Aerosol Bronchodilator Therapy Aerosol n Is a suspension

Aerosol Bronchodilator Therapy

Aerosol n Is a suspension of solid or liquid particles in gas n Used to deliver bland water solutions to the respiratory tract or to administer drugs to lungs, throat, or nose n Aim to is to deliver therapeutic dose of the selected agent to the desired site of action with minimal side effects and greater efficacy and safety

Characteristics of Aerosol n Aerosol output n Particle size n Particle deposition n Aging

Characteristics of Aerosol n (i) Aerosol output n n Indicates the weight or mass of the aerosol particle produced by the nebuliser per min This can be measured by collecting the aerosol that leaves the nebuliser on filters, and measuring either the weight or the quantity of the drug

n (ii) Particle size (Ranges from 0. 5 - 3. 0 micrometre) n n Depends on substance being nebulised, the nebuliser chosen, the method used to deliver the aerosol, and environmental conditions surrounding the particle Only way to determine the particle size is by laboratory measurement. Two common laboratory methods are n n n Cascade impaction n n cascade impaction laser diffraction The particle size is measured in terms of Mass Median Aerosol Diameter (MMAD) Laser diffraction n Particle size is measured in terms of Volume Median Diameter (VMD) These two terms give particle size in terms of micrometres

Characteristics cont. n (iii) Particle deposition Ø Ø Aerosol particles are deposited when they leave the suspension in gas There are two forms of aerosol deposition Inhaled dose – Only a portion of aerosol is inhaled Ø Respirable dose – A smaller fraction of fine particles is deposited in the lungs The mass of drug deposition is of two types * Inhaled mass – The inhaled amount of drug * Respirable mass – The proportion of the drug of proper size reaching the lower respiratory tract Ø

Factors Affecting Penetration and Deposition n Inertial impaction n Gravimetric sedimentation n Diffusion

Inertial Impaction n Occurs when suspended particles in motion colloid with and are deposited on a surface n This occurs in particle size larger than 5 micrometres n Larger particles have greater inertia, which keeps them moving in straight line. When they pass through the airway they cannot make directional changes, so they easily deposit.

Gravimetric Sedimentation n This occurs when a particle settles out of suspension and/or is deposited due to gravity n The greater the mass, the faster it settles n This occurs in particles ranging from 1 to 5 micrometres n Breath-holding after inhalation of the aerosol increases the residence time of the particle in the lung and increases sedimentation

Brownian Diffusion n A primary mechanism through which deposition of particles less than 3 micrometres occurs n Since these particles are 0. 5 micrometres in size, they have greater retention in the lungs

Aging n Particles constantly grow, shrink, collapse, and fall out of suspension n The process by which an aerosol suspension changes over time is called aging n Aging is inversely proportional to the size of the particle, so smaller particles grow or shrink faster than larger particles

Aerosol Therapy n A therapeutic administration of a drug in the form of an aerosol n Indications n Administer medication n n Bronchospasm Inflammation Mucosal edema Copious secretion For mobilization of secretion Home regimen n Physician’s order n Need to obtain sputum n

Hazards of Aerosol Therapy n Infection n Airway reactivity n Pulmonary and systemic effects n Drug reconcentration

Aerosol Drug Delivery Systems MDIs with and without spacer n Nebuliser n A device used for converting a liquid drug into a fine mist which can then be inhaled easily n Two types n Jet nebuliser n Ultrasonic nebuliser n

Jet Nebuliser § Powered by high-pressure air or oxygen provided by a portable compressor, compressed gas cylinder, or 50 psi valve outlet § Principle – If a stream of gas is passed through a small hole, the gas creates a lower pressure as it emerges from the hole

Small-Volume Nebuliser n Definition – Nebulisers commonly used in hospital and home for drug administration have small medication reservoirs (<10 ml) n Factors affecting SVN performance n Nebuliser design n Gas pressure n Density

Nebuliser Design n Baffles n Fill volume n Residual volume n Nebuliser position

Gas Source (Wall, cylinder, compressor) n Pressure n Flow-through nebuliser n Gas density n The lower the density of the carrier gas, the less aerosol impaction occurs and the better the deposition in the lungs

Large-Volume Nebuliser n Used to deliver aerosolized drug to the lung n Can be used for continuous nebulization n Has a reservoir of more than 240 ml producing aerosol of MMAD 2. 2 - 3. 5 micrometres n Actual output and particle size vary with pressure and flow at which nebuliser operates n If pt. is on CBT, drug toxicity should be monitored since CBT causes drug reconcentration

Ultrasonic Nebuliser n n n A nebuliser in which an electric crystal is used to produce an aerosol The crystal transducer converts an electrical signal into a high-frequency vibration (1. 2 - 2. 4 MHz) These vibrations enter the liquid above the transducer and disrupt the surface to create oscillation waves If the frequency increases, the amplitude is strong enough that the oscillation waves form a geyser of droplets that break as fine aerosol particles This is capable of producing higher aerosol output (0. 2 - 0. 5 ml/min) Particle size is inversely proportional to frequency of vibration

Types of USNs n Large-Volume USN Used mainly for bland aerosol therapy and sputum induction n Uses air blowers to carry the mist to the patient n n Small-Volume USN n Medication is directly placed on top of the transducer, which is connected by cable to a power source. The patient’s inspiratory flow draws the aerosol from the nebuliser into the lung.

Nebulization Therapy n Definition – A process of dispersing a liquid (medication) into microscopic particles and delivering this liquid into the lungs as the patient inhales through the nebuliser n Purposes To administer medication directly into the respiratory tract to induce sputum expectoration in case of sputum induction n To reduce the difficulty of bringing out the secretions n To increase VC n

Prerequisites n Optimal volume of solutions in nebuliser chamber (2 - 4 ml) n Oxygen- or air-driven device which produces a flow rate of 4 - 6 lts/min n Advantages n n n High doses can be given Tidal breathing is adequate for inhalation Aerosolized drugs which cannot be administered through MDIs can be given through this Avoids reflux coughing Allows mixing of drugs

Disadvantages n High doses may result in toxicity n Requires continuous supply of electricity n Expensive n Requires regular maintenance n Risk of transmission of airborne infection where cleaning is not adequate

Equipment n Nebuliser solution (Terbutaline 10 mg/ml, Ipravent n n 250 mcg/ml) Normal saline Oxygen source or air-driven device Oxygen tube Face mask or mouthpiece

Procedure n n n Wash hands Arrange equipment needed Explain the use of nebuliser Warn about side effects Assemble nebuliser equipment Add prescribed medicine and diluent Hold the mouthpiece between lips with gentle pressure Ask the patient to take deep breaths and exhale passively Turn the nebuliser machine on and ensure sufficient mist is formed Turn off when the mist stops If a steroid is given, gargle or rinse mouth

Practical Points n Saline should be used as a diluent, not distilled water (Hypoosmolar solution can lead to reflex bronchospasm) n Drug delivery is effective depending on the source (Mouthpiece or face mask) n If a mask is used, it should be used as close to the face as possible since any gap reduces drug delivery significantly n Check for adequate mist production

n In absence of mist, check for n n n Any leak Obstruction of flow (Kinking of tube) Misalignment of the nebuliser Inadequate solution Position of the nebuliser

Post-Procedure n Vital signs to be checked before and after therapy n Assess for side effects like coughing and cardiac dysarrythmias n In case of sputum induction, note the amount, colour, and consistency of the expectorant

Cleaning n After each Rx n Disassemble the nebuliser completely n Rinse tubing, medication cup, mouthpiece, and mask in warm water n Shake off excess water and allow to air-dry n Avoid drying in dusty and smoky areas n After each day n Disassemble the nebuliser completely n Submerge the tubing, medication cup, mouthpiece, and mask in mild liquid detergent and warm water n Use a small brush to remove any sediment that is accumulated n Rinse parts thoroughly after washing n Immerse all parts in cidex n Remove and rinse under water n Air-dry all parts

Bronchodilators n Two types n n n Adrenergic bronchodilators Anticholinergic bronchodilators Bronchodilators delivered through n MDI n Nebulisers

Adrenergic Bronchodilators n Stimulates Alpha receptor stimulation, which causes vasoconstriction and vasopressor effect n Beta 1 receptor stimulation causes increased HR and myocardial contractility n Beta 2 receptor stimulation, which relaxes bronchial smooth muscle, stimulating mucociliary activity n

Sub-Groups n Ultra short-acting bronchodilator E. g. Epinephrine (1: 100%) 0. 25 - 0. 5 ml through neb n Shorter duration of action n Used for reducing swelling and controlling bleeding n Short-acting, non-catecholamine agents n Action is app. for 4 - 6 hours, so they can be taken PRN or QID n Terbutaline n 2. 5 mg through neb n Inj 1 mg/ml n Tab 2. 5/5 mg n Salbutamol n Neb 2. 5/5 mg, n MDI 100 mcg/puff 2 puffs PRN n DPI 200 mcg/cap 1 cap PRN n Tab 2/4 mg n

Long-Acting Adrenergic Bronchodilator n Long-acting adrenergic bronchodilator Onset of action is within 20 min and peak effect is within 3 to 5 hours. Overall duration of action is 12 hours. n E. g. Salmeterol n MDI 25 mcg/puff 2 puff BD n Formeterol n MDI n

Adverse Effects of Adrenergic Bronchodilators n Common side effects Headache, insomnia, nervousness, tremor, palpitations, and tachycardia • Specific side effects n n n Dizziness, nausea, hypokalemia, loss of bronchoprotection, CFC-induced bronchospasm, worsening ventilation perfusion ratio CFC-induced bronchospasm is managed by replacing HFA propellants

Assessment of Bronchodilator Therapy n General assessment Monitoring vital signs (RR, PR, breath sounds) n Correct technique • Specific n n n n n Monitor PEFR ABG or Sp. O 2 in acute state K and blood glucose If on long-term, monitor PFT Action plan for asthma patients Patient education Technique of aerosol delivery Cleaning of aerosol device

Anti-Cholinergic Bronchodilators n Acts by producing airway relaxation through blockage of cholinergic-induced bronchoconstriction n Indications n COPD (chronic bronchitis, emphysema), severe asthma n E. g. Ipratropium bromide n 250 mcg/ml neb 0. 5 mg n MDI 18 mcg/puff 2 puffs qid

Mode of Action n Acts on the acetyl choline at the muscarinic receptors on the airway smooth muscle n Drugs n Ipratropium bromide MDI 18 mcg/puff 2 puffs QID n SVN 0. 5 mg QID

Adverse Effects n Common n Cough and dry mouth n Occasional (MDI) n Nervousness, irritation, dizziness, headache, palpitation, rash n SVN Pharyngitis, dyspnea, flu-like symptoms, bronchitis, URI, nausea, occasional bronchoconstriction, eye pain, urinary retention

Aerosol Therapy
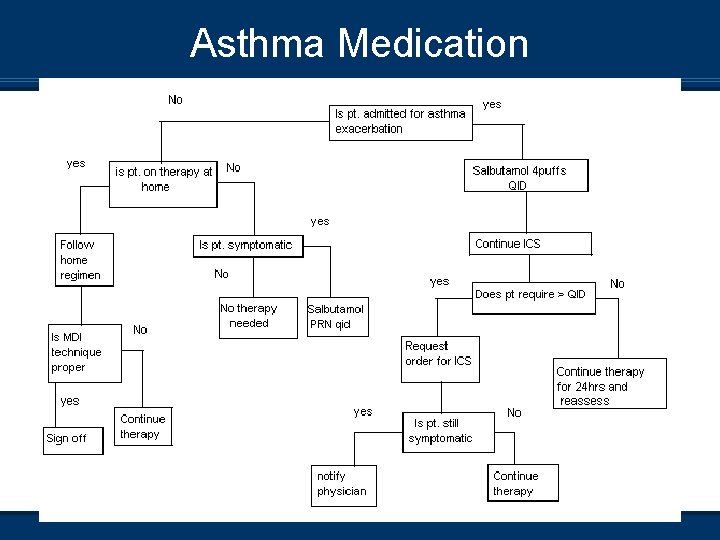
Asthma Medication

- Slides: 42