Acute respiratory failure Definitions acute respiratory failure occurs















































- Slides: 75

Acute respiratory failure

Definitions • acute respiratory failure occurs when: – pulmonary system is no longer able to meet the metabolic demands of the body • hypoxaemic respiratory failure: – Pa. O 2 60 mm. Hg when breathing room air • hypercapnic respiratory failure: – Pa. CO 2 50 mm. Hg k. Pa

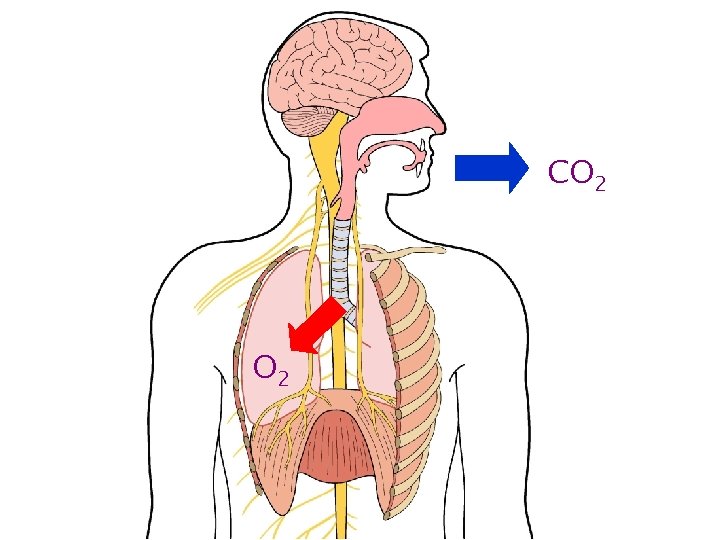
Basic respiratory physiology

CO 2

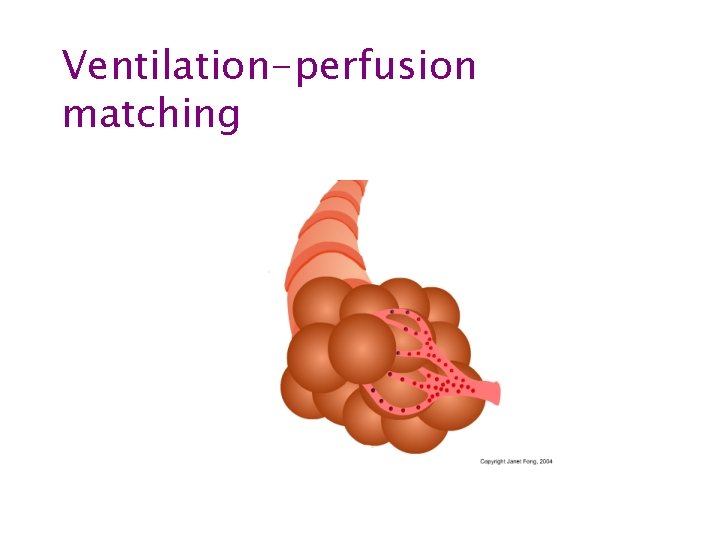
Oxygen in • Depends on – PAO 2 – Diffusing capacity – Ventilation – Perfusion – Ventilation-perfusion matching

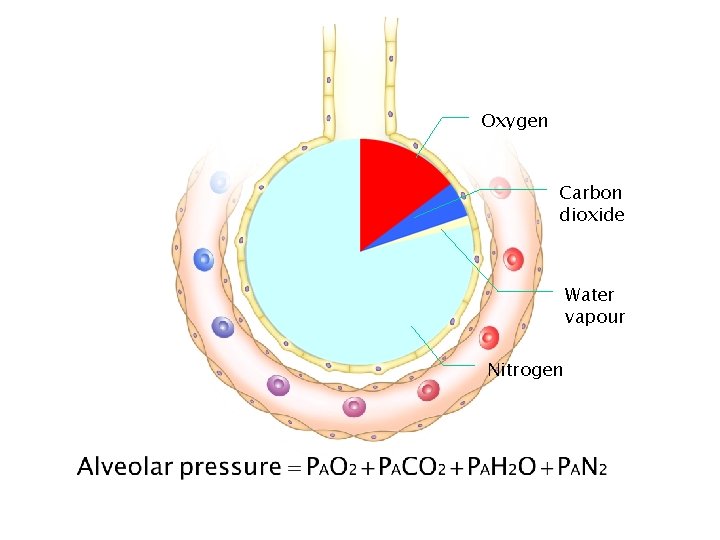
Oxygen Carbon dioxide Water vapour Nitrogen

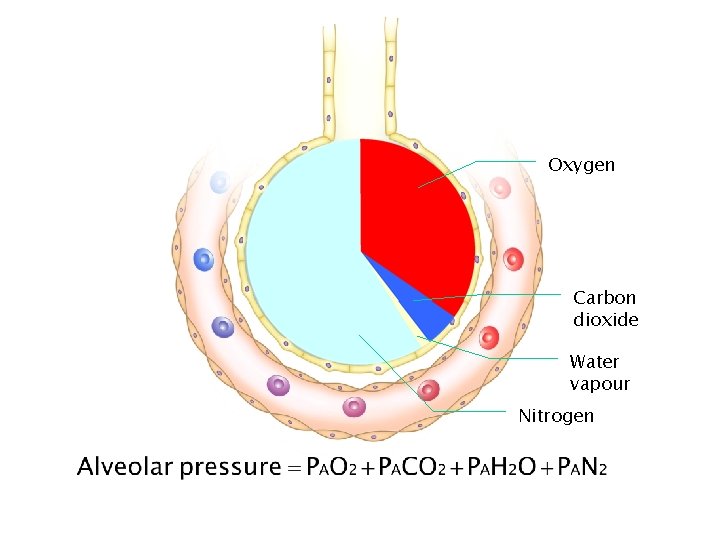
Oxygen Carbon dioxide Water vapour Nitrogen

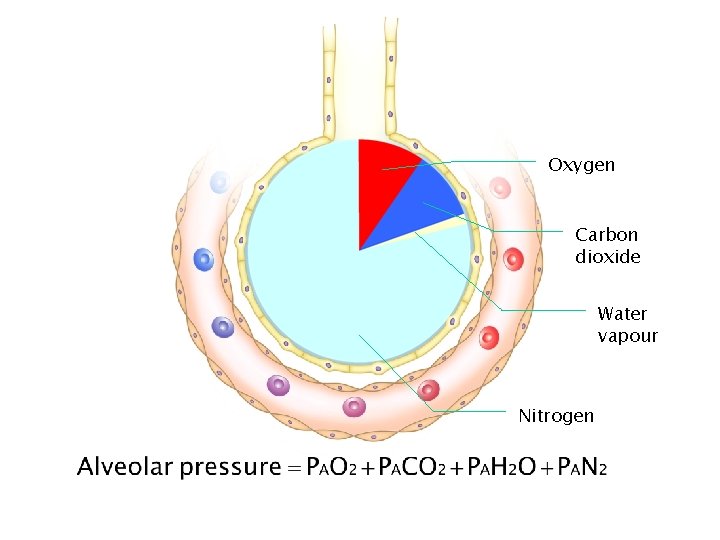
Oxygen Carbon dioxide Water vapour Nitrogen

Oxygen in • Depends on – PAO 2 • F IO 2 • Alveolar pressure • PACO 2 • Ventilation – Ventilation-perfusion matching – Perfusion – Diffusing capacity

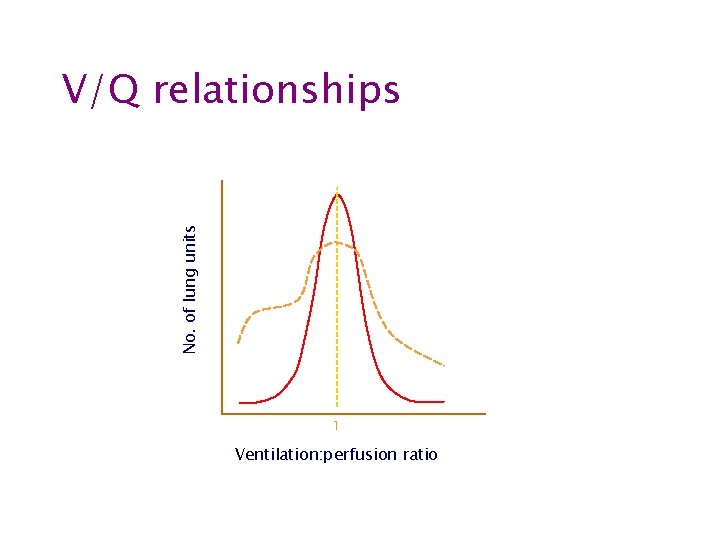
Ventilation-perfusion matching

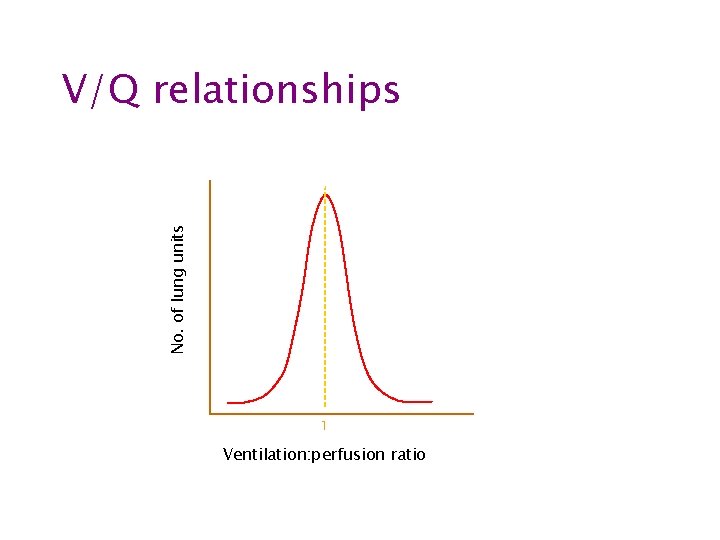
No. of lung units V/Q relationships 1 Ventilation: perfusion ratio

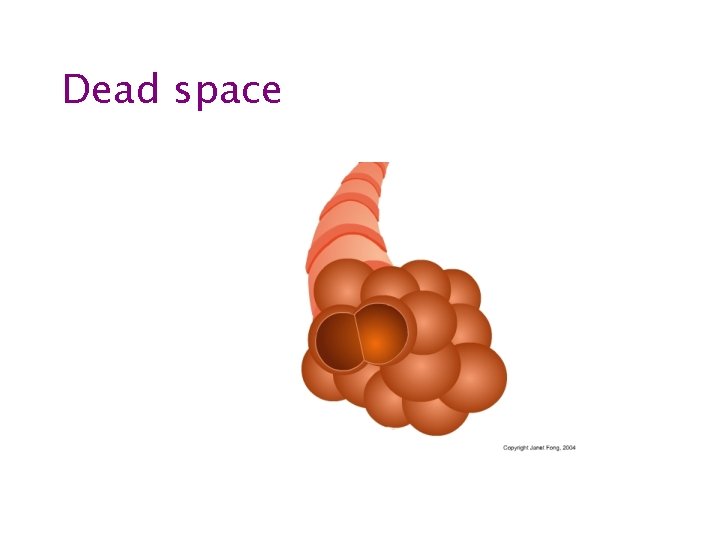
Carbon dioxide out • Largely dependent on alveolar ventilation • Anatomical dead space constant but physiological dead space depends on ventilation-perfusion matching

Carbon dioxide out • Respiratory rate • Tidal volume • Ventilation-perfusion matching

Pathophysiology

Pathophysiology • Low inspired Po 2 • Hypoventilation • Ventilation-perfusion mismatch – Shunting – Dead space ventilation • Diffusion abnormality

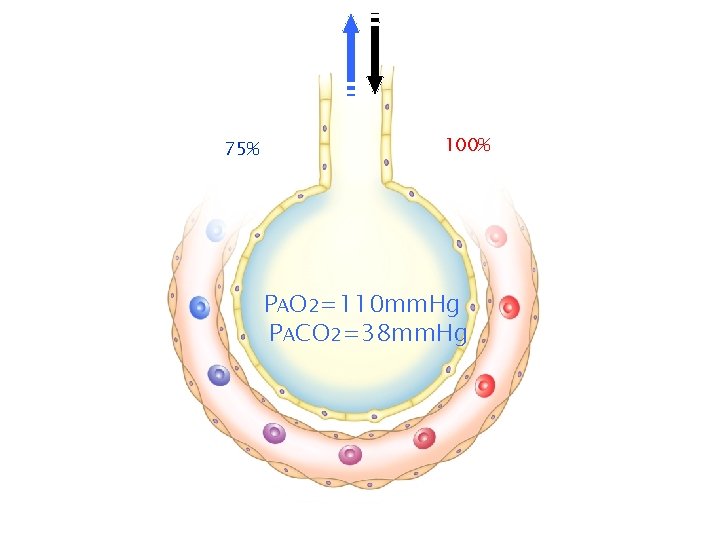
75% 100% PAO 2=110 mm. Hg PACO 2=38 mm. Hg

Pathophysiology • Low inspired oxygen concentration • Hypoventilation • Shunting • Dead space ventilation • Diffusion abnormality

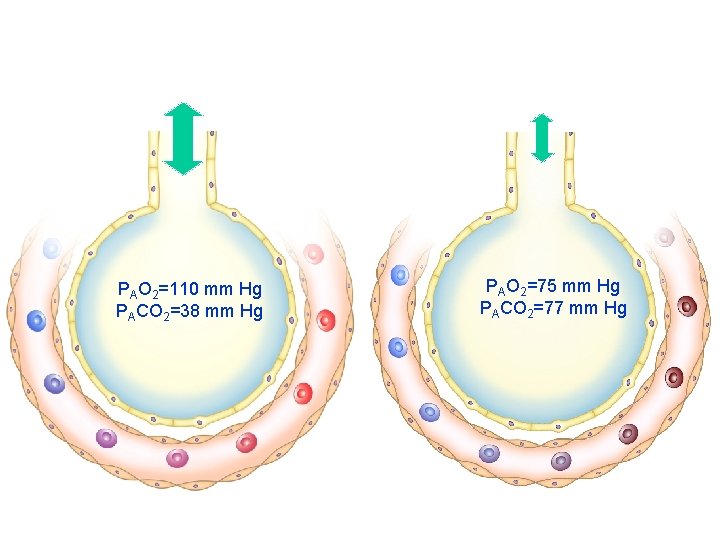
PAO 2=110 mm Hg PACO 2=38 mm Hg PAO 2=75 mm Hg PACO 2=77 mm Hg

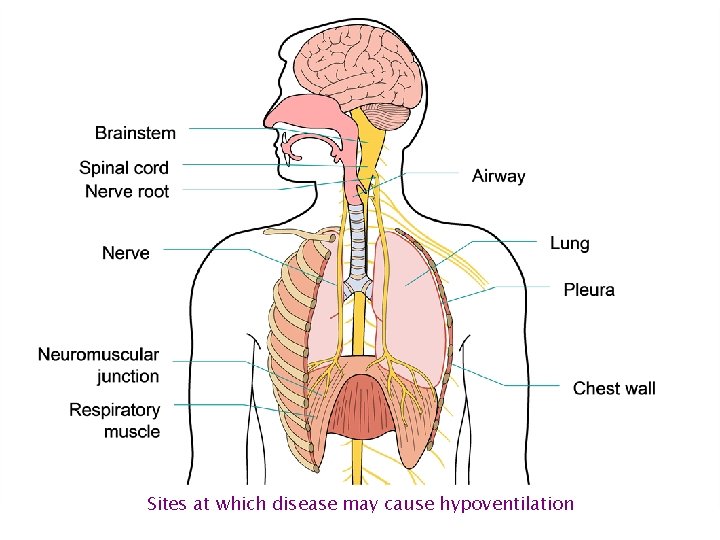
Sites at which disease may cause hypoventilation

Pathophysiology • Low inspired oxygen concentration • Hypoventilation • Shunting • Dead space ventilation • Diffusion abnormality

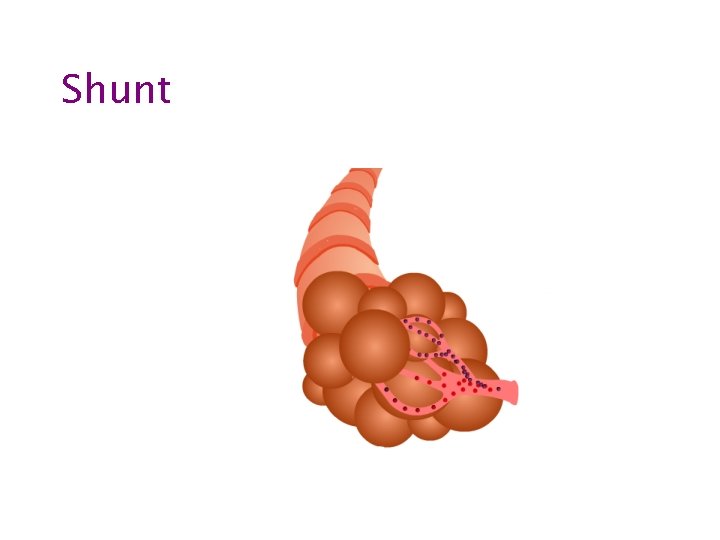
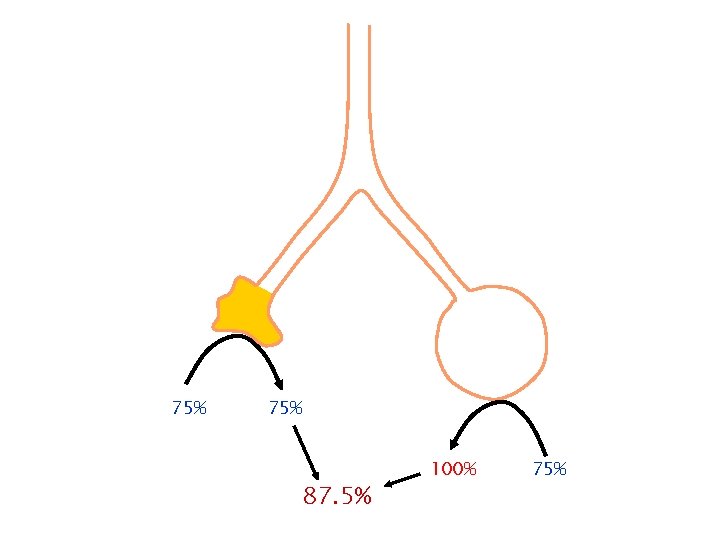
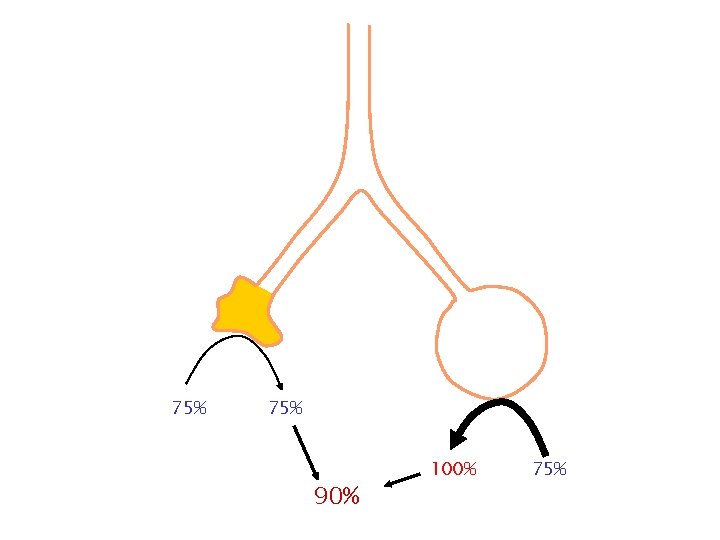
Shunt

75% 87. 5% 100% 75%

75% 90% 100% 75%

Shunting • Intra-pulmonary – – – Pneumonia Pulmonary oedema Atelectasis Collapse Pulmonary haemorrhage or contusion • Intra-cardiac – Any cause of right to left shunt • eg Fallot’s, Eisenmenger, • Pulmonary hypertension with patent foramen ovale

Pathophysiology • Low inspired oxygen concentration • Hypoventilation • Shunting • Dead space ventilation • Diffusion abnormality

Dead space

No. of lung units V/Q relationships Diseased Normal 1 Ventilation: perfusion ratio

Pathophysiology • Low inspired oxygen concentration • Hypoventilation • Shunting • Dead space ventilation • Diffusion abnormality

Respiratory monitoring

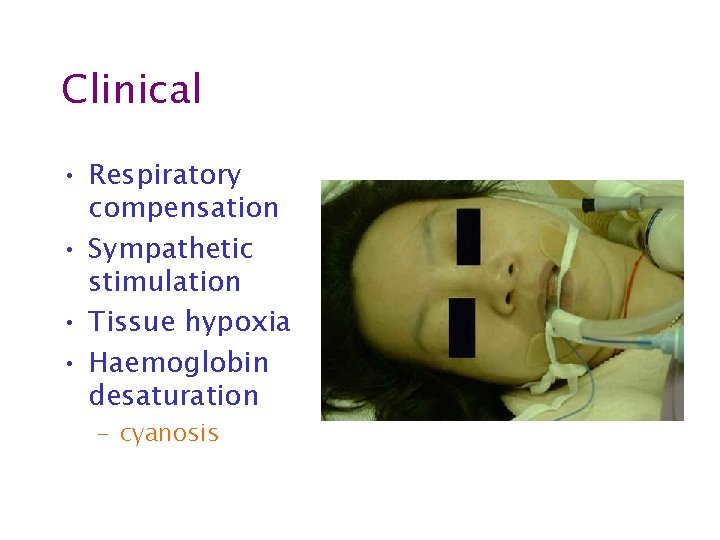
Clinical • Respiratory compensation • Sympathetic stimulation • Tissue hypoxia • Haemoglobin desaturation

Clinical • Respiratory compensation – Tachypnoea – Accessory muscles – Recesssion – Nasal flaring • Sympathetic stimulation • Tissue hypoxia • Haemoglobin desaturation

Clinical • Respiratory compensation • Sympathetic stimulation – HR – BP (early) – sweating • Tissue hypoxia • Haemoglobin desaturation

Clinical • Respiratory compensation • Sympathetic stimulation • Tissue hypoxia – Altered mental state – HR and BP (late) • Haemoglobin desaturation

Clinical • Respiratory compensation • Sympathetic stimulation • Tissue hypoxia • Haemoglobin desaturation – cyanosis

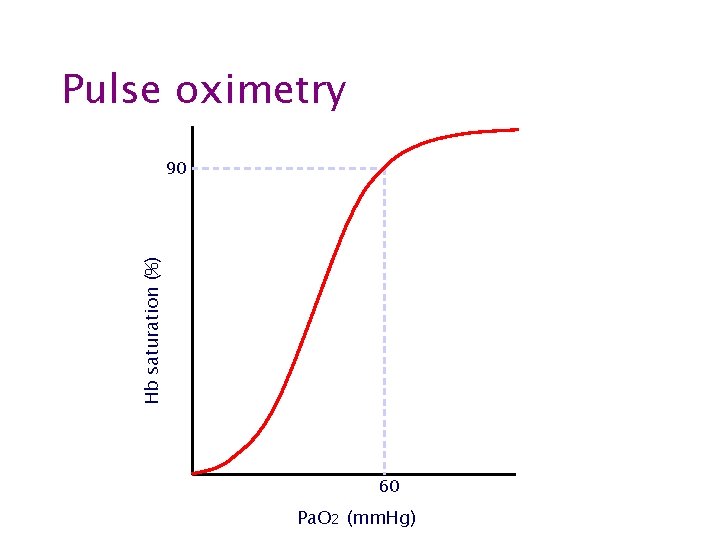
Pulse oximetry Hb saturation (%) 90 60 Pa. O 2 (mm. Hg)

Oxygen delivery

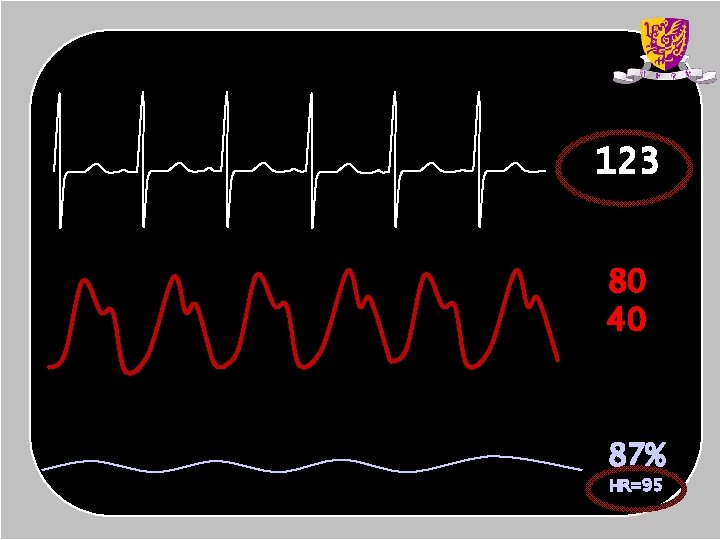
Sources of error • • Poor peripheral perfusion Poorly adherent/positioned probe False nails or nail varnish Lipaemia Bright ambient light Excessive motion Carboxyhaemoglobin or methaemoglobin

123 80 40 87% HR=95

Summary • worry if • RR > 30/min (or < 8/min) • unable to speak 1/2 sentence without pausing • agitated, confused or comatose • cyanosed or Sp. O 2 < 90% • deteriorating despite therapy • remember • normal Sp. O 2 does not mean severe ventilatory problems are not present

Treatment

Treatment • Treat the cause • Supportive treatment – Oxygen therapy – CPAP – Mechanical ventilation

Oxygen therapy • Progressive hypercarbia due to loss of hypoxic drive is RARE • Hypoxia KILLS • The appropriate response to progressive hypercarbia is assisted ventilation NOT removal of oxygen

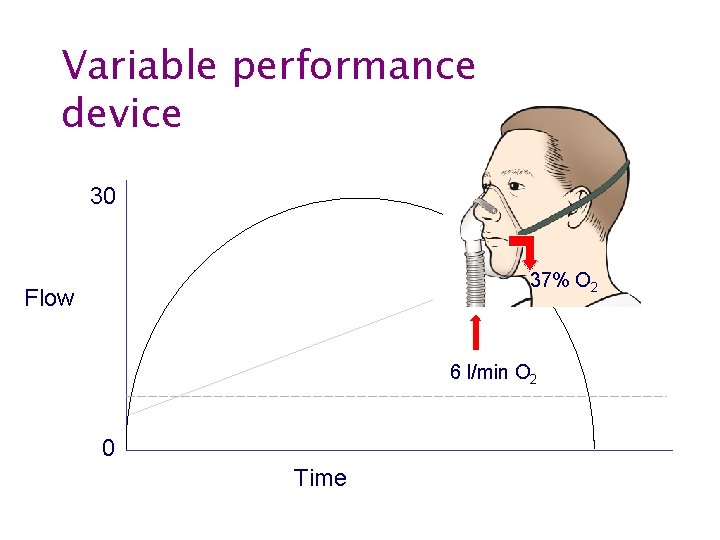
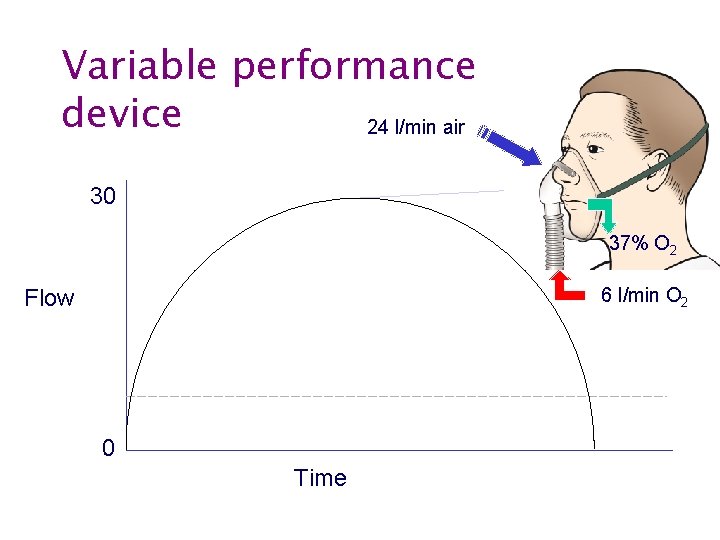
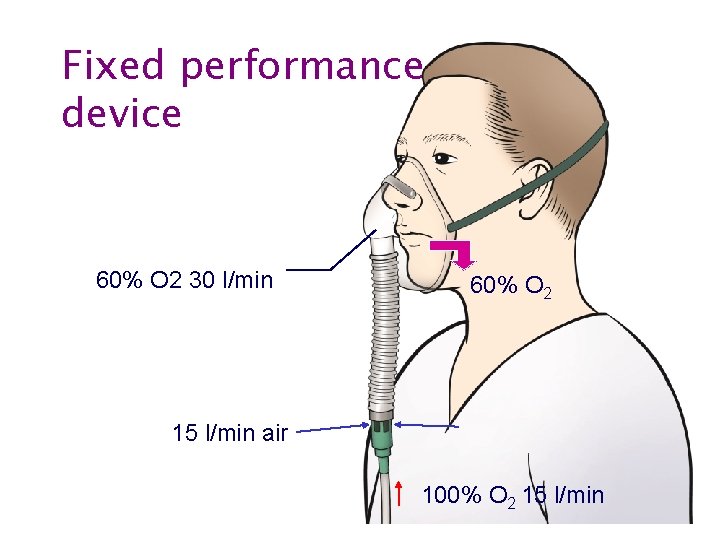
Oxygen therapy • Fixed performance devices • Variable performance devices

Variable performance device 30 37% O 2 Flow 6 l/min O 2 6 0 Time

Variable performance device 24 l/min air 30 37% O 2 6 l/min O 2 Flow 6 0 Time

Fixed performance device 60% O 2 30 l/min 60% O 2 15 l/min air 100% O 2 15 l/min

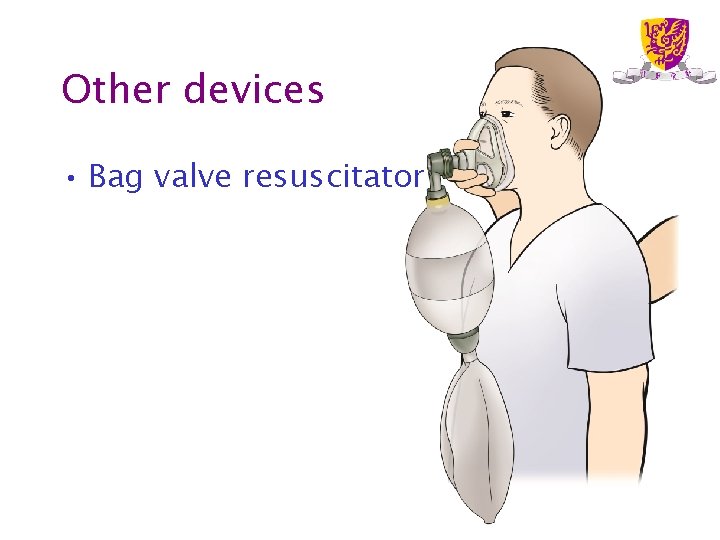
Other devices • Bag valve resuscitator

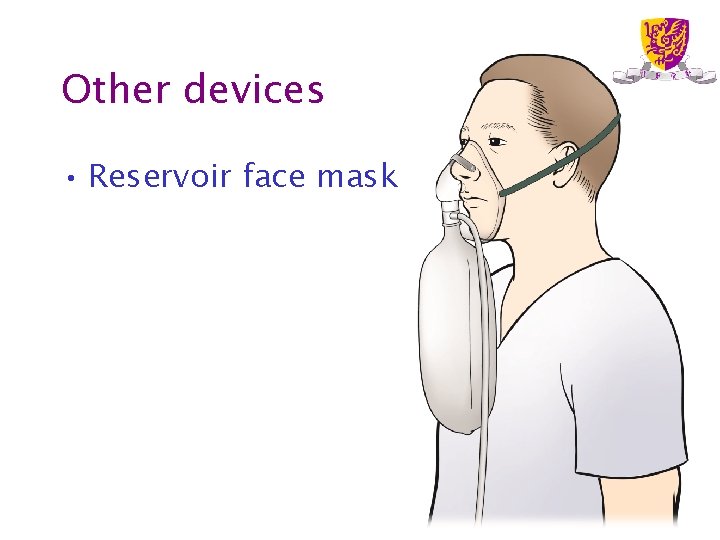
Other devices • Reservoir face mask

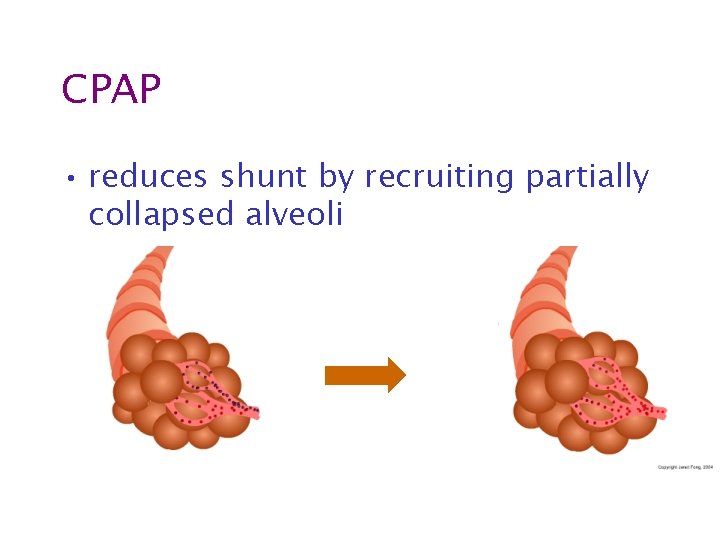
CPAP • reduces shunt by recruiting partially collapsed alveoli

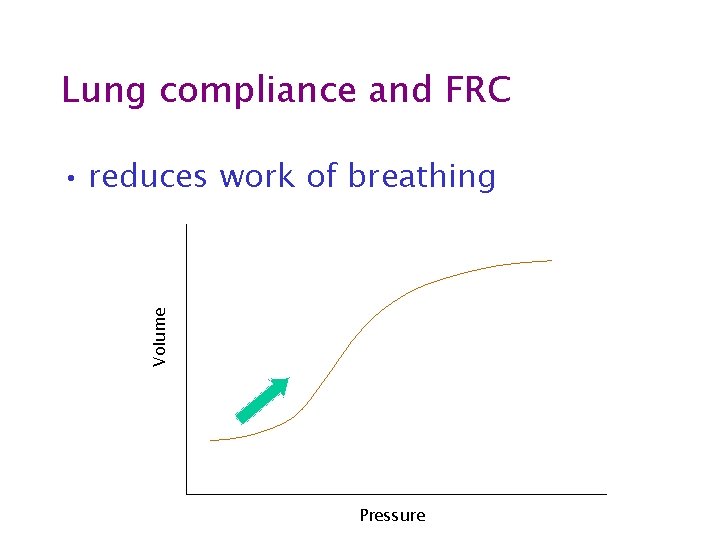
Lung compliance and FRC Volume • reduces work of breathing Pressure

Mechanical ventilation • Decision to ventilate – Complex – Multifactorial – No simple rules

Ventilate? • Severity of respiratory failure

Ventilate? • Severity of respiratory failure • Cardiopulmonary reserve

Ventilate? • Severity of respiratory failure • Cardiopulmonary reserve • Adequacy of compensation – Ventilatory requirement

Ventilate? • Severity of respiratory failure • Cardiopulmonary reserve • Adequacy of compensation – Ventilatory requirement • Expected speed of response – Underlying disease – Treatment already given

Ventilate? • Severity of respiratory failure • Cardiopulmonary reserve • Adequacy of compensation – Ventilatory requirement • Expected speed of response – Underlying disease – Treatment already given • Risks of mechanical ventilation

Ventilate? • Severity of respiratory failure • Cardiopulmonary reserve • Adequacy of compensation – Ventilatory requirement • Expected speed of response – Underlying disease – Treatment already given • Risks of mechanical ventilation • Non-respiratory indication for intubation


Ventilate? • 43 year old male • Community acquired pneumonia • Day 1 of antibiotics • Pa. O 2 60 mm. Hg, Pa. CO 2 30 mm. Hg, p. H 7. 15 on 15 l/min O 2 via reservoir facemask • Respiratory rate 35/min • Agitated

Yes • 43 year old male • Community acquired pneumonia • Day 1 of antibiotics • Pa. O 2 60 mm. Hg, Pa. CO 2 30 mm. Hg, p. H 7. 15 on 15 l/min O 2 via reservoir facemask • Respiratory rate 35/min • Agitated

Yes • 43 year old male • Community acquired pneumonia • Day 1 of antibiotics • Pa. O 2 60 mm. Hg, Pa. CO 2 30 mm. Hg, p. H 7. 15 on 15 l/min O 2 via reservoir facemask • Respiratory rate 35/min • Agitated

Yes • 43 year old male • Community acquired pneumonia • Day 1 of antibiotics • Pa. O 2 60 mm. Hg), Pa. CO 2 30 mm. Hg, p. H 7. 15 on 15 l/min O 2 via reservoir facemask • Respiratory rate 35/min • Agitated

Yes • 43 year old male • Community acquired pneumonia • Day 1 of antibiotics • Pa. O 2 8 k. Pa (60 mm. Hg), Pa. CO 2 4 k. Pa (30 mm. Hg), p. H 7. 15 on 15 l/min O 2 via reservoir facemask • Respiratory rate 35/min • Agitated

Yes • 43 year old male • Community acquired pneumonia • Day 1 of antibiotics • Pa. O 2 8 k. Pa (60 mm. Hg), Pa. CO 2 4 k. Pa (30 mm. Hg), p. H 7. 15 on 15 l/min O 2 via reservoir facemask • Respiratory rate 35/min • Agitated

Ventilate? • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25 Pa. CO 2 51 mm. Hg, Pa. O 2 315 mm. Hg on Fi. O 2 0. 6 • RR 35/min • Alert

No • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25 Pa. CO 2 51 mm. Hg, Pa. O 2 315 mm. Hg on Fi. O 2 0. 6 • RR 35/min • Alert

No • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25, Pa. CO 2 51 mm. Hg, Pa. O 2 315 mm. Hg on Fi. O 2 0. 6 • RR 35/min • Alert

No • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25 Pa. CO 2 51 mm. Hg, Pa. O 2 315 mm. Hg on Fi. O 2 0. 6 • RR 35/min • Alert

No • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25 Pa. CO 2 51 mm. Hg, Pa. O 2 315 mm. Hg on Fi. O 2 0. 6 • RR 35/min • Alert

No • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25 Pa. CO 2 6. 8 k. Pa (51 mm. Hg), Pa. O 2 42 k. Pa (315 mm. Hg) on Fi. O 2 0. 6 • RR 35/min • Alert

No • 24 year old woman • Presents to A&E with acute asthma – SOB for 2 days • Salbutamol inhaler, no steroids • PFR 60 L/min, HR 105/min • p. H 7. 25, Pa. CO 2 51 mm. Hg, Pa. O 2 315 mm. Hg on Fi. O 2 0. 6 • RR 35/min • Alert

Summary • Shunting is the most common cause of acute respiratory failure in acutely ill patients – High concentrations of oxygen are required • Hypoventilation due to abolition of hypoxic drive is RARE

Summary • worry if • RR > 30/min (or < 8/min) • unable to speak 1/2 sentence without pausing • agitated, confused or comatose • cyanosed or Sp. O 2 < 90% • deteriorating despite therapy • remember • normal Sp. O 2 does not mean severe ventilatory problems are not present

Treatment • Treat the cause • Supportive treatment – Oxygen therapy – CPAP – Mechanical ventilation

Ventilation • Severity of respiratory failure • Cardiopulmonary reserve • Adequacy of compensation – Ventilatory requirement • Expected speed of response – Underlying disease – Treatment already given • Risks of mechanical ventilation • Non-respiratory indication for intubation