ALLERGY AN OVERVIEW Contents q Allergy q Hypersensitivity



















- Slides: 37

ALLERGY: AN OVERVIEW

Contents q Allergy q Hypersensitivity q Allergy: Ig. E Mediated: Type I q Immunopathogenesis q Performed Mediators q Food Hypersensitivity q Laboratory Tests q Prevention q Treatment

Allergy § Type of hypersensitivity reactions of the immune system. Allergy may involve more than one type of reaction. § An allergy is a reaction to something that does not affect most other people. Substances that often cause reactions are Pollen Dust mites Mold spores Pet dander Food Insect stings Medicines ……. q q q q Mechanisms of tissue injury are the same as the effector mechanisms of defense against infectious pathogens • • The problem is that these reactions are poorly controlled

Allergy Risk factor §Host factors; heredity, gender, race, and age §HLA and non-HLA genes § Environmental factor; infectious diseases during early childhood, environmental pollution, allergen levels and dietary changes.

Allergens • Allergens bind to Ig. E and trigger degranulation of chemical mediators. Characteristics of allergens • Small 15 -40, 000 MW proteins. • Specific protein components. • Low dose of allergen are sufficient to trigger the reaction • Most allergens promote a Th 2 immune response

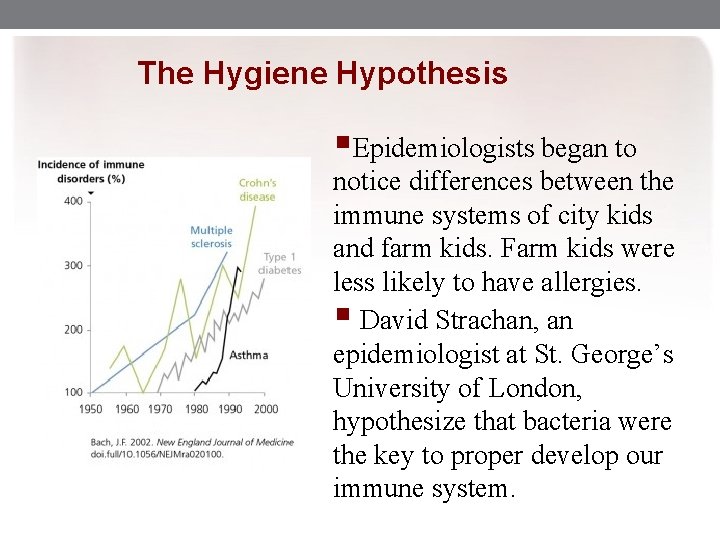
The Hygiene Hypothesis §Epidemiologists began to notice differences between the immune systems of city kids and farm kids. Farm kids were less likely to have allergies. § David Strachan, an epidemiologist at St. George’s University of London, hypothesize that bacteria were the key to proper develop our immune system.

Hypersensitivity §Hypersensitivity (hypersensitivity reaction) refers to undesirable immune reactions produced by the normal immune system. §Hypersensitivity reactions require a pre-sensitized (immune) state of the host. §Hypersensitivity reactions: four types; based on the mechanisms involved and time taken for the reaction, a particular clinical condition (disease) may involve more than one type of reaction.

Classification of Immunologic Reactions (Gell and Coombs)

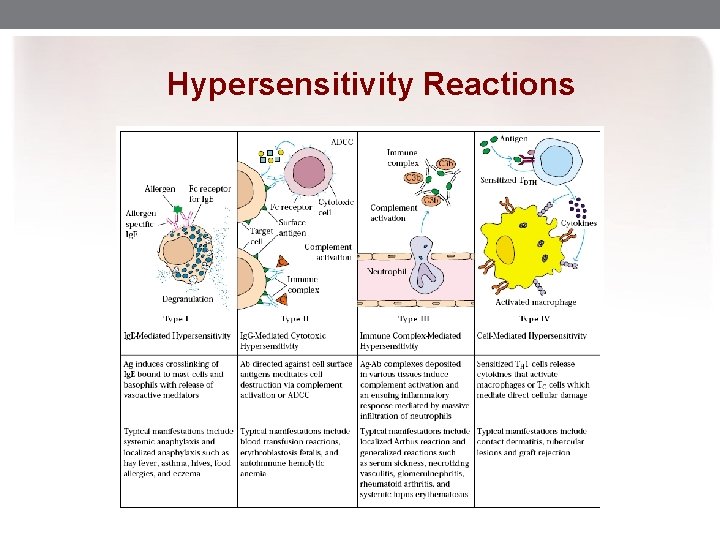
Hypersensitivity Reactions

Ig. E Mediated §Overreaction to an allergen that is contacted through skin, inhaled through lung, swallowed or injected. Individuals must be previously sensitized §Triggered by harmless substances such as; pollen, dust, animal danders, food, … can also occur as a result of drug or bee stings or stings from other insects (an allergen)

Atopy § Atopy is the genetic predisposition to make Ig. E antibodies in response to allergen exposure. § Etiology is unknown but there is strong evidence for a complex of genes with a variable degree of expression encoding protein factors. § Allergic rhinitis, allergic athma, atopic dermatitis are the most common manifestation of atopy. Allergic gastroenteropathy is rara. These manifestation may coexist in the same patients at different times. Atopy can be asymptomatic.

Common allergens associated with type I hypersenstivity § Proteins § Foods q Foreign q Nuts serum q Vaccines § Plant pollens q Rye grass q Ragweed q Timothy grass q Birch trees § Drugs q Penicillin q Sulfonamides q Local anethetics q Salicylates q Seafood q Eggs q Peas, beans q Milk § Insect products q Bee venom q Wasp venom q Ant venom q Cockroach calyx q Dust mites § Mold spores q Animal hair and dander

Mechanism §While first-time exposure may only produce a mild reaction, repeated exposures may lead to more serious reactions. Once a person is sensitized (has had a previous sensitivity reaction), even a very limited exposure to a very small amount of allergen can trigger a severe reaction. §Most occur within seconds or minutes after exposure to the allergen, but some can occur after several hours, particularly if the allergen causes a reaction after it is partially digested. In very rare cases, reactions develop after 24 hours.

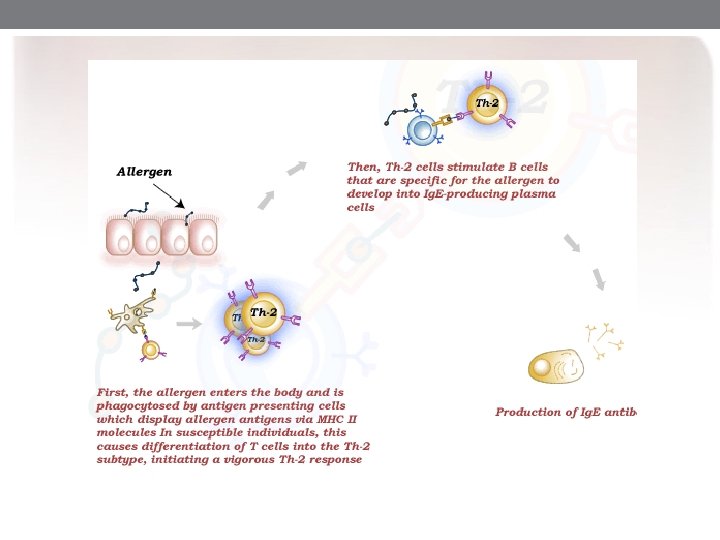
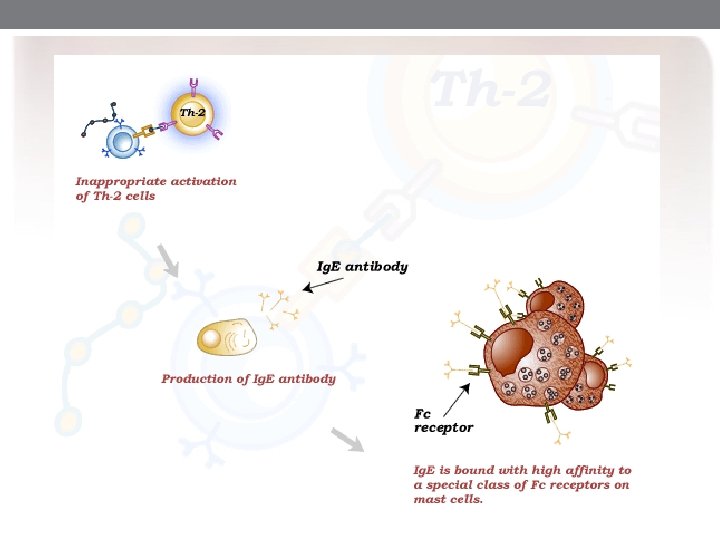
Immunopathogenesis § Both mast cells and basophils are involved in immunopathogenesis of Ig. E mediated diseases. Mast cells and basophils have a high affinity Ig. E cell membrane receptors for Ig. E. § Immediate hypersensitivity reactions are mediated by Ig. E, but T and B cells play important roles in the development of these antibodies

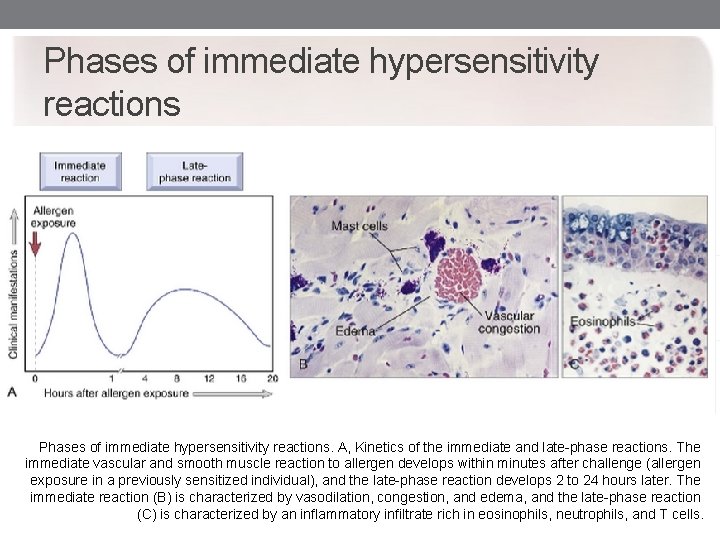
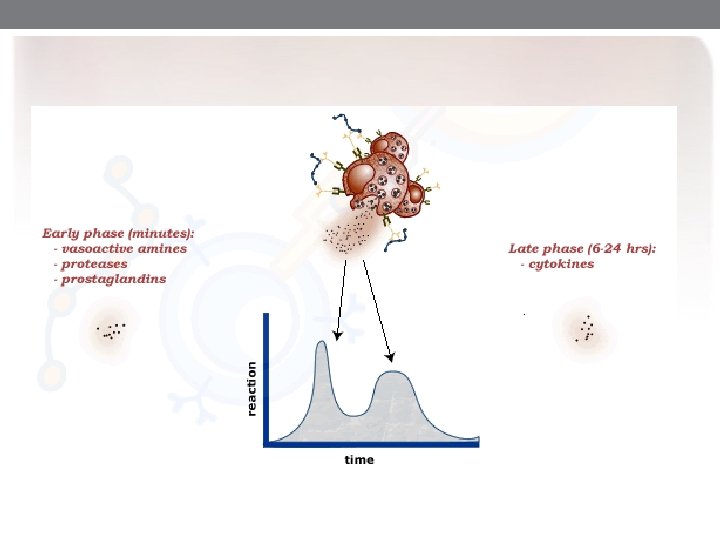
Phases of immediate hypersensitivity reactions. A, Kinetics of the immediate and late-phase reactions. The immediate vascular and smooth muscle reaction to allergen develops within minutes after challenge (allergen exposure in a previously sensitized individual), and the late-phase reaction develops 2 to 24 hours later. The immediate reaction (B) is characterized by vasodilation, congestion, and edema, and the late-phase reaction (C) is characterized by an inflammatory infiltrate rich in eosinophils, neutrophils, and T cells.





Mast Cell §Mast cell are abundant in the mucosa of the respiratory, gastrointestinal tracts and in the skin, where atopic reaction localize. §Mast cell release mediator cause the pathophysiology of the immediate and late phases of atopic diseases.

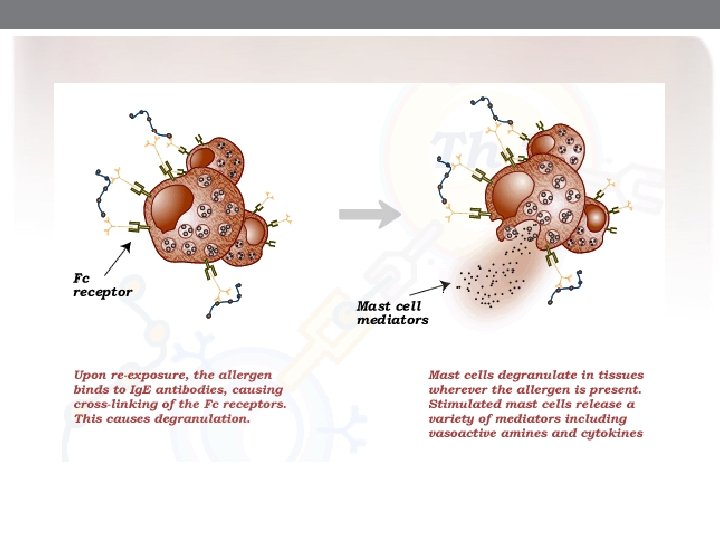
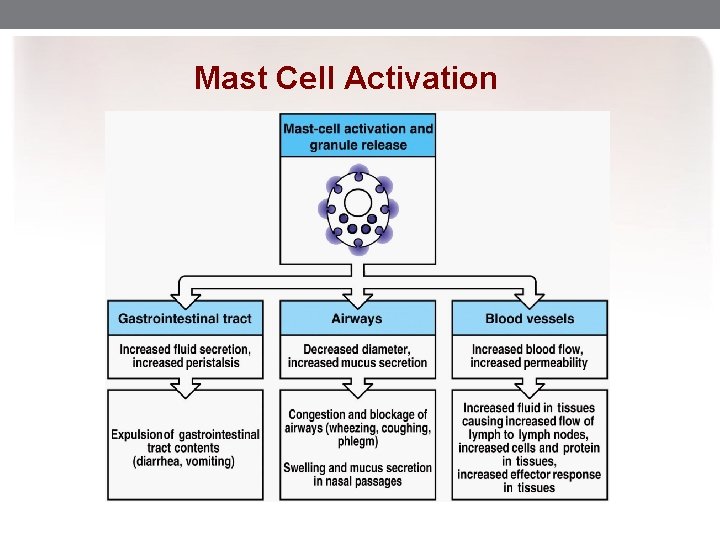
Mast Cell Activation

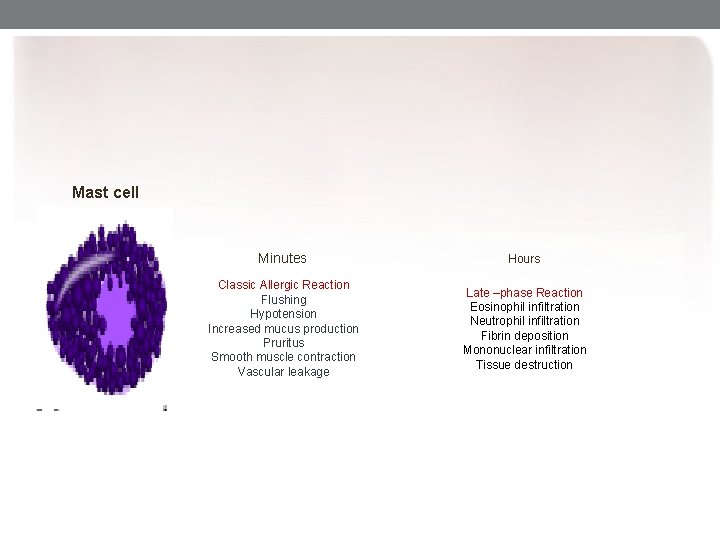
Mast cell Minutes Hours Classic Allergic Reaction Flushing Hypotension Increased mucus production Pruritus Smooth muscle contraction Vascular leakage Late –phase Reaction Eosinophil infiltration Neutrophil infiltration Fibrin deposition Mononuclear infiltration Tissue destruction


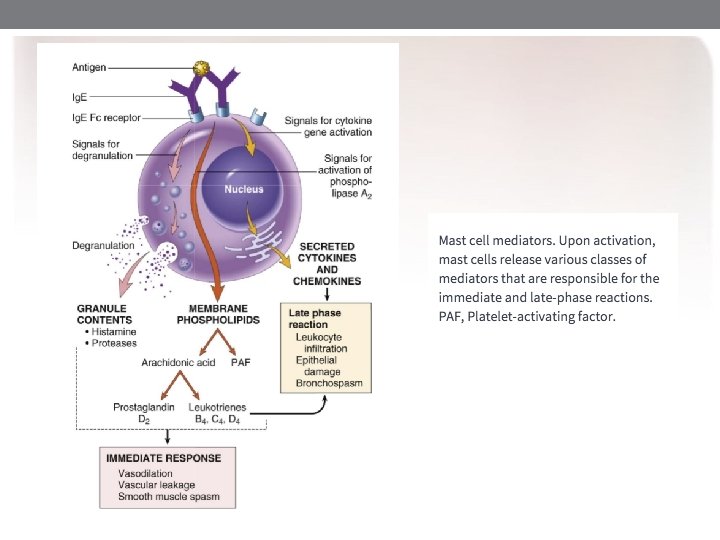
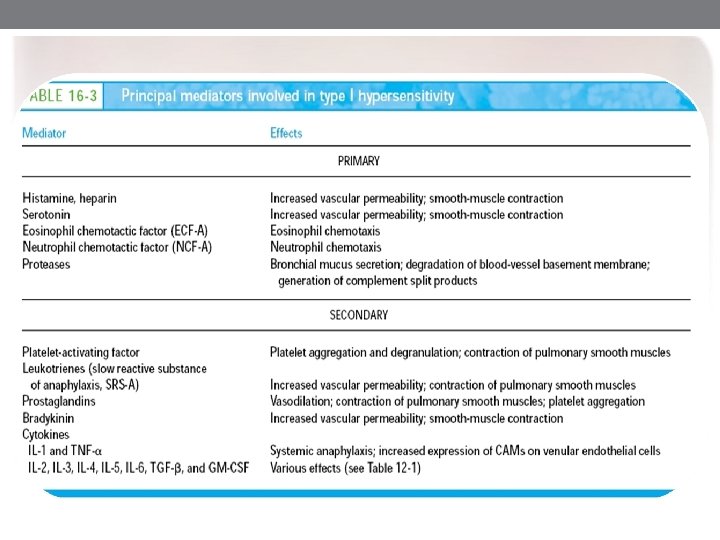
Preformed Mediators/ Primary Mediators Histamine: is one well-known mediator. This mediator acts on histamine 1 (H 1) and histamine 2 (H 2) receptors to cause: contraction of smooth muscles of the airway and GI tract, increased vascular permeability and vasodilation, nasal mucus production, airway mucus production, pruritus, cutaneous vasodilation, and gastric acid secretion. Serotonin: increased vascular permeability and contraction of smooth Muscles. Tryptase: is a major protease released by mast cells; its exact role is uncertain, but it can cleave C 3 and C 3 a. Tryptase is found in all human mast cells but in few other cells and thus is a good marker of mast cell activation. Proteoglycans: include heparin and chondroitin sulfate. Chemotactic factors ………………….

Preformed Mediators/ Secondary Mediators • Platelet activating factor • Leukotriens • Prostaglandinin • Bardykainin • Cytokines • IL 1 , TNF • IL 2, IL 3, IL 4, IL 5, L 6


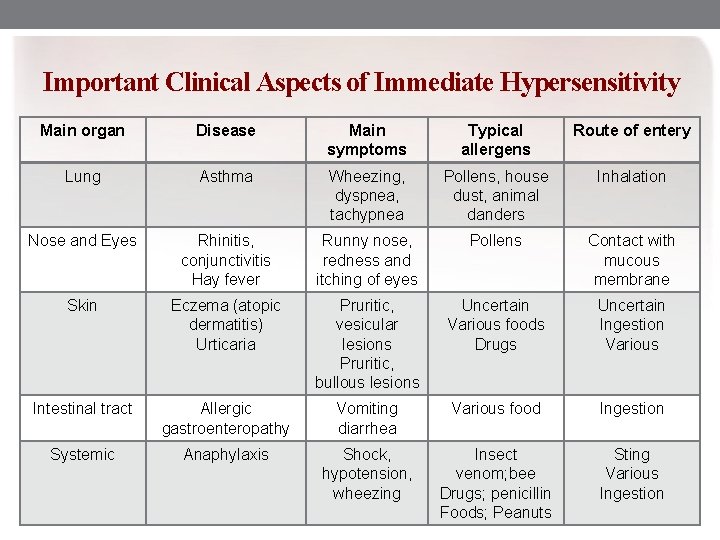
Important Clinical Aspects of Immediate Hypersensitivity Main organ Disease Main symptoms Typical allergens Route of entery Lung Asthma Wheezing, dyspnea, tachypnea Pollens, house dust, animal danders Inhalation Nose and Eyes Rhinitis, conjunctivitis Hay fever Runny nose, redness and itching of eyes Pollens Contact with mucous membrane Skin Eczema (atopic dermatitis) Urticaria Pruritic, vesicular lesions Pruritic, bullous lesions Uncertain Various foods Drugs Uncertain Ingestion Various Intestinal tract Allergic gastroenteropathy Vomiting diarrhea Various food Ingestion Systemic Anaphylaxis Shock, hypotension, wheezing Insect venom; bee Drugs; penicillin Foods; Peanuts Sting Various Ingestion

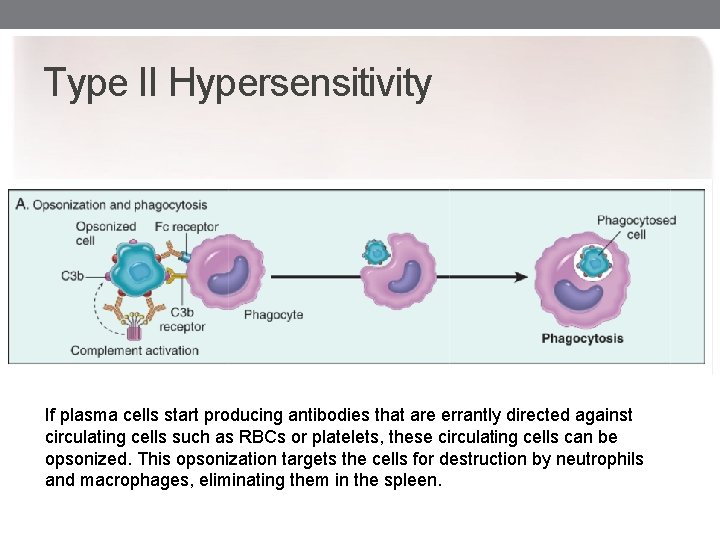
Type II Hypersensitivity If plasma cells start producing antibodies that are errantly directed against circulating cells such as RBCs or platelets, these circulating cells can be opsonized. This opsonization targets the cells for destruction by neutrophils and macrophages, eliminating them in the spleen.

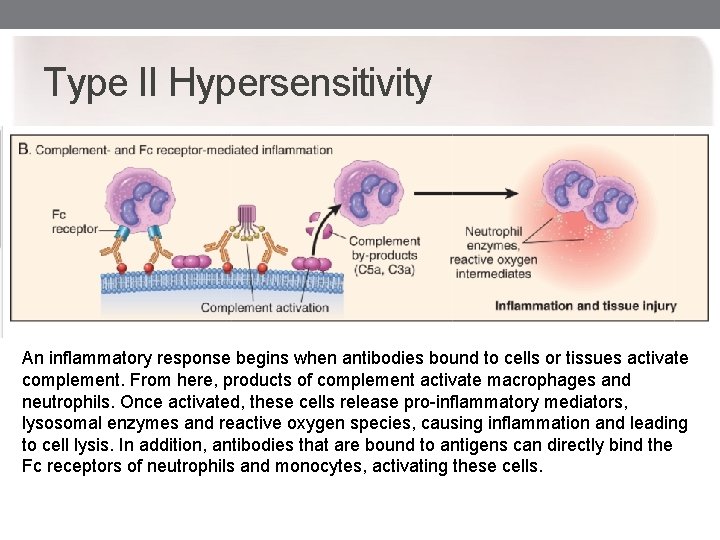
Type II Hypersensitivity An inflammatory response begins when antibodies bound to cells or tissues activate complement. From here, products of complement activate macrophages and neutrophils. Once activated, these cells release pro-inflammatory mediators, lysosomal enzymes and reactive oxygen species, causing inflammation and leading to cell lysis. In addition, antibodies that are bound to antigens can directly bind the Fc receptors of neutrophils and monocytes, activating these cells.

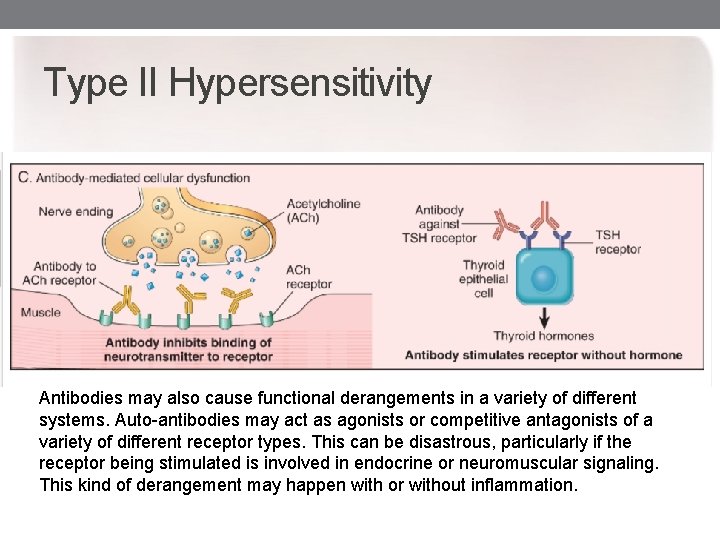
Type II Hypersensitivity Antibodies may also cause functional derangements in a variety of different systems. Auto-antibodies may act as agonists or competitive antagonists of a variety of different receptor types. This can be disastrous, particularly if the receptor being stimulated is involved in endocrine or neuromuscular signaling. This kind of derangement may happen with or without inflammation.

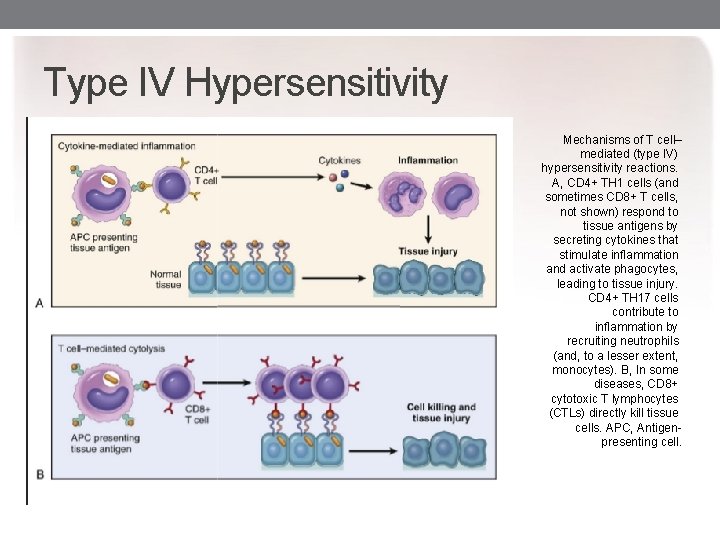
Type IV Hypersensitivity Mechanisms of T cell– mediated (type IV) hypersensitivity reactions. A, CD 4+ TH 1 cells (and sometimes CD 8+ T cells, not shown) respond to tissue antigens by secreting cytokines that stimulate inflammation and activate phagocytes, leading to tissue injury. CD 4+ TH 17 cells contribute to inflammation by recruiting neutrophils (and, to a lesser extent, monocytes). B, In some diseases, CD 8+ cytotoxic T lymphocytes (CTLs) directly kill tissue cells. APC, Antigenpresenting cell.

Laboratory Diagnosis Ig. E-Mediated Allergies Skin Tests Blood Tests

Skin Tests § The cutaneous test § (prick test, puncture test epicutaneous test) § Routine diagnosis in diseases (atopic or anaphylactic). § A single drop of concentrated aqueous allergen extract placed on the skin which is then pricked lightly with a needle point at the center of the drop. After 20 minutes the reaction is graded and recorded

Laboratory Tests §Ig. E levels may be elevated in patients who are atopic, but the level does not necessarily correlate with clinical symptoms. §The tryptase level can be elevated, which is indicative of mast cell degranulation. False-negative results can occur. §An elevated eosinophil count may be observed in patients with atopic disease. §RAST/CAP FEIA (fluorenzymeimmunoassay): measures antigen-specific Ig. E.

Standardized diagnostic allergens are not available for drugs Penicillin is the only drug for which a standardized diagnostic allergen exists. While nonstandardized skin tests can be performed for the minor determinants in penicillin or for other drugs (ie, by pricking the skin where drug solution has been placed), these tests are only useful if findings are positive.

Prevention §Avoid triggers such as foods and medications, …… that have caused an allergic reaction, even a mild one. This includes detailed questioning about ingredients when eating away from home. Ingredient labels should also be carefully examined. §A medical ID tag should be worn by people who know that they have serious allergic reaction. §If any history of a serious allergic reactions, carry emergency medications (such as diphenihydramine and injectable epinephrine). §Do not use your injectable epinephrine on anyone else. They may have a condition (such as a heart problem) that could be affected by this drug.

Treatment • Anaphylaxis: epinephrine (vasoconstriction, bronchospasm resolution), oxygen (intubation sometimes required), anti-histamine, glucocorticoids • Urticaria: anti-histamine, adrenergic agonists • Allergic rhinitis: anti-histamine, adrenergic agonists, glucocorticoids, Immunotherapy • Asthma: • Quick relief: ß-adrenergic agonists to release bronchospams • Long-term control: glucocorticoids