Affordable Care Act and American Health Care Act

Affordable Care Act and American Health Care Act Overview June 16, 2017 Medical Administrators Conference Diane Rowland, Sc. D. Executive Vice President, Kaiser Family Foundation Karen Pollitz Senior Fellow, Kaiser Family Foundation
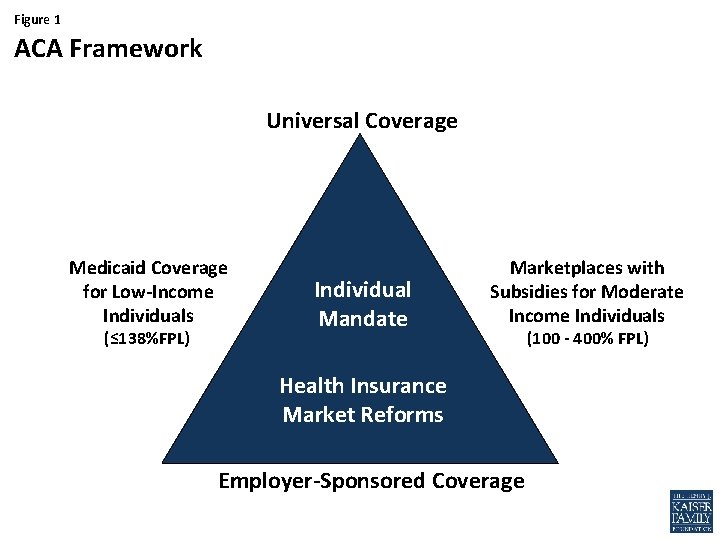
Figure 1 ACA Framework Universal Coverage Medicaid Coverage for Low-Income Individuals (≤ 138%FPL) Individual Mandate Marketplaces with Subsidies for Moderate Income Individuals Health Insurance Market Reforms Employer-Sponsored Coverage (100 - 400% FPL)
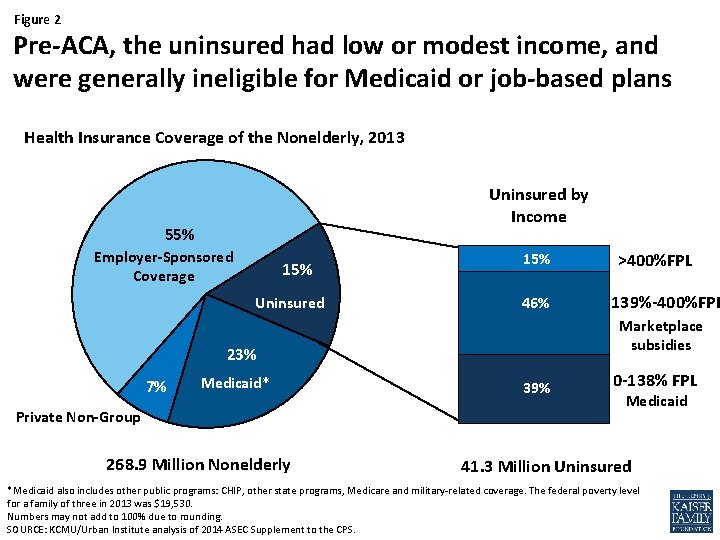
Figure 2 Pre-ACA, the uninsured had low or modest income, and were generally ineligible for Medicaid or job-based plans Health Insurance Coverage of the Nonelderly, 2013 Uninsured by Income 55% Employer-Sponsored Coverage 15% Uninsured 15% 46% Medicaid* Private Non-Group 268. 9 Million Nonelderly 139%-400%FPL Marketplace subsidies 23% 7% >400%FPL 39% 0 -138% FPL Medicaid 41. 3 Million Uninsured *Medicaid also includes other public programs: CHIP, other state programs, Medicare and military-related coverage. The federal poverty level for a family of three in 2013 was $19, 530. Numbers may not add to 100% due to rounding. SOURCE: KCMU/Urban Institute analysis of 2014 ASEC Supplement to the CPS.
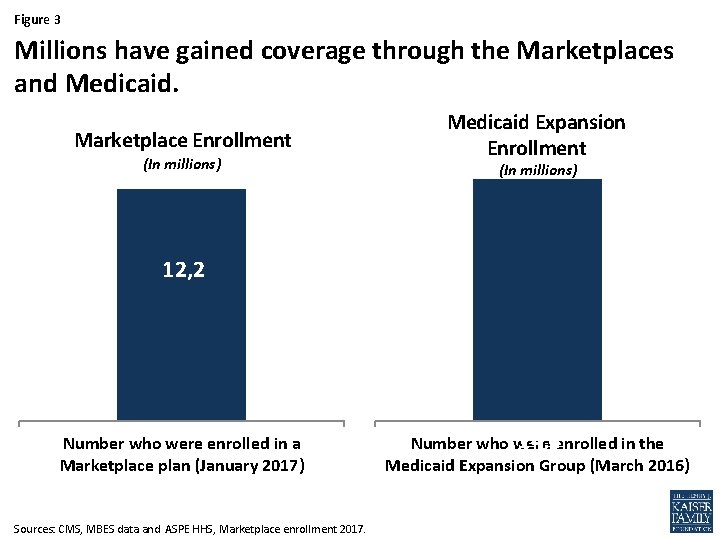
Figure 3 Millions have gained coverage through the Marketplaces and Medicaid. Marketplace Enrollment (In millions) Medicaid Expansion Enrollment (In millions) 12, 2 Number who were enrolled in a Marketplace plan (January 2017) Sources: CMS, MBES data and ASPE HHS, Marketplace enrollment 2017. 14, 4 enrolled in the Number who were Medicaid Expansion Group (March 2016)
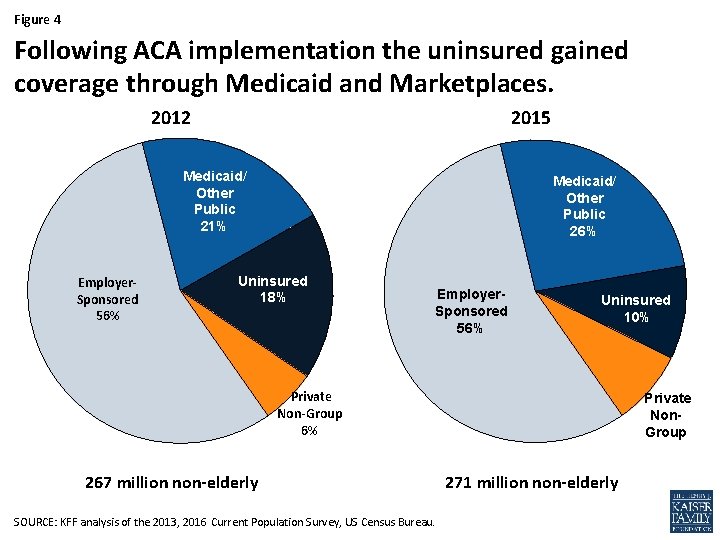
Figure 4 Following ACA implementation the uninsured gained coverage through Medicaid and Marketplaces. 2012 2015 Medicaid/ Other Public 21% Employer. Sponsored 56% Medicaid/ Other Public 26% Uninsured 18% Employer. Sponsored 56% Uninsured 10% Private Non-Group 6% 267 million non-elderly SOURCE: KFF analysis of the 2013, 2016 Current Population Survey, US Census Bureau. Private Non. Group 271 million non-elderly
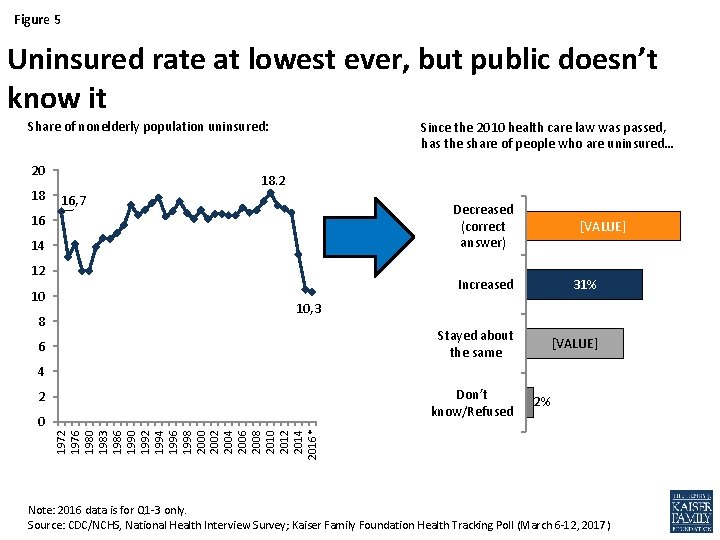
Figure 5 Uninsured rate at lowest ever, but public doesn’t know it Share of nonelderly population uninsured: 20 18 Since the 2010 health care law was passed, has the share of people who are uninsured… 18. 2 16, 7 Decreased (correct answer) 16 14 12 10 8 [VALUE] Increased 31% Stayed about the same [VALUE] 10, 3 6 4 Don’t know/Refused 0 2% 1972 1976 1980 1983 1986 1990 1992 1994 1996 1998 2000 2002 2004 2006 2008 2010 2012 2014 2016* 2 Note: 2016 data is for Q 1 -3 only. Source: CDC/NCHS, National Health Interview Survey; Kaiser Family Foundation Health Tracking Poll (March 6 -12, 2017)

Figure 6 Key elements of the American Health Care Act passed by the House • Repeal of almost all ACA tax increases (Cadillac plan tax remains but delayed until 2025). • Scaled back Medicaid expansion and per capita cap on federal funding. • Repeal of the individual and employer mandates. • Federal grants for state high-risk pools or other stabilization mechanisms. • Refundable tax credits that vary by age, but not income or local premiums (phasing out above income of $75 k for individuals). • Guaranteed access to insurance for people with pre-existing conditions, with late enrollment penalties for people with gaps in coverage. • Continuation of the ACA’s required insurance benefits. • 5 -1 variation in premiums allowed for age. • Mac. Arthur/Upton amendments: State waivers for the essential benefits and community rating (with $8 billion over five years in grants to states).

Figure 7 AHCA by the numbers* • Reduce Federal revenue by $1 trillion over 10 years • Reduce Federal health spending by more than $1 trillion over 10 years, including – $834 billion in Medicaid outlays – $192 billion in reduced premium subsidies for individual market – $98 billion from repeal of cost sharing subsidies for individual market • Patient and State Stability Fund provides $138 billion/9 years to offset impacts – – $15 billion earmarked for federal reinsurance (invisible high risk program)/9 years $15 billion earmarked for maternity/mental health/substance abuse services (2020 only) $100 billion for high-risk pools, reinsurance, cost sharing help, pay providers, other options $8 billion/5 years to help people subject to health status rating in waiver states • Net deficit reduction of $119 billion over 10 years • CBO estimates number of uninsured individuals will grow by 23 million to 51 million (19% of nonelderly population) by 2026 – 14 million lose Medicaid, 9 million lose private coverage * Congressional Budget Office estimates May 24, 2017

Figure 8 The Medicaid Saga
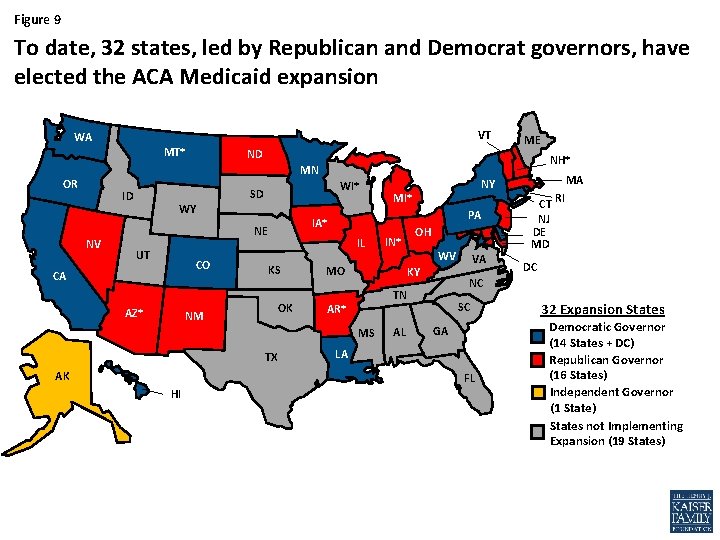
Figure 9 To date, 32 states, led by Republican and Democrat governors, have elected the ACA Medicaid expansion VT WA MT* ND NH* MN OR NV WI* SD ID WY CO CA AZ* PA IL KS OK NM AK IN* MO OH WV KY AR* AL VA SC GA LA FL HI MA CT RI NJ DE MD DC NC TN MS TX NY MI* IA* NE UT ME 32 Expansion States Democratic Governor (14 States + DC) Republican Governor (16 States) Independent Governor (1 State) States not Implementing Expansion (19 States)
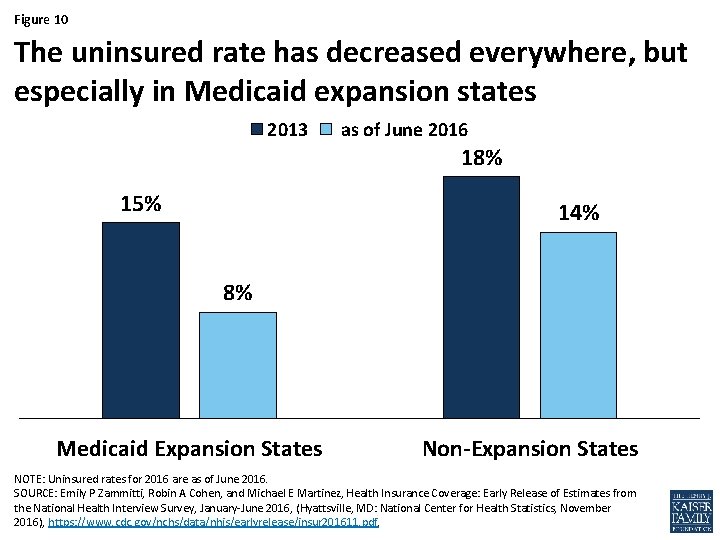
Figure 10 The uninsured rate has decreased everywhere, but especially in Medicaid expansion states 2013 as of June 2016 18% 15% 14% 8% Medicaid Expansion States Non-Expansion States NOTE: Uninsured rates for 2016 are as of June 2016. SOURCE: Emily P Zammitti, Robin A Cohen, and Michael E Martinez, Health Insurance Coverage: Early Release of Estimates from the National Health Interview Survey, January-June 2016, (Hyattsville, MD: National Center for Health Statistics, November 2016), https: //www. cdc. gov/nchs/data/nhis/earlyrelease/insur 201611. pdf.

Figure 11 Key Medicaid Provisions of the AHCA • Phases-out Medicaid Expansion – Ends enhanced match 1/1/2020 for expansion adults – Grandfathers continuously enrolled expansion adults with higher match • Converts full Medicaid program to capped financing in 2020 – Ends open-ended federal financing to limit federal spending – Establishes person spending cap by eligibility group: children, disabled, elderly, expansion adults, and other adults based on 2016 spending – Amounts increased over time by an inflation factor – States have option for block grant for children and adults • Safety Net Pool for non-expansion states – $10 billion for 2018 -2022 and eliminates DSH cuts • Eliminates Medicaid funding for family planning
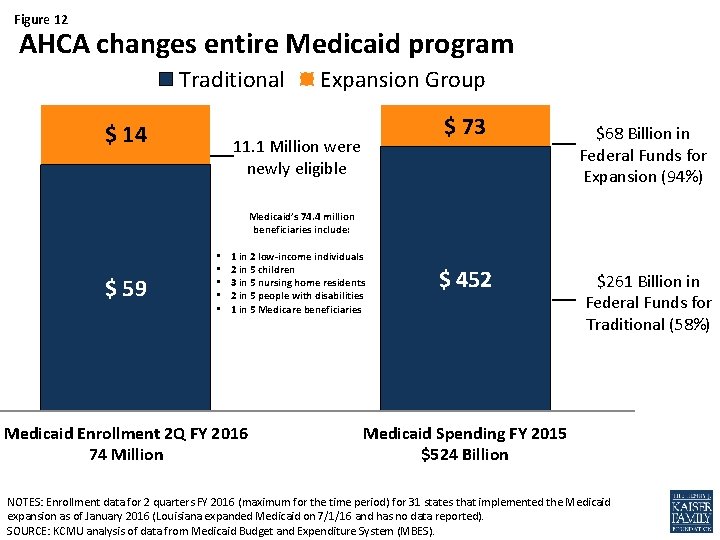
Figure 12 AHCA changes entire Medicaid program Traditional $ 14 Expansion Group $ 73 11. 1 Million were newly eligible $68 Billion in Federal Funds for Expansion (94%) Medicaid’s 74. 4 million beneficiaries include: $ 59 • • • 1 in 2 low-income individuals 2 in 5 children 3 in 5 nursing home residents 2 in 5 people with disabilities 1 in 5 Medicare beneficiaries Medicaid Enrollment 2 Q FY 2016 74 Million $ 452 $261 Billion in Federal Funds for Traditional (58%) Medicaid Spending FY 2015 $524 Billion NOTES: Enrollment data for 2 quarters FY 2016 (maximum for the time period) for 31 states that implemented the Medicaid expansion as of January 2016 (Louisiana expanded Medicaid on 7/1/16 and has no data reported). SOURCE: KCMU analysis of data from Medicaid Budget and Expenditure System (MBES).
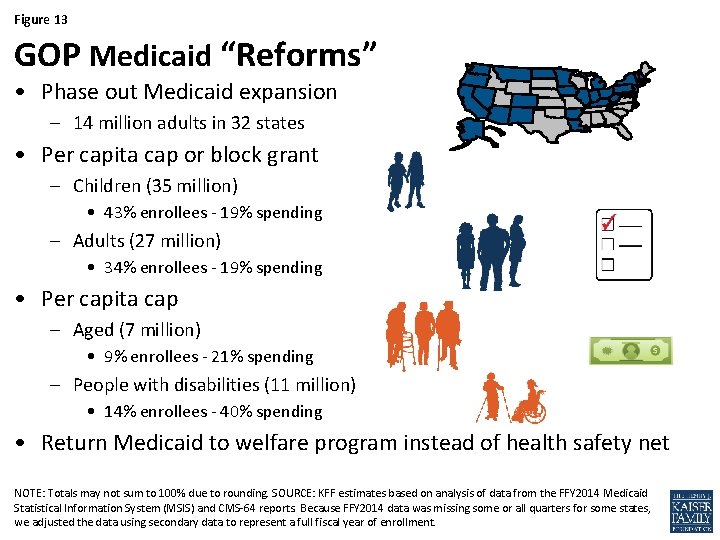
Figure 13 GOP Medicaid “Reforms” • Phase out Medicaid expansion – 14 million adults in 32 states • Per capita cap or block grant – Children (35 million) • 43% enrollees - 19% spending – Adults (27 million) • 34% enrollees - 19% spending • Per capita cap – Aged (7 million) • 9% enrollees - 21% spending – People with disabilities (11 million) • 14% enrollees - 40% spending • Return Medicaid to welfare program instead of health safety net NOTE: Totals may not sum to 100% due to rounding. SOURCE: KFF estimates based on analysis of data from the FFY 2014 Medicaid Statistical Information System (MSIS) and CMS-64 reports. Because FFY 2014 data was missing some or all quarters for some states, we adjusted the data using secondary data to represent a full fiscal year of enrollment.
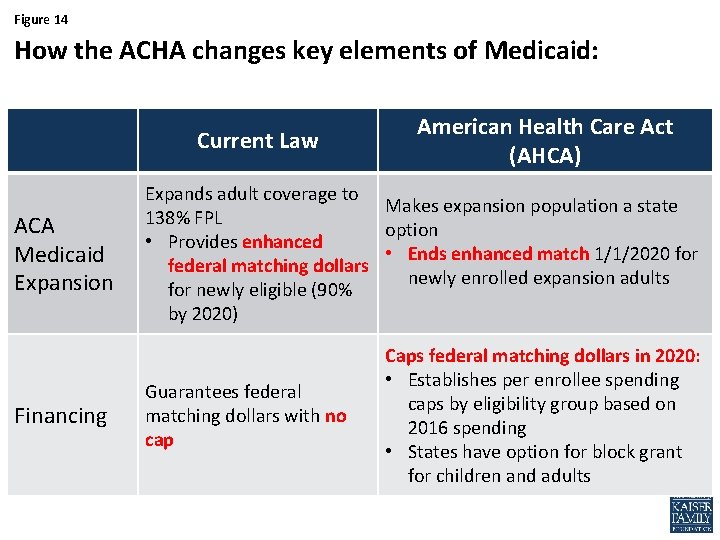

Figure 14 How the ACHA changes key elements of Medicaid: Current Law ACA Medicaid Expansion Financing American Health Care Act (AHCA) Expands adult coverage to Makes expansion population a state 138% FPL option • Provides enhanced • Ends enhanced match 1/1/2020 for federal matching dollars newly enrolled expansion adults for newly eligible (90% by 2020) Guarantees federal matching dollars with no cap Caps federal matching dollars in 2020: • Establishes per enrollee spending caps by eligibility group based on 2016 spending • States have option for block grant for children and adults
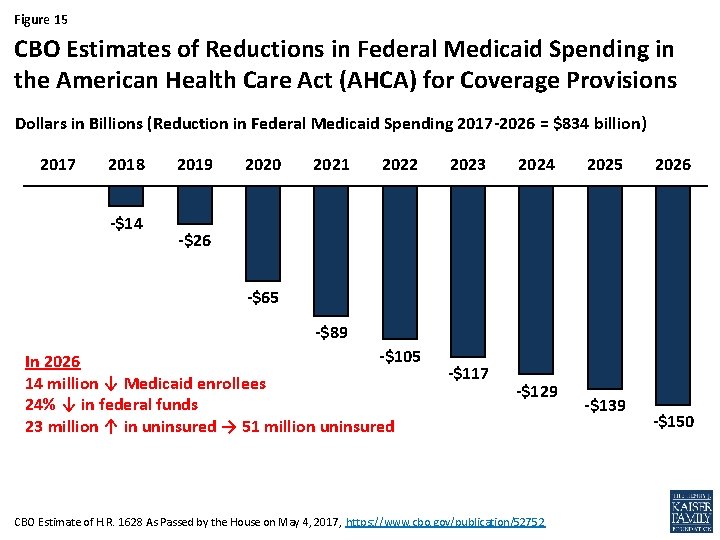
Figure 15 CBO Estimates of Reductions in Federal Medicaid Spending in the American Health Care Act (AHCA) for Coverage Provisions Dollars in Billions (Reduction in Federal Medicaid Spending 2017 -2026 = $834 billion) 2017 2018 -$14 2019 2020 2021 2022 2023 2024 2025 2026 -$65 -$89 -$105 In 2026 14 million ↓ Medicaid enrollees 24% ↓ in federal funds 23 million ↑ in uninsured → 51 million uninsured -$117 -$129 CBO Estimate of H. R. 1628 As Passed by the House on May 4, 2017, https: //www. cbo. gov/publication/52752 -$139 -$150
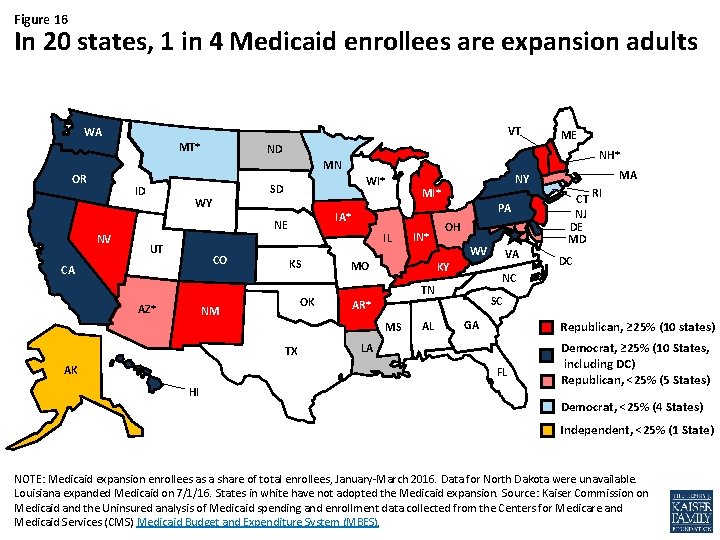
Figure 16 In 20 states, 1 in 4 Medicaid enrollees are expansion adults VT WA MT* ND NH* MN OR NV WI* SD ID WY UT CO CA AZ* PA IL KS OK NM AK IN* MO OH WV KY GA DC Republican, ≥ 25% (10 states) LA FL HI CT RI NJ DE MD SC AR* AL VA MA NC TN MS TX NY MI* IA* NE ME Democrat, ≥ 25% (10 States, including DC) Republican, <25% (5 States) Democrat, <25% (4 States) Independent, <25% (1 State) NOTE: Medicaid expansion enrollees as a share of total enrollees, January-March 2016. Data for North Dakota were unavailable. Louisiana expanded Medicaid on 7/1/16. States in white have not adopted the Medicaid expansion. Source: Kaiser Commission on Medicaid and the Uninsured analysis of Medicaid spending and enrollment data collected from the Centers for Medicare and Medicaid Services (CMS) Medicaid Budget and Expenditure System (MBES).
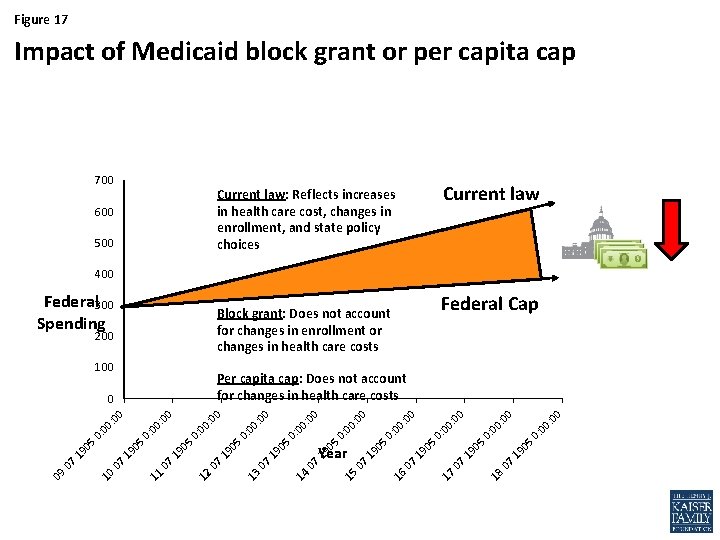
Figure 17 Impact of Medicaid block grant or per capita cap 700 Current law: Reflects increases in health care cost, changes in enrollment, and state policy choices 600 500 400 Federal 300 Spending 200 100 0 0 : 0 00 0: 05 05 . 1 9. 0 7 18 17 . 0 7 . 1 9 05. 1 9. 0 7 16 00 : 0 00 0: 05. 1 9 . 0 7 15 0 0 00 : 0 00 0: 05 . 1 9 Year . 0 7 14 : 0 0 0 : 0 0: 05 . 1 9. 0 7 13 . 1 9. 0 7 12 00 : 0 0: 05. 1 9 . 0 7 11 00 : 0 00 00 0: 05 . 1 9. 0 7 10 0 0 : 0 00 0: 05. 1 9. 0 7 0 Per capita cap: Does not account for changes in health care costs 0 09 Federal Cap Block grant: Does not account for changes in enrollment or changes in health care costs

Figure 18 Reducing federal funds through per capita cap or block grant: • Shifts costs and risks to states, beneficiaries, and providers if states restrict eligibility, benefits, and provider payment • Locks in historic spending patterns – If expansion funding is cut, the impact could be even greater for the 32 states that expanded Medicaid • Limits states’ ability to respond to rising health care costs, increases in enrollment due to a recession, or a public health emergency such as the opioid epidemic, HIV, Zika, etc. • Leads to more low income uninsured Americans

Figure 19 Medicaid policy choices place some states at higher risk with federal Medicaid cuts or caps and could lock in historic decisions. Low Eligibility for Parents Low Physician Fee Index High MCO Penetration Low Share of Community. Based LTC Care Alabama Rhode Island Tennessee Mississippi Texas New Jersey Hawaii Indiana Missouri Michigan Iowa Florida Idaho California New Hampshire Michigan Mississippi Missouri Kansas Louisiana NOTE: States in multiple categories are shown in orange.

Figure 20 What is the Senate debating? • The structure of how Medicaid is financed • The size of the proposed cuts and impact on states • The impact and timing of the phase out of the Medicaid expansion for 32 states • Treatment of expansion vs non-expansion states • Setting payment rates by state to adjust for state variations • The impact of these changes on Medicaid’s 74 million beneficiaries (14 M expansion/60 M traditional) • The provisions allowed under Byrd

Figure 21 Looking Ahead • Pressure to finish health care in order to move on to other priorities, including tax reform • Deep divide among Senate Republicans on level of savings and treatment of Medicaid and Medicaid expansion • Many Republican-led states (16) have expanded Medicaid, and many Governors have expressed concern about capped federal financing for Medicaid and AHCA • Administration plans additional changes – Trump budget calls for additional $610 billion over AHCA cuts from 2018 -2027 – Waivers will also reshape coverage – Regulatory changes on managed care and benefits likely

Figure 22 The Marketplace Saga

Figure 23 ACA transformed non-group health insurance market • Discrimination based on health status prohibited – Pre-ACA, insurers denied coverage, charged more based on health status, excluded coverage for pre-existing conditions • Policies redefined to provide major medical coverage (EHB, OOP limits) – Pre-ACA, insurance defined as anything sold by licensed health insurer; exclusions, coverage limits, “mini-meds” were common • Individual mandate – Pre-ACA, voluntary coverage made insurers fear adverse selection • Subsidize premiums (to 400% FPL) and cost sharing (to 250% FPL) – Pre-ACA, non-group coverage unsubsidized. 90% of uninsured had income <400% FPL; 75% of uninsured had income <250% FPL • New Marketplaces deliver subsidies, provide standard comparison info and inperson help to consumers – Pre-ACA, lack of transparency in insurance, help through brokers/insurance sales force.

Figure 24 Transition to reformed market challenging in 2014 -2016 • • Early years of ACA implementation were difficult transition Insurers adopted an entirely new business model, faced new competition Many insurers underpriced policies in early years to gain market share Average 2014 premiums much lower than predicted 2017 premium increases largely corrected for previous under-pricing Most enrollees eligible for subsidies, shielded from 2017 rate increases Market enrollment grew 50% from pre-ACA and holding steady Industry experts confirm insurers are getting the hang of new ACA market* – The U. S. ACA individual market shows signs of improvement, as most insurers' 2016 results were better than 2015 results. – But the market is still developing and will need a couple more years to reach target profitability. • The ACA individual market is not in a "death spiral“ * S&P Global, “The US ACA Individual Market Showed Progress in 2016, but Still Needs Time to Mature, ” April 7, 2017
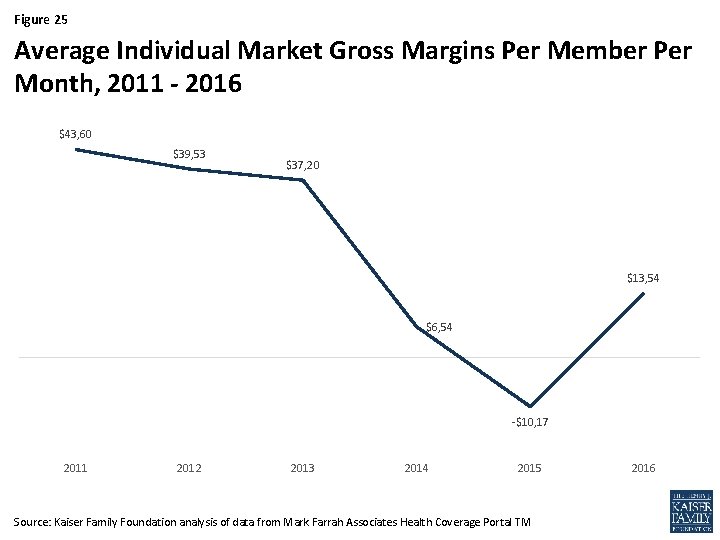
Figure 25 Average Individual Market Gross Margins Per Member Per Month, 2011 - 2016 $43, 60 $39, 53 $37, 20 $13, 54 $6, 54 -$10, 17 2011 2012 2013 2014 2015 Source: Kaiser Family Foundation analysis of data from Mark Farrah Associates Health Coverage Portal TM 2016
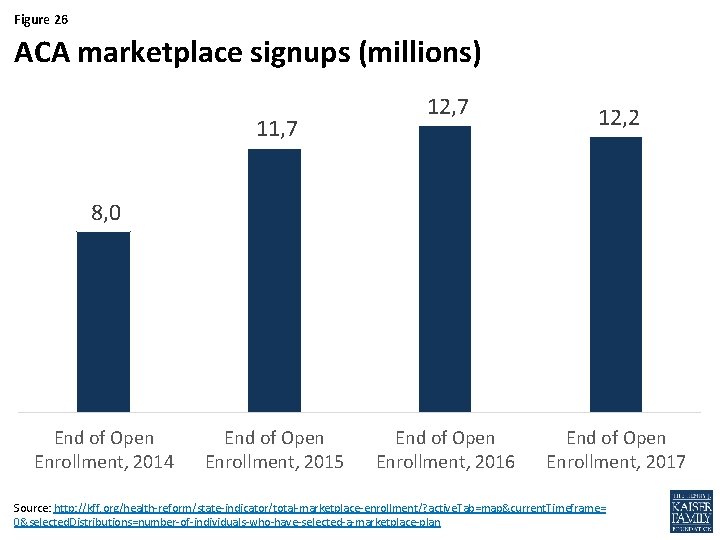
Figure 26 ACA marketplace signups (millions) 11, 7 12, 2 8, 0 End of Open Enrollment, 2014 End of Open Enrollment, 2015 End of Open Enrollment, 2016 End of Open Enrollment, 2017 Source: http: //kff. org/health-reform/state-indicator/total-marketplace-enrollment/? active. Tab=map¤t. Timeframe= 0&selected. Distributions=number-of-individuals-who-have-selected-a-marketplace-plan
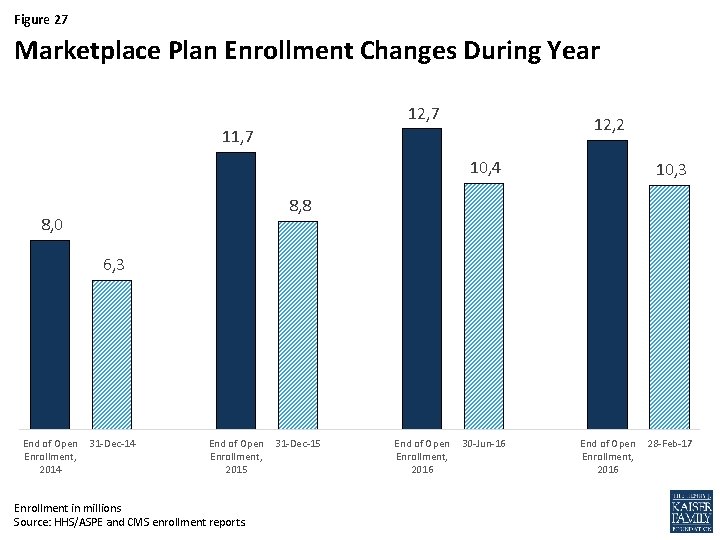
Figure 27 Marketplace Plan Enrollment Changes During Year 12, 7 12, 2 11, 7 10, 4 10, 3 8, 8 8, 0 6, 3 End of Open Enrollment, 2014 31 -Dec-14 End of Open Enrollment, 2015 Enrollment in millions Source: HHS/ASPE and CMS enrollment reports. 31 -Dec-15 End of Open Enrollment, 2016 30 -Jun-16 End of Open Enrollment, 2016 28 -Feb-17
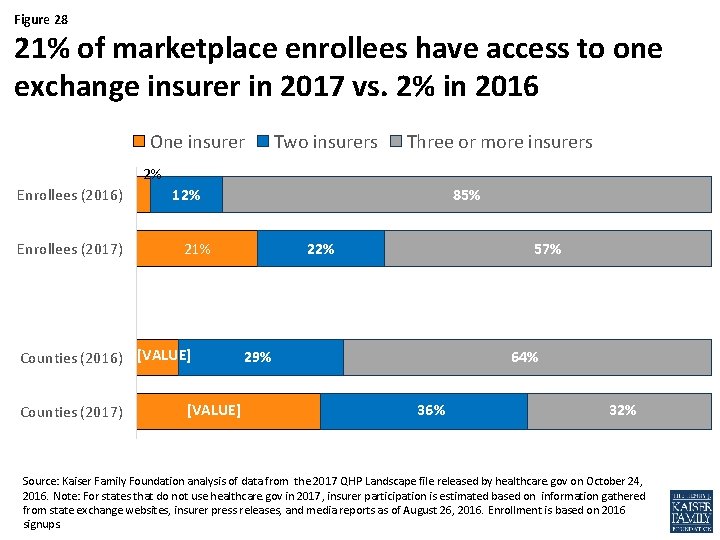
Figure 28 21% of marketplace enrollees have access to one exchange insurer in 2017 vs. 2% in 2016 One insurer Two insurers Three or more insurers 2% Enrollees (2016) Enrollees (2017) 12% 21% Counties (2016) [VALUE] Counties (2017) 85% [VALUE] 22% 57% 29% 64% 36% 32% Source: Kaiser Family Foundation analysis of data from the 2017 QHP Landscape file released by healthcare. gov on October 24, 2016. Note: For states that do not use healthcare. gov in 2017, insurer participation is estimated based on information gathered from state exchange websites, insurer press releases, and media reports as of August 26, 2016. Enrollment is based on 2016 signups.

Figure 29 In selected areas in 2017, other factors impacted market competition and stability • “Risk scores” highest in areas that did not expand Medicaid • In states that extended “grandmothered” plans (pre-2014, underwritten), profitability of ACA compliant plans is lower • In rural areas with sparse population, it is especially hard for multiple insurers to compete • Even pre-ACA, a single health insurer held majority market share in most states • Midstream changes to ACA introduced added challenges: • Congressional cuts to ACA Risk Corridor program cut payments expected by many insurers • As result, prior to 2016 election, some insurers in some areas decided to exit marketplaces in 2017 Source: http: //www. kff. org/health-reform/issue-brief/data-note-effect-of-state-decisions-on-state-risk-scores/
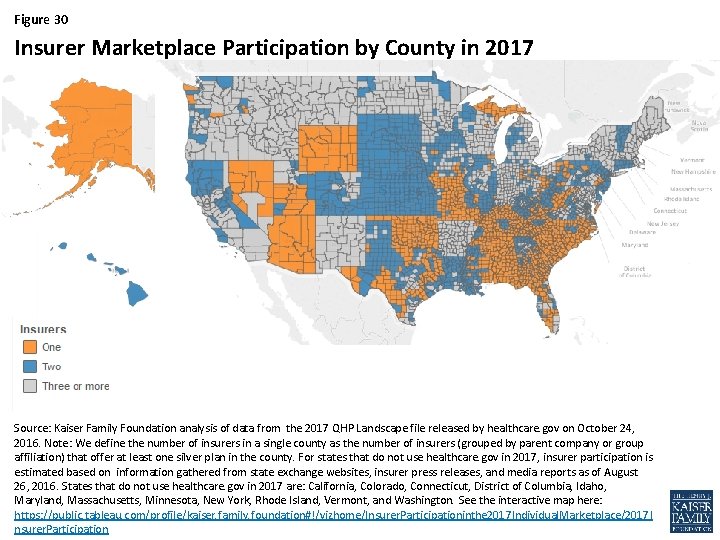
Figure 30 Insurer Marketplace Participation by County in 2017 Source: Kaiser Family Foundation analysis of data from the 2017 QHP Landscape file released by healthcare. gov on October 24, 2016. Note: We define the number of insurers in a single county as the number of insurers (grouped by parent company or group affiliation) that offer at least one silver plan in the county. For states that do not use healthcare. gov in 2017, insurer participation is estimated based on information gathered from state exchange websites, insurer press releases, and media reports as of August 26, 2016. States that do not use healthcare. gov in 2017 are: California, Colorado, Connecticut, District of Columbia, Idaho, Maryland, Massachusetts, Minnesota, New York, Rhode Island, Vermont, and Washington. See the interactive map here: https: //public. tableau. com/profile/kaiser. family. foundation#!/vizhome/Insurer. Participationinthe 2017 Individual. Marketplace/2017 I nsurer. Participation

Figure 31 For 2018, new uncertainty worries insurers in all states • “Every time something new (and potentially disruptive) is thrown into the works, it impedes the individual market's path to stability. ”* • Anthem BCBS of Ohio recently announced exiting 20 counties in 2018 – "A stable insurance market is dependent on products that create value for consumers through the broad spreading of risk and a known set of conditions upon which rates can be developed…Today, planning and pricing for ACA-compliant health plans has become increasingly difficult due to the shrinking individual market as well as continual changes in federal operations, rules and guidance. “ • Will cost sharing reduction (CSR) payments continue? – Estimated cost is $10 billion in 2018; To recoup losses and remain in marketplace, insurers would need to increase premiums 19% • Will the individual mandate be enforced? – CBO estimates repeal of mandate, alone, could increase premiums 20% • How will the next Open Enrollment Period be conducted? – Administration cancelled outreach, advertising for final days of OE 4 – OE 5 will be shortened from 12 weeks to 6 weeks – ACA described as “horrible health care, ” “collapsing, ” “a disaster” * S&P Global, “The US ACA Individual Market Showed Progress in 2016, but Still Needs Time to Mature, ” April 7, 2017

Figure 32 President Trump: “Insurance for everybody…Much less expensive and much better…Much lower deductibles. ” Washington Post, January 15, 2017

Figure 33 Key Private Insurance Provisions in AHCA • Repeal individual and employer mandate • Retain most ACA market rules/health plan standards – Guaranteed issue – Modified community rating, with changes: • Age rating 5: 1 • Late enrollment penalty = 30% premium surcharge • State waivers – Pre-ex exclusion periods prohibited – Essential health benefits for individual/small group market (state waivers) – Lifetime annual limits prohibited (for essential health benefits) – Limits on annual OOP cost sharing (metal tiers sunset 2020) • Repeal/replace ACA subsidies – Total subsidies reduced 40% on average in 2020, 50% on average by 2026; deeper cuts for lowincome, older adults, residents of high cost areas – Premium subsidies now based on income, age, health plan cost, geography will be replaced by flat tax credits based on age ($2, 000 -$4, 000) – No tax credit for plans that cover abortion – Cost sharing subsidies repealed • State waivers for EHB; community rating for people with coverage gap • New Patient State Stability Fund ($138 billion over 9 years)
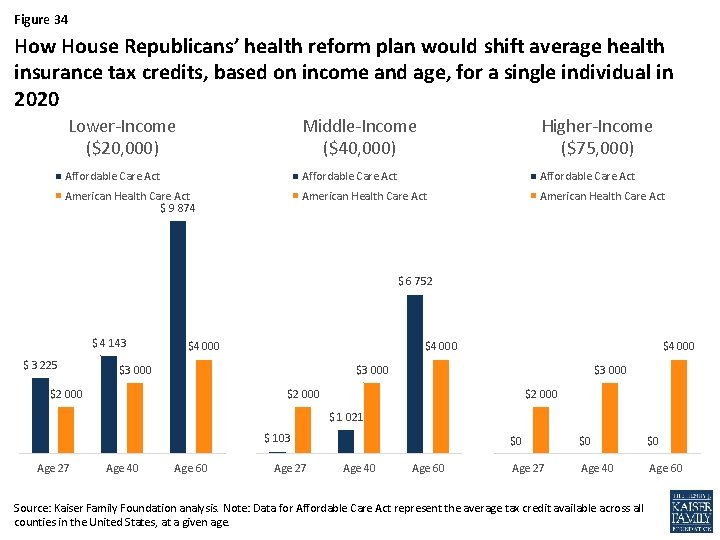
Figure 34 How House Republicans’ health reform plan would shift average health insurance tax credits, based on income and age, for a single individual in 2020 Lower-Income ($20, 000) Middle-Income ($40, 000) Higher-Income ($75, 000) Affordable Care Act American Health Care Act $ 9 874 American Health Care Act $ 6 752 $ 4 143 $ 3 225 $4 000 $3 000 $2 000 $ 1 021 $ 103 Age 27 Age 40 Age 60 $0 $0 $0 Age 27 Age 40 Age 60 Source: Kaiser Family Foundation analysis. Note: Data for Affordable Care Act represent the average tax credit available across all counties in the United States, at a given age.
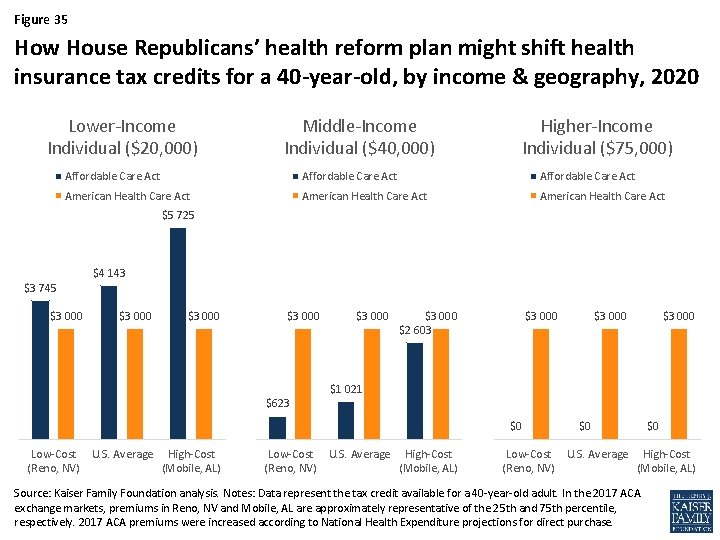
Figure 35 How House Republicans’ health reform plan might shift health insurance tax credits for a 40 -year-old, by income & geography, 2020 Lower-Income Individual ($20, 000) Middle-Income Individual ($40, 000) Higher-Income Individual ($75, 000) Affordable Care Act American Health Care Act $5 725 $4 143 $3 745 $3 000 $3 000 $2 603 $3 000 $1 021 $623 $0 Low-Cost U. S. Average High-Cost (Reno, NV) (Mobile, AL) $0 $0 Low-Cost U. S. Average High-Cost (Reno, NV) (Mobile, AL) Source: Kaiser Family Foundation analysis. Notes: Data represent the tax credit available for a 40 -year-old adult. In the 2017 ACA exchange markets, premiums in Reno, NV and Mobile, AL are approximately representative of the 25 th and 75 th percentile, respectively. 2017 ACA premiums were increased according to National Health Expenditure projections for direct purchase.
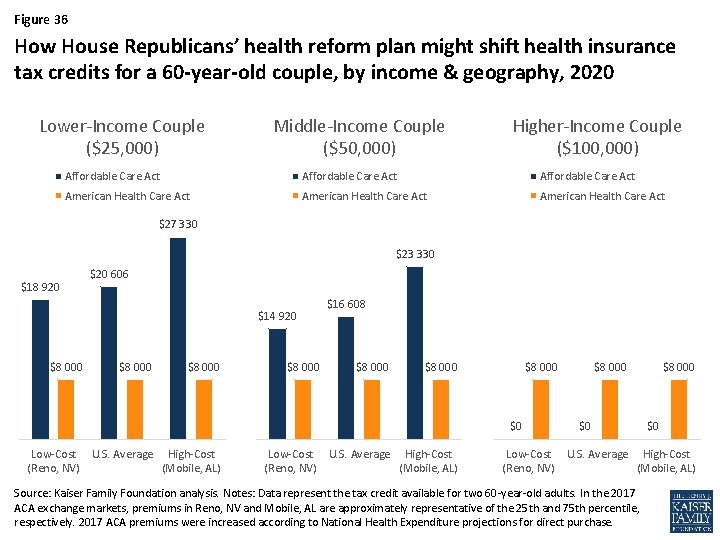
Figure 36 How House Republicans’ health reform plan might shift health insurance tax credits for a 60 -year-old couple, by income & geography, 2020 Lower-Income Couple ($25, 000) Middle-Income Couple ($50, 000) Higher-Income Couple ($100, 000) Affordable Care Act American Health Care Act $27 330 $23 330 $18 920 $20 606 $14 920 $8 000 $16 608 $8 000 $0 Low-Cost U. S. Average High-Cost (Reno, NV) (Mobile, AL) $8 000 $0 Low-Cost U. S. Average High-Cost (Reno, NV) (Mobile, AL) Source: Kaiser Family Foundation analysis. Notes: Data represent the tax credit available for two 60 -year-old adults. In the 2017 ACA exchange markets, premiums in Reno, NV and Mobile, AL are approximately representative of the 25 th and 75 th percentile, respectively. 2017 ACA premiums were increased according to National Health Expenditure projections for direct purchase.
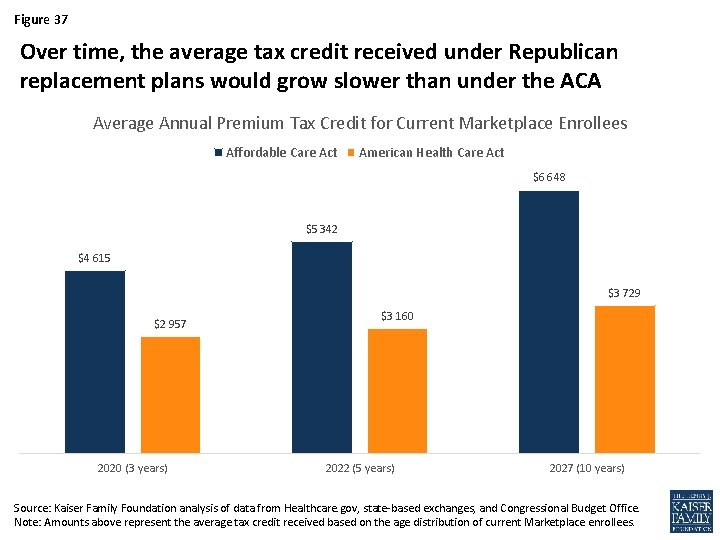
Figure 37 Over time, the average tax credit received under Republican replacement plans would grow slower than under the ACA Average Annual Premium Tax Credit for Current Marketplace Enrollees Affordable Care Act American Health Care Act $6 648 $5 342 $4 615 $3 729 $2 957 2020 (3 years) $3 160 2022 (5 years) 2027 (10 years) Source: Kaiser Family Foundation analysis of data from Healthcare. gov, state-based exchanges, and Congressional Budget Office. Note: Amounts above represent the average tax credit received based on the age distribution of current Marketplace enrollees.

Figure 38 Impact on individual health insurance market? • Premiums expected to rise 15 -20% per year in 2018 -2019 due to mandate repeal • From 2020 -2026, nongroup premiums expected to fall 10% below baseline – Stability Fund used primarily for reinsurance, lowering average premiums – Combination of higher age rating and lower age-adjusted premium subsidies causes disproportionate coverage loss among older adults; remaining market participants younger on average, lowering average premiums – Repeal of “metal levels” will raise deductibles generally, lowering average premiums • CBO estimates 14 million will lose/leave individual health insurance by 2026 • Will states elect EHB waivers? – Average premiums will decline if policies cover less – People who need medical services could be underinsured; mini-meds re-emerge • Will states elect community rating waivers/health status rating for break in coverage? – 27 million people experienced gap in coverage in 2015 – 6. 3 million (23%) had “declinable” pre-existing conditions

Figure 39 What is the Senate debating? • Under Senate rules, Senate bill must achieve at least as much deficit reduction as the House bill • News reports suggest AHCA is starting point, with modifications likely – More modest cuts in private insurance subsidies: • For lower income? • For older adults? – Added funding to states for opioid epidemic? – Keep state waivers for EHB, but not community rating? – Delay or limit some of the ACA tax cuts? • Other substantive/procedural changes to address potential “Byrd” problems – Abortion – Cost sharing for Native Americans – Allocation of budget savings between HELP and Finance Committees
- Slides: 40