Adjuvant treatment of Locally Advanced Bladder Cancer Acad

Adjuvant treatment of Locally Advanced Bladder Cancer Acad F. Todua , Natia Jokhadze. MD, Z. Kvirikashvili MD Research Institute of Clinical Medicine
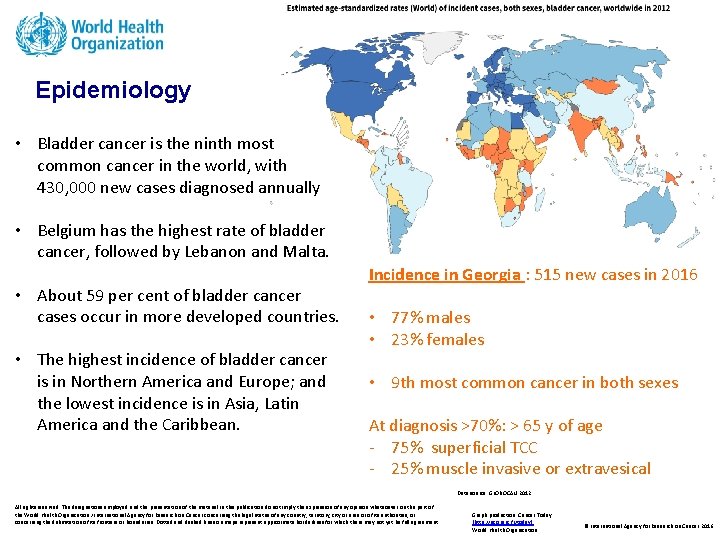
Epidemiology • Bladder cancer is the ninth most common cancer in the world, with 430, 000 new cases diagnosed annually • Belgium has the highest rate of bladder cancer, followed by Lebanon and Malta. • About 59 per cent of bladder cancer cases occur in more developed countries. • The highest incidence of bladder cancer is in Northern America and Europe; and the lowest incidence is in Asia, Latin America and the Caribbean. Incidence in Georgia : 515 new cases in 2016 • 77% males • 23% females • 9 th most common cancer in both sexes At diagnosis >70%: > 65 y of age - 75% superficial TCC - 25% muscle invasive or extravesical Data source: GLOBOCAN 2012 All rights reserved. The designations employed and the presentation of the material in this publication do not imply the expression of any opinion whatsoever on the part of the World Health Organization / International Agency for Research on Cancer concerning the legal status of any country, territory, city or area or of its authorities, or concerning the delimitation of its frontiers or boundaries. Dotted and dashed lines on maps represent approximate borderlines for which there may not yet be full agreement. Graph production: Cancer Today (http: //gco. iarc. fr/today) World Health Organization © International Agency for Research on Cancer 2016
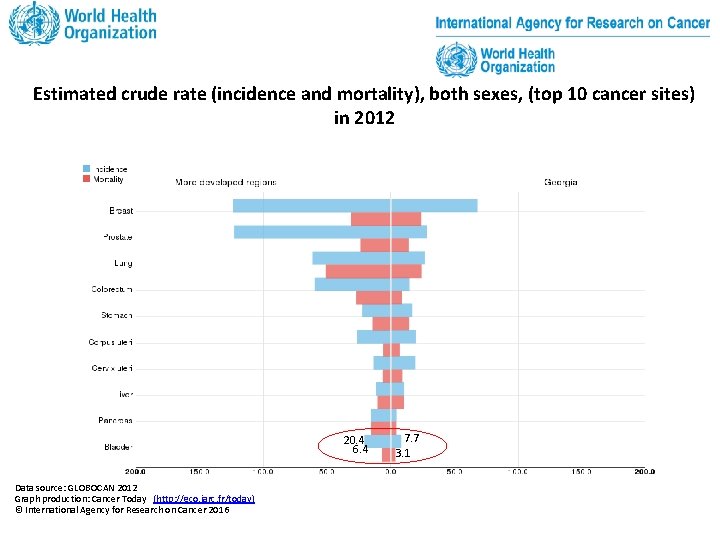
Estimated crude rate (incidence and mortality), both sexes, (top 10 cancer sites) in 2012 20. 4 6. 4 Data source: GLOBOCAN 2012 Graph production: Cancer Today (http: //gco. iarc. fr/today) © International Agency for Research on Cancer 2016 7. 7 3. 1
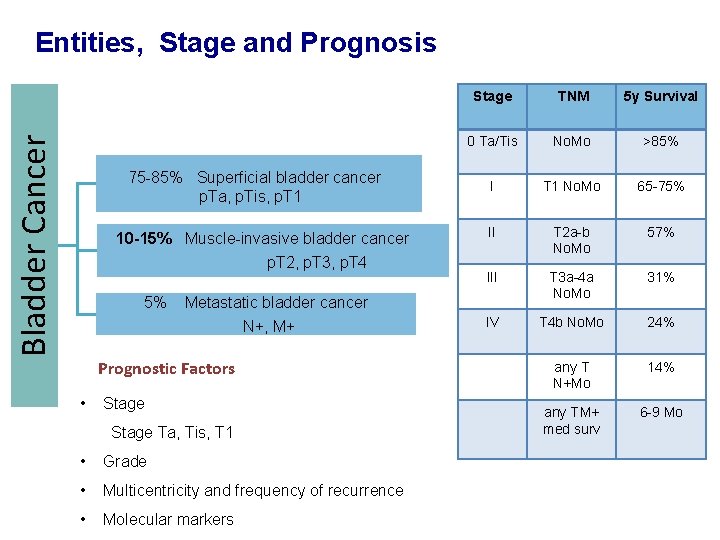
Bladder Cancer Entities, Stage and Prognosis 75 -85% Superficial bladder cancer p. Ta, p. Tis, p. T 1 10 -15% Muscle-invasive bladder cancer p. T 2, p. T 3, p. T 4 5% TNM 5 y Survival 0 Ta/Tis No. Mo >85% I T 1 No. Mo 65 -75% II T 2 a-b No. Mo 57% III T 3 a-4 a No. Mo 31% IV T 4 b No. Mo 24% any T N+Mo 14% any TM+ med surv 6 -9 Mo Metastatic bladder cancer N+, M+ Prognostic Factors • Stage Ta, Tis, T 1 • Grade • Multicentricity and frequency of recurrence • Molecular markers
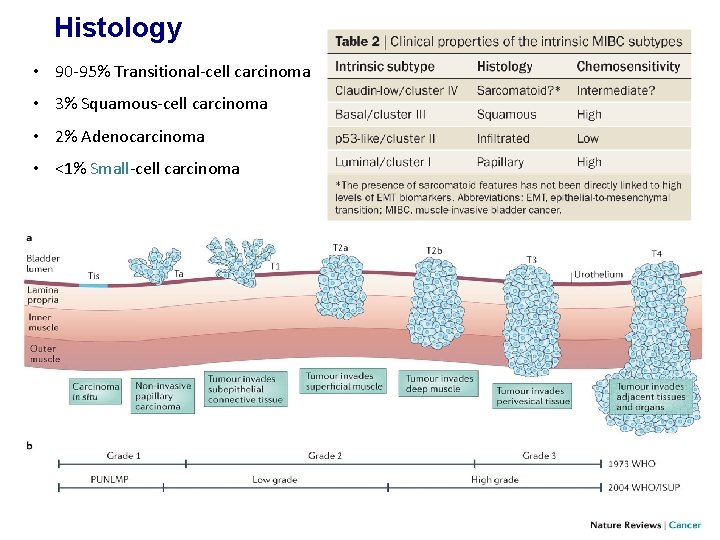
Histology • 90 -95% Transitional-cell carcinoma • 3% Squamous-cell carcinoma • 2% Adenocarcinoma • <1% Small-cell carcinoma

Treatment of Superficial Disease Ta , T 1 , TIS N 0 M 0 ”Non Muscle-invasive"

Treatment options for NMIBC: • Endoscopic surgical management • Immunotherapy • Intravesical chemotherapy • Radical cystectomy • Radiotherapy
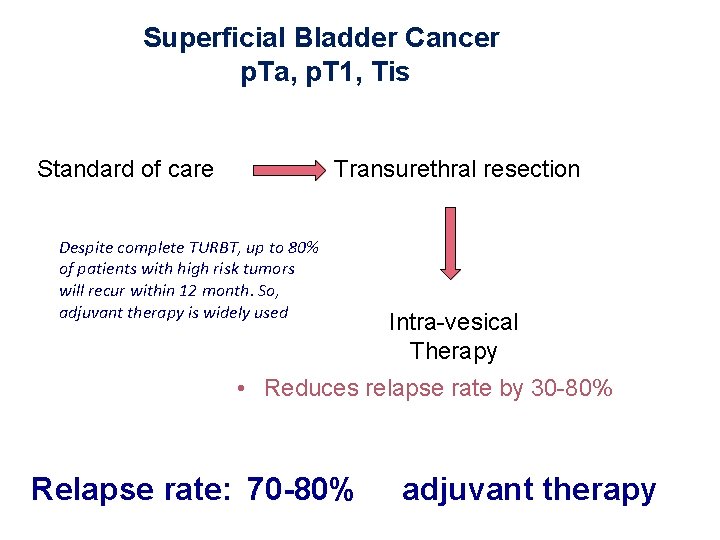
Superficial Bladder Cancer p. Ta, p. T 1, Tis Standard of care Transurethral resection Despite complete TURBT, up to 80% of patients with high risk tumors will recur within 12 month. So, adjuvant therapy is widely used Intra-vesical Therapy • Reduces relapse rate by 30 -80% Relapse rate: 70 -80% adjuvant therapy

Intravesical therapy Permits high local concentrations of a therapeutic agent within the bladder, potentially destroying viable tumor cells that remain following TURBT and preventing tumor implantation Indications : • Multiple, or large (>3 cm) at presentation • Recurrence within 1 year • High grade Ta • Any T 1 • Cis • Positive cytology after resection of a visible tumor Metaanalysis of seven randomized trial has demonstrated that one immediate installation of chemotherapy after TUR decrease the relative risk of recurrence by 40 %!

BCG : weekly 6 -8 w. /Mo 3 and 6 next maintenance for 1 year. • Live attenuated form of Mycobacterium Bovid • The exact mechanism of action is UNKNOWN • Mononuclear cell infiltratration (CD 4 T, Macrophages) • Interferon gamma and cytokines level are increased in the urine following treatment • BCG is superior to chemotherapy for preventing recurrence in patients with intermediate risk and high risk tumors • At least 1 year maintenance therapy is recommended for complete treatment , but the optimal schedule and does have not yet been defined Mitomycin C : weekly 6 -8 w. / monthly 6 -12 • Alkylating agent that is minimally absorbed from the bladder circulation into the systemic circulation. 20 -60 mg. Weekly for 6 -8 weeks • Side effects include chemical cystitis and skin reactions Anthracyclines : weekly 6 -8 w. / monthly 6 -12 • • Epirubicin, Doxorubicin, and Valrubicin Approved for use in patients who have failed BCG, and in whom immediate cystectomy is either refused or contraindicated

Summary Recommendations for Intravesical Treatment POST-OP SINGLE INSTALATION • All Low risk tumors DELAYED INDUCTION CHEMOTHERAPY • Intermediate Risk • 6 weeks appear OK BCG • Intermediate and high risk bladder tumors • Needs Maintenance to reduce recurrence and progression of Disease

Treatment of Locally Advanced Disease T 2 a-T 4 a. N 0 M 0 "Muscle-invasive"
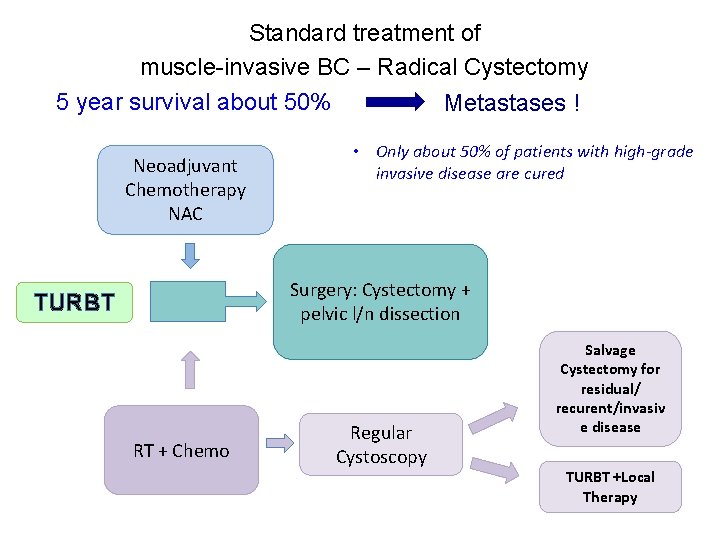
Standard treatment of muscle-invasive BC – Radical Cystectomy 5 year survival about 50% Metastases ! Neoadjuvant Chemotherapy NAC • Only about 50% of patients with high-grade invasive disease are cured Surgery: Cystectomy + pelvic l/n dissection TURBT RT + Chemo Regular Cystoscopy Salvage Cystectomy for residual/ recurent/invasiv e disease TURBT +Local Therapy

Peri-operative chemotherapy of Invasive Bladder Cancer Deaths from TCC are generally not local events Patients die as a result of metastatic disease Local interventions will not deal with micro-metastatic disease Systemic therapy must be given to eradicate micrometastatic disease • For many malignancies, there is clear cut evidence for the order of therapies colon cancer: surgery first then chemotherapy later Inflammatory breast cancer: chemo first then local therapy • • • For a long time, there was little evidence to guide us in TCC as to optimal sequencing

Clinical Case Medically fit 75 y. o patient with Resectable Muscle Invasive Urothelial Carcinoma T 3 N 0 M 0 How to treat ü Radical Cystectomy alone ü Neoadjuvant Chemotherapy followed by Radical Cystectomy ü Radical Cystectomy followed by Adjuvant Chemotherapy ü Bladder preserving approach
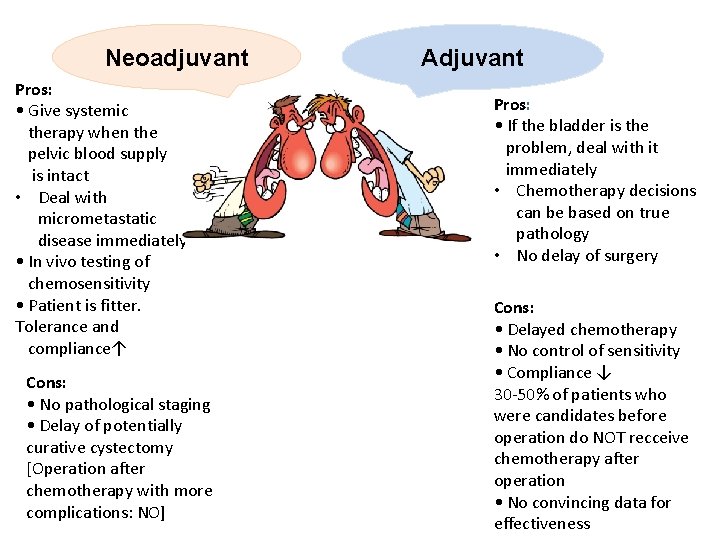
Neoadjuvant Pros: • Give systemic therapy when the pelvic blood supply is intact • Deal with micrometastatic disease immediately • In vivo testing of chemosensitivity • Patient is fitter. Tolerance and compliance↑ Cons: • No pathological staging • Delay of potentially curative cystectomy [Operation after chemotherapy with more complications: NO] Adjuvant Pros: • If the bladder is the problem, deal with it immediately • Chemotherapy decisions can be based on true pathology • No delay of surgery Cons: • Delayed chemotherapy • No control of sensitivity • Compliance ↓ 30 -50% of patients who were candidates before operation do NOT recceive chemotherapy after operation • No convincing data for effectiveness
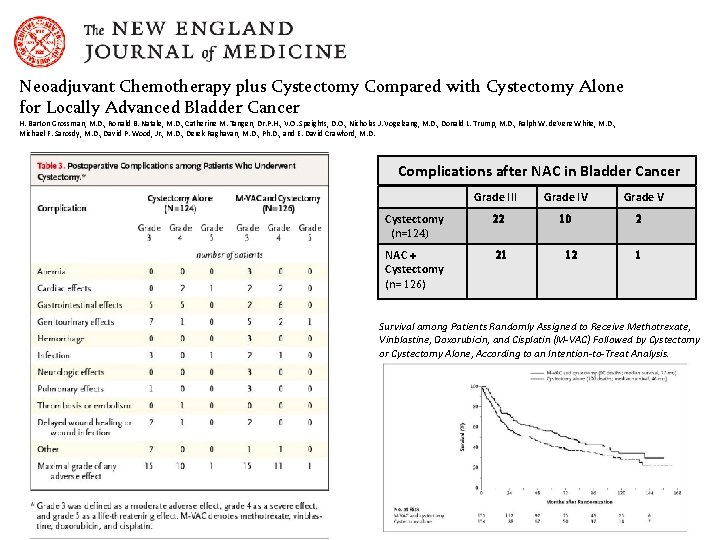
Neoadjuvant Chemotherapy plus Cystectomy Compared with Cystectomy Alone for Locally Advanced Bladder Cancer H. Barton Grossman, M. D. , Ronald B. Natale, M. D. , Catherine M. Tangen, Dr. P. H. , V. O. Speights, D. O. , Nicholas J. Vogelzang, M. D. , Donald L. Trump, M. D. , Ralph W. de. Vere White, M. D. , Michael F. Sarosdy, M. D. , David P. Wood, Jr. , M. D. , Derek Raghavan, M. D. , Ph. D. , and E. David Crawford, M. D. Complications after NAC in Bladder Cancer Grade III Grade IV Cystectomy (n=124) 22 10 NAC + Cystectomy (n= 126) 21 12 Grade V 2 1 Survival among Patients Randomly Assigned to Receive Methotrexate, Vinblastine, Doxorubicin, and Cisplatin (M-VAC) Followed by Cystectomy or Cystectomy Alone, According to an Intention-to-Treat Analysis.
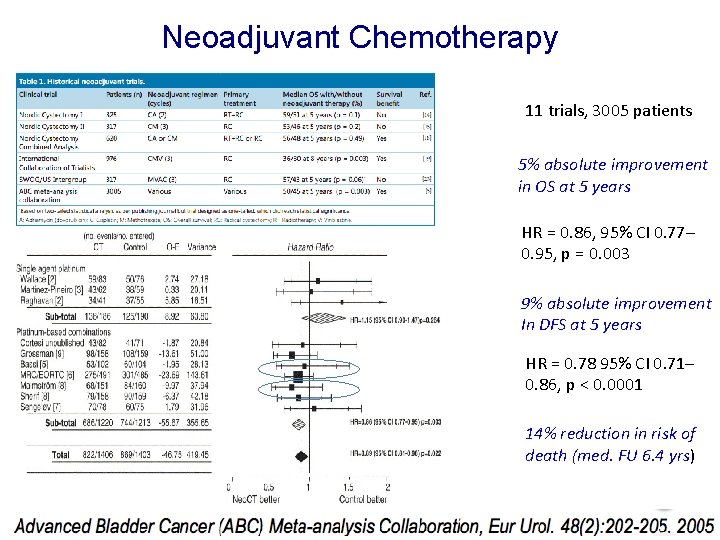
Neoadjuvant Chemotherapy 11 trials, 3005 patients 5% absolute improvement in OS at 5 years HR = 0. 86, 95% CI 0. 77– 0. 95, p = 0. 003 9% absolute improvement In DFS at 5 years HR = 0. 78 95% CI 0. 71– 0. 86, p < 0. 0001 14% reduction in risk of death (med. FU 6. 4 yrs)
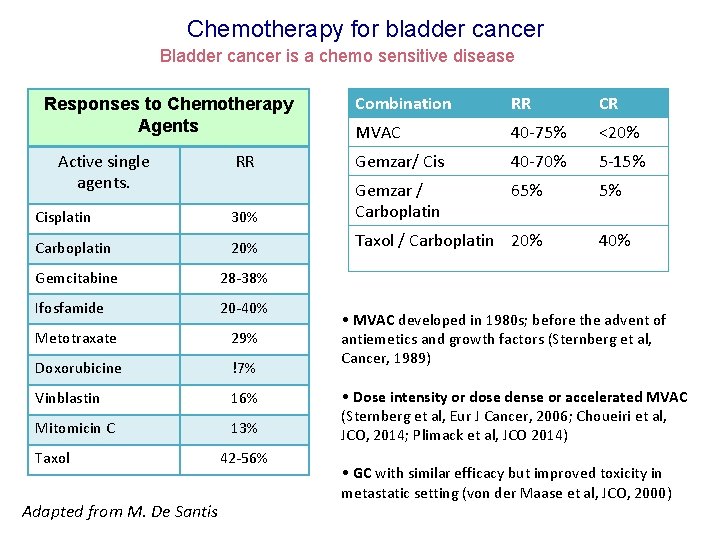
Chemotherapy for bladder cancer Bladder cancer is a chemo sensitive disease Combination RR CR MVAC 40 -75% <20% RR Gemzar/ Cis 40 -70% 5 -15% 65% 5% Cisplatin 30% Gemzar / Carboplatin 20% Taxol / Carboplatin 20% Gemcitabine 28 -38% Ifosfamide 20 -40% Responses to Chemotherapy Agents Active single agents. Metotraxate 29% Doxorubicine !7% Vinblastin 16% Mitomicin C 13% Taxol Adapted from M. De Santis 42 -56% 40% • MVAC developed in 1980 s; before the advent of antiemetics and growth factors (Sternberg et al, Cancer, 1989) • Dose intensity or dose dense or accelerated MVAC (Sternberg et al, Eur J Cancer, 2006; Choueiri et al, JCO, 2014; Plimack et al, JCO 2014) • GC with similar efficacy but improved toxicity in metastatic setting (von der Maase et al, JCO, 2000)

Adjuvant Chemotherapy • • • Multiple trials Small number of patients ranging from 49 -102 NO survival benefit • Two trials suggest survival benefit Skinner et al. J Urol 1991 An updated meta-analysis of nine randomized trials (after 2005) including 945 patients found ü OS benefit [hazard ratio (HR) 0. 77, 95% confidence interval (CI) 0. 59– 0. 99, P = 0. 049] ü DFS benefit (HR 0. 66, 95% CI 0. 45– 0. 91, P = 0. 014) among those who received cisplatin-based adjuvant chemotherapy. The DFS benefit was more apparent among those with positive lymph node involvement 70% of the patients assigned to chemotherapy are free of disease at 3 years compared to 46% in the observation group. No standard of care • Node positive disease, lymphovascular invasion, positive margins, Pts without NAC

International Guidelines Witjes JA et al. EAU guidelines on muscle invasive bladder cancer http: //uroweb. org/guideline/bladder-cancer

Bladder-sparing therapy for invasive bladder cancer Transurethral Resection Induction Therapy : Radiation+ Chemotherapy ( Cisplatin+Paclitaxel) Cystoscopy after 1 month No Tumor Consolidation: RT+CT Tumor Cystectomy • High probability of subsequent distant metastasis after cystectomy or radiotherapy alone (50% within 2 years) • Radiotherapy in comparison with cystectomy has inferior results (local control 40%) • muscle-invasive bladder cancer is often a systemic disease • �combined modality therapy
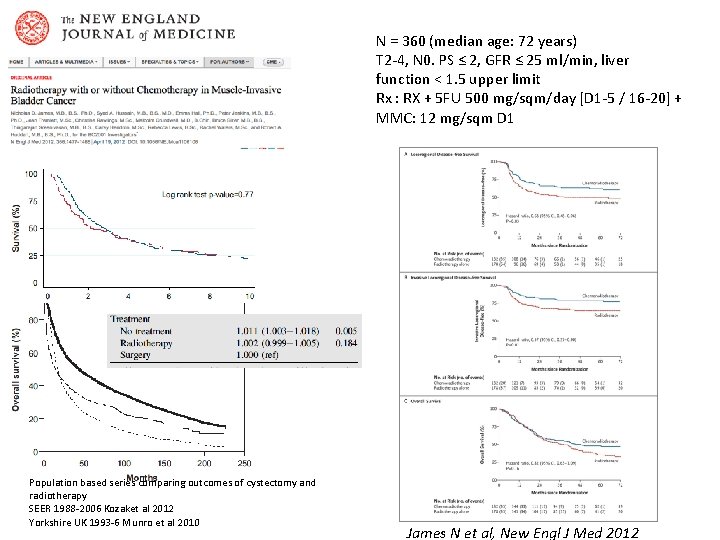
N = 360 (median age: 72 years) Kaplan–Meier Analysis of Survival. T 2 -4, N 0. PS ≤ 2, GFR ≤ 25 ml/min, liver function < 1. 5 upper limit Rx : RX + 5 FU 500 mg/sqm/day [D 1 -5 / 16 -20] + MMC: 12 mg/sqm D 1 Population based series comparing outcomes of cystectomy and radiotherapy SEER 1988 -2006 Kozaket al 2012 Yorkshire UK 1993 -6 Munro et al 2010 James N et al, New Engl J Med 2012

Bladder sparing procedures for muscle-invasive bladder cancer Benefits: • Preserves bladder function • Preserves sexual function • Maintains QOL • Avoids Major surgery: elderly and Pt with comorbidities • Equivalent survival to cystectomy • Lower peri-treatment mortality • Improving local control with radiosensitisers • Modest toxicity In most countries reserved for patients: • unfit / unsuitable for cystectomy • unwilling to undergo radical cystectomy Best results if • T 2, complete TUR-B, single lesion • NO hydronephrosis. NO CIS • NO tumour invasion into stroma of the prostate • Well functioning bladder

Conclusions for MIBC: • Muscle invasive bladder cancer carries a significant risk of mortality • Most deaths are due to systemic disease • Strength of evidence for perioperative chemotherapy lies with neoadjuvant therapy • Treatment should be a cisplatin-based combination therapy • Magnitude of benefit is similar to many other oncology situations – node negative breast cancer, high risk stage II colon cancer • Despite evidence, referrals are still low • Multidisciplinary approach is critical for good outcomes • Hopefully in the future we will be able to better select patients for therapy

Thank you For Attention!
- Slides: 26