Airway Management Part 2 Prof M H MUMTAZ

































































- Slides: 90

Airway Management: Part 2 Prof. M. H. MUMTAZ

Risks/Protective Measures z. Be prepared for: y. Coughing y. Spitting y. Vomiting y. Biting z. Body Substance Isolation y. Gloves y. Face, eye shields y. Respirator, if concern for airborne disease

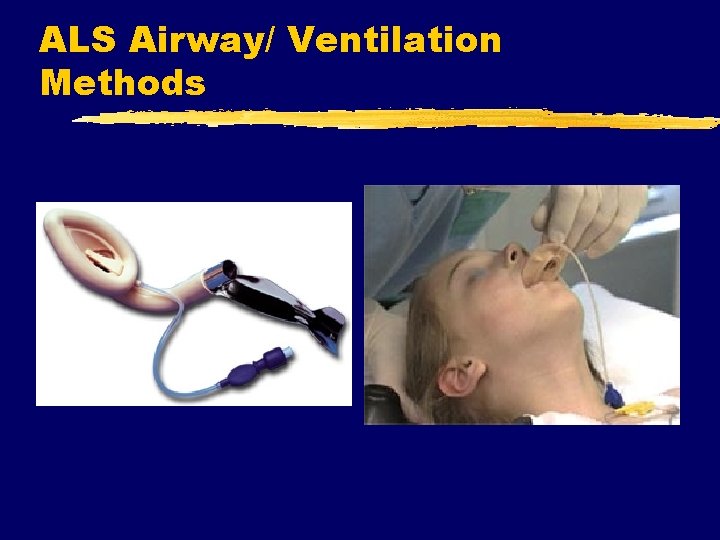
ALS Airway/Ventilation Methods z. Gastric Tubes y. Nasogastric x. Caution with esophageal disease or facial trauma x. Tolerated by awake patients, but uncomfortable x. Patient can speak x. Interferes with BVM seal y. Orogastric x. Usually used in unresponsive patients x. Larger tube may be used x. Safe in facial trauma

ALS Airway/Ventilation Methods z. Nasogastric Tube Insertion y. Select size (French) y. Measure length (nose to ear to xiphoid) y. Lubricate end of tube (water soluble) y. Maintain aseptic technique y. Position patient sitting up if possible

ALS Airway/Ventilation Methods z. Nasogastric Tube Insertion y. Insert into nare towards angle of jaw y. Advance gradually to measured length y. Have patient swallow y. Assess placement x. Instill air, ausculate xaspirate gastric contents y. Secure y. May connect to low vacuum (80 -100 mm Hg)

ALS Airway/Ventilation Methods z. Orogastric Tube Insertion y. Select size (French) y. Measure length y. Lubricate end of tube y. Position patient (usually supine) y. Insert into mouth y. Advance gradually but steadily y. Assess placement (instill air or aspirate) y. Secure y. Evacuate contents as needed

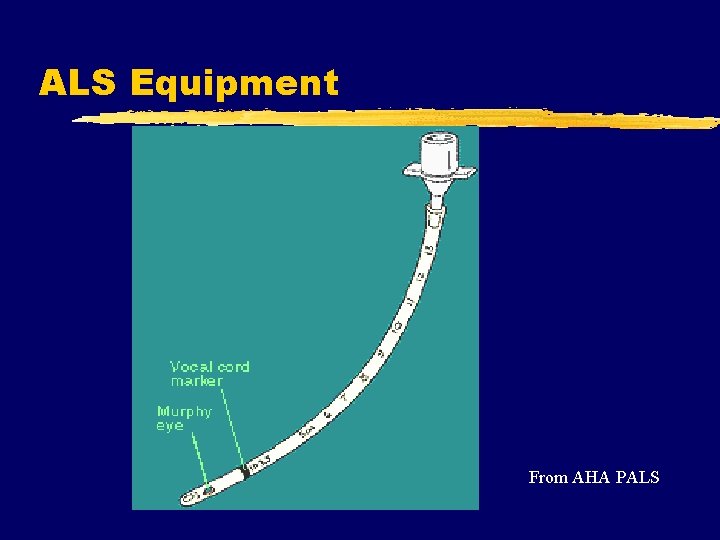
ET Introduction z. Endotracheal Intubation y. Tube into trachea to provide ventilations using BVM or ventilator y. Sized based upon inside diameter (ID) in mm y. Lengths increase with increased ID (cm markings along length) y. Cuffed vs. Uncuffed

Endotracheal Intubation z. Advantages y. Secures airway y. Route for a few medications (LANE) y. Optimizes ventilation, oxygenation y. Allows suctioning of lower airway

Endotracheal Intubation z. Indications y. Present or impending respiratory failure y. Apnea y. Unable to protect own airway

Endotracheal Intubation z. These are NOT Indications y. Because I can intubate y. Because they are unresponsive y. Because I can’t show up at the hospital without it

Endotracheal Intubation z Complications y. Soft tissue trauma/bleeding y. Dental injury y. Laryngeal edema y. Laryngospasm y. Vocal cord injury y. Barotrauma y. Hypoxia y. Aspiration y. Esophageal intubation y. Mainstem bronchus intubation

Endotracheal Intubation z. Insertion Techniques y. Orotracheal Intubation (Direct Laryngoscopy) y. Blind Nasotracheal Intubation y. Digital Intubation y. Retrograde Intubation y. Transillumination

Orotracheal Intubation z. Technique y. Position, ventilate patient y. Monitor patient x. ECG x. Pulse oximeter y. Assess patient’s airway for difficulty y. Assemble, check equipment (suction) y. Hyperventilate patient (30 -120 sec)

ALS Airway/Ventilation Methods z. Orotracheal Intubation y. Position patient y. Open mouth y. Insert laryngoscope blade on right side y. Sweep tongue to left y. Identify anatomical landmarks y. Advance laryngoscope blade x. Vallecula for curved (Miller) blade x. Under epiglottis for straight (Miller) blade

ALS Airway/Ventilation Methods z. Orotracheal Intubation y. Elevate epiglottis y. Directly with straight (Miller) blade y. Indirectly with curved (Macintosh) blade y. Visualize vocal cords, glottic opening y. Enter mouth with tube from corner of mouth

ALS Airway/Ventilation Methods z. Orotracheal Intubation y. Advance tube into glottic opening about 1/2 inch past vocal cords y. Continue to hold tube, note location y. Ventilate, ausculate x. Epigastrium x. Left and right chest y. Inflate cuff until air leak around cuff stops y. Reassess tube placement

ALS Airway/Ventilation Methods z. Orotracheal Intubation y. Secure tube y. Reassess tube placement, ventilation effectiveness

Intubation Total time between ventilations should not exceed 30 seconds!

Intubation Death occurs from failure to Ventilate, not failure to Intubate

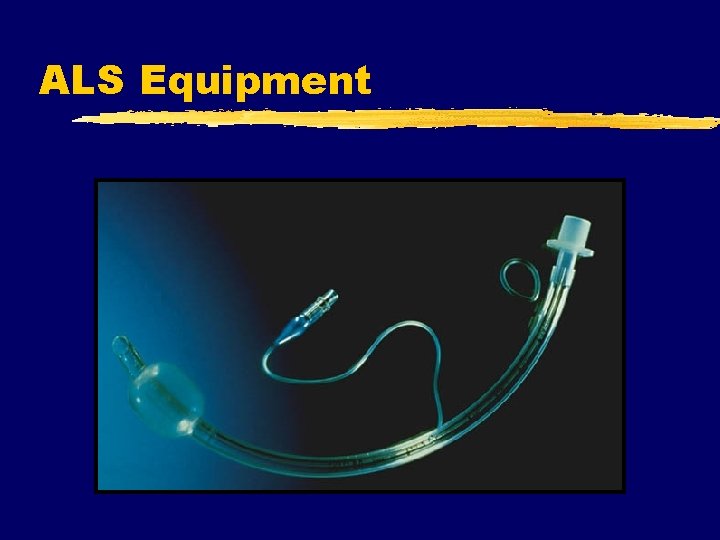
ALS Equipment z Equipment y. Laryngoscope Handle (lighted) & Blades y. Stylet y. Syringe y. Magills y. Lubricant y. Suction y. BVM y. BAAM (Blind Nasal) z Selection y. Typical Adult ET Tube Sizes x. Male - 8. 0, 8. 5 x. Female - 7. 0, 7. 5, 8. 0 y. Blade x. Mac - 3 or 4 x. Miller - 3 y. Tube Depth x. Usually 20 - 22 cm at the teeth

ALS Equipment

ALS Equipment From AHA PALS

ALS Equipment

Pediatric ET Intubation z Pediatric Equipment Differences y. Uncuffed tube < 8 yoa y. Miller blade preferred y. Tube Size x. Premie: 2. 0, 2. 5 x. Newborn: 3. 0, 3. 5 x 1 year: 4 x. Then: (age/4)+4 z Pediatric Differences y. Anatomic Differences y. Depth (cm) x. Tube ID x 3 x 12 + (age/2) xeasily dislodged y. Intubation vs BVM

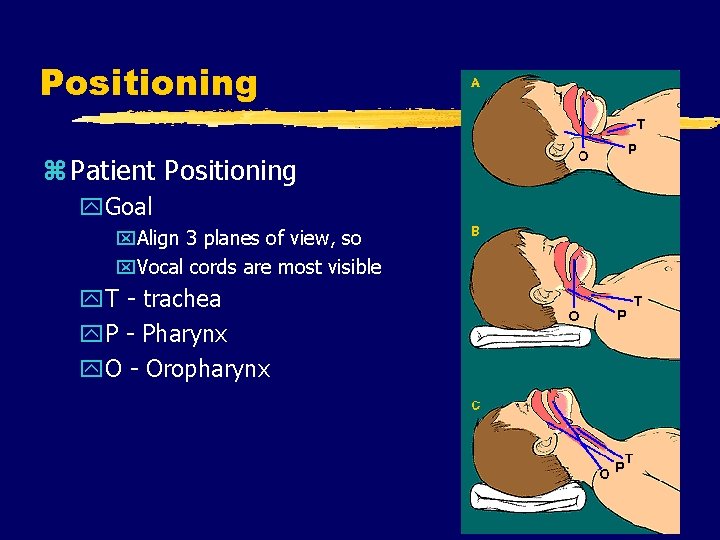
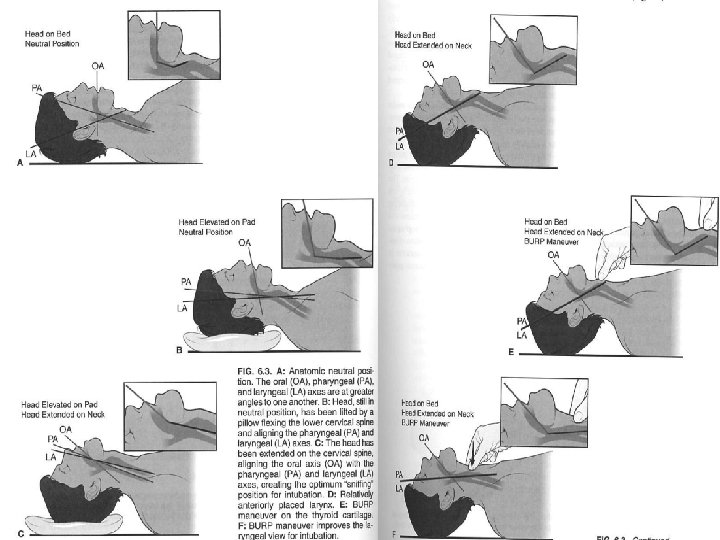
Positioning z Patient Positioning y. Goal x. Align 3 planes of view, so x. Vocal cords are most visible y. T - trachea y. P - Pharynx y. O - Oropharynx


Airway Assessment z. Cervical Spine z. Temporal Mandibular Joint z. A/O Joint z. Neck length, size and muscularity z. Mandibular size in relation to face z. Over bite z. Tongue size

Assessment Acronym z. M z. O z. U z. T z. H z. S Mandible Opening Uvula Teeth Head Silhouette

The Lemon Law z. L z. E z. M z. O z. N Look externally Evaluate the 3 -3 -2 rule Mallampati score Obstruction? Neck Mobility

Look z. Morbidly obese z. Facial hair z. Narrow face z. Overbite z. Trauma

Evaluate 3 -3 -2 z. Temporal Mandibular Joint y. Should allow 3 fingers between incisors y 3 -4 cm

Evaluate 3 -3 -2 z. Mandible y 3 fingers between mentum & hyoid bone y. Less than three fingers x. Proportionately large tongue x. Obstructs visualization of glottic opening y. Greater than three fingers x. Elongates oral axis x. More difficult to align the three axis

Evaluate 3 -3 -2 z. Larynx y. Adult located C 5, 6 y. If higher, obstructive view of glottic opening y. Two fingers from floor of mouth to thyroid cartilage

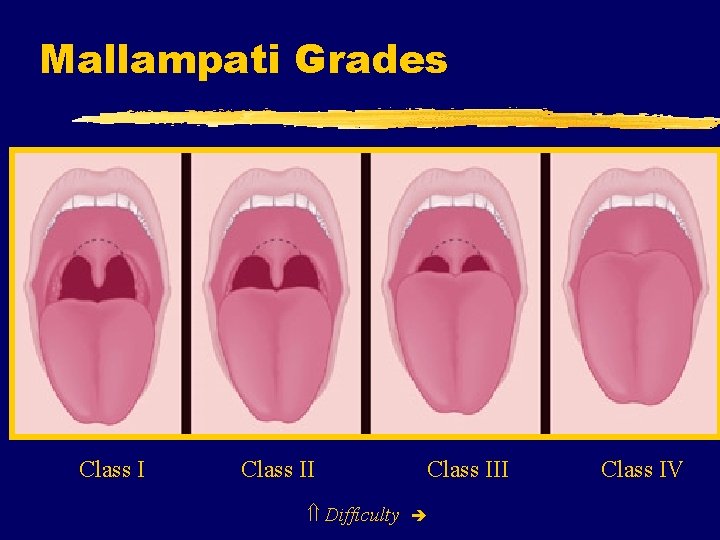
Mallampati Score z. Evaluates ability to visualize glottic opening y. Patient seated with neck extended y. Open mouth as wide as possible y. Protrude tongue as far as possible y. Look at posterior pharynx y. Grade based on visual field x. Grades 1, 2 have low intubation failure rates x. Grades 3, 4 have higher intubation failure rates

Mallampati Score z. Not useful in emergent situations z. Informal version y. Use tongue blade to visualize pharynx


Mallampati Grades Class II Difficulty Class III Class IV

Obstruction z. Know or suspected y. Foreign bodies y. Tumors y. Abscess y. Epiglottitis y. Hematoma y. Trauma

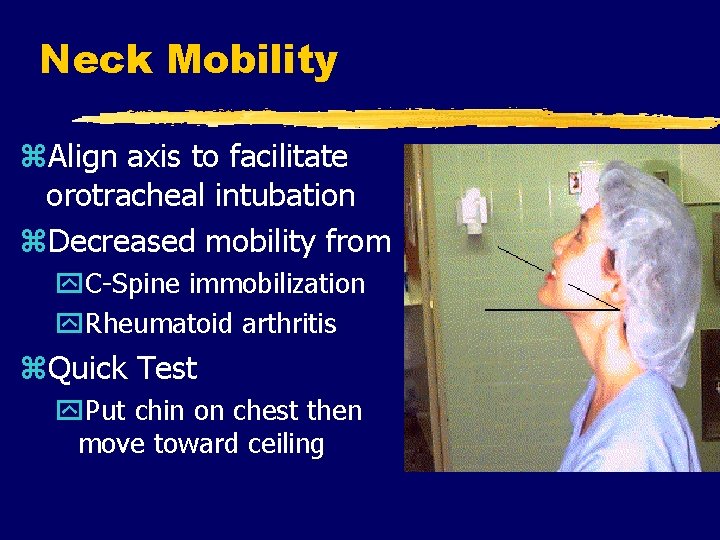
Neck Mobility z. Align axis to facilitate orotracheal intubation z. Decreased mobility from y. C-Spine immobilization y. Rheumatoid arthritis z. Quick Test y. Put chin on chest then move toward ceiling

Curved Blade (Macintosh) z Insert from right to left z Visualize anatomy z Blade in vallecula z Lift up and away DO NOT PRY ON TEETH z Lift epiglottis indirectly From AHA ACLS

Straight Blade (Miller) z Insert from right to left z Visualize anatomy z Blade past vallecula and over epiglottis z Lift up and away DO NOT PRY ON TEETH z Lift epiglottis directly From AHA ACLS

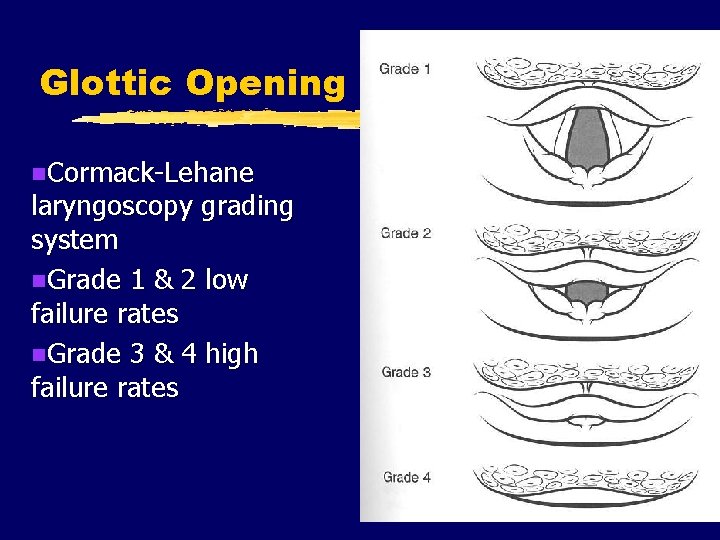
Glottic Opening n. Cormack-Lehane laryngoscopy grading system n. Grade 1 & 2 low failure rates n. Grade 3 & 4 high failure rates

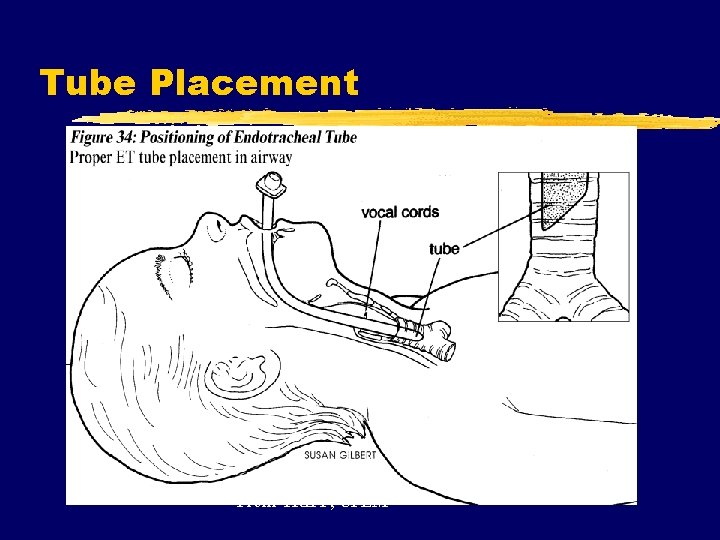
Tube Placement From TRIPP, CPEM

Confirmation of Placement

Placement of the ETT within the esophagus is an accepted complication. However, failure to recognize and correct is not!

Traditional Methods z. Observation of ETT passing through vocal cords. z. Presence of breath sounds z. Absence of epigastric sounds z. Symmetric rise and fall of chest z. Condensation in ETT z. Chest Radiograph

All of these methods have failed in the clinical setting

Additional Methods z. Pulse Oximetry z. Aspiration Techniques z. End Tidal CO 2

Confirming ETT Location z. Fail Safe z. Near Fail Safe z. Non-Fail Safe

Fail Safe z. Improvement in Clinical Signs z. ETT visualized between vocal cords z. Fiberoptic visualization of y. Cartilaginous rings y. Carina

Near Failsafe z. CO 2 detection z. Rapid inflation of EDD

Non-Failsafe z. Presence of breath sounds z. Absence of epigastric sounds z. Absence of gastric distention z. Chest Rise and Fall z. Large Spontaneous Exhaled Tidal Volumes

Non Failsafe z. Condensation in tube disappearing and reappearing with respiration z. Air exiting tube with chest compression z. Bag Valve Mask having the appropriate compliance z. Pressure on suprasternal notch associated with pilot balloon pressure

ALS Airway/Ventilation Methods z. Blind Nasotracheal Intubation y. Position, oxygenate patient y. Monitor patient x. ECG monitor x. Pulse oximeter

ALS Airway/Ventilation Methods z. Blind Nasotracheal Intubation y. Assess for difficulty or contraindication x. Mid-face fractures x. Possible basilar skull fracture x. Evidence of nasal obstruction, septal deviation y. Assemble, check equipment x. Lubricate end of tube; do not warm x. Attach BAAM (if available)

ALS Airway/Ventilation Methods z. Blind Nasotracheal Intubation y. Position patient (preferably sitting upright) y. Insert tube into largest nare y. Advance slowly, but steadily y. Listen for sound of air movement in tube or whistle via BAAM y. Advance tube y. Assess placement y. Inflate cuff, reassess placement y. Secure, reassess placement

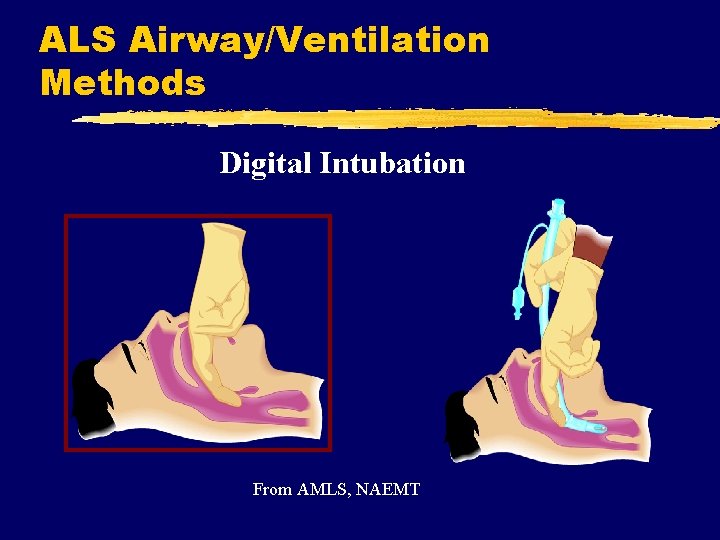
ALS Airway/Ventilation Methods z. Digital Intubation y. Blind technique y. Variable probability of success y. Using middle finger to locate epiglottis y. Lift epiglottis y. Slide lubricated tube along index finger y. Assess tube placement/depth as with orotracheal intubation

ALS Airway/Ventilation Methods Digital Intubation From AMLS, NAEMT

ALS Airway Ventilation Methods z. Surgical Cricothyrotomy y. Indications x. Absolute need for definitive airway, AND • unable to perform ETT due for structural or anatomic reasons, AND • risk of not securing airway is > than surgical airway risk x. OR x. Absolute need for definitive airway AND • unable to clear an upper airway obstruction, AND • multiple unsuccessful attempts at ETT, AND • other methods of ventilation do not allow for effective ventilation, respiration

ALS Airway/Ventilation Methods z. Surgical Cricothyrotomy y. Contraindications (relative) x. No real demonstrated indication x. Risks > Benefits x. Age < 8 years (some say 10, some say 12) x. Evidence of fractured larynx or cricoid cartilage x. Evidence of tracheal transection

ALS Airway/Ventilation Methods z. Surgical Cricothyrotomy y. Tips x. Know anatomy x. Short incision, avoid inferior trachea x. Incise, do not saw x. Work quickly x. Nothing comes out until something else is in x. Have a plan x. Be prepared with backup plan

ALS Airway/Ventilation Methods z. Needle Cricothyrotomy/Transtracheal Jet Ventilation y. Indications x. Same as surgical cricothyrotomy with x. Contraindication for surgical cricothyrotomy y. Contraindications x. None when demonstrated need x. Caution with tracheal transection

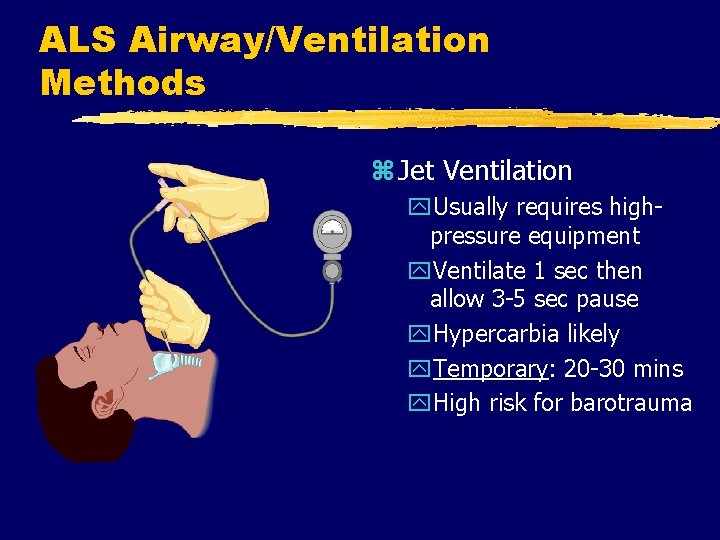
ALS Airway/Ventilation Methods z Jet Ventilation y. Usually requires highpressure equipment y. Ventilate 1 sec then allow 3 -5 sec pause y. Hypercarbia likely y. Temporary: 20 -30 mins y. High risk for barotrauma

ALS Airway/ Ventilation Methods z. Alternative Airways y. Multi-Lumen Devices (Combi. Tube, PTLA) y. Laryngeal Mask Airway (LMA) y. Esophageal Obturator Airways (EOA, EGTA) y. Lighted Stylets

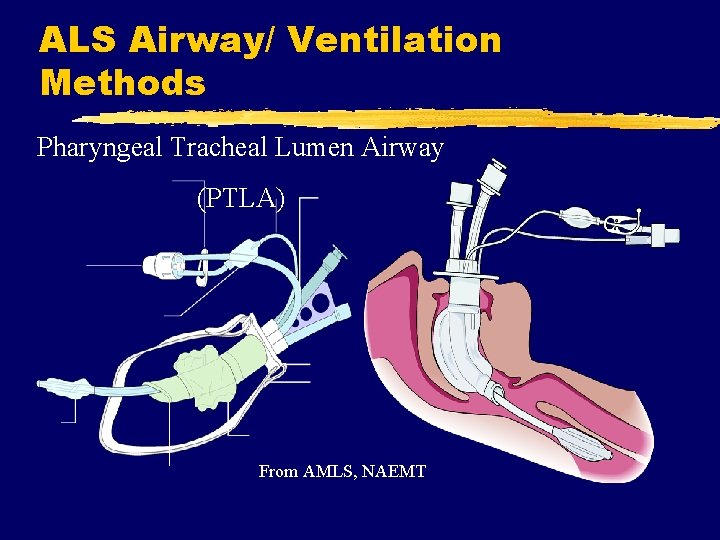
ALS Airway/ Ventilation Methods Pharyngeal Tracheal Lumen Airway (PTLA) From AMLS, NAEMT

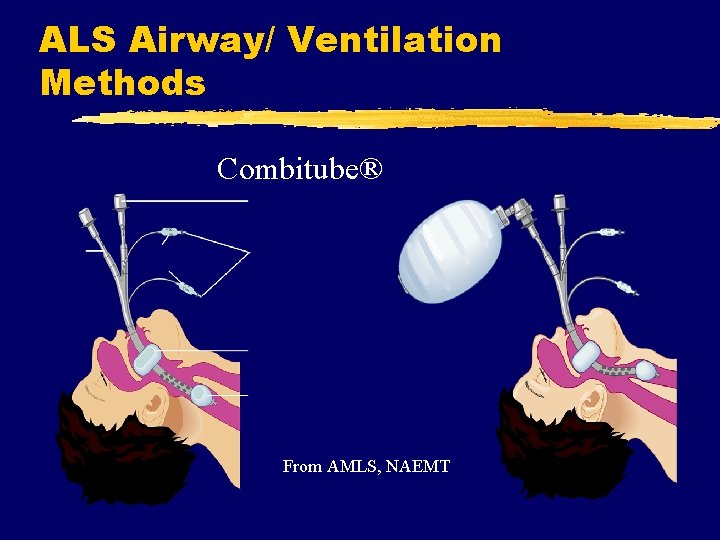
ALS Airway/ Ventilation Methods Combitube® From AMLS, NAEMT

ALS Airway/ Ventilation Methods z. Combitube® y. Indications y. Contraindications x. Height x. Gag reflex x. Ingestion of corrosive or volatile substances x. Hx of esophageal disease

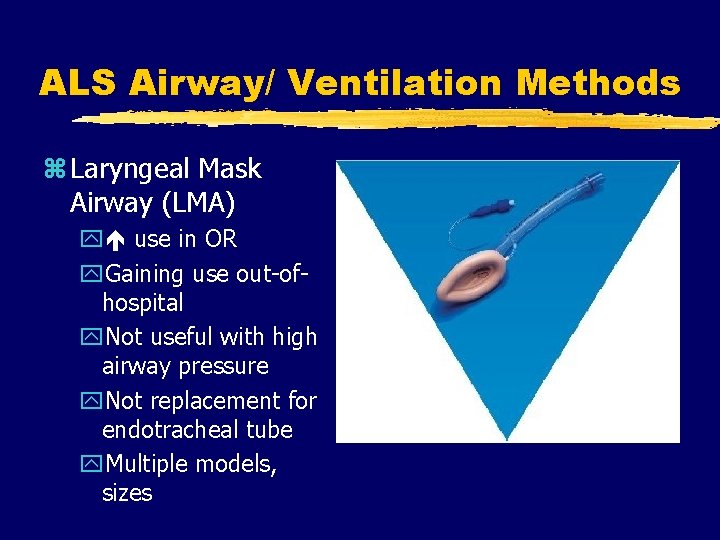
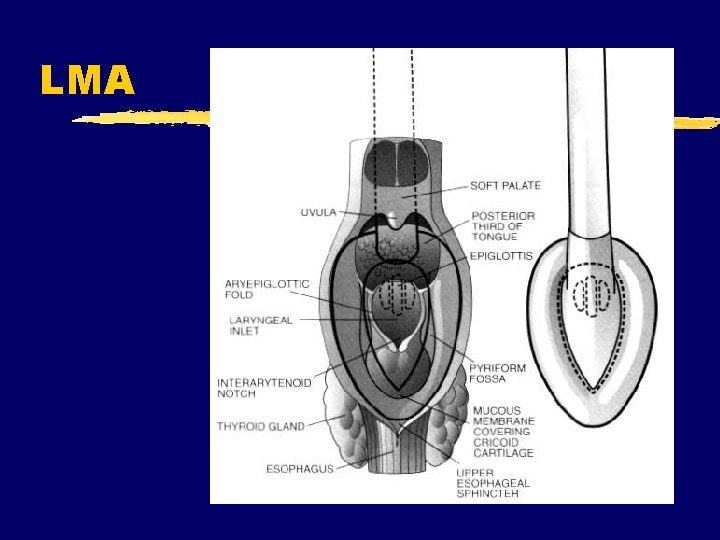
ALS Airway/ Ventilation Methods z Laryngeal Mask Airway (LMA) y use in OR y. Gaining use out-ofhospital y. Not useful with high airway pressure y. Not replacement for endotracheal tube y. Multiple models, sizes

LMA

ALS Airway/ Ventilation Methods

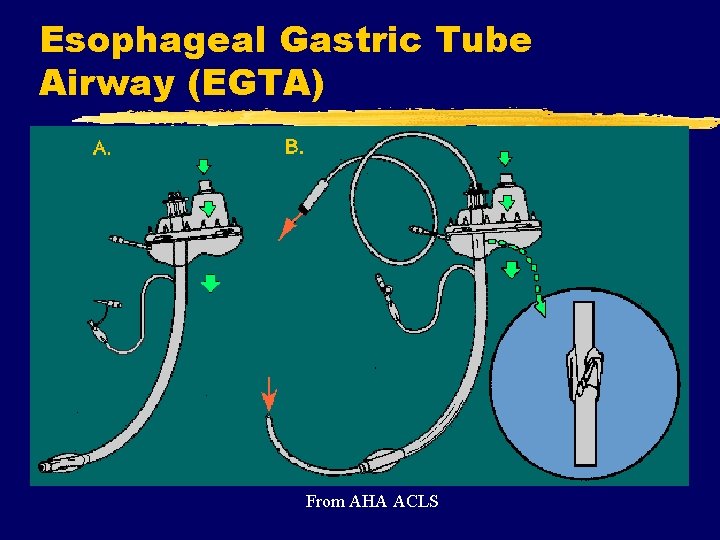
BLS & ALS Airway/ Ventilation Methods z. Esophageal Obturator Airway, Esophageal Gastric Tube Airway y. Used less frequently today y. Increased complication rate y. Significant contraindications x. Patient height x. Caustic ingestion x. Esophageal/liver disease y. Better alternative airways are now available

Esophageal Gastric Tube Airway (EGTA) From AHA ACLS

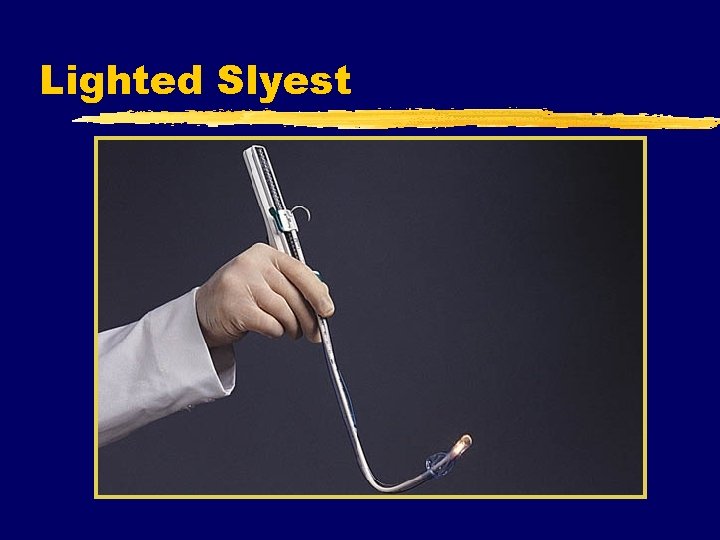
ALS Airway/ Ventilation Methods z. Lighted Stylette y. Not yet widely used y. Expensive y. Another method of visual feedback about placement in trachea

Lighted Slyest

ALS Airway/Ventilation Methods

Pharmacologic Assisted Intubation “RSI” z Sedation y. Reduce anxiety y. Induce amnesia y. Depress gag reflex, spontaneous breathing y. Used for xinduction xanxious, agitated patient y. Contraindications xhypersensitivity xhypotension

Pharmacologic Assisted Intubation “RSI” z. Common Medications for Sedation y. Benzodiazepines (diazepam, midazolam) y. Narcotics (fentanyl) y. Anesthesia Induction Agents x. Etomidate x. Ketamine x. Propofol (Diprivan®)

Pharmacologic Assisted Intubation z. Neuromuscular Blockade y. Temporary skeletal muscle paralysis y. Indications x. When intubation required in patient who: • is awake, • has gag reflex, or • is agitated, combative

Pharmacologic Assisted Intubation z. Neuromuscular Blockade y. Contraindications x. Most are specific to medication x. Inability to ventilate once paralysis induced y. Advantages x. Enables provider to intubate patients who otherwise would be difficult, impossible to intubate x. Minimizes patient resistance to intubation x. Reduces risk of laryngospasm

Pharmacologic Assisted Intubation z NMB Agent Mechanism of Action y. Acts at neuromuscular junction where ACh normally allows nerve impulse transmission y. Binds to nicotinic receptor sites on skeletal muscle y. Depolarizing or non-depolarizing y. Blocks further action by ACh at receptor sites y. Blocks further depolarization resulting in muscular paralysis

Pharmacologic Assisted Intubation z. Disadvantages/Potential Complications y. Does not provide sedation, amnesia y. Provider unable to intubate, ventilate after NMB y. Aspiration during procedure y. Difficult to detect motor seizure activity y. Side effects, adverse effects of specific drugs

Pharmacologic Assisted Intubation z. Common Used NMB Agents y. Depolarizing NMB agents xsuccinylcholine (Anectine®) y. Non-depolarizing NMB agents xvecuronium (Norcuron®) xrocuronium (Zemuron®) xpancuronium (Pavulon®)

Pharmacologic Assisted Intubation y. Summarized Procedure x. Prepare all equipment, medications while ventilating patient x. Hyperventilate x Administer induction/sedation agents and pretreatment meds (e. g. lidocaine or atropine) x. Administer NMB agent x. Sellick maneuver x. Intubate per usual x. Continue NMB and sedation/analgesia prn

Pharmacologic Assisted Intubation Failure is not an option!

ALS Airway/Ventilation Methods z. Needle Thoracostomy y. Indications x. Positive signs/symptoms of tension pneumothorax x. Cardiac arrest with PEA or asystole with possible tension pneumothorax y. Contraindications x. Absence of indications

ALS Airway/Ventilation Methods z. Tension Pneumothorax Signs/Symptoms y. Severe respiratory distress y or absent lung sounds (usually unilateral) y resistance to manual ventilation y. Cardiovascular collapse (shock) y. Asymmetric chest expansion y. Anxiety, restlessness or cyanosis (late) y. JVD or tracheal deviation (late)

ALS Airway/Ventilation Methods z Needle Thoracostomy y. Prepare equipment x. Large bore angiocath y. Locate landmarks: 2 nd intercostal space at midclavicular line y. Insert catheter through chest wall into pleural space over top of 3 rd rib (blood vessels, nerves follow inferior rib margin) y. Withdraw needle, secure catheter like impaled object

ALS Airway/Ventilation Methods z. Chest Escharotomy y. Indications x. Presence of severe edema to soft tissue of thorax as with circumferential burns xinability to maintain adequate tidal volume, chest expansion even with assisted ventilation y. Considerations x. Must rule out upper airway obstruction x. Rarely needed

ALS Airway/Ventilation Methods z. Chest Escharotomy y. Procedure x. Intubate if not already done x. Prepare site, equipment x. Vertical incision to anterior axillary line x. Horizontal incision only if necessary x. Cover, protect

Airway & Ventilation Methods z Saturday’s class y. Practice using equipment xorotracheal intubation xnasotracheal intubation xgastric tube insertion xsurgical airways xneedle thoracostomy xcombitube xretrograde intubation