Aerosol Physics and Bland Aerosol Therapy Aerosol Information

Aerosol Physics and Bland Aerosol Therapy


Aerosol Information • “Aerosols occur in nature as pollens, spores, dust, smoke, smog, fog, and mist. • In the clinical setting, medical aerosols are generated with atomizers, nebulizers or inhalers that physically disperse matter into small particles and suspend them in a gas. ”

Aerosol definitions • Aerosol – a suspension of particulate matter, either solid or liquid, in a carrier gas. • Bland aerosol therapy – the delivery of sterile water or saline to the airways with or without supplemental oxygen • Aerosol drug therapy – the delivery of a therapeutic dose of a drug to the desired site of action within the pulmonary system

CHARACTERISTICS OF THERAPEUTIC AEROSOLS • Output: the weight or mass of aerosol particles produced by a nebulizer, usually measured particles per minute. • Aerosol Density: the weight or mass of aerosol output per unit of gas volume, usually measured in mg/L or g/L.

Aerosol Physics • Depth and effectiveness of aerosol delivery is dependent upon: – Aerosol output – Particle size – Deposition or depth of penetration • Aging • Breathing pattern of patient

• Output Aerosol physics – Rate of aerosol generation. – Mass of fluid or drug contained in aerosol by a nebulizer • Bland aerosol therapy – amount of solution generated per minute • Aerosol drug therapy – the proportion of the dose leaving the nebulizer – Emitted dose – the mass of drug leaving the mouthpiece of a nebulizer or inhaler

Aerosol physics • Particle size – A function of the • • Substance being nebulized Method used to make the aerosol Environment around the aerosol The final location of an aerosol particle in the respiratory tract is determined by its size. – Factors that affect the size of aerosol particles: • Condensation - as water condenses on aerosol particles, their size increases. • Evaporation - if the particles lose water through evaporation, their size decreases.

Measurement of Particle Size q. Measured in microns ( µ ) = 1/1000 of mm or 1/ 1, 000 of m Size Examples: therapeutic aerosols: grain of sand: pollen: tobacco smoke 1 -10 microns 200 -2000 microns 10 -100 microns 0. 2 -2 microns q Final location of aerosol particles in the respiratory tract is affected by their size. .

Deposition of Aerosol Particles in the Lungs Size Place of Deposition > 10 microns Do not enter the respiratory tract 5 -10 microns Nose breathing; upper airway 5 -10 microns Mouth breathing; oropharynx & large airways 1 -4 microns Small airways 1 -2 microns Increased alveolar deposition ≤ 0. 5 microns Remain suspended and are exhaled

Aerosol physics • Deposition or depth of penetration – A function of method of deposition (inertial impaction, sedimentation, diffusion, aging and the breathing pattern of the patient).

Aerosol physics • Inertial impaction – The collision of a particle with a surface; a function of mass and velocity. – Inertial impaction explains why large (>5 m) and/or fast moving aerosol particles primarily impact in the upper airways.

Aerosol physics • Sedimentation – The “raining or settling out” of aerosol particles due to gravity. Primary reason for the deposition of particles 1 -5 m size. • Diffusion – Brownian diffusion or movement is the primary reason for the deposition of particles smaller than 3 m in size mainly in the alveolar regions where bulk flow has ceased and gases move by diffusion.

Aerosol physics • Aging – The process by which an aerosol suspension changes over time – Dependent upon the composition of the aerosol, the initial size of its particles, the time in suspension, and the ambient conditions (temperature and humidity). – Particles change size as a result of either evaporation or water absorption (hygroscopic tendency).

Aerosol physics • Breathing pattern of patient – Flow pattern – Inspiratory flow rate – Respiratory rate – Inhaled volume – I: E ratio – Breath-holding

Indications for Aerosol Therapy • • Humidification of the respiratory tract Mobilization of secretions Sputum Induction Administering Medications
Humidification of the Respiratory Tract • Used to deliver liquid water to the mucosal surface • Particles will evaporate as they are warmed by the body, which will increase the humidity of the inspired gas. • Humidification can be increased by heating the water. • Heated aerosols can be used to provide adequate humidity for patients with artificial airways (T-piece). • Cool aerosols have been used for their soothing effect on inflamed upper airway tissues (after extubation).

Hazards of Aerosol Therapy • Infection – Aerosol generators are capable of transmitting bacteria from the device to the patient. – CDC guidelines state “start with sterile equipment and change or replace with sterile water every 24 hours. ” • Pulmonary and Systemic Effects: – Overhydration – hypernatremia (too much Na. Cl) – tissue damage, atelectasis, and pulmonary edema – fluid and electrolyte imbalance – airway obstruction

BLAND AEROSOL THERAPY • A bland aerosol consists of liquid particles suspended in a gas. • Involves the delivery of sterile water or hypertonic, isotonic or hypotonic saline. • May be accompanied by oxygen therapy. • Bronchodilators are not delivered by bland aerosols!!!!

Indications • Upper airway inflammation (cool aerosol only). • Subglottic edema • Post extubation • Bypassed upper airway • Sputum inductions

Contraindications • Bronchospasm • Hx of upper airway hyperresponsiveness • Hazards and Complications -Wheezing or Bronchospasm -Infection -Overhydration -Patient discomfort -Therapist exposure to airborne pathogens

Delivery of Bland Aerosols • Large-Volume Air-Entrainment Nebulizers

Large Volume Nebulizers • Most commonly used device to deliver a bland aerosol. • Employ a jet or restricted orifice to disperse the liquid into the gas. • Particle size is 1 -10 microns (deposits from alveoli-upper airways) • Large reservoir capacity (0. 5 L-3. 0 L) for continuous use. • Incorporates an air-entrainment system to increase flow and control Fi. O 2.

REVIEW • MINIMUM FLOW NEEDS OF A PATIENT • TOTAL FLOW 24

Minimum Flow Needs of a Patient Estimate the patient’s minimum inspiratory flow need by multiplying the Ve X 3.

Total Flow Output of an Air-Entrainment Device (given the oxygen input): • Use the answer from the Air-to-Oxygen Ratio Equation. • Add the air-to-oxygen ratio parts together. • Then multiply the sum of the ratio parts by the oxygen input flow.

Air-to-Oxygen Ratio to Obtain a Given O 2 Percentage Liters air = Liters O 2 (100 - %O 2) ( %O 2 - 21)

Large Volume Nebulizers • Produce a cool or heated aerosol mist. -Cool aerosols can deliver a total water output (humidity) of 26 -35 mg/L, or 60 -80% body humidity. (body humidity is the capacity at body temperature). -Used for: - Upper airway inflammation - New trach patient • Heated aerosols can deliver 33 -55 mg/L, or 75 -95% body humidity, because of increased water vapor capacity.

Types of Saline – Isotonic saline – aka normal saline (N/S) 0. 9% – Hypotonic saline – less than 0. 9% • Often 0. 45 % or half-normal – Hypertonic saline – greater than 0. 9% • Often 3% or 10%

Mobilization of Secretions • Therapeutic Use – Generally use bland aerosols to add water to secretions. – Use large-volume, high density mist to induce sputum production – Duration of therapy will vary according to the patient’s need and tolerance. – May need to pre-treat with a bronchodilator; because of increased sputum production. – Must provide for removal of secretions; cough or suction.

Mobilization of Secretions • Sputum Induction – Is used as a diagnostic procedure that is useful, cost effective and a safe method for diagnosis of tuberculosis, Pneumocystis carinii pneumonia (AIDS related), lung cancer, and other bacterial lung infections – Used to help increase sputum production so that a culture and sensitivity test – Can be performed to identify and treat specific bacteria. – Use inhaled irritants to increase sputum production and stimulate a cough. – Common irritants include distilled water and hypertonic saline. – Duration of therapy is variable. – Try not to mix oral/nasal secretions with sputum. – Collect samples in the early am. • Administering Medications – Documented to be effective for delivering bronchodilators, more controversial for other agents such as antibiotics.
Sputum Induction Procedure • Gather necessary equipment: aerosol mask, specimen container, hypertonic saline (if the patient can tolerate). • Check the chart for the order and other pertinent information. • Wash hands and follow any listed precautions (Resp. isolation ect. ) • Intro self and explain procedure • Have patient: -Sit upright -Rinse mouth, blow nose, clear excess saliva 1. 2. 3. 4. 5. 6. Perform pre treatment assessment Place mask on the patient Reassess patient periodically for adverse reactions Terminate after 30 minutes if no sputum is obtained. Collect sputum in cup, label with patient identification Chart therapy and results.
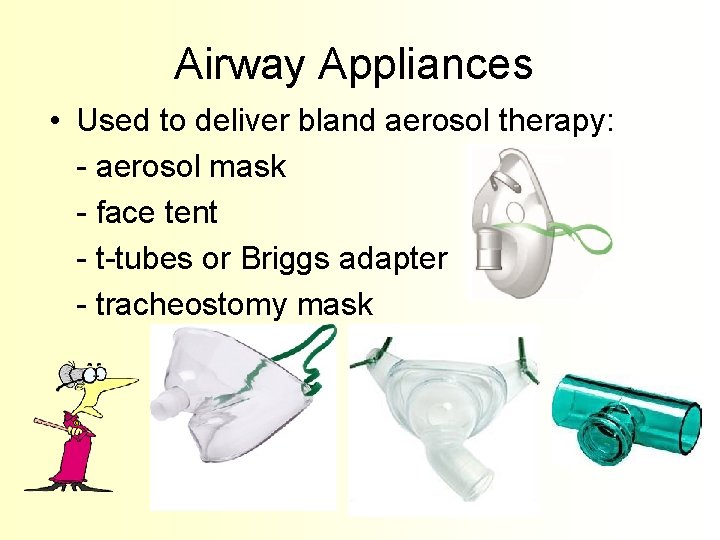
Airway Appliances • Used to deliver bland aerosol therapy: - aerosol mask - face tent - t-tubes or Briggs adapter - tracheostomy mask

Troubleshooting Bland Aerosols • Most common problem is cross contamination and infection - Disinfect aerosol units regularly • Inadequate mist productions • Pneumatically powered bland aerosols – – inadequate input flow capillary tube obstruction jet orifice misalignment if all check out and is still not functioning, take out of service.

- Slides: 35