ADRENAL GLAND SYMPATHOADRENAL SYSTEM Adrenal Gland 3 arterial





















- Slides: 33

ADRENAL GLAND; SYMPATHOADRENAL SYSTEM


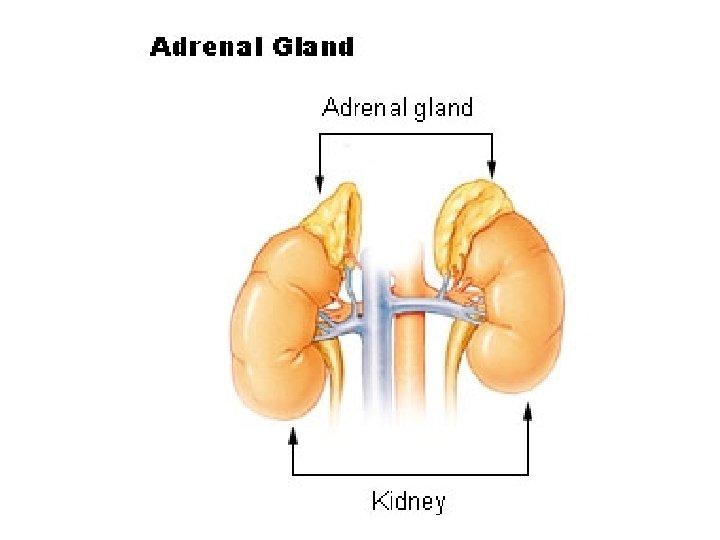
Adrenal Gland • 3 arterial supply sources – Perfuse gland • Periph center • Sinusoids • Medulla receives blood w/ cortex prod’s – Medulla has own arterial supply



• Medulla, cortex diff embryo origins – Cortex from posterior abdominal wall lining – Medullary pheochromocytes from sympathogonia • Neural crest cells • Also give rise to neuroblasts; sympathetic ganglia • SF-1 req’d for adrenal gland dev’t – Also gonads, ventromedial nucleus of hypothal – Also DAX-1 req’d • During dev’t, pheochromoblasts migrate to other areas (aorta, organ of Zuckerkandl)

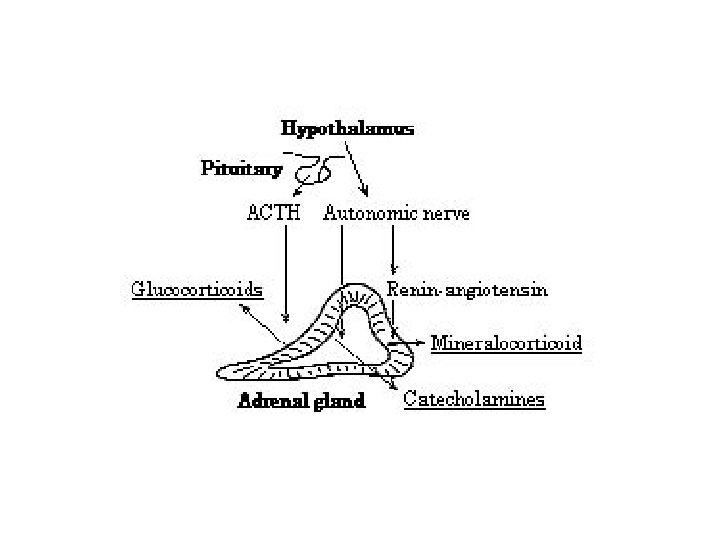
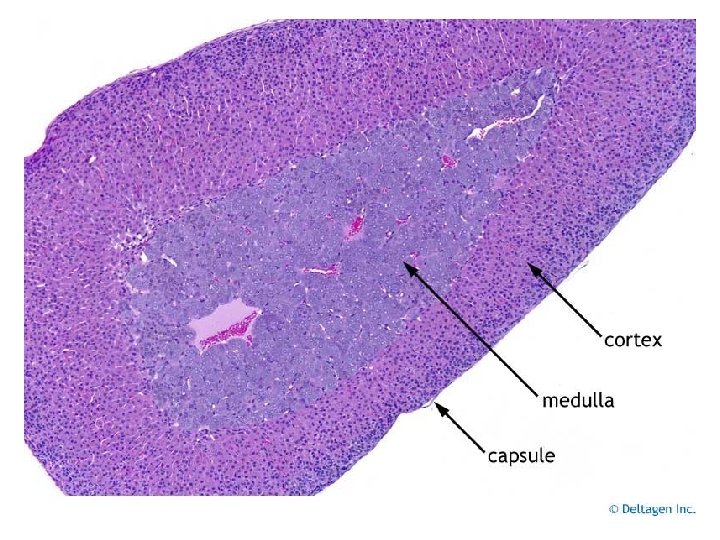
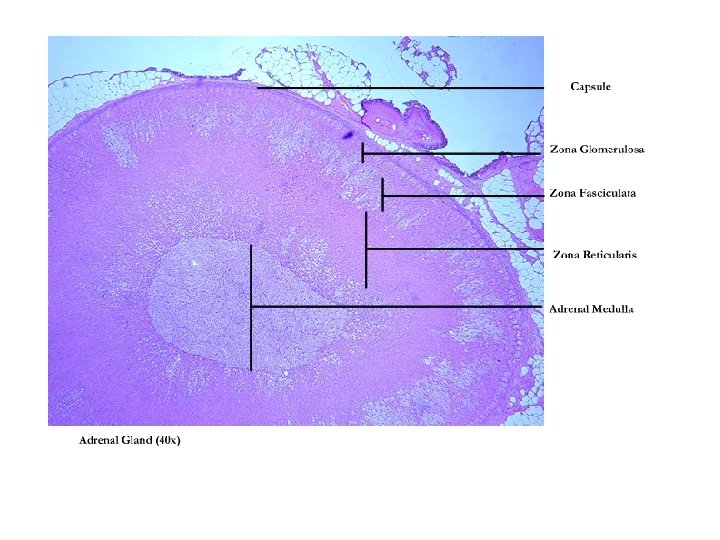
Adrenal Cortex • Produces steroid hormones • Cholesterol-processing enz’s in s. ER, inner mitoch membr – Tubulovesicular mitoch • Much inner membr surface area • Much P 450 scc • Parenchymal cells can produce cholesterol de novo – Mainly endocytosis of LDL – Cholesterol-rich lipid droplets in cytoplasm • Capsule + 3 cell layers


Adrenal Medulla • Mod’d sympathetic ganglion – BUT no axons at targets – Release catecholamines to ECF bloodstream • Cells = pheochromocytes – Axonless secr cells – Two cell subpopulations • Same cell pop’n under diff physiologic states – Concent cortisol exposure • Noradrenaline (norepinephrine) producing cells • Adrenaline (epinephrine) producing cells – Secrete prod’s from granules ECF by exocytosis

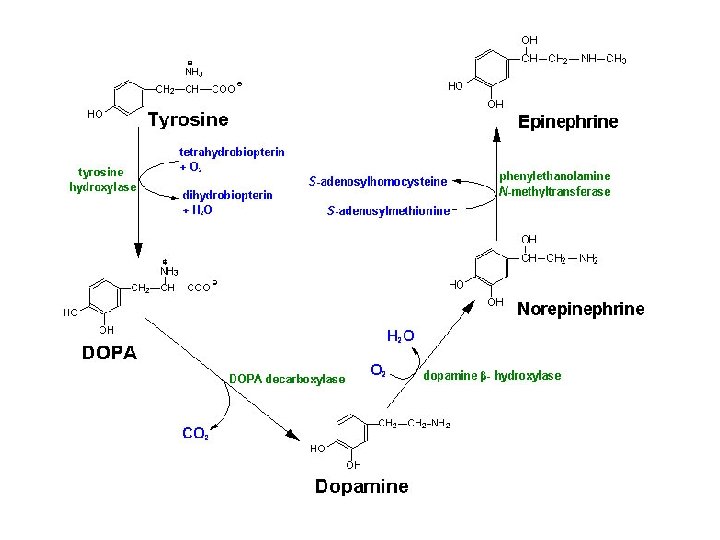
Catecholamines • • • Synth’d from L-tyrosine Dopamine, noradrenaline, adrenaline L-tyr in plasma (1 -1. 5 mg/d. L) Active transport into cells Conversion L-tyr by 4 enz’s – Compartmentalized • Adrenal medulla catecholamine output approx 80% adrenaline – BUT plasma ratio 9: 1 noradrenaline: adrenaline


1) Tyrosine Hydroxylase • Ring hydroxylation to L-DOPA (L-Dihydroxy. Phenyl. Alanine) • Contains Fe+2; tetrahydrobiopterin cofactor • Activity reg’d by preganglionic nerves – Get phosph’n PKA, PKC and calmodulin-dependent kinases • Long-term stim’n upreg’n transcription, translation • Incr’d L-DOPA prod inhib’n

2) DOPA Decarboxylase (aromatic L-amino acid decarboxylase) • Pyridoxal phosphate cofactor • End product in CNS • Stored in secretory vesicles – Enter by active transport – MVATs (Vesicular Mono. Amine Transporters)

3) Dopamine b-Hydroxylase (DBH) • side chain hydroxylation to noradrenaline • Contains Cu; Vit C cofactor • Rxn w/in secretory vesicle • End prod in symp nerves, most central catecholaminergic neural tracts

4) Phenylethanolamine NMethyl. Transferase (PNMT) • N-methylation to adrenaline • Methyl donor = S-Adenosyl. Methionine • Cytoplasmic – Noradrenaline leaves vesicle • Passive transport • Concent gradient – Adrenaline must reenter secretory vesicle • Active transport

PNMT • Expression depends on high local cortisol – From adrenal cortex – Through sinusoid system • Transcr’l activation of PNMT gene through ligand-act’d glucocort receptor – Also other transcription factors • • Also activity stim’d by glucocort Adrenaline prod feedback inhib’n Also found in kidney, lung, pancreas Also nonspecific NMT – Contributes to periph conversion norepi to epi

Secretory Vesicles • Catecholamine storage • Active transport via VMATs – ATP-driven proton pump – In vesicle membranes – p. H, electrical gradient – Antiporter • 12 transmembr helical segments – Related to plasma membr monoamine transporters


Catecholamine Release from Storage Vesicles • ACh rel’d from preganglionic fibers – Nicotinic receptors – Get depol’n pheochromocytes – act’n voltage-gated Ca channels – influx Ca – exocytosis of secretory vesicles • Chromogranins, DBH, ATP, other peptides released

Actions of Catecholamines • Circ’ng catecholamines reach most tissues – BUT cannot penetrate • BBB • Fetus – Fetal prod’n (mostly norepi) through fetal zone • Impt in intrauterine life (cardiovascular responses) • Large • Placenta expresses catecholamine degrading enzymes • Placental norepi transporter – Delivers circ’ng fetal chatechol’s for degrad’n

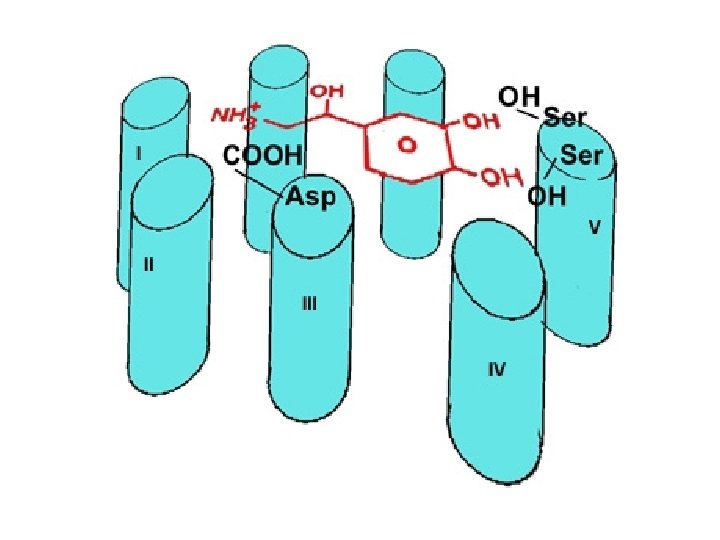
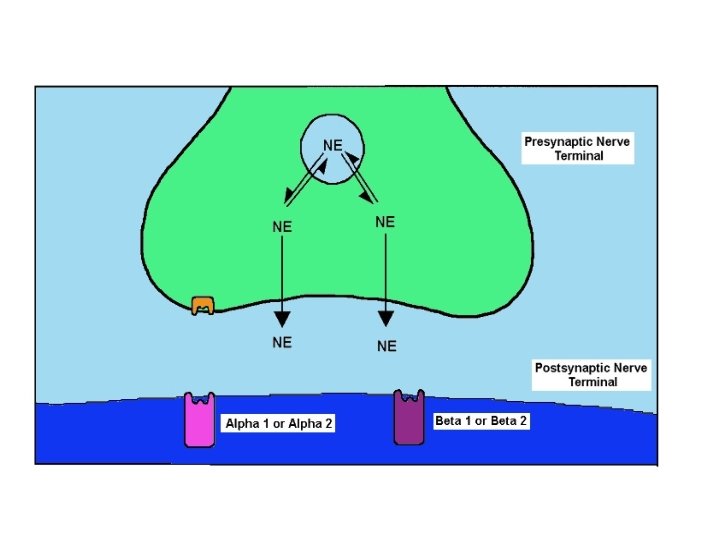
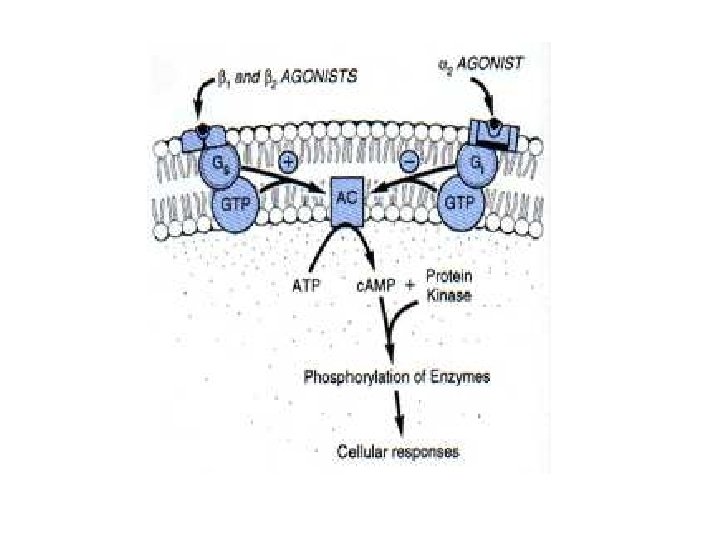
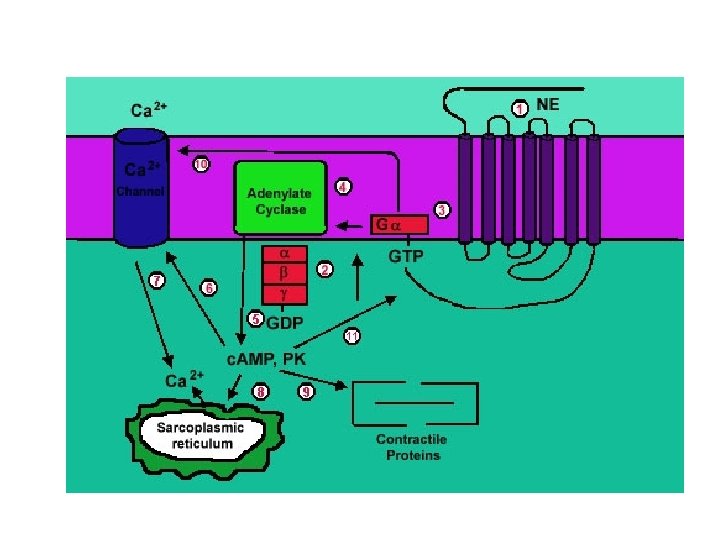
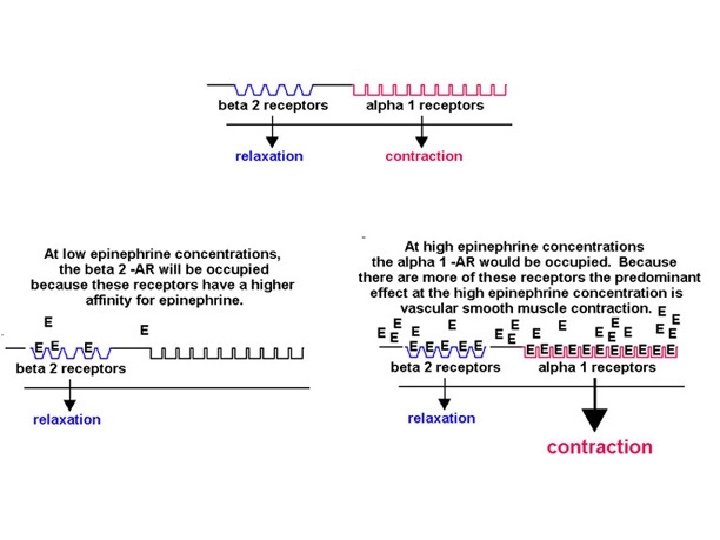
Adrenergic Receptors • Heptahelical, G-prot-linked transmembr receptors • 2 categories: a and b, subcategories • a – affinity for adrenaline > noradrenaline – a 1 (A, B, D) mostly use Gaq G prot’s • Usually activate PLC ( PKC and DAG and intracell Ca through IP 3) • And/or activate PLA 2 – a 2 (A, B, C) varied • Gai and G 0 couple to decr’d activity adenylyl cyclase • Can act’n K+ channels, inhib’n Ca channels, act’n PLC and/or PLA 2 • b – affinity for adrenaline > noradrenaline • All (1, 2, 3) use Gas G prot act’n ad cyclase


Tissue Receptor Subtype Heart beta 1 Adipose tissue beta 1 beta 3? Vascular Smooth Muscle beta 2 Airway Smooth Muscle beta 2





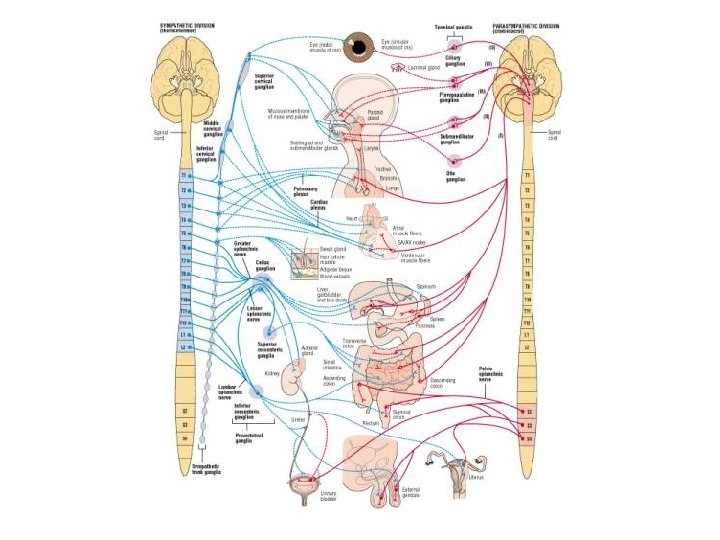
Physiological Implications of Sympathoadrenal Catecholamines • Gen’l: activates fight/flight mech’s – Mobilizes energy, redist’s blood • Opposes parasymp – Promotes digestion, storage of energy – BUT distinct target cell pop’ns w/in organs • Many targets; overall – Incr’s cardiac output, blood pressure – Bronchodilation matched perfusion w/ incr’d ventilation – Blood diverted from viscera and skin to muscle • Retain blood to brain – Mobilize fuel from energy stores


• Stress sympathoadrenergic, adrenocortical systems activated simultaneously – Catecholamines instantaneous action • From adrenal medulla and symp neurons • Rapid elimin’n w/ end release – Cortisol delayed 20 -30 mins, action prolonged • Involved in body weight regulation – Leptin secr’d by adipocytes • Acts on hypothal decr’d appetite, incr’d energy expenditure – Adipocytes have b 3 receptors • More responsive to norepi – Stim’n receptors enhanced lipolysis red’n fat stores decr’d leptin • BUT apparently not mediated through adrenal medulla

Dopamine • Five receptor types – All G-prot coupled heptahelical – D 1 stim’s adenylyl cyclase • vasodilation in splachnic region – D 2 inhibits adenylyl cyclase • Impt: antihypertensive, natriuretic through autocrine/paracrine mech’s – Opposes aldosterone

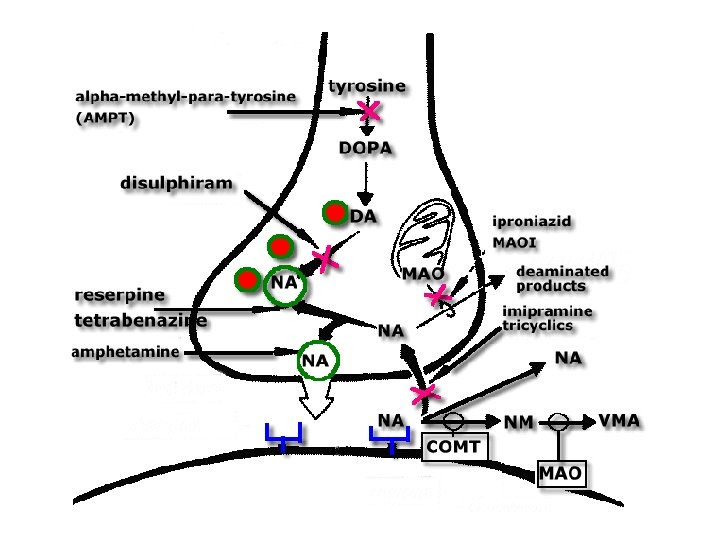
Catecholamine Elimination • Short-lived mol’s – 10 sec to 1. 7 min • 50 -60% assoc’d w/ albumin • Elimin’n – At synapse, ISF near symp neurons • Reuptake into nerve terminals • Reenter vesicles via VMAT OR • Become degraded by MAO – In target cells • Degraded by Catechol-O-Methyl. Transferase (COMT) – 5% directly filtered into urine

• MAO – – – In outer mitoch membr Substr’s also serotonin, histamine Oxidizes amino grp aldehydes Further ox’d by nonspecific aldehyde de. Hase Ultimate prod dihydroxymandelic acid (DOMA) • COMT – extraneuronal degradation – Uses SAM as methyl donor – Impt to circ’g catecholamines • Get final conjugation – Sulfate, glucuronate in liver, gut – Excr’n through urine