Acute Liver Failure Dr Eduardo Martinez Foie Gras
























































- Slides: 57

Acute Liver Failure Dr. Eduardo Martinez


Foie Gras � Foie gras (pronounced /fwɑːˈɡrɑː/ in English; French for "fat liver") is a food product made of the liver of a duck or goose that has been specially fattened.

Functions of the Liver � Metabolic ◦ ◦ Carb metabolism Protein and lipoprotein metabolism Fatty acid metabolism Biotransformation of drugs � Storage ◦ Glycogen ◦ Vitamins A, D, E, and K ◦ Iron and copper

Functions of the Liver � Immunological ◦ ◦ function s Synthesis of immunoglobulins Phagocytosis by Kupffer cells Filtration of bacteria Degradation of endotoxins � Excretion of bilirubin and urea formation � Haematological functions ◦ Blood reservoir ◦ Haematopoiesis in the foetus

ALF • Syndrome that leads to MOF and death o Previously normal liver may fail within days • High grade encephalopathy, survival is <20% • Early death: o cerebral oedema, CVS collapse • Late death: o Sepsis , MOF

Definition and Classifications • ALF: Sd. defined by o Encephalopathy o Coagulopathy o Jaundice o Individual with previously normal liver

Definition and Classifications • Fulminant Hepatic Failure o Potentially reversible condition o Consequence of severe liver injury o Encephalopathy appears within 8 wks. of initial Sx. o Absence of pre-existing liver ds.

Definition and Classifications • King’s classification: o Hyperacute: encephalopathy within <7 days § Paracetamol, ischaemic, viral, toxins o Acute: 8 -28 days o Subacute: 5 -26 weeks § Seronegative, idiopathic, drug-related § Different etiology § Poorer prognosis

Etiology Cause Agent Responsible Viral Hepatitis Hep. A, B, D, E, CMV, HSV, seronegative hepatitis (14 -25% in UK) Drug-related Dose-related, e. g. paracetamol; idiosyncratic reactions, e. g. anti-TB, statins, recreational drugs, anticonvulsants, NSAIDs, many others Toxins Carbon tetrachloride, amanita phalloides Vascular events Iscahemic hepatitis, veno-occlusive disease, Budd -Chiari, heatstroke Other Pregnancy-related liver disease, Wilson’s disease, lymphoma, carcinoma, trauma

Etiology • Most common causes: o Worldwide: § Hepatotrophic viruses A-E o UK § Paracetamol overdose § Seronegative or non-A-E hepatitis § Idiosynchratic drug rxs. or Wilson’s ds.

Workup • Identify the etiology o Hx. , examination, viral and autoimmune profiles • Bloods o FBC, EUC, CMP, coags, LFTs, drug levels • Abdo USG and CT o Vascular pattern, ascitis, splenomegaly

Workup • Liver Bx. o Done by transjugular route o Mays suggest specific Dx. o Watch for sample from healthy liver o >50% necrosis assoc. with poor prognosis o Need to reverse coagulopathy before doing it

Pathophysiology • Hepatic encephalopathy o alteration in mental status and cognitive function occurring in the presence of liver failure • Liver failure leads to: o o o portal HTN splachnic vasodilation Hypoalbuminaemia Reduced plasma oncotic pressure Leads to ascitis and organ oedema

Pathophysiology • Decreased intravascular volume o Kidneys try to “compensate” and retain Na+ and water making oedema worse • Also, • Gut-derived toxins reach the liver o Ammonia levels are often high o Correlation between ammonia and symptoms is poor

Clinical Features • Depend on the severity, which depends on: o Etiology o Speed of onset of symptoms • Non-specific o N&V, abdo pain • Neurological o Confusion, agitation, coma

Scale Of Hepatic Encephalopathy Grade Level of Consciousness Personality and Intellect Neurologic Signs Electroencephalogram (EEG) Abnormalities 0 Normal None Subclini cal Normal Abnormalities only on psychometric testing None 1 Day/night sleep reversal, restlessness Forgetfulness, mild confusion, agitation, irritability Tremor, apraxia, incoordination, impaired handwriting Triphasic waves (5 Hz) 2 Lethargy, slowed responses Disorientation to time, loss of inhibition, inappropriate behavior Asterixis, dysarthria, ataxia, hypoactive reflexes Triphasic waves (5 Hz) 3 Somnolence, confusion Disorientation to place, aggressive behavior Asterixis, muscular rigidity, Babinski signs, hyperactive reflexes Triphasic waves (5 Hz) 4 Coma None Decerebration Delta/slow wave activity

Clinical Features • Mortality is higher for Grade III/IV o Mostly due to cerebral oedema o Occurs in 80% of pts. w/ALF § Due to lack of equilibration of osmotic gradient § 30% of those have cerebellar tonsil and/or temporal lobe herniation causing death o We’re now better at treating cerebral oedema

Clinical Features • Elevated ICP o HTN, bradycardia, blown pupils: occur late o CTB won’t tell you o ICP monitor is best way of knowing • CVS changes o Similar to sepsis o Might be due to infection

Clinical Features • Renal failure o Oliguric o Poor prognosis § Except with paracetamol overdose where it has a good prognosis • Impaired immunity o Decreased complement synthesis, Kupffer cell dysfunction, poor neutrophil adhesion and superoxide production

Clinical Features • Increased susceptibility to infection o 80% of pts. have bacteriologically proven infections o Major sepsis is contributor to death in 20% of cases § Staph. aureus 70% of gram (+) § E. Coli most common gram (-) § C. albicans in 30% of pts.

Monitoring • Pts. need HDU/ICU • Need CVC and continuous IBP monitoring and IDC • Baseline ABG and lactate o Lactate >3 mmo/L after adequate resus has same sensi. and speci. for death as The King’s College Hospital criteria

Prognosis • Early indicators of prognosis in fulminant hepatic failure. § O'Grady JG, Alexander GJ, Hayllar KM, Williams R. § Gastroenterology. 1989 Aug; 97(2): 439 -45. • King’s Collage Hospital Criteria Originally devised as prognostic criteria to predict patient survival without liver transplant o Now used as selection criteria for potential liver transplant recipients o


KCH Criteria • Patients with paracetamol toxicity o o o o p. H <7. 3 (7. 25 if given NAC) Or all three of the following: Prothrombin time >100 s Serum creatinine level >300 μmol/l Grade III or IVencephalopathy • Other patients o o o Prothrombin time >100 seconds or Three of the following variables: Age <10 yr or >40 yr Jaundice >7 days before encephalopathy PT > 50 s Bilirubin > 300 mmol/L

KCH Criteria � Positive predictive value for ICU death without transplantation of 0. 98 � Negative predictive value of 0. 82

Treatment • Intensive care of patients with acute liver failure: recommendations of the U. S. Acute Liver Failure Study Group. § Stravitz RT, Kramer AH, Davern T, Shaikh AO, Caldwell SH et al. § Critical Care Medicine 2007; 35: 2498 -508

Treatment • Adult U. S. Acute Liver Failure Study Group o Data from § 23 liver transplant centers § >1, 110 pts. o In 2005 convened to § review literature on management § Care of pts. w/high ICPs § Compare practices of different centers

General Management • Admit to hospital and HDU/ICU o When evidence of ALF § E. g. : INR>1. 5 o D/W: § Physician § Intensivist § Nearest transplant center § Regarding best time to refer

General Management • Etiology-specific treatment o Studies only for paracetamol overdose o NAC regardless of time of overdose § IV if Grade I encephalopathy § Hypotension § Any other reason PO NAC is not tolerated o HELLP or acute fatty liver of pregnancy § Tx. Is immediate delivery

General Management • NAC o 150 mg/kg IV in 200 ml NS over 15 -60 mins o 50 mg/kg IV over 4 hrs o 100 mg/kg IV over 16 hrs § Total dose: 300 mg/kg over 20 hrs o Infusion recommended until there is evidence of improved hepatic function rather than time or paracetamol levels

Management of Complications • Hepatic encephalopathy and hyperammonaemia • Infections • Sedation and analgesia • Bleeding diathesis • Nutrition • Seizures • Circulatory dysfunction

Encephalopathy • Standard treatment: o Lactulose § Watch for: § Abdo distension § Oesophageal varices will need a scope § Avoid intravascular depletion o Non-absorbable ATBs § Neomycin not recommended by ALFSG because of nephrotoxicity

Infection prophylaxis and surveillance • Infection is one of main causes of death in ALF • Most common sites: o o o Lung Urinary tract Blood o o o Gram (+) cocci: Staph aureus Gram (-) rods: E. coli Fungi: candida • Most common M. O.

Infection prophylaxis and surveillance • Empirical ATBs are recommended by ALFSG when: o o Surveillance cultures reveal significant isolates Advanced stage (III/IV) encephalopathy Refractory hypotension SIRS • 3 rd gen. Cephalosporin or Timentin, Vancomycin, Fluconazole

Sedation and analgesia • Agitation contributes to raised ICP • Propofol vs. Benzos Both increase GABA neurotransmission, therefore may exacerbate encephalopathy o Propofol decreases ICP and wears off quickly o • Opioids o o Shorter acting are preferable When there is concommitant ARF, avoid morphine or pethidine due to metabolite accumulation

Correction of bleeding diathesis • Pts. with ALF are by definition coagulopathic o o Low plts. and fibrinogen, Vit. K deficient Spontaneous bleeding is rare o o INR 1. 5 Plts. 50, 000 • Very difficult to obtain complete correction • ALFSG recommends aiming for:

Correction of bleeding diathesis • Prophylactic FFP not recommended o Obscures the trend of PT as prognostic marker o o Should be given before planned procedures Avoid in patients with risk of thrombotic complication • Cryo recommended when fibrinogen low • When FFP fails to correct PT/INR, then recombinant factor VIIa can be given § MI, DVTs, etc.

Correction of bleeding diathesis • UGI bleeding o reduced by H 2 antagonists or PPIs • TEDS and Scuds

Nutrition • ALF is a catabolic state o Negative nitrogen balance o Immunodeficiency • Enteral nutrition when possible o Hi-cal o Avoid free water and hypo-osmolarity • TPN when: o Specific contraindication for enteral feeds

Seizure Prophylaxis and Surveillance • Nonconvulsive seizure activity is common o o Prophylactic antiepileptics not recommended EEG when: § § Grade II/IV encephalopathy Sudden neuro deterioration Myoclonus To titrate use of barbiturates • Tx. o o Phenytoin Propofol, midaz, barbiturates

CVS Dysfunction • Correct hypovolaemia before starting vasopressors • Pressors needed for hypotension and low CPP o o o Norad is first line, can give high dose dopamine Adrenaline may compromise HBF Vasopressin not recommended because directly causes cerebral vasodilation and high ICPs • Medium doses of steroid may improve pressor response

Mx. of Cerebral Oedema and Intracranial Hypertension • Raised ICP due to cerebral oedema is one of major causes of M&M • CTB for Grade III/IV o To rule out anything else, i. e. bleed • ICP monitor o Grade III/IV encephalopathy o To optimize CPP o Not routine

Raised ICP • Aim for o ICP<25 mm. Hg o CPP 50 -80 • General recommendations o Keep it quiet , minimize chest physio and ETT suctioning, head at 30 o o Don’t treat spontaneous hyperventilation, keep Pa. CO 2 35 -40 mm. Hg, treat fever aggressively with physical measures

Raised ICP • Specific management o Manitol: first line therapy o Hypertonic Saline o Induced hypothermia o Barbiturate coma o Indomethacin: 25 mg IV over 1 min.

Mechanical Ventilation • When to intubate: o Respiratory failure o Airway protection in advanced encephalopathy o Agitation o Imminent ICP monitor placement

Mechanical Ventilation • Pts. w/ALF often develop ALI/ARDS o Follow ARDSNet protocol o Avoid high PEEP § Use the minimum needed

CRRT • Indicated for: o Renal failure o Fluid overload o Metabolic derangements o Need to create space for IV colloids, i. e. FFP • CRRT preferred over IRRT o HD instability common

CRRT • Use citrate over heparin o Monitor ionized calcium • Use bicarb buffer over lactate or citrate buffer o Liver won’t be able to convert them to HCO 3 - • Avoid hyponatraemia o May exacerbate cerebral oedema

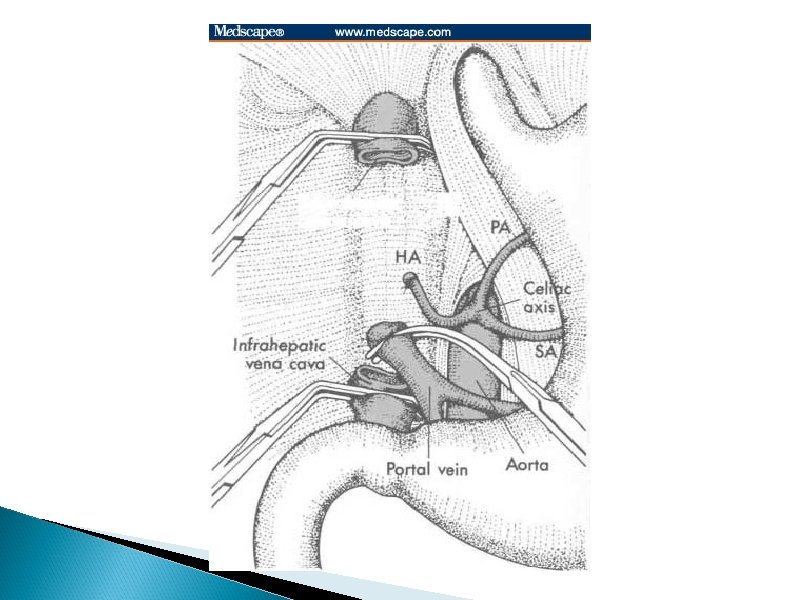
Liver Transplant � Orthotopic liver transplant is the definitive treatment for patients who meet the criteria ◦ or·tho·top·ic (ôrth-tpk)adj. In the normal or usual position � 1 yr. and 5 yr. survival of patients undergoing OLT for ALF is about 20% lower than elective cases for cirrhotic patients � Auxiliary liver transplantation is and alternative

Liver Transplant � Absolute ◦ ◦ contraindications Overwhelming sepsis Refractory hypotension AIDS Uncontrolled raised ICP with likely permanent damange


Hepatic assist devices � MARS: molecular absorption and recirculation system ◦ Adaptation of haemodialysis ◦ Blood is dialysed against 20% albumin �Shown to improve encephalopathy, renal function and haemodynamic parameters ◦ The efficacy of this technique has not yet been studied


So, what have we learned?


Thank you!