AKI Organ Dysfunction CRRT Highlights Hyderabad India October
AKI & Organ Dysfunction CRRT Highlights Hyderabad, India October 1, 2016 Kianoush B. Kashani, MD, FASN, FCCP © 2013 MFMER | 3322132 -1

Disclosure • I have no financial conflict with this activity © 2013 MFMER | 3322132 -2

Outlines • Heart: • ADHF and biomarkers • CSA-AKI • Systematic analysis of interventional trials • GDRRT • Liver: • MELD-Na • MELD ♀ vs. ♂ © 2013 MFMER | 3322132 -3

HEART © 2016 MFMER | 3572290 -4
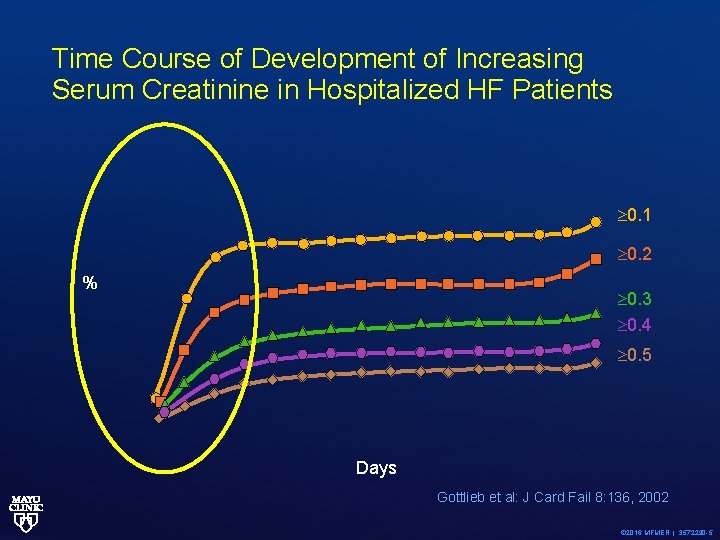
Time Course of Development of Increasing Serum Creatinine in Hospitalized HF Patients 0. 1 0. 2 % 0. 3 0. 4 0. 5 Days Gottlieb et al: J Card Fail 8: 136, 2002 © 2016 MFMER | 3572290 -5
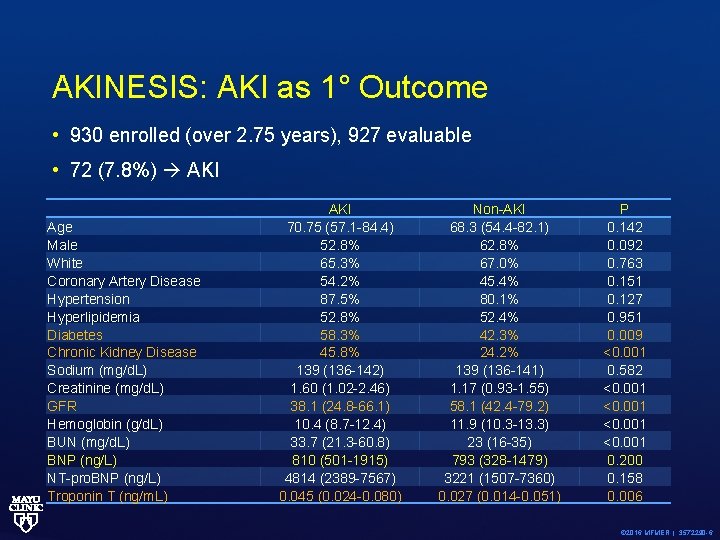
AKINESIS: AKI as 1° Outcome • 930 enrolled (over 2. 75 years), 927 evaluable • 72 (7. 8%) AKI Age Male White Coronary Artery Disease Hypertension Hyperlipidemia Diabetes Chronic Kidney Disease Sodium (mg/d. L) Creatinine (mg/d. L) GFR Hemoglobin (g/d. L) BUN (mg/d. L) BNP (ng/L) NT-pro. BNP (ng/L) Troponin T (ng/m. L) AKI 70. 75 (57. 1 -84. 4) 52. 8% 65. 3% 54. 2% 87. 5% 52. 8% 58. 3% 45. 8% 139 (136 -142) 1. 60 (1. 02 -2. 46) 38. 1 (24. 8 -66. 1) 10. 4 (8. 7 -12. 4) 33. 7 (21. 3 -60. 8) 810 (501 -1915) 4814 (2389 -7567) 0. 045 (0. 024 -0. 080) Non-AKI 68. 3 (54. 4 -82. 1) 62. 8% 67. 0% 45. 4% 80. 1% 52. 4% 42. 3% 24. 2% 139 (136 -141) 1. 17 (0. 93 -1. 55) 58. 1 (42. 4 -79. 2) 11. 9 (10. 3 -13. 3) 23 (16 -35) 793 (328 -1479) 3221 (1507 -7360) 0. 027 (0. 014 -0. 051) P 0. 142 0. 092 0. 763 0. 151 0. 127 0. 951 0. 009 <0. 001 0. 582 <0. 001 0. 200 0. 158 0. 006 © 2016 MFMER | 3572290 -6
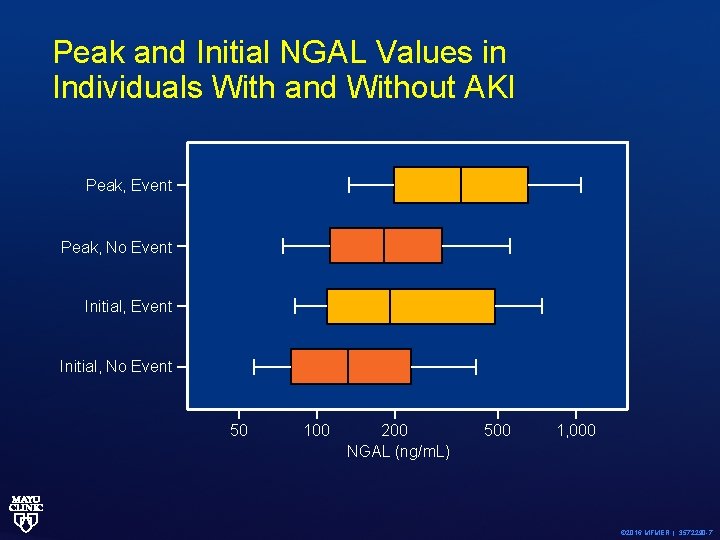
Peak and Initial NGAL Values in Individuals With and Without AKI Peak, Event Peak, No Event Initial, No Event 50 100 200 NGAL (ng/m. L) 500 1, 000 © 2016 MFMER | 3572290 -7
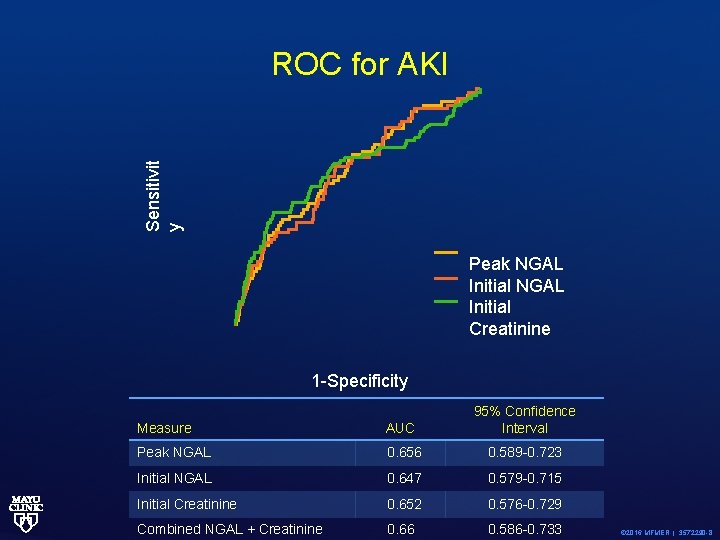
Sensitivit y ROC for AKI Peak NGAL Initial Creatinine 1 -Specificity AUC 95% Confidence Interval Peak NGAL 0. 656 0. 589 -0. 723 Initial NGAL 0. 647 0. 579 -0. 715 Initial Creatinine 0. 652 0. 576 -0. 729 0. 66 0. 586 -0. 733 Measure Combined NGAL + Creatinine © 2016 MFMER | 3572290 -8
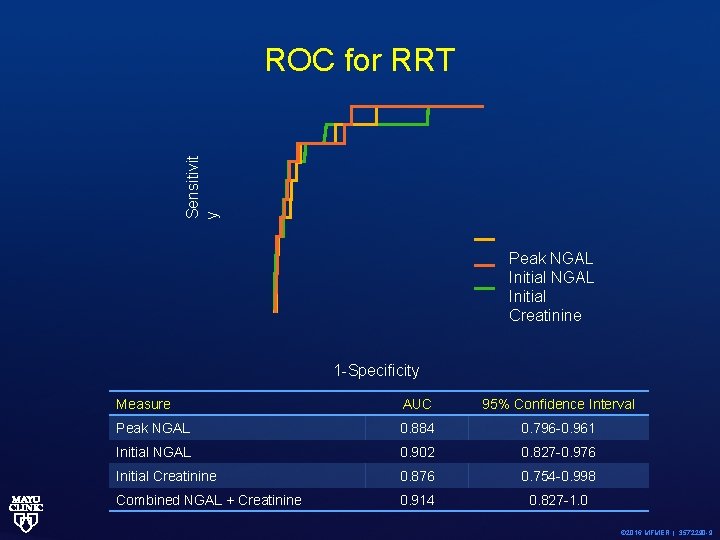
Sensitivit y ROC for RRT Peak NGAL Initial Creatinine 1 -Specificity Measure AUC 95% Confidence Interval Peak NGAL 0. 884 0. 796 -0. 961 Initial NGAL 0. 902 0. 827 -0. 976 Initial Creatinine 0. 876 0. 754 -0. 998 Combined NGAL + Creatinine 0. 914 0. 827 -1. 0 © 2016 MFMER | 3572290 -9
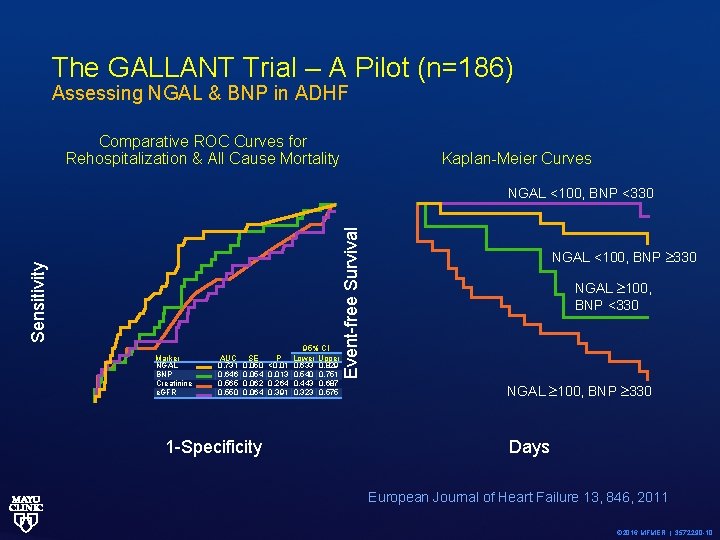
The GALLANT Trial – A Pilot (n=186) Assessing NGAL & BNP in ADHF Comparative ROC Curves for Rehospitalization & All Cause Mortality Kaplan-Meier Curves Marker NGAL BNP Creatinine e. GFR AUC 0. 731 0. 646 0. 565 0. 550 SE 0. 050 0. 054 0. 062 0. 064 1 -Specificity P <0. 013 0. 264 0. 391 95% CI Lower Upper 0. 633 0. 829 0. 540 0. 751 0. 443 0. 687 0. 323 0. 575 Event-free Survival Sensitivity NGAL <100, BNP <330 NGAL <100, BNP 330 NGAL 100, BNP <330 NGAL 100, BNP 330 Days European Journal of Heart Failure 13, 846, 2011 © 2016 MFMER | 3572290 -10

CSA-AKI © 2016 MFMER | 3572290 -11
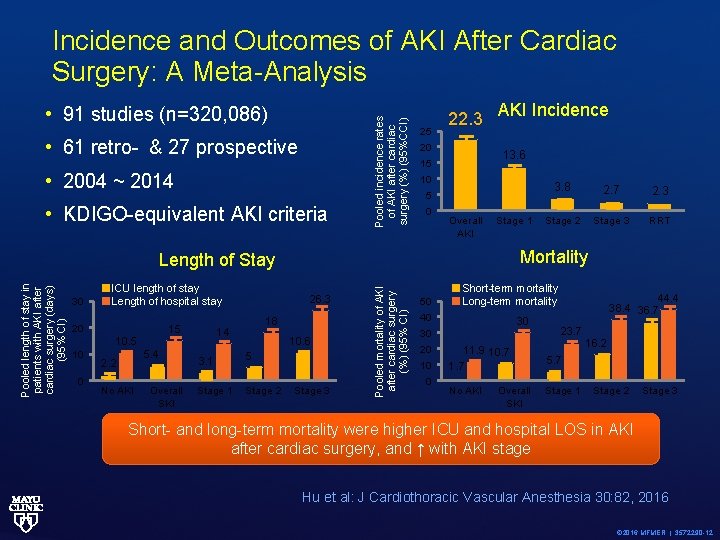
• 91 studies (n=320, 086) • 61 retro- & 27 prospective • 2004 ~ 2014 • KDIGO-equivalent AKI criteria Pooled incidence rates of AKI after cardiac surgery (%) (95%CCI) Incidence and Outcomes of AKI After Cardiac Surgery: A Meta-Analysis 25 22. 3 20 AKI Incidence 13. 6 15 10 5 0 Overall AKI Stage 1 20 15 10 0 5. 4 2. 2 No AKI Overall SKI 26. 3 18 14 10. 6 3. 1 5 Stage 1 Stage 2 Stage 3 Pooled mortality of AKI after cardiac surgery (%) (95% CI) Pooled length of stay in patients with AKI after cardiac surgery (days) (95% CI) 30 2. 7 2. 3 Stage 2 Stage 3 RRT Mortality Length of Stay ICU length of stay Length of hospital stay 3. 8 50 Short-term mortality Long-term mortality 40 30 30 20 10 0 44. 4 38. 4 36. 7 23. 7 11. 9 10. 7 1. 7 5. 7 No AKI Stage 1 Overall SKI 16. 2 Stage 3 Short- and long-term mortality were higher ICU and hospital LOS in AKI after cardiac surgery, and ↑ with AKI stage Hu et al: J Cardiothoracic Vascular Anesthesia 30: 82, 2016 © 2016 MFMER | 3572290 -12
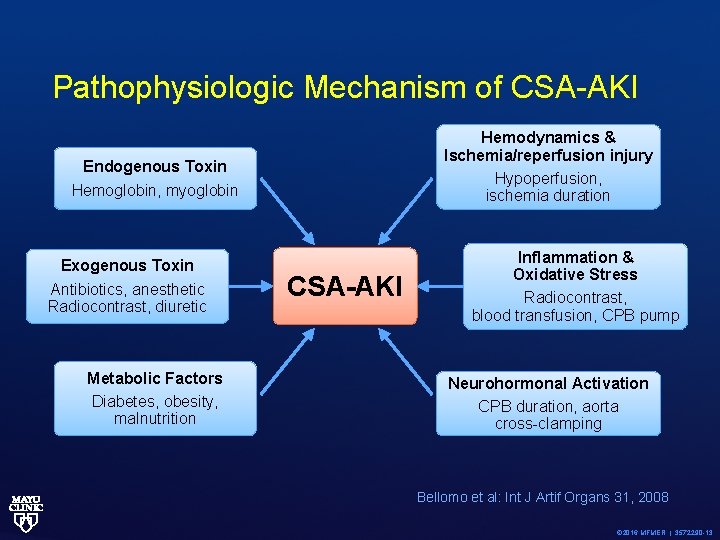
Pathophysiologic Mechanism of CSA-AKI Hemodynamics & Ischemia/reperfusion injury Hypoperfusion, ischemia duration Endogenous Toxin Hemoglobin, myoglobin Exogenous Toxin Antibiotics, anesthetic Radiocontrast, diuretic Metabolic Factors Diabetes, obesity, malnutrition CSA-AKI Inflammation & Oxidative Stress Radiocontrast, blood transfusion, CPB pump Neurohormonal Activation CPB duration, aorta cross-clamping Bellomo et al: Int J Artif Organs 31, 2008 © 2016 MFMER | 3572290 -13

Common Risk Factors of CSA-AKI Preoperative • ↓ Renal reserve • Reno-vascular dz. • Pre-renal azotemia • Recent diuresis Intraoperative • ↓ Renal perfusion • • Hypotension Lack of pulsatile flow Vasoactive agents Anesthetic effects • Impaired LV function • Embolic events • ACEI/ARB • Nephrotoxin • CPB-induced inflammation • Inflammation • Nephrotoxin • IABP • PVD • COPD • Free hemoglobin Postoperative • Systemic inflammation • Reduced LV function • Vasoactive agents • Hemodynamic instability • Nephrotoxin • Volume depletion or overload • Sepsis • Long CPB time • Mechanical ventilation CSA-AKI Rosner: CJASN, 2006 © 2016 MFMER | 3572290 -14

Perioperative Sodium Bicarbonate Therapy A Meta-Analysis • 5 randomized trials +1 prospective observational cohort study • 1673 patients Hospital death Sodium bicarbonate Control Study or Events Total Weight subgroup (%) Katja R. Turner 2014 9 63 10 58 54. 2 Matthias Heringlake 2012 4 280 4 304 22. 9 Michael Haase 2009 1 50 5. 9 Michael Haase 2013 11 171 3 176 17. 0 Total (95% CI) 567 588 100. 0 Total events 25 18 2 2 Heterogeneity: Chi =3. 83; df=3 (P=0. 28); I =22% Test for overall effect: Z=1. 05 (P=0. 29) Odds ratio M-H, fixed, 95% CI 0. 80 (0. 30, 2. 13) 1. 09 (0. 27, 4. 39) 1. 00 (0. 06, 16. 44) 3. 89 (1. 07, 14. 20) 1. 40 (0. 75, 2. 64) Michael Haase 2013 13 174 Shay P. Mc. Guinness 2013 8 215 Total (95% CI) 389 Total events 21 2 Heterogeneity: Chi =0. 91; df=1 (P=0. 34); I 2=0% Test for overall effect: Z=1. 78 (P=0. 08) 2. 76 (0. 96, 7. 91) 1. 33 (0. 45, 3. 89) 1. 96 (0. 93, 4. 12) Odds ratio (95% CI) Sodium bicarbonate infusion failed to reduce the AKI incidence or other outcomes in patients undergoing cardiac surgery, and might even prolong ICU stay. Mortality within 90 days 5 6 176 212 388 44. 2 55. 8 100. 0 11 0. 01 0. 1 1 10 100 Favors Bicarbonate Favors control Tian et al: J Cardiovasc Pharmacol 65(2): 130, 2015 © 2016 MFMER | 3572290 -15

Fenoldopam for RRT & In-Hospital Death in Cardiovascular Surgery A Meta-Analysis Mortality RRT • 13 randomized and case-matched studies • 1, 059 patients Study or subcategory Cicchetti Cogliati Halpenny II Caimmi Pittarello Sheinbaum Renzini Bove Ranucci Roasio Tumlin Martinelli Oliver Total (95% CI) Total events: 30 (Fenoldopam), 71 (control) Total for heterogeneity: Chi 2=5. 26; df=6 (P=0. 51); I 2=0% Test for overall effect: Z=4. 24 (P<0. 0001) Fenoldopam n/N 0/10 0/95 0/14 0/80 0/12 3/28 0/15 4/40 12/108 8/46 3/34 0/19 0/29 528 Control n/N 0/10 8/98 0/13 3/80 0/12 4/30 0/15 4/40 24/108 18/46 10/36 0/13 0/30 531 OR (fixed) 95% CI Weight (%) 13. 03 5. 44 5. 40 5. 63 33. 38 23. 27 13. 86 100. 0 Fenoldopam may prevent RRT and reducing mortality in patients undergoing cardiovascular surgery. Cicchetti Cogliati Caimmi Pittarello Sheinbaum Bove Ranucci Roasio Tumlin Martinelli Oliver Total (95% CI) Total events: 28 (Fenoldopam), 55 (control) Total for heterogeneity: Chi 2=4. 12; df=6 (P=0. 66); I 2=0% Test for overall effect: Z=3. 10 (P=0. 002) 0/10 4/95 0/80 0/12 2/28 4/40 7/108 8/46 3/36 0/17 0/29 501 0/10 5/98 0/80 0/12 6/30 3/40 17/108 19/46 4/36 0/13 1/30 503 0. 1 0. 2 0. 5 1 Favors Fenoldopam 2 5 OR (fixed) 95% CI Not estimable 0. 06 (0. 00, 0. 98) Not estimable 0. 14 (0. 01, 2. 71) Not estimable 0. 78 (0. 16, 3. 84) Not estimable 1. 00 (0. 23, 4. 31) 0. 44 (0. 21, 0. 93) 0. 33 (0. 12, 0. 86) 0. 25 (0. 06, 1. 01) Not estimable 0. 37 (0. 23, 0. 59) Not estimable 0. 82 (0. 21, 3. 14) Not estimable 0. 31 (0. 06, 1. 67) 1. 37 (0. 29, 6. 56) 0. 37 (0. 15, 0. 94) 0. 30 (0. 11, 0. 78) 0. 73 (0. 15, 3. 51) Not estimable 0. 33 (0. 01, 8. 52) 0. 46 (0. 29, 0. 75) 10 Favors control Landoni et al: J Cardiothorac Vasc Anesth 22(1): 27, 2008 © 2016 MFMER | 3572290 -16

Preoperative Statin Therapy: Mortality Study or subcategory Christenson Dotani et l Pan et al Ali et al Subramanian et al Chello et al Clark et al Collard et al Pascual et al Patti et al Colman et al Magovern et al Mariscalco et al Powell et al Thielmann et al Total (95% CI) Total events: 340 (Statin), 490 (control) Total for heterogeneity: X 2=14. 06; df=12 (P=0. 30); I 2=14. 6% Test for overall effect: Z=7. 27 (P<0. 00001) CSA-AKI A Meta-Analysis • 3 RCTs + 16 observational studies • 31, 725 patients Christenson Pan et al Chello et al Tabata et al Thielmann et al Total (95% CI) Total events: 165 (Statin), 97 (control) Total for heterogeneity: X 2=9. 59; df=4 (P=0. 05); 1 2=58. 3% Test for overall effect: Z=0. 95 (P=0. 34) Statin n/N 0/40 0/104 17/943 92/3555 6/654 0/20 26/1044 26/1352 2/87 2/101 53/1248 17/1004 0/218 32/2334 67/2592 15296 Control n/N 0/37 8/219 27/720 96/1914 9/654 0/20 155/2785 32/1314 7/54 2/99 42/686 39/1373 1/187 53/2405 19/754 13221 3/40 59/943 1/20 10/641 92/2592 4236 8/37 39/720 1/20 25/641 24/754 2172 OR (fixed) 95% CI Weight (%) 18. 04 6. 97 1. 85 0. 43 11. 36 7. 09 0. 35 11. 27 6. 28 100. 00 OR (fixed) 95% CI Not estimable 0. 12 (0. 01 -2. 08) 0. 47 (0. 25 -0. 87) 0. 50 (0. 38 -0. 67) 0. 66 (0. 23 -1. 88) Not estimable 0. 43 (0. 28 -0. 66) 0. 79 (0. 47 -1. 33) 0. 16 (0. 03 -0. 79) 0. 98 (0. 14 -7. 10) 0. 68 (0. 45 -1. 03) 0. 59 (0. 33 -1. 05) 0. 28 (0. 01 -7. 03) 0. 62 (0. 40 -0. 96) 1. 03 (0. 61 -1. 72) 0. 57 (0. 49, 0. 67) 10. 29 32. 67 3. 13 22. 55 31. 36 100. 0 0. 29 (0. 07 -1. 21) 1. 17 (0. 77 -1. 77) 1. 00 (0. 06 -17. 18) 0. 39 (0. 19 -0. 82) 1. 12 (0. 71 -1. 77) 0. 78 (0. 46 -1. 31) 1. 20 6. 58 26. 62 1. 95 Use of preoperative statin can reduce early all-cause mortality, but can not prevent CSA-AKI 0. 1 0. 2 0. 5 1 2 5 10 Favors statins Favors control Liakopoulos et al: Eer Heart J, 2008 © 2016 MFMER | 3572290 -17

N-acetylcysteine A Meta-Analysis Mortality Study or subcategory Molnar 2003 Tossios 2003 Burns 2005 Hynninen 2006 Macedo 2006 Ristikankare 2006 El-Hamamsy 2007 Haase 2007 Wijeysundera 2007 Sisillo 2008 Total (95% CI) Total events: 28 (NAC), 31 (control) Total for heterogeneity: Chi 2=8. 52; df=8 (P=0. 4); 1 2=6. 1% Test for overall effect: Z=0. 17 (P=0. 9) RRT • 10 RCTs • 1, 193 patients Burns 2005 Hynninen 2006 Macedo 2006 Ristikankare 2006 Haase 2007 Wijeysundera 2007 Sisillo 2008 Total (95% CI) Total events: 14 (NAC), 14 (control) Total for heterogeneity: Chi 2=5. 17; df=5 (P=0. 4); 1 2=3. 3% Test for overall effect: Z=0. 09 (P=0. 9) NAC n/N 7/40 0/20 5/148 1/34 6/18 1/38 3/50 0/30 0/88 5/129 595 Control n/N 7/39 0/20 4/147 0/35 4/24 2/39 0/50 1/30 7/87 6/127 598 1/148 0/34 1/18 1/38 0/30 1/88 10/129 485 3/147 0/35 0/24 0/39 2/30 3/87 6/125 487 OR (fixed) 95% CI Weight (%) 23. 56 18. 25 3. 40 15. 65 5. 88 3. 97 3. 39 4. 27 21. 63 100. 00 Perioperative N-acetylcysteine can not reduce mortality of major surgery does not reduce AKI-RRT 0. 01 0. 1 Favors NAC 12. 83 6. 35 6. 46 7. 10 12. 74 54. 52 100. 00 OR (fixed) 95% CI 0. 97 (0. 31, 3. 08) Not estimable 1. 25 (0. 33, 4. 75) 3. 18 (0. 13, 80. 79) 2. 50 (0. 58, 10. 70) 0. 50 (0. 04, 5. 76) 7. 44 (0. 37, 147. 92) 0. 32 (0. 01, 8. 24) 0. 06 (0. 00, 1. 08) 0. 81 (0. 24, 2. 74) 1. 05 (0. 58, 1. 92) 0. 33 (0. 03, 3. 18) No estimable 4. 20 (0. 16, 109. 28) 3. 16 (0. 12, 80. 02) 0. 19 (0. 01, 4. 06) 0. 32 (0. 03, 3. 16) 1. 67 (0. 59, 7. 73) 1. 04 (0. 45, 2. 37) 1 10 100 Favors control Ho et al: Am J Kidney Dis, 2009 © 2016 MFMER | 3572290 -18

Remote Ischemic Preconditioning Randomized Clinical Trial • 240 patients at high risk for AKI: Cleveland score > 6 • RIPC: 3 cycles of 5 -minute ischemia and 5 -minute reperfusion in one upper arm after induction of anesthesia Primary and secondary study outcomes, by group Control n=120 RIPC n=120 14 (11. 7) 17 (14. 2) 8 (6. 7) 7 (5. 8) 19 (15. 8) 15 (12 -21) 4 (2 -7) 13 (10 -19) 4 (3. 3) 5 (4. 2) 3 (2. 5) 7 (5. 8) 14 (11 -21) 3 (2 -5) 12 (9 -19) 6 (5. 0) 7 (5. 8) 6 (5. 0) 2 (1. 7) ARR or median difference (95% CI) P RIPC significantly reduced the rate of AKI and Primary outcome, no. (%) use of RRT among high-risk patients AKI within 72 hr 63 (52. 5) 45 (37. 5) 15 (2. 56 to 27. 44) 0. 02 AKI stage undergoing cardiac surgery 1 32 (26. 7) 30 (25) 2 3 Second outcomes RRT, no. (%) Mechanical ventilation, median (IQR), hr Intensive care unit stay, median (IQR), d Hospital stay, median (IQR), d In-hospital death, no. (%) 30 -d mortality, no. (%) Myocardial infarction, no. (%) Stroke, no. (%) 10 (2. 25 to 17. 5) 1 (-1. 54 to 4) 1 (0 to 2) 1 (-2 to 2. 5) 1. 67 (0 to 6. 72) 1. 67 (0 to 7. 18) 0. 83 (0 to 6. 12) 0. 83 (0 to 4. 45) 0. 01 0. 16 0. 04 0. 45 0. 54 0. 77 0. 76 0. 65 Zarbock et al: JAMA, 2015 © 2016 MFMER | 3572290 -19

KDIGO AKI Guideline Provide RRT to achieve the goals of electrolyte, acid-base, solute, and fluid balance that will meet the patient’s needs Goal directed renal replacement therapy GDRRT Jiarui et al, Journal of Cardio Surg, 2014 © 2016 MFMER | 3572290 -20

Goals of GDRRT Solute • sp. Kt/V 1. 4 per session • BUN 25 mmol/L • Qdialysate 25 m. L/kg/h Volume • 24 h fluid output intake • Urine output 0. 5 m. L/kg/h • Controlled acute pulmonary edema • Reduction of peripheral edema • Hematocrit 30% Electrolyte and p. H • Electrolyte and acid-base parameters normal or near normal • 3. 5 < K+ 5. 5 mmol/L • HCO 3 16 mmol/L • p. H 7. 20 Hemodynamics • MAP 65 mm Hg • CVP 8 -12 mm Hg • Sa. O 2 93% © 2016 MFMER | 3572290 -21

Goals of GDRRT CV surgery ICU Nephrology TEAM! M multiple-organ support O oxygen saturation V volume I immune function E electrolyte & p. H © 2016 MFMER | 3572290 -22
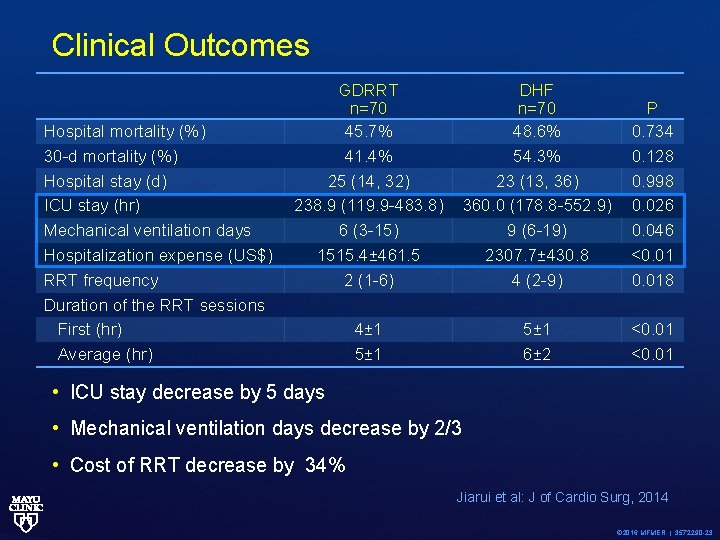
Clinical Outcomes Hospital mortality (%) 30 -d mortality (%) Hospital stay (d) ICU stay (hr) Mechanical ventilation days Hospitalization expense (US$) RRT frequency Duration of the RRT sessions First (hr) Average (hr) GDRRT n=70 45. 7% 41. 4% 25 (14, 32) 238. 9 (119. 9 -483. 8) 6 (3 -15) 1515. 4± 461. 5 2 (1 -6) DHF n=70 48. 6% 54. 3% 23 (13, 36) 360. 0 (178. 8 -552. 9) 9 (6 -19) 2307. 7± 430. 8 4 (2 -9) P 0. 734 0. 128 0. 998 0. 026 0. 046 <0. 018 4± 1 5± 1 6± 2 <0. 01 • ICU stay decrease by 5 days • Mechanical ventilation days decrease by 2/3 • Cost of RRT decrease by 34% Jiarui et al: J of Cardio Surg, 2014 © 2016 MFMER | 3572290 -23
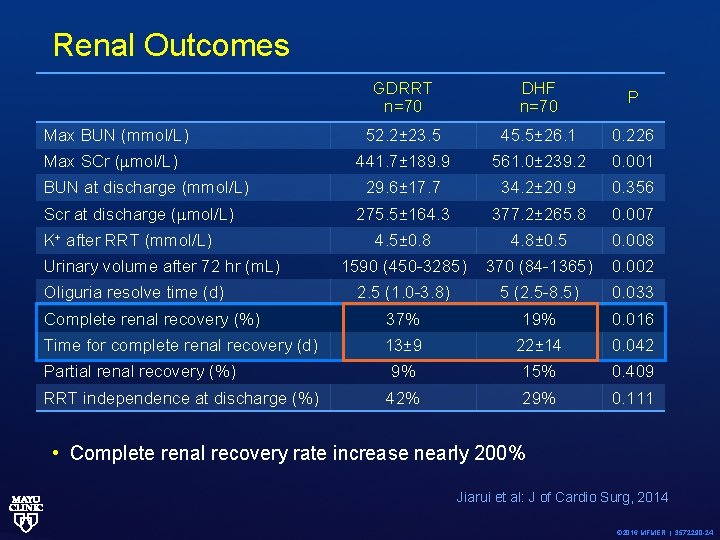
Renal Outcomes GDRRT n=70 DHF n=70 P 52. 2± 23. 5 45. 5± 26. 1 0. 226 441. 7± 189. 9 561. 0± 239. 2 0. 001 29. 6± 17. 7 34. 2± 20. 9 0. 356 275. 5± 164. 3 377. 2± 265. 8 0. 007 4. 5± 0. 8 4. 8± 0. 5 0. 008 1590 (450 -3285) 370 (84 -1365) 0. 002 2. 5 (1. 0 -3. 8) 5 (2. 5 -8. 5) 0. 033 Complete renal recovery (%) 37% 19% 0. 016 Time for complete renal recovery (d) 13± 9 22± 14 0. 042 Partial renal recovery (%) 9% 15% 0. 409 RRT independence at discharge (%) 42% 29% 0. 111 Max BUN (mmol/L) Max SCr ( mol/L) BUN at discharge (mmol/L) Scr at discharge ( mol/L) K+ after RRT (mmol/L) Urinary volume after 72 hr (m. L) Oliguria resolve time (d) • Complete renal recovery rate increase nearly 200% Jiarui et al: J of Cardio Surg, 2014 © 2016 MFMER | 3572290 -24
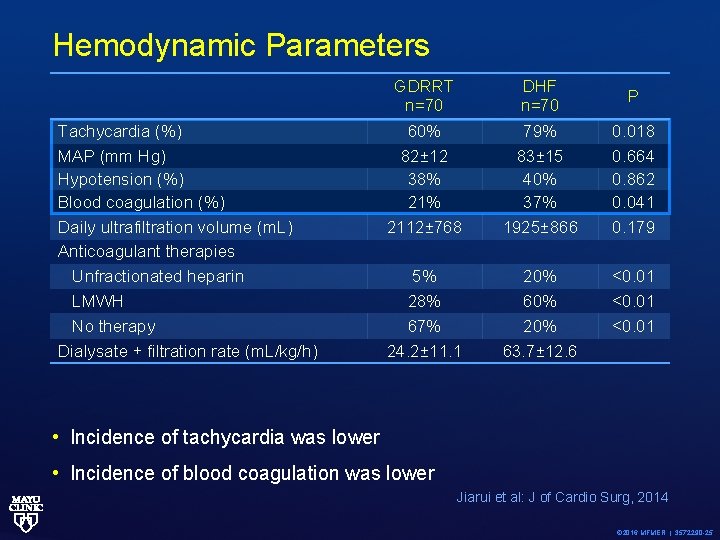

Hemodynamic Parameters Tachycardia (%) MAP (mm Hg) Hypotension (%) Blood coagulation (%) Daily ultrafiltration volume (m. L) Anticoagulant therapies Unfractionated heparin LMWH No therapy Dialysate + filtration rate (m. L/kg/h) GDRRT n=70 DHF n=70 P 60% 82± 12 38% 2112± 768 79% 83± 15 40% 37% 1925± 866 0. 018 0. 664 0. 862 0. 041 0. 179 5% 28% 67% 24. 2± 11. 1 20% 60% 20% 63. 7± 12. 6 <0. 01 • Incidence of tachycardia was lower • Incidence of blood coagulation was lower Jiarui et al: J of Cardio Surg, 2014 © 2016 MFMER | 3572290 -25
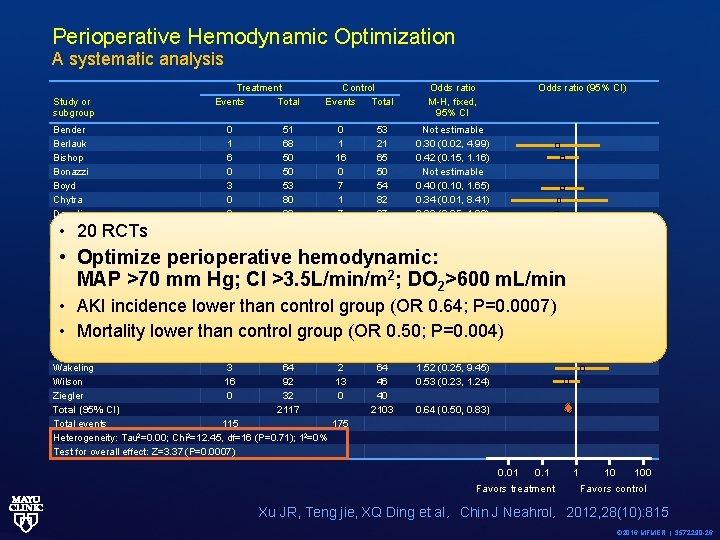

Perioperative Hemodynamic Optimization A systematic analysis Study or subgroup Treatment Events Total Control Events Total Bender 0 51 Berlauk 1 68 Bishop 6 50 Bonazzi 0 50 Boyd 3 53 Chytra 0 80 Donati 2 68 Gan 2 50 Lobo 2 19 Malhotra 1 13 Mc. Kendry 1 89 Noblett 0 51 Pearse 3 62 Polonen 1 196 Sandham 70 941 Shoemaker 0 28 Valentine 4 60 Wakeling 3 64 Wilson 16 92 Ziegler 0 32 Total (95% CI) 2117 Total events 115 Heterogeneity: Tau 2=0. 00; Chi 2=12. 45, df=16 (P=0. 71); 12=0% Test for overall effect: Z=3. 37 (P=0. 0007) • 20 RCTs 0 1 16 0 7 1 7 4 1 1 3 2 4 3 95 14 1 2 13 0 53 21 65 50 54 82 67 50 18 14 85 2 52 60 197 965 60 60 64 46 40 2103 Odds ratio M-H, fixed, 95% CI Odds ratio (95% CI) Not estimable 0. 30 (0. 02, 4. 99) 0. 42 (0. 15, 1. 16) Not estimable 0. 40 (0. 10, 1. 65) 0. 34 (0. 01, 8. 41) 0. 26 (0. 05, 1. 30) 0. 48 (0. 08, 2. 74) 2. 00 (0. 17, 24. 19) 1. 08 (0. 06, 19. 31) 0. 31 (0. 03, 3. 05) 0. 20 (0. 01, 4. 19) 2 0. 71 (0. 15, 3. 32) 0. 33 (0. 03, 3. 22) 0. 74 (0. 53, 1. 02) 0. 06 (0. 00, 0. 98) 4. 21 (0. 46, 38. 86) 1. 52 (0. 25, 9. 45) 0. 53 (0. 23, 1. 24) • Optimize perioperative hemodynamic: MAP >70 mm Hg; CI >3. 5 L/min/m ; DO >600 m. L/min • AKI incidence lower than control group (OR 0. 64; P=0. 0007) • Mortality lower than control group (OR 0. 50; P=0. 004) 0. 64 (0. 50, 0. 83) 175 0. 01 0. 1 Favors treatment 1 10 100 Favors control Xu JR, Teng jie, XQ Ding et al,Chin J Neahrol,2012, 28(10): 815 © 2016 MFMER | 3572290 -26
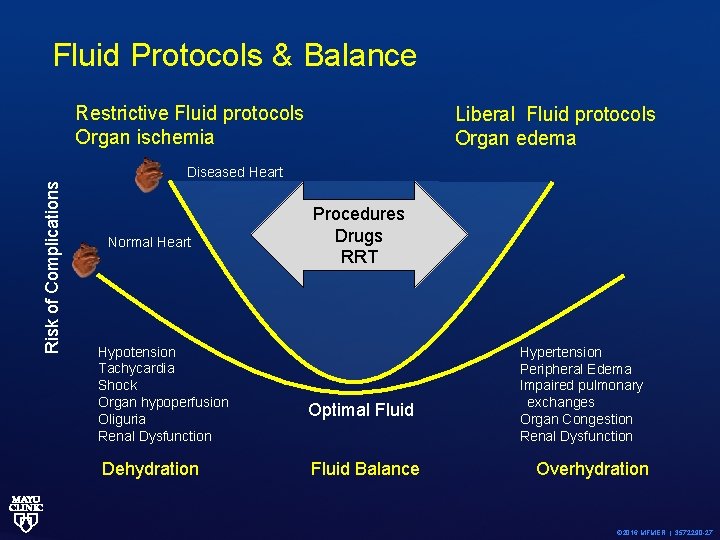
Fluid Protocols & Balance Restrictive Fluid protocols Organ ischemia Liberal Fluid protocols Organ edema Risk of Complications Diseased Heart Normal Heart Hypotension Tachycardia Shock Organ hypoperfusion Oliguria Renal Dysfunction Dehydration Procedures Drugs RRT Optimal Fluid Balance Hypertension Peripheral Edema Impaired pulmonary exchanges Organ Congestion Renal Dysfunction Overhydration © 2016 MFMER | 3572290 -27

Fluid Overload – Common Complication of CS • Retrospective • CSA-AKI-RRT patients • n=312 • Fluid overload • Relative fluid balance ≥ 10% baseline weight No Fluid overload 44. 2% Early Postoperative Fluid overload 32% Late Postoperative Fluid Overload 23. 8% Xu JR, Teng jie, XQ Ding et al,Chin J Neahrol,2012, 28(10): 815 © 2016 MFMER | 3572290 -28
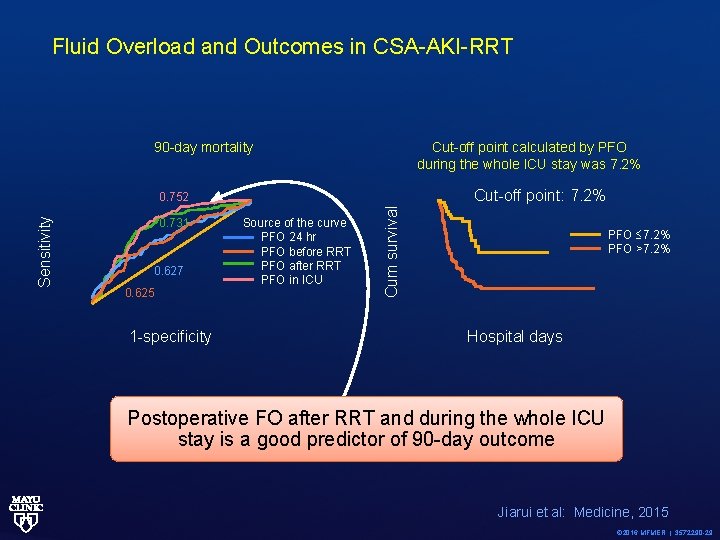
Fluid Overload and Outcomes in CSA-AKI-RRT 90 -day mortality Cut-off point calculated by PFO during the whole ICU stay was 7. 2% Cut-off point: 7. 2% 0. 731 0. 627 0. 625 1 -specificity Source of the curve PFO 24 hr PFO before RRT PFO after RRT PFO in ICU Cum survival Sensitivity 0. 752 PFO 7. 2% PFO >7. 2% Hospital days Postoperative FO after RRT and during the whole ICU stay is a good predictor of 90 -day outcome Jiarui et al: Medicine, 2015 © 2016 MFMER | 3572290 -29
LIVER © 2016 MFMER | 3572290 -30
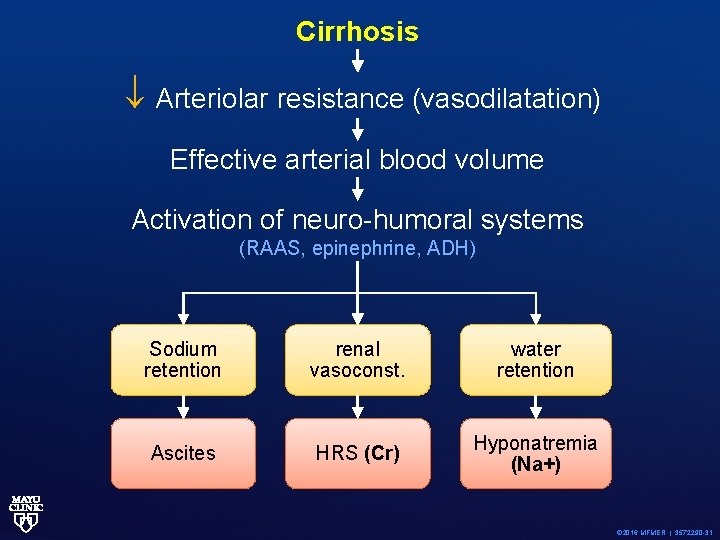
Cirrhosis Arteriolar resistance (vasodilatation) Effective arterial blood volume Activation of neuro-humoral systems (RAAS, epinephrine, ADH) Sodium retention renal vasoconst. water retention Ascites HRS (Cr) Hyponatremia (Na+) © 2016 MFMER | 3572290 -31

MELD Equation • MELD =(0. 957 log(creatinine) + 0. 378 x log(bilirubin) +1. 12 log(INR) +0. 643) x 10 • http: //www. mayoclinic. org/gi-rst/mayomodel 6. html © 2016 MFMER | 3572290 -32
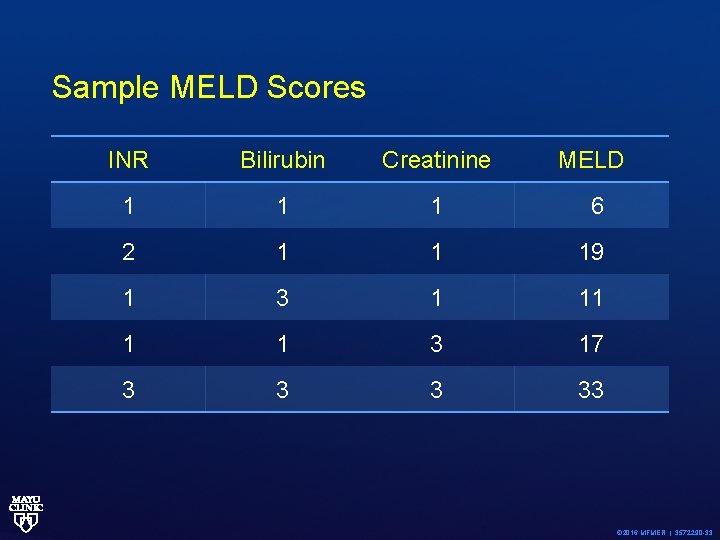
Sample MELD Scores INR Bilirubin Creatinine MELD 1 1 1 6 2 1 1 19 1 3 1 11 1 1 3 17 3 33 © 2016 MFMER | 3572290 -33
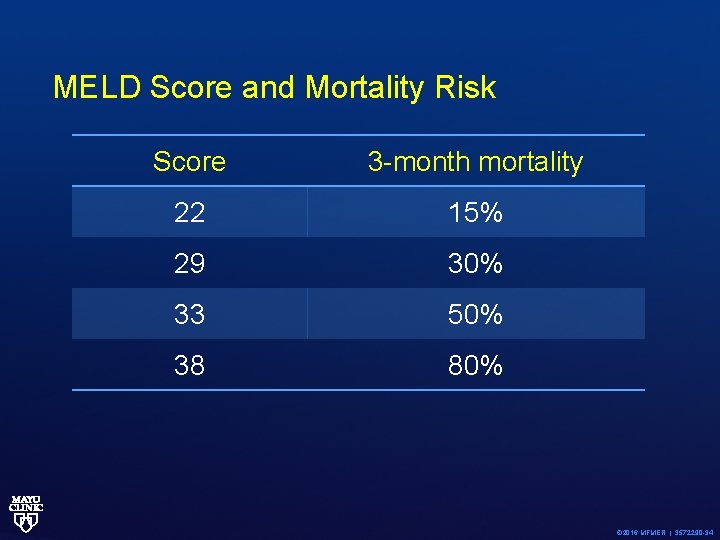
MELD Score and Mortality Risk Score 3 -month mortality 22 15% 29 30% 33 50% 38 80% © 2016 MFMER | 3572290 -34
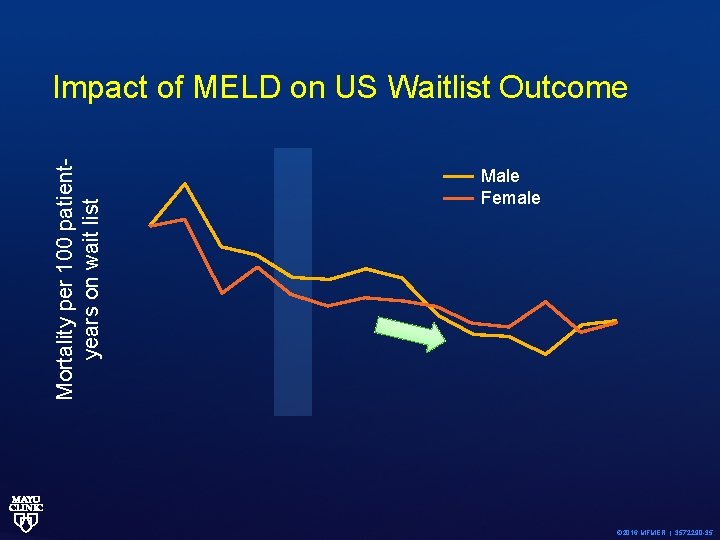
Mortality per 100 patientyears on wait list Impact of MELD on US Waitlist Outcome Male Female © 2016 MFMER | 3572290 -35
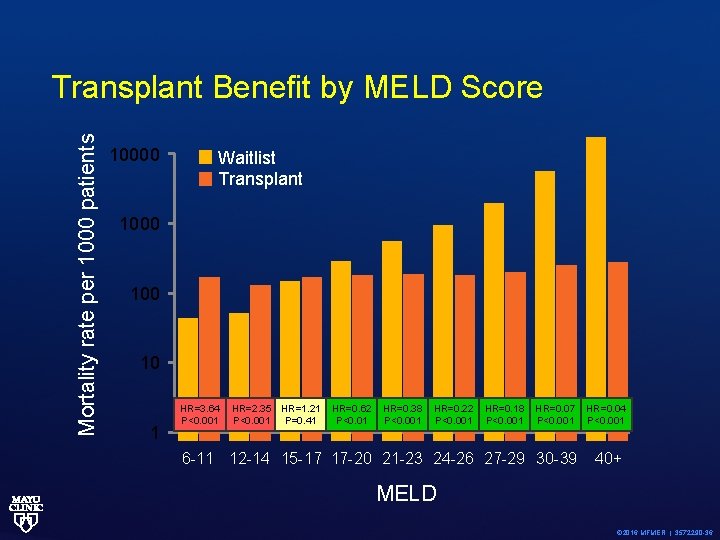
Mortality rate per 1000 patients Transplant Benefit by MELD Score 10000 Waitlist Transplant 1000 10 1 HR=3. 64 P<0. 001 HR=2. 35 HR=1. 21 P<0. 001 P=0. 41 HR=0. 62 P<0. 01 HR=0. 38 P<0. 001 HR=0. 22 P<0. 001 HR=0. 18 P<0. 001 HR=0. 07 P<0. 001 6 -11 12 -14 15 -17 17 -20 21 -23 24 -26 27 -29 30 -39 HR=0. 04 P<0. 001 40+ MELD © 2016 MFMER | 3572290 -36
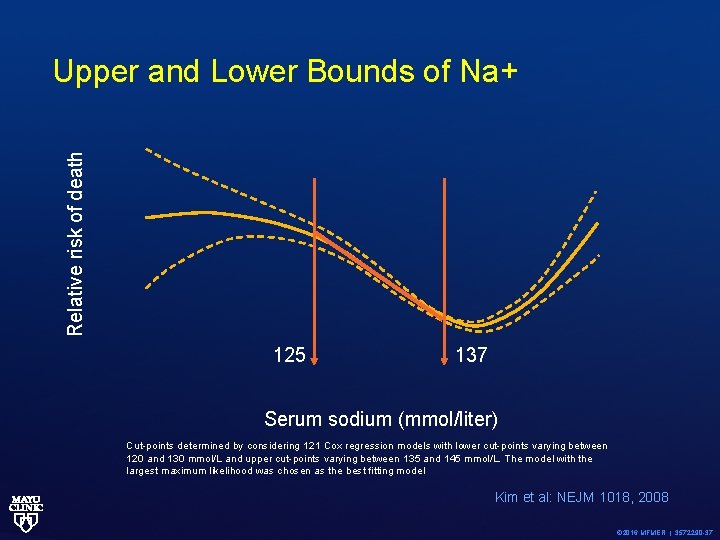
Relative risk of death Upper and Lower Bounds of Na+ 125 137 Serum sodium (mmol/liter) Cut-points determined by considering 121 Cox regression models with lower cut-points varying between 120 and 130 mmol/L and upper cut-points varying between 135 and 145 mmol/L. The model with the largest maximum likelihood was chosen as the best fitting model Kim et al: NEJM 1018, 2008 © 2016 MFMER | 3572290 -37
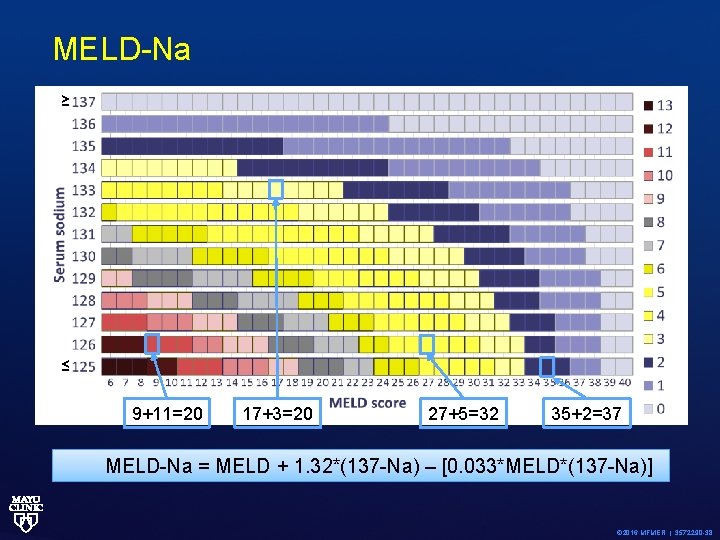
MELD-Na ≥ ≤ 9+11=20 17+3=20 27+5=32 35+2=37 MELD-Na = MELD + 1. 32*(137 -Na) – [0. 033*MELD*(137 -Na)] © 2016 MFMER | 3572290 -38
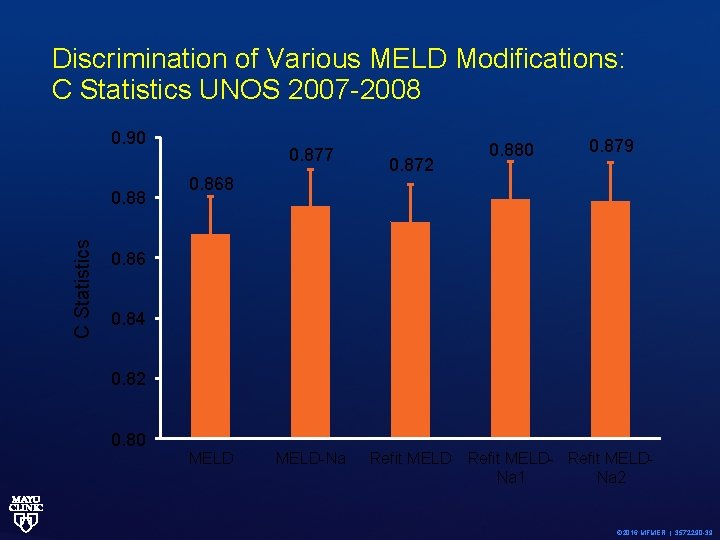
Discrimination of Various MELD Modifications: C Statistics UNOS 2007 -2008 0. 90 C Statistics 0. 88 0. 877 0. 868 0. 872 0. 880 0. 879 0. 86 0. 84 0. 82 0. 80 MELD-Na Refit MELD- Refit MELDNa 1 Na 2 © 2016 MFMER | 3572290 -39
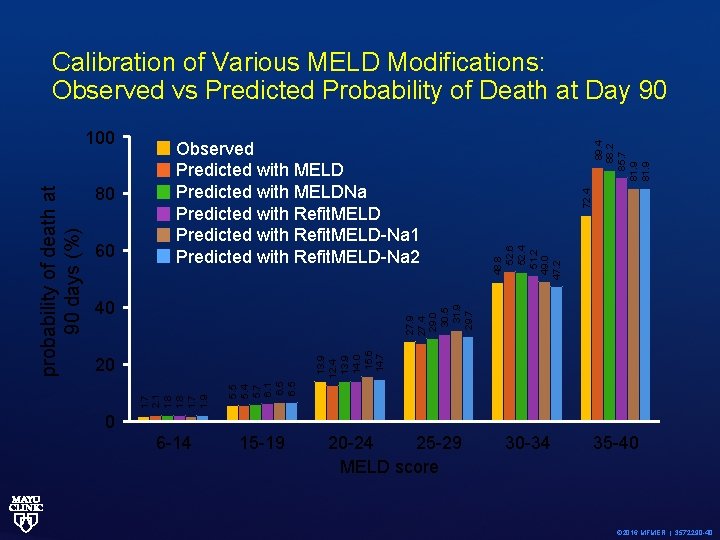
60 72. 4 13. 9 14. 0 15. 6 14. 7 27. 9 27. 4 29. 0 30. 5 31. 9 29. 7 40 48. 8 52. 6 52. 4 51. 2 49. 0 47. 2 80 Observed Predicted with MELDNa Predicted with Refit. MELD-Na 1 Predicted with Refit. MELD-Na 2 5. 5 5. 4 5. 7 6. 1 6. 5 20 1. 7 2. 1 1. 8 1. 7 1. 9 probability of death at 90 days (%) 100 89. 4 88. 2 85. 7 81. 9 Calibration of Various MELD Modifications: Observed vs Predicted Probability of Death at Day 90 0 6 -14 15 -19 20 -24 25 -29 MELD score 30 -34 35 -40 © 2016 MFMER | 3572290 -40
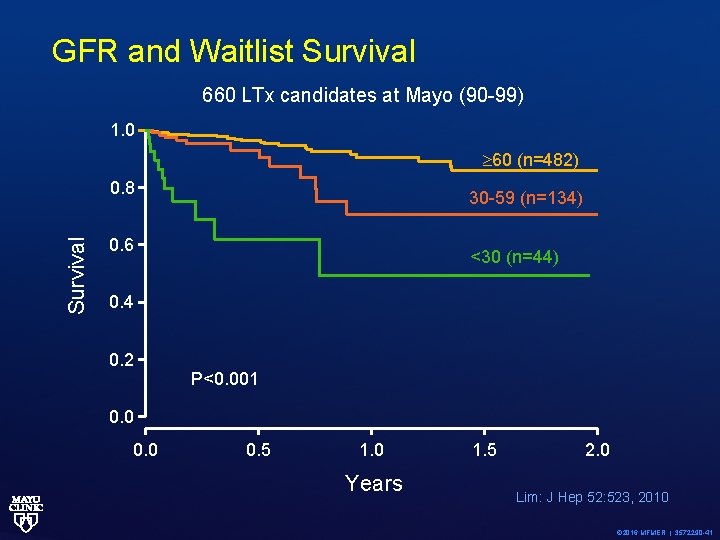
GFR and Waitlist Survival 660 LTx candidates at Mayo (90 -99) 1. 0 60 (n=482) Survival 0. 8 30 -59 (n=134) 0. 6 <30 (n=44) 0. 4 0. 2 P<0. 001 0. 0 0. 5 1. 0 Years 1. 5 2. 0 Lim: J Hep 52: 523, 2010 © 2016 MFMER | 3572290 -41
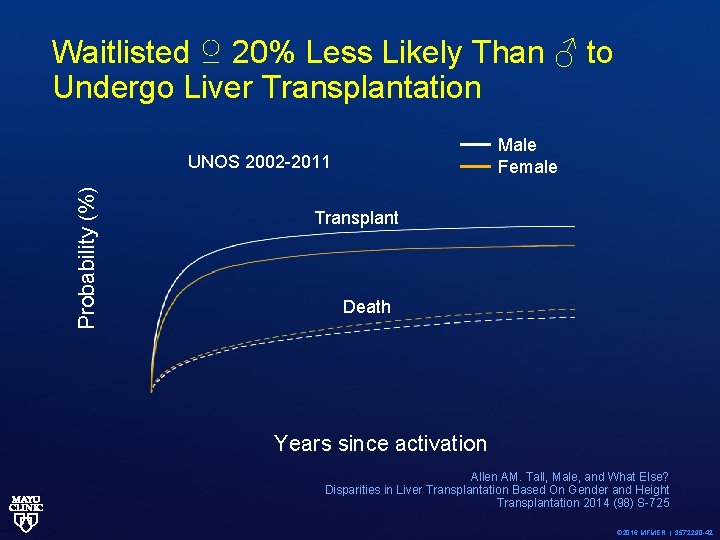
Waitlisted ♀ 20% Less Likely Than ♂ to Undergo Liver Transplantation Male Female Probability (%) UNOS 2002 -2011 Transplant Death Years since activation Allen AM. Tall, Male, and What Else? Disparities in Liver Transplantation Based On Gender and Height Transplantation 2014 (98) S-725 © 2016 MFMER | 3572290 -42

Factors That Disadvantage Women Men Women Shorter Small body ≠ big liver Height Less muscle mass Lower creatinine = lower MELD exceptions More hepatocellular carcinoma = MELD exception points ? © 2016 MFMER | 3572290 -43
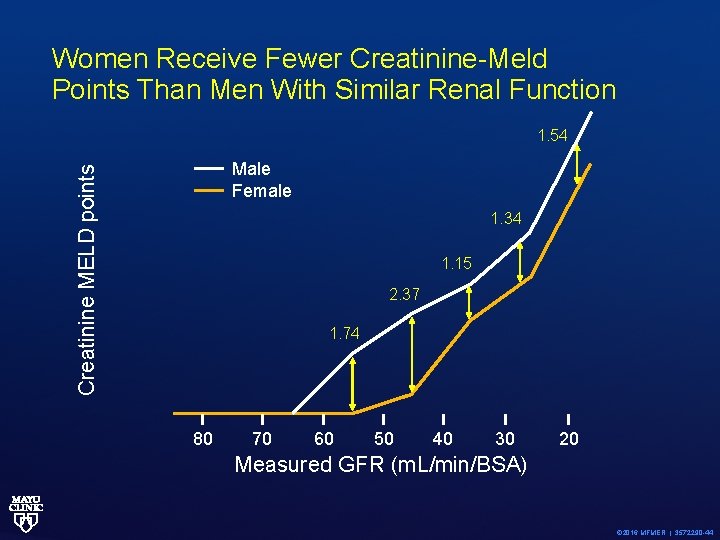
Women Receive Fewer Creatinine-Meld Points Than Men With Similar Renal Function 1. 54 Creatinine MELD points Male Female 1. 34 1. 15 2. 37 1. 74 80 70 60 50 40 30 20 Measured GFR (m. L/min/BSA) © 2016 MFMER | 3572290 -44
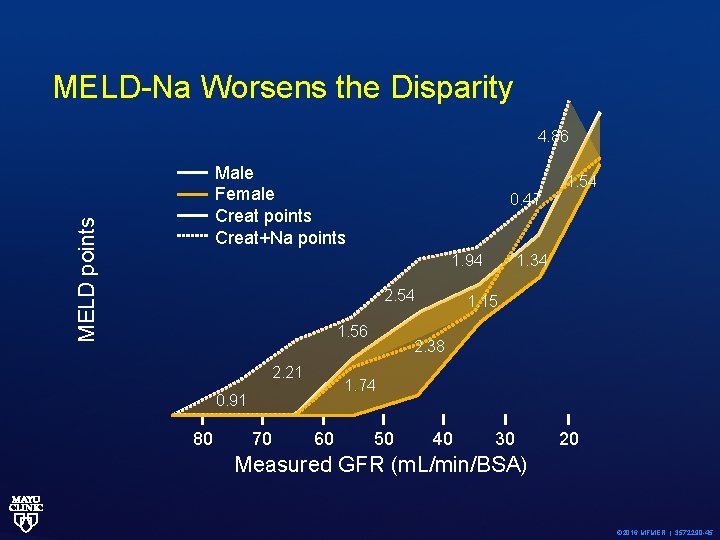
MELD-Na Worsens the Disparity 4. 86 MELD points Male Female Creat points Creat+Na points 0. 47 1. 94 2. 54 1. 56 2. 21 70 1. 34 1. 15 2. 38 1. 74 0. 91 80 1. 54 60 50 40 30 20 Measured GFR (m. L/min/BSA) © 2016 MFMER | 3572290 -45

Thank you for your attention Questions © 2016 MFMER | 3572290 -46
- Slides: 46