Advanced Imaging for Early Prostate Cancer Staging When




















- Slides: 30

Advanced Imaging for Early Prostate Cancer Staging When to Image Based on Choosing Wisely® and ACR Appropriateness Criteria®

What Is R-SCAN? § Collaborative activity for referring clinicians and radiologists to improve patient care through clinical improvement § R-SCAN Collaboration Goals: § Ensure patients receive the most appropriate imaging exam at the most appropriate time based on evidence -based appropriate use criteria § Reduce unnecessary imaging tests focused on imaging Choosing Wisely® topics § Lower the cost of care 2

Why Participate? § R-SCAN Offers: 3 § Data-driven system for moving toward value-based imaging and patient care § Opportunity to focus on highly relevant imaging exams to improve utilization § Collaborators can fulfill their Improvement Activity requirements under the MIPS § Easy way to practice with clinical decision support (CDS) technology § In preparation for PAMA § Free and immediate access to Web-based tools and CME activities

Problem: Unnecessary Use of CT, bone, PET scans in Staging of Low Risk Prostate Cancer § Multiple studies have shown CT and radionuclide bone scans do not improve detection of metastatic disease in men with low risk prostate cancer. § A 2004 study looked at the efficacy of bone and CT scans in prostate cancer from 23 studies of bone scans and 25 studies of CT. § Bone scans detected metastases in 2. 3% of men with PSA < 10 ng/m. L and 5. 6% of men with Gleason scores ≤ 7. § CT detected metastases in 0. 7% of men with clinically localized disease and 1. 2% of men with Gleason scores ≤ 7, with nodal metastases detected in no patients with PSA < 20 ng/m. L [1]. 4 § FDG PET scans involve technical challenges, making FDG unpopular for prostate cancer detection and staging generally. § CT and bone scans in the low risk population may produce incidental findings causing patient anxiety, using clinician time to explain them, and resulting in further unnecessary testing and cost.

Using Evidence to Guide Imaging Ordering § Choosing Wisely campaign § Collaborative effort between ABIM Foundation and over 70 medical specialty societies § Helps patients and medical professionals avoid wasteful or unnecessary medical tests, treatments, and procedures § Many medical associations agree that CT scans are not necessary in the staging of early prostate cancer at low risk for metastasis, including: § American Society of Clinical Oncology § American Urological Association 5

Using Evidence to Guide Imaging Ordering ® § ACR Appropriateness Criteria § Assist referring physicians and other providers in making the most appropriate imaging or treatment decisions for specific clinical conditions § Employs input of physicians from other medical specialties and societies to provide important clinical perspectives 6

ACR Appropriateness Criteria: The Facts § 178 clinical imaging topics and over 875 clinical variants § Basic access is free § Learn more at acr. org/ac 7

ACR Appropriateness Criteria for Prostate Cancer–Pretreatment Detection, Surveillance, and Staging Variant 1: Clinically suspected prostate cancer, no prior biopsy (biopsy naïve). Detection. Variant 2: Clinically suspected prostate cancer, prior negative TRUSguided biopsy. Detection. Variant 3: Clinically established low-risk prostate cancer. Active surveillance. Variant 4: Clinically established intermediate-risk prostate cancer. Staging and/or surveillance. Variant 5: Clinically established high-risk prostate cancer. Staging. 8

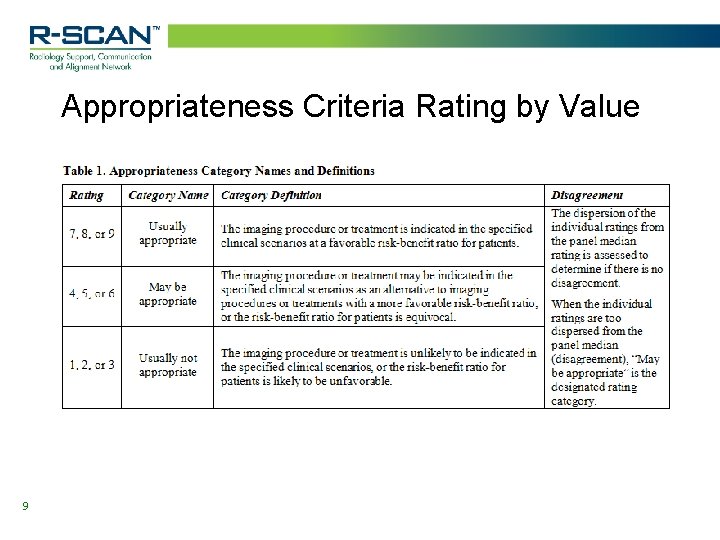
Appropriateness Criteria Rating by Value 9

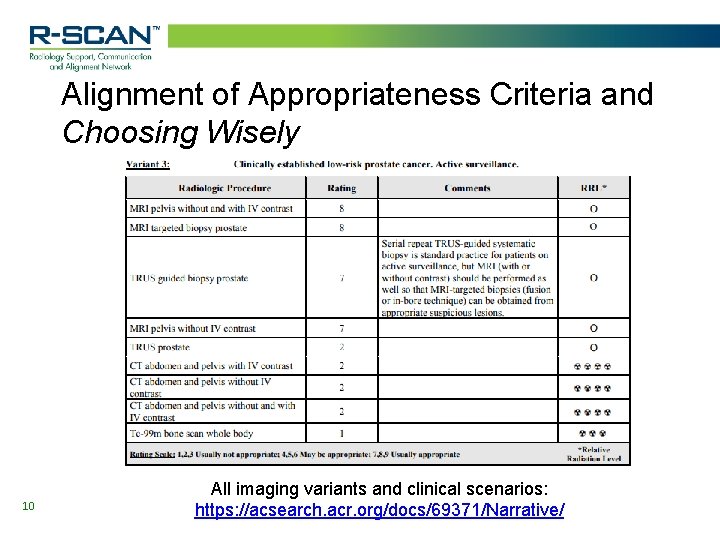
Alignment of Appropriateness Criteria and Choosing Wisely 10 All imaging variants and clinical scenarios: https: //acsearch. acr. org/docs/69371/Narrative/

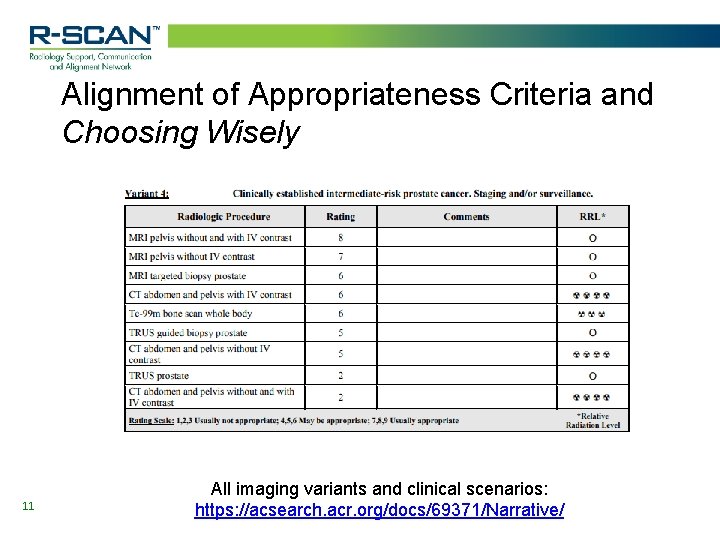
Alignment of Appropriateness Criteria and Choosing Wisely 11 All imaging variants and clinical scenarios: https: //acsearch. acr. org/docs/69371/Narrative/

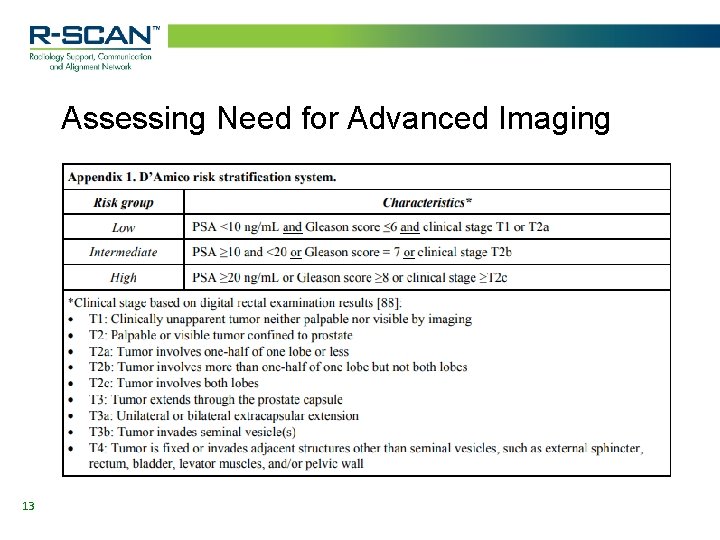
Assessing Need for Advanced Imaging § Standard clinical tools, such as digital rectal examination, serum prostate-specific antigen (PSA) assay, and systematic biopsy results such as fraction of cores positive for cancer and Gleason score are used to determine prostate risk stratification. § The D’Amico risk stratification system classifies low risk prostate cancer in patients who have all of the following: § PSA <10 ng/m. L § Gleason sum ≤ 6 § Clinical stage T 1 -T 2 a 12

Assessing Need for Advanced Imaging 13

Assessing Need for Advanced Imaging 14 § The primary role of CT in prostate cancer is the detection of nodal metastases. The poor performance of CT for detection of nodal metastases has been confirmed in recent studies. § Bone scintigraphy remains the standard test used for detection of bone metastases. § Patients with low risk prostate cancer are unlikely to have metastatic disease documented by bone scan or CT. Therefore, these scans are generally not recommended unless higher risk disease has been established. § Evidence has emerged that MRI or MRI-targeted biopsy may be appropriate for detection and active surveillance in low risk men, and can provide better evaluation when compared with traditional systematic biopsy.

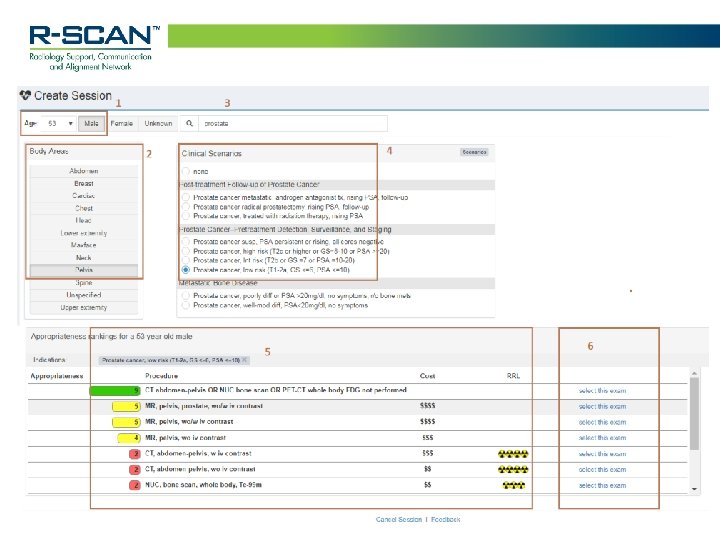
R-SCAN and Clinical Decision Support § Care. Select is a web-based version of the ACR Appropriateness Criteria, comprising over 3, 000 clinical scenarios and 15, 000 imaging indications § Care. Select provides evidence-based decision support for the appropriate utilization of medical imaging procedures § R-SCAN participants gain free access to a customized, web-based version of Care. Select, a helpful first step for aligning ordering patterns with appropriate use criteria 15

Getting Started With R-SCAN rscan. org 16

17

18

19

20

R-SCAN Early Prostate Cancer Staging Educational Resources 1. 2. 3. 21 Visit: rscan. org Click: Resources Click: Topicspecific Resources § Podcast § Imaging Order Simulation activity § Articles § Materials to share with patients

R-SCAN Resources With CME § Podcast § A radiologist and referring physician discuss appropriate image ordering for early prostate cancer staging; approved for. 5 CME § Learn more § Imaging Order Simulation Activity § Test your knowledge in selecting the best imaging exam for various indications § Free with CME 22

Key Points: Talking With Patients Here are talking points to explain to patients why imaging is not necessary for low risk prostate cancer: § If the Gleason test shows that you have low risk prostate cancer, you usually do not need more testing. Evidence has shown the cancer is not likely to have spread to other organs, and that CT and bone scans do not produce useful results in low risk patients. § Additional imaging may produce incidental findings, requiring further tests and time just to confirm they are benign. § CT scans expose you to a strong dose of radiation, which can increase your risk for cancer. In some cases, it’s the same as having about 200 chest x-rays. § Certain costs associated with imaging are not covered by insurance, such as payments to meet deductible thresholds and co-pays. 23

Self-Assessment Question Which of the following characterize low risk prostate cancer? A. PSA <10 ng/m. L B. Gleason sum ≤ 6 C. Clinical stage T 1 -T 2 a D. All of the above 24

Case 1 § A 60 -year-old man presents with a recent diagnosis of prostate cancer (Gleason score = 2; low risk). § Questions: § What imaging would be most appropriate for this patient? § What other questions would you ask? § What is the focus of your physical exam? 25

Case 2 § A 71 -year-old man with prostate cancer is diagnosed with transrectal ultrasound-guided biopsy (with a Gleason score of 7) and is clinically staged as T 2 b. § Questions: § What imaging would be most appropriate for this patient? § What other questions would you ask? § What is the focus of your physical exam? 26

Blank slide for radiologist to add custom info 27

Blank slide for radiologist to add custom info 28

Summary § Evidence has shown that men who are risk stratified into the low risk prostate cancer group do not benefit from CT or bone scans, since their early stage cancer is unlikely to have metastasized to other organs. § FDG PET scans are considered a modality not generally selected for this scenario. § Use the D’Amico risk stratification system to identify patients as low risk. § Radiation, cost, and time (of both patients and clinicians) are not worth the low yield of metastatic findings from CT and bone scans in this population. 29

Questions? 30