AICE Biology Chapter 9 The Mammalian Heart The

AICE Biology, Chapter 9 The Mammalian Heart

The Heart • Location – Thorax between the lungs in the inferior mediastinum • Orientation – Pointed apex directed toward left hip – Base points toward right shoulder • About the size of your fist
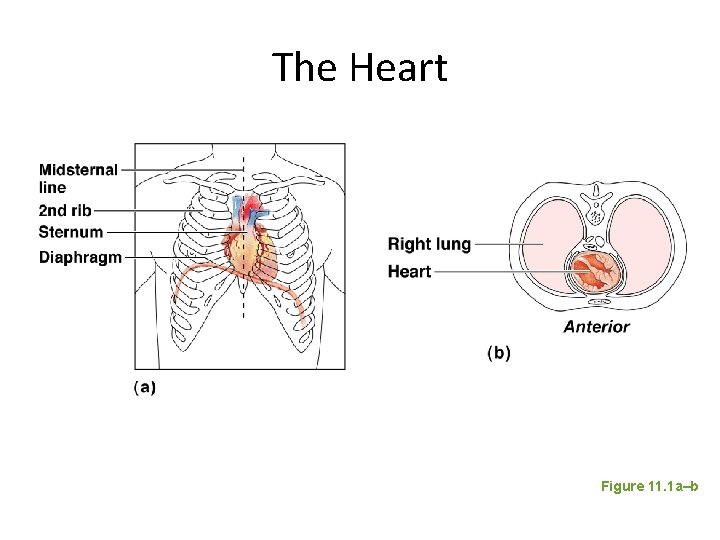
The Heart Figure 11. 1 a–b
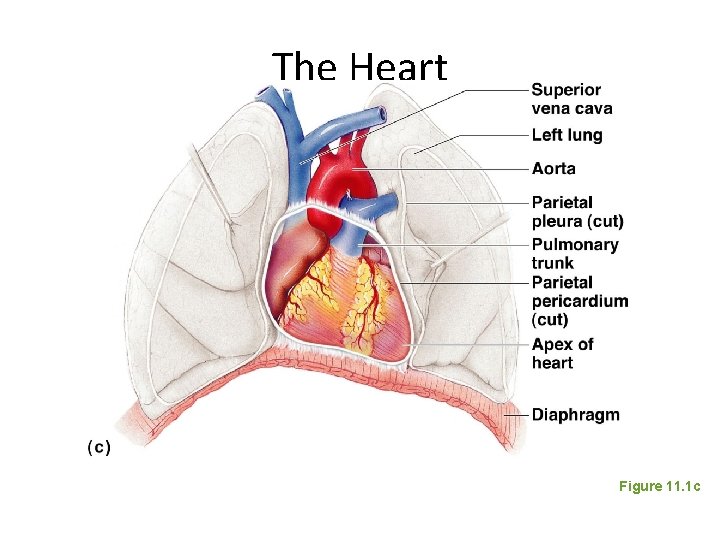
The Heart Figure 11. 1 c
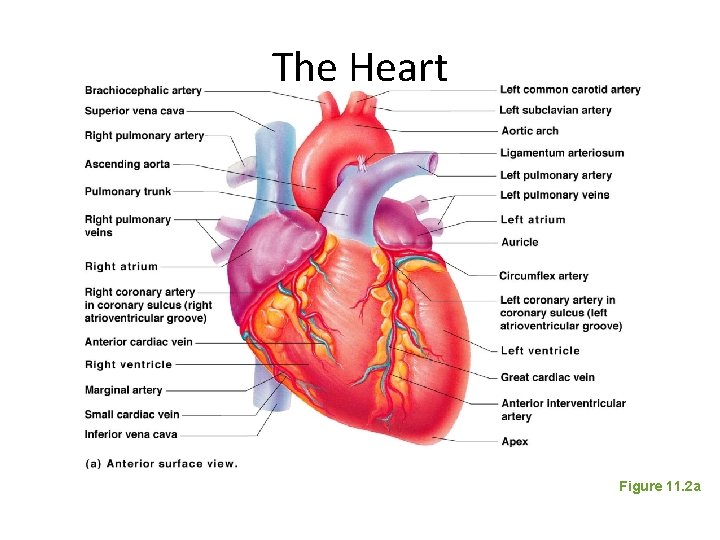
The Heart Figure 11. 2 a

The Heart: Coverings • Pericardium—a double-walled sac – Fibrous pericardium is loose and superficial – Serous membrane is deep to the fibrous pericardium and composed of two layers • Visceral pericardium – Next to heart; also known as the epicardium • Parietal pericardium – Outside layer that lines the inner surface of the fibrous pericardium – Serous fluid fills the space between the layers of pericardium
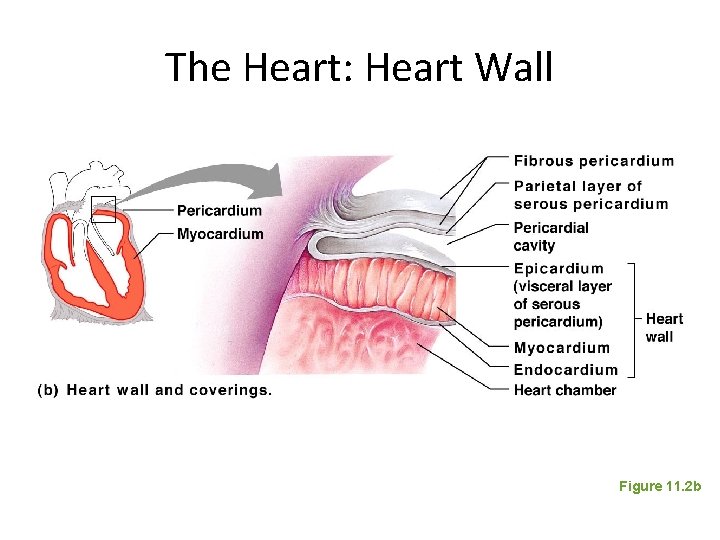
The Heart: Heart Wall Figure 11. 2 b

The Heart: Heart Wall • Three layers – Epicardium • Outside layer • This layer is the visceral pericardium • Connective tissue layer – Myocardium • Middle layer • Mostly cardiac muscle – Endocardium • Inner layer • Endothelium
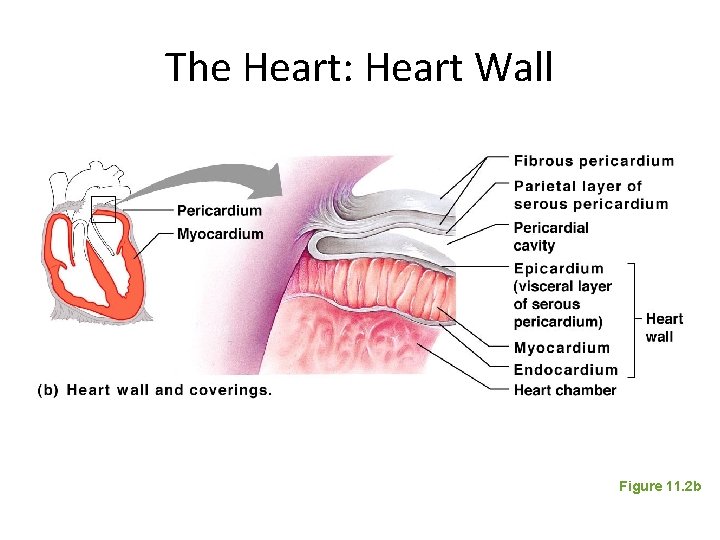
The Heart: Heart Wall Figure 11. 2 b
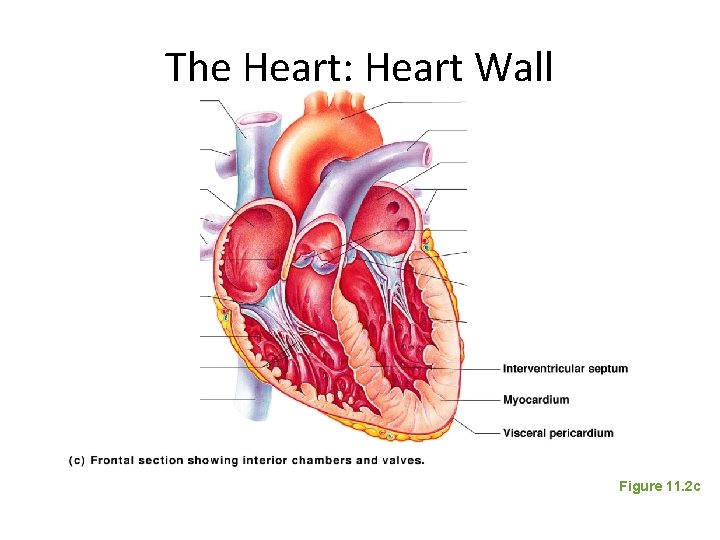
The Heart: Heart Wall Figure 11. 2 c

The Heart: Chambers • Right and left side act as separate pumps • Four chambers – Atria • Receiving chambers – Right atrium – Left atrium – Ventricles • Discharging chambers – Right ventricle – Left ventricle
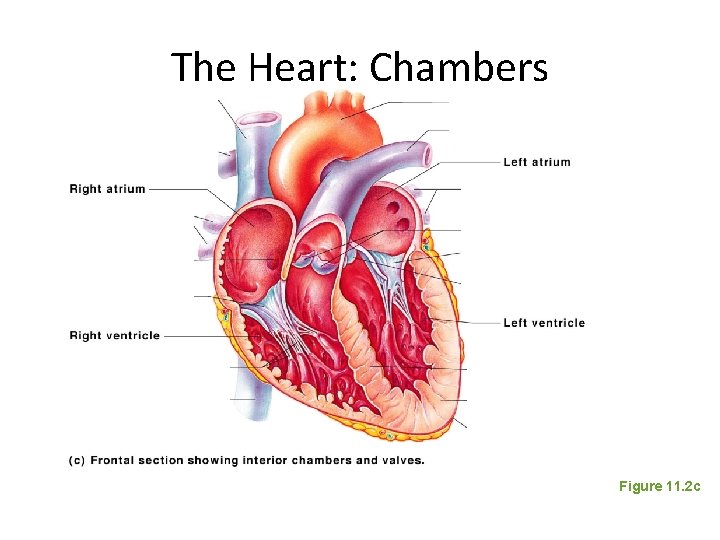
The Heart: Chambers Figure 11. 2 c
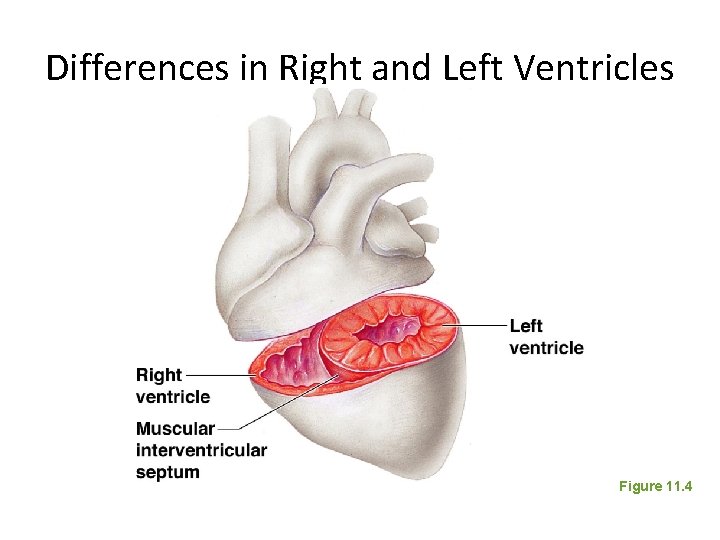
Differences in Right and Left Ventricles Figure 11. 4

The Heart: Septa • Interventricular septum – Separates the two ventricles • Interatrial septum – Separates the two atria
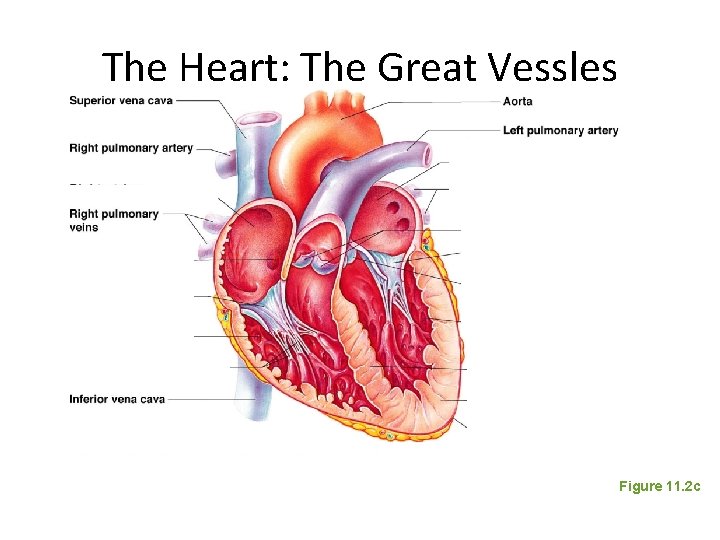
The Heart: The Great Vessles Figure 11. 2 c

The Heart: Valves • Allow blood to flow in only one direction to prevent backflow • Four valves – Atrioventricular (AV) valves—between atria and ventricles • Bicuspid (mitral) valve (left side of heart) • Tricuspid valve (right side of heart) – Semilunar valves—between ventricle and artery • Pulmonary semilunar valve • Aortic semilunar valve
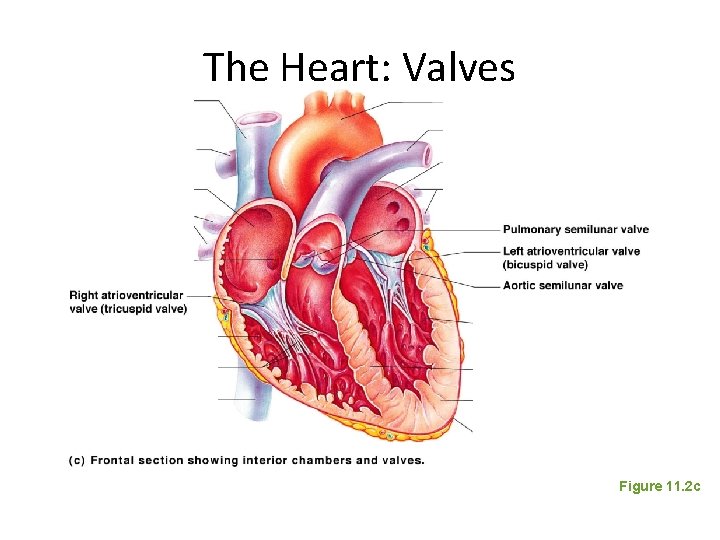
The Heart: Valves Figure 11. 2 c

The Heart: Valves • AV valves – Anchored in place by chordae tendineae (“heart strings”) – Open during heart relaxation and closed during ventricular contraction • Semilunar valves – Closed during heart relaxation but open during ventricular contraction • Notice these valves operate opposite of one another to force a one-way path of blood through the heart
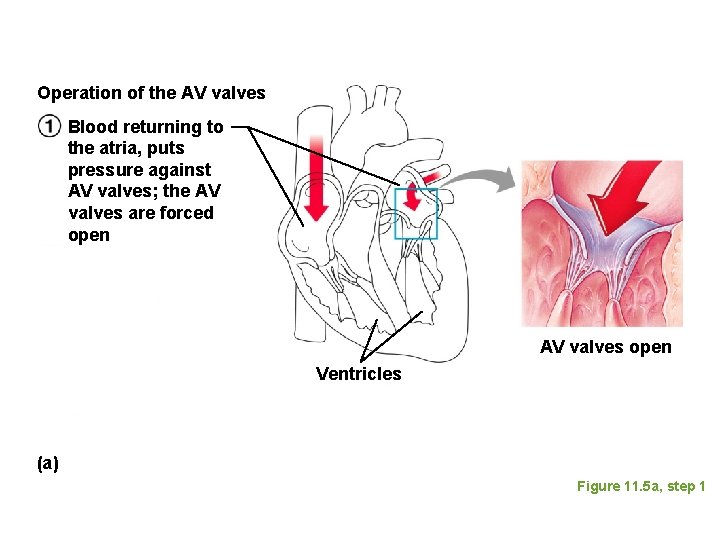
Operation of the AV valves Blood returning to the atria, puts pressure against AV valves; the AV valves are forced open AV valves open Ventricles (a) Figure 11. 5 a, step 1
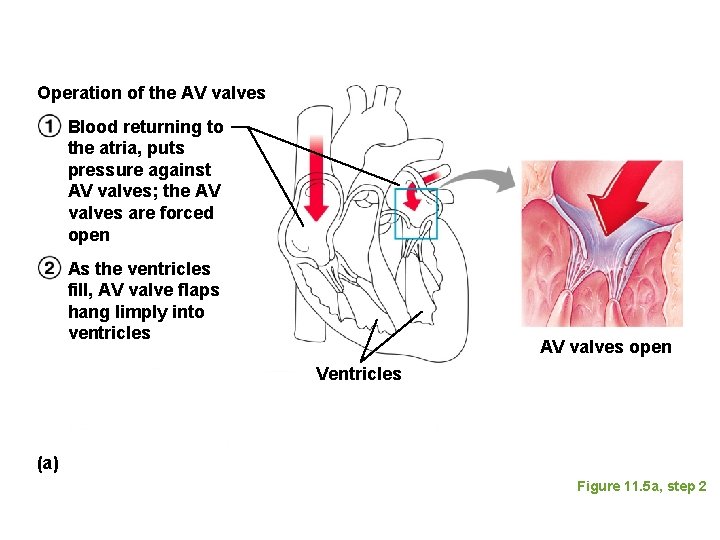
Operation of the AV valves Blood returning to the atria, puts pressure against AV valves; the AV valves are forced open As the ventricles fill, AV valve flaps hang limply into ventricles AV valves open Ventricles (a) Figure 11. 5 a, step 2
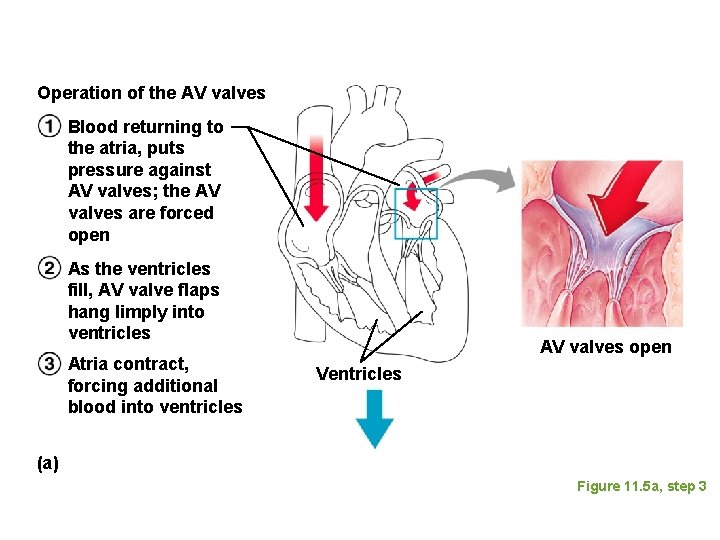
Operation of the AV valves Blood returning to the atria, puts pressure against AV valves; the AV valves are forced open As the ventricles fill, AV valve flaps hang limply into ventricles Atria contract, forcing additional blood into ventricles AV valves open Ventricles (a) Figure 11. 5 a, step 3
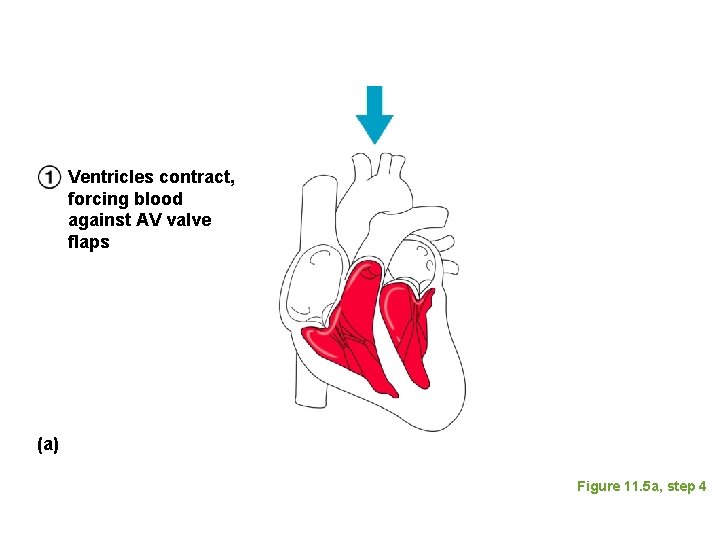
Ventricles contract, forcing blood against AV valve flaps (a) Figure 11. 5 a, step 4
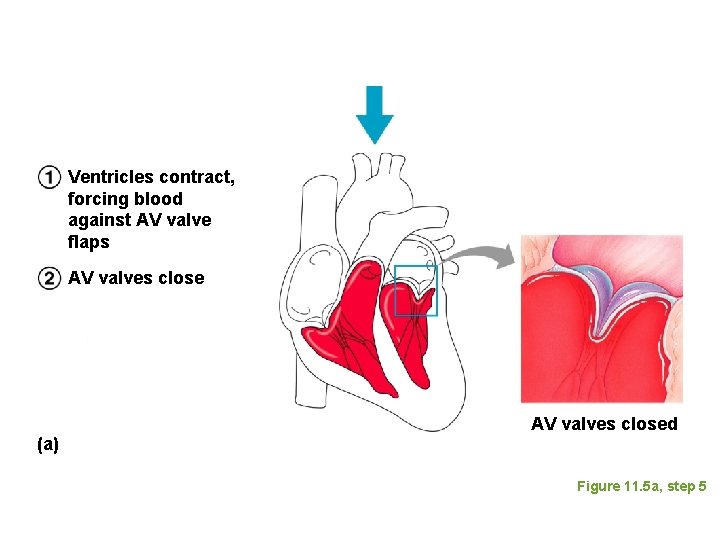
Ventricles contract, forcing blood against AV valve flaps AV valves close (a) AV valves closed Figure 11. 5 a, step 5
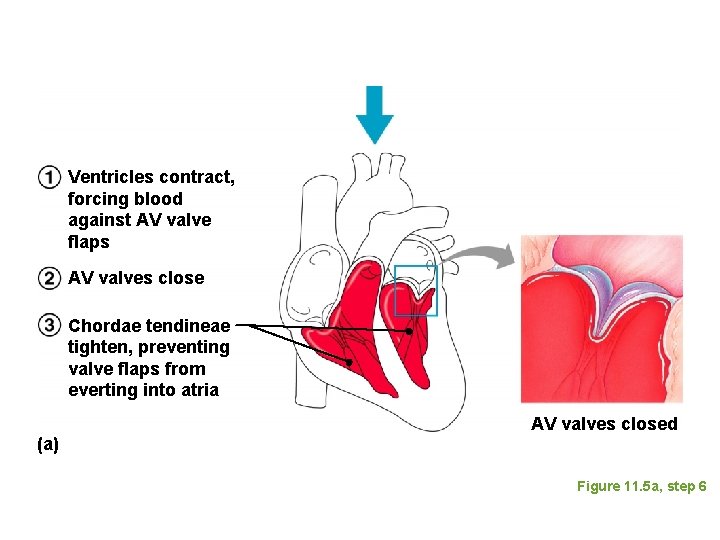
Ventricles contract, forcing blood against AV valve flaps AV valves close Chordae tendineae tighten, preventing valve flaps from everting into atria (a) AV valves closed Figure 11. 5 a, step 6
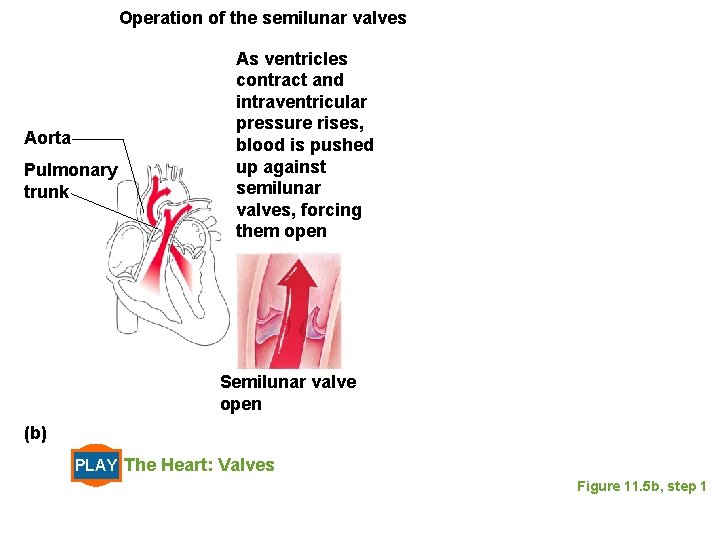
Operation of the semilunar valves Aorta Pulmonary trunk As ventricles contract and intraventricular pressure rises, blood is pushed up against semilunar valves, forcing them open Semilunar valve open (b) PLAY The Heart: Valves Figure 11. 5 b, step 1
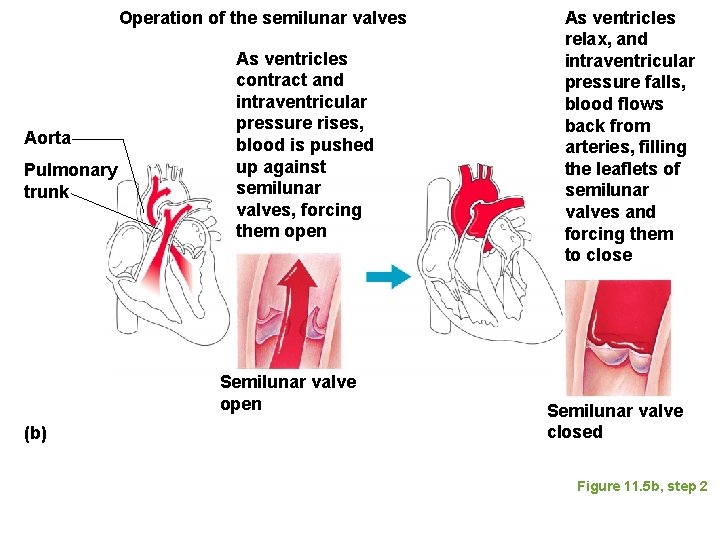
Operation of the semilunar valves Aorta Pulmonary trunk As ventricles contract and intraventricular pressure rises, blood is pushed up against semilunar valves, forcing them open Semilunar valve open (b) As ventricles relax, and intraventricular pressure falls, blood flows back from arteries, filling the leaflets of semilunar valves and forcing them to close Semilunar valve closed Figure 11. 5 b, step 2

The Heart: Cardiac Cycle • Cardiac cycle—events of one complete heart beat – Atrial Systole: Atria contract simultaneously – Ventricular Systole: Atria relax, then ventricles contract – Diastole: relaxation
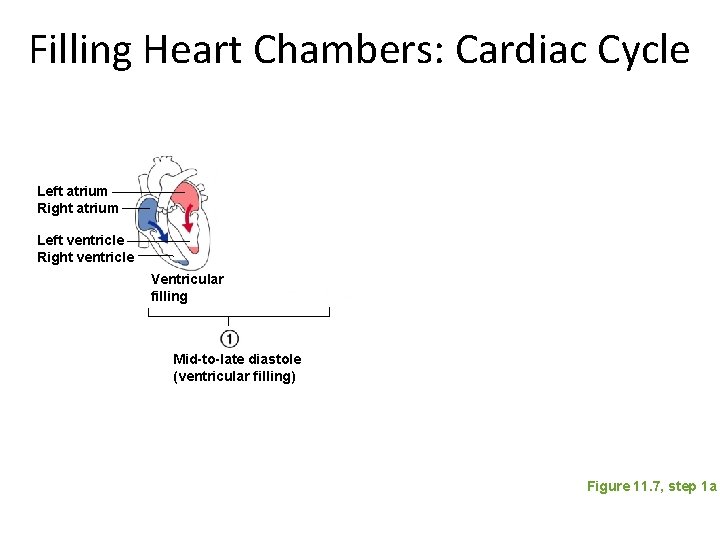
Filling Heart Chambers: Cardiac Cycle Left atrium Right atrium Left ventricle Right ventricle Ventricular filling Mid-to-late diastole (ventricular filling) Figure 11. 7, step 1 a
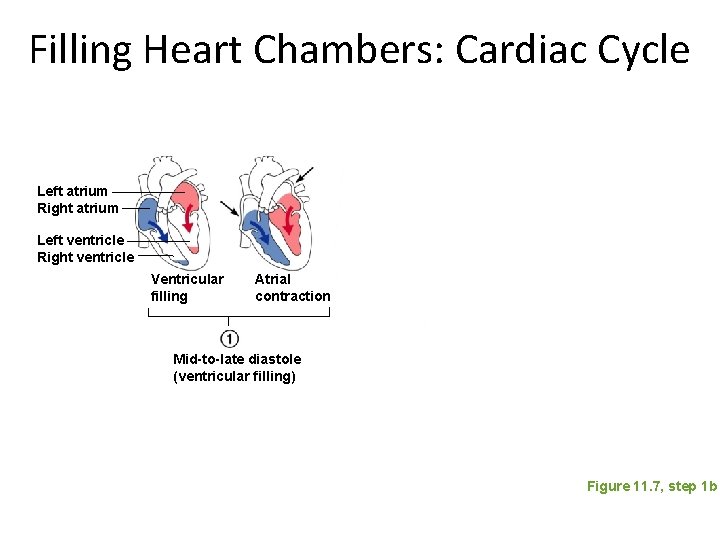
Filling Heart Chambers: Cardiac Cycle Left atrium Right atrium Left ventricle Right ventricle Ventricular filling Atrial contraction Mid-to-late diastole (ventricular filling) Figure 11. 7, step 1 b
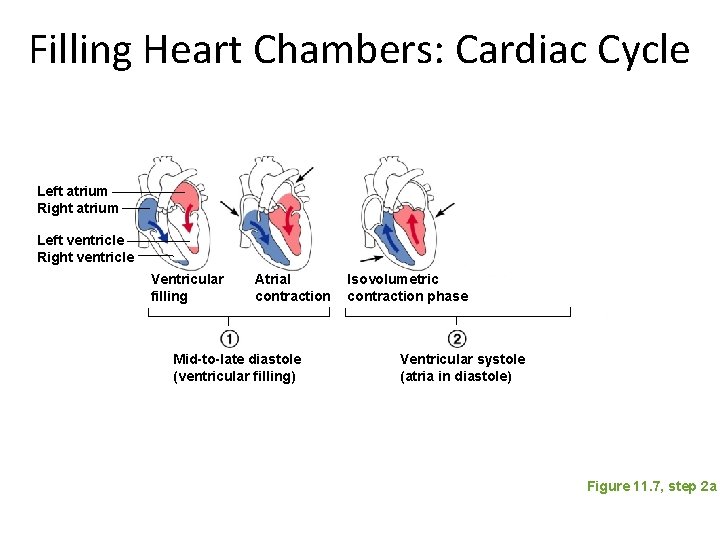
Filling Heart Chambers: Cardiac Cycle Left atrium Right atrium Left ventricle Right ventricle Ventricular filling Atrial contraction Mid-to-late diastole (ventricular filling) Isovolumetric contraction phase Ventricular systole (atria in diastole) Figure 11. 7, step 2 a
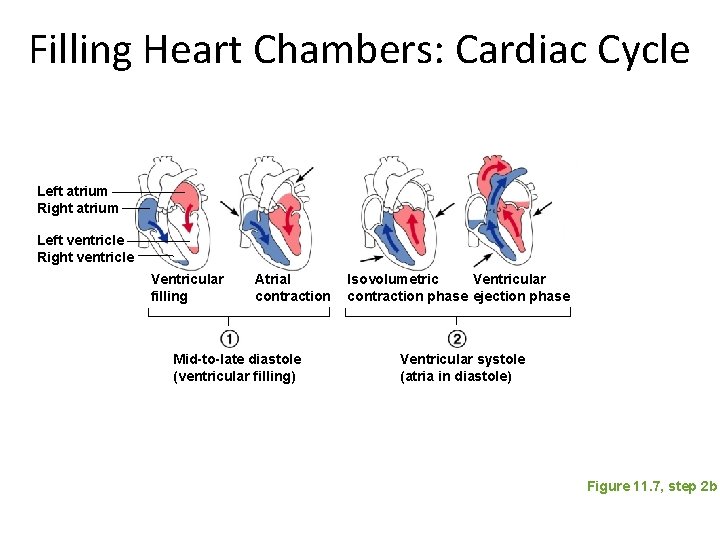
Filling Heart Chambers: Cardiac Cycle Left atrium Right atrium Left ventricle Right ventricle Ventricular filling Atrial contraction Mid-to-late diastole (ventricular filling) Isovolumetric Ventricular contraction phase ejection phase Ventricular systole (atria in diastole) Figure 11. 7, step 2 b
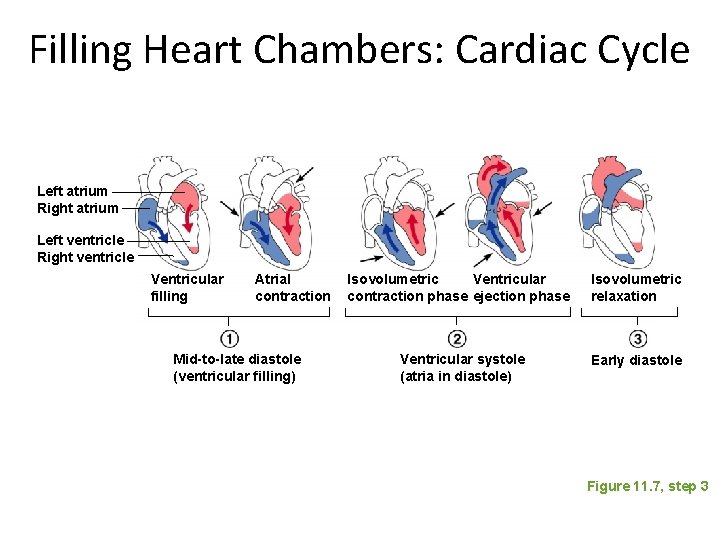
Filling Heart Chambers: Cardiac Cycle Left atrium Right atrium Left ventricle Right ventricle Ventricular filling Atrial contraction Mid-to-late diastole (ventricular filling) Isovolumetric Ventricular contraction phase ejection phase Isovolumetric relaxation Ventricular systole (atria in diastole) Early diastole Figure 11. 7, step 3

Measuring Blood Pressure • A typical blood pressure for a healthy young adult is about 120/70. • Blood pressure is commonly measured using a sphygmomanometer. • Hypertension is a serious cardiovascular problem in which blood pressure is persistent at or above – 140 systolic and/or – 90 diastolic. © 2012 Pearson Education, Inc.
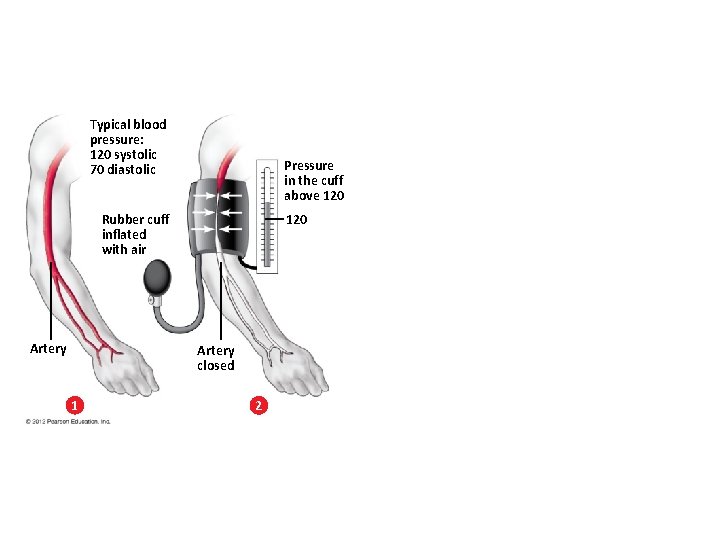
Typical blood pressure: 120 systolic 70 diastolic Pressure in the cuff above 120 Rubber cuff inflated with air Artery 120 Artery closed 1 2
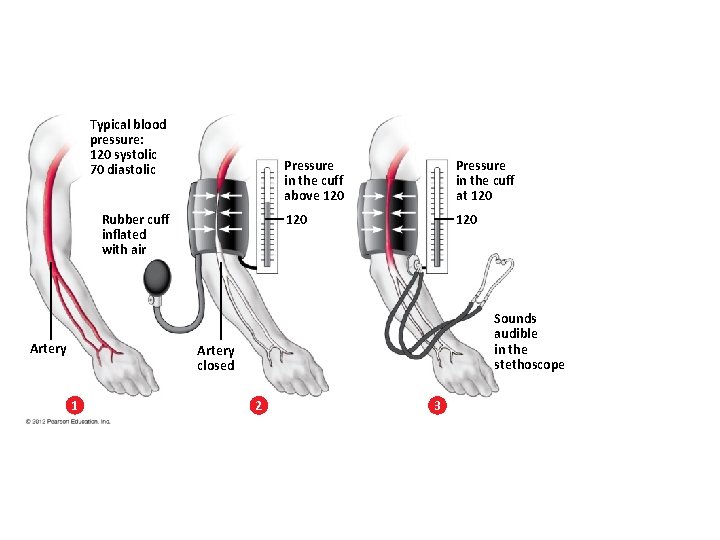
Typical blood pressure: 120 systolic 70 diastolic Rubber cuff inflated with air Artery Pressure in the cuff above 120 Pressure in the cuff at 120 120 Sounds audible in the stethoscope Artery closed 1 2 3
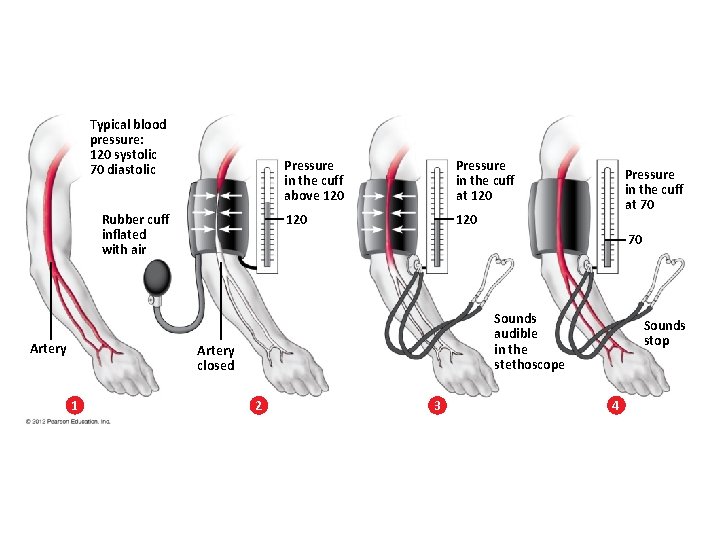
Typical blood pressure: 120 systolic 70 diastolic Rubber cuff inflated with air Artery Pressure in the cuff above 120 Pressure in the cuff at 120 120 70 Sounds audible in the stethoscope Artery closed 1 Pressure in the cuff at 70 2 3 Sounds stop 4

• Hypertension causes – the heart to work harder, weakening the heart over time, – increased plaque formation from tiny ruptures, and – increased risk of blood clot formation. • Hypertension can contribute to – heart attacks, – strokes, and/or – kidney failure. © 2012 Pearson Education, Inc.

The Heart: Conduction System • Intrinsic conduction system (myogenic heart) – Heart muscle cells contract, without nerve impulses, in a regular, continuous way

The Heart: Conduction System • Special tissue sets the pace • Sinoatrial node = SA node (“pacemaker”), is in the right atrium • Atrioventricular node = AV node, is at the junction of the atria and ventricles • Atrioventricular bundle = AV bundle (bundle of His), is in the interventricular septum • Bundle branches are in the interventricular septum • Purkinje fibers (Purkyne fibers) spread within the ventricle wall muscles
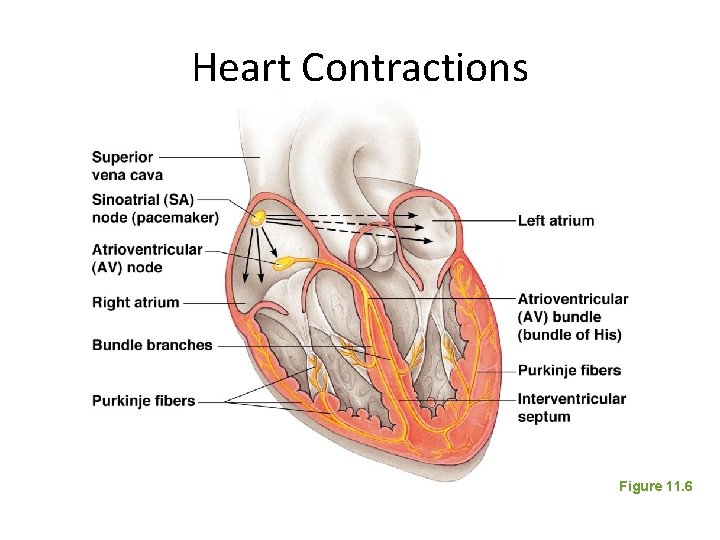
Heart Contractions Figure 11. 6

Heart Contractions • Contraction is initiated by the sinoatrial node (SA node) • Sequential stimulation occurs at other autorhythmic cells • Force cardiac muscle depolarization in one direction—from atria to ventricles

Heart Contractions • Once SA node starts the heartbeat – Impulse spreads to the AV node – Then the atria contract • At the AV node, the impulse passes through the AV bundle, bundle branches, and Purkinje fibers • Blood is ejected from the ventricles to the aorta and pulmonary trunk as the ventricles contract
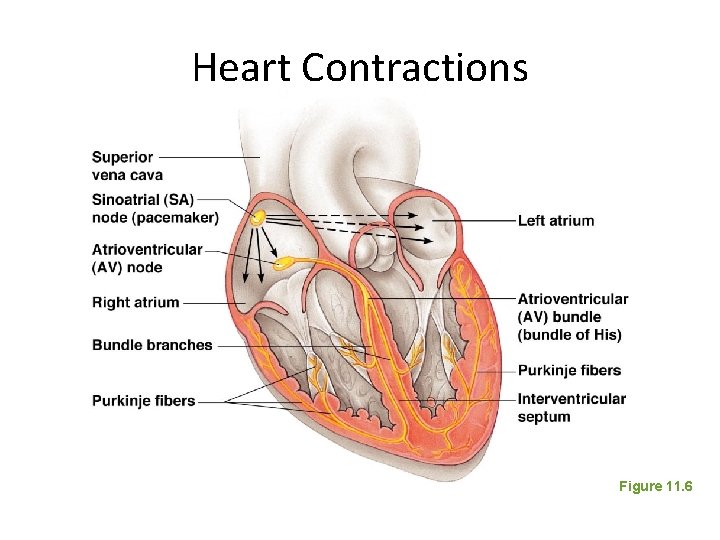
Heart Contractions Figure 11. 6

Problems with Control & Conduction • Heart block—failure of a part of the conduction system, usually due to ischemia or infarction • Ischemia – low oxygenation of heart tissue, often resulting from arterial disease • Arrhythmia—an abnormal rhythm, often the result of a damage to the SA node • Tachycardia—rapid heart rate over 100 beats per minute • Bradycardia—slow heart rate less than 60 beats per minutes • Fibrillation—uncoordinated, unproductive contraction of heart muscle

Coronary Circulation • Blood in the heart chambers does not nourish the myocardium • The heart has its own nourishing circulatory system consisting of – Coronary arteries—branch from the aorta to supply the heart muscle with oxygenated blood – Cardiac veins—drain the myocardium of blood – Coronary sinus—a large vein on the posterior of the heart, receives blood from cardiac veins • Blood empties into the right atrium via the coronary sinus

Electrocardiograms • ECG measures electrical activity associated with conduction and contraction. • Parts of the wave correspond to events of the Cardiac Cycle: – P wave – atrial contraction – QRS complex – ventricular contraction – T wave – ventricular repolarization during diastole
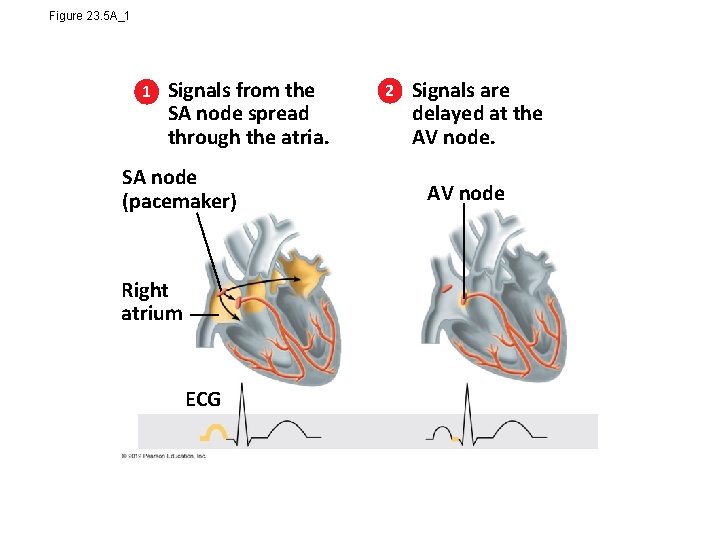
Figure 23. 5 A_1 1 Signals from the SA node spread through the atria. SA node (pacemaker) Right atrium ECG 2 Signals are delayed at the AV node
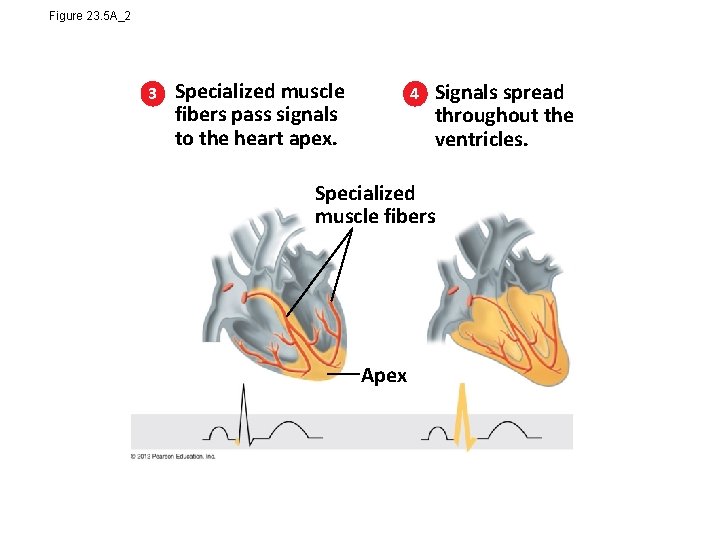
Figure 23. 5 A_2 3 Specialized muscle fibers pass signals to the heart apex. 4 Signals spread throughout the ventricles. Specialized muscle fibers Apex
- Slides: 48