Adrenalectomy from the back Dr Leung Yuen Ki

Adrenalectomy from the back Dr Leung Yuen Ki Department of Surgery, Kwong Wah Hospital

Content �Anatomy of the adrenal glands �Indication of different surgical approaches �Surgical technique of retroperitoneal adrenalectomy (RPA) �Outcome of transperitoneal adrenalectomy (TPA) vs RPA �Learning curve of RPA �Special condition: Phaeochromocytoma
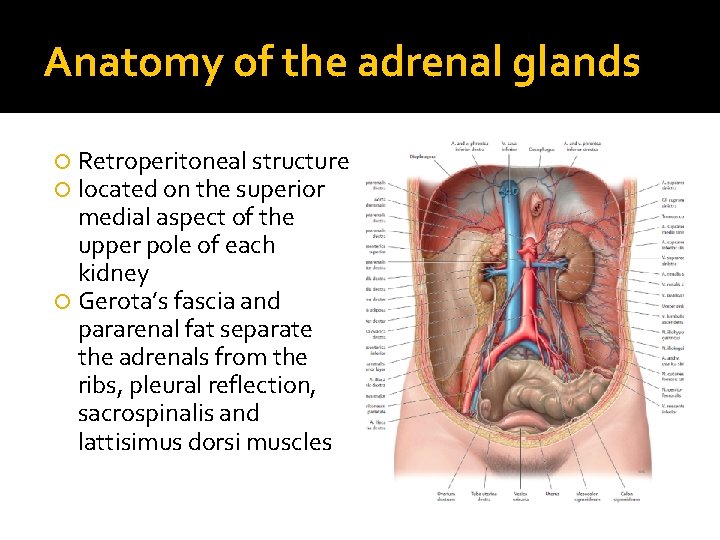
Anatomy of the adrenal glands Retroperitoneal structure located on the superior medial aspect of the upper pole of each kidney Gerota’s fascia and pararenal fat separate the adrenals from the ribs, pleural reflection, sacrospinalis and lattisimus dorsi muscles

Minimal Access Adrenalectomy � 2 main approaches �Laparoscopic transperitoneal (TPA) or the retroperitoneal approach (RPA) �Transperitoneal approach is favored by many because of the familiarity of intraperitoneal anatomy and larger working space

Transperiotneal Approach �Transperiotneal laparoscopic adrenalectomy was first described in 1992 �Now considered the gold standard for the removal of most benign adrenal tumors Gagner M, et al. Laparoscopic adrenalectomy in Cushing’s syndrome and pheochromocytoma. N Engl J med. 1992; 327: 1033 Higashihara E, et al. A case report of laparoscopic adrenlaectomy. Nihon hinyokika Gakkai Zasshi. 1992; 83: 1130 -1133.

Approach by indication �Dictated by surgeon expertise Laparoscopic transabdominal adrenalectomy (TPA) Laparoscopic retroperiotneal adrenalectomy (RPA) • Large tumours (>8 cm) • Obese patients • Potential need for other abdominal procedures • History of extensive upper abdominal surgeries • Bilateral adrenalectomy • Primary functioning tumors (size < 67 cm) • Metastasis (< 4 cm and without infiltration of surrounding structures) Agaoglu O, et al, Selection algorithm for posterior versus lateral approach in laparoscopic adrenalectomy. Surgery 2012; 151: 731
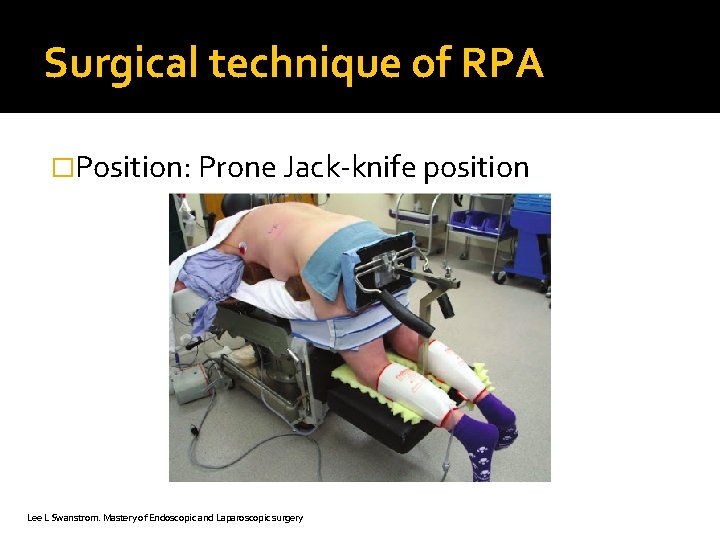
Surgical technique of RPA �Position: Prone Jack-knife position Lee L Swanstrom. Mastery of Endoscopic and Laparoscopic surgery
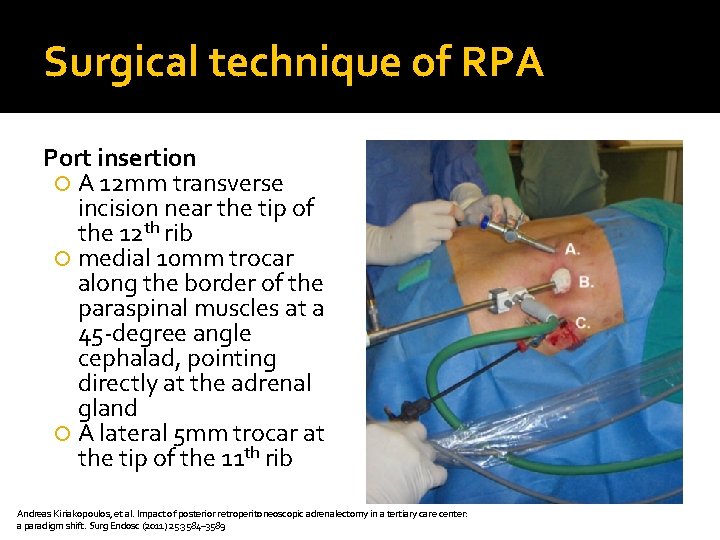
Surgical technique of RPA Port insertion A 12 mm transverse incision near the tip of the 12 th rib medial 10 mm trocar along the border of the paraspinal muscles at a 45 -degree angle cephalad, pointing directly at the adrenal gland A lateral 5 mm trocar at the tip of the 11 th rib Andreas Kiriakopoulos, et al. Impact of posterior retroperitoneoscopic adrenalectomy in a tertiary care center: a paradigm shift. Surg Endosc (2011) 25: 3584– 3589
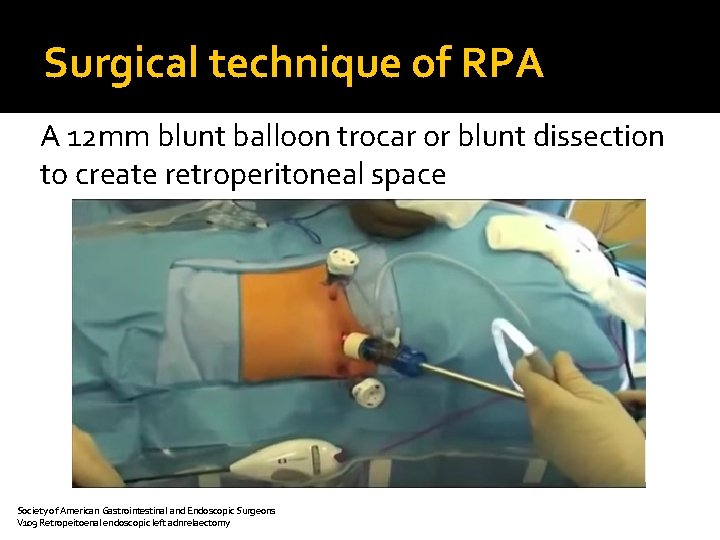
Surgical technique of RPA A 12 mm blunt balloon trocar or blunt dissection to create retroperitoneal space Society of American Gastrointestinal and Endoscopic Surgeons V 109 Retropeitoenal endoscopic left adnrelaectomy
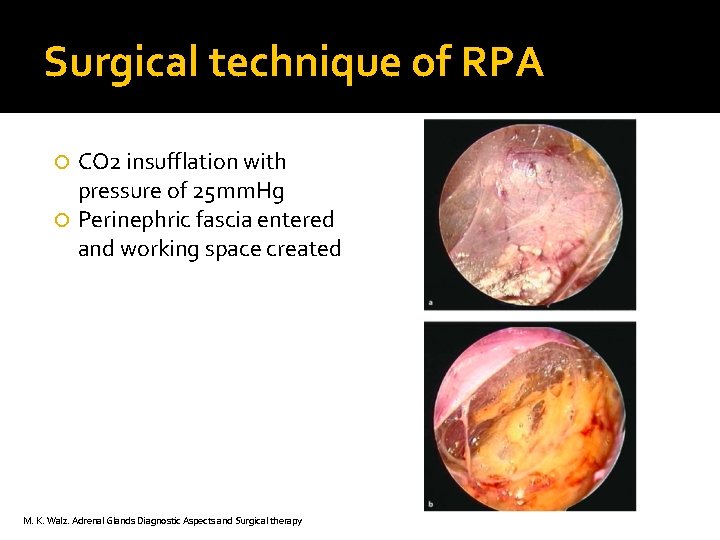
Surgical technique of RPA CO 2 insufflation with pressure of 25 mm. Hg Perinephric fascia entered and working space created M. K. Walz. Adrenal Glands Diagnostic Aspects and Surgical therapy

Creation of working space � Retroperitoneal insufflation pressures of 20 to 25 mm. Hg greatly facilitate exposure � Do not result in the adverse hemodynamic consequences if these pressure achieved within the peritoneal cavity � Higher CO 2 pressures tend to tapenade bleeding from small vessels, further improving visibility. Giebler RM, Behrends M, Steffens T, et al. Intraperitoneal and retroperitoneal carbon dioxide insufflation evoke different effects on caval vein pressure gradients in humans: evidence for the starling resistor concept of abdominal venous return. Anesthesiology. 2000; 92: 1568– 1580. Giebler RM, Kabatnik M, Stegen BH, et al. Retroperitoneal andintraperitoneal CO 2 insufflation have markedly different cardiovascular effects. J Surg Res 1997; 68: 153– 160. Giebler RM, Walz MK, Peitgen K, Scherer RU. Hemodynamic changes after retroperitoneal CO 2 insufflation for posterior retroperitoneoscopic adrenalectomy. Anesth Analg 1996; 82: 827– 831.

Left sided RPA Adrenal vein in space between the gland diaphragmatic branch medial to the upper pole of the kidney Walz et al. Posterior retroperitoneoscopic adrenalectomy – results of 560 procedures in 520 patients. Surgery. 2006; 140: 943 -948

Left sided RPA After dissection of the main vein, preparation of adrenal gland is continued medially, laterally and cranially M. K. Walz. Adrenal Glands Diagnostic Aspects and Surgical therapy
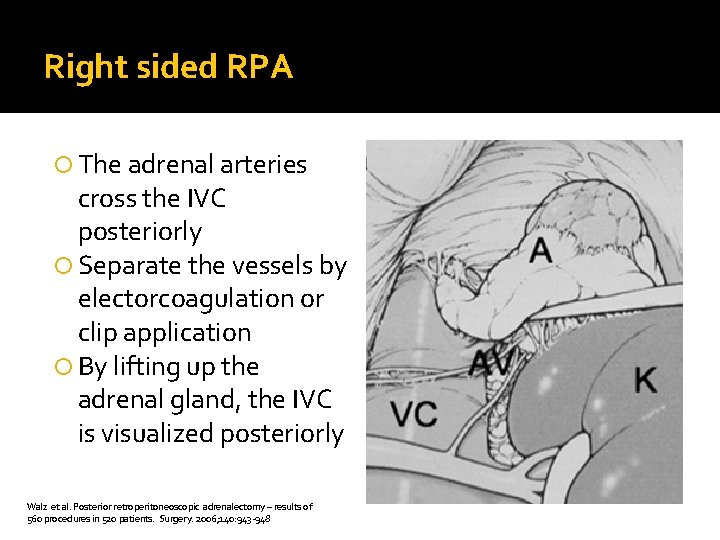
Right sided RPA The adrenal arteries cross the IVC posteriorly Separate the vessels by electorcoagulation or clip application By lifting up the adrenal gland, the IVC is visualized posteriorly Walz et al. Posterior retroperitoneoscopic adrenalectomy – results of 560 procedures in 520 patients. Surgery. 2006; 140: 943 -948

Right sided RPA The suprarenal vein then becomes clearly visible running posterolaterally and can be divided Mobilization of the right adrenal gland is completed by lateral and cranial dissection M. K. Walz. Adrenal Glands Diagnostic Aspects and Surgical therapy
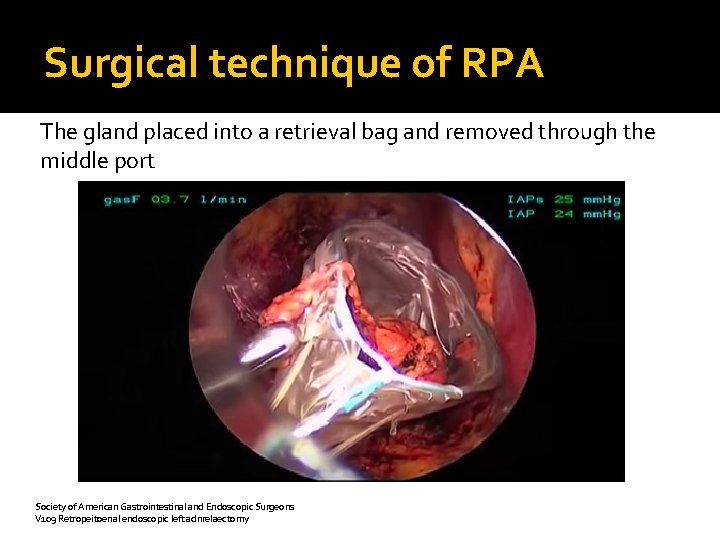
Surgical technique of RPA The gland placed into a retrieval bag and removed through the middle port Society of American Gastrointestinal and Endoscopic Surgeons V 109 Retropeitoenal endoscopic left adnrelaectomy

Results of RPA
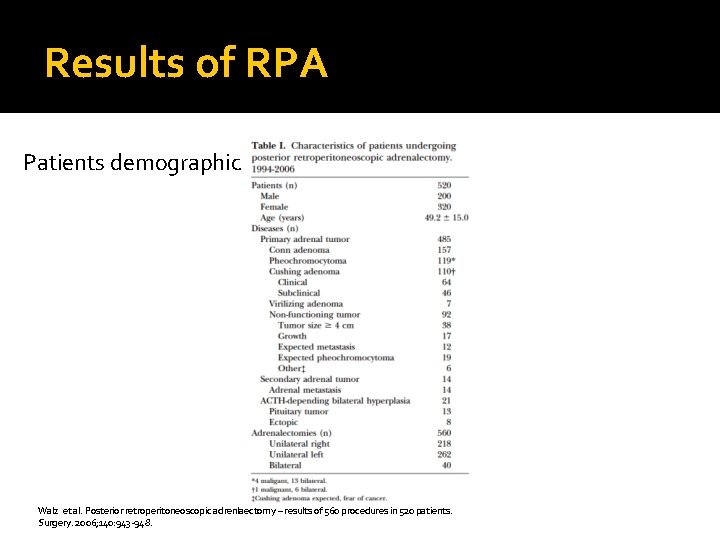

Results of RPA Patients demographic Walz et al. Posterior retroperitoneoscopic adrenlaectomy – results of 560 procedures in 520 patients. Surgery. 2006; 140: 943 -948.
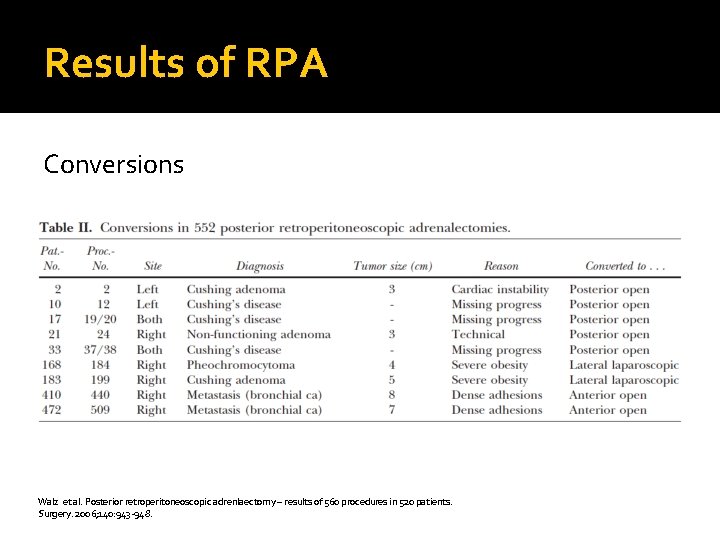
Results of RPA Conversions Walz et al. Posterior retroperitoneoscopic adrenlaectomy – results of 560 procedures in 520 patients. Surgery. 2006; 140: 943 -948.
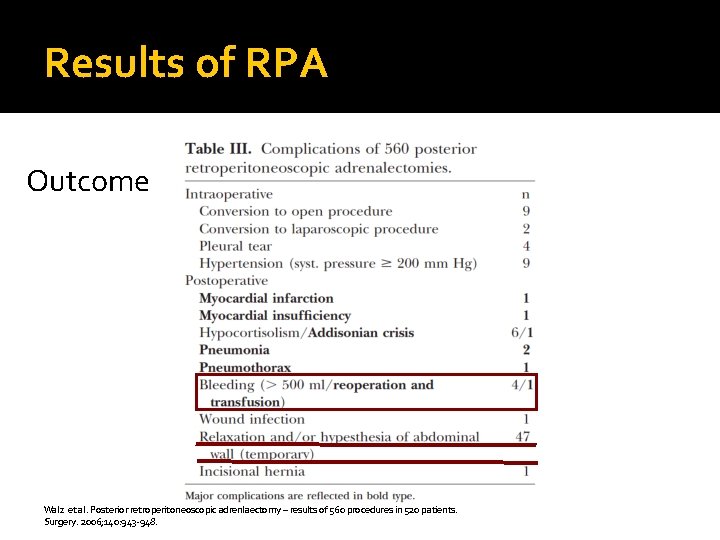

Results of RPA Outcome Walz et al. Posterior retroperitoneoscopic adrenlaectomy – results of 560 procedures in 520 patients. Surgery. 2006; 140: 943 -948.
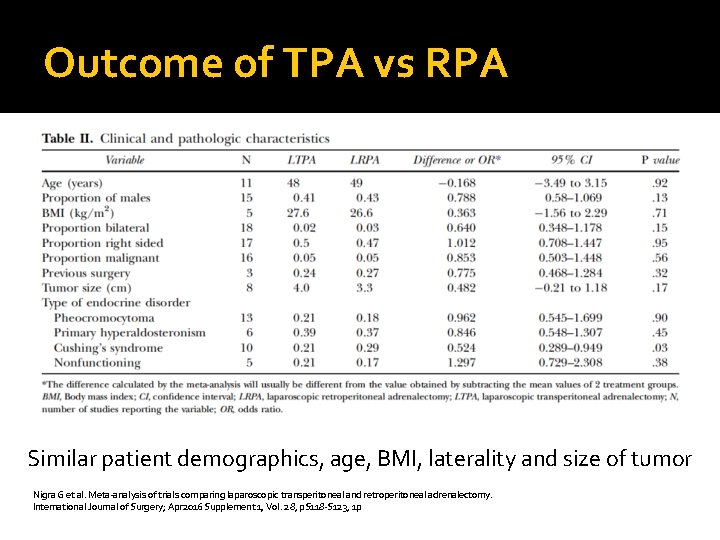
Outcome of TPA vs RPA Similar patient demographics, age, BMI, laterality and size of tumor Nigra G et al. Meta-analysis of trials comparing laparoscopic transperitoneal and retroperitoneal adrenalectomy. International Journal of Surgery; Apr 2016 Supplement 1, Vol. 28, p. S 118 -S 123, 1 p
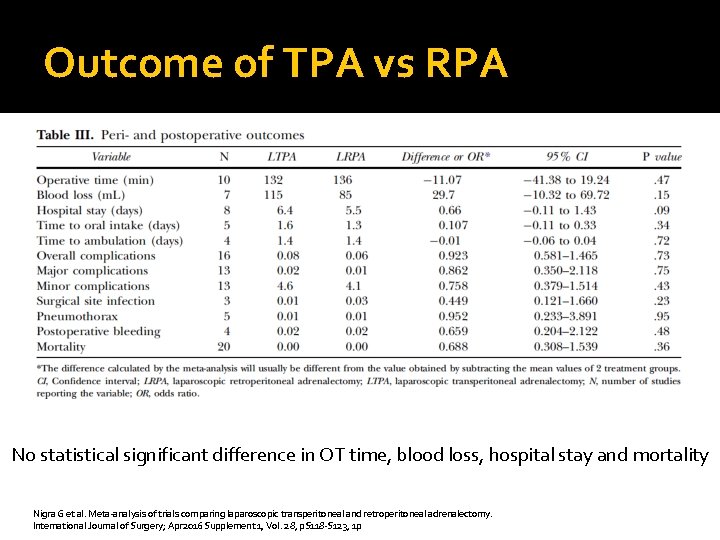
Outcome of TPA vs RPA No statistical significant difference in OT time, blood loss, hospital stay and mortality Nigra G et al. Meta-analysis of trials comparing laparoscopic transperitoneal and retroperitoneal adrenalectomy. International Journal of Surgery; Apr 2016 Supplement 1, Vol. 28, p. S 118 -S 123, 1 p
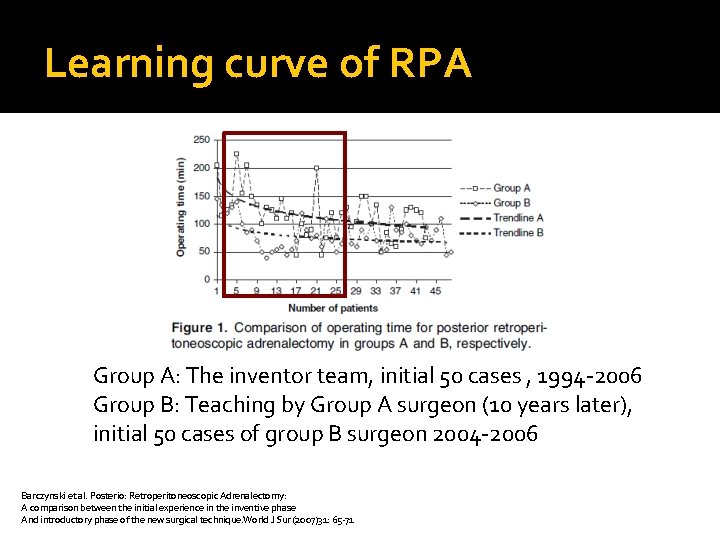
Learning curve of RPA Group A: The inventor team, initial 50 cases , 1994 -2006 Group B: Teaching by Group A surgeon (10 years later), initial 50 cases of group B surgeon 2004 -2006 Barczynski et al. Posterio: Retroperitoneoscopic Adrenalectomy: A comparison between the initial experience in the inventive phase And introductory phase of the new surgical technique. World J Sur (2007)31: 65 -71
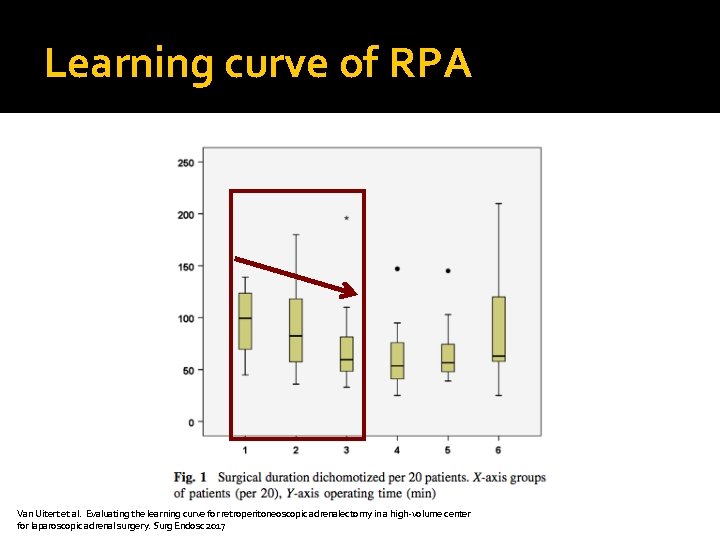
Learning curve of RPA Van Uitert et al. Evaluating the learning curve for retroperitoneoscopic adrenalectomy in a high-volume center for laparoscopic adrenal surgery. Surg Endosc 2017

Special condition: Phaeochromocytoma Intraoperative concern Secretion of catecholamine during surgical manipulation liable blood pressure Highly vascularized adrenal gland bleeding
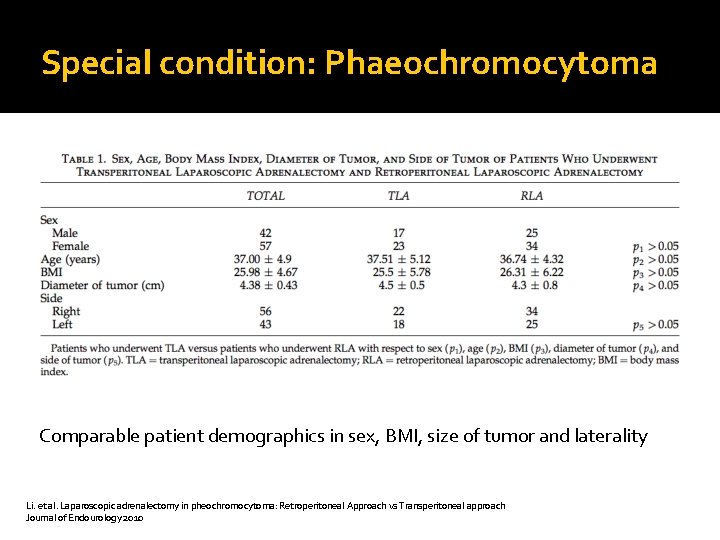
Special condition: Phaeochromocytoma Comparable patient demographics in sex, BMI, size of tumor and laterality Li. et al. Laparoscopic adrenalectomy in pheochromocytoma: Retroperitoneal Approach vs Transperitoneal approach Journal of Endourology 2010

Special condition: Phaeochromocytoma RPA takes less time, lower blood loss and shorter hospital stay Li. et al. Laparoscopic adrenalectomy in pheochromocytoma: Retroperitoneal Approach vs Transperitoneal approach Journal of Endourology 2010
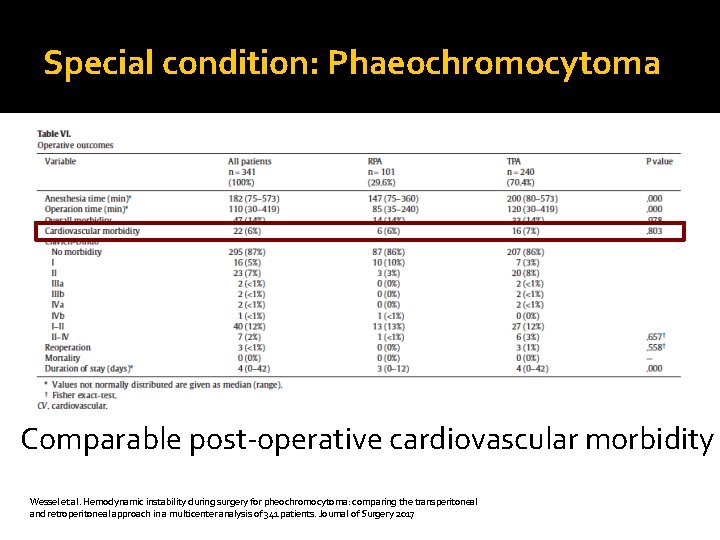
Special condition: Phaeochromocytoma Comparable post-operative cardiovascular morbidity Wessel et al. Hemodynamic instability during surgery for pheochromocytoma: comparing the transperitoneal and retroperitoneal approach in a multicenter analysis of 341 patients. Journal of Surgery 2017

Special condition: Phaeochromocytoma RPA �Avoid respiratory and hemodynamic effects of CO 2 pneumoperitoneum �Direct access without the need to mobilize abdominal organs Lack of large scaled RCT to evaluate the outcomes of 2 approaches on the disease Li. et al. Laparoscopic adrenalectomy in pheochromocytoma: Retroperitoneal Approach vs Transperitoneal approach Journal of Endourology 2010

Conclusion �Posterior retroperitoneoscopic adrenalectomy is a safe and feasible option �There may be circumstances where one approach may be preferable, and surgeons should be able to perform each approach routinely

Thank You
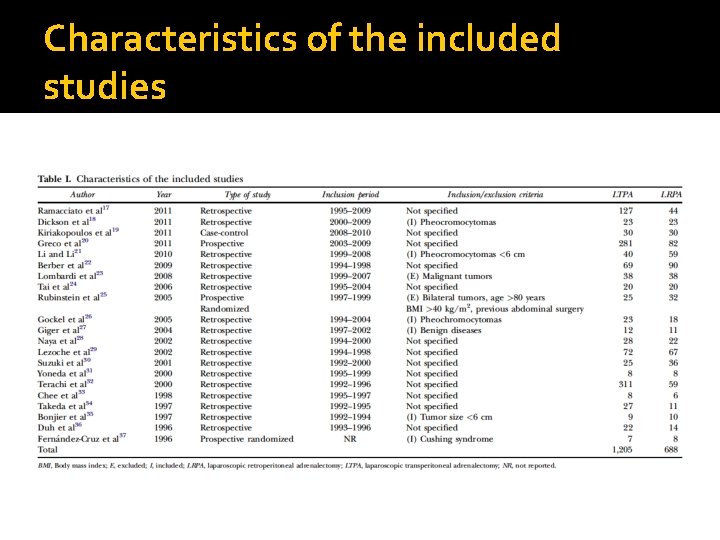
Characteristics of the included studies
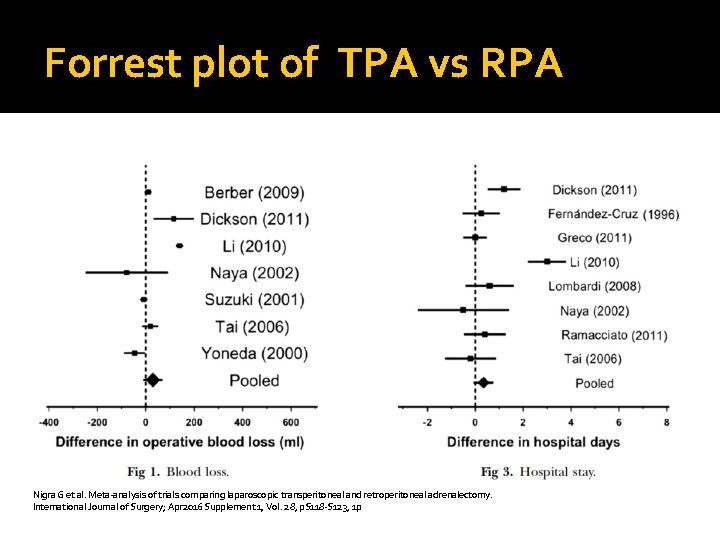
Forrest plot of TPA vs RPA Nigra G et al. Meta-analysis of trials comparing laparoscopic transperitoneal and retroperitoneal adrenalectomy. International Journal of Surgery; Apr 2016 Supplement 1, Vol. 28, p. S 118 -S 123, 1 p
- Slides: 33