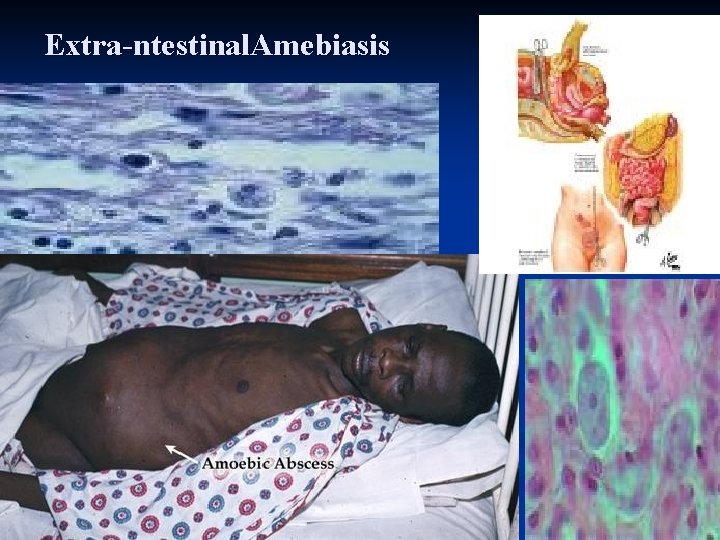
Extra-ntestinal. Amebiasis
Pyogenic- Liver Abscess

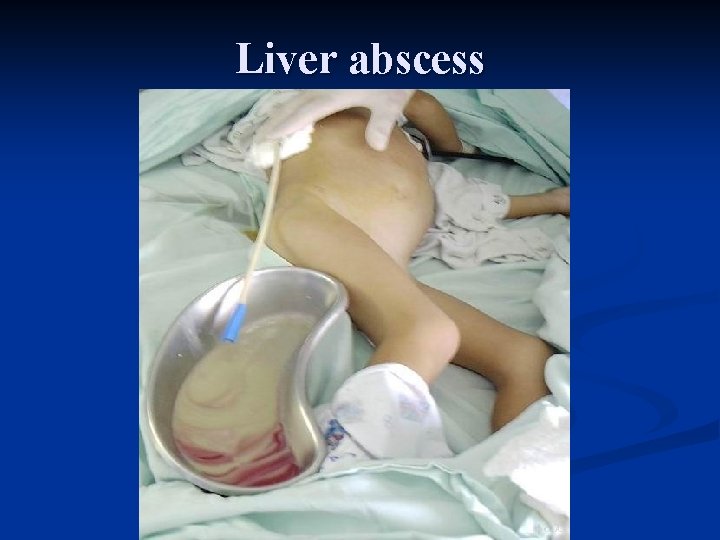
Liver abscess
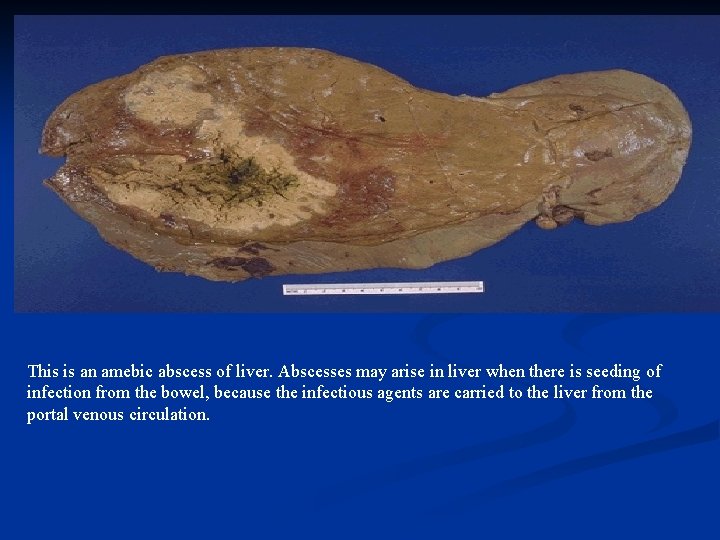
This is an amebic abscess of liver. Abscesses may arise in liver when there is seeding of infection from the bowel, because the infectious agents are carried to the liver from the portal venous circulation.
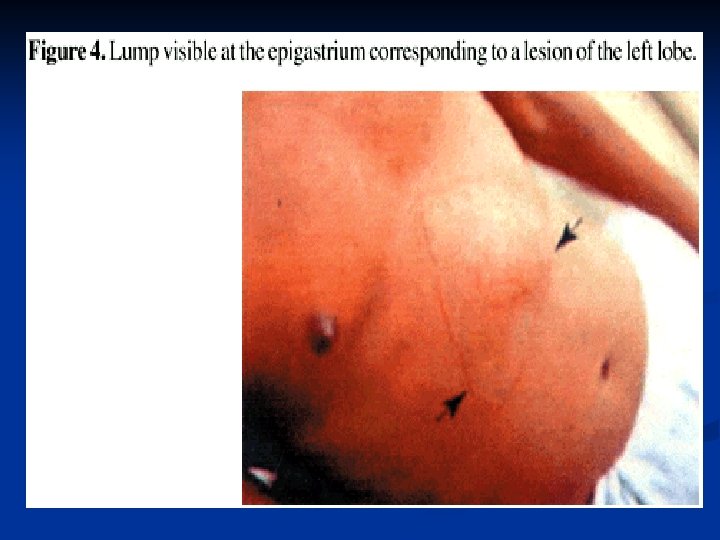

Diagnosis Paraclinical Diagnosis: n Sigmoidoscopic examination: precence of a grossly normal mucosa between the ulcers serves to n differentiate amebic from bacillary dysentery, ( the entire mucosa being involvoed in bacillary dysentery). Hepatomegally n C. B. C. : leukocytosis in Amebic dys. rises above 12000 per microliter, but counts may reach 16000 to 20000 per microliter. n

Laboratory Diagnosis n Entamoeba histolytica must be differentiated from other intestinal protozoa including: E. coli, E. hartmanni, E. dispare, …… n Differentiation is possible, but not always easy, based on morphologic characteristics of the cysts and trophozoites. n The nonpathogenic Entamoeba dispar, however, is morphologically identical to E. histolytica, and differentiation must be based on isoenzymatic or immunologic analysis. n Molecular methods are also useful in distinguishing between E. histolytica and E. dispar and can also be used to identify E. polecki.

Microscopy Microscopic identification This can be accomplished using: n n Fresh stool: wet mounts and permanently stained preparations (e. g. , trichrome). n Concentrates from fresh stool: wet mounts, with or without iodine stain, and permanently stained preparations (e. g. , trichrome).
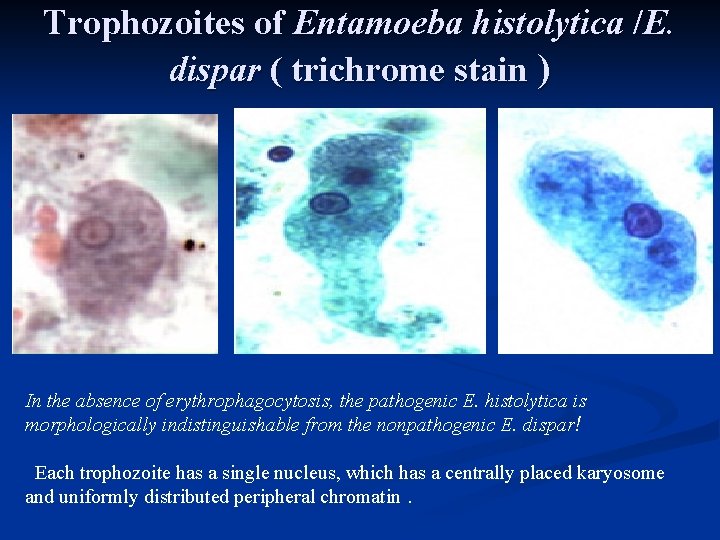
Trophozoites of Entamoeba histolytica /E. dispar ( trichrome stain ) Microscopy B A In the absence of erythrophagocytosis, the pathogenic E. histolytica is morphologically indistinguishable from the nonpathogenic E. dispar! Each trophozoite has a single nucleus, which has a centrally placed karyosome and uniformly distributed peripheral chromatin.
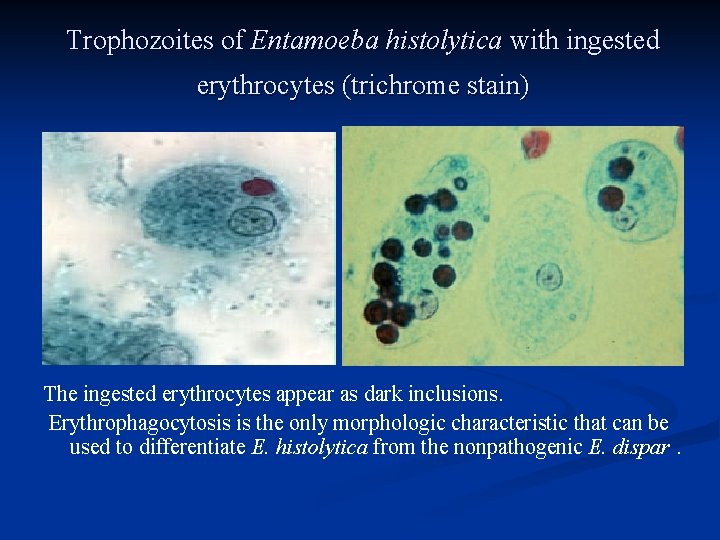
Trophozoites of Entamoeba histolytica with ingested erythrocytes (trichrome stain) E F The ingested erythrocytes appear as dark inclusions. Erythrophagocytosis is the only morphologic characteristic that can be used to differentiate E. histolytica from the nonpathogenic E. dispar.
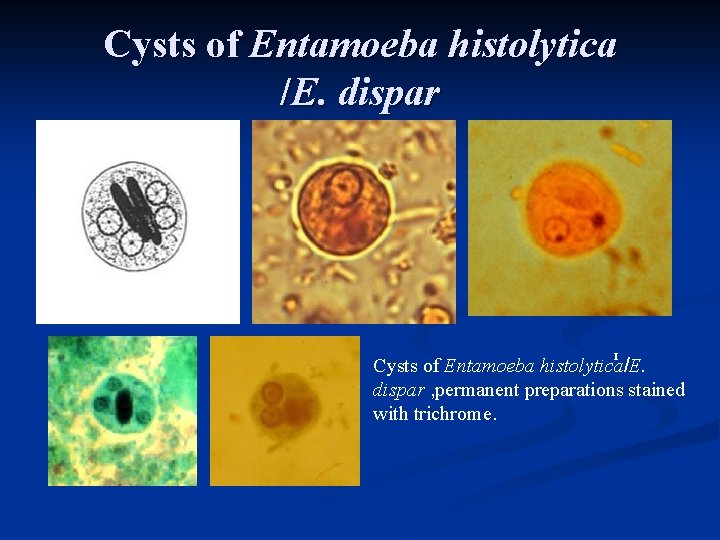
Cysts of Entamoeba histolytica /E. dispar n GHI H I Cysts of Entamoeba histolytica/E. dispar , permanent preparations stained with trichrome.

Immunodiagnosis (Antibody Detection) n 1 - Antibody detection n 2 - Antigen detection may be useful as an adjunct to microscopic diagnosis n The indirect hemagglutination (IHA) n The EIA test detects antibody specific for E. histolytica in approximately 95% of patients with extraintestinal amebiasis, 70% of patients with active intestinal infection, and 10% of asymptomatic persons who are passing cysts of E. histolytica.

Antigen Detection Antigen detection may be useful as an adjunct to microscopic diagnosis in detecting parasites and to distinguish between pathogenic and nonpathogenic infections. Recent studies indicate improved sensitivity and specificity of fecal antigen assays with the use of monoclonal antibodies which can distinguish between E. histolytica and E. dispar infections.

Molecular diagnosis n In reference diagnosis laboratories, PCR is the method of choice for discriminating between the pathogenic species (E. histolytica) from the (nonpathogenic species) E. dispar.

Treatment n Intestinal Amebiasis: n *Asymptomatic amebiasis(cyst passer): Diloxanide furoate ( furamide) 500 mg 3 times daily / 10 days n *Symptomatic amebiasis ( troph. & cyst): - Iodoquinol , 650 mg 3 times daily/ 20 days or Metronidazole (Flagyl) , 750 mg 3 times daily/ 10 days n *Amebic colitis: Chloroquine, 250 mg 2 times daily n * Acute amebic dysentery: Emetine hydrochloride, 1 mg/kg daily IM or SC

Treatment n Extraintestinal Amebiasis: n *Amebic liver abscess, ameboma: Metronidazole, as above plus dehydroemetine / 10 days or Metronidazole or dehydroemetine as above plus Chloroquine , 500 mg 2 times daily / 2 days, …. .

- Slides: 34