Alcoholic Liver Disease Pathogenesis and New Therapeutic Targets





































- Slides: 38

Alcoholic Liver Disease: Pathogenesis and New Therapeutic Targets By G Sadasiva Rao M. Pharm, (Ph. D) Asst. Professor & HOD Dept. Of pharmacy practice Hindu College of Pharmacy, Gnt, AP.

� in 2014, the World Health Organization or the WHO released its Global Status report on Alcohol and Health. According to the report, about 38. 3 percent of the world’s population is reported to consume alcohol regularly. On an average an individual consumption amounts to 6. 2 litres of alcohol each year. The report only considers individuals over 15 years of age.

�The report says that about 30 percent of India’s population, just less than a third of the country’s populace – consumed alcohol regularly (as of 2010). Some 11 percent are moderate to heavy drinkers. The average Indian consumes about 4. 3 litres of alcohol per annum, says the report. The rural average is much higher at about 11. 4 liters a year.

�According to an Organization for Economic Cooperation and Development (OECD) report released in May 2015, alcoholism increased by about 55 percent between 1992 and 2012. It is a quickly rising concern among the youth of the country.

�Alcohol related deaths and deaths caused by diseases due to alcoholism are a major cause for concern in the country. In 2012 alone about 3. 3 million deaths in India were attributed to alcohol consumption. This amounts to some 5. 9 percent of the global deaths that year.

�Most doctors and health agencies have repeatedly warned Indians of the disastrous health effects of alcohol consumption. Alcoholism is one of the leading causes of liver cirrhosis and failure. About 10 percent of strokes, tuberculosis, hypertension, and epilepsy are caused by excess alcohol consumption.

Introduction � Alcohol consumption is a major risk factor for chronic disease worldwide; � It is also a major cause of chronic liver disease in Western countries. � Alcohol-related liver deaths account for up to 48% of cirrhosis- associated deaths in the United States and are also major contributors to liver disease-related mortality in other countries. � Research on alcoholic liver disease (ALD) has been rapidly growing since the early 1960 s; at that time, Lieber et al used experimental models to show that alcohol is a true hepatotoxin, which causes hepatocellular damage, and that ALD is not simply caused by malnutrition.

� Early studies indicated that ethanol metabolism-associated oxidative stress, glutathione depletion, abnormal methionine metabolism, malnutrition, ethanol-mediated induction of leakage of gut endotoxins, and subsequent activation of Kupffer cells have important roles in the pathogenesis of ALD. � Advanced studies made in the past 10 years in the roles of lipopolysaccharide (LPS) signaling, innate immunity, and transcription factors in the pathogenesis of ALD. � The recent studies showing that alcohol mediates changes in epigenetic features, micro. RNAs (mi. RNAs), and stem cells, which could also contribute to ALD.

Spectrum � ALD presents as a broad spectrum of disorders, ranging from simple fatty liver to more severe forms of liver injury, including alcoholic hepatitis (AH), cirrhosis, and superimposed hepatocellular carcinoma (HCC). � Fatty liver, is an early response to alcohol consumption, develops in most (more than 90%) heavy drinkers, with early-mild steatosis in zone 3 (perivenular) hepatocytes; it can also affect zone 2 and even zone 1 (periportal) hepatocytes when liver injury is more severe. � Interestingly, only about 30% of heavy drinkers develop more severe forms of ALD, such as advanced fibrosis and cirrhosis. � In patients with underlying ALD and heavy alcohol intake, episodes of superimposed AH may occur. In severe cases and in patients with liver cirrhosis, AH leads to severe complications related to liver failure and portal hypertension and has high mortality.

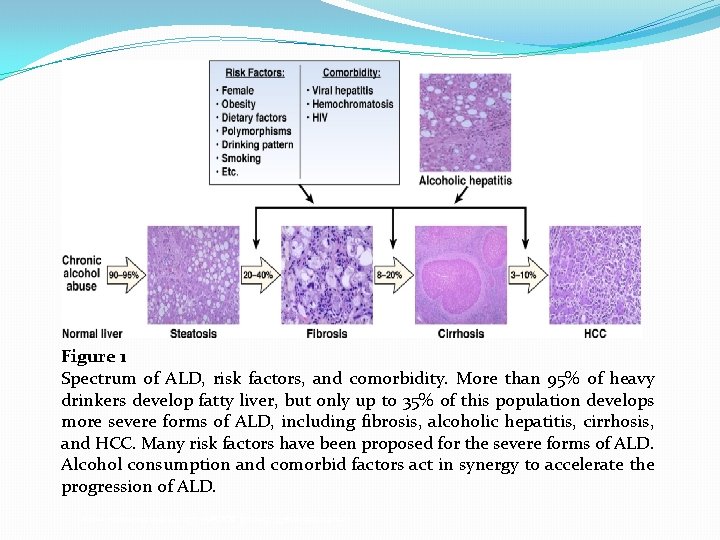
Figure 1 Spectrum of ALD, risk factors, and comorbidity. More than 95% of heavy drinkers develop fatty liver, but only up to 35% of this population develops more severe forms of ALD, including fibrosis, alcoholic hepatitis, cirrhosis, and HCC. Many risk factors have been proposed for the severe forms of ALD. Alcohol consumption and comorbid factors act in synergy to accelerate the progression of ALD. Gastroenterology 2011 141, 1572 -1585 DOI: (10. 1053/j. gastro. 2011. 09. 002)

Risk Factors �The fact that only about 35% of heavy drinkers develop advanced ALD indicates that other factors are involved. Several risk factors for ALD have been identified (Figure 1). These include �Sex, �Obesity, �Quantity of alcohol, �Dietary factors, �Non-sex-linked genetic factors, and �Cigarette smoking

Quantity of alcohol � Among susceptible people, a linear correlation generally exists between the amount and duration of alcohol use and the development of liver disease. � Alcohol content is estimated to be the beverage volume (in m. L) multiplied by its percentage of alcohol. � For example, the alcohol content of 45 m. L of an 80 -proof (40% alcohol) beverage is 18 m. L by volume. Each m. L contains about 0. 79 g of alcohol. � Although values can vary, the percentage of alcohol averages 2 to 7% for most beers and 10 to 15% for most wines. Thus, a 12 -oz glass of beer contains between about 5 to 20 g of alcohol, and a 5 -oz glass of wine contains between about 12 to 18 g, and a 1 1/2 -oz shot of hard liquor contains about 14 g.

�Risk of liver disease increases markedly for men who drink > 40 g, particularly > 80 g, of alcohol/day (eg, about 2 to 8 cans of beer, 3 to 6 shots of hard liquor, or 3 to 6 glasses of wine) for > 10 yr. �For cirrhosis to develop, consumption must usually be > 80 g/day for > 10 yr. If consumption exceeds 230 g/day for 20 yr, risk of cirrhosis is about 50%. �But only some chronic alcohol abusers develop liver disease. Thus, indicating that other factors are involved

Sex �Female sex is a well-documented risk factor for susceptibility to ALD; �The increased risk among women likely results from lower levels of gastric alcohol dehydrogenase, a higher proportion of body fat, and the presence of estrogens. �Women require only 20 to 40 g of alcohol to be at risk —half of that for men.

Genetic factors �Alcoholic liver disease often runs in families, suggesting genetic factors (eg, deficiency of cytoplasmic enzymes that eliminate alcohol). �Variations in genes that encode antioxidant enzymes, cytokines and other inflammatory mediators, and alcohol-metabolizing enzymes could have a role �Recent studies indicate that variations in patatin-like phospholipase domain-containing protein 3 (PNPLA 3) affect development of alcoholic cirrhosis in white alcoholic subjects.

Obesity �Obesity represents another important risk factor that accelerates fibrosis progression and the development of cirrhosis in ALD. � Experimental studies indicate that the synergistic effects of obesity and alcohol abuse involve the endoplasmic reticulum response to cell stress, type I macrophage activation, and adiponectin resistance.

Pathophysiology Alcohol absorption and metabolism �Alcohol (ethanol) is readily absorbed from the stomach, but most is absorbed from the small intestine. Alcohol cannot be stored. �A small amount is degraded in transit through the gastric mucosa, but most is catabolized in the liver, primarily by alcohol dehydrogenase (ADH) but also by cytochrome P 450 2 E 1 (CYP 2 E 1) and the microsomal enzyme oxidation system (MEOS).

Metabolism via the ADH pathway involves the following: �ADH, a cytoplasmic enzyme, oxidizes alcohol into acetaldehyde. Genetic polymorphisms in ADH account for some individual differences in blood alcohol levels after the same alcohol intake but not in susceptibility to alcoholic liver disease. �Acetaldehyde dehydrogenase (ALDH), a mitochondrial enzyme, then oxidizes acetaldehyde into acetate. Chronic alcohol consumption enhances acetate formation. Asians, who have lower levels of ALDH, are more susceptible to toxic acetaldehyde effects (eg, flushing); the effects are similar to those of disulfiram, which inhibits ALDH.

� These oxidative reactions generate hydrogen, which converts nicotinamide-adenine dinucleotide (NAD) to its reduced form (NADH), increasing the redox potential (NADH/NAD) in the liver. � The increased redox potential inhibits fatty acid oxidation and gluconeogenesis, promoting fat accumulation in the liver. � Chronic alcoholism induces the MEOS (mainly in endoplasmic reticulum), increasing its activity. The main enzyme involved is CYP 2 E 1. When induced, the MEOS pathway can account for 20% of alcohol metabolism. This pathway generates harmful reactive O 2 species, increasing oxidative stress and formation of O 2 -free radicals.

Hepatic fat accumulation Fat (triglycerides) accumulates throughout the hepatocytes for the following reasons: �Export of fat from the liver is decreased because hepatic fatty acid oxidation and lipoprotein production decrease. �Input of fat is increased because the decrease in hepatic fat export, increases peripheral lipolysis and triglyceride synthesis, resulting in hyperlipidemia. �Hepatic fat accumulation may predispose to subsequent oxidative damage.

Endotoxins in the gut �Alcohol changes gut permeability, increasing absorption of endotoxins released by bacteria in the gut. In response to the endotoxins, liver macrophages (Kupffer cells) release free radicals, increasing oxidative damage

Oxidative damage Oxidative stress is increased by � Liver hypermetabolism, caused by alcohol consumption � Free radical–induced lipid peroxidative damage � Reduction in protective antioxidants (eg, glutathione, vitamins A and E), caused by alcohol-related undernutrition � Binding of alcohol oxidation products, such as acetaldehyde, to liver cell proteins, forming neoantigens and resulting in inflammation � Accumulation of neutrophils and other WBCs, which are attracted by lipid peroxidative damage and neoantigens � Inflammatory cytokines secreted by WBCs

Resultant inflammation, cell death, and fibrosis � A vicious circle of worsening inflammation occurs: Cell necrosis and apoptosis result in hepatocyte loss, and subsequent attempts at regeneration result in fibrosis. � Stellate cells, which line blood channels (sinusoids) in the liver, proliferate and transform into myofibroblasts, producing an excess of type I collagen and extracellular matrix. � As a result, the sinusoids narrow, limiting blood flow. Fibrosis narrows the terminal hepatic venules, compromising hepatic perfusion and thus contributing to portal hypertension. Extensive fibrosis is associated with an attempt at regeneration, resulting in liver nodules. This process culminates in cirrhosis

Pathology �Fatty liver, alcoholic hepatitis, and cirrhosis are often considered separate, progressive manifestations of alcoholic liver disease. However, their features often overlap. �Fatty liver (steatosis) is the initial and most common consequence of excessive alcohol consumption. Fatty liver is potentially reversible. Macrovesicular fat accumulates as large droplets of triglyceride and displaces the hepatocyte nucleus, most markedly in perivenular hepatocytes. The liver enlarges.

�Alcoholic hepatitis (steatohepatitis) is a combination of fatty liver, diffuse liver inflammation, and liver necrosis (often focal)—all in various degrees of severity. � The damaged hepatocytes are swollen with a granular cytoplasm (balloon degeneration) or contain fibrillar protein in the cytoplasm (Mallory or alcoholic hyaline bodies). �Severely damaged hepatocytes become necrotic. �Sinusoids and terminal hepatic venules are narrowed. �Cirrhosis may also be present

�Alcoholic cirrhosis is advanced liver disease characterized by extensive fibrosis that disrupts the normal liver architecture. �The amount of fat present varies. Alcoholic hepatitis may coexist. The feeble compensatory attempt at hepatic regeneration produces relatively small nodules (micronodular cirrhosis). As a result, the liver usually shrinks. In time, even with abstinence, fibrosis forms broad bands, separating liver tissue into large nodules (macronodular)

HCC �Alcoholic cirrhosis is a major risk factor for HCC. �The mechanisms that contribute to development of HCC in patients with cirrhosis, including alcoholic cirrhosis, are complex and include telomere shortening (which induces chromosomal instability), alterations of the microenvironment and macroenvironment that promote tumor cell survival and proliferation, impairment of hepatocyte proliferation, loss of cell cycle checkpoints, and activation of oncogenic pathways

� What are the complications of alcohol-related liver disease? � Complications from alcohol-related liver disease usually occur after years of heavy drinking. These complications can be serious. � They may include liver related conditions that are a consequence of portal hypertension: � Build up of fluid in the abdomen � Bleeding from veins in the esophagus or stomach � Enlarged spleen � Brain disorders and coma � Kidney failure � Liver cancer

Symptoms � Symptoms of alcoholic liver cirrhosis typically develop when a person is between the ages of 30 and 40 yrs � severe problems appear about a decade later. � Fatty liver is often asymptomatic. In one third of patients, the liver is enlarged and smooth, but it is not usually tender. � Alcoholic hepatitis ranges from mild and reversible to life threatening. Most patients with moderate disease are undernourished and present with fatigue, fever, jaundice, right upper quadrant pain, tender hepatomegaly, and sometimes a hepatic bruit. � Cirrhosis: Symptoms range from those of alcoholic hepatitis to the complications of end-stage liver disease, such as portal hypertension(often with esophageal varices and upper GI bleeding, splenomegaly, ascites, and portosystemic encephalopathy).

Diagnosis � Doctors can diagnose alcoholic liver cirrhosis by first taking a medical history and discussing a person’s history of drinking. A doctor will also run some tests that can confirm a cirrhosis diagnosis. � Anemia (low blood levels due to too little iron) � High blood ammonia level � High blood sugar levels � Leukocytosis (large amount of white blood cells) � Unhealthy liver tissue when a sample is removed from a biopsy and studied in a laboratory � Liver enzyme blood tests that show the level of aspartate aminotransferase (AST) is two times that of alanine aminotransferase (ALT) � Low blood magnesium levels � Low blood potassium levels � Low blood sodium levels � Portal hypertension

Treatment �Abstinence �Supportive care �Corticosteroids and enteral nutrition for severe alcoholic hepatitis �Sometimes transplantation

Abstinence (Restricting alcohol intake) �Abstinence is the most important therapeutic intervention for patients with ALD. � Abstinence has been shown to improve the outcome and histological features of hepatic injury, to reduce portal pressure and decrease progression to cirrhosis, and to improve survival at all stages in patients with ALD �Drugs, Opioid antagonists (naltrexone or nalmefene) and drugs that modulate gamma-aminobutyric acid receptors (baclofen or acamprosate) appear to have a short-term benefit by reducing the craving and withdrawal symptoms.

Supportive treatment— �Patients with severe AH could require admission to an intensive care unit. The airway should be protected in patients with acute alcoholic intoxication or an advanced degree of hepatic encephalopathy. �The use of benzodiazepines is contraindicated in these patients. �In Wernicke encephalopathy among alcoholic and malnourished patients, the administration of B-complex vitamins is often required. �A daily protein intake of 1. 5 g/kg body wt has been proposed. �Patients with AH are predisposed to develop severe infections, so early diagnosis and empiric antibiotic treatment are advised.

Specific treatment �Corticosteroids (eg, PREDNISOLONE 40 mg/day po for 4 wk, followed by tapered doses) improve outcome in patients who have severe acute alcoholic hepatitis and who do not have infection, GI bleeding, renal failure, or pancreatitis.

�Pentoxifylline— Pentoxifylline is a phosphodiesterase inhibitor that blocks transcription of TNF-α to decrease serum levels of the gene product. �Pentoxifylline can be used to treat patients with severe AH who cannot be given corticosteroids.

�Anti-TNF-α agents— TNF-α has an important role in the pathogenesis of ALD in animal models, so there have been several clinical studies of the effects of infliximab or etanercept (reagents that block this cytokine) in patients with AH. �Early-stage studies showed positive results in terms of survival and safety

Nutrition therapy �The presence of significant protein calorie malnutrition is a common finding in alcoholics, as are deficiencies in a number of vitamins and trace minerals, including vitamin A, vitamin D, thiamine, folate, pyridoxine, and zinc. �which can promote bacterial infections. Nutritional support is recommended in patients with AH; �it improves liver function and results from histologic analyses and might increase survival times

�Antioxidants phosphatidylcholine, (eg, S -adenosyl-L-methionine, metadoxine) show promise in ameliorating liver injury during early cirrhosis but require further study �Liver transplantation—Liver transplantation has been used to treat patients with decompensated ALD. Outcomes are equal to or better than those obtained when it is used to treat end-stage liver disease from other causes. �Most programs require 6 months of abstinence before transplantation is done; recent data suggest that earlier transplantation may offer a survival advantage.