Age Appropriate Cancer Screening James Mason DO PGY2
































- Slides: 37

Age Appropriate Cancer Screening James Mason, DO PGY-2

Historical Tid-Bit Hippocrates (460 -370 BC) : carcinos, carcinoma used to describe various tumors. Celsus (28 -50 BC) : translated above terms from Greek to Latin = Cancer “Cancer” means “Crab”

Tid-Bit continued Image 7

Tid-Bit continued Image 7

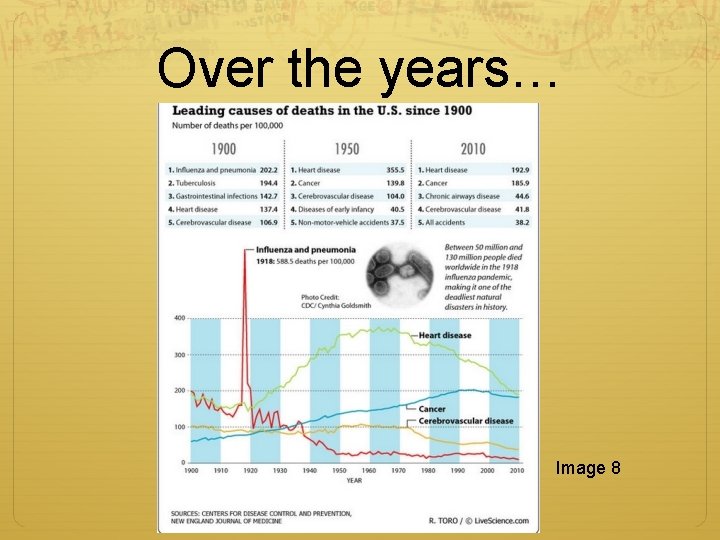
Over the years… Image 8

Cancer Screening Looking for disease (or signs of disease) in people who are not showing any symptoms. Goal: To find/prevent a disease process when it is most easily treated. Image 9

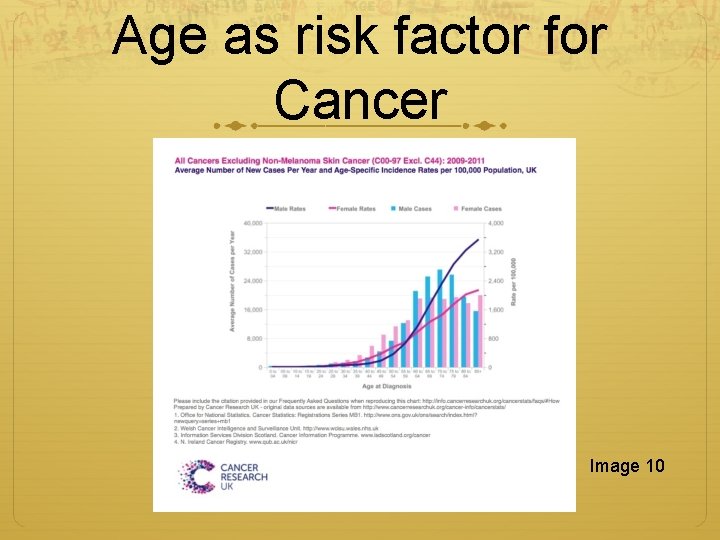
Age as risk factor for Cancer Image 10

Where do you get your info? American Cancer Society (ACS) U. S. Preventative Services Task Force (USPSTF) American Congress of Obstetricians and Gynecologists (ACOG) American Gastroenterology Association American College of Radiology

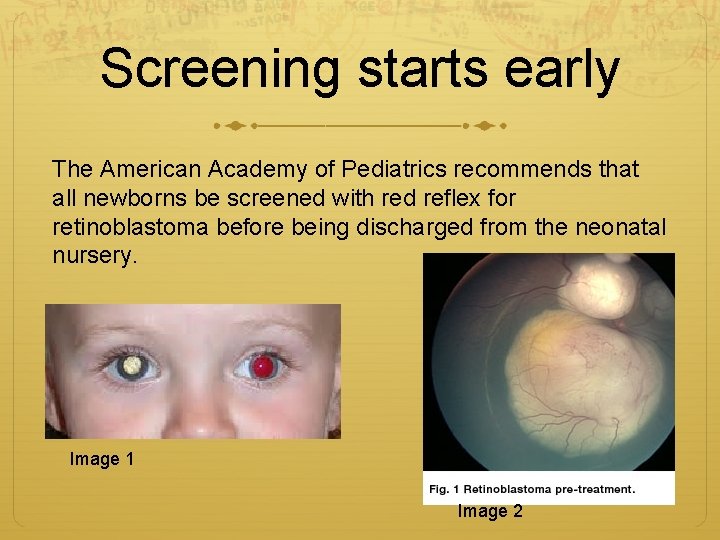
Screening starts early The American Academy of Pediatrics recommends that all newborns be screened with red reflex for retinoblastoma before being discharged from the neonatal nursery. Image 1 Image 2

Useful resources American Cancer Society (ACS) http: //www. cancer. org/healthy/toolsandcalculators/reminders/scr eening-recommendations-by-age US Preventative Service Task Force (USPSTF) http: //www. uspreventiveservicestaskforce. org/Browse. Rec/Index Up. To. Date American Congress of Obstetricians and Gynecologists (ACOG) American Gastroenterology Association All are broken down by age, very helpful.

Interpreting USPSTF recommendations Image 3

Age 20 -29 Men: No screening recommended unless you have high risk for colon cancer and require earlier screening. HNPCC (Lynch) start 20 -25 yo, q 1 -2 yrs Or 2 -5 years prior to earliest age of CRC in family. FAP Classical: flex sig or colonoscopy age 10 -12, q 1 year to age 35 -40 if neg. EGD with end & side viewing start age 25 -30 or sooner if symptoms of pancreatitis, biliary obst. Intervals based on spigelman classification. Attenuated: Colonoscopy (risk for right colonic lesions) age 25 and q 1 -2 years Peutz-Jeghers: EGD, Pill cam, colonoscopy age 8 + polyps: repeat q 3 years to age 50 then every 1 -2 years >50. - polyps: repeat age 18 Women: Start cervical and breast cancer screening (colon cancer if high risk). Clinical breast exam recommendations to follow.

High risk breast cancer screening Annual breast MRI and mammogram (alternate q 6 months) recommended in following groups: Age>=25 Lifetime breast cancer risk >20% (Gail, Claus etc. ) Known BRCA 1 or 2 + 1 st degree relative with known BRCA 1 or 2 History of chest radiation from 10 -30 yo If lifetime risk is moderate (15 -20%, not enough evidence to support MRI screening or mammogram yet) No MRI screening recommended if <15%.

Clinical breast exams ACS recommends q 3 years 20 to 39, and annually thereafter. ACOG recommends q 1 -3 years 20 to 39, and annually thereafter. “The US Preventive Services Task Force concludes that evidence is insufficient to assess additional benefits of clinical breast examination beyond mammography, and the Canadian Task Force on Preventive Health Care recommends against clinical breast examination. The World Health Organization does not recommend clinical breast examination. No group recommends clinical breast examination alone. ” (uptodate)

Age 20 -29: Cervical ACS and USPSTF: Age 21 -29, PAP smear q 3 years. HPV only if abnormal PAP. [GRADE A] HPV as screening tool with or without PAP? “USPSTF recommends against screening for cervical cancer using HPV testing, alone or in combination with cytology, in women younger than 30 years. [GRADE D]”

Age 20 -29: Cervical Screen patients s/p hysterectomy? “The USPSTF recommends against screening for cervical cancer in women who have had a hysterectomy with removal of the cervix and who do not have a history of CIN 2, CIN 3 or cervical cancer. [GRADE D]

30 -39 Men: Colon only if high risk group Women Colon only if high risk group Breast: no change (unless additional risk) Cervical Starting age 30, cervical cancer screening should include HPV and PAP every 5 years. OR Continue PAP alone every 3 years.

PAP & HPV testing There are 4 HPV tests approved by FDA: Hybrid capture 2: tests 13 strands: results pooled Cervista HPV HR: tests 14 strands: results pooled Cobas HPV: tests 14 strands, specific results for 16/18 Aptima m. RNA: tests 14 strands, results pooled.

PAP & HPV testing alone or combined with PAP is more sensitive than PAP alone in detecting both cervical histopathology and adenocarcinoma. Decreased incidence of cancer in HPV testing groups No mortality benefit has been shown Increased number of positive results=>increased number of colposcopies performed.

PAP & HPV screening in women <30 Testing this age group leads to detection of significantly more transient HPV infections and unnecessary colposcopies. A 2011 systematic review concluded HPV testing with cytology testing found more CIN 3 or cancer than cytology screening alone, but concluded that more evidence is needed to determine and compare benefit and harm from HPV testing.

When to stop screening When adequate screening has been performed, screening can be discontinued at age 65 if the following criteria met. No increased risk (ie, history of abnormal screening, current smoker or history of smoking, unknown screening history, previous HPV-related disease, new partners, immunocompromised, in utero diethylstilbestrol exposure) Adequate prior screening: two negative consecutive co-tests or three negative Pap tests within the past 10 years, with the most recent test within the previous five years If inadequate testing, continue PAP q 3 years or co-tests q 5 years till age 70 -75. No history of high-grade dysplasia or worse

40 -49 Men Colon: ACS: not recommended unless high risk USPSTF: not recommended ACG: colonoscopy screening for AA males starting age 45. Prostate: not recommended, discuss risks/benefits with high risk individuals Women ACS: CBE annually, mammogram should be done yearly now. USPSTF: evidence insufficient to make recommendation. They recommend starting at age 50.

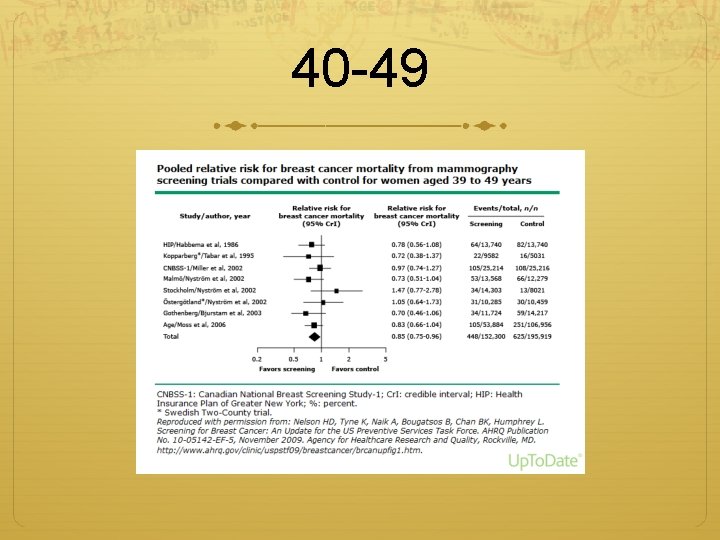
Breast cancer screening 40 -49 “A systematic review and meta-analysis of eight randomized trials found a 15 percent reduction of breast cancer mortality in women ages 39 to 48 who were randomly assigned to mammographic screening (RR 0. 85, 95% CI 0. 750. 96)”

40 -49

40 -49

50 -65 Men Colon Cancer: all men should start screening at age 50. Prostate cancer: discuss risks and possible benefits of testing. Lung Cancer screening with annual low dose CT chest. Age ACS: 55 -70, USPSTF: 55 -80 Current or previous smoker (quit within last 15 years) Total of 30 pack year smoking history USPSTF recommends stop when quit 15 or more years ago or limited life expectancy. LEVEL B RECOMMENDATION

50 -65 Women Breast cancer ACS: annual clinical breast exam and mammogram USPSTF: mammography every other year Cervical cancer PAP q 3 or PAP + HPV q 5 Stop age 65 if “adequate” 10 years normal testing Screen 20 years if CIN 2 or greater found, up to age 80 with good life exp If inadequate testing, offer screening up to about age 70 -75 Colon cancer age 50 Lung cancer age 55 with same risk factors.

Colon Cancer Screening LOTS of different but similar recommendations. Up. To. Date summarizes them well. Guidelines provided by… American Cancer Society (ACS) USPSTF National Comprehensive Cancer Network (NCCN) ACP American College of Gastroenterology (ACG)

Colon Cancer Screening Tools Flexible sigmoidoscopy Colonoscopy Double contrast barium enema (poor sens/spec and not recommended) CT colonography Annual FOBT (32% mortality benefit) Annual fecal immunochemical test “FIT” Stool DNA (s. DNA)

Comparison Stool Guiac: low sn and sp for significant dz, both true and false + are worked up with colonoscopy FIT: Better sn, similar sp to guiac. More expensive Stool DNA: looking for DNA mutations associated with cancer. Better sn than FIT, less sp than FIT. Study in 2014: FIT vs s. DNA vs Colonoscopy Number of screenings to detect 1 cancer: FIT: 208 s. DNA: 166 Colonoscopy: 154

Comparison Double barium cont. enema: falling out of favor, requires technical expertese, only detects ½ of large polyps >1 cm. Flex sig: only inspects distal 60 cm of colon. Distal pathology may require colonoscopy. Less prep required. Colonoscopy: Highest sn and sp of all tests currently. Risks include perforation, bleeding. CT colonoscopy: no sedation or perforation risk. + tests require colonoscopy Radiation increases risk for cancer.

Colon Cancer Screening American Cancer Society- Multi-Society Task Force (ACS-MSTF) guidelines: Start age 50 average risk individuals Discontinue when life expectancy <10 years No single test recommended, discuss with patient, participation with screening is important. Colonoscopy q 10 years CT colon q 5 years Flex sig q 5 FOBT (sensitive) annually FIT annually

Colon Cancer Screening USPSTF guidelines: Screen average risk adults 50 -75 FOBT annually (sensative) Flex sig q 5 years with FOBT q 3 Colonoscopy q 10 years

>65 years old Colon: stop age 75 or when life exp. <10 years. Lung: Annual low dose CT in high risk groups. choose guidelines for age range ACS: 55 -70, USPSTF: 55 -80 Men: consider prostate Women: Breast: ACS: Annual Mammography, no specific recommendations on age to stop USPSTF: Biennial mammography up to age 74, insufficient evidence >75. ACR: stop when life exp <5 -7 years ACOG: women >75 discuss with doctor whether to continue. Cervical : most stop age 65, offer up to 75 if inadequate testing.

References Cervical Cancer Screening Guidelines. USPSTF. http: //www. uspreventiveservicestaskforce. org/Page/Topic/recommendation-summary/cervicalcancer-screening? ds=1&s=cervical cancer screening. Accessed February 28, 2015. American Cancer Society. The History of Cancer. org. June 2014. Available at URL. http: //www. cancer. org/acs/groups/cid/documents/webcontent/002048 -pdf. Accessed March 30, 2015 Efficacy of human papillomavirus testing for the detection of invasive cervical cancers and cervical intraepithelial neoplasia: a randomised controlled trial. Ronco G, Giorgi-Rossi P, Carozzi F, Confortini M, Dalla Palma P, Del Mistro A, Ghiringhello B, Girlando S, Gillio-Tos A, De Marco L, Naldoni C, Pierotti P, Rizzolo R, Schincaglia P, Zorzi M, Zappa M, Segnan N, Cuzick J, New Technologies for Cervical Cancer screening (NTCC) Working Group. Lancet Oncol. 2010; 11(3): 249. Efficacy of HPV-based screening for prevention of invasive cervical cancer: follow-up of four European randomised controlled trials. Ronco G, Dillner J, Elfström KM, Tunesi S, Snijders PJ, Arbyn M, Kitchener H, Segnan N, Gilham C, Giorgi-Rossi P, Berkhof J, Peto J, Meijer CJ, International HPV screening working group. Lancet. 2014; 383(9916): 524. Screening for breast cancer: an update for the U. S. Preventive Services Task Force. Nelson HD, Tyne K, Naik A, Bougatsos C, Chan BK, Humphrey L, U. S. Preventive Services Task Force. Ann Intern Med. 2009; 151(10): 727. US Preventative Service Task Force. USPSTF. www. uspreventativeservicetaskforce. org/page/Topic/recommendation-summary. Accessed April 1, 2015 Up. To. Date Image 1 http: //jackiekazik. tumblr. com/post/52187458630/strabismus-and-amblyopia

References cont. Image 2 http: //www. aapos. org/terms/conditions/93 Image 3 http: //www. uspreventiveservicestaskforce. org/Page/Name/grade-definitions Image 4 and 5 http: //www. my-breast-cancer-guide. com/mammogram-jokes. html Image 6 http: //ultimate-radiology. blogspot. com/2013/09/case-of-ca-lung. html Image 7 http: //www. greateratlantic. fisheries. noaa. gov/nero/fishermen/images/redcrab 1. jpg Image 8 http: //www. livescience. com/21213 -leading-causes-of-death-in-the-u-s-since-1900 -infographic. html Image 9 http: //commonhealth. wbur. org/tag/prostate-cancer Image 10 http: //info. cancerresearchuk. org/cancerstats/incidence/age/

Questions?