Alcohol Brief Interventions Alcohol Drugs and Hepatitis C

Alcohol Brief Interventions Alcohol, Drugs and Hepatitis C, Brewing Up a Storm, 24. 6. 15 Dr. Niamh Fitzgerald Lecturer in Alcohol Studies, Institute for Social Marketing, School of Health Sciences, University of Stirling

What is an alcohol brief intervention? “Brief interventions are those practices that aim to identify a real or potential alcohol problem and motivate an individual to do something about it. ” (Babor & Higgins. Biddle 2001). Brief interventions are heterogeneous and vary in ways including length, content, delivery, deliverer and target group (Heather, 1995). With this caveat, good evidence for efficacy in primary care, as well as for cost effectiveness (or even savings). Babor TF, Higgins-Biddle JC. Brief Intervention for Hazardous and Harmful Drinking. A Manual for Use in Primary Care. Geneva: World Health Organisation; 2001. Heather N. Interpreting the evidence on brief interventions for excessive drinkers: the need for caution. Alcohol. 1995 May 1; 30(3): 287– 96. 2

Acronym-tastic ABI Alcohol Brief Intervention BI Brief intervention IBA Identification and Brief Advice BMI Brief Motivational Interviewing EBI Extended brief intervention BA Brief advice SBI Screening and brief intervention SBIRT Screening, Brief Intervention and Referral to Treatment BLC Brief lifestyle counselling EBA Extended brief advice HBCC Health Behaviour Change Counselling EIBI: Early Identification and Brief Intervention MET: Motivational Enhancement Therapy 3

What is Motivational Interviewing? Simply: A collaborative conversation style for strengthening a person’s own motivation and commitment to change. Specifically: A collaborative, goal-oriented style of communication with particular attention to the language of change…designed to strengthen personal motivation and commitment to a specific goal by eliciting and exploring the person’s own reasons for change within and atmosphere of acceptance and compassion. NB: BIs ≠ Motivational Interviewing: some forms of ABI are influenced by MI and share some principles.

Scottish national ABI programme = just one model of ABI Brief Intervention (Scotland? ) Somewhat flexible structure Guiding style Variable length Typically longer training > Informed by ‘stages of change’ and MI > 400, 000 ABIs implemented in 6 years but fidelity to model in real-life unknown. Brief Advice (England/SIPS) Largely pre-determined structure More directive Shorter (5 m? ) Typically minimal training < Focus on ‘stages of change’/MI Easier to implement widely? 5
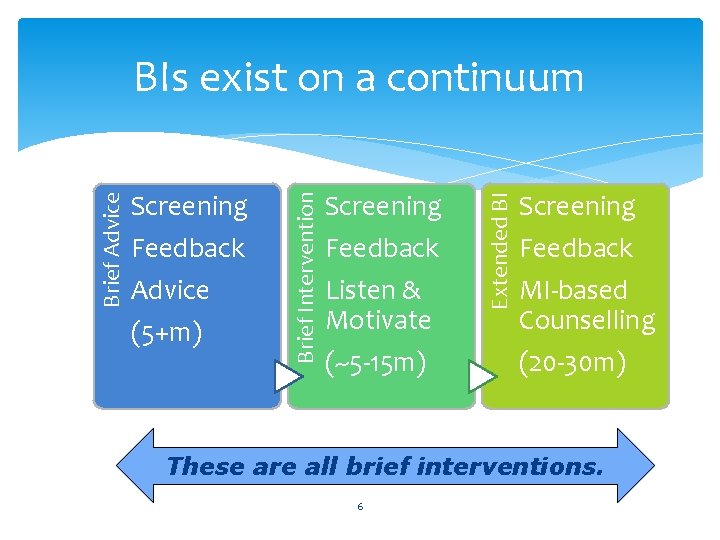
Feedback Advice (5+m) Screening Feedback Listen & Motivate (~5 -15 m) Extended BI Screening Brief Intervention Brief Advice BIs exist on a continuum Screening Feedback MI-based Counselling (20 -30 m) These are all brief interventions. 6

What about Screening? Use of a single question or set of questions to determine likelihood of various alcohol problems – usually hazardous drinking or dependence. Can be universal (everyone is asked), targeted (certain groups are always asked), or opportunistic (individuals are asked as and when relevant) Self-report screening has historically been considered superior to blood tests in terms of sensitivity and specificity 7
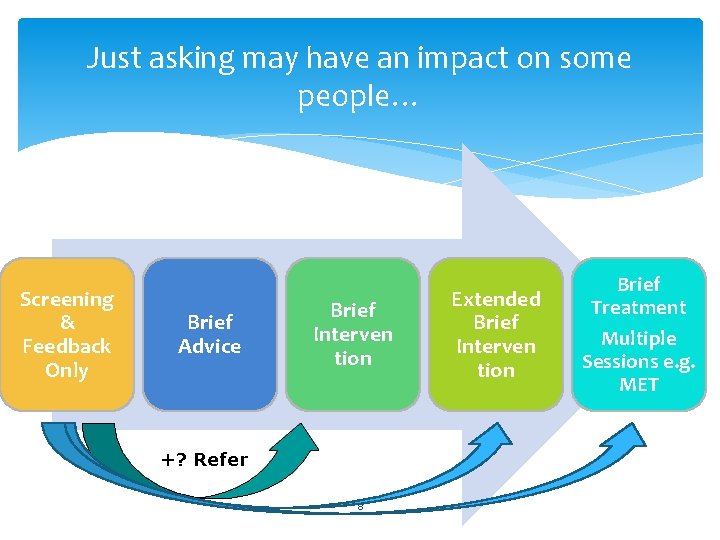
Just asking may have an impact on some people… Screening & Feedback Only Brief Advice Brief Interven tion +? Refer 8 Extended Brief Interven tion Brief Treatment Multiple Sessions e. g. MET

e. BI, e. SBI – online interventions Internet, text, mobile phone apps – social media in future? Most published work is on internet. Single session SBI - fully automated, no personal contact - often built on normative feedback, cheap, direct, small effect. (White et al. , 2010) More extended on-line interventions - A number of modules e. g. over 6 weeks 9 Thank you to Preben Bendsen Linkoping University for this data.

We don’t know… What content of BI works? How different elements of content work? With different people? With different levels of problem? Delivered by different practitioners? In different settings? In different combinations? . . . SIPS? What training, skills and style are needed? How long they need to be applied? “BI content matters and we should study it” (Mc. Cambridge, 2013, Drug and Alcohol Review, 32(4)) 10

Considering ABI delivery in a New Setting 1. 2. Is there a need for ABI delivery in this service? How are practitioners currently addressing alcohol use – how when, where do ABIs fit in? 3. Will ABIs be perceived as legitimate by practitioners and acceptable to service-users? 4. Will practitioners have the ability to deliver ABIs? 5. What support will be needed? 6. Will ABIs work/do harm in this setting? 7. What will establish routine implementation of ABIs in this setting? 11

1. Is there a need for ABI delivery in this setting? Not always obvious Subject to prejudice “Nobody on our whole team has delivered it – the consensus of the team as a whole is that its not particularly applicable to our clients. ” CMHT Requires evidence that there alcohol-related problems in the service user population. 12

2. How are practitioners currently addressing alcohol use – how when, where do ABIs fit in? What, exactly, needs to change about current practice? When, how, with whom… What is feasible? “Its not one size fits all, you need to build on what’s already there” May simply measure current practice. Is the initiative actually about improving the quality of conversations about alcohol that already happen? Or is it about frequency of conversations? 13

WHO Practice Recommendation “An alcohol intake assessment is recommended for all persons with HCV infection followed by the offer of a behaviour alcohol reduction intervention for persons with moderate to high alcohol intake. ” Refers the reader to other guidance for more detail – which is written for primary care-based ABI The type of intervention may need to be different The cut-offs for intervention/other points on care pathway may be different The information and support needed by practitioners is specific to HCV. 14

3. Will ABIs be perceived as legitimate by practitioners and acceptable to service users? Personally legitimate: Fears about hypocrisy Will service users expect/welcome ABI delivery? Consider alcohol culture & policy in the workplace? Professionally legitimate: Does it fit with the ‘raison d’etre’ of the service? Does the service have a health remit? (the main remit? ) 15

4. Will practitioners be able to deliver ABIs? How difficult is it to deliver ABIs? How can it be learned? Does this vary across settings? We know very little about what training works… Training can address ability, as well as attitudes and confidence; can give messages about importance; but it is rarely enough to secure change. 16
5. What support will be needed? “The Can of Worms” Support close at hand Clear care pathways Referral mechanisms Service co-operation Resources to fund the time needed? (or will practitioners have to stop doing something else? ) 17

6. Will ABIs work/do harm in this setting? Cannot assume transfer of efficacy from health settings …it seems unlikely that any fixed ABI content/design works equally well for any person, in any setting… Very little evidence in most non-health settings and many health settings too. Does it matter? Can be a barrier to implementation (though not always) 18

ABIs in Treatment/Hep C Systematic Review (Doyle et al. for WHO, searched to May 2013) Could lead to abstinence or reduce drinking days/month Practitioners should be encouraged and trained. Dieperink, 2014: RCT of a type of MET versus lifestyle education (not inclg alcohol) in patients with chronic Hep C. Significant reduction in days abstinent but not consumption. Cochrane review (Klimas et al. 2014) of psychosocial interventions for alcohol in illicit drug users found some impact but overall was inconclusive. Systematic review (E. F. S. Kaner, Brown, & Jackson, 2011): patients with co-morbid substance use and severe & enduring mental health problems: unconvincing evidence. 19

Will it do harm? Is this the most important use of time and resources? Harm by diversion – opportunity costs? Other possible mechanisms of harm: Focus on ‘pros and cons’ can reinforce reasons for drinking Advice alone may entrench the position of someone not yet ready for change. Ill-timed/ill-thought through interventions could damage relationships with service users/close an intervention window Important to evaluate this. 20

7. What will establish routine implementation of ABIs in this setting? Top-down pressure/monitoring/targets/senior management priority Embedding bespoke intervention into existing systems: learning from implementation science Targets work but need to be used selectively: Intervention is the or close to the top priority for the service? Intervention is likely to, and then shown to, work? 21

Conclusions ABIs are needed but we don’t know what works. Diversity in current service provision is likely Ensure it is informed by latest evidence e. g. MI & ABI ingredients Need to document and evaluate (including unintendeds) Opportunity to establish which model of intervention is best - call strongly for pragmatic robust research Particularly important if burden of disease is driven by alcohol, not just HCV. 22

Thank You Sharon Hutchinson and Anastasia Karachalia Sandri, Glasgow Caledonian University for pointing me towards relevant literature. www. inebria. net INEBRIA (also google discussion group) niamh. fitzgerald@stir. ac. uk ; Twitter: @niamhcreate UK Centre for Tobacco and Alcohol Studies www. ukctas. net Twitter: @UKCTAS 23
- Slides: 23