Acute Respiratory Distress Syndrome Jason D Sciarretta M


















- Slides: 24

Acute Respiratory Distress Syndrome Jason D. Sciarretta, M. D. Critical Care Conference October 13, 2010

History ARDS n The syndrome of acute pulmonary failure was recognized during World War I n “The acute onset of severe respiratory distress and cyanosis that was refractory to oxygen therapy and associated with diffuse CXR abnormality and decreased lung compliance” – Ashbaugh DG. Acute Respiratory distress in Adults. Lancet 1967

History ARDS n In 1988, Murray: – 4 point scoring system: Lung Injury Score (LIS) § PEEP, compliance, CXR, Pa. O 2/Fi. O 2 ratio n North American-European Consensus Committee – devised of multiple subcommitees: – 1994: “Adult” RDS now referred back to “acute” – Study the pathophysiologic mechanisms, prevention & treatment – further defined diagnostic criteria, future studies – 1998: severity ARDS should be assessed by the Lung Injury Score or by APACHE Bernard GR et al. , Am J Respir Crit Care Med. 1994 Murray JF, et al. Am Rev Respir Dis. 1988; 138: 720 Bernard GR et al. , Am J Respir Crit Care Med. 1994 Artigas A, et al. , Am J Respir Crit Care Med 1998 3

Epidemiology n 1972 - Incidence US: ~ 150, 000 cases/yr n “true” incidence defined by LIS lower— 1. 5 to 8 cases per 100, 000 people n ARDS Network Study (NAECC definitions), 2003 – Incidence United States: 32 cases per 100, 000/y Goss CH et al. , ARDS Network, Crit Care Med 2003 n 10 % ICU admission in US related ARDS 4

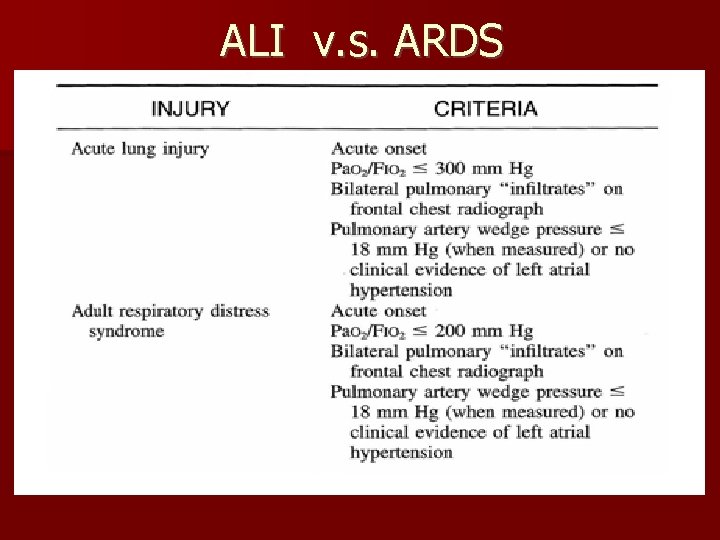
ALI v. s. ARDS

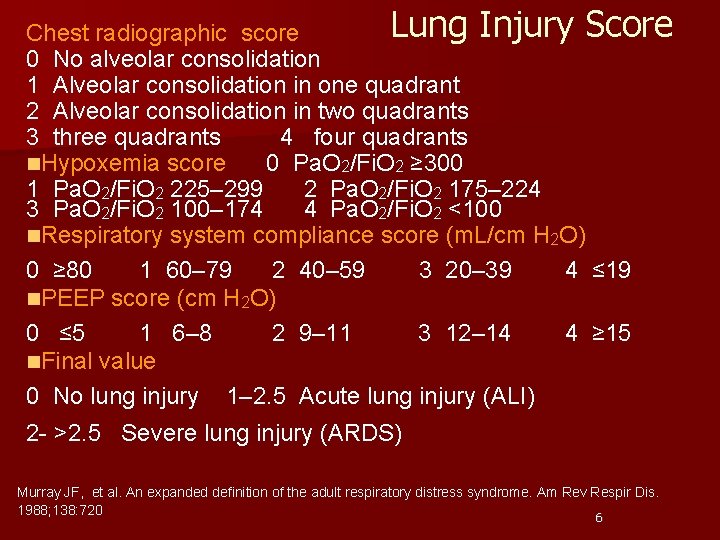
Lung Injury Score Chest radiographic score 0 No alveolar consolidation 1 Alveolar consolidation in one quadrant 2 Alveolar consolidation in two quadrants 3 three quadrants 4 four quadrants n. Hypoxemia score 0 Pa. O 2/Fi. O 2 ≥ 300 1 Pa. O 2/Fi. O 2 225– 299 2 Pa. O 2/Fi. O 2 175– 224 3 Pa. O 2/Fi. O 2 100– 174 4 Pa. O 2/Fi. O 2 <100 n. Respiratory system compliance score (m. L/cm H 2 O) 0 ≥ 80 1 60– 79 2 40– 59 3 20– 39 4 ≤ 19 n. PEEP score (cm H 2 O) 0 ≤ 5 1 6– 8 2 9– 11 3 12– 14 4 ≥ 15 n. Final value 0 No lung injury 1– 2. 5 Acute lung injury (ALI) 2 - >2. 5 Severe lung injury (ARDS) Murray JF, et al. An expanded definition of the adult respiratory distress syndrome. Am Rev Respir Dis. 1988; 138: 720 6

ARDS Risk DIRECT - Common: n Pneumonia n Aspiration – Less common n Pulmonary contusion n Fat emboli n Near-drowning n Inhalational injury n Reperfusion after lung transplant or pulmonary embolectomy INDIRECT Common: n Sepsis (40%) n Severe trauma n Shock - Less Common: n Multiple transfusions n Cardiopulmonary bypass n Drug overdose n Burns n Acute pancreatitis n Multiple transfusions The American-European Consensus Conference on ARDS. Am J Respir Crit Care Med. 1994; 149: 818. Atabai K, Matthay MA. Thorax. 2000. Estenssoro E et al Crit Care Med 2002 Frutos-Vivar F, et al. Curr Opin Crit Care. 2004. 8

n Shock Associated Conditions – Hemorrhagic, Cardiogenic, Septic, Anaphylactic n Trauma – Burns, Nonthoracic trauma (especially head trauma), Fat emboli, Lung contusion, Near-drowning n Infection – Viral/bacterial/fungal pneumonia, Gram- negative sepsis, TB n Inhalation of toxic Gas – Oxygen, smoke, Cadmium, Phosgene NO 2, NH 3, Cl 2 n Drug ingestion – Cocaine, Heroin, Methadone, Barbiturates, Ethchlorvynol, Thiazides, Fluorescein, Propoxyphene, Salicylates, Chlordiazepoxide, Colchicine, Dextran 40 n Aspiration of Gastric contents and Metabolic n Miscellaneous – Pancreatitis, Postcardiopulmonary bypass, Postcardioversion, Multiple transfusions, DIC, Leukoagglutinin reaction, Eclampsia, Air or amniotic fluid emboli, Bowel infarction, Carcinomatosis The American-European Consensus Conference on ARDS. 1994 9

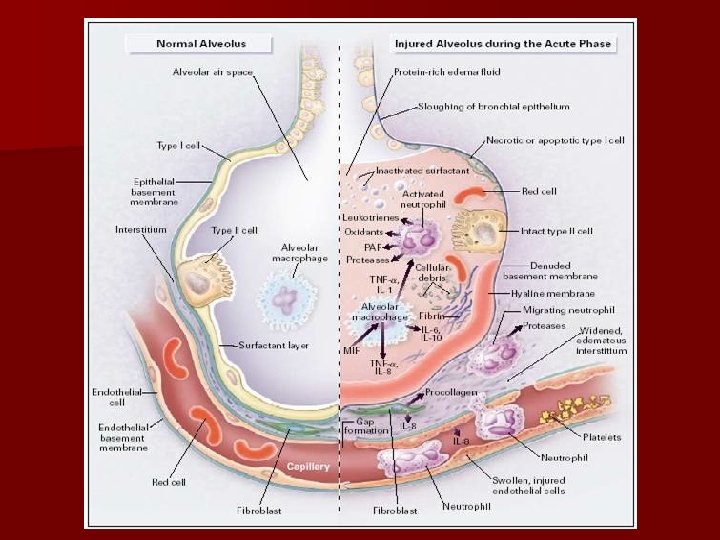
Pathophysiology n Neutrophils release inflammatory mediators -->degrading integrity of capillary endothelial cells--->capillary permeability, interstitial edema. n Influx of proteinaceous plasma fluid, erythrocytes, and inflammatory cells into the interstitium – destroyed surfactant and type 1 and 2 pneumocyte § Increases alveolar surface tension, thus producing alveolar collapse Asensio J, Trunkey D: Current Therapy Trauma & Surgical Critical Care Civetta: Critical Care, 4 th edition Chapter 136: Acute Lung Injury & Acute Respiratory Distress Syndrome 9

Stages of ARDS n 1. Exudative (acute): 0 -4 d n 2. Proliferative: 4 -8 d n 3. Fibrotic: >8 d n 4. Recovery 10

11

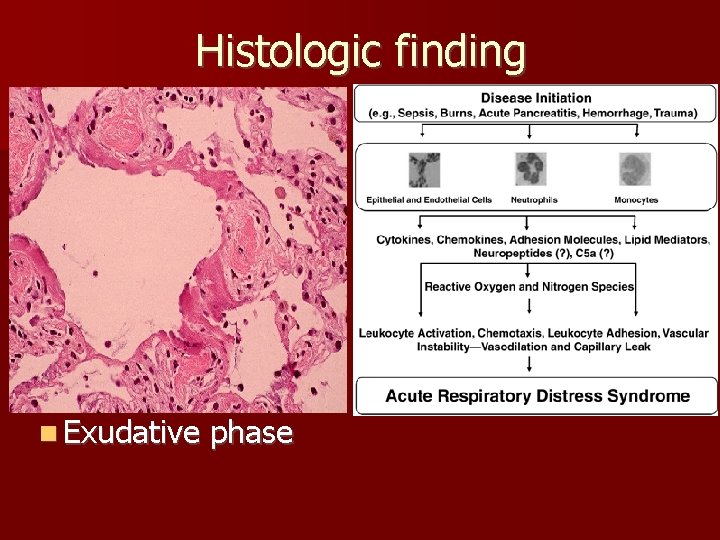
Histologic finding n Exudative phase

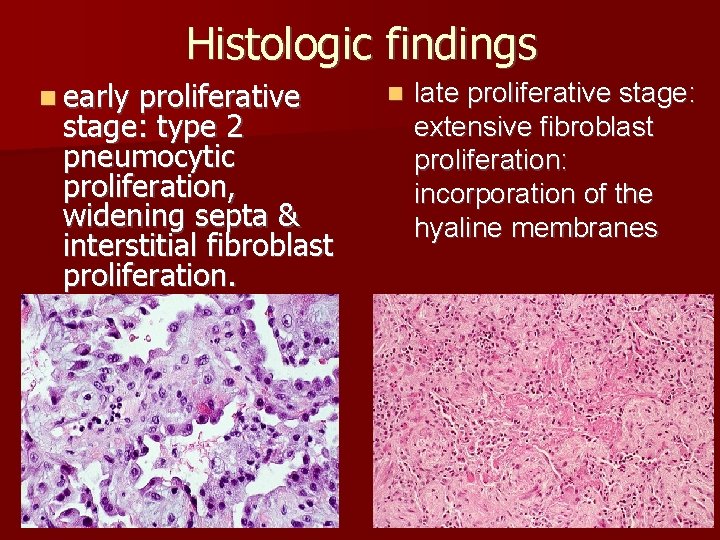
Histologic findings n early proliferative stage: type 2 pneumocytic proliferation, widening septa & interstitial fibroblast proliferation. n late proliferative stage: extensive fibroblast proliferation: incorporation of the hyaline membranes

Plasma Biologic Markers Predictive of a Poor Outcome Acute inflammation Endothelial injury Epithelial type II cell Adhesion molecule IL-6, IL-8 v. WF antigen Surfactant protein-D Intercellular adhesion molecule (ICAM-1) Neutrophil-endothelial Soluble TNF receptors I & II (s. TNFRI/II) interation Procoagulant activity Protein C Plasminogen activator inhibitor-1 Fibrinolytic activity 5 Ware LB, Crit Care Med. 2005

Clinical Progression n Phase 1: Acute Injury • • Normal physical examination and chest radiograph Tachycardia, tachypnea, and respiratory alkalosis develop n Phase 2: Latent Period • Lasts ~ 6– 48 h after injury: remains clinical stable • Hyperventilation & hypocapnia persist; mild increase work breathing • Minor abnormalities on physical examination and chest radiograph n Phase 3: Acute Respiratory Failure • Decreased lung compliance: marked tachypnea & dyspnea • Diffuse infiltrates on chest radiograph • High-pitched crackles heard throughout all lung fields n Phase 4: Severe Abnormalities • Severe hypoxemia unresponsive to therapy • Metabolic and respiratory acidosis • lethargy, obtunded Gomez AC: Pulmonary insufficiency in non-thoracic trauma [discussion]. J Trauma. 1968; 8: 666 15

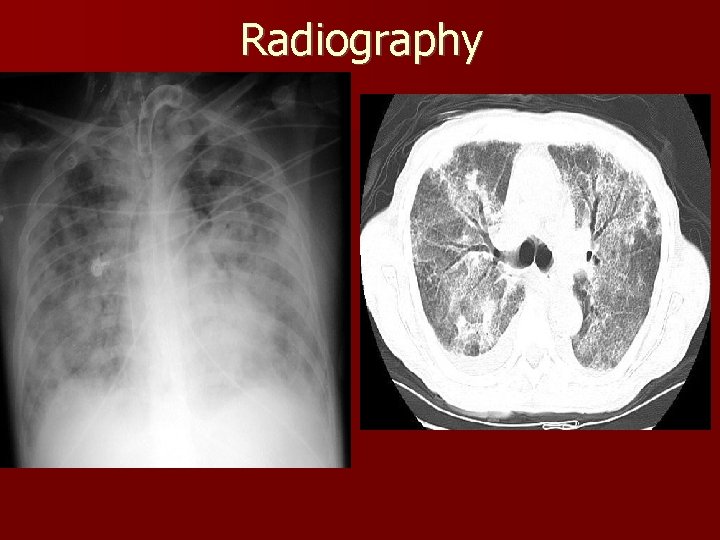
Radiography

Radiography n CT scan findings: 74 patient review – Bilateral abnormalities in almost all the patients, predominantly dependent abnormalities (86%) – Patchy abnormalities (42%) – Homogeneous abnormalities (23%) – Ground-glass attenuation (8%) – Mixed ground-glass appearance and consolidation (27%) – Basilar predominant abnormalities (68%) – Areas of consolidation with air bronchograms (89%) – Tagliabue M, Casella TC, Zincone GE, Fumagalli R, Salvini E. CT and chest radiography in the evaluation of adult respiratory distress syndrome. Acta Radiol. May 1994; 35(3): 230 -4

Clinical Risk Factors Predictive of Poor Outcomes n Independent predictors repeatedly: higher mortality rates – Severity of the illness – Non-pulmonary organ dysfunction – Comorbid diseases, Sepsis, Liver dysfunction/cirrhosis – Advanced age n Other independent risk factors: – Organ transplantation – HIV infection and Immunosuppression – Active malignancy – Mechanisms of lung injury – Barotrauma – Fio 2 (High) – Atabai K, Matthay MA. Thorax. 2000. Ware LB. Crit Care Med. 2005. Ferguson ND, et al. Crit Care Med. 2005. 18

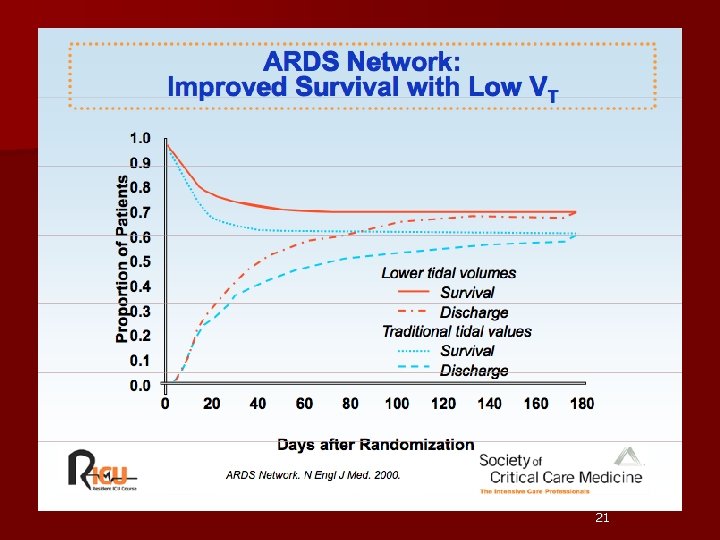
Management n In 1990, Hickling et al. : improved mortality w/ lower than “traditional” Vt n ARMA (Acute Respiratory Distress Syndrome Network Low Tidal Volume) trial: – limited Vt & plateau pressures compared to higher values § result: reduction in mortality from 40% to 31% n Considered Standard: Vt = 6– 8 m. L/kg ideal body wt & plateau pressure <30 cm H 2 O – Strategy associated with: § Pa. O 2/Fi. O 2 lower § High RR prevented hypercapnia § less organ failures § reduction in IL-6 and IL-8 levels § ~ 10% mortality reduction Hickling KG, et al. , Intensive Care Med. 1990; 16(6): 372– 377. ARDS Network. N Engl J Med. 2000. Hough CL, et al. , Critical Care Med 2005. 19

Non-Ventilatory Base Strategies n Inhaled Nitric Oxide – selectively vasodilates pulmonary capillaries – anti-inflammatory properties n Prone Positioning n Steroids: ? controversial n Further Investigations: – Liquid Ventilation – Surfactant Davis JW. et al, J Trauma. 2007 May; 62(5): 1201 -6. 20

21

Mortality n ARDS mortality rates - 31% to 74% --> 30 -58% 1990 s – Variability: difference populations studied & definitions used. – age & etiology of lung injury Main causes of death: nonrespiratory (i. e. , die w/, rather than of ARDS). n Respiratory failure cause of death: 9% to 16% of patients with ARDS. n Early deaths (within 72 hours): underlying illness or injury; n late deaths sepsis or multi-organ dysfunction. Frutos-Vivar F, et al. Curr Opin Crit Care. 2004. Vincent JL, et al. Crit Care Med. 2003. Ware LB. Crit Care Med. 2005. 6

One-year Outcomes in Survivors of ARDS Persistent functional limitation • Extrapulmonary diseases (primarily): Muscle wasting and weakness (corticosteroid-induced & critical-illness-associated myopathy), • Intrinsic pulmonary morbidity (5%): Bronchiolitis obliterans organizing pneumonia Herridge MS, et al. N Engl J Med. 2003. 18

Long term outcomes n Outcomes variable n Lung mechanics may return to normal 1 year – gas exchange abnormalities may persist n Spirometry normal at 6 months n Mild to moderate: Quality of Life n 78% patients return to work Mc. Hugh LG, et al. Recovery of function in survivors of the acute respiratory distress syndrome. Am J Respir Crit Care Med. 1994; 150: 90. Herridge MS, Cheung AM, Tansey CM, et al. One-year outcomes in survivors of the acute respiratory distress syndrome. N Engl J Med. 2003; 348: 683 24