Aetna Better Health of Michigan LAKELAND PAYOR CONFERENCE

Aetna Better Health of Michigan LAKELAND PAYOR CONFERENCE © 2019 Aetna Inc. 1 OCTOBER 16, 2019

ABH-MI Provider Experience Team o Patricia Pogodzinski - Provider Relations Representative o Margaret Campbell, MBA - Manager Provider Relations o Joyce Poole, Director Provider Experience © 2019 Aetna Inc. 2

Member Identification Cards – New ID cards are sent to all new Members and when PCP changes are made – If Members do not have their new ID card, Providers can obtain enrollment verification via the Secure Web Portal at http: //aetnabetterhealth. com/michigan – A temporary ID card can be faxed to a provider’s office by request by calling: • 1 -855 -676 -5772 (TTY 711)t Member Services prompt – Members can request a new copy of their card anytime from Member Services © 2019 Aetna Inc. 3

Participating Provider Confirmation – Providers newly added to the Aetna Better Health of MI Network can be found in our online directory at: http: //aetnabetterhealth. com/michigan – Newly added providers receive a Welcome Letter upon acceptance into the Aetna Better Health of Michigan network – Providers can verify their participation status by calling • 1 (855) 676 -5772 , then • Press “*”, then • Say “Provider Services’” © 2019 Aetna Inc. 4

Member Eligibility & Benefit Verification Providers can verify member eligibility, PCP assignment, benefits, co-pays/deductibles through three ways: 1. By using the State CHAMPS system accessed at: www. michigan. gov/medicaidproviders 2. By logging onto the Aetna Better Health Provider Portal at: http: //aetnabetterhealth-michigan. aetna. com/ 3. By calling Aetna Better Health Provider Services at: • 1 (855) 676 -5772, then • Press “*”, then • Say “ Eligibility and Benefits” © 2019 Aetna Inc. 5

Prior Authorization Information Services Requiring Prior Authorization Services (Partial List): – – – – – Inpatient Services Long term support services Surgical services Therapy Imaging Durable Medical Equipment Dental (select services) Injectables To access a Complete List of Prior Authorization Services and Requirements, go to the Aetna Better Health Provider Portal at: http: //aetnabetterhealth. com/michigan Then select “Pro. Pat Auth Lookup Tool” Orthotics/Prosthetics Transportation © 2019 Aetna Inc. 6

Medical Prior Authorization Phone Secure Web Portal Fax (Only for ABH-MI Contracted Providers) 1 -844 -241 -2495 1 -855 -676 -5772, Press “*” High Tech Radiology Authorizations Pharmacy Authorizations evi. Core: - By Phone: Caremark. CVS: - By Phone: • • • 1 (888) 693 -3211 FAX : 1 (844) 822 -3862 www. evi. Core. com 1 (855) 676 -5772, Press “*”, then • Say, “Pharmacy Helpdesk”, then • Press “Option 3” • 1 (888) 624 -1135(CVS Caremark) • Press “Option 3” - By FAX: 1 (844) 242 -0914 (CVS Caremark) • NOTE: A current list of services which require prior authorization can be found online at http: //aetnabetterhealth. com/michigan then select “Pro Pat Auth Lookup Tool”. © 2019 Aetna Inc. 7

Claims Submission – 3 WAYS to Submit MAIL SUBMISSION ELECTRONIC SUBMISSION • Submit claims to ABH through your EDI clearinghouse • Use EDI submitter ID #128 MI Note: Provider clearinghouse used must support Aetna claims submissions and link registration to Change. Health 1 © 2019 Aetna Inc. Send to: Aetna Better Health of Michigan P. O. Box 66215 Phoenix, AZ 850826215 • • UB 04 and CMS 1500 forms accepted only PORTAL SUBMISSION • Submit claims to ABH through Change Health at : https: //office. emdeon. co m/vendorfiles/Aetna. MI. html • Use EDI submitter ID #128 MI • Change. Health - Office Web. Connect is offered at no charge. Payer ID 128 MI 2 3 8
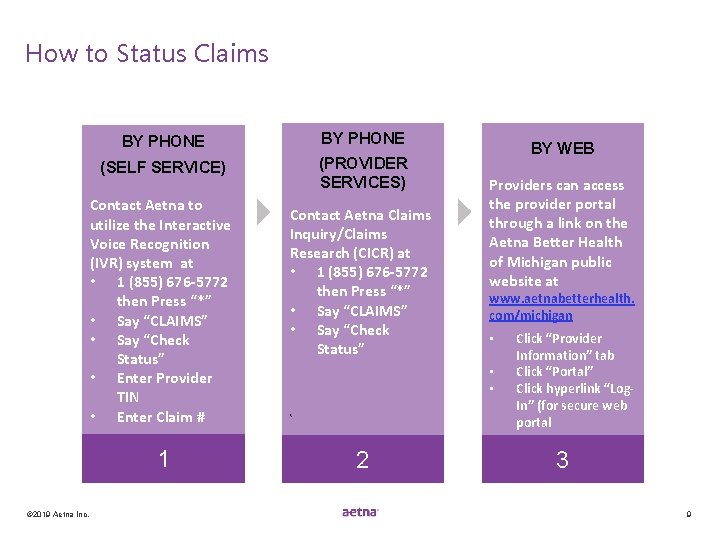
How to Status Claims BY PHONE (SELF SERVICE) (PROVIDER SERVICES) Contact Aetna to utilize the Interactive Voice Recognition (IVR) system at • 1 (855) 676 -5772 then Press “*” • Say “CLAIMS” • Say “Check Status” • Enter Provider TIN • Enter Claim # 1 © 2019 Aetna Inc. Contact Aetna Claims Inquiry/Claims Research (CICR) at • 1 (855) 676 -5772 then Press “*” • Say “CLAIMS” • Say “Check Status” BY WEB Providers can access the provider portal through a link on the Aetna Better Health of Michigan public website at www. aetnabetterhealth. com/michigan • • • 2 Click “Provider Information” tab Click “Portal” Click hyperlink “Log. In” (for secure web portal 3 9
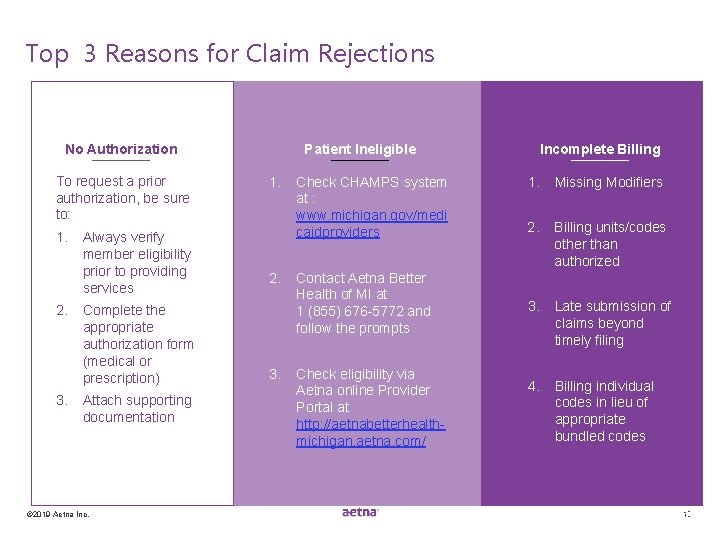
Top 3 Reasons for Claim Rejections No Authorization To request a prior authorization, be sure to: 1. 2. 3. Always verify member eligibility prior to providing services Complete the appropriate authorization form (medical or prescription) Attach supporting documentation © 2019 Aetna Inc. Patient Ineligible 1. 2. 3. Check CHAMPS system at : www. michigan. gov/medi caidproviders Contact Aetna Better Health of MI at 1 (855) 676 -5772 and follow the prompts Check eligibility via Aetna online Provider Portal at http: //aetnabetterhealthmichigan. aetna. com/ Incomplete Billing 1. Missing Modifiers 2. Billing units/codes other than authorized 3. Late submission of claims beyond timely filing 4. Billing individual codes in lieu of appropriate bundled codes 10 10

Provider Claim Resubmissions, Disputes & Grievances Claims Resubmissions/Disputes Provider Grievances - Provider Grievances are used when provider has a concern related to an overall policy or procedure, service experience or other non-claim related matter - Provider Grievances are submitted directly to Aetna Better Health of Michigan at: BY PHONE: 1 (866) 314 -3784, then Press “*”, then Say “Provider Services” BY MAIL : Aetna Better Health of Michigan P. O. Box 66215 Phoenix, AZ 85082 -6215 Non-Par Providers: Aetna Better Health of Michigan 1333 Gratiot Ave, Suite 400 Detroit, MI 48207 Step #1 – Download Aetna PAR Provider Dispute Form located at: www. aetnabetterhealth. com/michigan Step #2 – Complete form and Submit via Provider Portal at www. aetnabetterhealth. com/michigan -OR- – – – – Mail to: Aetna Better Health of Michigan P. O. Box 66215 Phoenix, AZ 85082 -6215 Resubmission Claims must be mailed with attached documentation/medical records Resubmitted claims must be submitted as a “Corrected Claim” Corrected Claims can be submitted electronically only if medical records are not required The appropriate reason on the dispute form must be selected All lines must be rebilled Include a copy of the original claim Copy of the Remittance Advice denial (as indicated on the form) © 2019 Aetna Inc. IMPORTANT: • • • Claims Disputes are only done via portal or mail Claim Disputes sent to the wrong address will not be re-routed Non-Par providers follow a different Appeal Process (Reconsideration) 11

Remittance Advice – Remittance advices are located within the Aetna Better Health of Michigan provider portal located at: http: //aetnabetterhealth. com/michigan – Electronic Remittance Advice (ERA) are available via your electronic vendor/clearinghouse, if applicable. You can also sign up to receive ERA via Aetna’s Provider Portal. • If you prefer to enroll/ change/ cancel electronically, please go to http: //aetnabetterhealth. com/michigan for the electronic form and instructions. – Claims and remit information will remain available on Aetna’s provider portal for up to three (3) years. © 2019 Aetna Inc. 12

Remittance Advice Sample © 2019 Aetna Inc. 13

Member Services Staff can assist Members with: – Understanding eligibility and benefits – Providing information on available programs and resources – Finding providers, including changing Primary Care Provider (PCP) assignments – Resolving any billing issues – Filing Member grievances or appeals – Call Member Services at • 1 (855) 676 -5772, then • Press “*”, then • Say “ Eligibility and Benefits © 2019 Aetna Inc. 14

Provider Relations Aetna Better Health of Michigan Provider Relations staff is available Monday through Friday 8 AM-5 PM Your Aetna Provider Relations Liaison • • • Patricia Pogodzinski PH#: (313) 465 -1524 Email Address: pogodzinskip@aetna. com You can reach Provider Relations by: – PHONE: Provider Relations Phone – 1 (855) 676 -5772, then • Press “*”, then • Say “Provider Services” – EMAIL: E-mail: Aetna. Better. Health-MIProvider. Services@aetna. com – FAX: Provider Relations – 1 (844) 300 -7473 © 2019 Aetna Inc. 15

Member Grievance and Appeals Member Appeals – Member appeals are not claim disputes and are specific to service authorization denials only – Member authorization is required before a provider or other party can appeal on behalf of a member – An Integrated Denial Notification (IDN) is issued by Aetna Utilization Management (UM) team after issuing an authorization denial • Details are included in the IDN as to appeal rights/instructions for these non-claim denials Decision Response – Pre-service: within 35 calendar days – Post service: within 35 calendar days • Appeal is reviewed by a physician not involved in original decision and not subordinate to original decision maker • The Appeal decision is the final decision © 2019 Aetna Inc. 16

Provider Manual Aetna Better Health of Michigan’s Provider Manual is available online at www. aetnabetterhealth. com/michigan. In addition to policies and procedures, this resource includes: – Important contact information – Provider rights and responsibilities – Credentialing – Member eligibility and enrollment – Billing and claims – Reconsiderations, appeals and complaints – Utilization Management Program and requirements – Quality Improvement Program © 2019 Aetna Inc. 17

Provider Portal Registration & Access Providers should register for the provider web portal. To get started: – Complete the web portal registration form – Submit web portal registration form to Provider Relations – Review our provider web portal navigation guide – If need help registering or would like a demonstration, contact Provider Relations at 1 (855) 676 -5772 (Press “*”, then Say “Provider Services”) Each TIN will have one account, with a primary administrator. – The primary representative can add authorized representatives within their office Don’t forget to register for the provider web portal. If you have questions, call Provider Relations at 1 (855) 676 -5772 (Press “*”, then say “Provider Relations”) © 2019 Aetna Inc. WHAT YOU CAN DO IN AETNA’S PROVIDER PORTAL 1. VERIFY ENROLLMENT 2. INITIATE AUTHORIZATIONS (PROPAT) 3. STATUS CLAIMS AND REVIEW EOB & RA’S 4. VIEW PROVIDER PANEL ROSTER 5. CONTACT AETNA VIA SECURE MESSAGING 6. REVIEW HEDIS GAPS IN CARE 7. SIGN UP FOR EFT/ERA 18
Aetna Better Health of MI - Website Members and Providers can access the Aetna Better Health of Michigan website at www. aetnabetterhealth. com/mi. You can access the following at www. aetnabetter health. com/mi: – The secure provider web portal – Our Provider Manual, communications and newsletters – A searchable Provider Directory – A Reconsideration Form – Clinical Practice Guidelines – Member materials – Fraud & Abuse information and reporting – Information on reconsideration and provider appeals © 2019 Aetna Inc. 19

Thank You
- Slides: 20