Aging and Diseases of the Salivary Glands Biology

Aging and Diseases of the Salivary Glands Biology of Salivary Glands Domenica G. Sweier DDS June 4, 2003

Saliva § Frustrating for the dental team yet necessary for the patient! June 4, 2003 2

When there is not Enough § Too little saliva can significantly alter a person’s quality of life and the morbidity associated with multiple systemic conditions • How little is too little? • What affects the quality and quantity of saliva production and flow? June 4, 2003 3

June 4, 2003 4

Objective vs Subjective § Objective • Major gland secretions § Resting flow rate with a Carlson-Crittenden Cup • Minor gland secretions • Whole saliva § Stimulated flow rate with citric acid, wax June 4, 2003 § Subjective • Complaints of dry mouth (xerostomia) • Questionnaire • Thirst • The “cracker” test 5

Xerostomia § Commonly referred to as “dry mouth” § Diminished salivary flow rate, typically accepted as a 50% decrease in the clinically determined rate in healthy individuals not taking medications • Resting Flow Rate 0. 3 -0. 4 ml/min • Stimulated Flow Rate 1 -2 ml/min June 4, 2003 6

Clinical Signs/Symptoms of Xerostomia § Dryness of mucous membranes § Tongue fissuring and lobulation (scrotal tongue) § Angular cheilosis/cheilitis § Fungal infections § Prosthesis-induced stomatitis § Amputation caries § Thick, ropey saliva June 4, 2003 § Dysphagia § Dysgeusia § Difficulty eating/speaking/ wearing prosthesis § Swelling of the salivary glands § Difficulty expressing saliva § Cheek biting § Persistent need for fluids § Burning tongue 7

What Contributes to Xerostomia? § Aging • Hormonal Changes/Menopause § Disease • Local • Systemic § Environmental Insults/Trauma § Medications June 4, 2003 8

Aging § Salivary Quantity in Health • No changes in major secretions (parotid, submandibular) • No changes in minor secretions June 4, 2003 § Salivary Quality in Health • No general changes in salivary constituents 9

Aging § If the quality and quantity of saliva doesn’t change with age, then what accounts for the increased incidence of xerostomia and associated morbidity among the elderly? • Medications, diseases, and other environmental insults affect both the quality and quantity of saliva § An increase in incidence of these insults generally associated with an increase in age June 4, 2003 10

Menopause § Average of onset of menopause in USA is 50 years § Oral symptoms common, particularly among those with systemic complaints § Cross-sectional and longitudinal studies have failed to provide significant and reproducible evidence that salivary flow is affected by menopause • Oral complaints most likely the result of the types and numbers of xerostomic medications taken § Anti-hypertensives, anti-depressants, and anti-histamines are common in this group June 4, 2003 11

Diseases/Environmental Factors § Diseases • Local • Systemic § Environmental Factors • Head and Neck Radiation • Chemotherapy • Medications June 4, 2003 12

Local Diseases § Tumors/Growths • Benign • Malignant § Obstructive Diseases • Calculi, mucus plugs • Unusual anatomy June 4, 2003 § Inflammatory Diseases • Acute viral sialadenitis • Acute and recurrent bacterial sialadenitis • Inflammation/Infection secondary to systemic disease 13

Tumors/Growths § Primary benign and malignant tumors • Determine whether benign or malignant since they are treated differently • Incisional biopsy for definitive diagnosis • Smaller the involved gland, more likely malignant June 4, 2003 § Malignant • Seek medical attention for swelling under the chin or around the jawbone, if the face becomes numb, facial muscles do not move, or there is persistent pain • Usually treated with a combination of surgery and radiation 14

Obstruction: Sialolithiasis § Calculi form in the duct, blocking the egress of saliva • Majority in submandibular gland § § Painful swelling which increases at meal time Bi-manual palpation in submandibular gland X-ray, sialography, CT, ultrasound Analgesics, try to push stone out, may need to dilate orifice to remove June 4, 2003 15
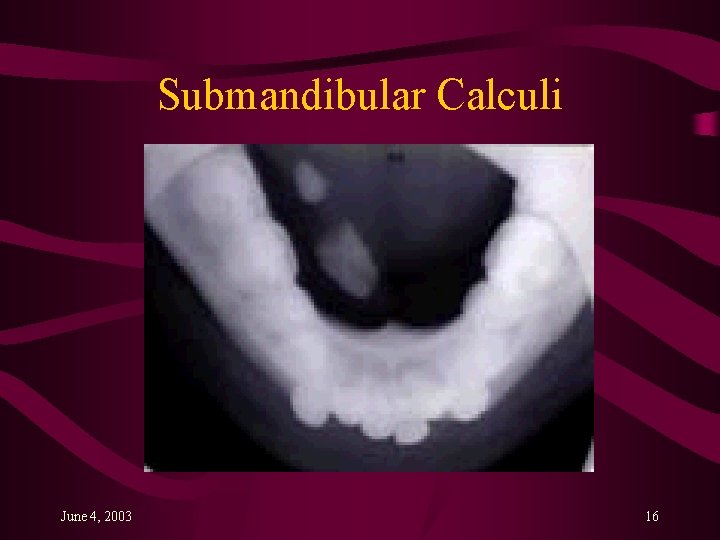
Submandibular Calculi June 4, 2003 16

Unusual Anatomy § Unusual anatomy in the gland manifested as strictures in the duct system • Recurrent obstruction with associated pain and inflammation of glands • Pooling of saliva leading to secondary infection § May need surgery to remove affected area of gland or entire gland June 4, 2003 17

Inflammation/Infection: Viral § Mumps is the most frequent diagnosis of acute viral sialadenitis • • Member of the paramyxoviridae Mostly in parotid The incubation period is 2 -3 weeks Acute painful swelling and enlargement Fever, headache, loss of appetite Most common in children Very effective vaccine June 4, 2003 18

Inflammation/Infection: Bacterial § Types • Acute suppurative bacterial sialadenitis § Commonly S. aureus, S. viridans, H. influenzae, E. coli • Chronic recurrent sialadenitis § May be secondary to some type of obstruction or unusual anatomy § May be due to resistant organism; culture to determine § Treatment • Antibiotics and analgesics • Rehydrate and stimulate saliva • May need open drainage/surgery June 4, 2003 19

Bacterial Parotiditis June 4, 2003 20

Systemic Diseases § § § § Sjögren’s Syndrome Sarcoidosis Cystic Fibrosis Diabetes Alzheimer’s Disease AIDS Graft vs Host Disease Dehydration June 4, 2003 21

Sjögren’s Syndrome § Autoimmune disorder affecting lacrimal and salivary glands • Xerostomia and keratoconjunctivitis sicca § Primary and Secondary disease • The latter associated with another autoimmune disorder such as RA, SLE, etc. § Dense inflammatory infiltrate with destruction of glandular tissue § Treatment is palliative June 4, 2003 22

Sarcoidosis § Unknown cause; believed to be alteration in cellular immune function and involvement of some allergen § Any organ but most often the lungs; can affect the parotid gland § Granulomatous inflammation § Most often drugs of choice are corticosteroids June 4, 2003 23

Cystic Fibrosis § Faulty transport of sodium and chloride from within cells lining lungs and pancreas to their outer surface § Causes production of an abnormally thick sticky mucus § Obstruction of pancreas leads to digestive problems; inability to digest and absorb nutrients § Gene has been identified and cloned § No known “cure” therefore palliative treatment June 4, 2003 24

Diabetes § Uncontrolled blood glucose levels may contribute to xerostomia § Medications may induce xerostomia § May get enlargement and inflammation of parotid glands (common in endocrine diseases) § Difficulty to ward off infection: candidiasis, gingivitis, periodontitis, and caries June 4, 2003 25

Alzheimer’s Disease § A neurodegenerative disorder leading to a decrease in cognition and mobility § May affect the neurological component to salivary production and/or flow § Xerostomic medications • Complicated by behavior which makes it difficult to maintain a healthy dentition § Poor oral hygiene § Poor cooperation for dental care and treatment in a conventional setting June 4, 2003 26

AIDS § HIV-Associated Salivary Gland Disease (HIV-SGD) • • Enlargement of the major salivary glands Xerostomia Some similarities to autoimmune diseases HIV itself not consistently found to be in glandular tissue § Medications June 4, 2003 27

Graft vs Host Disease (GVHD) § Immune cells of an allogenic transplant attack recipient § Acute, < 100 days, and chronic > 100 days § Major cause of morbidity and mortality § Initial presentation as a red rash § Salivary gland involvement with swelling and inflammation § Progresses quickly to life-threatening condition § Treat by increasing immunosuppression June 4, 2003 28

Dehydration § Defined as the loss of water and essential body salts (electrolytes) needed for body function • Sweating, diarrhea, emesis, blood loss, etc. § Symptoms include flushed face, dry, warm skin, fatigue, cramping, reduced amount of urine § Oral signs/symptoms • Xerostomia, dry tongue • Thick, sticky saliva • Dry, cracked lips (cheilosis) June 4, 2003 29
Head and Neck Cancer: Radiation Therapy § Goal is to kill cancer cells § Measured in Gray (Gy) units of absorbed radiation: 1 Gy = 100 c. Gy = 100 rads § Can be used alone or combined with surgery and/or chemotherapy § Three main routes • External beam (most head and neck) • Brachytherapy (body cavities) • Interstitial June 4, 2003 30

Radiation Dose § Dependent on tumor tissue/type § Average of 200 c. Gy daily for 5 consecutive days with two days of rest § Total cummulative dose ranges from 5000 c. Gy to 8000 c. Gy for advanced tumors § Threshold of permanent destruction is 21004000 c. Gy June 4, 2003 31

Tissue Response § 25 Gy: Bone marrow, lymphocytes, GI epithelium, germinal cells § 25 -50 Gy: Oral epithelium, endothelium of blood cells, salivary glands, growing bone and cartilage, collagen § Doses > 50 Gy: bone and cartilage, skeletal muscle June 4, 2003 32

Tissue Changes § Irradiated tissue becomes hypocellular, hypovascular, and hypoxic resulting in fibrosis and vascular occlusion § The destruction is mostly permanent • Irradiated tissue does not re-vascularize with time § As a result, irradiated tissue does not heal well after injury June 4, 2003 33

Common Side Effects: Systemic § § § Nausea Vomiting Neutropenia Alopecia Fatigue June 4, 2003 34

Common Side Effects: Oral § § § Mucositis and Dermatitis Dysphagia Dysgeusia Trismus Osteo- and soft tissue necrosis Xerostomia • Fungal infections • Radiation Caries June 4, 2003 35

Radiation: Xerostomia § Parotid gland is more susceptible than the submandibular or sublingual glands § See a slight improvement after therapy but will soon plateau at a lower level than pretherapy § Result is thick, ropey saliva, decreased in amount, with markedly diminished lubricating and protective qualities June 4, 2003 36

Radiation: Mucositis § The oral eipthelium will get a “sun burn” like inflammation § This will be exacerbated by the lack of the lubricating properties of saliva § The result will be a red, irritated, dry mucosa June 4, 2003 37

Saliva Post-Radiation June 4, 2003 38

Mucositis June 4, 2003 39

Radiation Caries June 4, 2003 40

Prosthesis-Induced Stomatitis June 4, 2003 41

Fungal Infections June 4, 2003 42

Scrotal Tongue June 4, 2003 43

Chemotherapy § Is given orally, IV, by injection (SQ, IM, IL), or topically in cycles depending on the treatment goals (type of cancer, how your body responds, how well you body recovers, etc. ) § Affects all rapidly dividing cells • Many side effects in all body systems § Oral complications from direct damage to oral tissues secondary to chemotherapy and indirect damage due to regional or systemic toxicity • Frequency and severity related to systemic immune compromise, i. e. myelosuppresion June 4, 2003 44

Chemotherapeutics § Drugs commonly associated with oral complications • • • Methotrexate Doxorubicin 5 -Fluorouracil (5 -FU) Busulfan Bleomycin Platinum coordination complexes § Cisplatin § Carboplatin June 4, 2003 45

Tissue Damage § The propensity of chemotherapy to damage tissue, specifically oral tissues, is dependent on each individual drug and its ability to induce myelosuppresion (neutropenia) § Drugs differ on the timing of myelosuppresion • Consider this when treating patients undergoing chemotherapy § Tissues, oral tissues, return to pre-chemotherapy state when allowed time to heal after therapy June 4, 2003 46

Common Side Effects: Systemic § § § § Fatigue Nausea Constipation Diarrhea Hemorrhage Anemia Neutropenia June 4, 2003 § § § Pain Alopecia Peripheral neuropathy CNS disturbances Fluid retention Bladder and kidney problems 47

Common Side Effects: Oral § § § Mucositis (ulcerative) Reactivation of HSV Dysgeusia Dysphagia Infections § Neuropathies § Salivary gland dysfunction/toxicity • xerostomia • Fungal • Periodontium • periapices June 4, 2003 48

Summary § While there appear to be many insults leading to salivary hypofunction, healthy aging does not appear to be one of them § The main insults leading to salivary gland damage and/or hypofunction are • Disease § Local § Systemic • Environmental insults/trauma § Radiation § Chemotherapy • Medications June 4, 2003 49
- Slides: 49