Addressing the Uninsured Medicaid Rebalancing Act of 2020

Addressing the Uninsured: Medicaid Rebalancing Act of 2020 Becky Pasternik-Ikard CEO of the Oklahoma Health Care Authority October 11, 2016 1
OKLAHOMA MEDICAID The Oklahoma Health Care Authority (OHCA) was established to administer the Medicaid program, Sooner. Care, in Oklahoma. Sooner. Care is the largest public purchaser of health care in the state. In state fiscal year 2016, Sooner. Care covered 1, 025, 038 lives. Sooner. Care has a network of 47, 344 contracted providers. Sooner. Care spent $5. 12 billion in SFY 2016 with funding from the state and federal government. 2
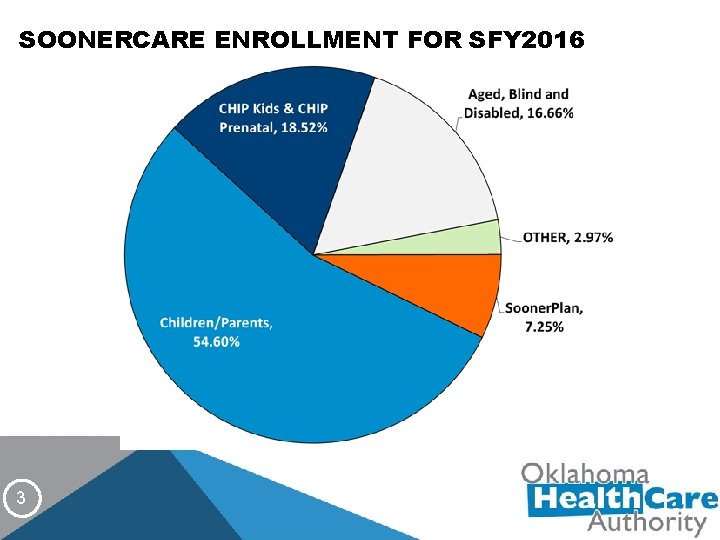
SOONERCARE ENROLLMENT FOR SFY 2016 3

INSURE OKLAHOMA Employer Sponsored Insurance (ESI) Individual Plan 14, 580 employees and spouses enrolled 4, 596 individuals enrolled 3, 956 businesses participating Average monthly premium paid by the member: $36. 71 19 commercial carriers The Individual Plan utilizes the Sooner. Care provider network 19, 176 ENROLLED 4

MEDICAID REBALANCING ACT OF 2020 5

PRINCIPLES OF THE MEDICAID REBALANCING ACT Multi Year Plan Provider Rate Stabilization Cigarette Tax Insure Oklahoma: Private/Public Partnership Children’s Health Insurance Program 6
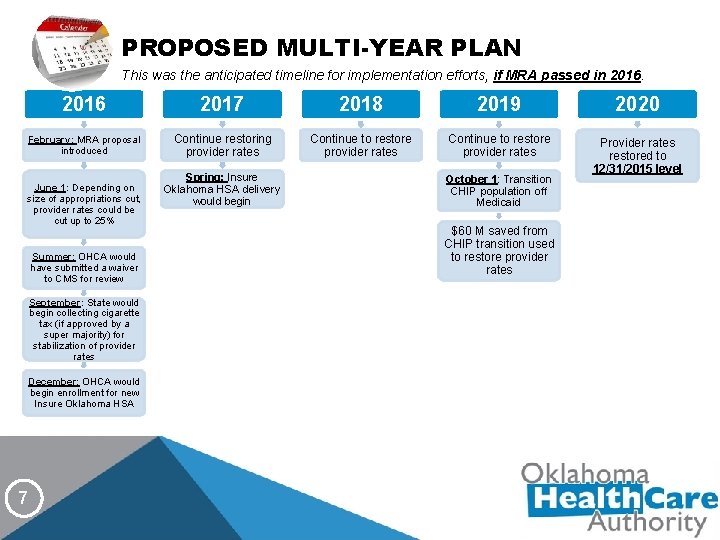
PROPOSED MULTI-YEAR PLAN This was the anticipated timeline for implementation efforts, if MRA passed in 2016 2017 2018 2019 February: MRA proposal introduced Continue restoring provider rates Continue to restore provider rates June 1: Depending on size of appropriations cut, provider rates could be cut up to 25% Summer: OHCA would have submitted a waiver to CMS for review September: State would begin collecting cigarette tax (if approved by a super majority) for stabilization of provider rates December: OHCA would begin enrollment for new Insure Oklahoma HSA 7 Spring: Insure Oklahoma HSA delivery would begin October 1: Transition CHIP population off Medicaid $60 M saved from CHIP transition used to restore provider rates 2020 Provider rates restored to 12/31/2015 level
PROVIDER RATE STABILIZATION • Today’s Medicaid rate is 86. 57% of the Medicare fee schedule • Rates have been reduced in FY-2010, FY-2015 and FY-2016 • With a $1. 3 billion shortfall during the 2016 legislative session, state agencies were anticipating significant cuts to their annual appropriations for SFY 2017 8
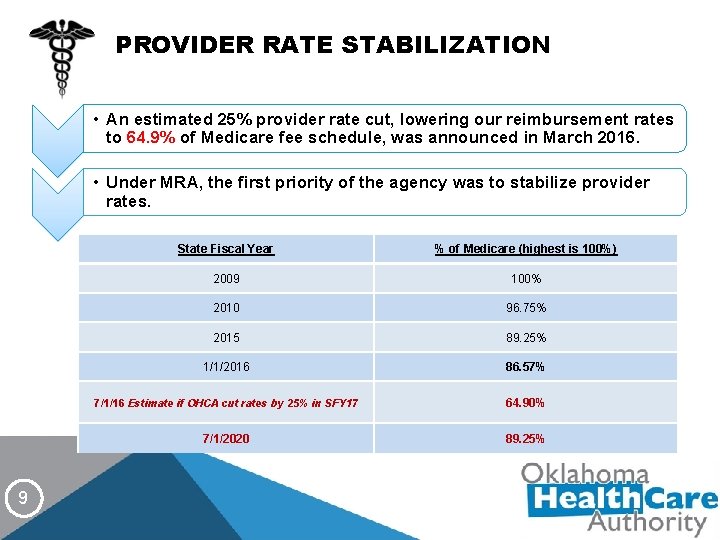
PROVIDER RATE STABILIZATION • An estimated 25% provider rate cut, lowering our reimbursement rates to 64. 9% of Medicare fee schedule, was announced in March 2016. • Under MRA, the first priority of the agency was to stabilize provider rates. 9 State Fiscal Year % of Medicare (highest is 100%) 2009 100% 2010 96. 75% 2015 89. 25% 1/1/2016 86. 57% 7/1/16 Estimate if OHCA cut rates by 25% in SFY 17 64. 90% 7/1/2020 89. 25%

CIGARETTE TAX § Current tax on cigarettes is $1. 03/pack § Last increase passed in 2004 § New revenue was dedicated to a variety of healthrelated purposes: Insure Oklahoma, a comprehensive cancer center, trauma care, tobacco cessation, and others § During the 2016 legislative session, HJR 1058 and HB 3210 proposed a $1. 50/pack increase. § Expected to collect approximately $180 million/year 10

CIGARETTE TAX HB 3210 - $1. 50/pack increase in excise tax § Revenue would be directed to the “Health revolving fund” to be appropriated by the Legislature for any Medicaid reimbursable service § Under MRA, portions of the new revenue would be used for the further growth of the Insure Oklahoma program § Large coalition of supporters 11

INSURE OKLAHOMA Health. Stead Account Private/Public partnership to address the uninsured • 13. 9% of Oklahoma’s population was uninsured in 2015 • Developing a new option through the commercial market could offer coverage for Oklahomans currently uninsured New “Health. Stead Account” option • Emphasizes personal responsibility • Individuals would be required to contribute towards monthly premium payments based on their income • Health savings account model incentivizes healthy behaviors and saving for future health care expenses Who is eligible? • Oklahomans, 19 -64 years of age, below 133% FPL • Approximately 215, 243 uninsured Oklahomans are eligible • Under MRA, an estimated 75% of that population would participate: 176, 219 12
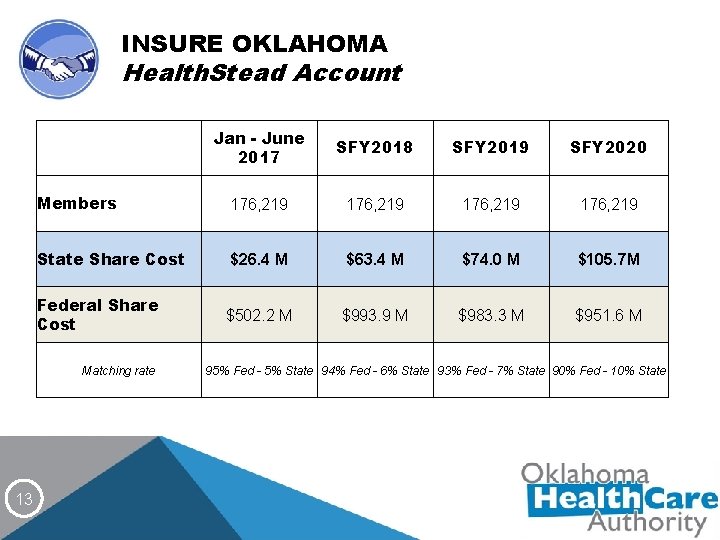
INSURE OKLAHOMA Health. Stead Account Jan - June 2017 SFY 2018 SFY 2019 SFY 2020 Members 176, 219 State Share Cost $26. 4 M $63. 4 M $74. 0 M $105. 7 M Federal Share Cost $502. 2 M $993. 9 M $983. 3 M $951. 6 M Matching rate 13 95% Fed - 5% State 94% Fed - 6% State 93% Fed - 7% State 90% Fed - 10% State

CHILDREN'S HEALTH INSURANCE PROGRAM CHIP coverage began on December 1, 1997 under Governor Frank Keating • CHIP covers children and pregnant women up to 185% FPL • SFY 2016: 197, 449 (187, 230 children; 10, 099 pregnant women) Population is required under a “maintenance of effort” until 2019 • The American Recovery and Reinvestment Act and the Affordable Care Act MOE requires each state to maintain 2009 eligibility levels through October 1, 2019. Federal government cover CHIP population at a different matching rate • Today: 95% federal – 5% state • Beginning October 1, 2017 WITHOUT REAUTHORIZATION by Congress: 58. 57% federal – 41. 43% state. • An additional $50 million will be needed to cover this population 14

CHIP Under MRA, CHIP moves to private health insurance plans • When the state has the authority to reduce eligibility levels to the federal minimum (133% FPL) in 2019, approximately 197, 000 individuals would be removed from the state’s Medicaid program. Coverage is available in the health care marketplace • Individuals with income between 100 – 400% FPL would qualify for a premium tax credit to assist with monthly premium payments. Reduces the size of the overall Medicaid program • Resetting the eligibility levels to the federal minimum would reduce Oklahoma’s Medicaid program by approximately 20%. • The CHIP transition saves the state approximately $60 million annually beginning in SFY 2020. 15

PRINCIPLES OF THE MEDICAID REBALANCING ACT Multi Year Plan Provider Rate Stabilization Cigarette Tax Insure Oklahoma: Private/Public Platform Children’s Health Insurance Program 16
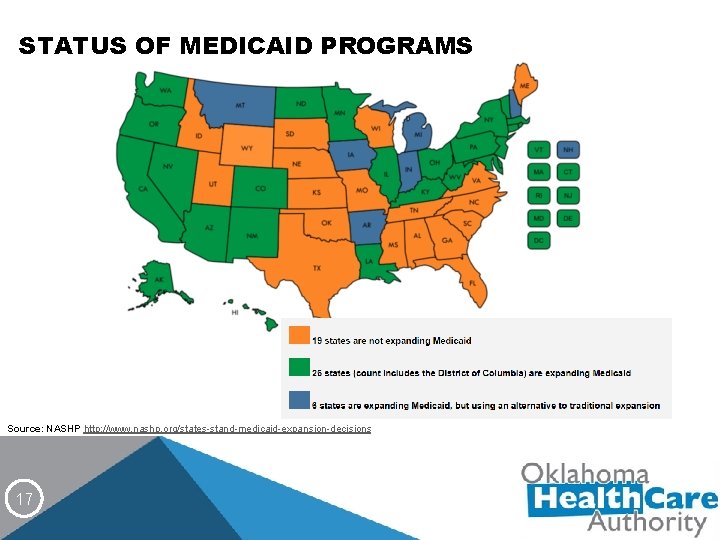
STATUS OF MEDICAID PROGRAMS Source: NASHP http: //www. nashp. org/states-stand-medicaid-expansion-decisions 17
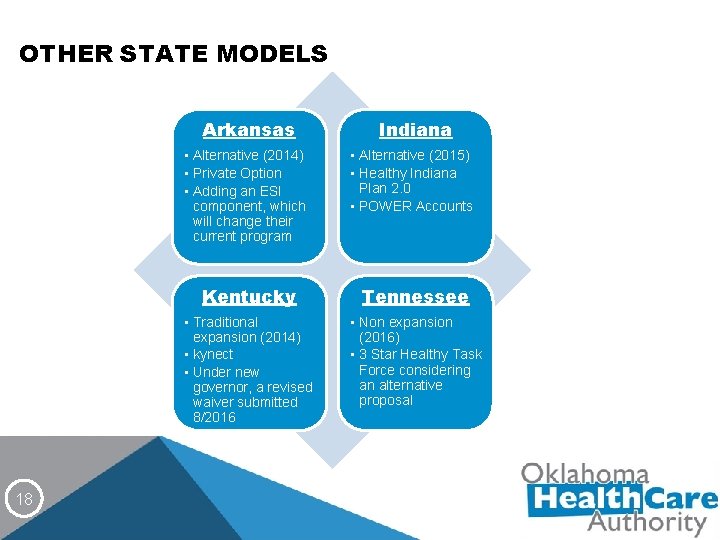
OTHER STATE MODELS 18 Arkansas Indiana • Alternative (2014) • Private Option • Adding an ESI component, which will change their current program • Alternative (2015) • Healthy Indiana Plan 2. 0 • POWER Accounts Kentucky Tennessee • Traditional expansion (2014) • kynect • Under new governor, a revised waiver submitted 8/2016 • Non expansion (2016) • 3 Star Healthy Task Force considering an alternative proposal
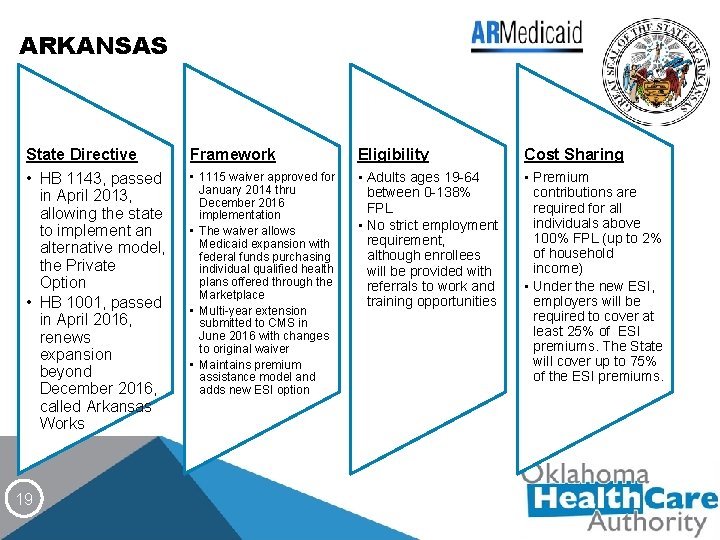
ARKANSAS State Directive Framework Eligibility Cost Sharing • HB 1143, passed in April 2013, allowing the state to implement an alternative model, the Private Option • HB 1001, passed in April 2016, renews expansion beyond December 2016, called Arkansas Works • 1115 waiver approved for January 2014 thru December 2016 implementation • The waiver allows Medicaid expansion with federal funds purchasing individual qualified health plans offered through the Marketplace • Multi-year extension submitted to CMS in June 2016 with changes to original waiver • Maintains premium assistance model and adds new ESI option • Adults ages 19 -64 between 0 -138% FPL • No strict employment requirement, although enrollees will be provided with referrals to work and training opportunities • Premium contributions are required for all individuals above 100% FPL (up to 2% of household income) • Under the new ESI, employers will be required to cover at least 25% of ESI premiums. The State will cover up to 75% of the ESI premiums. 19

ARKANSAS - Since the program began in 2014, Arkansas has seen a 12. 9% drop in the state’s uninsured rate. * - In 2015, the Private Option had an 82. 5% participation rate. - Eligible enrollees: 247, 173 - Actual enrollment: 204, 001 Notable changes in the 2016 waiver (Arkansas Works): - Termination of Independence Accounts - Instead, Arkansas Works will offer incentives for healthy behaviors and timely payments - Employer-Sponsored Insurance option - Provision allows Arkansas the authority to terminate the program if the federal matching rate decreases *Source: Gallup, http: //www. gallup. com/poll/189023/arkansas-kentucky-set-pace-reducing-uninsured-rate. aspx/ 20

INDIANA State Directive Framework Eligibility Cost sharing • 3 pieces of legislation introduced in 2014 supporting expansion, but all failed. • 1115 waiver approved for 2/1/2015 thru 1/31/2018 implementation • Expands upon existing Healthy Indiana Program (HIP) to create HIP 2. 0 • Premium assistance model with ESI • HIP 2. 0 offers HIP Plus and HIP Basic • Adults ages 19 -64 under 138% FPL • No employment requirement; however, Indiana is allowed to administer a voluntary state-run work search and job training program (separate from HIP 2. 0) • HIP 2. 0 collects premiums through contributions to Personal Wellness and Responsibility (POWER) accounts. • Individuals between 100138% FPL are required to contribute to a POWER account. • Contributions cannot exceed 2% of household income • If individuals below 100% FPL do not contribute to a POWER account, the member can only access HIP Basic. • After the 2014 session, Governor Mike Pence submitted waiver to CMS for implementation of an alternative expansion model, HIP 2. 0. 21

INDIANA • HIP 2. 0 is conditioned on the availability of the enhanced federal matching rate and the continuation of the State’s provider assessment on hospitals. • Commercial coverage for HIP 2. 0 members becomes effective on the date of the first premium payment rather than on the date of application. • Employment requirement was not approved by CMS • Indiana is allowed to refer HIP 2. 0 enrollees to “Gateway to Work” (a separate state run program). In the 1 st year… • 73% of the eligible population participated in HIP 2. 0 • The program added over 5, 300 additional providers to serve Medicaid and HIP 2. 0 members. 22
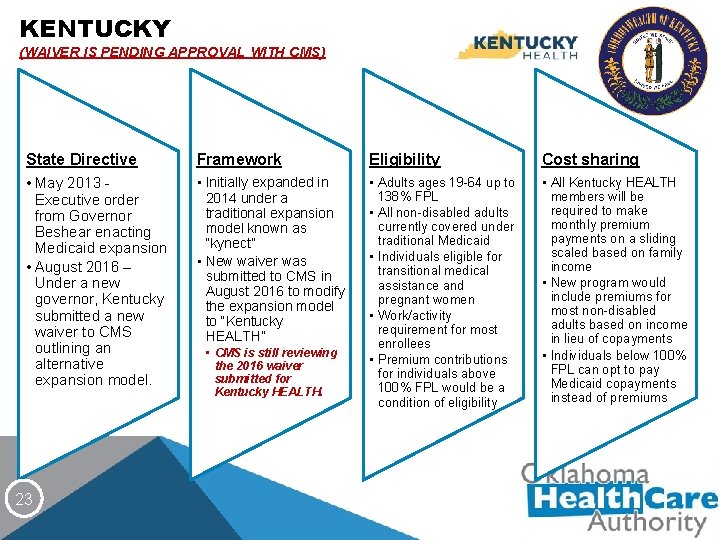
KENTUCKY (WAIVER IS PENDING APPROVAL WITH CMS) State Directive • May 2013 - Executive order from Governor Beshear enacting Medicaid expansion • August 2016 – Under a new governor, Kentucky submitted a new waiver to CMS outlining an alternative expansion model. 23 Framework Eligibility Cost sharing • Initially expanded in 2014 under a traditional expansion model known as “kynect” • New waiver was submitted to CMS in August 2016 to modify the expansion model to “Kentucky HEALTH” • Adults ages 19 -64 up to 138% FPL • All non-disabled adults currently covered under traditional Medicaid • Individuals eligible for transitional medical assistance and pregnant women • Work/activity requirement for most enrollees • Premium contributions for individuals above 100% FPL would be a condition of eligibility • All Kentucky HEALTH members will be required to make monthly premium payments on a sliding scaled based on family income • New program would include premiums for most non-disabled adults based on income in lieu of copayments • Individuals below 100% FPL can opt to pay Medicaid copayments instead of premiums • CMS is still reviewing the 2016 waiver submitted for Kentucky HEALTH.

KENTUCKY • Kentucky has seen a 12. 9% decrease to its uninsured rate between 2013 and 2015. * Notable changes under the Kentucky HEALTH plan: • Includes two health care spending accounts to cover deductible expenses and to accrue savings for enhanced benefits • The state will make contributions and enrollees can earn funds by completing health focused activities. • Funds in the accounts can be used to purchase benefits not covered, such as dental, vision, OTC medications and gym memberships *Source: Gallup, http: //www. gallup. com/poll/189023/arkansas-kentucky-set-pace-reducing-uninsured-rate. aspx/ 24

TENNESSEE (Proposal from 3 Star Healthy Task Force) State Directive Framework Eligibility Cost Sharing • In February 2015, Tennessee’s Senate Health and Welfare Committee voted against a Medicaid expansion plan presented by Governor Bill Haslam. • Later that year, Republican lawmakers established the “ 3 Star Healthy Task Force” to study Medicaid. • The proposal would expand upon the existing Tenn. Care MCO model. • The Task Force is recommending a twophase approach: • Phase 1: pilot would focus on behavioral health disorders and uninsured veterans • Phase 2: all qualifying Tennesseans with incomes up to 138% FPL • Phase 1: Adults 19 -64 with incomes up to 138% FPL who have a qualifying diagnosis of a mental illness or substance abuse disorder OR proof of an honorable discharge from the military • Phase 2: All adults 19 -64 with income up to 138% FPL (not contingent upon BH disorder or veteran status) • Both phases would include state assistance in finding employment, securing job training and/or obtaining a degree. • Individuals would pay premiums and varying co-payments based on FPL • Health savings accounts would be piloted in Phase 1 25

QUESTIONS?
- Slides: 26