ADVANCES IN INFLAMMATORY BOWEL DISEASE 2004 presented by

ADVANCES IN INFLAMMATORY BOWEL DISEASE 2004 presented by The Foundation for Clinical Research in Inflammatory Bowel Disease

ADVANCES IN INFLAMMATORY BOWEL DISEASE 2004 presented by The Foundation for Clinical Research in Inflammatory Bowel Disease

ADVANCES IN INFLAMMATORY BOWEL DISEASE 2004 presented by The Foundation for Clinical Research in Inflammatory Bowel Disease

Inflammatory Bowel Disease (IBD) vs. Irritable Bowel Syndrome (IBS) • IBD = Inflammatory Bowel Disease – Chronic intestinal inflammation – Crohn’s disease, Ulcerative Colitis • IBS = Irritable Bowel Syndrome – No tissue abnormality • Change in bowel habits – Diarrhea/ Constipation/ Alternating bowel patterns • Pain relieved with bowel movement • Increased sensitivity to intestinal motility

IBD: Overview • Total number of cases – More than 1 million cases estimated in United States – Ulcerative Colitis: 50% – Crohn’s disease: 50% • Number of new cases annually – 10 new cases per 100, 000 people per year – Peak onset occurs between ages of 10 and 19 – Young children: 2%

IBD: Overview • Scope of the disorder (United States) – 700, 000 physician visits per year – 100, 000 hospitalizations per year • Long-term outlook – Chronic, lifelong disease without medical cures – Surgery for 50% to 80% of Crohn’s disease patients – Surgery for 20% of Ulcerative Colitis patients • Most patients live normal, productive lives!
The Spectrum of IBD UC CD Indeterminate colitis
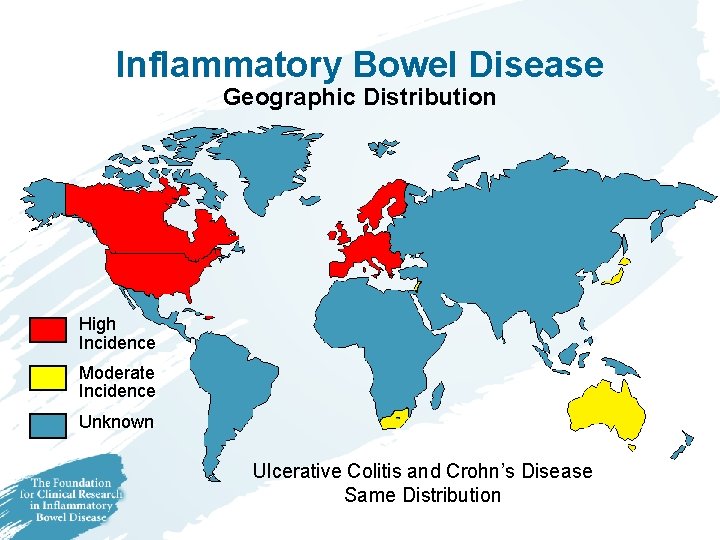
Inflammatory Bowel Disease Geographic Distribution High Incidence Moderate Incidence Unknown Ulcerative Colitis and Crohn’s Disease Same Distribution
Potential Causes of IBD Immune System Genetics Environment
Do All Causes Contribute Equally? Genetics Immune System Environment

Evidence for Genetic Susceptibility to IBD • Racial and ethnic risks of IBD • Multiple family members with IBD • Patterns of IBD in identical vs. fraternal twins

Genetic Susceptibility: Twin Studies Disease Presence in Twins Identical twins (%) Fraternal twins (%) UC 6. 3 0 CD 58 3. 9

Genetic Susceptibility: Twin Studies Disease Presence in Twins Identical twins (%) Fraternal twins (%) UC 6. 3 0 CD 58 3. 9

Searching for IBD Genes • Candidate Gene Approach – Based on “hunch” – Investment low, likelihood of success low • Genome Wide Screen – Better in families with multiply members affected – Looking for evidence of “linkage”

Searching for IBD Genes • Candidate Gene Approach – Based on “hunch” – Investment low, likelihood of success low • Genome Wide Screen – Better in families with multiply members affected – Looking for evidence of “linkage”
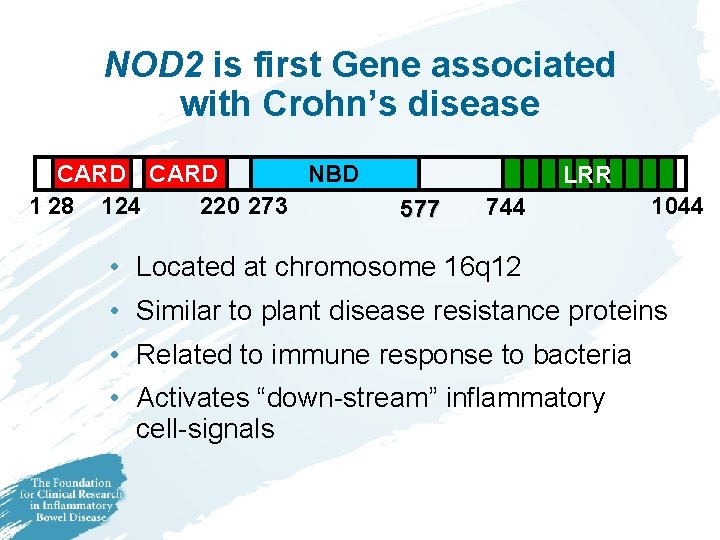
NOD 2 is first Gene associated with Crohn’s disease CARD NBD 1 28 124 220 273 LRR 577 744 1044 • Located at chromosome 16 q 12 • Similar to plant disease resistance proteins • Related to immune response to bacteria • Activates “down-stream” inflammatory cell-signals

Significance of NOD 2 Risk to Developing Crohn’s disease • One copy of Mutated Gene – 1. 5 -4. 0 fold risk • Two Copies: 15 -40 fold risk – 10% of CD patients carry two copies – 28% of CD patients carry one copy – Actual disease presence with one or two gene copies is less than 10%
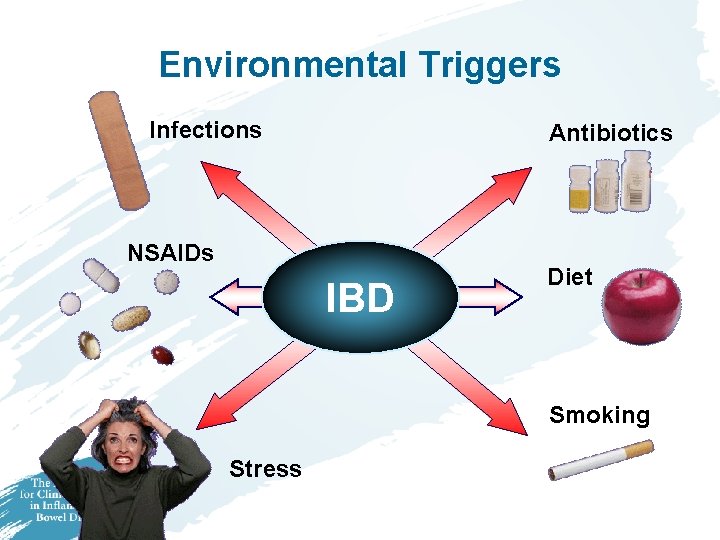
Environmental Triggers Infections Antibiotics NSAIDs IBD Diet Smoking Stress
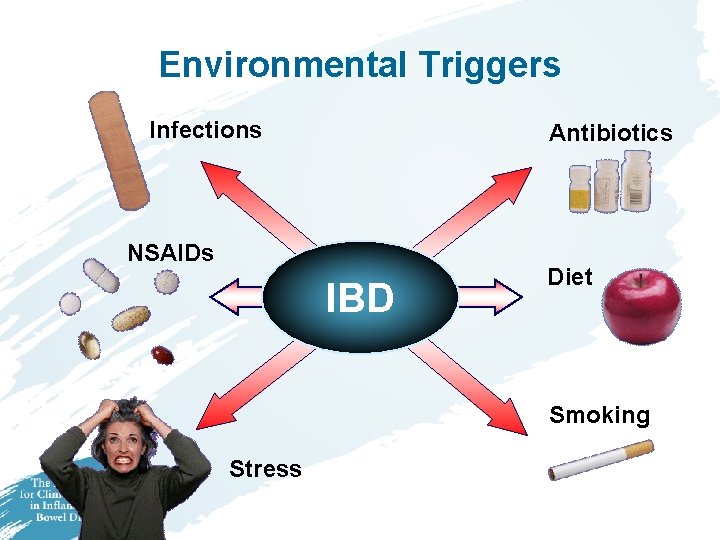
Environmental Triggers Infections Antibiotics NSAIDs IBD Diet Smoking Stress

Smoking in IBD • Ulcerative Colitis – Smoking can protect against UC – Ex-smokers are more likely to develop UC • Crohn’s disease – Twofold risk in current smokers – Smokers are less responsive to treatment – Smokers are more likely to develop recurrence of disease after surgery

What Causes IBD? Genetic predisposition Environmental triggers (infection, bacteria) Failure to control inflammation Chronic uncontrolled inflammation = Crohn’s disease Moderately Inflamed gut Normal gut Controlled inflammation Successful control of inflammation Normal gut Controlled inflammation

How IBD is Diagnosed • Clinical history • Physical examination • Laboratory tests • Endoscopy (Gastroscopy/Colonoscopy) • X-ray findings • Tissue biopsy (pathology)

How IBD is Diagnosed • Clinical history • Physical examination • Laboratory tests • Endoscopy (Gastroscopy/Colonoscopy) • X-ray findings • Tissue biopsy (pathology)

How IBD is Diagnosed • Clinical history • Physical examination • Laboratory tests • Endoscopy (Gastroscopy/Colonoscopy) • X-ray findings • Tissue biopsy (pathology)

Colonoscopy in IBD • Diagnosis of IBD (UC vs. CD) – Allows visualization of large intestine and ileum – Allows biopsies to examine colon tissue • Determines activity of disease • Important for pre-cancer surveillance in UC and CD

Colonoscopy in IBD • Diagnosis of IBD (UC vs. CD) – Allows visualization of large intestine and ileum – Allows biopsies to examine colon tissue • Determines activity of disease • Important for pre-cancer surveillance in UC and CD

Colonoscopy • Requires complete “cleansing” of colon to allow visualization of bowel lining • Preparations include: – Golytely®/Colyte® purge • Requires drinking 1 gallon of solution – Fleets prep® • Small volume of purge, large volume of water – Visicol® tablets
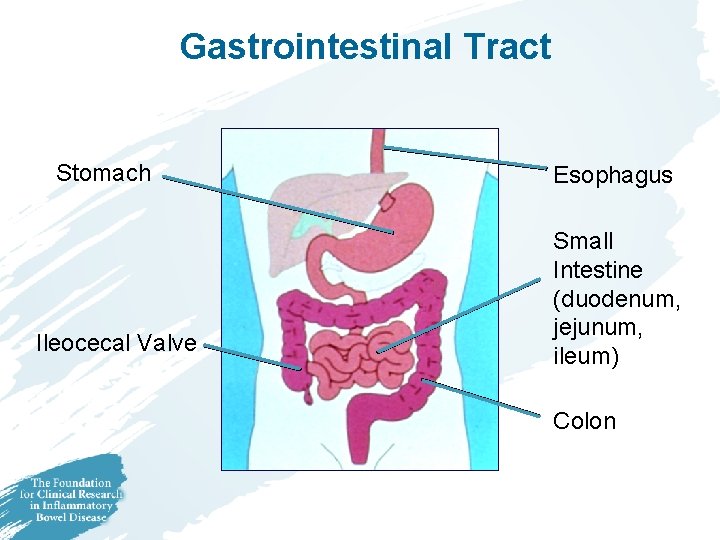
Gastrointestina. I Tract Stomach Ileocecal Valve Esophagus Small Intestine (duodenum, jejunum, ileum) Colon
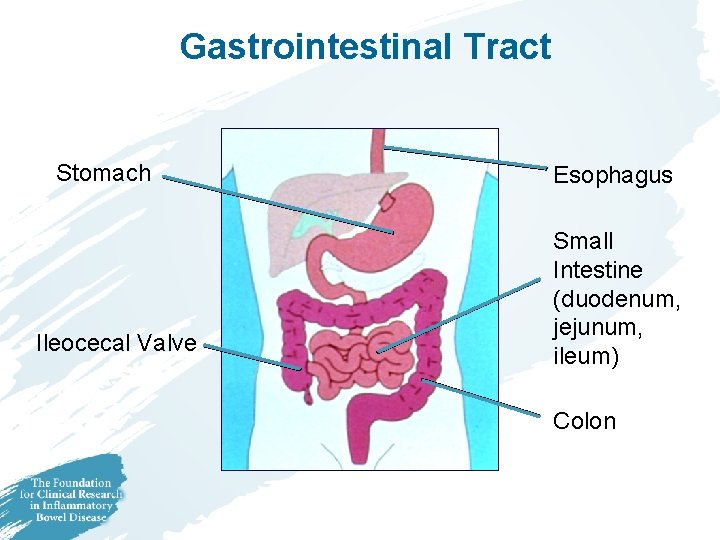
Gastrointestina. I Tract Stomach Ileocecal Valve Esophagus Small Intestine (duodenum, jejunum, ileum) Colon
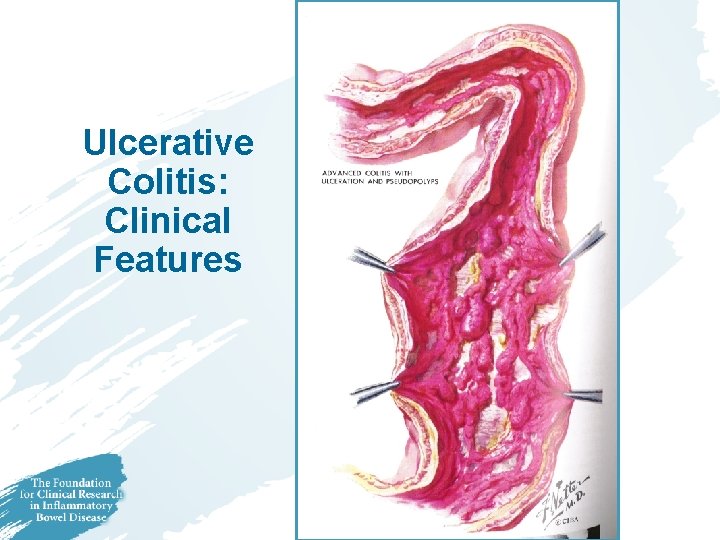
Ulcerative Colitis: Clinical Features
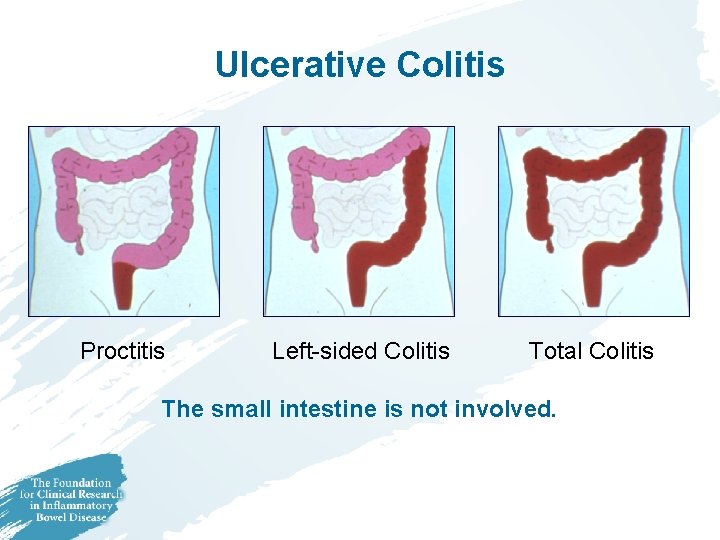
Ulcerative Colitis Proctitis Left-sided Colitis Total Colitis The small intestine is not involved.

Symptoms of Ulcerative Colitis • Symptoms depend on extent and severity of inflammation – – Rectal bleeding and urgency to evacuate Diarrhea Abdominal cramping Extraintestinal (systemic) symptoms • Joint pain/swelling • Eye inflammation • Skin lesions
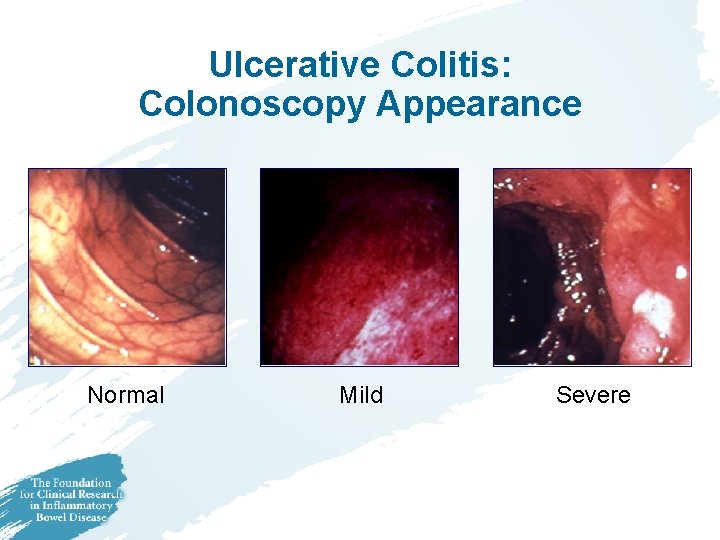
Ulcerative Colitis: Colonoscopy Appearance Normal Mild Severe
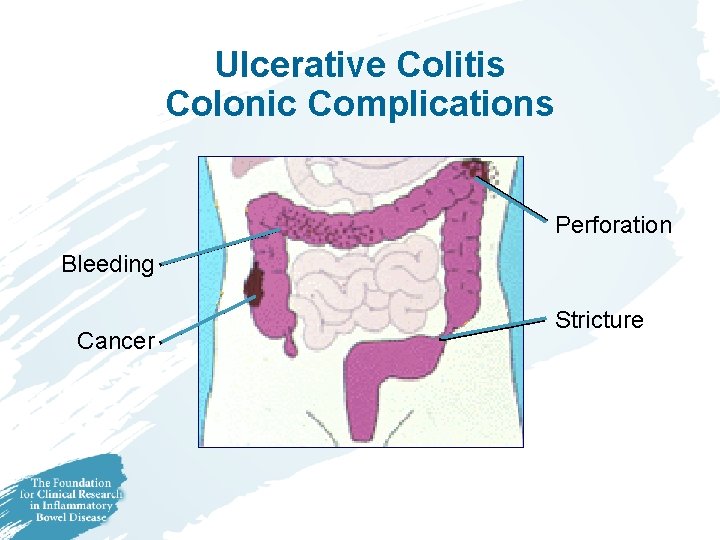
Ulcerative Colitis Colonic Complications Perforation Bleeding Cancer Stricture
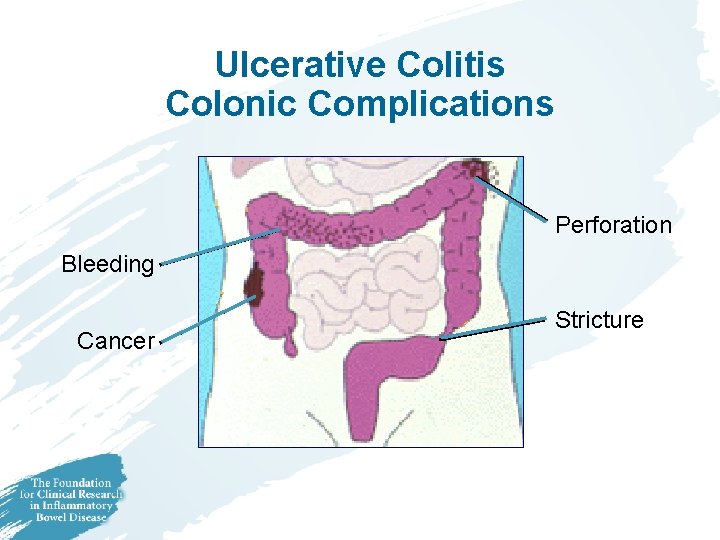
Ulcerative Colitis Colonic Complications Perforation Bleeding Cancer Stricture
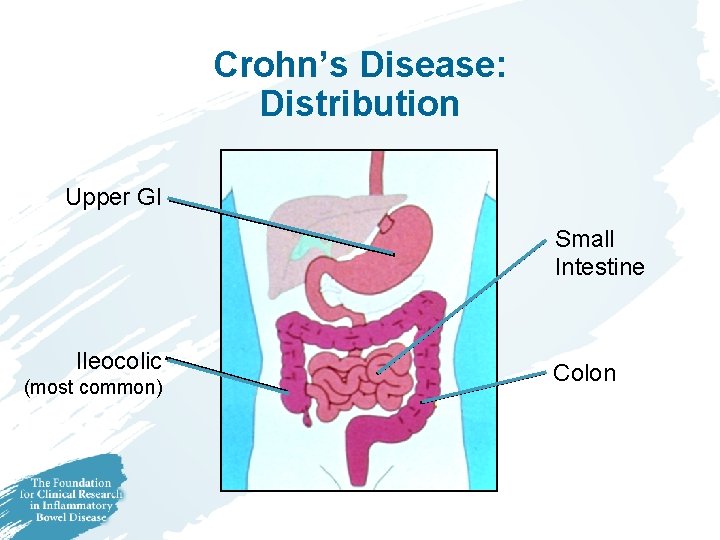
Crohn’s Disease: Distribution Upper GI Small Intestine Ileocolic (most common) Colon

Common Symptoms of Crohn’s Disease • Diarrhea • Abdominal pain and tenderness • Loss of appetite and weight • Fever • Fatigue • Rectal bleeding and anal ulcers • Stunted growth in children

Common Symptoms of Crohn’s Disease • Diarrhea • Abdominal pain and tenderness • Loss of appetite and weight • Fever • Fatigue • Rectal bleeding and anal ulcers • Stunted growth in children
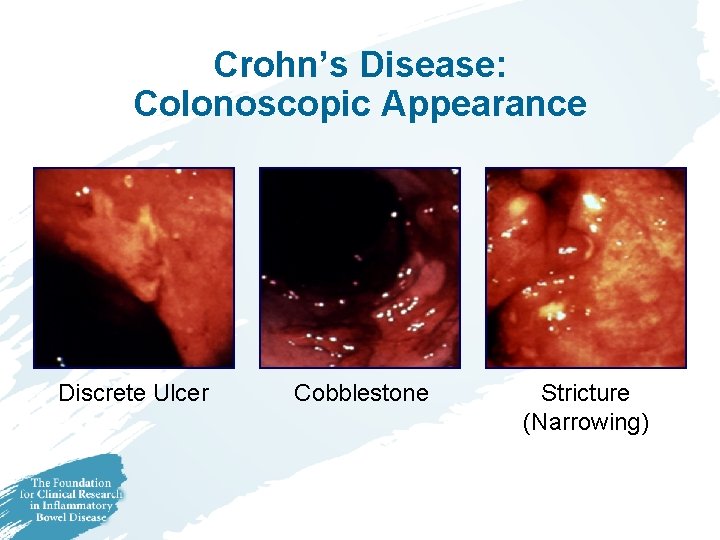
Crohn’s Disease: Colonoscopic Appearance Discrete Ulcer Cobblestone Stricture (Narrowing)
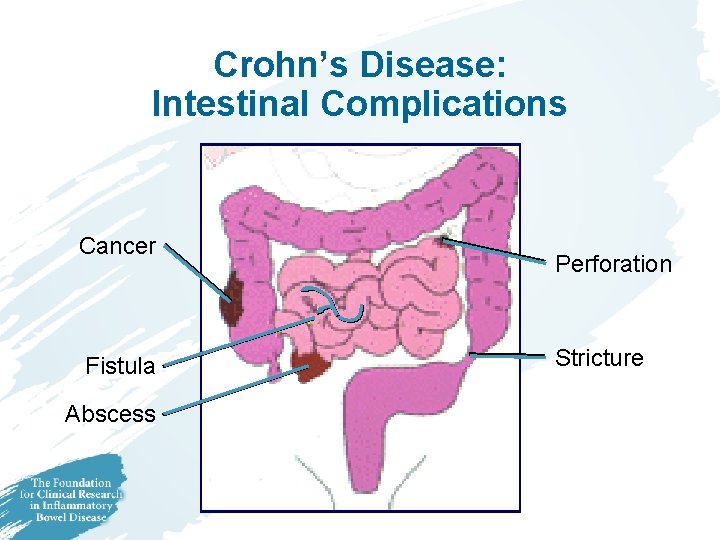
Crohn’s Disease: Intestinal Complications Cancer Fistula Abscess Perforation Stricture
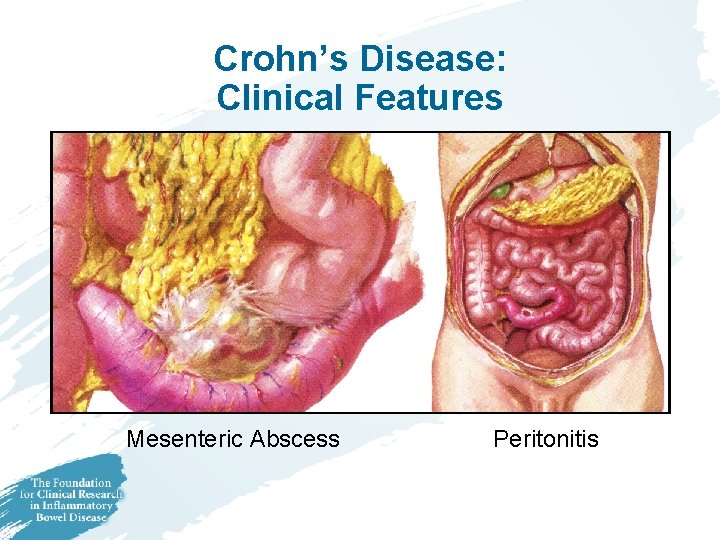
Crohn’s Disease: Clinical Features Mesenteric Abscess Peritonitis
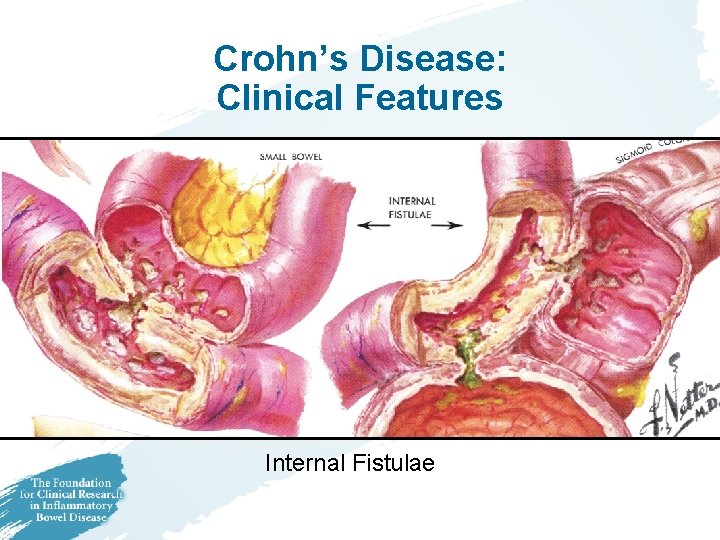
Crohn’s Disease: Clinical Features Internal Fistulae
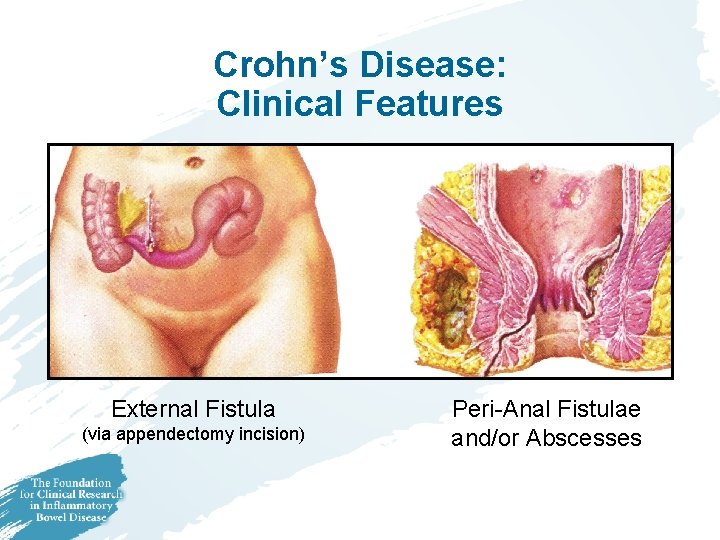
Crohn’s Disease: Clinical Features External Fistula (via appendectomy incision) Peri-Anal Fistulae and/or Abscesses
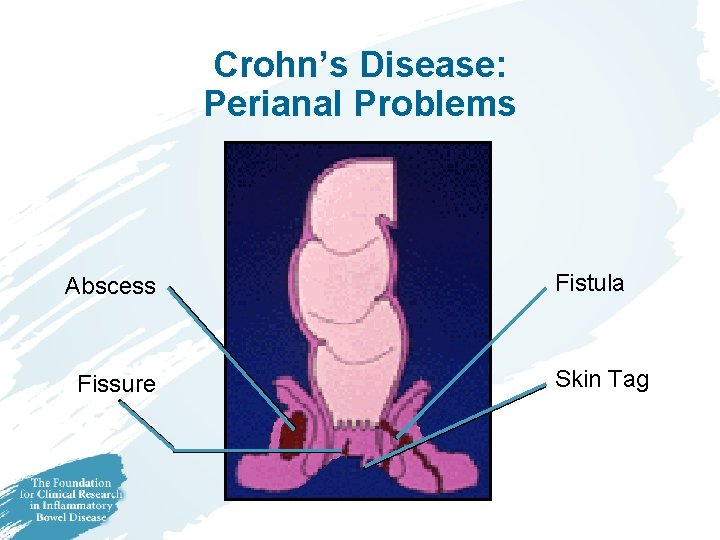
Crohn’s Disease: Perianal Problems Abscess Fissure Fistula Skin Tag
IBD: Extra-intestinal Manifestations Skin Eye Bones and Joints Kidney Liver/ Gall Bladder
IBD: Extra-intestinal Manifestations Skin Eye Bones and Joints Kidney Liver/ Gall Bladder
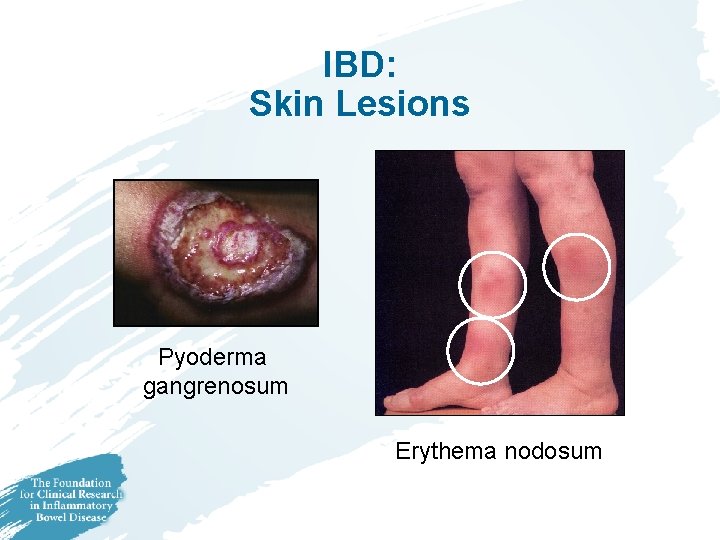
IBD: Skin Lesions Pyoderma gangrenosum Erythema nodosum
Treatment of Inflammatory Bowel Disease Surgery Emotional Support Medications Nutrition
IBD: Management Goals Address psychosocial issues Identify dysplasia and detect cancer Improve daily functioning Relieve symptoms Establish Diagnosis Replenish nutritional deficits Treat inflammation Treat complications Minimize treatment toxicity Maintain remission

What Patients Should Expect • Prior to diagnosis – Quick access/referral from Primary Care to Specialist (Gastroenterologist) • At diagnosis – Thoughtful explanation of disease with opportunity for discussion

What Patients Should Expect • Long-term follow-up – Continuity of care • Primary Care Physician (if confident) • Gastroenterologist should be available – – Consideration of quality of life Acknowledgement of problems Access to second opinions Maintain dignity!

What Patients Should Expect • Hospital management – – – Knowledgeable MD/nursing staff Willingness to refer to specialist center Communication with patients/families Encouragement of self-management Choice in medical/surgical therapies Access to dietitians, social workers

Medical Therapies for Inflammatory Bowel Disease • 5 -ASA agents – – – – Asacol® Azulfidine® Colazal® Dipentum® Pentasa® Rowasa® Enema Canasa® Suppository
Medical Therapies for Inflammatory Bowel Disease • Antibiotics – Cipro® – Flagyl® • Steroids – – – ACTH Medrol® Prednisone Cortenema® Cortifoam®
Medical Therapies for Inflammatory Bowel Disease • Immunologic agents – Imuran® (Azathioprine) – Purinethol® (6 -MP) – Neoral® (Cyclosporine) – Methotrexate • Biologic agents – Remicade® (Infliximab)

5 -ASA agents (Aminosalicylates) • Induce remissions in mild-moderate – UC/CD • Maintain remissions in mild-moderate UC • Maintain remissions in CD after: – Medical treatment – Surgical resections

5 -ASA agents (Aminosalicylates) • • • Benefits Well-tolerated Few side effects Relatively inexpensive Oral or Rectal Safe for all ages & pregnancy Risks • Rare allergies/ side effects • Not helpful in severe disease • Not helpful after steroids (particularly CD)
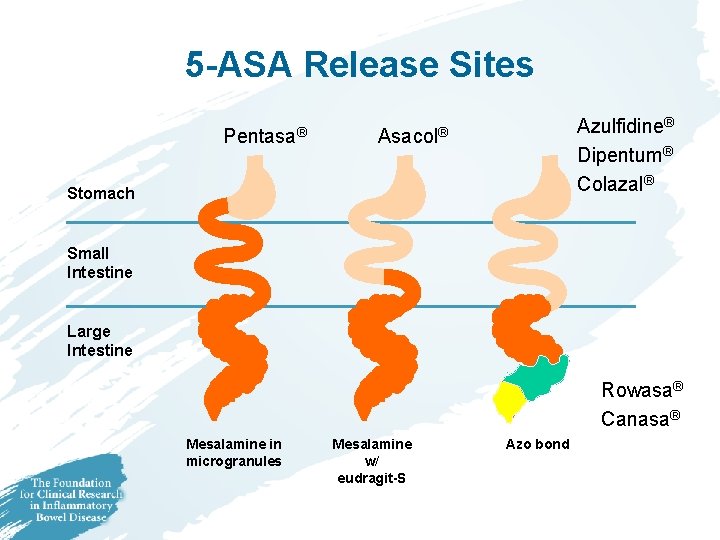
5 -ASA Release Sites Pentasa® Azulfidine® Dipentum® Colazal® Asacol® Stomach Small Intestine Large Intestine Rowasa® Canasa® Mesalamine in microgranules Mesalamine w/ eudragit-S Azo bond
Rationale for Topical Therapy 5 -ASA or Steroids • Treats the inflammation directly • Best initial choice for active ulcerative proctitis

Corticosteriods • Prednisone, Hydrocortisone, Medrol®, Decadron®, Cortenema®, Cortifoam®, ACTH • Administered by pill, IV or enema • Induce remissions in UC and CD • No maintenance benefits

Corticosteriods Benefits • Induces remissions in UC and CD • Quick fix • Inexpensive • Oral or rectal Risks • No long-term benefits • Numerous side effects – – – – Cushingoid changes Hypertension Diabetes Osteoporosis Acne Cataracts Depression Growth retardation

Antibiotics • Flagyl® (Metronidazole), Cipro® (Ciprofloxacin, Ampicillin, etc. ) • Treats mild symptoms of Crohn’s disease – Active disease when colon is involved – Peri-anal fistulae • Intravenous to treat severe colitis or infections such as abscess

Antibiotics Benefits • Mild-moderate CD • Fistula and peri-anal CD • Reduce recurrence after surgery (? ) Risks • Not effective in UC • Flagyl® (Metronidazole) – Neuropathy – Coated tongue – Yeast infections • Cipro® (Ciprofloxacin) – Yeast infections – Tendon injury

Immune-Modulators Imuran® (azathioprine) & Purinetheol® (6 -MP) • Long-term (maintenance) treatments for UC or CD – Can treat fistulas in CD over long-term • Primarily for patients unable to get off steroids • Requires continuous monitoring of blood counts

Immune-Modulators Imuran® (azathioprine) & Purinetheol® (6 -MP) Benefits • “Steroid-sparing” in UC and CD • Long-term maintenance • Relatively inexpensive Risks • Can lower blood counts and “immunity” – Small risk of infections • Requires long-term monitoring • Occasional allergies – Pancreatitis – Fever

Immune-Modulators • • • Imuran® (azathioprine) & Purinetheol® (6 -MP) Myths Facts Dangerous drugs used • Do not cause cancer to treat cancer • Can be used for more Cause cancer than 3 years Should not be used • If they don’t seem to longer than 3 years work at first, the dose needs to be reassessed If they don’t work over 3 -6 months, they will not • Can be used during work pregnancy, Must be stopped – Must be monitored before or during pregnancy

Cyclosporine Benefits • Effective in severe UC • Effective in Crohn’s disease? • Works rapidly Risks • Kidney damage • Increased infection, tumors, ?

Methotrexate • Used for many decades in Rheumatoid Arthritis • Useful in Crohn’s disease to reduce steroids • More effective given as injection once a week • Common side effects – Nausea, flu-like symptoms day of injection • Rare side effects – Liver disease and Pneumonia • Cannot be used if attempting pregnancy!!!

Biologic Therapy: Remicade® (infliximab) • Blocks the immune system reaction that causes inflammation • Rapidly relieves symptoms • Allows discontinuation of steroids without recurrence of symptoms • Can be given repeatedly over time to maintain remission

Biologic Therapy: Remicade® (infliximab) • • Benefits Induces and maintains remissions in CD Rapidly relieves symptoms & fistula drainage Steroid-sparing Effective even when otherapies fail • • Risks Allergic reactions to intravenous infusions Development of antibodies and loss of response Reactivation of TB and other rare infections Expensive

How is Remicade® administered? • Intravenous infusion • Allergic infusion reactions: 20% of patients – Usually manageable – Often preventable with repeated infusions • Discontinuation of therapy due to infusion reactions is rare
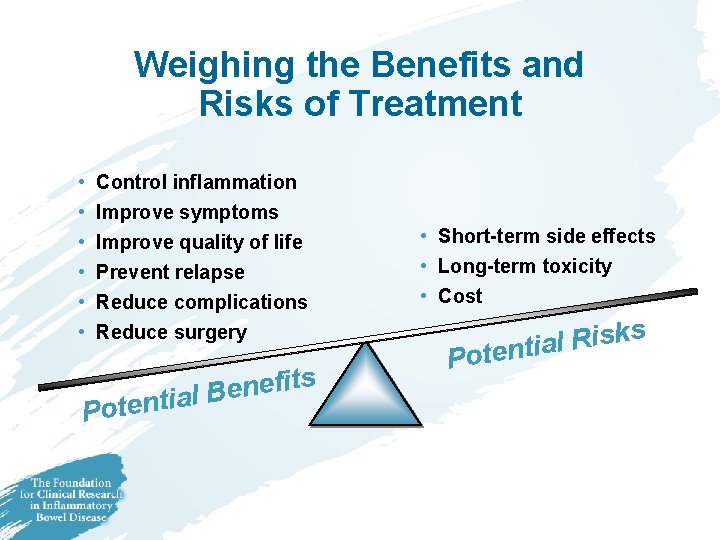
Weighing the Benefits and Risks of Treatment • • • Control inflammation Improve symptoms Improve quality of life Prevent relapse Reduce complications Reduce surgery Pote s t i f e ntial B • Short-term side effects • Long-term toxicity • Cost s k s i R l a i Potent

Managing Nutrition in IBD • Malnutrition can occur in IBD – Decreased intake of food • Symptoms • Overly zealous restriction – Decreased absorption of nutrients • Active disease, small intestine – Increased needs for calories and protein • Professional nutritional assessment • Tailor diet to individual needs & preferences • Dietary supplements

Managing Nutrition in IBD • Malnutrition can occur in IBD – Decreased intake of food • Symptoms • Overly zealous restriction – Decreased absorption of nutrients • Active disease, small intestine – Increased needs for calories and protein • Professional nutritional assessment • Tailor diet to individual needs & preferences • Dietary supplements

Surgery in IBD Ulcerative Colitis • Surgery (colectomy, removal of colon) is curative • Colectomy & ileostomy • Colectomy & ileo-anal anastomosis (J-pouch) Crohn’s Disease • Surgery does not cure • Disease recurs after a resection – Less after an “ostomy” • Resection of inflamed segments to treat complications or “refractory” disease

Surgery in IBD Ulcerative Colitis • Surgery (colectomy, removal of colon) is curative • Colectomy & ileostomy • Colectomy & ileo-anal anastomosis (J-pouch) Crohn’s Disease • Surgery does not cure • Disease recurs after a resection – Less after an “ostomy” • Resection of inflamed segments to treat complications or “refractory” disease

Ulcerative Colitis: Indications for Surgery • Failure to control severe attacks or toxic megacolon • Acute complications • Chronic symptoms despite medical therapy • Medication side effects without disease control • Dysplasia or Cancer

Crohn’s Disease: Indications for Surgery • Obstructing strictures • Complicating fistula • Peri-anal abscess • Toxic megacolon • Localized, unresponsive disease

Colorectal Cancer Risks in IBD • Compared to general population – Risk is 20 times higher and – Occurs at lower age • Risk is same for UC and CD according to: – How much of colon is affected – How long the disease is present – If patient has liver disease (PSC) • Risk is may be related to severity/activity of disease

Preventing Colon Cancer in IBD • Compliance with maintenance medications – 5 -ASA agents • Regular follow-up and surveillance colonoscopies – Every 1 -2 years after 10 years – Every year after 20 years • Colectomy (removal of colon) if: – Dysplasia (confirmed pre-cancerous changes) – Unwilling to continue surveillance examinations

Osteoporosis and IBD • Bone (skeletal) disease characterized by low bone density (mass) • Increased “fragility” of bone • Susceptibility to breaks (fractures) – Particularly of spine (vertebrae) and hip

Osteoporosis in IBD Risk Factors • Steroid therapy • Smoking • Active disease – Crohn’s disease > Ulcerative Colitis • Females – Small stature – Family history – Post-menopausal

Preventing Osteoporosis in IBD • Check bone density (DEXA or heel scan) • Control active disease • Weight bearing exercise • Supplement calcium and vitamin D (Crohn’s disease or steroids) • Bisphonates if low bone density – Actonel® or Fosomax®

IBD & Pregnancy • Fertility is normal if disease is controlled • Fertility is reduced in active disease • Pregnancy outcomes are normal – Low birth weight/prematurity if active disease – NO INCREASED RISK OF BIRTH DEFECTS • Risk of active disease after delivery – Stay on maintenance medications

IBD Medications & Pregnancy • Medications that are safe: – 5 -ASA agents – Steroids • Low risk of cleft palate – Most antibiotics – Imuran® (Azathioprine) and Purinethol® (6 -MP) – Remicade®(Infliximab) • MUST BE AVOIDED – Methotrexate

Research in IBD Where are We Heading?
Genetic Research • Identify the gene locations – Family studies – Correlate genes with clinical patterns • Identify the gene(s) – Likely multiple – Protective genes/harmful genes • Identify function of genes • How to manipulate genes

Research in the Environment • Identify bacteria capable of causing disease – Measles virus, Mycobacteria Paratuberculosis • Identify “normal” bacteria that produce “abnormal” immune response – Bacterial-Epithelial interactions • Identify gene-microorganism interactions – Do immune systems mistake “self” for bacteria?

Options for Environmental Causes • Treat patient if “infected” • Eradicate from the environment • Immunize to prevent “infection”

Research in Surgery • Ileo-anal pouches – Preventing, treating Pouchitis • Minimal invasive surgery – Laparoscopy • Prevention of post-operative recurrence – Select subgroups – 6 -MP, 5 -ASA, antibiotics, biologics(? )

IBD Summary • Ulcerative Colitis and Crohn’s disease are chronic diseases requiring longterm medical therapy • Quality of Life is impaired during flare-ups and should be normal during remissions • Life expectancy is same as general population • Surgery cures Ulcerative Colitis & treats complications in Crohn’s disease
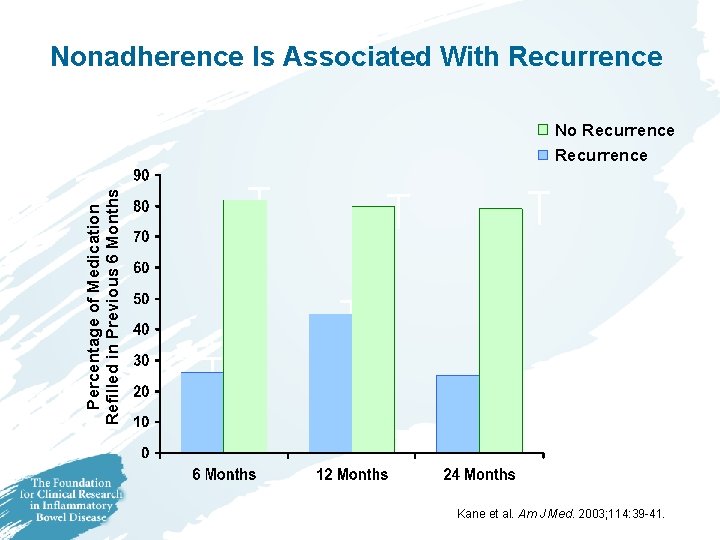
Nonadherence Is Associated With Recurrence No Recurrence Percentage of Medication Refilled in Previous 6 Months Recurrence Follow-up Kane et al. Am J Med. 2003; 114: 39 -41.
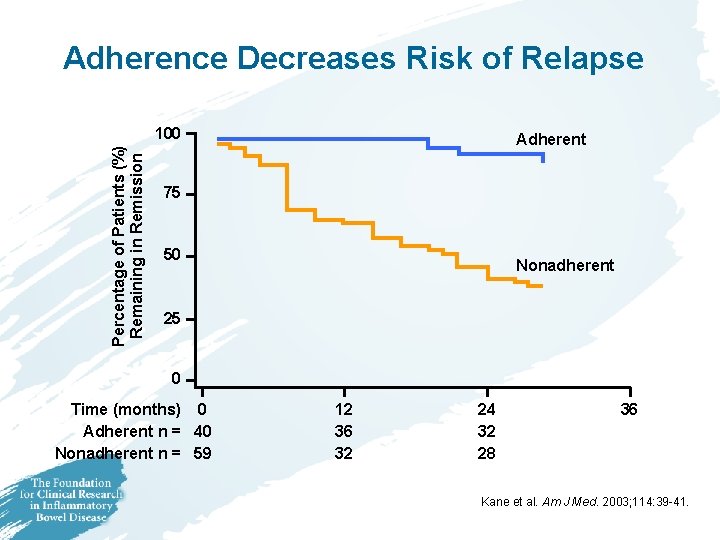
Adherence Decreases Risk of Relapse Percentage of Patients (%) Remaining in Remission 100 Adherent 75 50 Nonadherent 25 0 Time (months) 0 Adherent n = 40 Nonadherent n = 59 12 36 32 24 32 28 36 Kane et al. Am J Med. 2003; 114: 39 -41.

for more information: www. healthtalk. com
- Slides: 94