ALARM FATIGUE Jasmine Poon Meghan Simarro Laura Stanton













- Slides: 16

ALARM FATIGUE Jasmine Poon, Meghan Simarro, Laura Stanton, & Richard Tran

Admission ● 54 -year-old man with hypertension, diabetes, and end-stage renal disease admitted to the hospital with chest pain. ● ECG no evidence of ischemia, but elevated troponin T. ● Admitted and placed on telemetry monitoring and treated as NSTEMI. ● Patient’s alarms constantly sounded for “low voltage” and “asystole” ● Nurse checked on patient, who was alert and oriented no acute signs of distress. ● Doctor was paged and was unconcerned with patient’s condition without corresponding clinical presentation of problem. ● Nurse and resident decided to silence all of telemetry alarms.

The Next Morning ● The nurse did not check on the patient for 4 hours. ● When bedside nurse went to perform the patient’s morning vitals, he was found unresponsive, cold, and with no pulse. ● Code blue was called, but the patient was already dead for some time. ● Cause of death unclear, but likely fatal arrhythmia related to NSTEMI

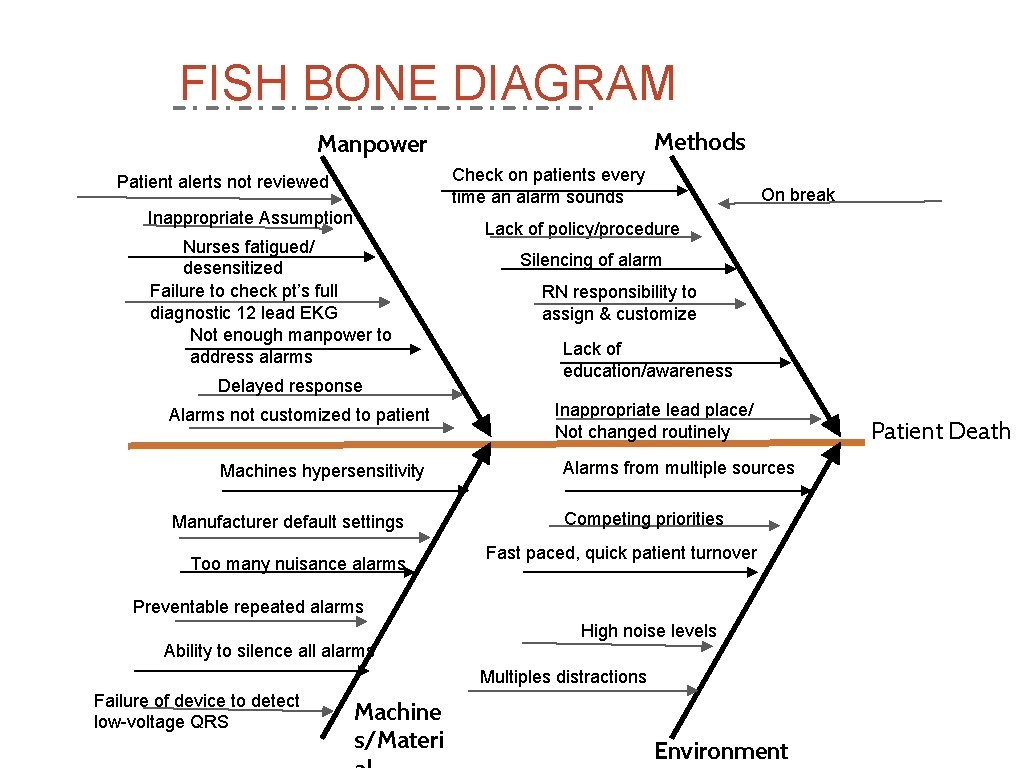
FISH BONE DIAGRAM Methods Manpower Check on patients every time an alarm sounds Patient alerts not reviewed Inappropriate Assumption Nurses fatigued/ desensitized Failure to check pt’s full diagnostic 12 lead EKG Not enough manpower to address alarms Delayed response Alarms not customized to patient Machines hypersensitivity Manufacturer default settings Too many nuisance alarms On break Lack of policy/procedure Silencing of alarm RN responsibility to assign & customize Lack of education/awareness Inappropriate lead place/ Not changed routinely Alarms from multiple sources Competing priorities Fast paced, quick patient turnover Preventable repeated alarms High noise levels Ability to silence all alarms Multiples distractions Failure of device to detect low-voltage QRS Machine s/Materi Environment Patient Death

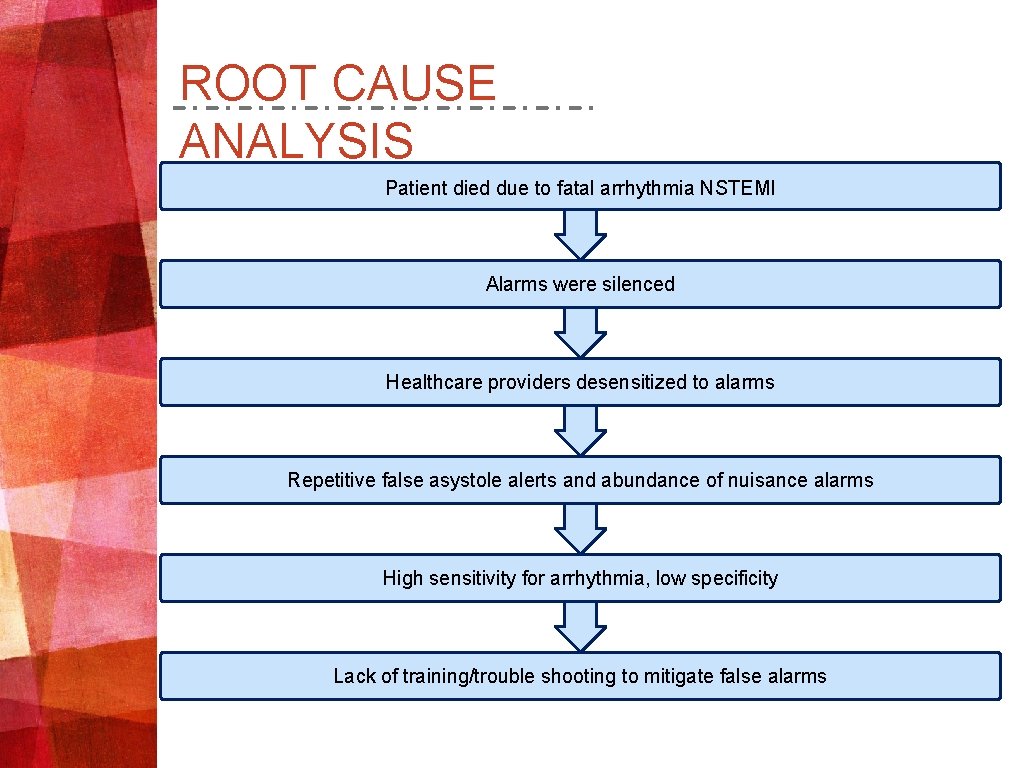
ROOT CAUSE ANALYSIS Patient died due to fatal arrhythmia NSTEMI Alarms were silenced Healthcare providers desensitized to alarms Repetitive false asystole alerts and abundance of nuisance alarms High sensitivity for arrhythmia, low specificity Lack of training/trouble shooting to mitigate false alarms

PDSA: AIM What are we trying to accomplish? ● The purpose of this PDSA is to decrease the number of patient deaths related to nuisance alarms and alarm fatigue to zero deaths on the observation unit within three months of implementing new protocol. ● Protocol: To require nurses to think critically when false alarms are sounding and troubleshoot complications to identify and solve possible causes. If troubleshooting is unsuccessful, know appropriate personnel to contact to ensure patient safety.

PDSA: PLAN Tasks Person Responsible When Where Create a central monitoring station for tele patients Unit Secretary Within 1 weeks of implementation Central Nursing Station Staff Central Monitoring System Telemonitoring Tech Upon creation of central monitoring station Tele central monitoring system Educate nurses on new telemonitoring protocol Charge RN Within 2 weeks of implementation Staff Meeting Room Nurses will tailor telemonitoring to patient Patient’s RN Upon admission or transfer to the unit Patient’s Room

PDSA: PLAN Prediction Measures to determine if prediction succeeds The nurse will follow up on all tele-tech The tele-tech will be able to identify 100% of alerts by charting patient assessment. Nurse irregular rhythms alert the nurse if there are manager will check charting to verify proper any concerning waveforms. documentation daily. Nurse manager will educate 90% of staff on new protocol within 2 weeks of implementation. Each nurse will need to sign off that they have received individual training and demonstrate understanding. All patients will have telemonitors tailored to Nurses will chart daily that they have verified individual parameters by their individual RN monitor settings upon initial assessment. The nurse will contact appropriate personnel Charge nurse will have nurses initial stating when unable to troubleshoot tele they received notification on contact complications within one month. protocols in event of tele complications.

PDSA: DO ● It will take one month for new telemonitoring protocol will be implemented into normal practice. ● Nurses will be educated on new protocols so alarms are never completely silenced. Rather, clinical staff should problem-solve why an alarm condition is occurring and work to resolve it. ● Managers will continue to monitor the effectiveness of the new protocol.

PDSA: STUDY Prediction Outcome The tele-tech will be able to identify 100% of Tele-techs were only about to identify 80% irregular rhythms alert the nurse if there are percent of rhythm. any concerning waveforms. Nurse manager will educate 90% of staff on new protocol within 2 weeks of Approximately 80% of staff was introduced implementation. to the new protocol within 2 weeks. All patients will have telemonitors tailored to individual parameters by their individual RN daily. 100% of patients had monitors tailored to individual parameters daily. The nurse will contact appropriate personnel 100% of nurses will receive notification on when unable to troubleshoot tele contact protocols in event of tele complications within one month. complications.

PDSA: STUDY Problem Solution 20% of nurses were on vacation or floated Charge nurse will train the nurse when they to other units during training and therefore return to the floor to ensure proper were not properly educated on new protocol. education on new protocol. Integrate parameters (HR/BP) with heart Tele-tech was not able to analyze all rhythm to determine if alarms are accurate available ECG leads, but rather only a select or false with simultaneous physiologic few which could lead to false alarms. impact. Summary of findings: Following the implementation of the protocol, zero patients died as a result of nuisance alarms and alarm fatigue. The implementation of a central monitoring station and tele-techs allowed for improved patient monitoring and appropriate response.

ACT What will you recommend as a result of your test of change? It is recommended that all units have a central monitoring station with 1 tele-tech per 10 patients in order to decrease the number of nuisance alarms. Nurses utilize critical thinking skills to problem-solve why an alarm condition is occurring and work efficiently to resolve it. Additionally it is recommended that all telemonitoring be tailored to the needs of the patient by each nurse. The new protocol will be implemented and used by current and future staff members.

STAKEHOLDER ANALYSIS ● Internal (unit) stakeholders -Nurses -Charge Nurse -Tele-Techs -Doctors -Management -Unit Clerks ● External stakeholders -Patients -Families -Community

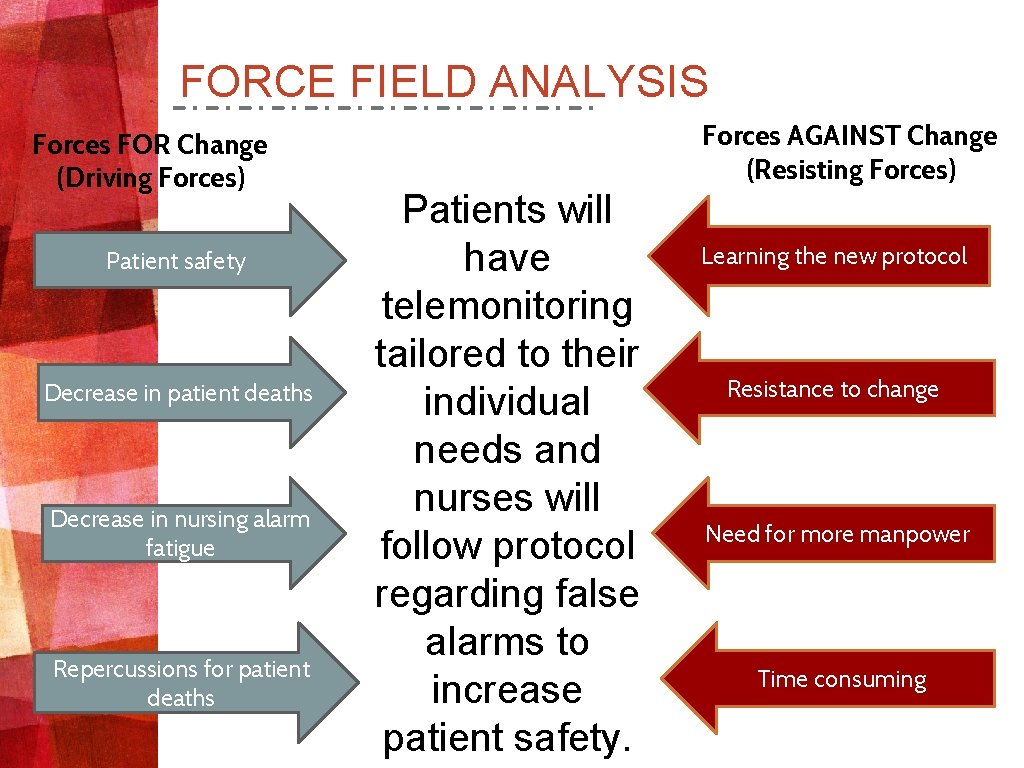
FORCE FIELD ANALYSIS Forces FOR Change (Driving Forces) Patient safety Decrease in patient deaths Decrease in nursing alarm fatigue Repercussions for patient deaths Forces AGAINST Change (Resisting Forces) Patients will have telemonitoring tailored to their individual needs and nurses will follow protocol regarding false alarms to increase patient safety. Learning the new protocol Resistance to change Need for more manpower Time consuming

TEAMWORK!

REFERENCES Institute for Healthcare Improvement. (2016). Plan-do-study-act (PDSA) worksheet. Retrieved from http: //www. ihi. org/resources/pages/tools/plandostudyactworkshe et. aspx Pelter, M. , & Drew, B. (2015, December). Harm From Alarm Fatigue. Retrieved October 30, 2016, from https: //psnet. ahrq. gov/webmm/case/362/harm-from-alarmfatigue U. S. Department of Veterans Affairs. (2015). Root cause analysis tools, VA national center for patient safety. Retrieved from http: //www. patientsafety. va. gov/professionals/onthejob/rca. asp