ALS Algorithm Learning outcomes This lecture should enable

ALS Algorithm

Learning outcomes This lecture should enable you to: • Describe the ALS algorithm • Recognise the importance of high quality chest compressions • Discuss the treatment of shockable and non-shockable rhythms • Define when to give drugs during cardiac arrest • Identify the treatment of potentially reversible causes of cardiac arrest • Discuss the roles within a resuscitation team

Resuscitation team • roles planned in advance • identify team leader • importance of non-technical skills • • task management team working situational awareness decision making • structured communication • debrief after event
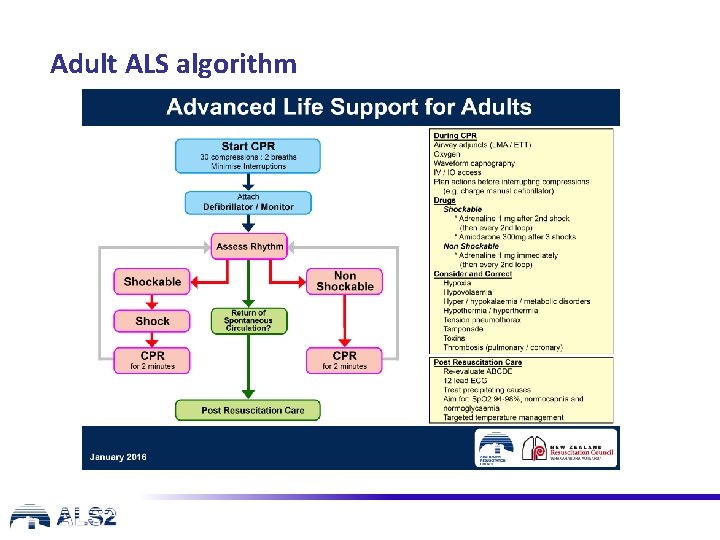
Adult ALS algorithm

To confirm cardiac arrest… • patient response • open airway • check for normal breathing • Caution agonal breathing • No longer than 10 seconds • check circulation • At same time as checking breathing • If doubt about pulse = not present • monitoring

Cardiac arrest confirmed
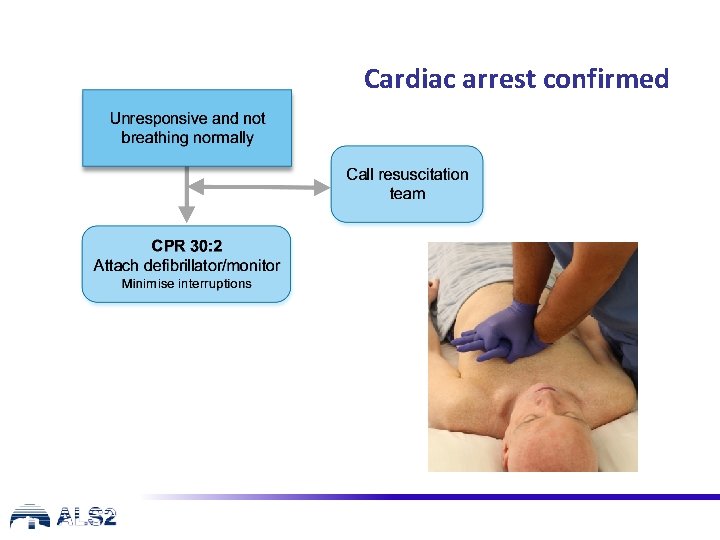
Cardiac arrest confirmed
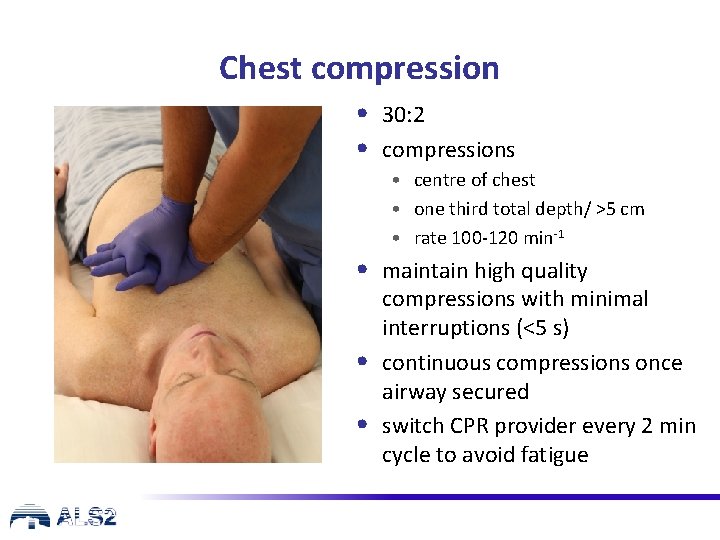
Chest compression • 30: 2 • compressions • centre of chest • one third total depth/ >5 cm • rate 100 -120 min-1 • maintain high quality • • compressions with minimal interruptions (<5 s) continuous compressions once airway secured switch CPR provider every 2 min cycle to avoid fatigue
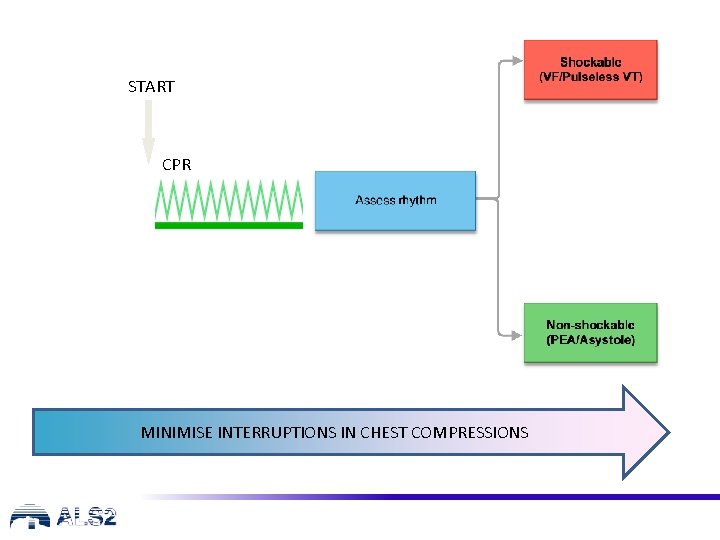
START CPR MINIMISE INTERRUPTIONS IN CHEST COMPRESSIONS
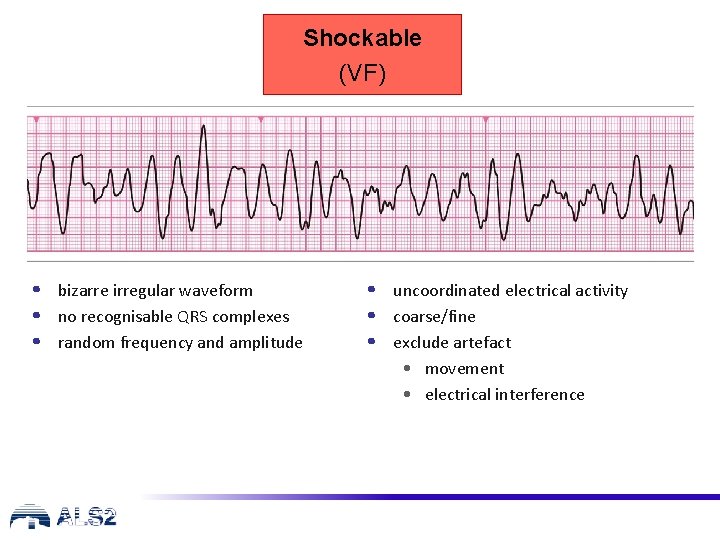
Shockable (VF) • bizarre irregular waveform • no recognisable QRS complexes • random frequency and amplitude • uncoordinated electrical activity • coarse/fine • exclude artefact • movement • electrical interference
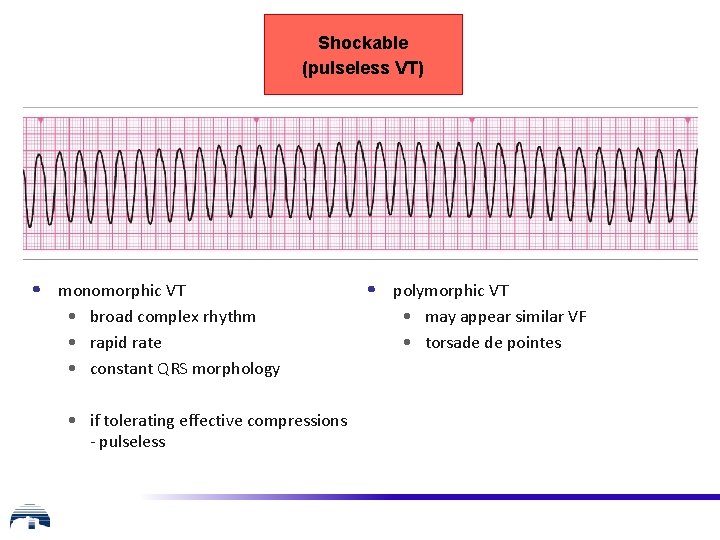
Shockable (pulseless VT) • monomorphic VT • broad complex rhythm • rapid rate • constant QRS morphology • if tolerating effective compressions - pulseless • polymorphic VT • may appear similar VF • torsade de pointes
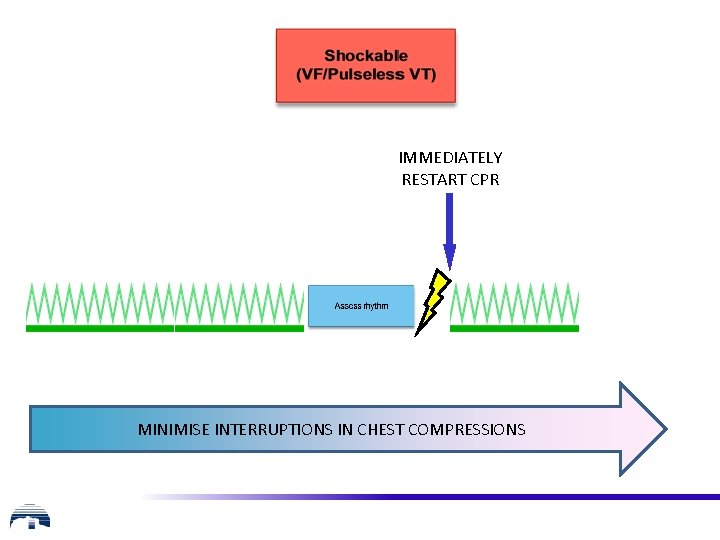
IMMEDIATELY RESTART CPR MINIMISE INTERRUPTIONS IN CHEST COMPRESSIONS

Manual Mode Defibrillator Operation • learn in defibrillation station • safety first – teamwork vital • wording / exact language used is less important than communicating principles to ensure safety

Defibrillation energies • vary with manufacturer check local equipment - • default energy level for adults is set at 200 J for all shocks • If first shock unsuccessful it is reasonable to increase to 360 J for following shocks • energy levels for defibrillators on this course…

If VF/p. VT persists Deliver 2 nd shock • 2 nd and subsequent shocks • 200 – 360 J biphasic CPR for 2 min During CPR Adrenaline 1 mg IV/IO Deliver 3 rd shock CPR for 2 min During CPR Amiodarone 300 mg IV/IO • give adrenaline after 2 nd shock during CPR • then every second loop • give amiodarone after 3 shocks during CPR • do not need to be sequential
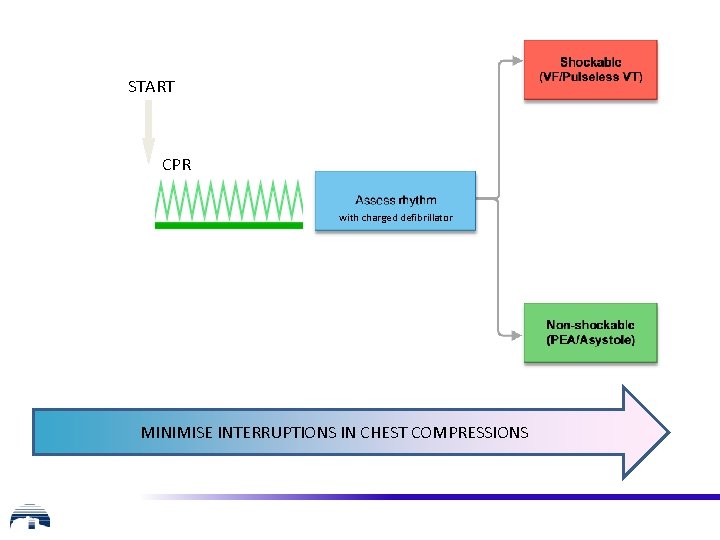
START CPR with charged defibrillator MINIMISE INTERRUPTIONS IN CHEST COMPRESSIONS
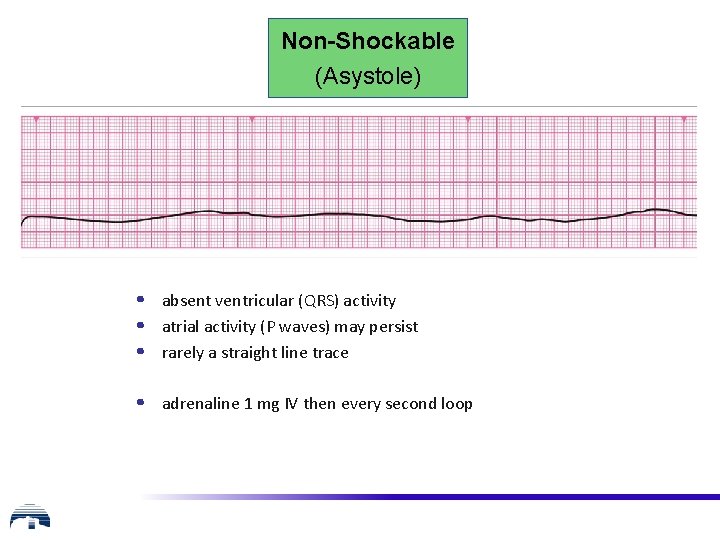
Non-Shockable (Asystole) • absent ventricular (QRS) activity • atrial activity (P waves) may persist • rarely a straight line trace • adrenaline 1 mg IV then every second loop
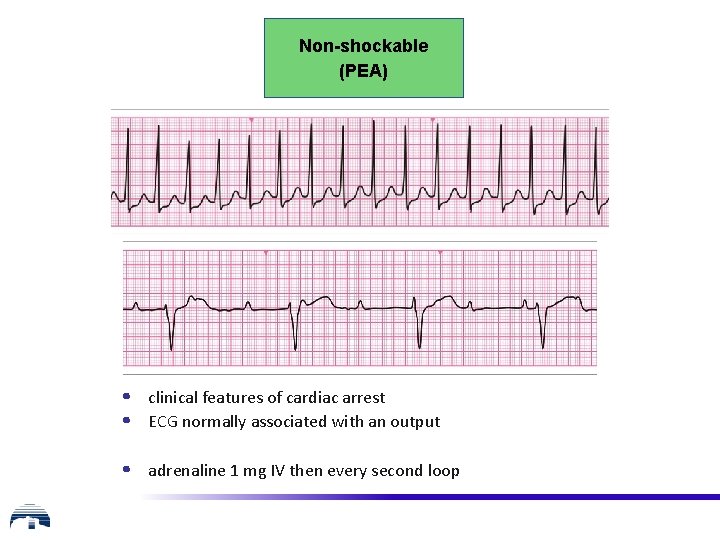
Non-shockable (PEA) • clinical features of cardiac arrest • ECG normally associated with an output • adrenaline 1 mg IV then every second loop
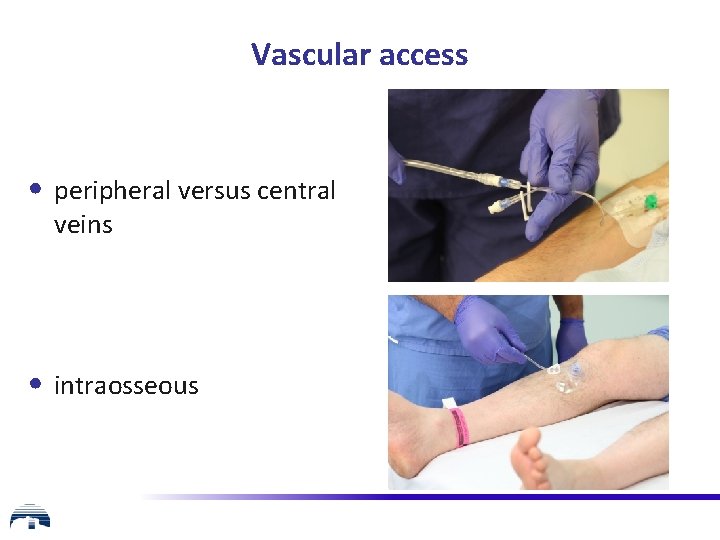
Vascular access • peripheral versus central veins • intraosseous

Airway and ventilation • secure airway: • supraglottic airway device (e. g. LMA, i-gel) • tracheal tube • do not attempt intubation unless trained and competent to do so • once airway secured, if possible, do not interrupt chest compressions for ventilation • avoid hyperventilation • waveform capnography
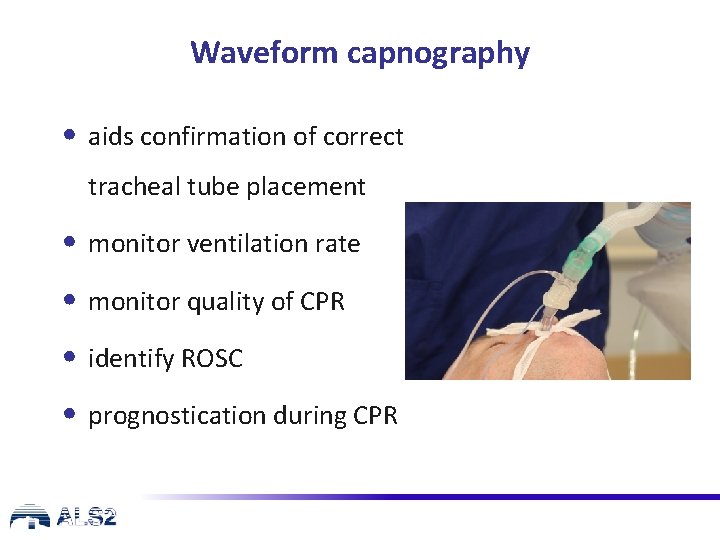
Waveform capnography • aids confirmation of correct tracheal tube placement • monitor ventilation rate • monitor quality of CPR • identify ROSC • prognostication during CPR
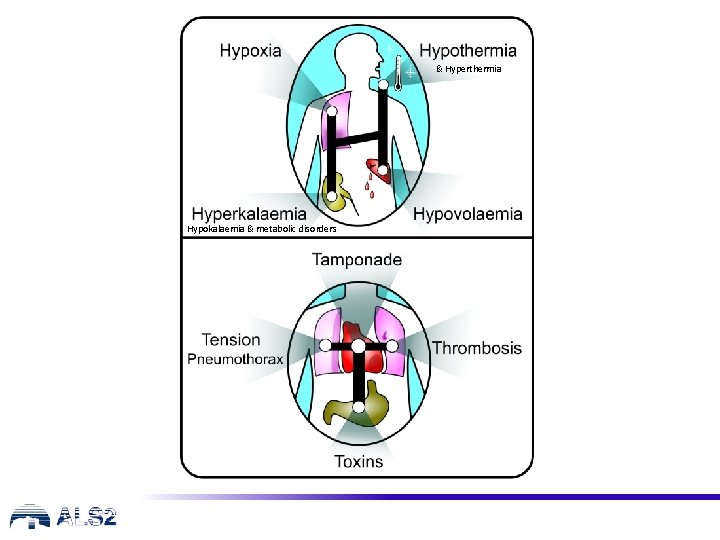
& Hyperthermia Hypokalaemia & metabolic disorders

Hypoxia • seek evidence of Hypoxia • history • pre-arrest Sp. O 2 and other observations

Oxygen in Cardiopulmonary Arrest • ensure patent airway • give as much oxygen as possible • No evidence in adults on best Fi. O 2 • Sp. O 2 measurement dependent on perfusion • consider advanced airway • avoid hyperventilation
Hypovolaemia • seek evidence of Hypovolaemia • history • examination - haemorrhage? - internal/external haemorrhage - check surgical drains • other Hypovolaemia causes • including • sepsis • anaphylaxis

Hypovolaemia • control haemorrhage • if Hypovolaemia suspected, give intravenous fluids/blood • blood loss • IV fluids and plan for emergency blood transfusion • distributive shock • IV fluids • restriction to flow (e. g. Thrombus/Tamponade/Pneumothorax/Pregnancy) • consider IV fluids with otherapeutic measures

Hypo/hyperkalaemia and metabolic disorders • seek evidence • examination • near patient testing for K+ and glucose • history • check latest laboratory results • medical history • drug chart • fluid input/output chart

Potassium Disorders • Hyperkalaemia • calcium chloride • calcium gluconate – if chloride unavailable • IV/IO insulin (10 units - short acting) / dextrose (25 g) • IV fluids • consider sodium bicarbonate • Hypokalaemia/ hypomagnesaemia • electrolyte supplementation • KCL 5 mmol bolus and consider 2 g Mg++

Hypothermia • rare if patient is an in-patient • evidence • touch patient and then take core temperature • use low reading thermometer • treat with active rewarming techniques • avoid warm IV fluids in pre-hospital setting • consider cardiopulmonary bypass /ECMO

Hyperthermia • core temp >40. 6 C • consider cause: • prolonged exercise in hot conditions/dehydration • drug toxicity, MDMA, malignant hyperthermia, thyroid storm • heat stroke can resemble septic shock • rhabdomyolysis, coagulopathy issues

Hyperthermia Treatment • rapid cooling to 39 C (similar techniques to TTM) • large fluid volumes – & correct electrolyte abnormalities/acidosis • no specific medications for heat stroke effective – dantrolene for anaesthetic agent reactions (and some MDMA)
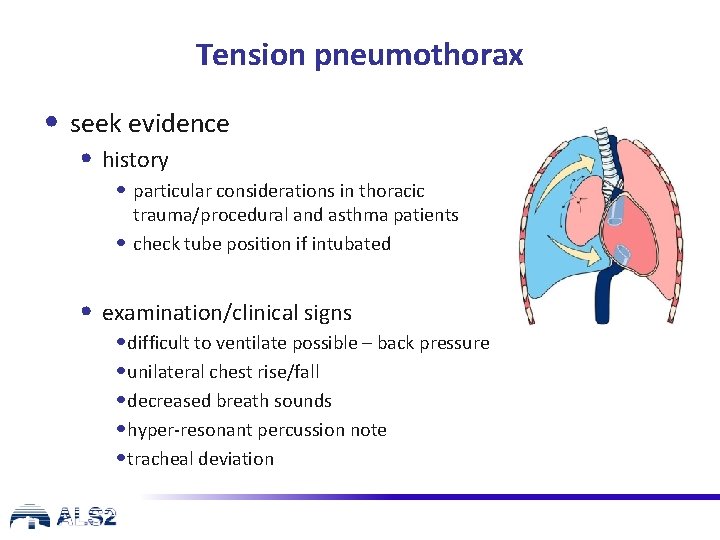
Tension pneumothorax • seek evidence • history • particular considerations in thoracic trauma/procedural and asthma patients • check tube position if intubated • examination/clinical signs • difficult to ventilate possible – back pressure • unilateral chest rise/fall • decreased breath sounds • hyper-resonant percussion note • tracheal deviation
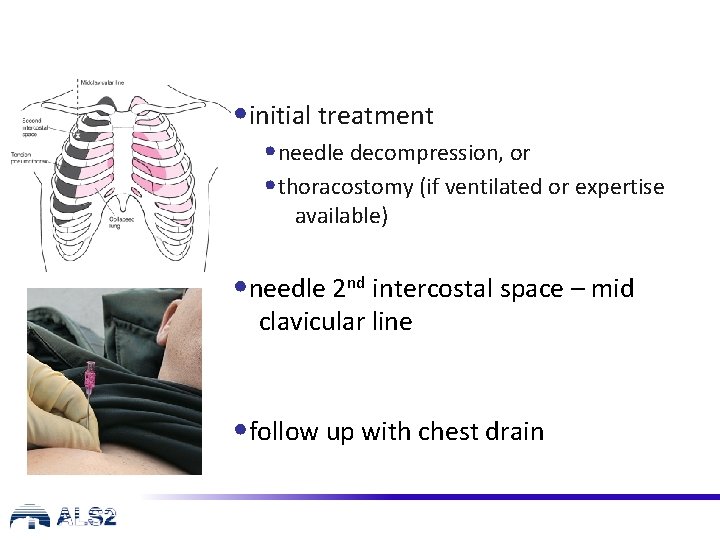
• initial treatment • needle decompression, or • thoracostomy (if ventilated or expertise available) • needle 2 nd intercostal space – mid clavicular line • follow up with chest drain
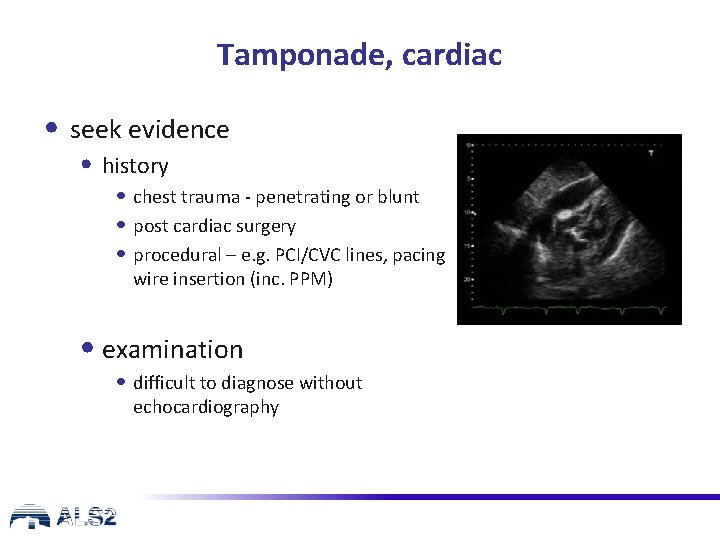
Tamponade, cardiac • seek evidence • history • chest trauma - penetrating or blunt • post cardiac surgery • procedural – e. g. PCI/CVC lines, pacing wire insertion (inc. PPM) • examination • difficult to diagnose without echocardiography
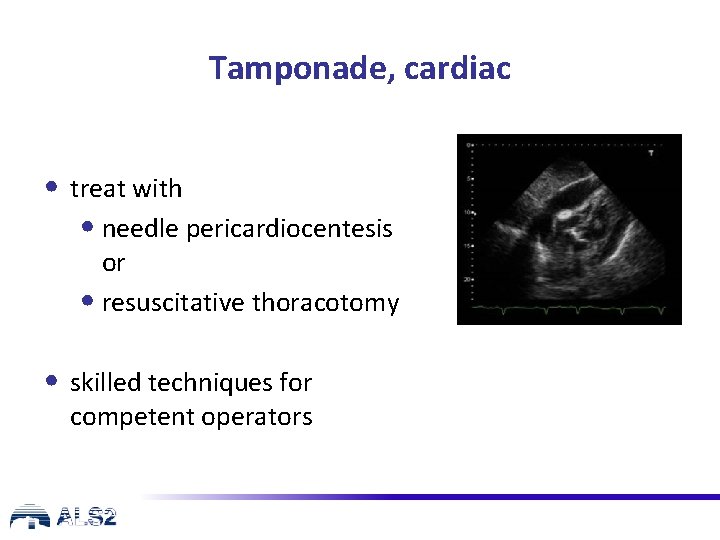
Tamponade, cardiac • treat with • needle pericardiocentesis or • resuscitative thoracotomy • skilled techniques for competent operators
Thrombosis • seek evidence • history • examination • ultrasound may help
Thrombosis • if high clinical probability for PE consider fibrinolytic therapy • percuteanous intervention • coronary • pulmonary • if fibrinolytic therapy given – minimum of 30 minutes CPR – consideration for continuing CPR for up to 60 -90 minutes

Toxins • seek evidence • History • review medication charts • rare unless evidence of deliberate • overdose recreational drugs complicated by purity / polypharmacy • examination • difficult

Toxins • specific antidotes • evidence during arrest poor

Other considerations during CPR • ultrasound • mechanical chest compression devices if • prolonged CPR • facilitate transport • facilitate safe angiography/radiological intervention • extracorporeal CPR

Ultrasound • in skilled hands may identify reversible causes • obtain images during safely • do not interrupt CPR
Post Resuscitation Care Re-evaluate ABCDE 12 lead ECG Treat precipitating causes Aim for: Sp. O 2 94 -98%, normocapnia and normoglygaemia Targeted temperature management

Any questions?

Summary • the ALS algorithm • importance of high quality chest compressions • potentially reversible causes of cardiac arrest • role of resuscitation team

Advanced Life Support Course Slide set All rights reserved © Australian Resuscitation Council (January 2016)
- Slides: 45