Additional Oxygen Devices Blenders Air Compressors Oxygen Concentrators

Additional Oxygen Devices Blenders, Air Compressors, Oxygen Concentrators, Transcutaneous Monitoring, Pulse Oximetry, and Analyzers

Blending Systems • Consider when air-entrainment devices cannot provide a high enough O 2 concentration or flow • Separate pressurized air and O 2 sources are input • Gases are mixed either manually or with a precision valve • This system allows precise control over both Fi. O 2 and total flow output • 2

Oxygen Blenders and Mixers • Mixes 50 psig source of oxygen and air to obtain precise FIO 2 • Precision metering device (proportioning valve). • Low pressure alarm (reed valve) sounding indicates low inlet pressure (< 40 PSI) • 3

Oxygen Blenders • Air and O 2 enter the blender and pass through dual pressure regulators that exactly match the two pressures • Gas flows to a precision proportioning valve • Because the two gas pressures at this point are equal, varying the size of the air and O 2 inlets provides precise control over the relative concentration • 4

Oxygen Blender • 5

Air Compressor • Provides a compressed gas source without using an air cylinder • Can be used in a hospital, out-patient clinic or in the home setting. • Can be used to power a hand-held nebulizer (SVN) for a COPD patient in the home setting. • 6

Oxygen Concentrators • Alternative to compressed-gas systems in the home • Principle of operation: -Electrically powered and have limited portability -Utilize a molecular sieve that removes nitrogen and other gases from room air to concentrate the oxygen -Oxygen can be provided at 1 -2 LPM continuously • 7

Oxygen Concentrator – continued • Safety: • -Instruct patients to routinely check and change filters • -A properly grounded electrical outlet is required • -A backup system (cylinder) must be available in case of a power failure. • 8

Oxygen Concentrator - continued • Troubleshooting • -If patient states that no flow is sensed from the cannula, ask the patient to verify this by inserting the cannula into a glass of water and checking for bubbles. • If no bubbles are seen: • Check power source • Check flow setting • Check humidifier for leaks (if using a humidifier) • Check tubing for leaks, disconnections, or • 9

Transcutaneous PO 2 Electrode (tc. PO 2) • Adaptations to Clark and Severinghaus electrodes • Heating skin around electrode to 43 -45 degrees centigrade improves capillary blood flow (perfusion) and enhances gas movement through the skin • Accuracy decreases with increased skin thickness, anemia, and conditions of decreased perfusion such as shock, burns, vascular disease or cardiac defects. • Best placement of the electrode is over flat areas with good perfusion. Normally on the chest, just beneath the center of the right or left clavicle.

Transcutaneous PO 2 Electrode (tc. PO 2) § Electrode site should be changed every 4 hours. If redness or blistering of the skin (erythema) occurs, the electrode should be moved to a new site more often. § Calibration is done on room air (PO 2 = 150 torr, PCO 2 = 0 torr) and with a zeroing solution. § If unable to calibrate, check for torn membrane, poor connections. § Air leaks will increase the Tc. PO 2 to read higher than the Pa. O 2 • 11
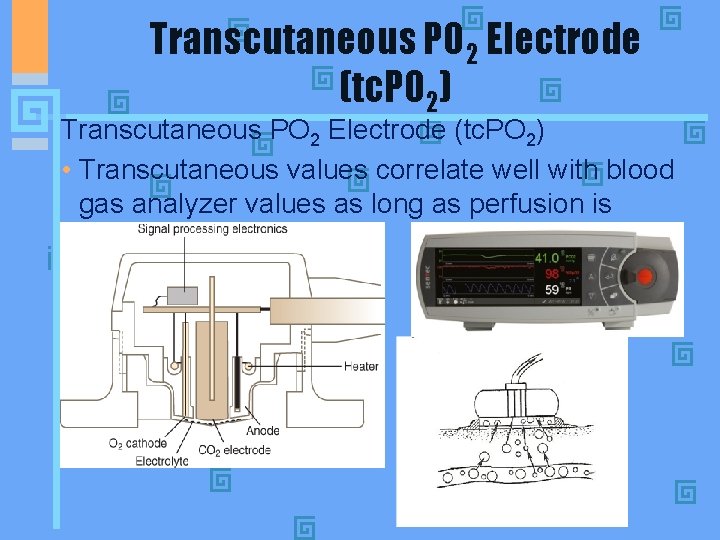
Transcutaneous PO 2 Electrode (tc. PO 2) • Transcutaneous values correlate well with blood gas analyzer values as long as perfusion is adequate.

What is a Pulse Oximeter? Pulse Oximeter is a device used to perform the diagnostic procedure for determining the: Percentage of hemoglobin (Hb) that is saturated with oxygen The oxygen saturation (Sp. O 2) is a measure of how much oxygen the blood is carrying as a percentage of the maximum it could carry and is sometimes referred to colloquially as the "sats" reading The heart rate refers to the number of times that the heart contracts in a period of one minute

Pulse Oximetry • Provides noninvasive measurement of oxygen saturation • Sensor can be placed on: • Digit • Earlobe • Forehead • Bridge of nose • Sensor measures absorption of selected wavelengths of light • 14

Pulse Oximetry • Works with absorption of red and infrared light • Types of hemoglobin measured with oximetry: • Reduced hemoglobin • Oxyhemoglobin • Carboxyhemoglobin • Methemoglobin • 15 • OPERATES on BEER’s LAW
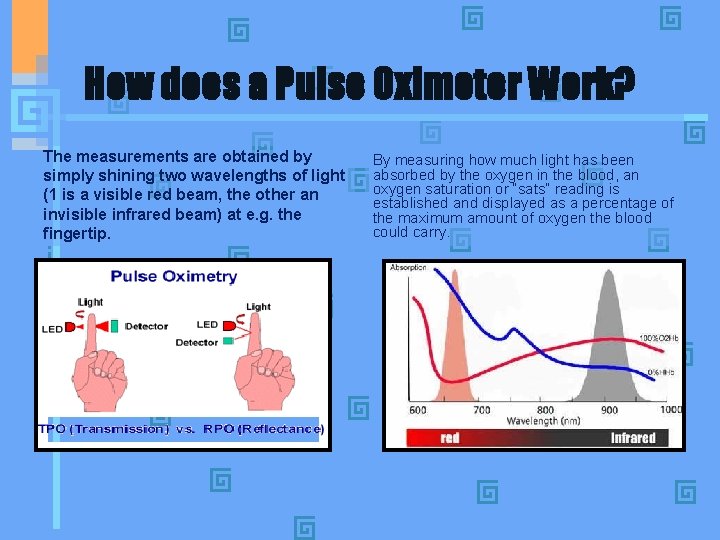
How does a Pulse Oximeter Work? The measurements are obtained by simply shining two wavelengths of light (1 is a visible red beam, the other an invisible infrared beam) at e. g. the fingertip. By measuring how much light has been absorbed by the oxygen in the blood, an oxygen saturation or “sats” reading is established and displayed as a percentage of the maximum amount of oxygen the blood could carry.

Pulse Oximetry (Cont. ) • 17
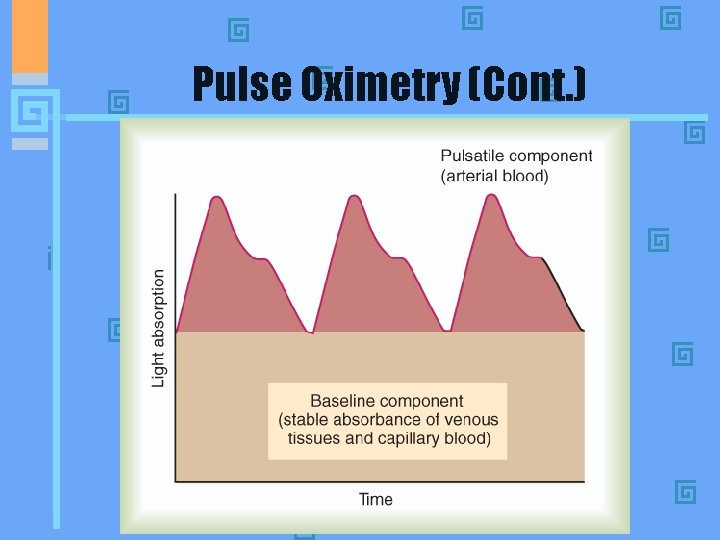
Pulse Oximetry (Cont. ) • 18

Factors Affecting Accuracy of Pulse Oximeter • Low perfusion states • Hypovolemia • Peripheral vasoconstriction from drugs or hypothermia • Low cardiac outputs • Heart lung bypass • 19

Factors Affecting Accuracy of Pulse Oximeter (Cont. ) • Dysfunctional hemoglobin • Carboxyhemoglobin has similar adsorption of light as oxyhemoglobin (monitored as oxyhemoglobin) • Methemoglobin adsorbs red and infrared light, preventing accurate measurement of red and infrared light • 20

Factors Affecting Accuracy of Pulse Oximeter (Cont. ) • Dyes • Intravascular dyes absorb portion of light from light- emitting diode • Dark nail polish (especially blue or black) severely affects accuracy of pulse oximeters • Ambient light • Fluorescent light and external light sources affect accuracy of Sp. O 2 and heart rate measurements • Newer pulse oximeters • 21 attempt to

The following won’t affect the Pulse Oximeter signal: Anemia-will read higher Jaundice

But what is a "normal" reading? Firstly, we would ask "normal for whom"? A fit, healthy person should have an oxygen saturation level between 95% & 99%. Results lower than this, and especially below 90% may be caused by problems including lung diseases, such as COPD, breathing difficulties, cigarette smoking or circulatory problems such as excessive bleeding or blood vessel problems.

Setting the Alarms • For continuous monitoring of children and adult (unhealthy patients) set the low alarm between 88 -92%. • For healthy patients during a procedure set the low alarm between 92 -94%. • 24

Calibration of Pulse Oximeters • Calibrated with data obtained from healthy subjects • Human volunteers breathe gases with various FIO 2 levels • Pulse oximeters provide accurate data if Sp. O 2 is above 80% • If Sp. O 2 is below 80%, results should be confirmed with ABG with co-oximetry • 25

Clinical Application of Pulse Oximetry • Probes available in neonatal, pediatric, and adult sizes • Improved technology allows development of fingertip pulse oximeters • Fingertip probes require 12 seconds or longer to obtain reading than other sites require • Useful in adjusting level of oxygen therapy • 26 • Can be used to qualify patient for home

CPG: Pulse Oximetry • Indications • Monitoring arterial oxyhemoglobin saturation • Quantifying arterial oxyhemoglobin saturation response to therapeutic intervention • Monitoring arterial oxyhemoglobin saturation during bronchoscopy or conscious-sedated procedures • Contraindications • May not be appropriate when ongoing measurement of p. H, Pa. CO 2, and Pa. O 2 are • 27 required

CPG: Pulse Oximetry (Cont. ) • Limitations (factors affecting accuracy) • Motion artifacts • Abnormal hemoglobin (COHb and Met. Hb) • Intravascular dyes • Exposure of sensor to ambient light sources • Low perfusion states • Skin pigmentation • Nail polish - dark • Low Sp. O 2 levels (<80%) • 28

CPG: Pulse Oximetry (Cont. ) • Monitors (information recorded with use of pulse oximeter): • Type of probe, measurement site, date and time of measurement, patient position, and activity level • FIO 2 and method of administration for supplemental oxygen • ABG and co-oximeter results • Clinical appearance of patient • Correlation of heart • 29 rate from pulse oximeter

Oxygen Analyzers • Galvanic fuel cell - -Creates electron flow as a result of the oxidation/reduction of oxygen (produces a current) - -Measures partial pressure, displays FIO 2 as % - -Accuracy can be affected by water on the sensor, high system pressures and changes in altitude - -If unable to calibrate, change fuel cell • 30

Oxygen Analyzers - continued • Polarographic -Operation is similar to a galvanic fuel cell except for the presence of a battery used to polarize the electrodes. -This type of device is analogous to the Clark electrode -Measures partial pressure, displays FIO 2 as % -Accuracy can be affected by water, high pressure, and altitude. -If unable to calibrate, change the battery and • 31

Oxygen Analyzers -continued • Polarographic • 32

Oxygen Analyzers - continued • Troubleshooting -If after setup of a ventilator, blender or venturi system the oxygen analyzer reads higher or lower – recalibrate analyzer and then recheck equipment -Must be accurate within 2% of the known value • 33

Additional analyzers • Helium analyzer -Thermal conductivity (Wheatstone bridge) -Measures % -Calibrate to room air (0%) and a known amount (10%), then re-zero. Use gain to adjust known amount. • 34

Additional analyzers - continued • Nitrogen analyzer -Geissler tube ionizer -Measures % -Calibrate to zero with 100% oxygen (0% N 2) and a known concentration • 35

WHEN TO MONITOR O 2 CONCENTRATIONS • All O 2 systems should be checked at least once a day. • More frequent checks by calibrated analyzers are necessary in systems: -Prone to FIO 2 changes: oxygen hoods, high flow blending systems, ventilators -Patients with artificial airways How to calibrate an O 2 analyzer: It is termed a “ 2 point- cal” you will accomplish this by analyzing a room air source 21% and then a pure O 2 source 100%.
- Slides: 36