AKI and Dialysis Management in the ICU Assessment


























- Slides: 37

AKI and Dialysis Management in the ICU Assessment, Dialysis modalities and special cases.

Disclosures I have one disclosure, Illustration credits: Maggie Murray.

Practicing Acute Nephrology, the good and bad. Good ● Even after injuries, Kidneys are resilient. ● You get to meet lots of different specialties, kidneys don’t like drugs, fevers, low BP’s, high BP’s, pressure. . . ● We can replace kidney function with dialysis, even long term. ● We can make your labs look better and remove edema which also looks better. ● Everybody just feels better when CRRT (maybe not HD) is running. Bad ● Kidneys are sensitive, they don’t like anyone. ● Always looking backwards. Once an injury occurs (ATN), there is little we can do to treat the underlying injury ● Dialysis is complicated with many potential difficulties (and $$$). ● “Stuff happens” on dialysis, we remove “good” stuff too (abx, ? immune complexes) ● Difficult to stop once started (mentally, not ethically). Can get “stuck” on CRRT

Nephrologists-Always keeping it simple.

Kidneys-The basics • There are 2 of them, usually. • They weigh 150 g each. (Less than 1# together). 10 -12 cm • Each have 1 -1. 2 million Glomeruli • Renal arteries (afferent arteriole) carry ~20% of the CO, 25% of the plasma is turned into glomerular filtrate, blood cells, protein and ~75% of fluid leaves the kidneys via the efferent arteriole. • Regulate volume/BP, maintain electrolyte and p. H homeostasis and clear “uremic toxins”, these are the goals of any dialysis as well.

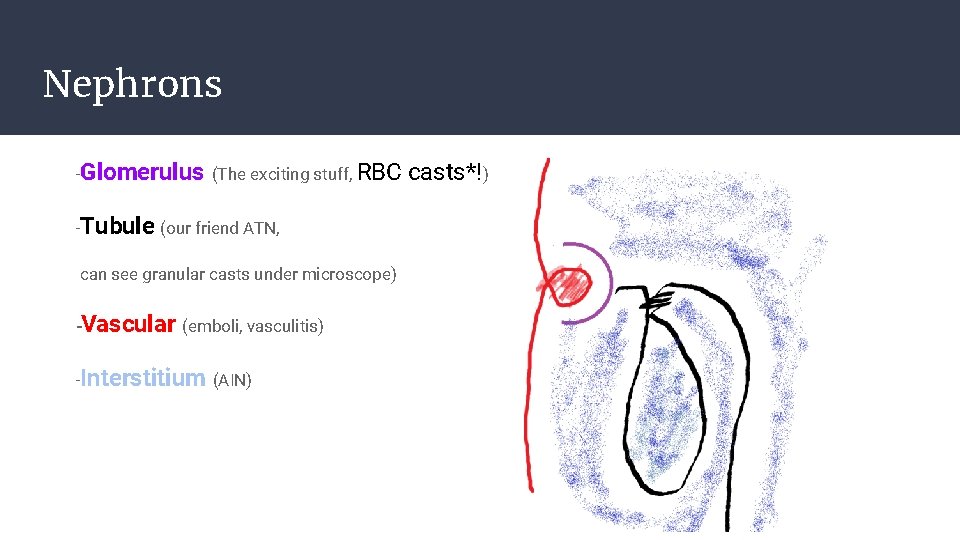
Nephrons -Glomerulus (The exciting stuff, RBC -Tubule (our friend ATN, can see granular casts under microscope) -Vascular (emboli, vasculitis) -Interstitium (AIN) casts*!)

Nephrology lingo UOP: With or without diuretics. Oliguric- <500 cc/24 h Anuric <50 cc/24 h Polyuric- >2. 5 -3 L/24 h. RRT-Renal replacement therapy-any form of dialysis. UF-Ultrafiltration-Volume removal Clearance-The removal of uremic toxins and measured chemistries (Cr, BUN, K etc)

AKI-Definition and Epidemiology -4% as primary indication for admission, 18% incidence during admission -Defined as Cr rise of >50% after ruling out pre/post-renal etiology. -Most (⅔) inpatient Cr rise is ATN, most ED (⅔) are prerenal. -Please order UA, foley (if UOP low), Renal US, with nephrology consult. -Best predictor of kidney recovery is baseline renal fx. If no CKD, chances of recovery from AKI is 75% -”Innocent bystanders” are most of ICU AKI’s, recovery depends on general recovery from other acute illness. Usually not the first organs back to the party.

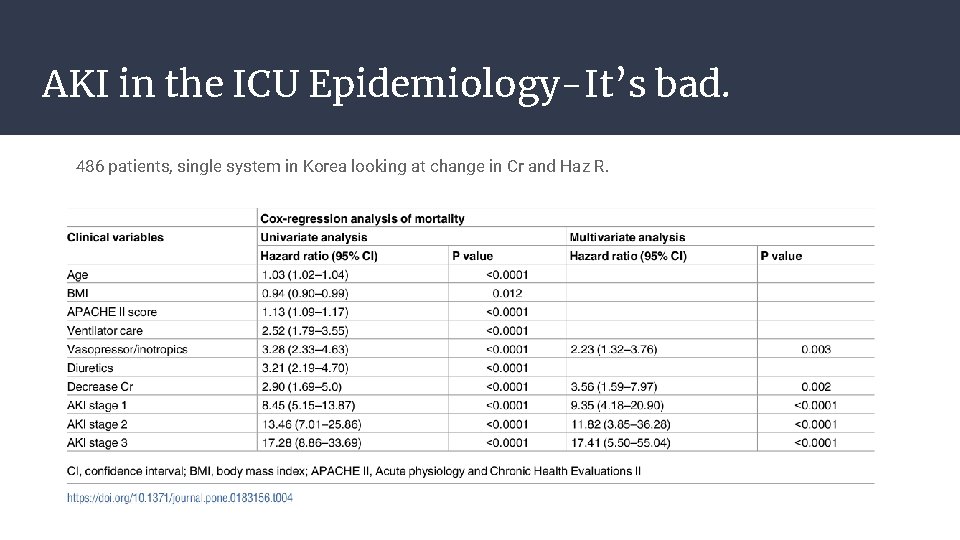
AKI in the ICU Epidemiology-It’s bad. 486 patients, single system in Korea looking at change in Cr and Haz R.

Let’s think about Creatinine -Normal muscle mass Cr production and excretion is ~1 g/day. Does your patient have normal muscle mass? (Be wary with CHF or Ascites). There is no magic number when dialysis is automatically started. -What was the Cr yesterday? What is the relationship between Cr and gfr with acute changes? If we did a bilateral nephrectomy on an otherwise healthy patient, what would the Cr be tomorrow? What would the gfr be? -Think about a ureteral-peritoneal fistula (kidney transplant) What’s the gfr vs Cr?

Elevated Creatinine vs AKI. Rule me out Prerenal -70% of community AKI’s -Low Urine Na -High SG on UA -High (20: 1) ratio of BUN/Cr (poor reabsorption of Cr by tubules) -FENA only useful if oliguric -Be suspicious if on diuretics ~70% ICU AKI’s. Intrarenal -70% of ICU AKI’s. -ATN is the vast majority -AIN, easy to miss. -RBC Casts are a sign of glomerular issue. -+ protein is common in AKI, should not be >1. 5 g/g Cr. -Different etiologies will behave differently Rule Me out too. Post Renal -Very Sharp Cr rise -Hydronephrosis on US or CT (RP fibrosis will not) -Be suspicious after any abdominal/pelvic surgery -Put a foley in before you consult renal for low UOP please.

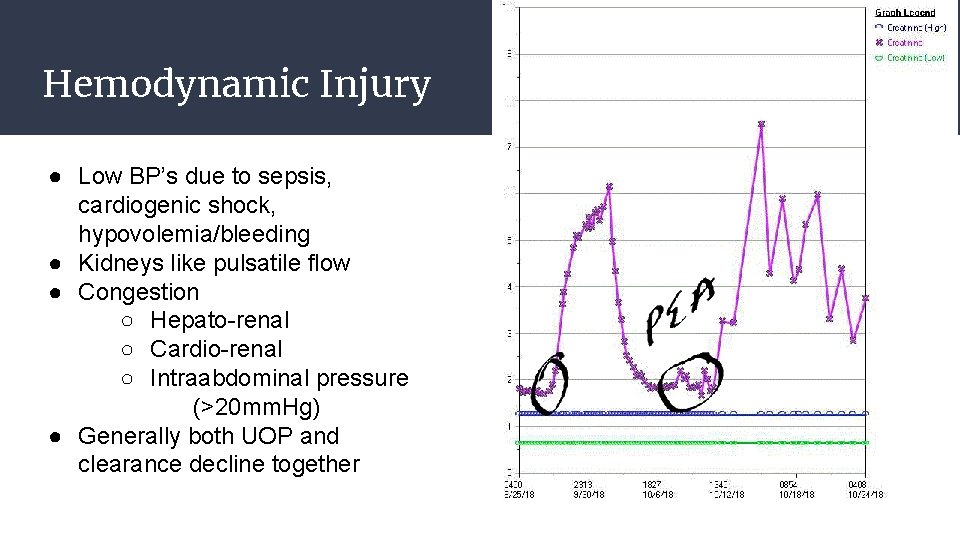
Hemodynamic Injury ● Low BP’s due to sepsis, cardiogenic shock, hypovolemia/bleeding ● Kidneys like pulsatile flow ● Congestion ○ Hepato-renal ○ Cardio-renal ○ Intraabdominal pressure (>20 mm. Hg) ● Generally both UOP and clearance decline together

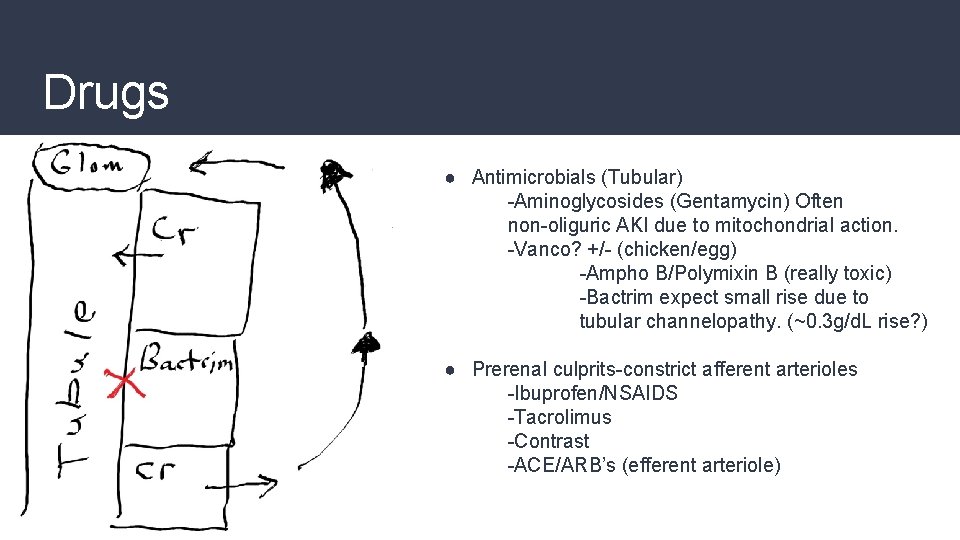
Drugs ● Antimicrobials (Tubular) -Aminoglycosides (Gentamycin) Often non-oliguric AKI due to mitochondrial action. -Vanco? +/- (chicken/egg) -Ampho B/Polymixin B (really toxic) -Bactrim expect small rise due to tubular channelopathy. (~0. 3 g/d. L rise? ) ● Prerenal culprits-constrict afferent arterioles -Ibuprofen/NSAIDS -Tacrolimus -Contrast -ACE/ARB’s (efferent arteriole)

Acute Interstitial Nephritis Something we can treat? ! ● Allergic reaction involving the interstitium of the kidney. ● Many meds can cause it, Abx are by % the most common, PPI’s cause the most due to # treated. ● Cr starts to rise 7 -10 days after initiation of the drug. ● Typically Cr will rise slowly (0. 3 -0. 5 g/d. L/day) and consistently, often non-oliguric or even polyuric. ● Rash, fever, eosinophils blood/urine, hematuria, but each are <50% incidence. ● Treatment is stopping the drug (obviously), steroids have been shown to benefit early in course 3 -5 days after Cr rise.

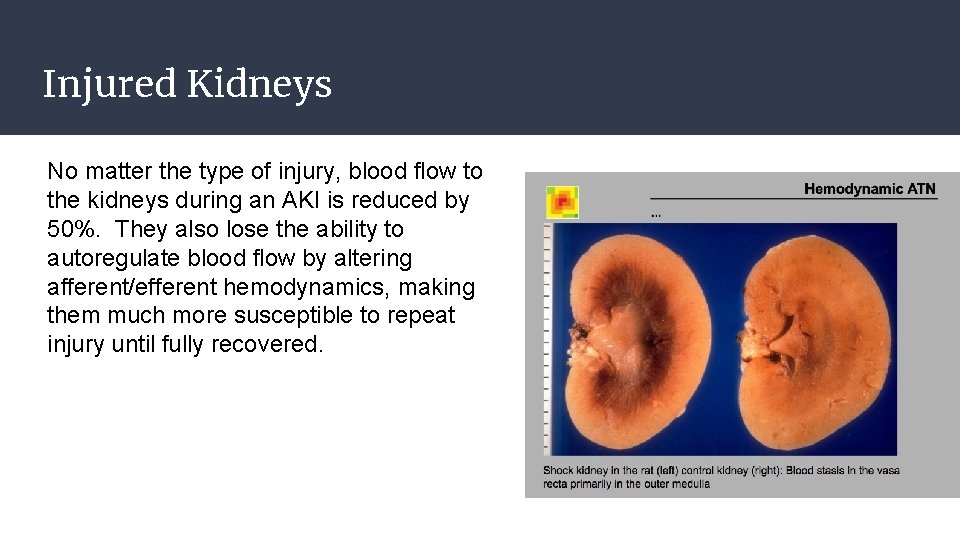
Injured Kidneys No matter the type of injury, blood flow to the kidneys during an AKI is reduced by 50%. They also lose the ability to autoregulate blood flow by altering afferent/efferent hemodynamics, making them much more susceptible to repeat injury until fully recovered.

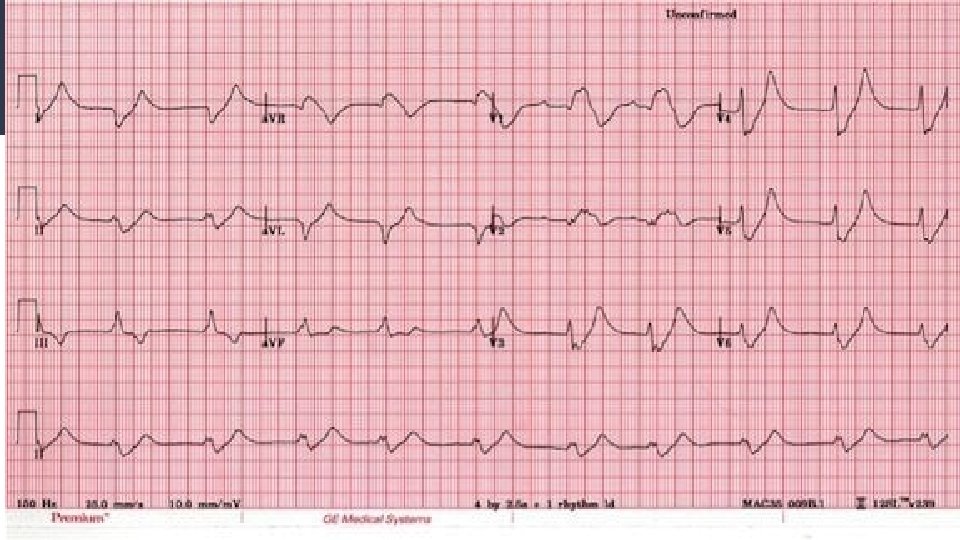
Indications for Dialysis-Hyperkalemia ● Hyperkalemia -Try to understand the cause ○ Intake/Output/Shifting-2 out of 3 are altered if K is high. (almost always multifactorial) ○ Lactic acidosis? Rhabdo? Hemolysis? (Phos will be up) ○ QRS widening generally starts at K of ~6. ○ Shifting will get you ~2 -3 hours and 1 -2 mmol/L (D 50/insulin, bicarb, albuterol) ○ Calcium will “stabilize” the cardiac membrane ○ Kayexalate can cause bowel ischemia. ○ Sodium Bicarb (Watch the serum sodium, each amp is 9% Na) ○ Heparin is an aldosterone antagonist, will bump a little.


Indications for Dialysis-Volume ● Hypervolemia ○ ○ Limit fluids, don’t keep fluid challenging an AKI after initial phase. Increasing O 2 needs w/Pulmonary edema suspected or on imaging Elevated JVD, PCWP and CVP Be careful with low albumin, low SVR states, they can be very edematous but intravascularly dry. ○ If we are giving fluid for low BP’s, don’t pull UF. ○ If filling pressures are high (>20 for CVP and PCWP), it’s time to try to pull fluid even with pressors.

Diuretics ● Diuretics are safe in AKI management, IF they are not prerenal. ○ Max dose of lasix=480 mg/day, bumex=10 -12 mg/day. Add metolazone if able (limited by metabolic acidosis). ○ There is no difference in IV absorbation of bumex/lasix, in PO form, bumex is 90%+ absorbed vs 60 -70% with lasix

Indications for Dialysis-HAGMA ● Metabolic Acidosis-What kind is it. p. H down to 7. 10 has been studied, no benefit to correcting. ● Computer will give the AG to you but correct for albumin. Another equation! Anion Gap=Na-(Cl-HCO 3)+ 2. 5(normal-measured albumin). ○ HAGMA (unmeasured missing acid) ■ If there is no suspicion of ingestion, it usually comes down to Lactate, renal failure or starvation ketones (2 -3 days of no sugar, body breaks down fat and can’t eliminate the acid via UOP) ■ Can buffer with bicarb, limited by Na or hypercapnia ○ NAGMA (Missing acid/base is accounted for but lost to the universe) ■ Loss of bicarb with diarrhea or with Renal Tubular acidosis, loss of H+ with upper GI ■ Replace the lost bicarb.

Indications for Dialysis-Uremia ● Uremia-It takes a few days at least. . . ○ NOT BUN >100, urea is not a toxin. ○ Buildup of unmeasured metabolites called “uremic toxins” ○ Gradual confusion, asterixis, nausea/vomiting, pericarditis, platelet dysfx ○ Difficult to assess in ICU patients due to vent/sedation/delerium ■ Often we run HD to “rule out” uremia. ■ If bleeding, can give DDAVP or conjugated estrogen, HD is +/- for “uremic plt’s” as plt function has been shown to drop after HD.

Does my patient need RRT? ● Do we acutely need to fix potassium or metabolic acidosis? ● Do we need to pull fluid? How much UF will we need to match intake? Is that the goal? ● If volume and electrolytes are issues, will diuretics be effective without causing electrolyte issues? ● What is the trajectory of renal function? If there is no sign of plateau in Cr and they are on track to gain multiple liters of fluid/day, you don’t need to wait until an emergency ● How much do you want to argue with your colleagues if the patient is headed towards RRT soon?

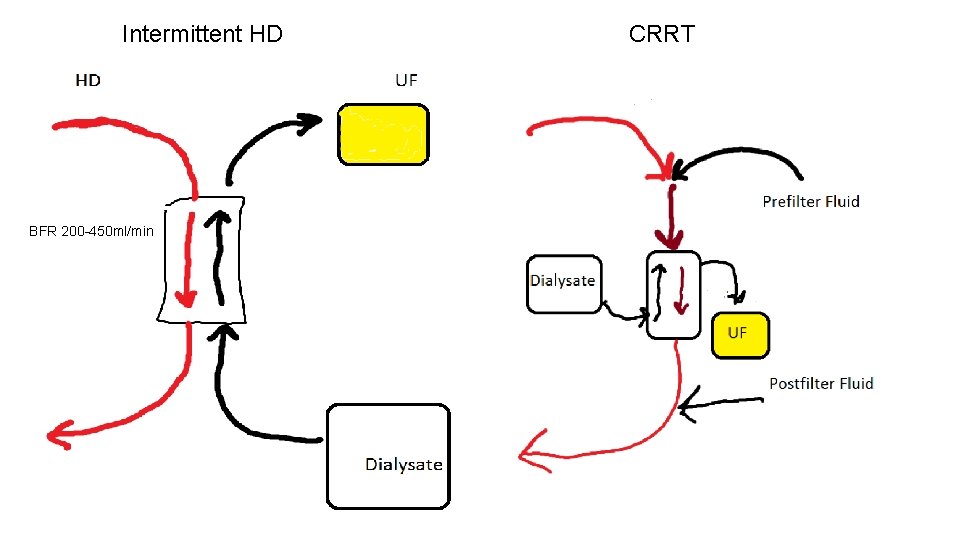
Types of Dialysis in the ICU Intermittent Hemodialysis ● 3 -4 hours, same amount of clearance as all day on CRRT. More hypotension ● Best for rapid correction of hyperkalemia/clearance. ● Issues with disequilibrium, potential rapid Na correction. ● Less time on, less time for clotting. Filter lasts 72 h or when clottted ● Can use fistula or catheter Continuous Renal Replacement Therapy ● Slower correction, less hemodynamic compromise. ● Can remove fluid more slowly and consistently which can net more UF ● Little risk of disequilibrium although there are some case studies ● More access issues, catheter only, clotting, can run heparin if able. ● Hypothermia (masks fevers) ● $$$, 1: 1 nursing. ● Indicated for ongoing breakdown (Rhabdo, hemolysis)

HD or CRRT? Ultimately: What is the UF you need to achieve the fluid balance goal? If you need to be even and intake is >4 L/day, you will have a hard time getting 4 L of UF in 4 hours on HD (watch your other sources of output). If you do not need volume removal and just clearance, most patients can do HD with increased pressor. There has never been a mortality difference between the two.

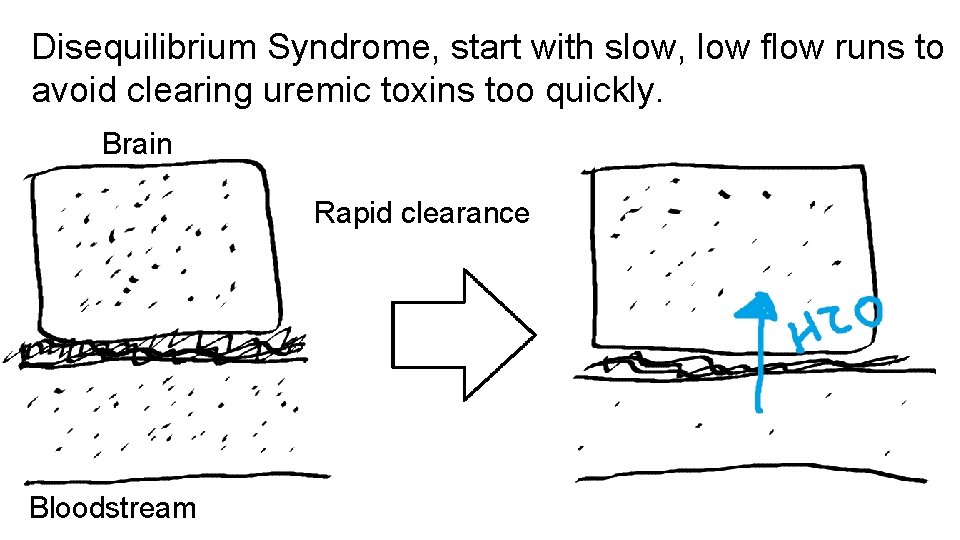
Disequilibrium Syndrome, start with slow, low flow runs to avoid clearing uremic toxins too quickly. Brain Rapid clearance Bloodstream

Intermittent HD BFR 200 -450 ml/min CRRT

Intermittent HD Prescription ● Needs catheter or fistula ● BFR=Blood flow rate. Usually 200 -400, directly relates to amount of clearance. ● UF ordered as total UF goal (independent of intake for patient) ● K 2, 3, or 4 (0 K is controversial) ● Na ~132 mmol/L=>~145 mmol/L ● Bicarb from 24 m. Eq/L up to ~40 m. Eq/L, patient still has to clear via lungs, if they have hypercapnia you can make it worse ○ H 2 O & CO 2 ⇔ H+ & HCO 3

CRRT Prescription ● Prefilter ○ 2 k/4 k ● Dialysate ○ 2/4 k ● Postfilter ○ Lots of options ■ 2 k/4 k ■ Bicarb ■ NS ■ D 5 ● Custom bags are a big ask from Pharmacy ○ Adding Na has been done, but is labor intensive. ● UF is ordered as overall goal (I=O, 50 cc/hr etc).

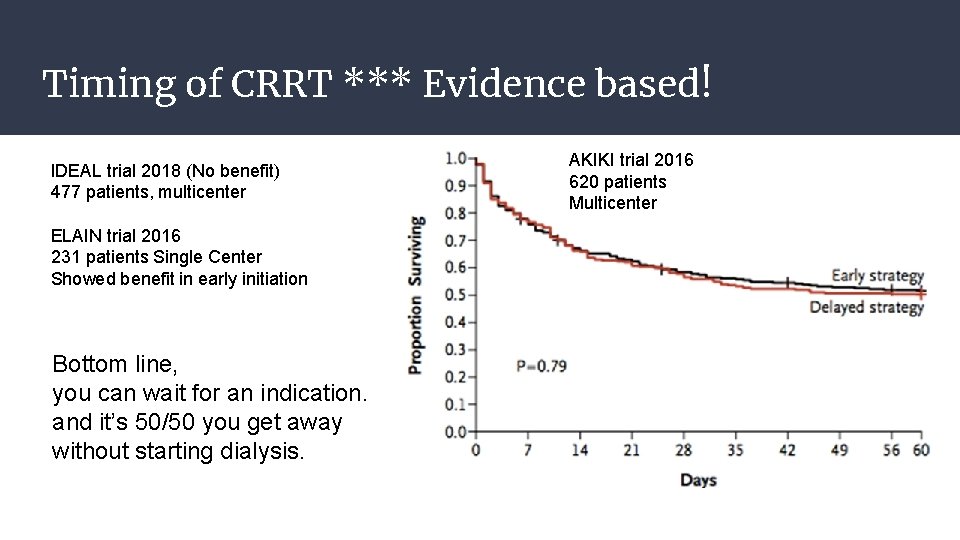
Timing of CRRT *** Evidence based! IDEAL trial 2018 (No benefit) 477 patients, multicenter ELAIN trial 2016 231 patients Single Center Showed benefit in early initiation Bottom line, you can wait for an indication. and it’s 50/50 you get away without starting dialysis. AKIKI trial 2016 620 patients Multicenter

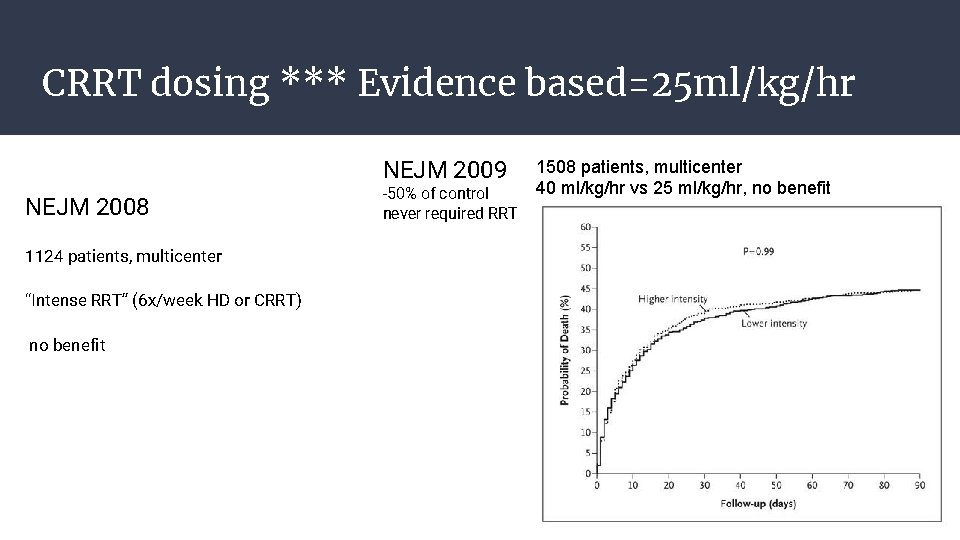
CRRT dosing *** Evidence based=25 ml/kg/hr NEJM 2009 NEJM 2008 1124 patients, multicenter “Intense RRT” (6 x/week HD or CRRT) no benefit -50% of control never required RRT 1508 patients, multicenter 40 ml/kg/hr vs 25 ml/kg/hr, no benefit

Troubleshooting RRT ● CRRT standard dose is 25 ml/kg/hr, but if K is still high, you can go up on your Rx. You will get more clearance from increasing the dialysate portion of your CRRT Rx. Where is it coming from? ● Consider recirculation issue if catheter is having issues and labs are not correcting. URR (Urea reduction ratio, drawn right before and right after intermittent HD) should be 60%. ● If your Na is >150 mmol/L, consider reducing dose to start, or (if CRRT) adding NS as post filter (Na of 154 mmol/L) to increase Na of CRRT Rx and slow correction of Na ● If there is frequent clotting and AC is not a good option, you can increase the prefilter portion of the Rx which will increase filter life but reduce clearance by ~15 -20%.

When can we change CRRT=>i. HD Sean’s Protocol ● Once off of pressors and UF goal is <4 L/day, go another 24 h on CRRT if filter lasts, don’t restart if it goes down/clots. ● Run i. HD the next day, short 2 hour run with enough UF to be even. ● If they do not do well on i. HD, we can go back to CRRT but being off promotes mobility and reduces resource utilization. ● When patients are getting off vent and mobilized, it’s time to try to get them off of CRRT. ● Goal is to get to 3 -4 x/week HD while monitoring for recovery with UOP and monitoring Cr on non-HD days.

Recovery! What to watch for. ● UOP is always the first sign (Not subtle, usually 500 cc or more) ● Cr rise will be less on non-HD days (jagged Cr line will trend downwards) ● The first thing kidneys will do will lose H 20 and K, watch for hypernatremia and correct with D 5 or free water via FT. If your patient is drinking water they will usually correct it on their own. High Na is a comfort/pain issue, unless neuro wants it high, correct it slowly (810 meq/24 h). ● One last equation. Free water deficit=0. 6 x weight (kg) x ((Current Sodium/142) - 1) ● Measure urine Na/K, if they add up to <~145, you’re losing water (it will usually be ~50 -75 in recovery, meaning you’re losing 1/2 NS)

Contrast Induced Nephropathy? ● Iodine based contrast does cause efferent vasoconstriction so historically has always been thought of as nephrotoxic ● Multiple recent trials have shown no difference in AKI’s between contrast and non-contrast CT’s in the ED (100, 000 patient meta-analysis involving 28 studies). ● Bottom line, it all depends on what you’re going to miss without contrast. The risk is low other than in kidneys recovering from AKI due to impaired autoregulation. ● ESRD-Go for it, you can’t hurt my kidneys any more. (**maybe not if they have residual UOP)

MRI contrast (Gadolinium) Can cause Nephrogenic systemic fibrosis ● ● Only occurs in renal failure, usually ESRD with inflammation at time of contrast. Delayed onset (weeks to months, sometimes years) Devastating disease, no major treatment options. Generally opposite risk profile of iodine based contrast

References "Initiation strategies for renal-replacement therapy in the intensive care unit". The New England Journal of Medicine. 2016. 375(2): 122 -133. “Risk of Acute Kidney Injury After Intravenous Contrast Media Administration” February 2017 Annals of Emergency Medicine Intensity of continuous renal-replacement therapy in critically ill patients N Engl J Med. 2009 Oct 22; 361(17): 1627 -38. doi: 10. 1056/NEJMoa 0902413. Initiation Strategies for Renal-Replacement Therapy in the Intensive Care Unit July 14, 2016 N Engl J Med 2016 Hemodialysis effect on platelet count and function and hemodialysis-associated thrombocytopenia Kidney International 82(2): 147 -57 · May 2012

References Intensity of Renal Support in Critically Ill Patients with Acute Kidney Injury N Engl J Med 2008; 359: 7 -20 DOI: 10. 1056/NEJMoa 0802639