Airway Management Techniques By Hwan Joo MD Airway

Airway Management Techniques By Hwan Joo MD

Airway Presentation § Normal Airway Management § Closed Claims § Difficult Intubation and Tools § Difficult Ventilation and Tools § Intubation tools for Surgeons § Overall goals § Teach surgeons about airway tools § Not necessarily how to intubate

Indication for Tracheal Intubation § Oxygenation and Peep § Ventilation § Airway protection from Aspiration § Tracheal toilet and/lung washings § Route for drug administration
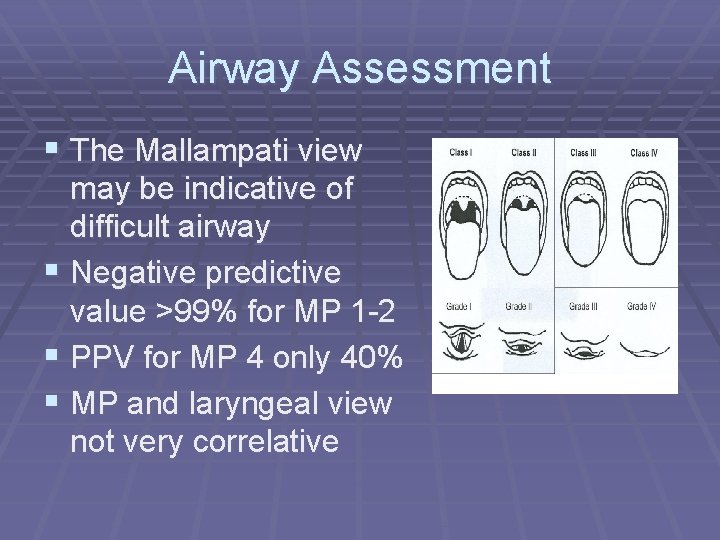
Airway Assessment § The Mallampati view may be indicative of difficult airway § Negative predictive value >99% for MP 1 -2 § PPV for MP 4 only 40% § MP and laryngeal view not very correlative

Difficult Airway Assessment § History of difficult Intubation § Physical examination § Trauma § C-spine precaution § Blood in airway § Airway trauma § Morbid obesity § RSI makes it worse!

Direct Laryngoscopy § 3# Mcintosh blade most § § § commonly used No change in design for 60 years High success rates in normal airways (99%) However, difficult to learn >50 uses to be proficient Not so good with difficult airways
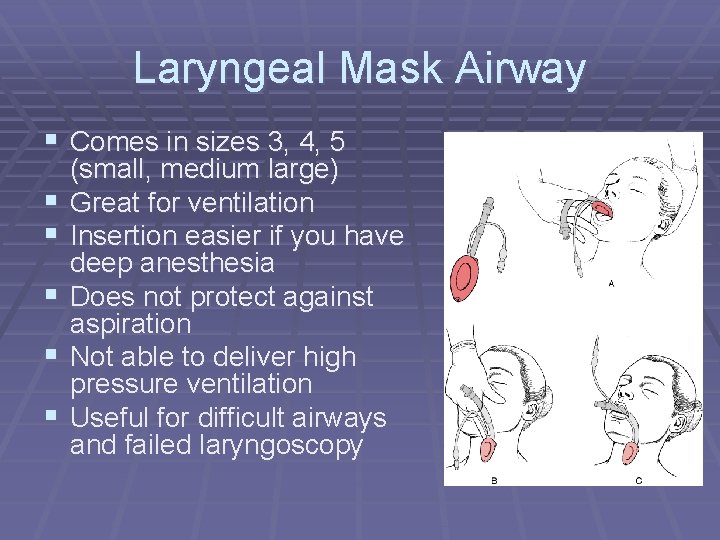
Laryngeal Mask Airway § Comes in sizes 3, 4, 5 § § § (small, medium large) Great for ventilation Insertion easier if you have deep anesthesia Does not protect against aspiration Not able to deliver high pressure ventilation Useful for difficult airways and failed laryngoscopy

Induction of for Intubation § Nothing § Patient already non-responsive § Medications contraindicated § Topical lidocaine § Midazolam, fentanyl § Etomidate±Sux § Ketamine±Sux § Propofol±Sux

Closed Claims -Caplan, Anesthesiology 1990 § Airway -Largest and most costly form of injury (34% of all claims, $200, 000+ US) § Inadequate ventilation (34%) § Esophageal intubation (18%) § Difficult intubation (17%) § 36% of claims against difficult intubation cases considered preventable

Closed Claims in Canada § Between 1993 -2003, 50% of all large CMPA suits in anesthesia were airway related § Average settlement was $500, 000 § 75% of patients suffered brain damage or deaths § 50% were associated with difficult airways § In half of these patients, difficult airway adjuncts were not used § Therefore, there is room for improvement

ASA Difficult Airway Algorithm § Recognized difficult airway § intubation vs non-intubation § facemask, LMA § regional § Unrecognized difficult airway § can ventilate § convert to spontaneous ventilation? § awake vs asleep § cannot ventilate § emergency measures required
Difficult Intubation -Ventilation Possible § Awaken patient § Asleep fiberoptic intubation § LMA without intubation § Intubation via LMA or ILMA § Lighted stylette § Combitube. TM § Video laryngoscope
Flexible Fiberoptic Intubation § Awake fiberoptic intubation is the gold (Rose CJA 1994) § Asleep FOI, successful but, § It may be more difficult due to § Airway obstruction or apnea § Blood in pharynx § Limited time before oxygen desaturation § Should be done with help!
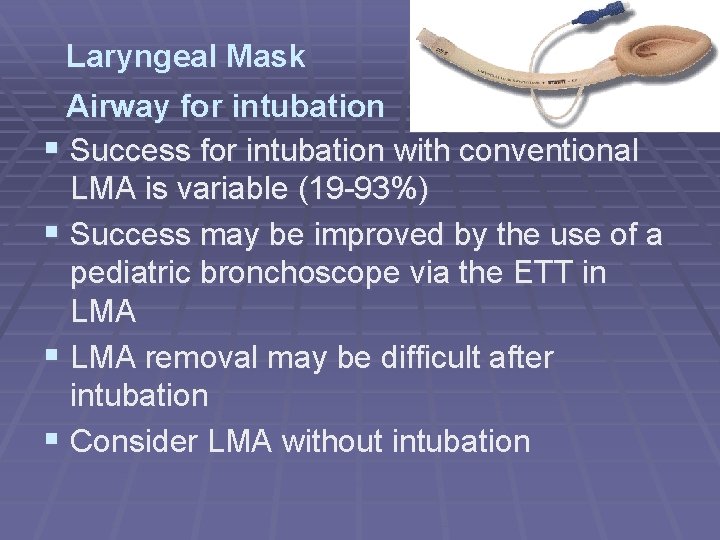
Laryngeal Mask Airway for intubation § Success for intubation with conventional LMA is variable (19 -93%) § Success may be improved by the use of a pediatric bronchoscope via the ETT in LMA § LMA removal may be difficult after intubation § Consider LMA without intubation

Lighted Stylette (Trachlite. TM) § With experience § Success rates reported to be up to 99% in patients with difficult airway (Hung, CJA 1995) § Success rates for novices 50% (Wilk, Resuc 1997) § Success rates decreased in patient with bull necks and obese patients
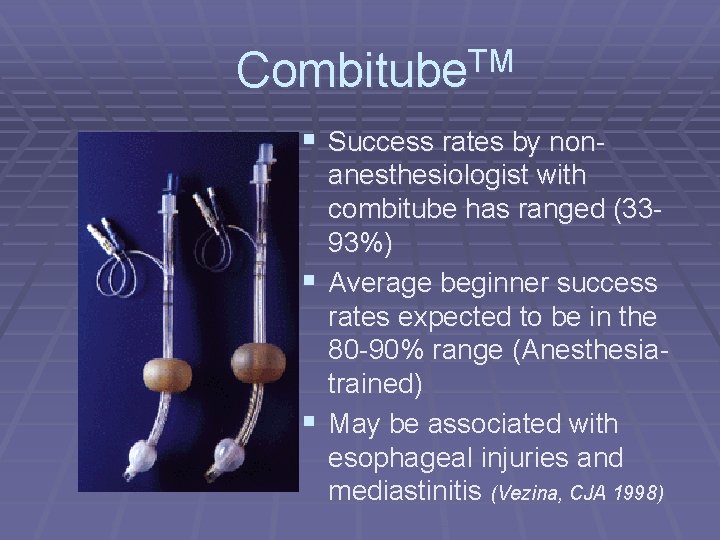
Combitube. TM § Success rates by nonanesthesiologist with combitube has ranged (3393%) § Average beginner success rates expected to be in the 80 -90% range (Anesthesiatrained) § May be associated with esophageal injuries and mediastinitis (Vezina, CJA 1998)

Video Laryngoscopes Glidescope § Rigid laryngoscope with CCD § View is very clear with no fogging § Blade angle 50 -60 deg § Easy to use § Very rapid learning curve § Can also be learned by ER physicians, Surgeons
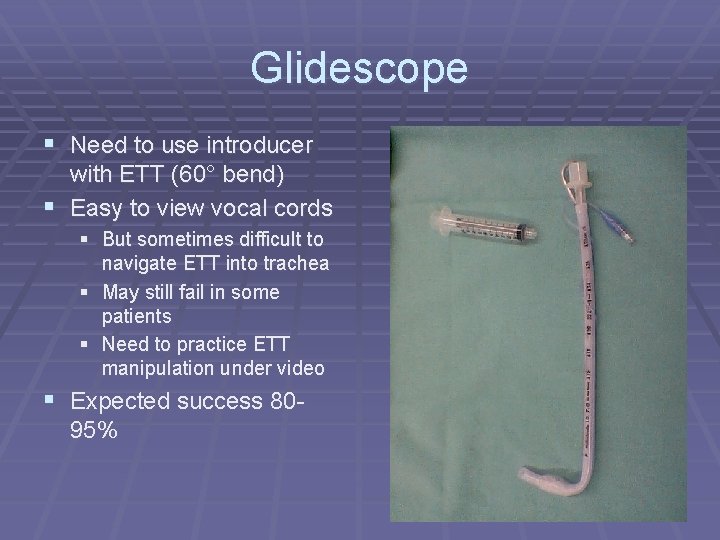
Glidescope § Need to use introducer with ETT (60° bend) § Easy to view vocal cords § But sometimes difficult to navigate ETT into trachea § May still fail in some patients § Need to practice ETT manipulation under video § Expected success 8095%
Glidescope in Use
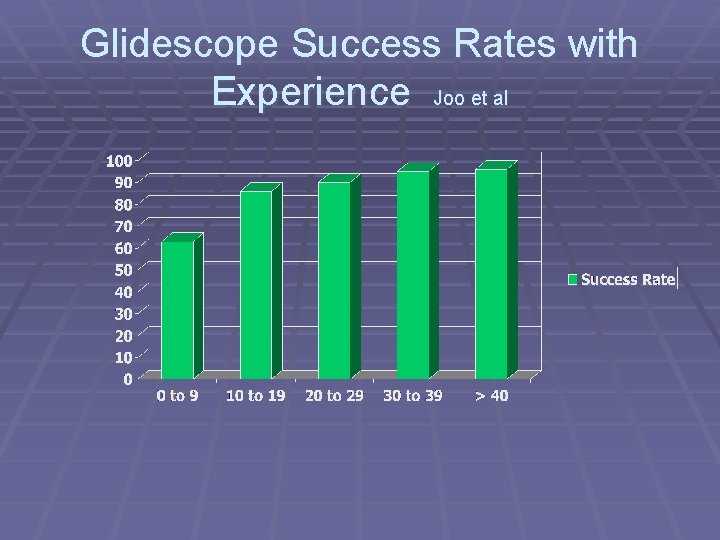
Glidescope Success Rates with Experience Joo et al

Glidescope with Disposable Blade

Mc. Grath Videolaryngoscope § § Similar to Glidescope Disposable blade cover Beautiful all in one design Optics not be as good § Narrow field of vision § More difficult? § More portable § More likely to disappear

Video Laryngoscopes RES-Q-SCOPE § § LCD Screen Disposable blade Much cheaper initial cost However, $50 per use
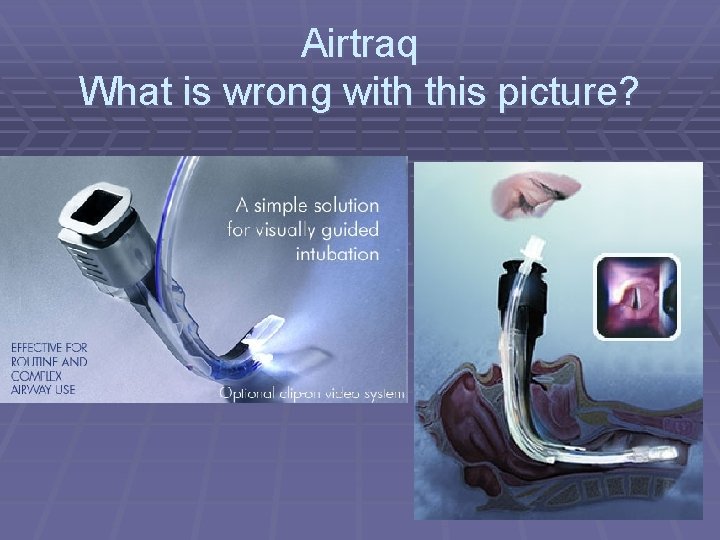
Airtraq What is wrong with this picture?

Ventilation Difficult or Impossible § Failed intubation is disturbing but…. . § Failed ventilation is universally fatal! § Choices § LMA (will discuss ILMA later) § Combitube § Transtracheal airway § cricothryotomy § transtracheal jet ventilation § tracheostomy

Laryngeal Mask Airway § Success rates for ventilation as high as § 95% after 1 attempt and 98% after 2 attempts § No decrease in success rates in patient’s with difficult airways § Overwhelming data of uses in difficult airways and in failed ventilation § may have saved 100’s of lives! § For IPPV use large LMA’s

What is the Best Device for Failed Ventilation? LMA vs. Combitube. TM § Success is dependent on more on the operator’s experience than to tool § Majority of anesthesiologist have little or no experience with the Combitube § LMA should be the first choice for difficult ventilation scenarios § However, Combitube theoretically prevents aspiration
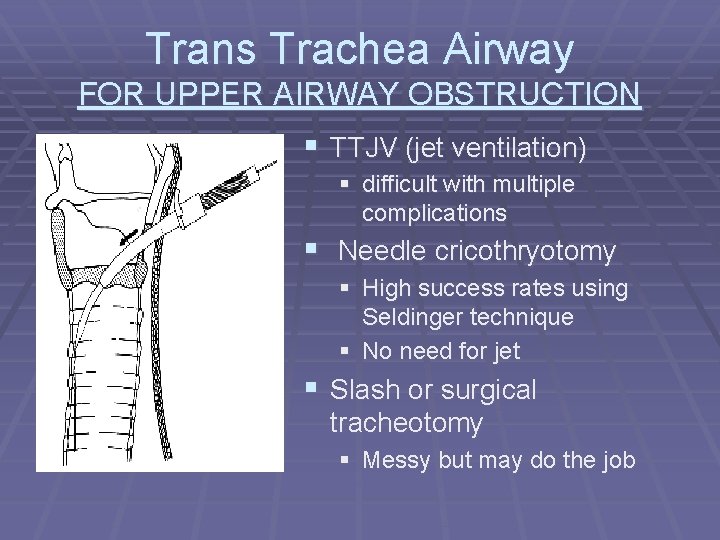
Trans Trachea Airway FOR UPPER AIRWAY OBSTRUCTION § TTJV (jet ventilation) § difficult with multiple complications § Needle cricothryotomy § High success rates using Seldinger technique § No need for jet § Slash or surgical tracheotomy § Messy but may do the job
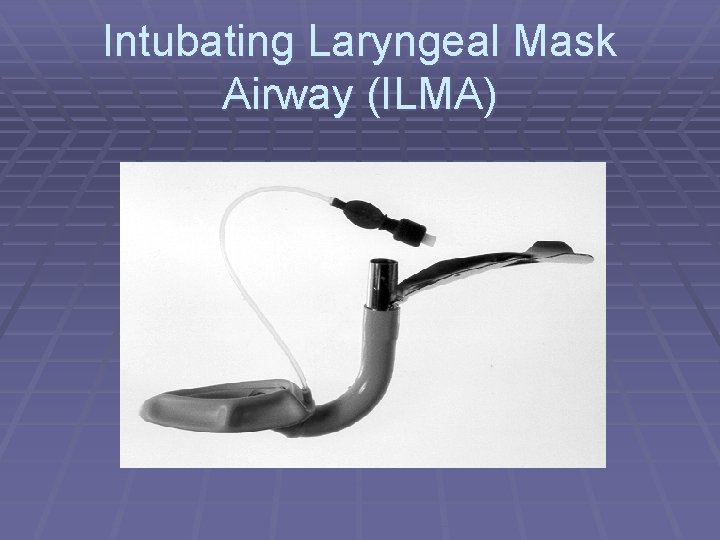
Intubating Laryngeal Mask Airway (ILMA)
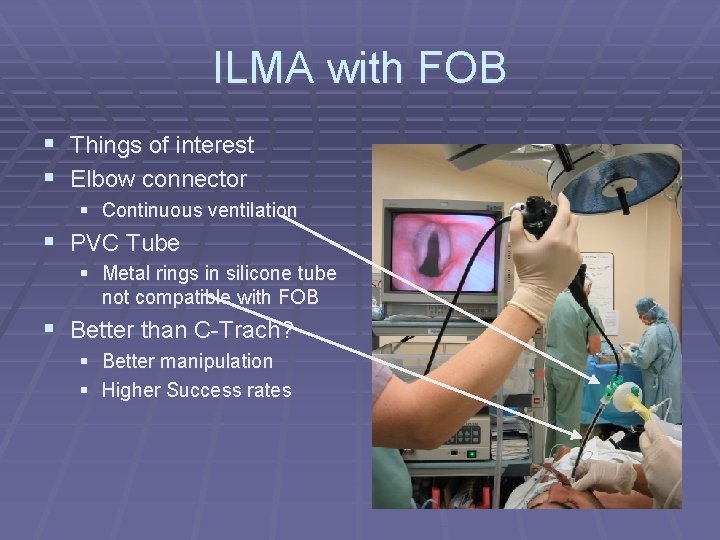
ILMA with FOB § Things of interest § Elbow connector § Continuous ventilation § PVC Tube § Metal rings in silicone tube not compatible with FOB § Better than C-Trach? § Better manipulation § Higher Success rates
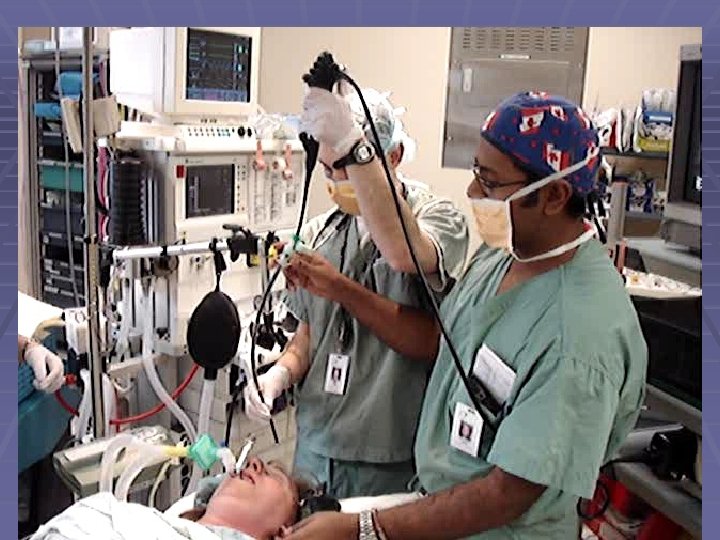
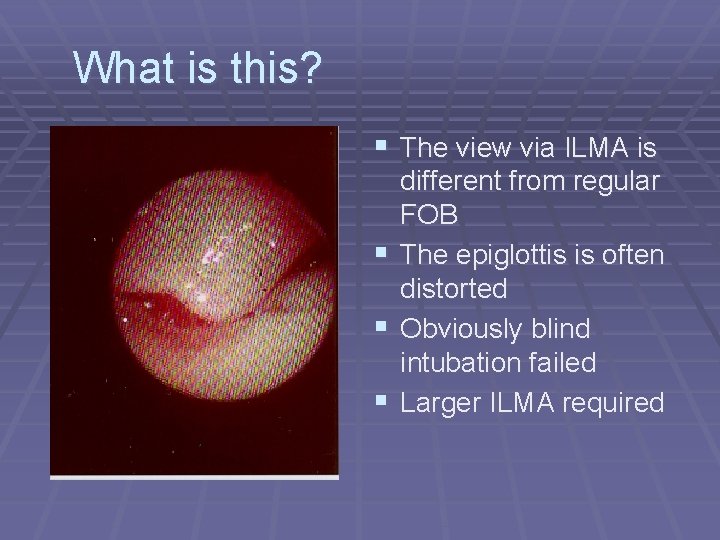
What is this? § The view via ILMA is different from regular FOB § The epiglottis is often distorted § Obviously blind intubation failed § Larger ILMA required

LMA C Trach § ILMA with LCD screen § Improved success rates for intubation over ILMA § Success on normal airways about 90 -95% based on limited studies § However, need greater mouth opening compared to ILMA, 2. 5 cm versus 2. 0 cm § Same success rate for ventilation § Less trauma
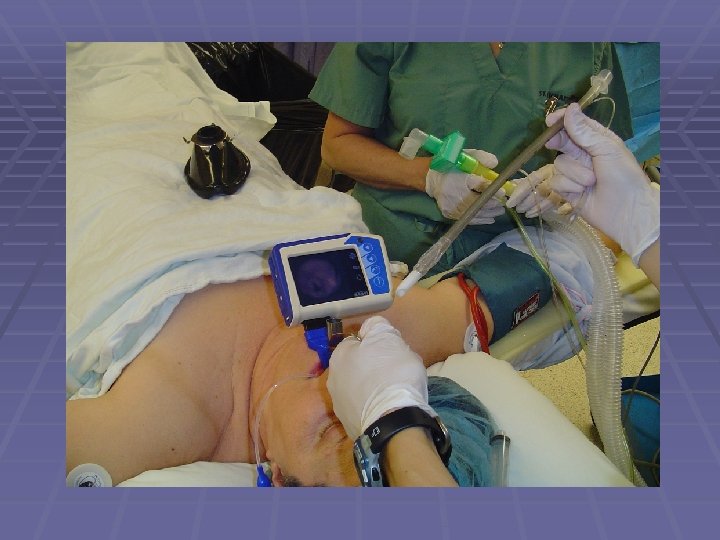

Failed Intubation What to do as a Surgeon § Awaken patient if possible/feasible § Maintain ventilation and oxygenation § Facemask § LMA § Combitube § Call Anesthesia § Surgical Airway § Attempt ventilation throughout

Airway Tools not for Surgeons § FOB § Too much effort required to learn § Hard to maintain in ER – expensive! § Not as useful in unplanned cases (ER) § Lighted Stylettes § Again, high learning curve § Not as useful in patients who are not paralyzed § High incidence of esophageal intubations

What is the Best Tool for Surgeons? § LCD Laryngoscopes are the way of the future § Currently, Glidescope is the easiest to use with the most literature supporting it § Must Practice on routine patients § Use it get familiarity § Bug the anesthesiologists to use it in the OR § Cost of acquisition about $6000 with $2030/use for disposable blade
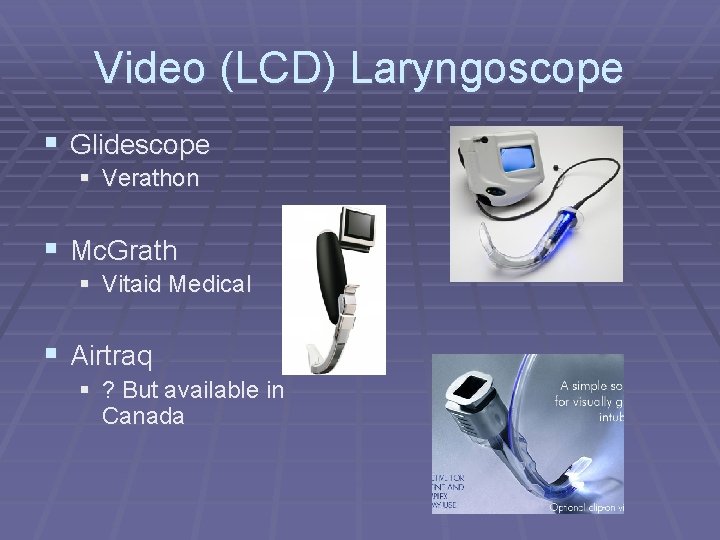
Video (LCD) Laryngoscope § Glidescope § Verathon § Mc. Grath § Vitaid Medical § Airtraq § ? But available in Canada
The Future The future of intubation will be video assisted § In the past, intubators intubated in the dark by themselves § PRIVATE (MASTURBATION!) § The future will have everybody involved in the process of intubation § (ER Doc, Nurses, RT) § PARTY! § Everyone is involved

Final Recommendation § When faced with a difficult airway, stay on the beaten path of § Practice, Practice… § Use familiar but advanced devices § Do not persist with techniques that have failed § Secure ventilation
- Slides: 40