ACUTE KIDNEY INJURY Role of Novel Biomarkers R

ACUTE KIDNEY INJURY Role of Novel Biomarkers R Bhimma Department of Paediatrics and Child Health Nelson R Mandela School of Medicine University of Kwa. Zulu-Natal
Definition of AKI Sudden impairment of kidney function occurring over a period of hours to days. Diagnosis Increase serum creatinine and/or blood urea nitrogen levels and/or decrease urine output

Why is it important to detect AKI early? u A rise in serum creatinine of just 0. 3 mg/dl (26. 5 mmol/l) has a four fold higher multivariable – adjusted risk of death. u Children with AKI may be at risk for long-term chronic kidney disease.
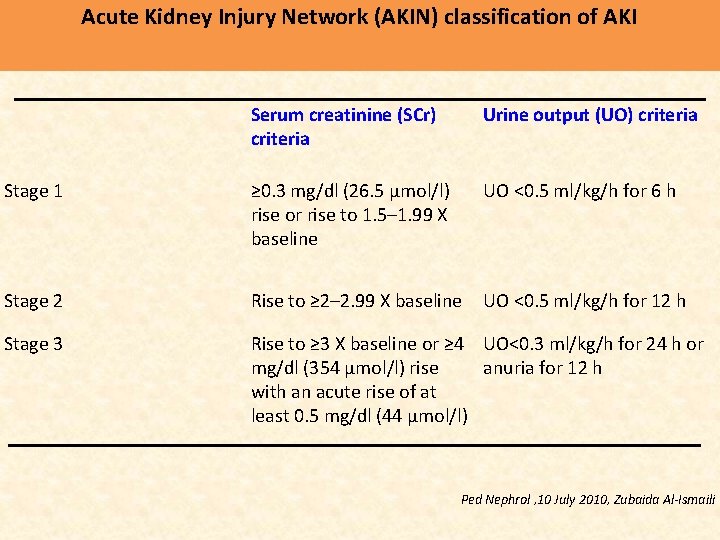
Acute Kidney Injury Network (AKIN) classification of AKI Serum creatinine (SCr) criteria Urine output (UO) criteria Stage 1 ≥ 0. 3 mg/dl (26. 5 μmol/l) rise or rise to 1. 5– 1. 99 X baseline UO <0. 5 ml/kg/h for 6 h Stage 2 Rise to ≥ 2– 2. 99 X baseline UO <0. 5 ml/kg/h for 12 h Stage 3 Rise to ≥ 3 X baseline or ≥ 4 UO<0. 3 ml/kg/h for 24 h or mg/dl (354 μmol/l) rise anuria for 12 h with an acute rise of at least 0. 5 mg/dl (44 μmol/l) Ped Nephrol , 10 July 2010, Zubaida Al-Ismaili
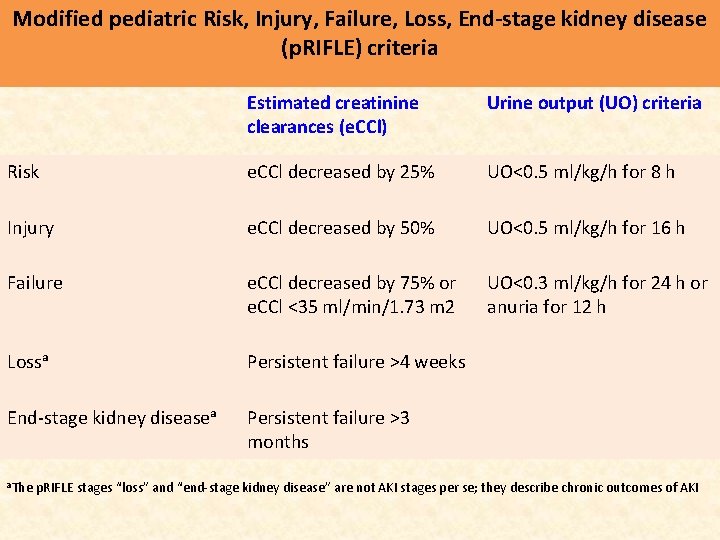
Modified pediatric Risk, Injury, Failure, Loss, End-stage kidney disease (p. RIFLE) criteria Estimated creatinine clearances (e. CCl) Urine output (UO) criteria Risk e. CCl decreased by 25% UO<0. 5 ml/kg/h for 8 h Injury e. CCl decreased by 50% UO<0. 5 ml/kg/h for 16 h Failure e. CCl decreased by 75% or e. CCl <35 ml/min/1. 73 m 2 UO<0. 3 ml/kg/h for 24 h or anuria for 12 h Lossᵃ Persistent failure >4 weeks End-stage kidney diseaseᵃ Persistent failure >3 months a. The p. RIFLE stages “loss” and “end-stage kidney disease” are not AKI stages per se; they describe chronic outcomes of AKI

Limitations of serum creatinine and BUN Change extracellular volume depletion decreased kidney blood flow Influenced by other factors, which are not directly related to kidney damage, such as: u age u sex u body mass u nutritional status

Limitations of Serum creatinine and BUN u cont… Elevated serum creatinine concentrations are not specific for AKI and require differentiation from other pre-renal or extra-renal causes. u Serum creatinine concentrations are not specific for renal tubular lesions, pathogenetically related to AKI development. u Reflect the loss of glomerular filtration function, accompanying the development of AKI.

Limitations of serum creatinine and BUN u cont… Increases in serum creatinine are detected later than the actual GFR changes as creatinine accumulates over time. u Serum creatinine is a poor marker of kidney dysfunction as changes in its concentrations are neither sensitive nor specific in response to slight GFR alterations. u Changes in serum creatinine become apparent only when the kidneys have lost ≥ 50% of their functional capacity.

What is a biomarker? “ a characteristics that is objectively measured and evaluated as an indicator of normal biological process, pathogenic process, or pharmacologic response to a therapeutic intervention”. Test Biomarker Height Growth Urinary dipsticks for nitrites UTI Proteinuria Disease severity in Ig. A nephropathy. Anti-GBM Ab Good pastures syndrome

Ideal Biomarker AKI u Non – invasive u Easily obtainable u Measurable using standardized assays u Fast results u Incur reasonable cost to perform

Possible roles for novel kidney injury biomarkers Ismaili Z Al et al Ped Nephrol , 2010
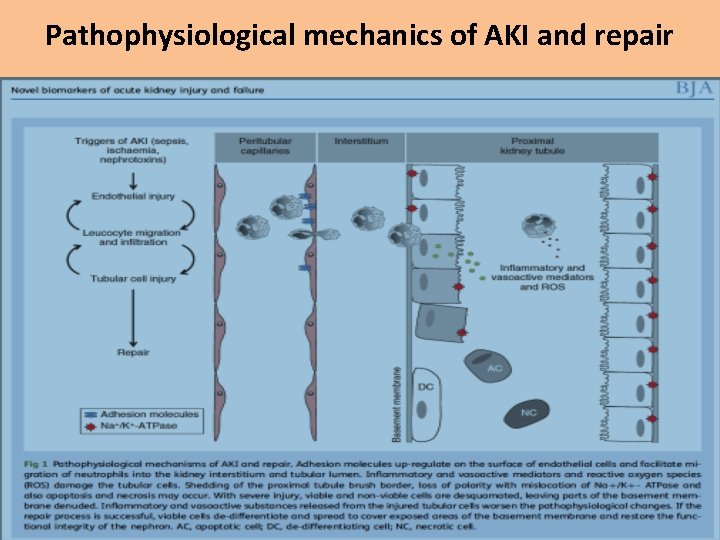
Pathophysiological mechanics of AKI and repair
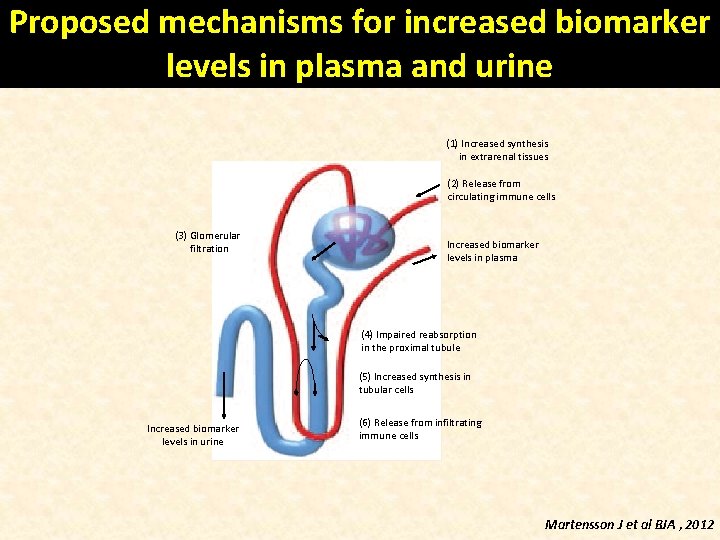
Proposed mechanisms for increased biomarker levels in plasma and urine (1) Increased synthesis in extrarenal tissues (2) Release from circulating immune cells (3) Glomerular filtration Increased biomarker levels in plasma (4) Impaired reabsorption in the proximal tubule (5) Increased synthesis in tubular cells Increased biomarker levels in urine (6) Release from infiltrating immune cells Martensson J et al BJA , 2012

Proposed phase of biomarker development Goals Phase Biomarker aims Discovery phase Phase 1 • • Translational phase Phase 2 • Evaluate diagnostic accuracy • Assess the ability to distinguish AKI from non-AKI Phase 3 • • Validation phase Identify leads for AKI biomarker. Prioritize identified leads Evaluate the capacity of the biomarker to detect preclinical AKI or other AKI characteristic (e. g. severity, prognosis) Define criteria for a positive screening test (e. g. cutoff) Phase 4 • Determine the operating characteristics of the biomarker-based screening test in a relevant population by determining the detection rate and the false referral rate (prospective study) Phase 5 • To estimate the reduction in AKI morbidity and mortality afforded by the screening test (effects on population) Coca SG, et al (2008) Urinary biomarkers for acute kidney injury: perspectives on translation. Clin J Am Soc Nephrol 3: 481– 490, Pepe MS, et al. (2001) Phases of biomarker development for early detection of cancer. J Natl Cancer Inst 93: 1054– 1061

Summary of calculating diagnostic characteristics: sensitivity, specificity, positive predictive value, and negative predicative value. Disease present Disease not present Biomarker test positive True positive (TP) False positive (FP) TP+FP=total with positive test Biomarker test negative False negative (FN) True negative (TN) FN+TN=total with negative test TP+FN=total with disease FP+TN=total with no disease How to calculate diagnostic characteristics Sensitivity TP/(TP+FN): TP/total with disease Specificity TN/(TN+FP): TN/total without disease Positive predictive value (PPV) TP/(TP+FP): TP/total with positive test Probability of actually having the disease when test is positive Negative predictive value (NPV) TN/(TN+FN): TN/total with negative test Probability of not having the disease when test is negative Ismaili Z Al et al Ped Nephrol , 10 July 2010,
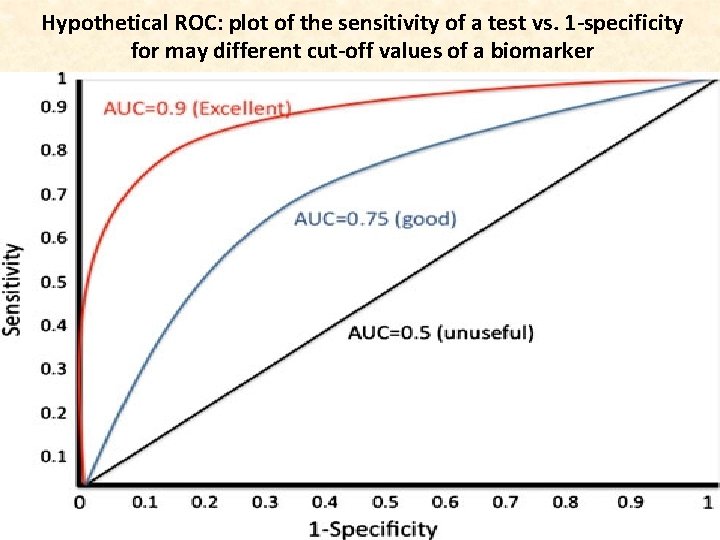
Hypothetical ROC: plot of the sensitivity of a test vs. 1 -specificity for may different cut-off values of a biomarker

Kidney Biomarkers v > 20 protein biomarkers have been intensively studied. v Urinary biomarkers are regarded as more non invasive, easy to measure, easily obtainable and provide earlier detection of AKI. v Depending on the time of appearance after AKI, urinary biomarkers many be classified as those of structural injury or functional injury.

Biomarkers of structural injury Type of biomarkers Selective sites and associated types of injury Kidney injury molecule-1 (KIM-1)* Proximal tubule injury (Ischemic AKI, nephrotoxins, RCC) n-acetyl glucosaminadase (NAG) Proximal tubule injury Neutrophil gelatinase-associated lipocalin (NGAL)* Tubule and collecting duct injury (Ischemic AKI, nephrotoxins, delay allograft renal function) Interleukin (IL)-18* Tubule injury (AKI, delayed allograft renal function) Clusterin Tubule injury

Biomarkers of functional injury Cystatin C* Glomerular injury; in urine indicates proximal tubule injury Total protein β 2 -microglobulin albumin Glomerular and tubular dysfunction Brush border antigens Adenosine deaminase binding protein Carbonic anhydrase Proximal tubule injury Other tubular antigens Urinary enzymes N-acetyl-β-D-glucosaminidase Alanine aminopeptidase Cathepsin B Proximal tubule injury γ-glutamyltransferase α-glutathione-S-transferase β-glucosidase Proximal tubule > distal tubule injury Alkaline phosphatase Lactate dehydrogenase Distal tubule > proximal tubule injury

Others Type IV Collagen Glomerular injury Gamma-glutamyl transferase (γ-GT) Liver type fatty acid binding protein (L- Tubular epithelium injury FABP) Retinol binding protein 4 (RBP 4) Sodium/hydrogen exchanger isoform Alpha-glutathione S-transferase (αGST) Proximal tubule injury Exosomal fetuin-A Tamm-horsfall glycoprotein pi-glutathione S-transferase (π-GST) Distal tubule injury
Neutrophil gelatinase – associated lipocalin (NGAL) v 25–k. Da polypeptide covalently bound to gelatinase secreted from activated human neutrophils. v Most consistent biomarkers found during AKI. v Predominantly found in proliferating nuclear antigen– positive proximal tubule cells. v Predicts the occurrence of AKI in paediatric and adult patients after cardiac surgery. Cont…

Neutrophil gelatinase – associated lipocalin (NGAL) v AUC- ROC for NGAL is 0, 92 at 2 hours and 1, 00 at 4 hours CBP. v Also predicts mobility and mortality in children who undergo cardiac surgery. v Also predicts development of DGF.

Kidney Injury Molecule-1 (KIM-1) v Orphan trans-membrane receptor of unknown function. v Undetectable in normal kidney tissue or urine. v Markedly increased in ischaemic and nephrotoxic proximal tubular cell injury, and in renal cell carcinoma. v Higher urinary KIM-1 associated with worse outcome in established AKI. Cont… W. K. Han et al Advances in Clinical Chemistry, Vol. 49, 2009, pp. 73 -97.

Kidney Injury Molecule-1 (KIM-1) v AUC – ROC 0, 57 at 2 hours, 0, 83 at 12 hours, and 0, 78 at 24 hours after cardiac surgery. v Also predicts graft loss in renal transplant patients. v Useful in some studies to differentiate between AKI, CKD and normal patients. W. K. Han et al Advances in Clinical Chemistry, Vol. 49, 2009, pp. 73 -97.

Interleukin (IL) -18 v Pro-inflammatory cytokine v Mediates inflammatory process during ischaemic, sepsis and nephrotic AKI. v Recruits neutrophils during ischaemic injury. v Can predict AKI 1 day ahead of serum creatinine. Cont…

Interleukin (IL) -18 v AUC – ROC 0. 73 for development of AKI in patients with acute respiratory distress syndrome. v Independent predictor of mortality in the above group of patients. v Also elevated after CPB --- ROC- AUC 0. 61 at 4 hours, 0. 75 at 12 hours and 0. 73 at 24 hours.

Cystatin C v 13 k. Da cysteine protease inhibitor. v Secreted by all nucleated cells into plasma. v Freely filtered at the glomerulus and not secreted in the tubules. v Less influenced by factors other than GFR (e. g. age, sex, race, or muscle mass). v Therefore change in serum and urinary cystatin C is more sensitive than a change in serum Cr in predicting change in GFR. Cont…

Cystatin C v Predicts the risk of AKI-associated CV morbidity. v Levels > 1. 0 mg/L also predict CV events and mortality in patients with a GFR >60 mls/min/1. 73 m². v Increase urinary cystatin C and alpha 1 - microglobulin are predictors of an unfavourable outcome in ATN. v Has higher sensitivity and higher negative predictive value in determining GFR in CKD.

Proposed Biomarker strategies for Renal Replacement Therapy (RRT)- initiation in AKI. u Some studies have shown better renal outcomes in patients who start RRT while in RIFLE-risk or injury compared to failure. u However some patients may recover spontaneously. u Biomarkers like NGAL, cystatin C, NAG, KIM-1 and alpha 1 microglobulin can help distinguish patients in whom RRT will be needed.

Proposed biomarkers – based strategy for RRT BM indicates RRT necessary Consider initiating RRT Severe AKI (AKIN stage 3) AKI present Measure BM BM Intermediate MILD/ MODERATE AKI (Akin stage 1 -2) BM indicate RRT Unlikely Conservative treatment

Conclusion u Need a ‘panel’ of biomarkers making it possible for early detection, treatment, and hopefully, preventing AKI. u As cardiology moved form LDH to troponins for the diagnosis of MI, intensive care nephrology will hopefully evolve from serum Cr to tissue specific injury biomarkers.



- Slides: 34