Advanced Laboratory Technique Lab 4 A L Lamieaa

Advanced Laboratory Technique Lab 4 A. L. Lamieaa Gh. Fajir

Swab coolecting swabs are often taken for microbiological analysis. Swabs are taken primarily for two reasons: - To identify organisms in wounds known or suspected to be infected; - As part of screening programes to identify patients who may be carrying infections without displaying any signs or symptoms.

The swab taken will undergo testing to identify the any organism that may be present. The three common tests are: - Microscopy - inspection using a microscope to identify organisms; - Culture - placing in an environment optimal for organism growth, usually for 48 -72 hours, after which it is re-examined for further growth; - Sensitivity - identified organisms are exposed to various antibiotics to ascertain which will be an effective treatment and any it is resistant to.

Collecting swabs Wound swabs. Obtain the specimen prior to any dressing or cleaning procedure of the wound. This will maximise the material obtained and prevent killing of the organism by the use of antiseptics. Use a sterile swab and gently rotate on the area to collect exudate from the wound and place into transport medium. Where there is pus collect as much as possible in a sterile syringe and put in a plain sterile container (do not use a swab) and send to the laboratory. For detection of Mycobacterium tuberculosis, pus collected neat into a pot or tissue biopsy is preferred, however a calcium alginate swab can be used. The alginate swab gradually dissolves maximising the isolation of the organism as the number of organisms is usually small.

Wound swab

Ear Swab No antibiotics or otherapeutic agents should have been in the aural region for about three hours prior to sampling the area as this may inhibit the growth of microorganisms. �Place a sterile swab into the outer ear and gently rotate to collect the secretions. �If there is purulent discharge this should be sampled. �For deeper ear swabbing a speculum may be used. Only experienced medical staff should undertake this procedure as damage to the eardrum may occur. �Place swab in transport medium.
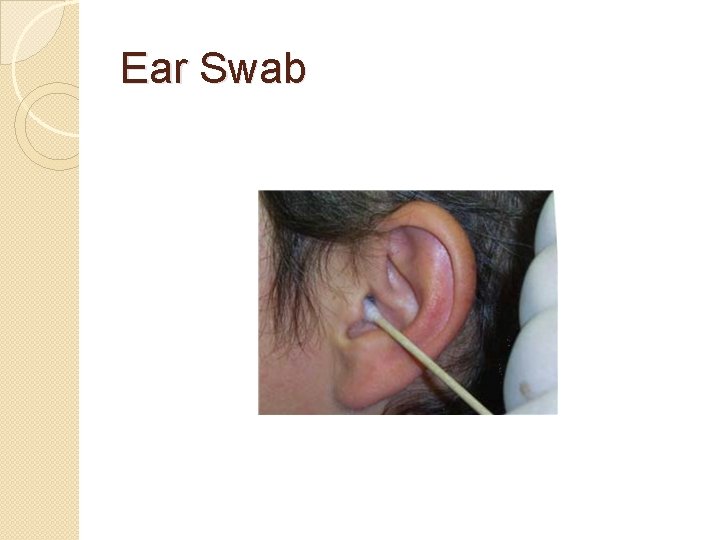
Ear Swab

Throat swab Specify on the laboratory form if this is a routine admission screen for methicillin-resistant Staphylococcus aureus (MRSA) or a swab for the investigation of a suspected infection. For the collection of throat swabs as part of screening for MRSA refer to the clinical guideline for the control of Meticillin-resistant Staphylococcus aureus (MRSA). � Place the child or the person in a position with a good light source. This will ensure maximum visibility of the tonsillar bed. � Either depress the tongue with a spatula or ask the person to say “aahh”. The procedure is likely to cause gagging and the tongue will move to the roof of the mouth. This can prevent accurate sampling it is therefore important to quickly but gently rub the swab over the tonsillar bed or area where there is exudate or a lesion. � Care should be taken not to contaminate the swab by contact with the tongue or the oral mucosa on removal. � Return swab to the container with transport medium. � For viral investigation same as above and place in viral transport medium.
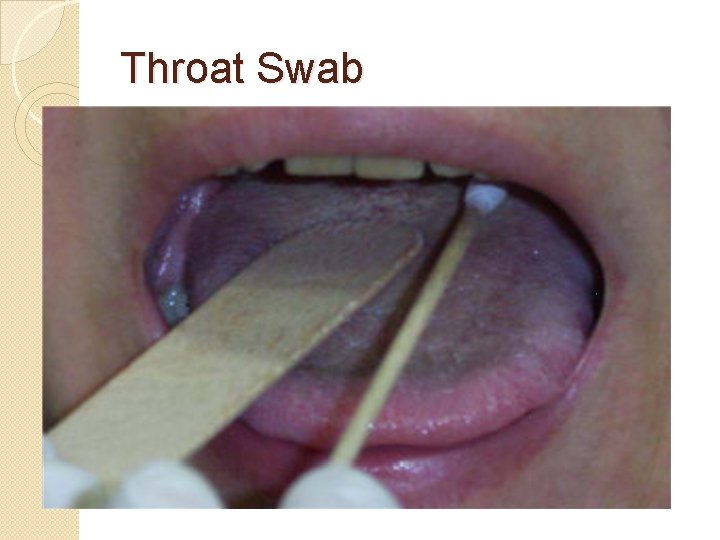
Throat Swab

Nose. Swab Specify on the lab form if this is a routine admission screen for MRSA or for the investigation of a suspected infection. For the collection of nose swabs as part of screening for MRSA refer to the clinical guideline for the control of Meticillin-resistant Staphylococcus aureus (MRSA). 1)If the nose is dry, moisten the swab in sterile 0. 9% saline solution beforehand to enhance the collection of material and alleviate discomfort. 2)Insert the swab into the anterior nares and direct it up into the tip of the nose and gently rotate. Both nares should be swabbed using the same swab to obtain adequate material. 3)Place in transport medium. 4)For viral investigation same as above and place in viral transport medium. 5)The outside of the nostrils may be rubbed after the procedure to alleviate the unpleasant sensation of swabbing.
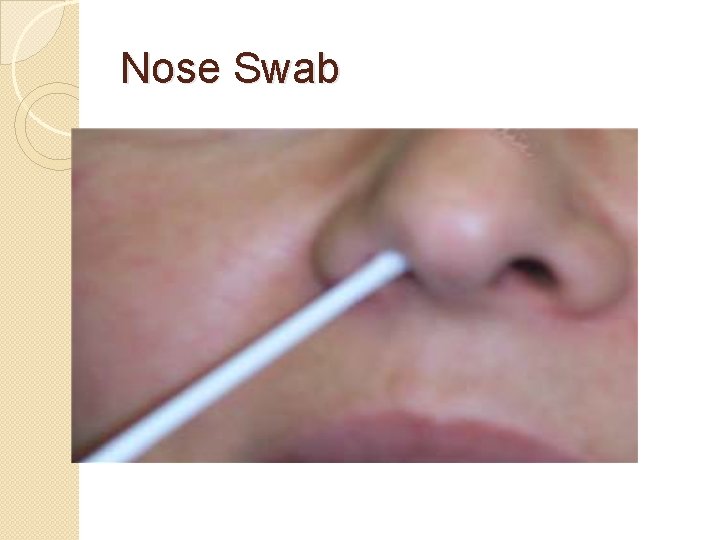
Nose Swab

Cerebrospinal Fluid (CSF) Cerebrospinal fluid (CSF) collection is a test to look at the fluid that surrounds the brain and spinal cord. CSF acts as a cushion, protecting the brain and spine from injury. The fluid is normally clear. It has the same consistency as water. The test is also used to measure pressure in the spinal fluid. Alternative Names Spinal tap; Ventricular puncture; Lumbar puncture; Cisternal puncture; Cerebrospinal fluid culture
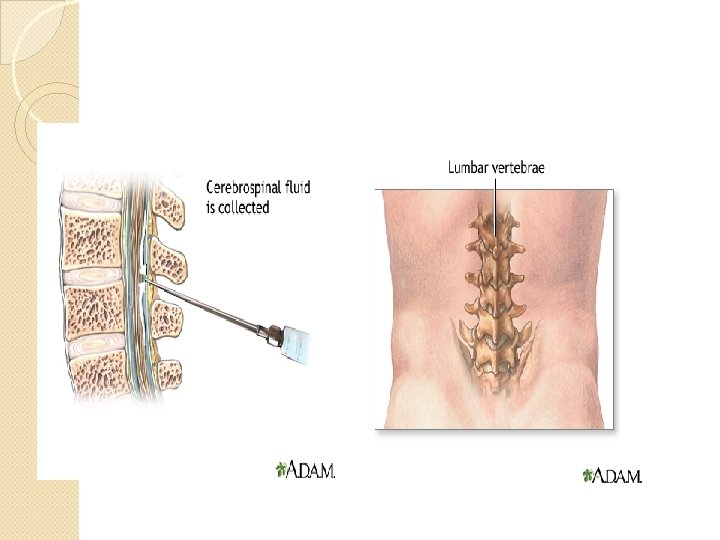

Cerebrospinal Fluid Sampling of cerebrospinal fluid (CSF) is essential for the accurate diagnosis of infectious meningitis and may aid in the diagnosis of encephalitis. Cerebrospinal fluid is most commonly obtained via a lumbar puncture performed by medical staff. A sterile technique is required as there is a risk of introducing infection itself causing meningitis. Specimens of CSF should be dispatched to the laboratory immediately. Outside normal working hours, it is essential that the on-call laboratory staff are contacted when the sample is being transported. It is important not to store the specimen in a refrigerator as this may cause the cells to deteriorate or lyse giving rise to misleading results. It is common practice to send three separate collection tubes of CSF when investigating for evidence of subarachnoid haemorrhage, as the initial part of the sample may be contaminated with blood from outside the sub-arachnoid space.

If this is performed, it is important to label the tubes as such and specifically request counts on the first and third samples. It is also important to remember that a CSF glucose level (sent separately to chemical pathology) can only be accurately interpreted in conjunction with a simultaneous plasma glucose level.
- Slides: 15