Alcohol Screening and Brief Intervention SBI City Mat

Alcohol Screening and Brief Intervention (SBI) City. Mat. CH Urban Practice Collaborative on the Prevention of Pregnancies Exposed to Alcohol and other Substances John C. Higgins-Biddle, Ph. D. October 17, 2011 1

Main Topics Part I • What is the alcohol problem? (Not just for women) • What is alcohol Screening? • What is Brief Intervention? Part II • Implementing SBI Discussion of My Mistakes and Common Objections 2

The Preventive Paradox • Who’s a good driver? – 16 -year-old males? You? • Who has more heart attacks? – With diagnosis? Without? Who should be screened for hypertension & cholesterol? • Large groups with small problems vs. small groups with big problems • How does this apply to alcohol use? 3
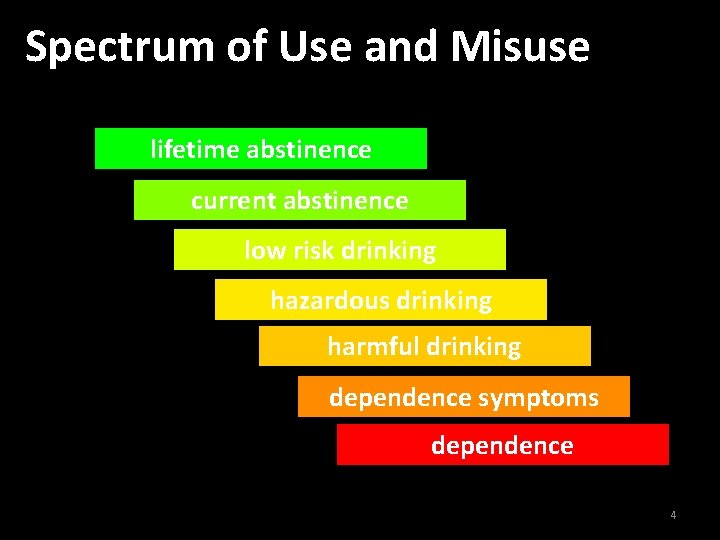
Spectrum of Use and Misuse lifetime abstinence current abstinence low risk drinking hazardous drinking harmful drinking dependence symptoms dependence 4
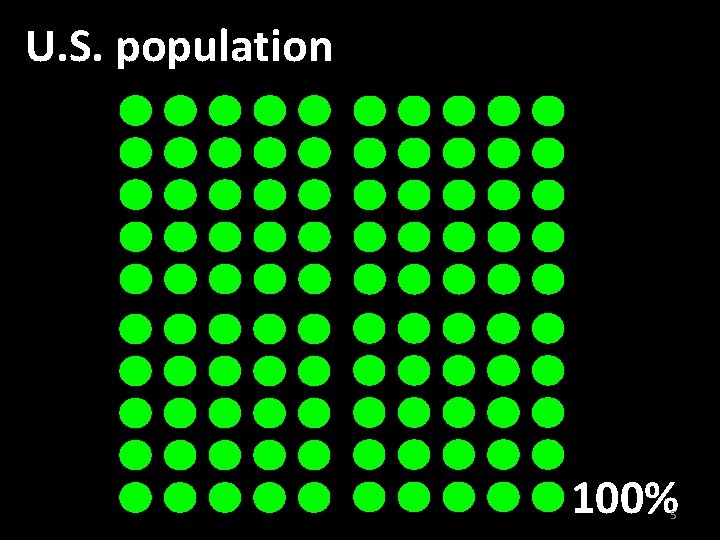
U. S. population 100% 5
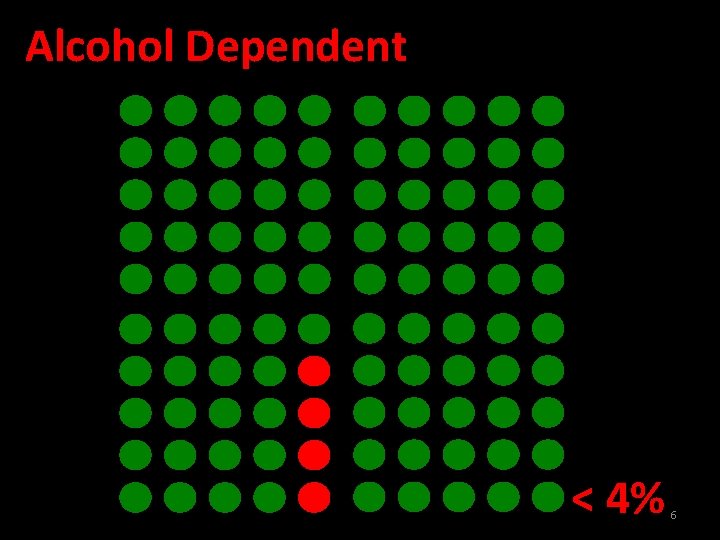
Alcohol Dependent < 4% 6
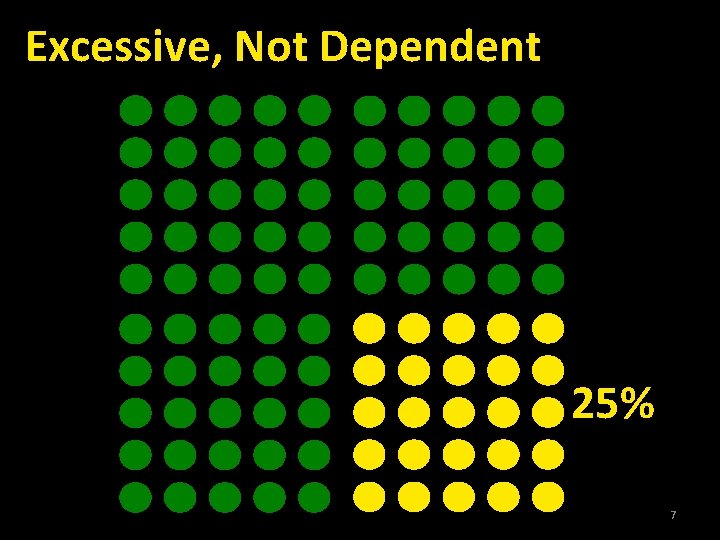
Excessive, Not Dependent 25% 7
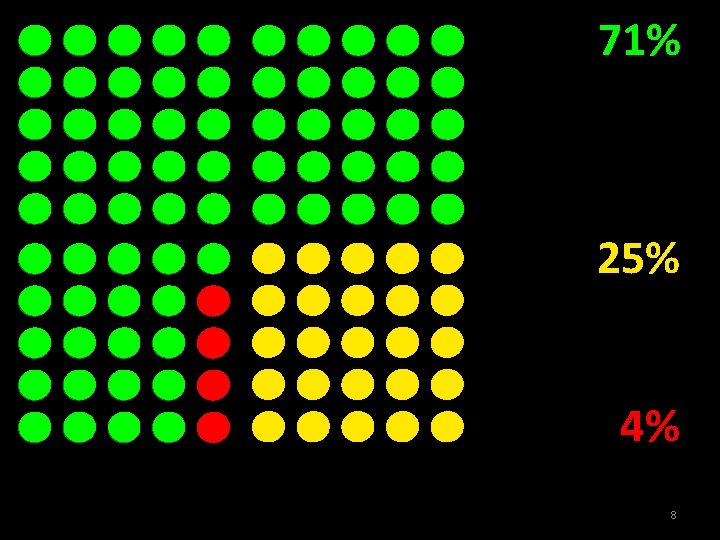
71% 25% 4% 8
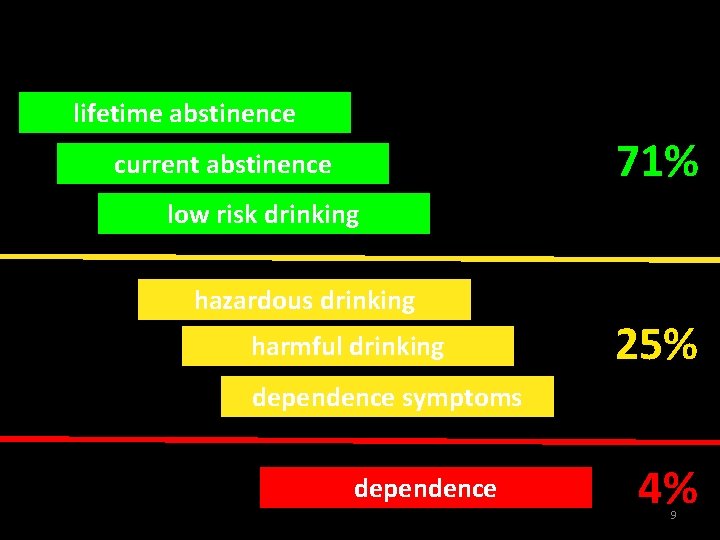
lifetime abstinence 71% current abstinence low risk drinking hazardous drinking harmful drinking 25% dependence symptoms dependence 4% 9

What’s the Problem? excessive drinking 10

Institute of Medicine (1990): “If the alcohol problems experienced by the population are to be reduced significantly, the distribution of these problems in the population suggests that a principal focus of intervention should be on persons with mild or moderate alcohol problems. ” 11

What is alcohol SBI? • Screening can identify degree of risk and likelihood of a condition (dependence) • Brief Intervention can help some patients reduce hazardous and harmful drinking and refer more severe patients to specialized alcohol services—mainly the dependent • A public health oriented clinical preventive service to improve aggregate health 12
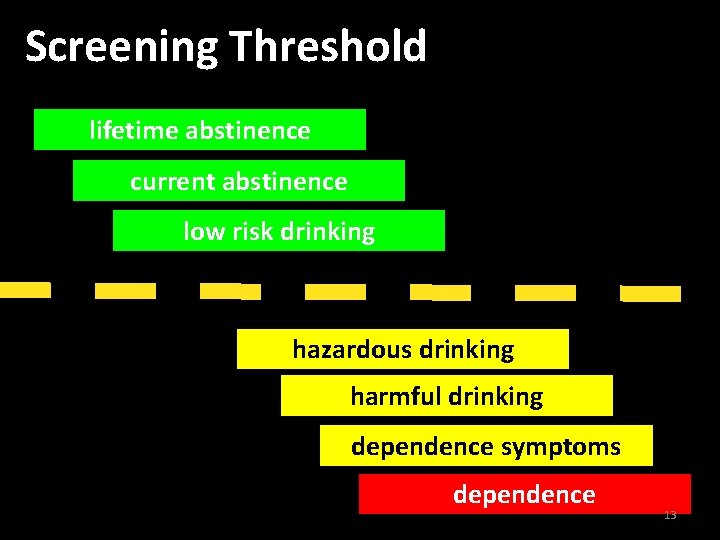
Screening Threshold lifetime abstinence current abstinence low risk drinking hazardous drinking harmful drinking dependence symptoms dependence 13

Note: Terminology • Previous slides used the WHO vocabulary • In 1990 USA had only “abuse”; diagnostic term • In 1993 I stole “misuse” from England; USPSTF used it in 2004 recommendation • In 1996 we invented “risky drinking” and “atrisk” use • Some today prefer “unhealthy” use • We only think in language; it’s important 14

Screening for Alcohol Use • So how can we identify misuse? • 25 years of research into screening • Self-report screening is quick, accurate, and inexpensive • Written, oral, computer options • Good screening tools distinguish risk levels • High level of patient acceptance 15
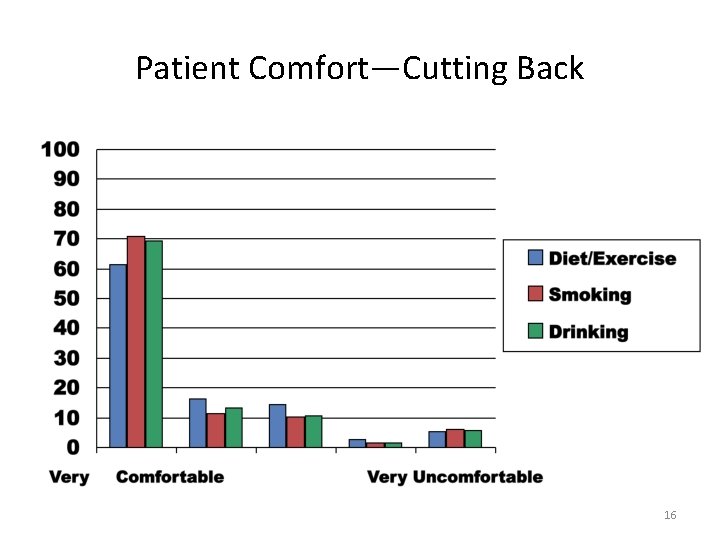
Patient Comfort—Cutting Back 16
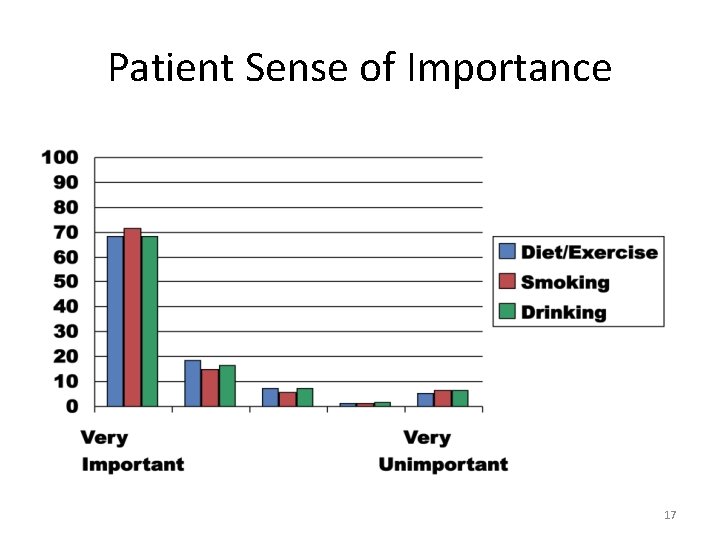
Patient Sense of Importance 17

Screening Essentials • It’s science! Validation research matters • Central issue is measurement of drinking • If patient drinks too much, knowing patient perception of problem aids intervention • Finally, signs of dependence aid referral • If a patient doesn’t drink too much, support good behavior and be open to talk; no more is needed 18

What’s Too Much? Healthy Men ≤ 65 Healthy Women (any age) & Healthy Men >65 • No more than 4 drinks/day AND • No more than 14 drinks/week • No more than 3 drinks/day AND • No more than 7 drinks/week 19

Exceptions • With medical conditions affected by alcohol— e. g. , hypertension, diabetes, many others • On medication that interacts with alcohol • Pregnant or likely to become pregnant (no known safe limit, so no drinking) • While, or about to be, working, driving, operating machinery, or any actions requiring normal motor functions and thinking 20

Recommended Instruments • Not instruments that ask only about dependence symptoms (e. g. , CAGE, TWEAK or TACE) • Two-stage system most efficient: – 1 st screen for everyone to measure drinking – 2 nd screen for positives to ID problems and dependence signs • 1 st Screen Options – Single-question screen – AUDIT-C 3 consumption questions • 2 nd Screen: AUDIT 10 Questions 21

Issues in Screening • Everyone needs to receive 1 st screen; Clinicians cannot tell who drinks too much any other way • Single-question can be oral • AUDIT-C & AUDIT are better when patient reads and chooses responses • Screening requires changing systems— reception, vital signs, or both (more later) 22

Brief Intervention • Study designs have varied widely, and “active ingredient” is unknown • Structured conversation, low intensity, short duration, non-judgmental, motivational • Meets patient where s/he is; moves patient to decide and act • Clear medical advice, but with encouragement 23

Typical Elements • Feedback of screening results—level of drinking, confirmation, cf. to guidelines • Professional advice—risks, relation to medical conditions/problems, need to reduce risks • Patient response—questions, willingness to take action, establishing a goal (reduce/stop) • Information—drinking limits, how-to tips • Encouragement—follow-up visits do help 24
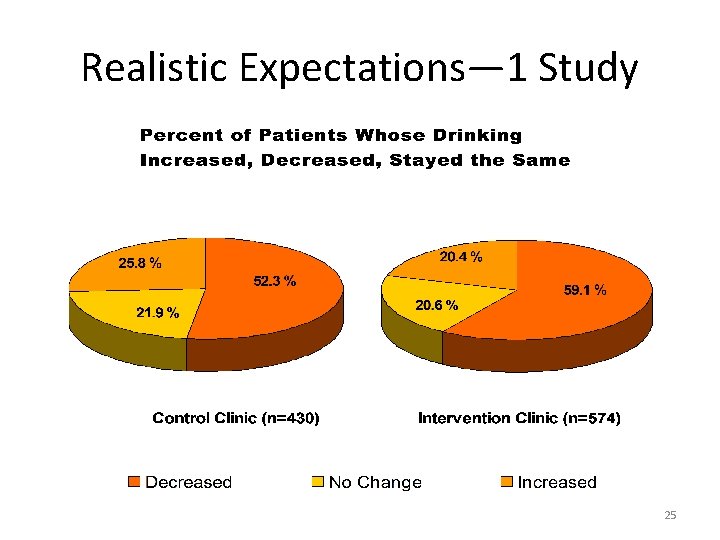
Realistic Expectations— 1 Study 25

Cases of Dependence Patients with dependence will be identified Don’t be afraid; they already know about it BI aim: patient accepts specialized services Need system of referral: list, knowledge, relationships, info-sharing, follow-up • Service variety, includes counseling, mutual help • Most will refuse, some will respond, now or later -- don’t worry, you’ve done some good • • 26

What SBI may, may not, accomplish • • Don’t sell what you can’t deliver Everyone will not be helped Most with dependence will not change now But many non-dependent will reduce drinking Health is likely to improve; costs are unknown Look for small population change over time Focus on measuring program performance 27

Evaluation Measures • • • # and % of patients screened # and % of those screening positive Ratio of at-risk drinking to likely dependence # and % of positives who get interventions # and % of dependents referred to treatment Satisfaction of people, providers, organizations Communicate results to everyone constantly! 28

Discussion • • What’s not clear? What do you need to know more about? What’s surprising? What seems strange? What’s upsetting? What’s not applicable? What time is the break? 29

Part II: Issues in Implementation • You’ve listened enough; time for you to talk • You already know a lot about implementing • I’ll offer two sets of conversation starters – My 5 biggest mistakes in implementing SBI – 5 common objections to doing SBI • You can practice now analyzing my mistakes and answering the objections you will encounter 30

My Biggest Mistake #1 Talking to anyone about SBI without first explaining what the problem is that it addresses 31

My Biggest Mistake # 2 Thinking that the people involved in providing health services are the only ones who decide what they do 32

My Biggest Mistake # 3 Training people without first establishing an organizational policy decision, communicated to everyone involved, to implement a new program 33

My Biggest Mistake # 4 Designing a program and delivering it to staff to implement, without having them participate in the program design 34

My Biggest Mistake # 5 Underestimating the need and complexity of changing the systems by which medical practices operate 35

Objections you will encounter # 1 There is no time to do more 36

Objections you will encounter # 2 Alcohol use is not a medical issue 37

Objections you will encounter # 3 We can’t deal with the alcoholics we already have, and we don’t want to find more 38

Objections you will encounter # 4 People won’t tell the truth People don’t change 39

Objections you will encounter # 5 Our clinic is unique; it won’t work here 40

41
- Slides: 41