Allergic Rhinitis allergic rhinitis immunology An inflammatory response
















- Slides: 31

Allergic Rhinitis

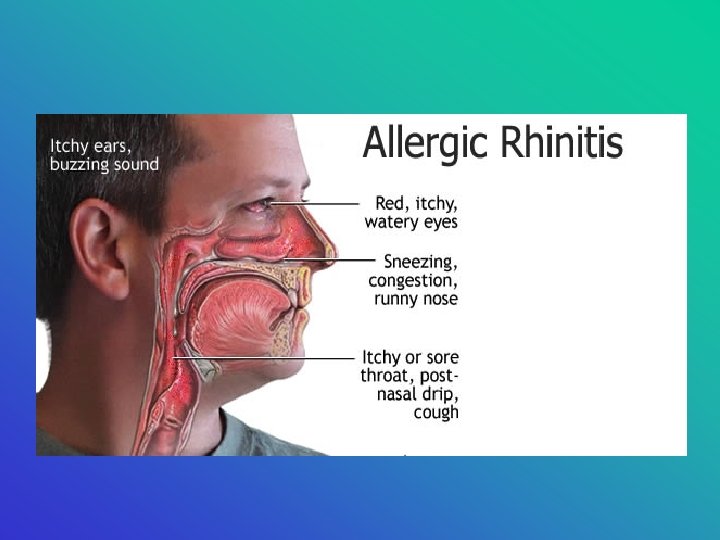
• allergic rhinitis • <immunology> An inflammatory response in the nasal passages to an allergic stimulus. Often includes: nasal congestion, sneezing, runny or itchy nose

Allergic Rhinitis • The most common atopic disease • The hallmark of ~: a temporal relationship between the exposure to allergens & the development of nasal symptoms • It takes at least 2 years of exposure to aeroallergens (airborne environmental allergens) to develop AR (thus, very rare in children <1 year) • The prevalence of AR: lowest in children < 5 yrs highest 2 nd---- 4 th decades • Genetic predisposition (60%)

• • In a sensitized individual, allergic rhinitis occurs when mucous membranes are exposed to inhaled allergenic materials that elicit a specific response mediated by immunoglobulin E (Ig. E). 5

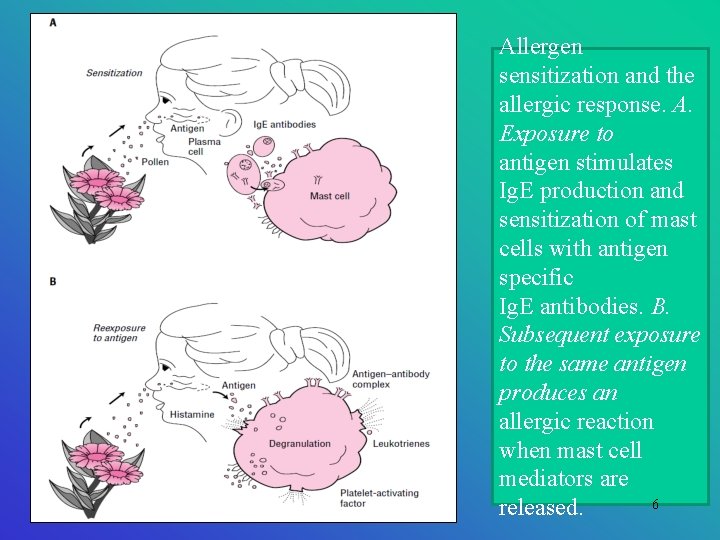
Allergen sensitization and the allergic response. A. Exposure to antigen stimulates Ig. E production and sensitization of mast cells with antigen specific Ig. E antibodies. B. Subsequent exposure to the same antigen produces an allergic reaction when mast cell mediators are 6 released.

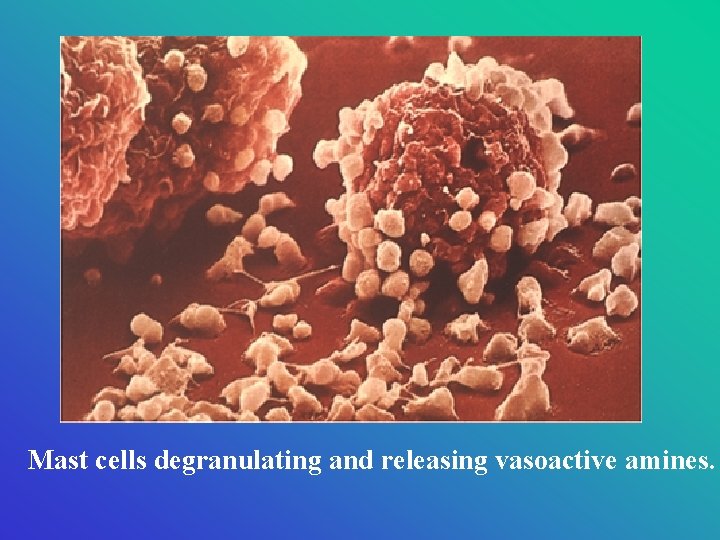
Mast cells degranulating and releasing vasoactive amines.

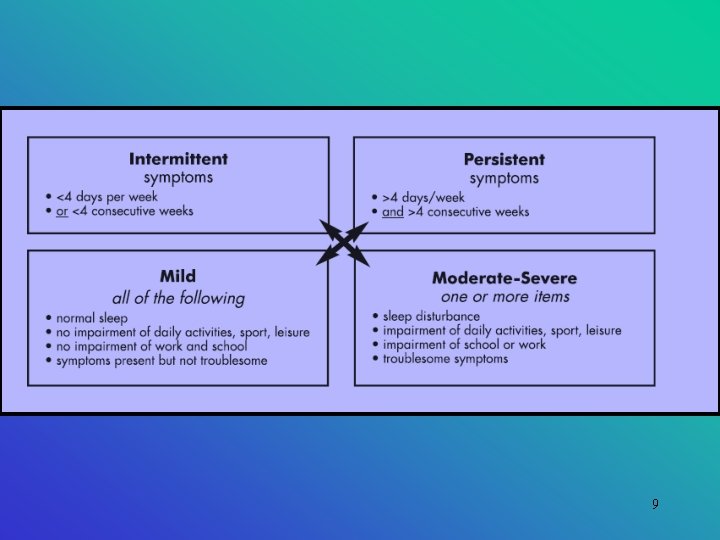
Classification • AR is classified as seasonal or perennial • Seasonal: repetitive and predictable symptoms (severe) • Perennial: symptoms persist throughout the year without any obvious seasonal pattern • WHO: replace terms with intermittent or persistent

9

Allergic Rhinitis • Most patients develop symptoms before age 30 • Asthma develops in about 19% of children with rhinitis (more likely with perrenial allergic rhinitis) • The term “rhinitis” refers to the inflammation of the nasal mucous membranes. Whenever a a causative allergen can be identified allergic rhinitis • It is difficult sometimes to distinguish between different types of rhinitis • Comparison between different types of rhinitis

Features of Common Rhinitis Symptoms Allergic rhinitis Infectious rhinitis Vasomotor rhinitis Rhinitis Medicamentosa Etiology Allergen Viral or bacterial Unknown Tachyphylaxis to topical decongestants Symptoms Rhinorrhea, congestion, sneezing, pruritis, cough with postnasal drip ocular itching etc Fever (more common in children), mucupurulent rhinorrhea, scratchy throat, congestion, cough Rhinorrhea, congestion Congestion Pattern Perennial or seasonal Any time Temporal relationship with use of topical decongestant Associated Factors Concurrent None atopic disease, family history Affects women primarily, strong odours, alcohol, stress, change in humidity and temperature Overuse of topical decongestants, concurrent use of antihypertensive therapy

Perennial Allergic Rhinitis 1 • Caused by continuous exposure to many different types of allergens • Dust Mite the most common cause of perennial allergic rhinitis • Commonly: household dust mites, molds, cockroaches, house pets • Less commonly: cottonseed & flaxseed (found in fertilizers, hair setting preparations and foods); some vegetable gums (found in hair setting prep & foods)

Caused by: Dust mites

Perennial Allergic Rhinitis 2 • Dust mite: thrive in carpets, beddings & reproduce best in warm (18 -21ºC) humid (>50%) environment found in most homes • Mites feed on human skin scales and their own faeces. • Mite itself is not allergen, the main allergen is the glycoprotein that coats their faeces. • Dust mite remain airborne for about 30 minutes after being disturbed • Molds: grow best in warm, moist environment • Cat-derived allergens: light small proteins secreted through the sebaceous glands in the skin. May remain airborne for up to 6 hrs. Can be detected at home even 6 months after removal of the cat.

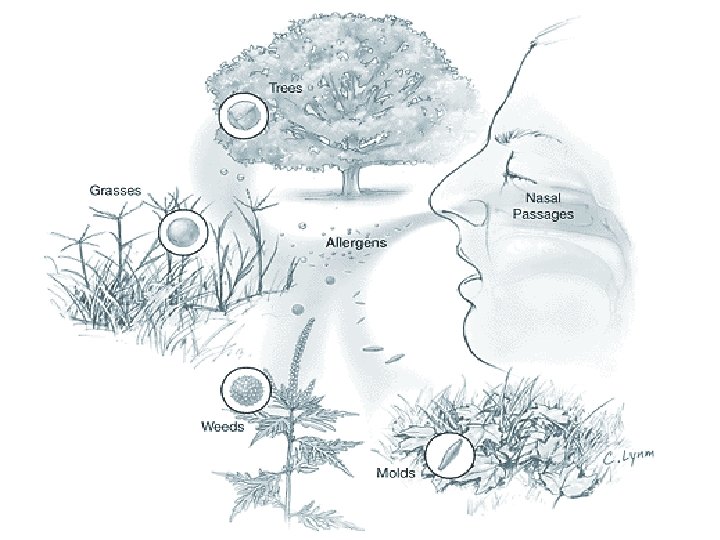
Seasonal Allergic Rhinitis • Caused by wind-borne plant pollens (e. g. tree, grass. etc) • “hay fever”, and “rose fever” are terms related to seasons associated grass pollinosis and NOT associated with FEVER!


Complications 1. 2. 3. • • Sinusitis Recurrent otitis media & hearing loss Patients who develop: fever, purulent nasal discharge, refer to Dr. for evaluation frequent HA, and treatment earache

Symptoms of Allergic Rhinitis • Ocular: itching, lacrimation, mild soreness, puffiness & conjuctival erythema • Nasal: congestion, watery rhinorrhea, itching, sneezing, postnasal drip and nasal pruritus • Head & Neck: loss of taste and smell, mild sore throat due to postnasal drip, earache, sinus HA, itching of the palate and throat • Systemic: malaise & fatigue:


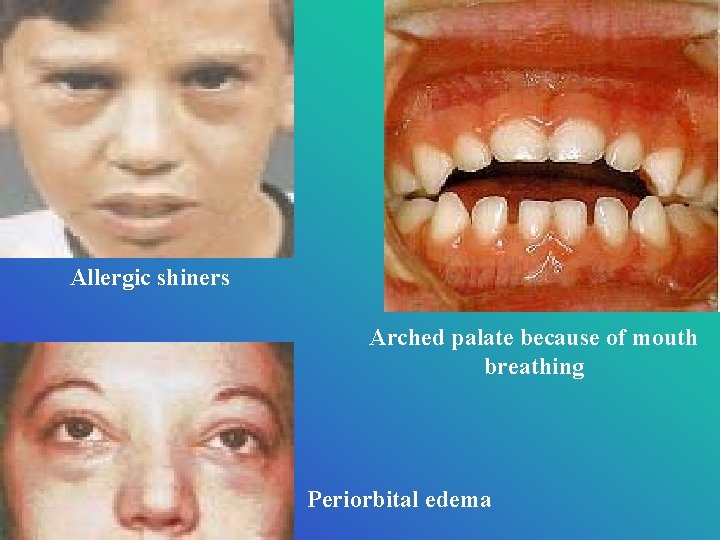
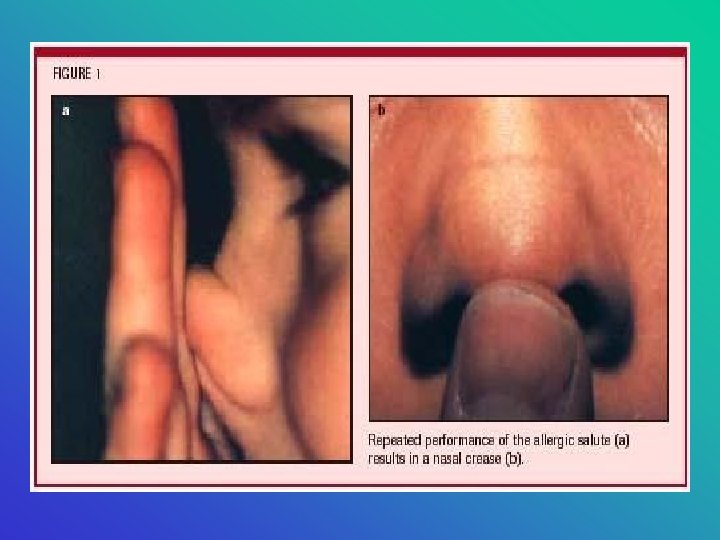
Physical Assessment • “allergic shiners” venous/lymphatic congestion • Chronic mouth breathing highly arched palate • A horizontal crease across the lower third of the nose (in patients repeatedly rub their noses upward) called “nasal salute” • Nasal mucosa: pale & swollen • Nasal secretions: clear & watery • Eyes: watery with scleral & conjuctival erythema and periorbital edema

Allergic shiners Arched palate because of mouth breathing Periorbital edema


23

24

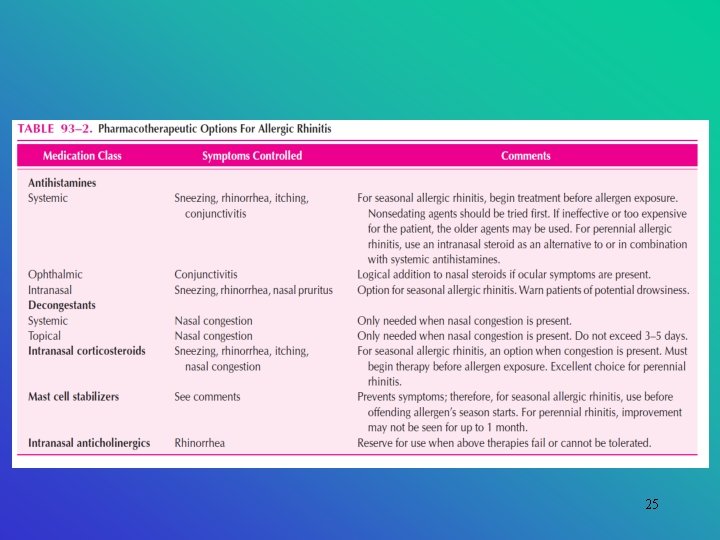
25

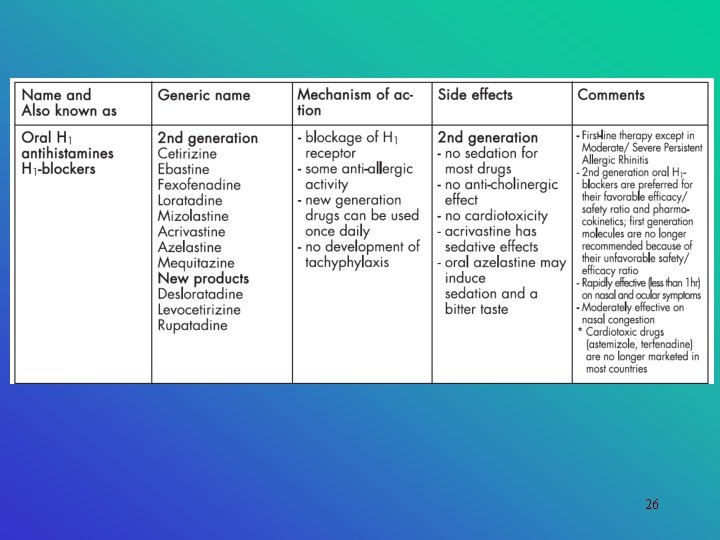
26

27

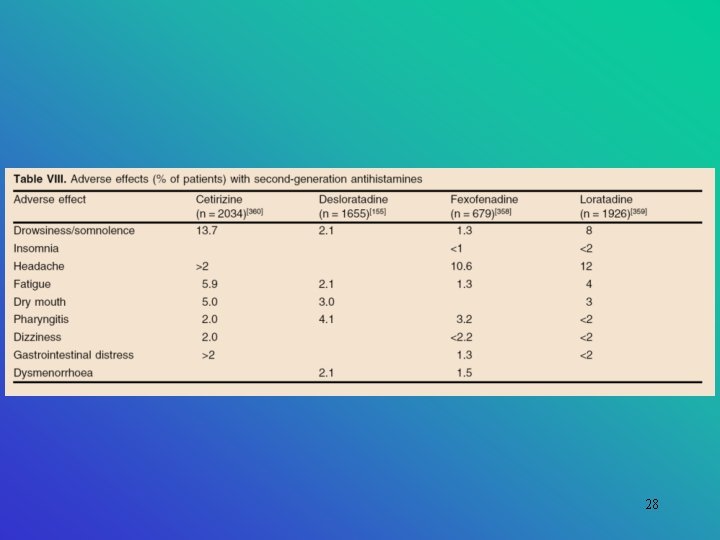
28

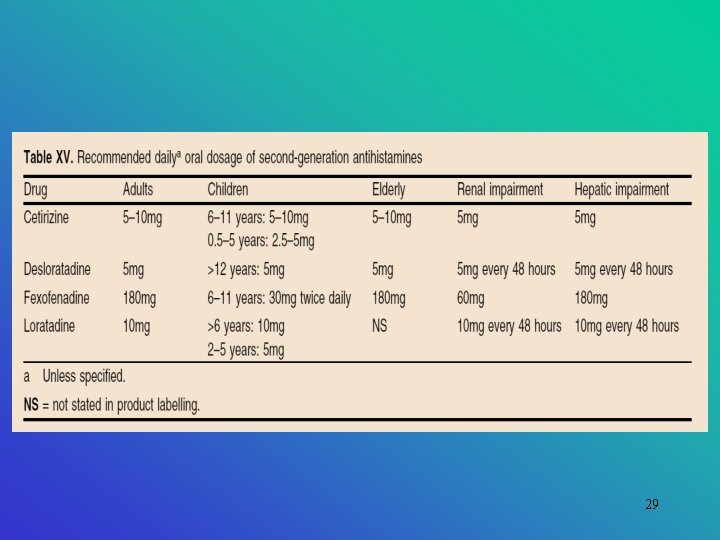
29

30


32