Advances in Hip Arthroplasty James Bried M D

Advances in Hip Arthroplasty James Bried, M. D. Fellowship-Trained Orthopedic Surgeon

Outline 1. 2. 3. 4. 5. Indications and Eligibility Requirements Surgical Technique Anterior vs. Posterior Hip Replacement Managing Post Surgical Pain Outcome Data
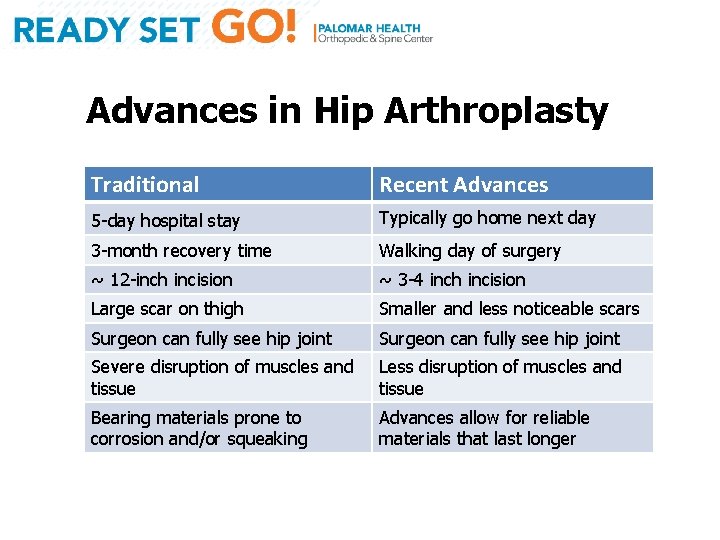
Advances in Hip Arthroplasty Traditional Recent Advances 5 -day hospital stay Typically go home next day 3 -month recovery time Walking day of surgery ~ 12 -inch incision ~ 3 -4 inch incision Large scar on thigh Smaller and less noticeable scars Surgeon can fully see hip joint Severe disruption of muscles and tissue Less disruption of muscles and tissue Bearing materials prone to corrosion and/or squeaking Advances allow for reliable materials that last longer

Indications and Eligibility Requirements 4
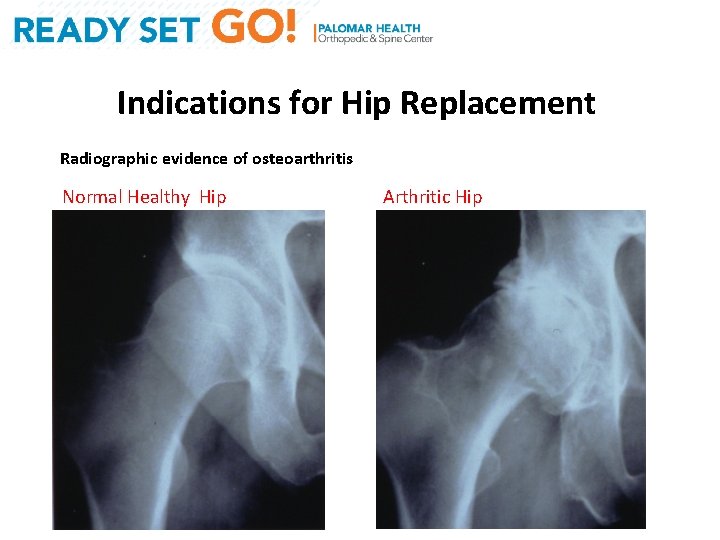
Indications for Hip Replacement Radiographic evidence of osteoarthritis Normal Healthy Hip Arthritic Hip

Indications for Hip Replacement (contd. ) • Difficulty walking, going up stairs, and bending to get in and out of chairs • Pain is moderate to severe even while resting • Stiffness that affects the patient’s range of motion during normal activities • Failure of non-surgical treatments, such as non -steroidal anti-inflammatory drugs (NSAIDs), physical therapy, steroid injections, or the use of a cane or walker

Contraindications for Hip Replacement Palomar’s guidelines: When Is Surgery Right for You?

Contraindications for Hip Replacement (contd. )
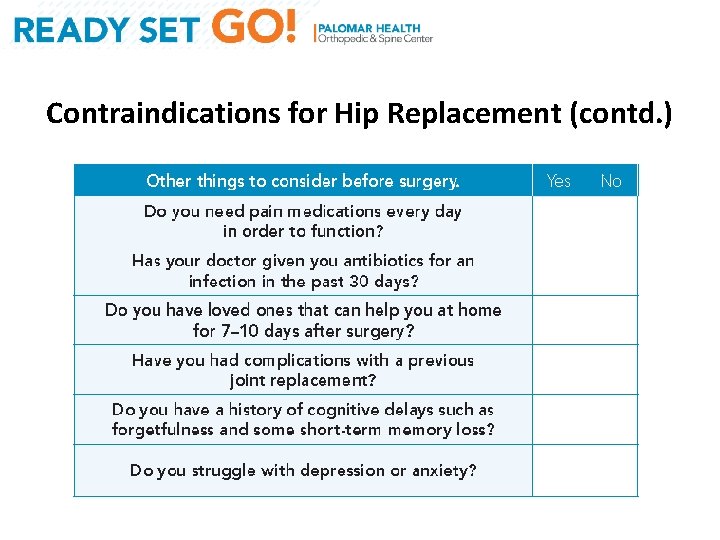
Contraindications for Hip Replacement (contd. )

Surgical Technique 10
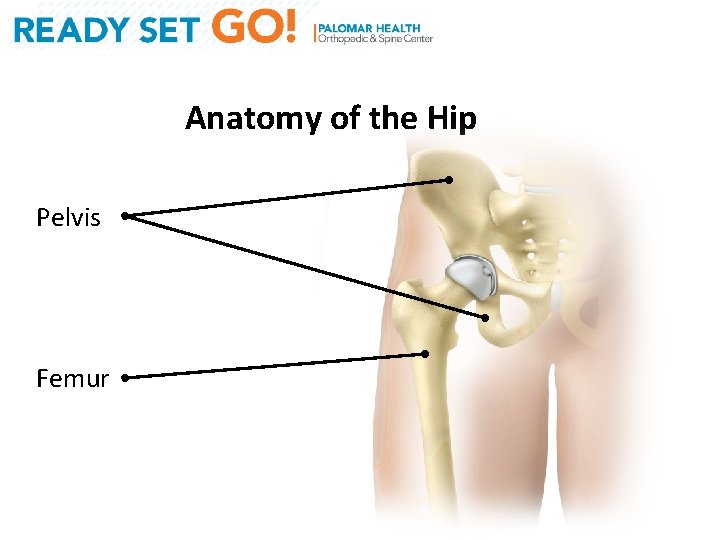
Anatomy of the Hip Pelvis Femur
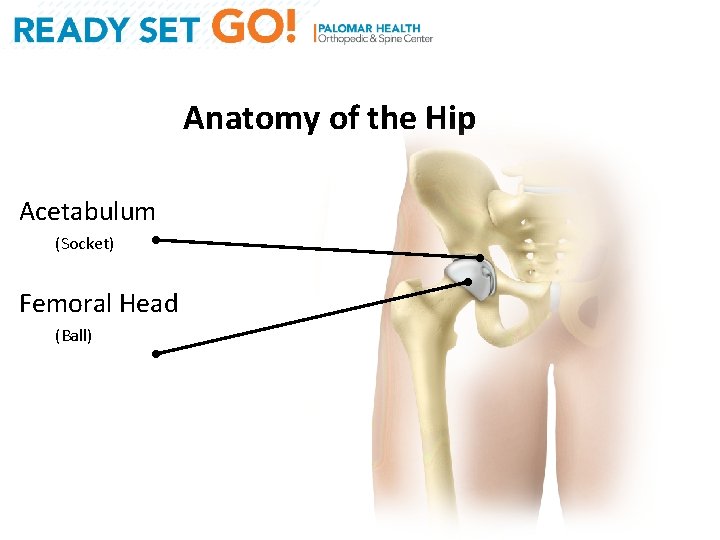
Anatomy of the Hip Acetabulum (Socket) Femoral Head (Ball)
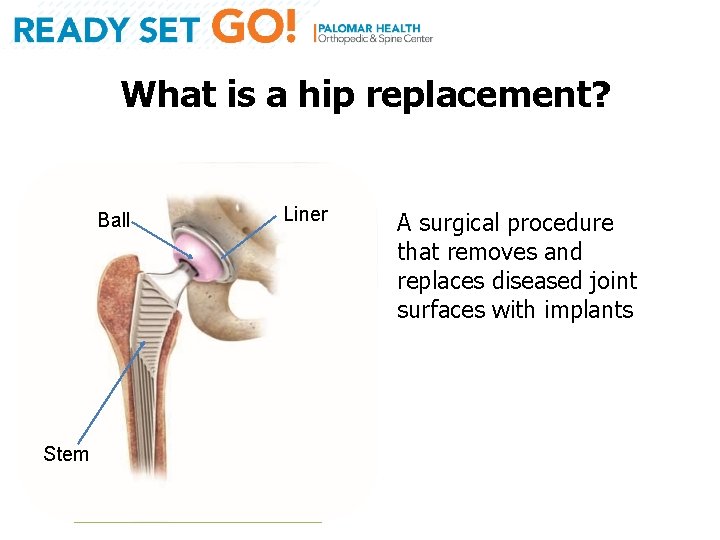
What is a hip replacement? Ball Stem Liner A surgical procedure that removes and replaces diseased joint surfaces with implants
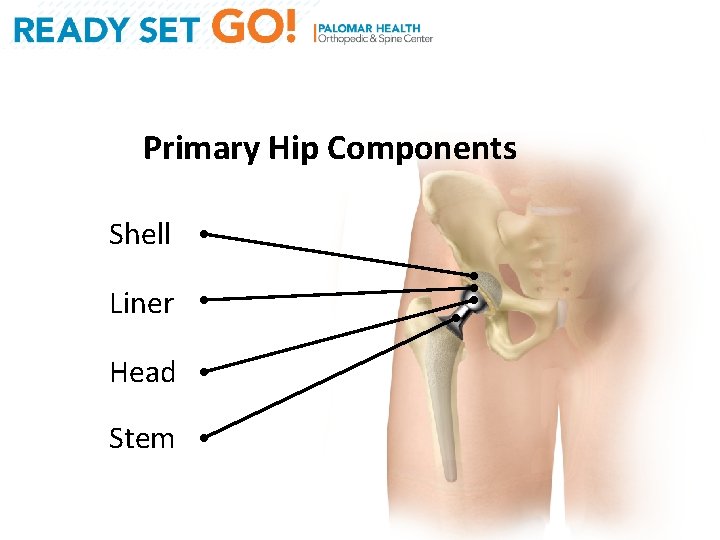
Primary Hip Components Shell Liner Head Stem
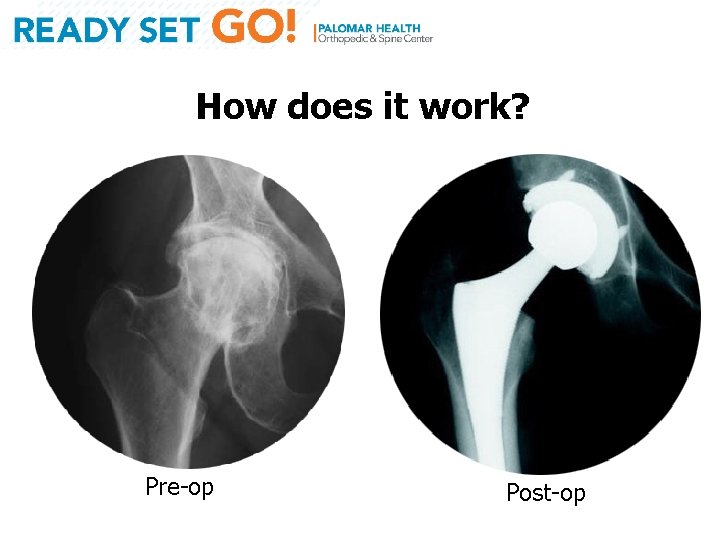
How does it work? Pre-op Post-op
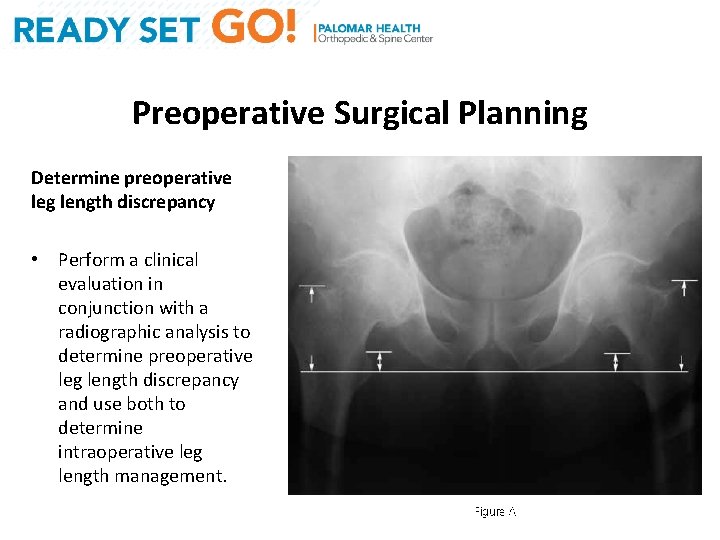
Preoperative Surgical Planning Determine preoperative leg length discrepancy • Perform a clinical evaluation in conjunction with a radiographic analysis to determine preoperative leg length discrepancy and use both to determine intraoperative leg length management.
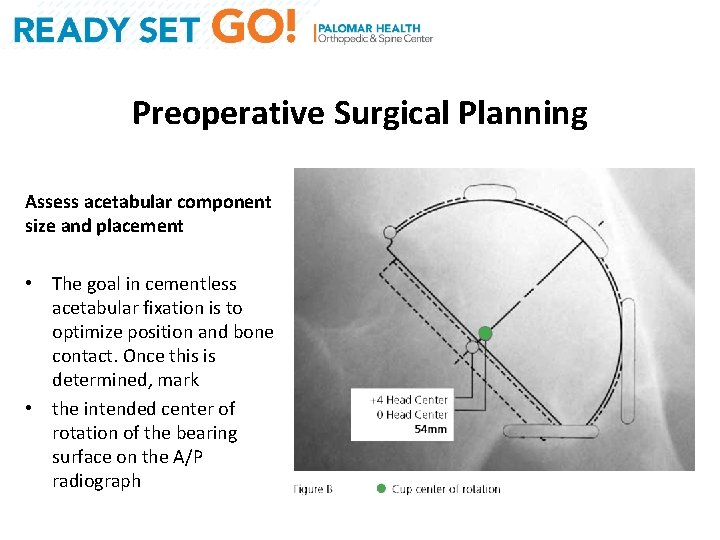
Preoperative Surgical Planning Assess acetabular component size and placement • The goal in cementless acetabular fixation is to optimize position and bone contact. Once this is determined, mark • the intended center of rotation of the bearing surface on the A/P radiograph
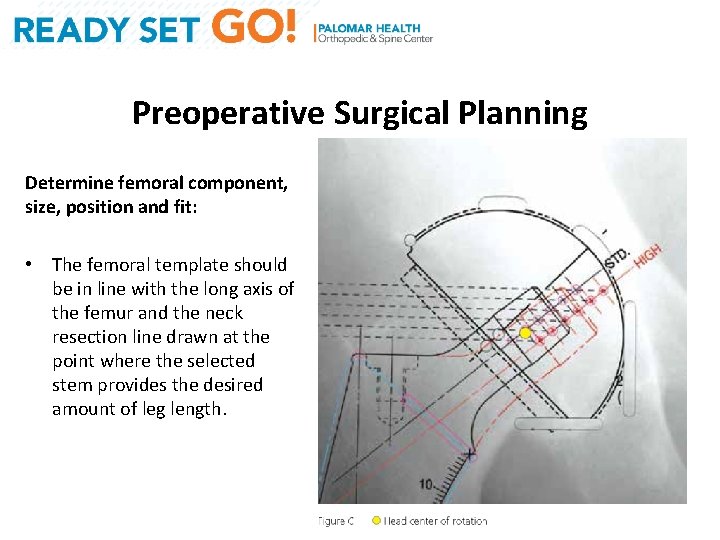
Preoperative Surgical Planning Determine femoral component, size, position and fit: • The femoral template should be in line with the long axis of the femur and the neck resection line drawn at the point where the selected stem provides the desired amount of leg length.
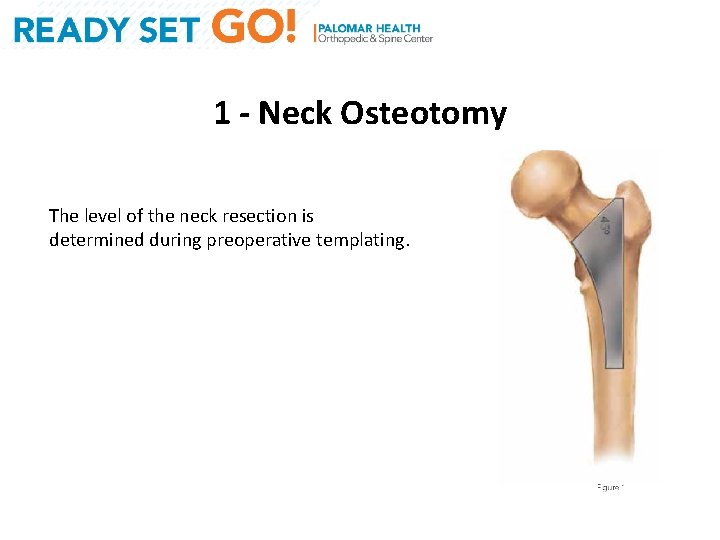
1 - Neck Osteotomy The level of the neck resection is determined during preoperative templating.
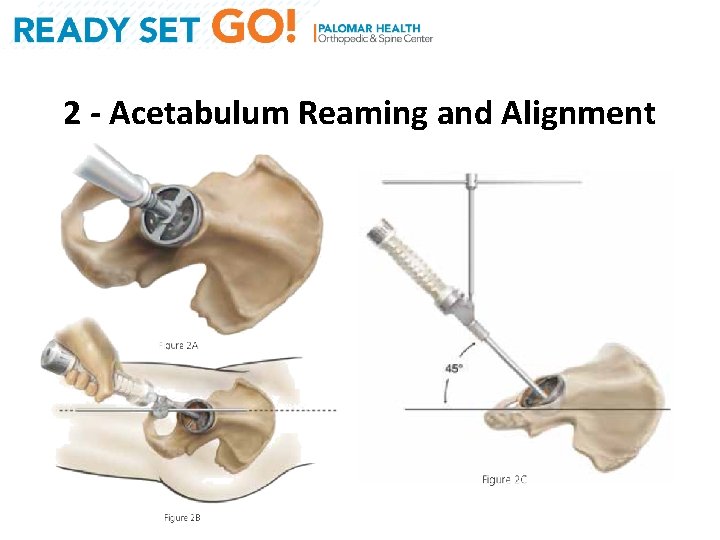
2 - Acetabulum Reaming and Alignment
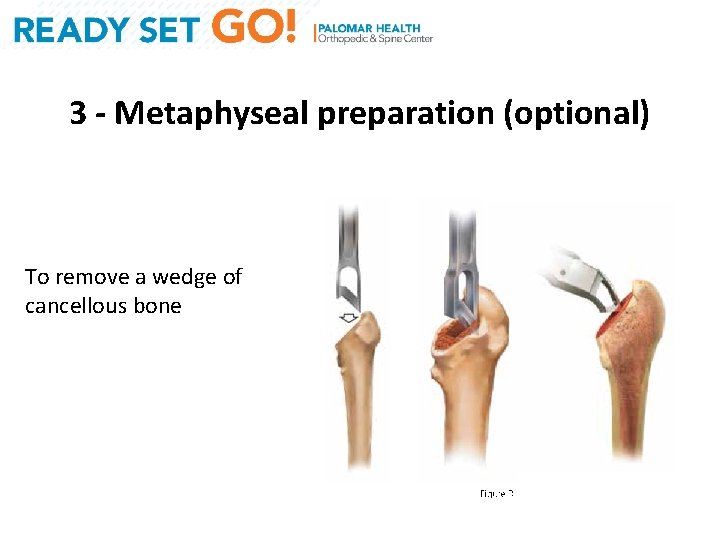
3 - Metaphyseal preparation (optional) To remove a wedge of cancellous bone
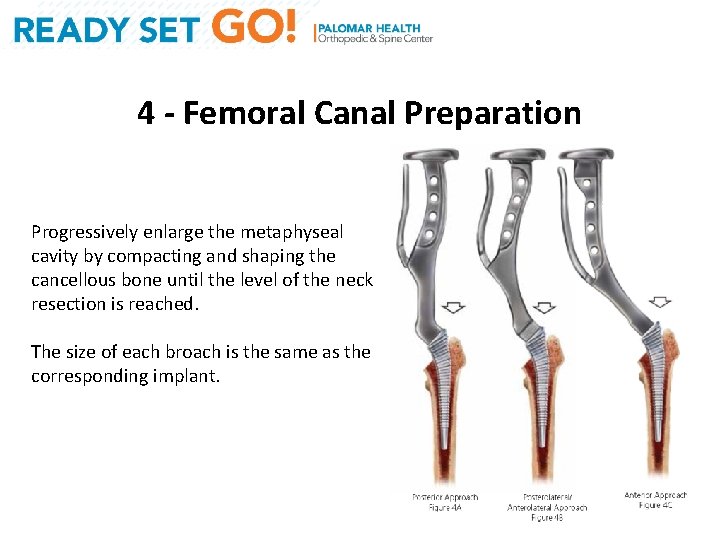
4 - Femoral Canal Preparation Progressively enlarge the metaphyseal cavity by compacting and shaping the cancellous bone until the level of the neck resection is reached. The size of each broach is the same as the corresponding implant.
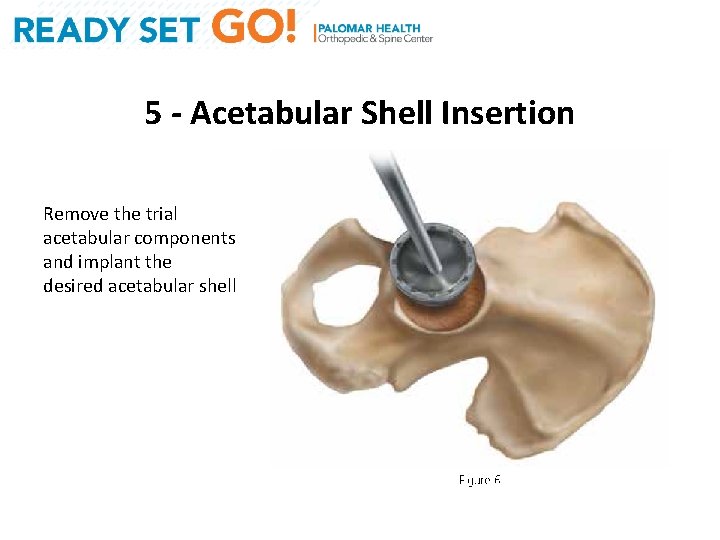
5 - Acetabular Shell Insertion Remove the trial acetabular components and implant the desired acetabular shell
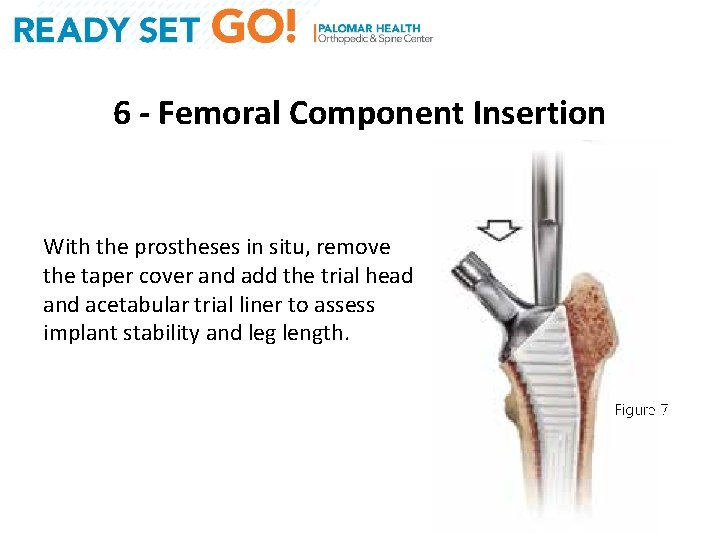
6 - Femoral Component Insertion With the prostheses in situ, remove the taper cover and add the trial head and acetabular trial liner to assess implant stability and leg length.
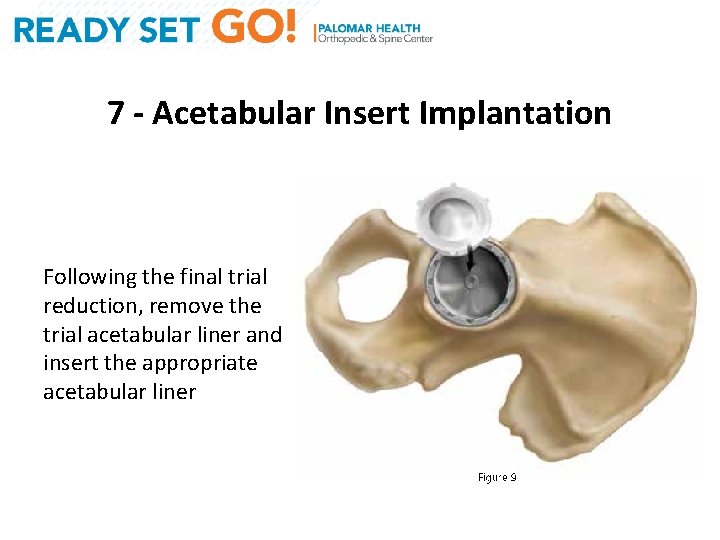
7 - Acetabular Insert Implantation Following the final trial reduction, remove the trial acetabular liner and insert the appropriate acetabular liner
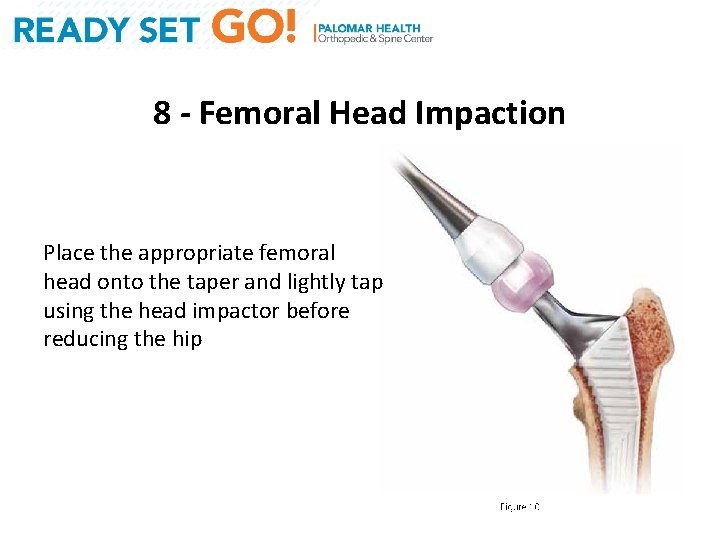
8 - Femoral Head Impaction Place the appropriate femoral head onto the taper and lightly tap using the head impactor before reducing the hip


Demand-Match the Patient to the Implant • Range of motion • Stability • Wear characteristics • Lifestyle • Age, weight & gender • Severity of disease Bearing options: • • • Metal-on-plastic (polyethylene) Metal-on-metal Ceramic-on-plastic (polyethylene) Ceramic-on-ceramic Ceramic-on-metal
Potential Complications • • Infection Blood clots Implant breakage Malalignment Nerve or artery damage Persistent pain Premature wear - other factors can affecting longevity

Follow-Up Visits • Every three months during the first year • Occasional visits after first year • Bi-Annual visits – Regular check-ups will assist in preventing complications

Returning to Low-Impact Daily Activities • Golfing, swimming between one to two months • Patients restricted from high-impact activities – Running – Jumping – Jogging – Contact sports – Heavy manual labor

Anterior vs. Posterior Hip Replacement 32
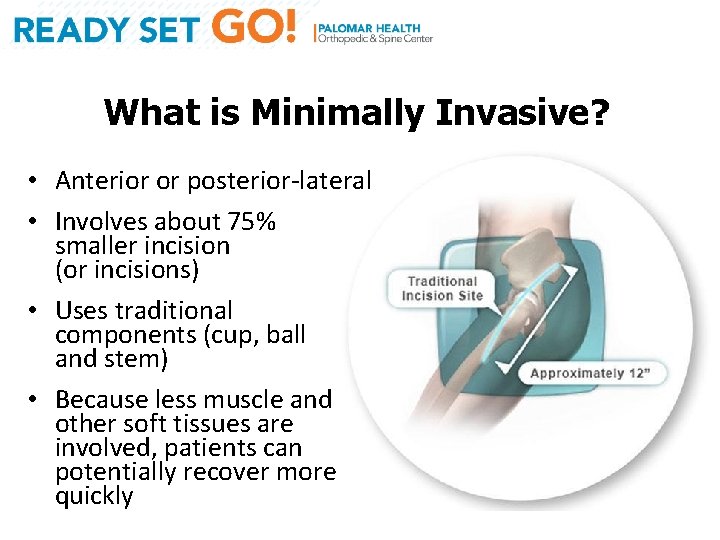
What is Minimally Invasive? • Anterior or posterior-lateral • Involves about 75% smaller incision (or incisions) • Uses traditional components (cup, ball and stem) • Because less muscle and other soft tissues are involved, patients can potentially recover more quickly
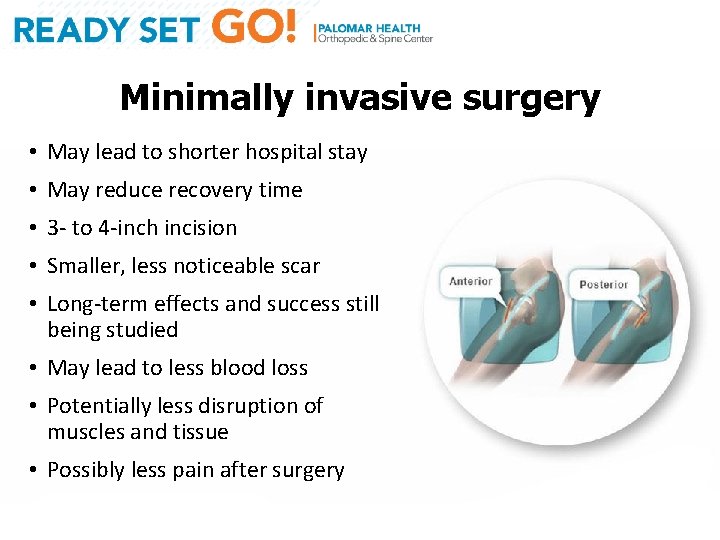
Minimally invasive surgery • May lead to shorter hospital stay • May reduce recovery time • 3 - to 4 -inch incision • Smaller, less noticeable scar • Long-term effects and success still being studied • May lead to less blood loss • Potentially less disruption of muscles and tissue • Possibly less pain after surgery

Does surgical approach impact hip replacement outcomes? • Study of 274 patients (anterior vs. posterior) • 6 -month measurements; pain, function and qualityof-life • Results: surgical approach alone is not the singular variable that yields a difference in six-month postoperative outcome “It’s the surgeon, not the approach” SOURCE: Benson, J. G. , MD, et al (2016). American Academy of Orthopaedic Surgeons: 2016 Annual Meeting. Orlando, FL: Are Patient-Reported Outcomes Different After Anterior Versus Posterior Approach to Total Hip Arthroplasty?

Managing Post Surgical Pain 36

The Palomar Health Pain Protocol A multi-disciplinary team convened by orthopedic surgeons, and included; anesthesiologists, pharmacists, Clinical Nurse Specialists, physical therapists, and bedside orthopedic RNs. Goals: • Decrease post-operative pain, • reduce physician variation, • improve patient compliance with ambulation and exercises, • increase patient satisfaction, and • reduce patient falls.
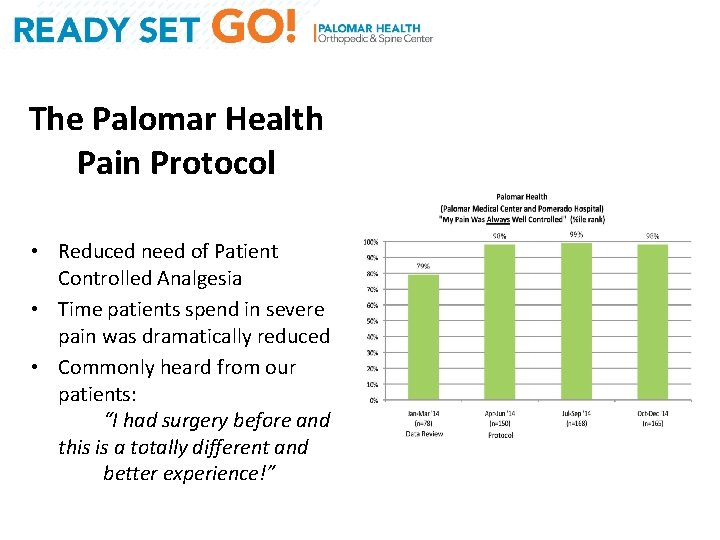
The Palomar Health Pain Protocol • Reduced need of Patient Controlled Analgesia • Time patients spend in severe pain was dramatically reduced • Commonly heard from our patients: “I had surgery before and this is a totally different and better experience!”

Outcome Data 39
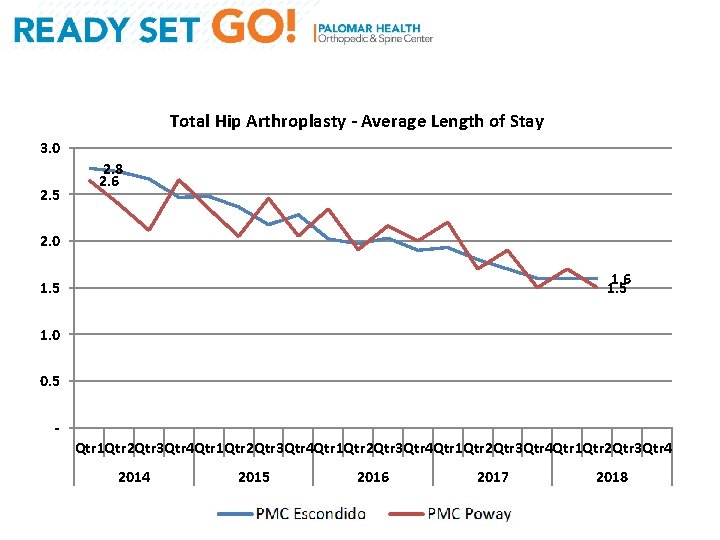
Total Hip Arthroplasty - Average Length of Stay 3. 0 2. 5 2. 8 2. 6 2. 0 1. 6 1. 5 1. 0 0. 5 - Qtr 1 Qtr 2 Qtr 3 Qtr 4 Qtr 1 Qtr 2 Qtr 3 Qtr 4 2015 2016 2017 2018
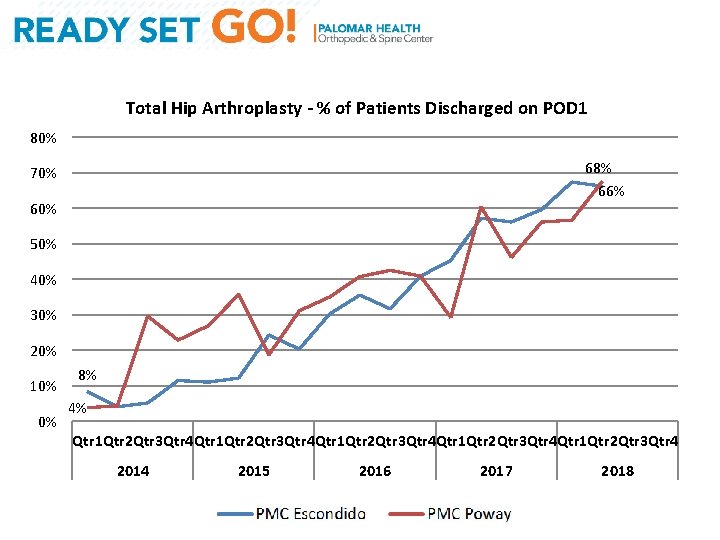
Total Hip Arthroplasty - % of Patients Discharged on POD 1 80% 68% 66% 70% 60% 50% 40% 30% 20% 10% 0% 8% 4% Qtr 1 Qtr 2 Qtr 3 Qtr 4 Qtr 1 Qtr 2 Qtr 3 Qtr 4 2015 2016 2017 2018
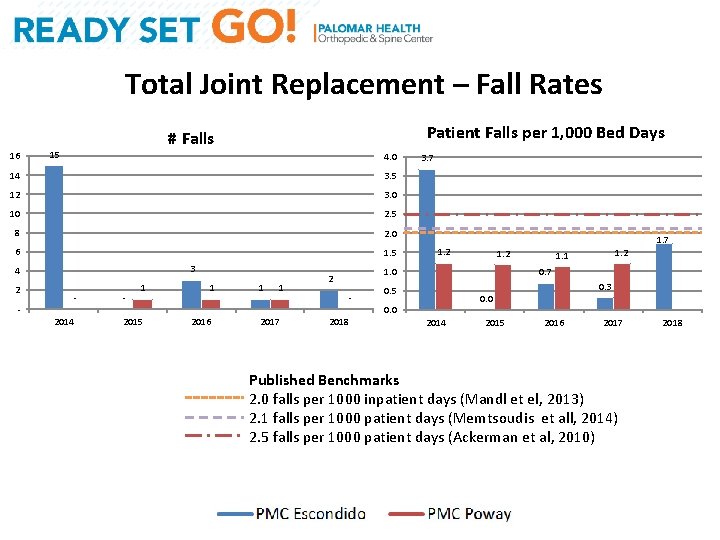
Total Joint Replacement – Fall Rates 16 Patient Falls per 1, 000 Bed Days # Falls 15 4. 0 14 3. 5 12 3. 0 10 2. 5 8 2. 0 6 1. 5 3 4 2 - 2014 - 1 2015 1 2016 1 1 2017 3. 7 1. 2 1. 0 2 2018 1. 2 1. 1 0. 7 0. 5 0. 3 0. 0 2014 2015 2016 2017 Published Benchmarks 2. 0 falls per 1000 inpatient days (Mandl et el, 2013) 2. 1 falls per 1000 patient days (Memtsoudis et all, 2014) 2. 5 falls per 1000 patient days (Ackerman et al, 2010) 2018
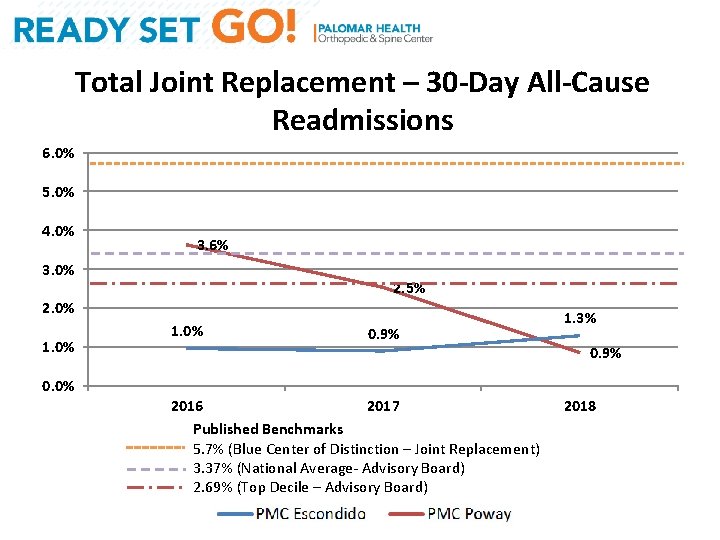
Total Joint Replacement – 30 -Day All-Cause Readmissions 6. 0% 5. 0% 4. 0% 3. 6% 3. 0% 2. 5% 2. 0% 1. 0% 0. 9% 1. 3% 0. 9% 0. 0% 2016 2017 Published Benchmarks 5. 7% (Blue Center of Distinction – Joint Replacement) 3. 37% (National Average- Advisory Board) 2. 69% (Top Decile – Advisory Board) 2018
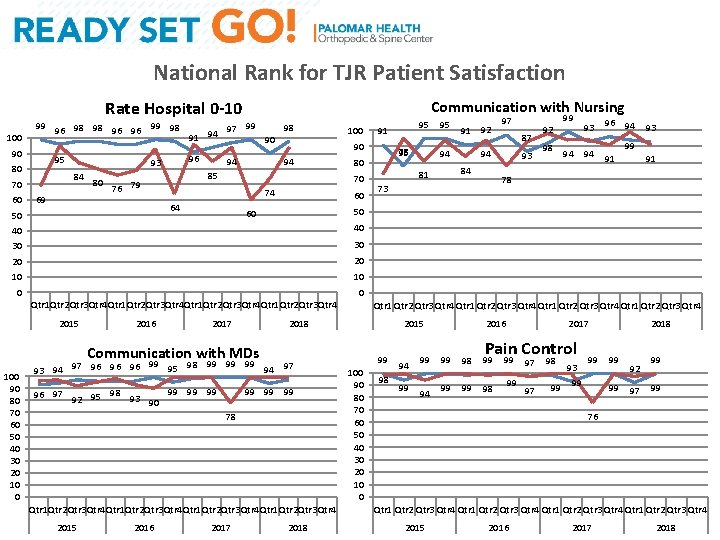
National Rank for TJR Patient Satisfaction Communication with Nursing Rate Hospital 0 -10 100 99 96 98 98 96 96 99 98 90 95 80 60 96 93 84 70 69 80 98 97 99 91 94 90 94 85 76 79 74 60 30 30 20 20 10 10 0 Qtr 1 Qtr 2 Qtr 3 Qtr 4 Qtr 1 Qtr 2 Qtr 3 Qtr 4 2017 99 99 99 78 Qtr 1 Qtr 2 Qtr 3 Qtr 4 Qtr 1 Qtr 2 Qtr 3 Qtr 4 2015 2016 2017 94 92 84 81 97 87 94 93 92 98 99 94 93 96 94 91 94 93 99 91 78 73 Qtr 1 Qtr 2 Qtr 3 Qtr 4 2018 99 95 98 99 99 99 94 97 93 94 97 96 96 96 99 99 99 96 97 92 95 98 93 90 91 0 2015 Communication with MDs 100 90 80 70 60 50 40 30 20 10 0 95 50 60 40 2016 78 95 80 40 2015 91 90 70 64 50 94 100 95 2018 99 100 90 80 70 60 50 40 30 20 10 0 98 94 99 99 94 2016 2017 Pain Control 99 98 99 99 97 97 98 99 93 99 99 2018 99 99 92 97 99 99 76 Qtr 1 Qtr 2 Qtr 3 Qtr 4 2015 2016 2017 2018

What’s Next for Total Hip Arthroplasty • Started measuring long-term functional outcomes (HOOS and KOOS) in August 2018 • Achieve zero avoidable readmissions and SSIs • At-home recovery vs. Skilled Nursing
- Slides: 45