Adrenergic Antagonists Adrenergic Blocking Agents Affect BPdecreased PVR

Adrenergic Antagonists
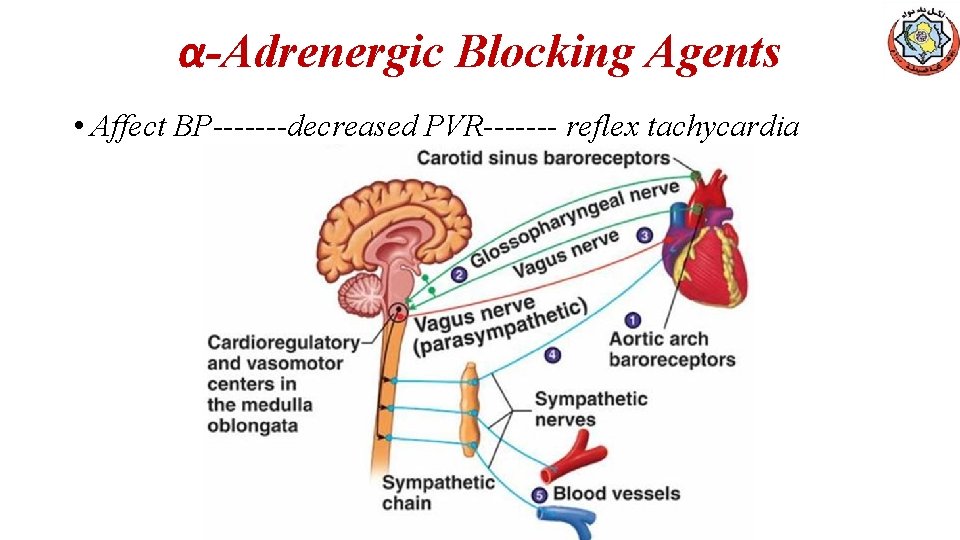
α-Adrenergic Blocking Agents • Affect BP-------decreased PVR------- reflex tachycardia

Phenoxybenzamine • Nonselective, irreversible, noncompetitive • Decrease PVR ----- reflex tachycardia • α 2 block----- increased CO ? ? ? • Pretreatment with phenoxybenzamine followed by Epi? ? ? • Used in Pheochromocytoma (before surgery or inoperable tumor) & in Raynaud disease • SEs: postural hypotension, nasal stuffiness, NV, sexual disturbances, & reflex tachycardia

Phentolamine • Competitive, nonselective α-blocker (4 hrs) • Postural hypotension • Reflex cardiac stimulation • CI in patients with coronary artery disease • Used locally to prevent T necrosis • Used for short term treatment of Pheochromacytoma • Useful in hypertensive crisis due to clonidine abrupt withdrawal & in (tyamine + MAOIs)

Prazocin, Terazocin, Doxazocin, Tamsulosin, Alfuzocin • Selective, competitive α 1 -blockers useful in hypertension • Tamsolosin & alfuzocin used in benign prostatic hyperplasia (BPH) • Metabolized & excreted in urine except for doxazocin • Doxazocin have long duration of action • Decreases PVR, BP (venous & arterial effect) • Minimum effect on CO, RBF, & glomer. Filtration rate • Tamsulosin has the least vascular effect (α 1 B) & higher effect on prostate (α 1 A)

α-blockers cont. • 1 st dose effect • Modest improvement in lipid profile & glucose metabolism in hypertension • SEs: dizziness, lack of energy, headache, orthostatic hypotension, Floppy iris syndrome • α-blockers + vasodilators (ex. Nitrates or PDEIs)? ? ? • Sexual dysfunction

Yohimbine • Selective, copmetetive α 2 -blocker • Treat erectile dysfunction • Increases CNS sympathetic out flow • CI in CVDs, psychiatric conditions & renal dysfunction

β-Adrenergic Blocking Agents • Competetive, nonselective β 1 & β 2 • Differ in intrinsic sympathomimetic activity, CNS effects, blockade of sympathetic Rs, vasodilation & kinetics • Decrease BP • No postural hypotension ? ? ? • Used in Hpertension, Angina, Arrhythmia, MI, HF, Hyperthyroidism, Glaucoma & prophylaxis of Migraine headache • All cpds end with (– olol)

Propranolol (nonselective) • CVS: • Decrease CO, -ve inotropic, chronotropic, & AV & SA inhibition--- • Decrease CO, workload, & oxygen consumption------- • Useful in supravent. Arrhythmia but not in vent. arrhythmia • Peripheral vasoconstriction(β 2, reflex response • Increase PVR ---- • Reflex vasoconst. ---- • In Hypertensive patients, total PVR return to normal ore below • Gradual decreasae in syst. & diast. BP

Propranolol (cont. ) üBronchoconstriction (precipitate COPD) üGlucose metabolism (glycogenolysis, Glucagon) ü Prop. + Isoproterenol üProp + Epi ? ? ? üProp + NE ? ? ?

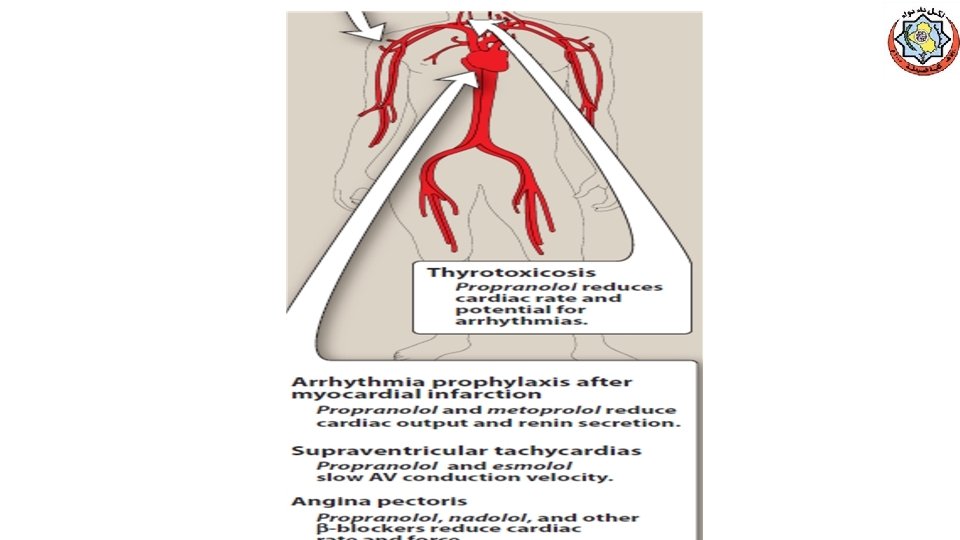
Therapeutic uses: • Hypertension (normotensive ? ? ? ) ØDecrease CO ØInhibit renin release from kidney ØDecrease total PVR ØDecrease sympathetic outflow • Angina, (chronic management of stable angina) • Myocardial infarction Ø Prophylactic Ø Immediate administration, …. . ? Ø Reduce incidence of sudden arrhythmic death after MI • Migraine (prophylactic, lipid soluble) • Hyperthyroidism

Propranolol (cont. ) üKinetics (absorption, metabolism, BBB) üAdverse effects: • Bronchoconstriction • Arrhythmia (upregulation, ppt arrhythmia) • Sexual impairment • Metabolic disturbances: ØGlycogenolysis, glucagon Øppt symptoms of hypoglycemia -----? ØMobilize energy molecules ex. FFA(lipase activation, β 2, β 3 , bad, good cholesterol, selective β 1 ) • CNS effects (CNS dep. , fatigue, weakness, ------, selective β antag. )

Drug interaction • Inhibitors: cimetidine, fluoxetine, paroxetine, and ritonavir • Inducers: barbiturates, phenytoin, and rifampin

Nadolol, Timolol: non-selective β agents • Non-selective • More potent than prop. • Nadolol: long duration • Timolol, betaxolol, carteolol------glaucoma (open-angle glaucoma, piloarpine? ? ? )

Acebutolol, Atenolol, Betaxolol, Bisoprolol, Esmolol, Metaprolol, & Nebivolol Selective β 1 antagonists • • Β 1 selective, no bronchoconstriction (β 2) This occurs at doses 50 – 100 fold less than β 1 This effect disappear at high doses So SEs are predictable • • Used for hypertension & to increase exercise tolerance in angina Esmolol given IV, short duration of action? ? ? Fewer effects on pulmonary system, PVR, & CHO metabolism ? ? ? nevibolol releases NO from endothelial SMs------? • Uses ? ? ?

Therapeutic uses: Ø hypertensive patients with impaired pulmonary function Øfirst-line therapy for chronic stable angina Ø Bisoprolol and the extended-release formulation of metoprolol are indicated for the management of chronic heart failure ØRaynaud phenomenon) is less frequent? ? ?

Acebutolol, Pindolol: antagonists with Partial Agonist Activity • Acebutolol β 1 selective antagonist • Pindolol nonselective β blocker • With Intrinsic Sympathomimetic Activity (ISA)? ? ? • Diminished effect on heart • Β blockers with ISA minimize disturbances in lipid & CHO metabolism compared with other β blockers • Effective in hypertensive patients with bradycardia

Labetalol & Carvedilol: antagonists of both α & β adrenoceptors • Labetalol, carvedilol: nonselective β-blocker with α 1 blocking effect---- • Decrease BP • Carvedilol decrease lipid peroxidation, vascular wall thickening, so useful in HF • Labetalol replaced methyldopa in pregnancy hypertension & used in hypertensive crisis (IV) • SEs include orthostatic hypot. & dizziness

Clinical Uses of β-blockers

Drugs Affecting Neurotransmitter Reuptake or Release EMT: extraneuronal MAO transporter, NET: neuronal noradrenal; ine transporter


Drugs Affecting Neurotransmitter Release or Uptake Reserpine (plant alkaloid): ØBlocks Mg/adenosine triphosphate (biogenic amine transporter) ØSlow onset of action, long duration of action ØUsed in hypertension replaced with newer drugs
- Slides: 24