Acute Kidney Injury Generic programme Dr Begho Obale

Acute Kidney Injury Generic programme Dr Begho Obale Associate Specialist Acute medicine

1) Basic Functioning of the kidney
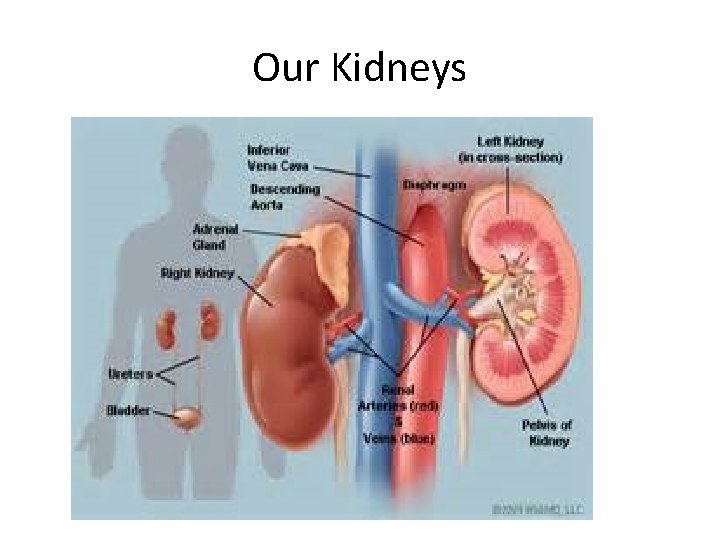
Our Kidneys

Basic anatomy and physiology • Anatomy- 2 kidneys, measure 10 -14 cm in length, 5 -6 cm in width and 3 -4 cm in depth • Found at the back of the abdomen(retroperitoneal)on either side of the vertebral column at level T 12 -L 3 • 1300 ml of blood which is 25% of the blood volume flows through the kidneys each minute • The kidneys are made up of over a million nephrons each that carry out the functions of the kidneys of filtration, getting rid of wastes, toxins, excess water and acids etc. • The kidney absorbs about 99. 9% of all the glucose passing through it. Blood and protein molecules are large and hence not excreted in the urine except if there is inflammation or damage to the kidneys
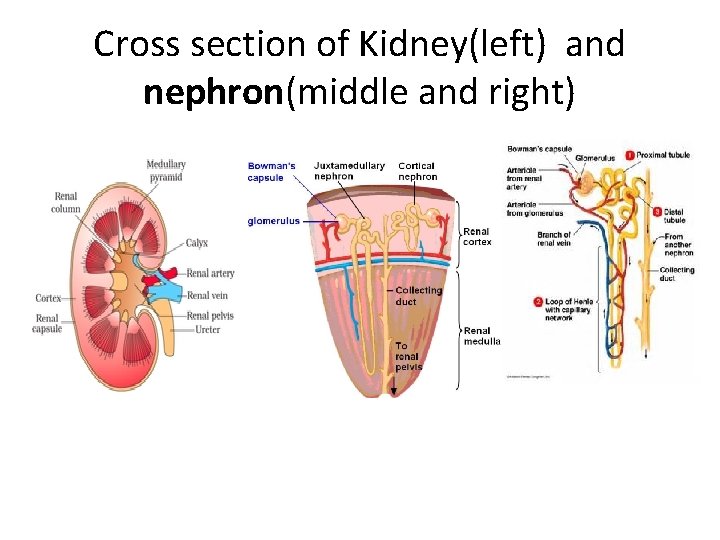
Cross section of Kidney(left) and nephron(middle and right)
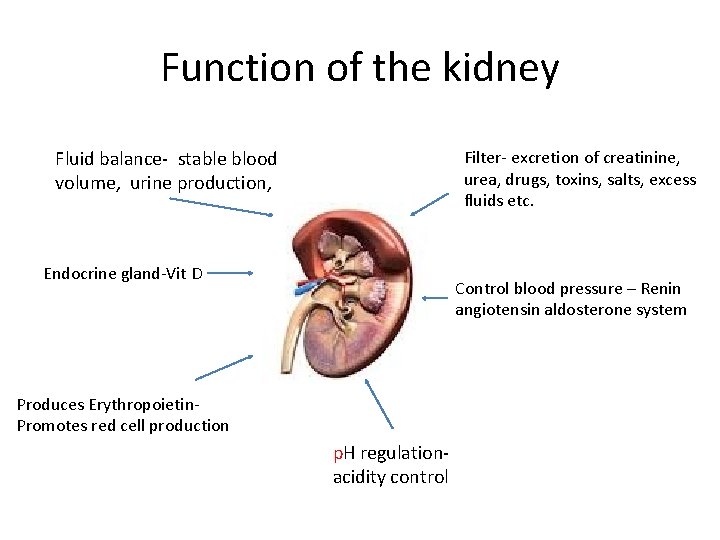
Function of the kidney Fluid balance- stable blood volume, urine production, Filter- excretion of creatinine, urea, drugs, toxins, salts, excess fluids etc. Endocrine gland-Vit D Control blood pressure – Renin angiotensin aldosterone system Produces Erythropoietin. Promotes red cell production p. H regulationacidity control

2. What is Acute Kidney Injury( AKI)

What is Acute Kidney Injury? • Rapid/sudden deterioration in kidney function over a few hours to days in an unwell patient • Resulting in a failure to excrete wastes, salts toxins, acids, excess fluids • Commonest causes of AKI : Hypovolaemia (Includes dehydration) and Sepsis

Hypovolaemia-is Reduced blood volume • Common Causes: § Dehydration- not eating/drinking , excess loss e. g. vomiting, diarrhoea( D/V), diuretics (water tablets) § Sepsis, severe infection § Bleeding- haematemesis, maleana, etc § Hypotension- low blood pressure< 100 mmhg § Reduced cardiac output; Heart failure, Myocardial infarction (MI)(heart attack), Cardiac arrhythmia § Drugs such as Ibuprofen, Ramipril, Losartan, (NSAID, ACE-I, ARB 2) affect blood vessels in the glomerulus reducing blood supply in the nephron (kidney)

Acute Kidney Injury is defined as: • Increase in Serum Creatinine of 26 mmol/l within 48 hours Or • An increase in Serum Creatinine of >/=1. 5 x above base line value within 1 week, Or • Urine Output of <0. 5 ml/kg/h for over 6 hours (oliguria)

Acute Kidney Injury (AKI) • The earliest sign of eminent AKI is reduced urine output, (identified within 2 hours) • AKI is easily reversible if identified early • Older patients can have a delay of up to 48 hours to show a significant deterioration in blood test results e. g increased creatinine

AKI the Facts • • 1: 5 of all acute or emergency admissions 500, 000 patients a year in UK suffer from AKI 1042 pts diagnosed with AKI 07/2015 - MBHT All patients groups affected, especially elderly AKI 100 x more dangerous than MRSA AKI cost the NHS over £ 1 billion/year, Post discharge cost of £ 179 million/year

AKI THE FACTS AKI inpatient mortality of 25 -30% 100, 000 AKI related inpatients deaths /year About 30% of these deaths could be prevented Early recognition, identification of risks and early treatment, could save 12, 000 - 40, 000 lives/y and over £ 150 m/y • Patients may not recover fully- develop chronic Kidney disease (CKD), needing dialysis • 40% of AKI starts newly in hospitalised patient • Prolong hospital stay up to x 2 longer(10 vs 4 days • •
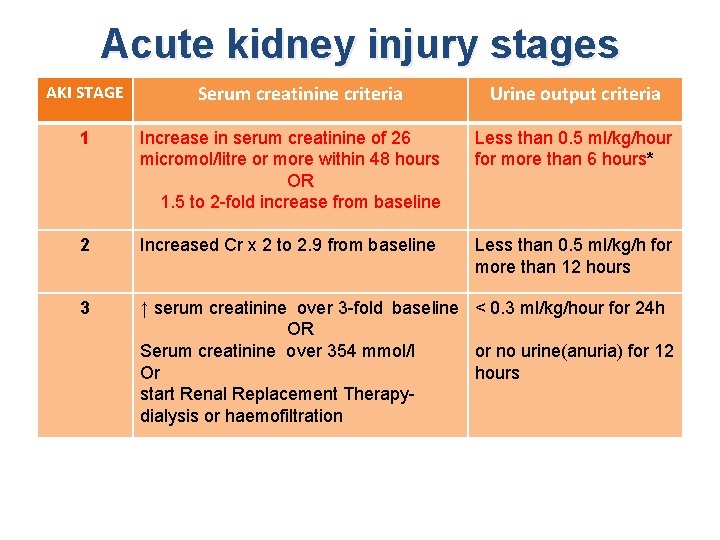
Acute kidney injury stages AKI STAGE Serum creatinine criteria Urine output criteria 1 Increase in serum creatinine of 26 micromol/litre or more within 48 hours OR 1. 5 to 2 -fold increase from baseline Less than 0. 5 ml/kg/hour for more than 6 hours* 2 Increased Cr x 2 to 2. 9 from baseline Less than 0. 5 ml/kg/h for more than 12 hours 3 ↑ serum creatinine over 3 -fold baseline < 0. 3 ml/kg/hour for 24 h OR Serum creatinine over 354 mmol/l or no urine(anuria) for 12 Or hours start Renal Replacement Therapydialysis or haemofiltration

AKI stages related to mortality • Stage 1: <10% mortality– commonest stage(50% or more) urine output<0. 5 ml/kg/h over 6 hours • Stage 2: 20 -30% mortality, urine <0. 5 ml/kg/h over 12 h • Stage 3: 30 -50% mortality Urine<0. 3 ml/kg/h x 24 h or no urine x 12 h

3. Identify Patients at risk of AKI

Identifying patients with risks for AKI • • Elderly patients over 65 years of age Chronic kidney disease CKD( [e. GFR<60] Liver Disease, Diabetes, Past History of AKI Recent use of Nephrotoxins: § § § NSAID-e. g ibuprofen, ACE-I e. g ramipril, ARB e. g losartan. Spironolactone, Metformin, Iodinated contrast Aminoglycosides, eg gentamicin • Cardiovascular disease e. g Heart attack (MI), stroke, peripheral vascular disease, heart failure

Patients at risk of AKI due to illness Oliguria urine output less than 0. 5 ml/kg /hr Dehydration, bleeding, diarrhoea and vomiting (D/V) High/deteriorating early warning scores EWS >/= 3 Infection or sepsis Fall, prolonged stay on floor-toxins from muscle crush toxic to kidneys- Rhabdomyolysis • Urinary obstruction • Emergency surgery especially intra-abdominal • Cognitive or neurological impairment that limits access to fluids- dehydration e. g dementia, stroke • • •


Causes of AKI by region and how common • Pre-renal-Due to reduced blood supply to the kidney (Hypovolaemia) due to dehydration, D/V, drugs, sepsis, bleeding, cardiac problems, hypotension, etc. 80% • Renal –Damage to Kidney by; infection/inflammation e. g nephritis, vasculitis. Hypoxia due to prolonged hypovoleamia, Drugs toxic to kidneys such as Gentamicin, NSAID e. g ibuprofen, iodinated contrast. Toxins, Rhabdomyolysis etc. 10%-15% • Post renal- Kidney stones, obstructed ureters, urethral obstruction, prostate problems 5%

Nephrotoxic drugs- recent use – account for 10%-20% of all AKI § NSAID-e. g ibuprofen, voltarol § ACE-I e. g ramipril, ARB e. g losartan. § Spironolactone, § Metformin, § Iodinated contrast § Aminoglycosides, eg gentamycin § Some herbal remedies Causes renal damage especially if some associated causes of hypovolaemia or new increased drug dose Damage to the kidney by hypovolaemia or toxicity to kidney Advisable to stop drug as likely to make AKI worse

4. Presentation of AKI( symptoms and signs)

AKI Presentation- Symptoms • Most patients have No Complaints/ nonspecific symptoms • Reduction in the amount of urine passed • Concentrated urine, deep yellow, brown etc • Dehydration or thirst • Nausea, vomiting • Abdominal pains and feeling generally unwell. • Confusion and drowsiness

AKI Presentations- clinical signs • There may be NO clinical signs initially • Lower abdominal fullness and tenderness e. g urinary obstruction • Pallor- Anaemia e. g gastrointestinal bleeding Maleana, Haematemesis • Features of infection- fever, pneumonia, Urinary tract infection (UTI), cellulitis etc. • Haemoptysis, haematuria, vasculitis rashrenal AKI causes

AKI signs- Features of hypovolaemia; • Dry Mucous membranes • Loss of skin turgor (elasticity) • Tachycardia HR>90 b/min, BP<100 mmhg, postural drop of 20 mmhg with increase in RR • Respiratory rate(RR) >20/min • Prolonged capillary refill time(CRT) >2 s • Cold sweaty peripheries • Urine output < 0. 5 ml/kg/h

Effects of hypovolaemia • Reduced cardiac output- tachycardia, ↓BP • Vasoconstriction- results in cool clammy skin, pallor and poor Capillary refill time (CRT)>2 s • ↓kidney perfusion- oliguria, ↑; acidosis, K, Cr • Tissue hypoxia- ↑ Lactic acid production, metabolic acidosis, raised respiratory rate( RR) • Reduced cerebral perfusion-confusion restless or unresponsiveness

5. Assessing Urine Output

HCSW/Nurses role in Assessing Urine output Find out when patient last made urine Calculate how many hours ago Weigh patient, (daily weights) Collect urine Calculate ml/kg/hr (Person weighing 60 kg should make 60 x 0. 5 ml= 30 ml/hour of urine) • Urine output less than (<) 0. 5 ml/kg/hr indicate oliguria and high risk of AKI or established AKI • • •

Case 1 • Mr J, 70 yr old man, presented with D/V of 3 days duration, urine dark in colour, last made urine at 6 am, 6 hours ago, Pt weighs 80 kg • Produced 150 ml of urine on admission • What is his expected urine output? • Is this output adequate? • What will you do about this situation?

Case 1 answer • Weight 80 kg • Urine output/hr = 40 ml ( 80 x 0. 5=50% of weight) • Urine output in 6 h will be 40 x 6 = 240 ml • 150 ml of urine is inadequate, <0. 5 ml/kg/h • Inform Doctor as patient may need IV fluid • Open fluid input/output chart • Offer patient water if able to tolerate it

Low urine output • Can indicate Dehydration or hypovolaemia • A drop in systolic BP of >40 mmhg will reduce blood supply and oxygen to the kidney and reduce urine production, if prolonged>6 h damage to kidney • Damage to the kidney e. g nephrotoxic drugs • Urinary obstruction- consider bladder scan • Assess EWS, if >3 discuss with doctor, increase monitoring of vital signs • Fluid balance chart- hydration, aim for urine output of >0. 5 ml/kg/h

Fluid output • • Urine output- cardboard bottles /liners Urinary Catheter hourly volumes Fluid loss from diarrhoea, vomiting Ileostomy and colostomy output Loss from wound drains, weeping wounds etc Weigh wet beddings/pads 1000 g extra= 1000 ml Insensible loss from breathing and sweating 4001000 ml ( Add 500 ml on current fluid balance)

Patients needing input/output charts Raised EWS Receiving IV fluid treatment Patients treated for Sepsis or hypovolaemia Pre/Post surgical and post contrast procedures Patients with swallowing difficulties e. g NBM Increased fluid loss ie: stoma, vomiting, diarrhoea, drains • Patients at ↑risk of AKI or with diagnosed AKI • • •


Fluid input • Oral intake of fluids- measure of fluid taken in and not just amount offered • Intravenous fluids administered • Intravenous fluid volume in i. v Medication • Nasogastric feeds volume • Daily fluid requirement 25 -30 ml/kg/24 h works at 1. 5 -2. 5 l/ day (maintenance fluid) 70 kg person needs about 2100 ml/day( 70 x 30 ml) (use 25 ml/kg for elderly 70 kg patient = 1, 750 ml) • Patients will need more if excess loss e. g D/V etc.
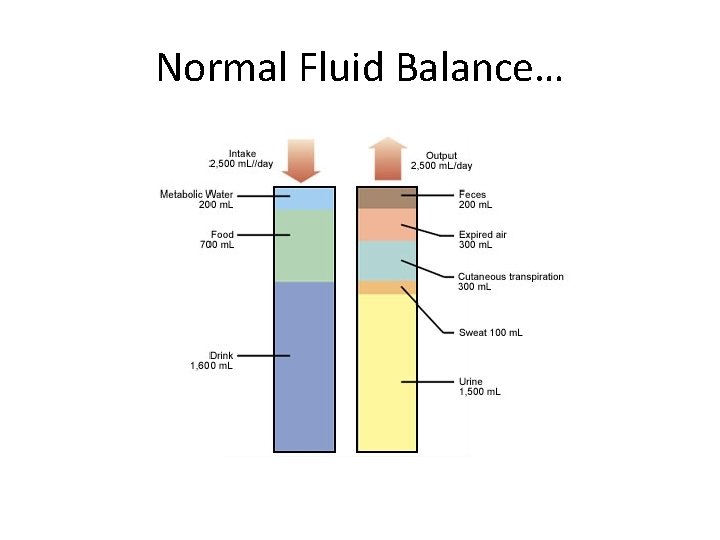
Normal Fluid Balance…

6. Urinalysis and other Investigations for AKI

Urinalysis • Blood and protein in the urine without nitrites indicates kidney inflammation or damage • Absence of nitrites make urinary infection unlikely • Send sample for microscopy culture and sensitivity • If >/= 2+ protein, send sample for protein creatinine ratio • Record all urinalysis report in patients notes • Inform nurse or doctor of abnormal urine result

Investigations for AKI Renal Function- U&E Venous gases, Bicarbonate (HCO 3), Full blood count(FBC) Infection screen-CRP, ESR, Lactate, culturesblood, urine • Bone profile • Liver function test (LFT), INR, Glucose • Creatinine Kinase (CK)- if falls- Rhabdomyolysis • •

Investigations 2 • ECG- MI, changes for hyperkalaemia • CXR- to check infection or pulmonary oedema • USS within 6 h if acute obstruction and sepsis Pyonephrosis. • USS within 12 -24 h if obstruction/ cause of AKI unknown or non resolving AKI 3

7. Management

Case 2 • Jack 75 y old man presented to A/E with fever and coughing green sputum for 4 days , not eating or drinking • He feels tired, lethargic and lightheaded, reduced urine output, dark urine • PMH; Hypertension, Diabetes, arthritis, • Drug Hx; Been taking Ramipril 10 mg, Metformin 1 g bd, Simvastatin 40 mg od , Amlodipine 10 mg, Aspirin, OTC-over the counter Ibuprofen and paracetamol

Case 2 cont • o/e dehydrated, dry mucus membranes, loss of skin turgor , BP 100/55 mmhg, 80/45 standing. Pulse 108/min, CRT 3 s, Bladder not distended, T 38⁰ C, Resp. RR 22/min, Rt lung creps, Oxy sat 96% air, weight 70 kg, 300 ml urine in 12 hr • Investigations; Creatinine 400 mmol/l(baseline 80 mmol/l 7 weeks ago) Urea 20 mmol/l, K 4. 9 mmol/l, FBC normal, Urinalysis protein + blood +, no nitrite • What are risk factors in this patient for AKI? What is the Minimum acceptable urine output/h, ? EWS , AKI stage? what will you do?

Answers to Case 2 - risks and stage • • • Patients age Dehydration /hypovolaemia, hypotension Chest infection/ sepsis, Diabetes, Blood and protein in urine Nephrotoxic drugs-ramipril, metformin, ibuprofen Reduced urine output 300 ml, <0. 5 ml/kg/h B) Expected minimum urine output is 420 ml in 12 hours C) EWS>3, D) AKI Stage 3 due to sepsis Management- awareness patient is critically ill and at risk of complications of AKI

Answer to Case 2 -management • Intravenous cannula and take bloods for-Blood culture, bicarbonate and lactate , glucose • Request a CXR • I. V bolus of balanced crystalloid 500 ml and reassess EWS, checking for improvement of EWS and hypovolaemia • Request input from Dr in charge, use SBAR as patient likely to need i. v antibiotics and more i. v fluid boluses • Stop nephrotoxic drugs- Ramipril, metformin and ibuprofen • Withhold amlodipine as hypotensive

Answer to Case 2 -management • Record urinalysis results in notes, request culture, inform doctor or nurse • (Send urine for legionella + pneumococcal antigen, - severe pneumonia) • Consider catheterization as patient very unwell & AKI 3 • Hourly monitoring of vital signs EWS >6 • 1 -2 hourly monitoring of urine output as AKI 3 • Repeat E&U and bicarbonate in 6 hours

9 - Complications of AKI

Complications of AKI • • • Metabolic acidosis Fluid overload, pulmonary oedema Hyperkalaemia Uraemic pericarditis Uraemic encephalitis Dialysis or haemofiltration if these do not respond to standard treatment

Consequences of persistent oliguria 1 Complications of AKI Deterioration in renal function- damage to kidney Deterioration in AKI stage progressing from 1 to 2 to 3 Increased risk of death Complications of AKI commoner in AKI 2/3 Accumulation of toxins e. g creatinine and urea Increase creatinine will cause increased stage of AKI, irritability, drowsy, confused • Ureamia- vomiting. Also causes irritation of heart muscle-pericarditis which gives chest pain, worse on lying flat. Irritation to brain-encephalopathy causing confusion, disorientation, fits or coma • • •

Consequences of persistent oliguria 2 Complications of AKI • Inability to excrete excess salts such as potassium with accumulation- Hyperkalaemia leads to abnormal heart rhythm and can cause a cardiac arrest • Inability to excrete excess fluids- leads to fluid overload - increased weight, and fluid in the lungs- Pulmonary oedema, causing increased shortness of breath, cough with frothy phlegm, inability to lie flat • Inability to excrete excess acid causes metabolic acidosis- increased respiratory rate, vomiting, confusion, hypotension, abnormal heart rhythm

10. Role of Clinical support workers and Nurses in Management of AKI

HCSW play a vital role in management of AKI • Identifying patients at risk of AKI • Analysing urinalysis in managing AKI • Assessing urine output and identifying patients with or at risk of AKI if urine output < 0. 5 ml/kg/h • Fluid balance- input/output interpretation • Informing nurse or doctor of abnormal urinalysis or urine output <0. 5 ml/kg/h results • Patient hydration • Preventing inpatient AKI • Reducing hospital stay and patient mortality

Nurses role in improving AKI care Covers all the roles of the HCSW and also; Early recognition of acutely unwell patients, EWS monitoring and taking appropriate action Understanding stage of AKI on e-alert and responding appropriately with monitoring, management and doctor input • Taking action if urine output <0. 5 ml/kg/h and discussion with doctors • Withholding nephrotoxic medications and discussing with medical team • •

HCSW/Nurses role in patient education • Patient education on importance of hydration and monitoring of urine output as an important aspect of their care. • Patient information-consider ideas when discussing with patient; • - Acute illness such as sepsis, dehydration, or low blood pressure can prevent the kidneys from working effectively to rid the body of wastes and toxins(AKI )this can happen within hours or days • AKI can be identified by reduced urine output within hours

HCSW/Nurses role in patient education 2 • AKI slows the response to treatment and a longer hospitalisation • AKI is easily reversible by treating cause, ensuring good hydration evidenced by adequate urine output >0. 5 ml/kg/h e. g 30 ml/h in 60 kg person • Good hydration and good urine output helps protect the kidneys, reverses AKI, better response to treatment, reduces duration of hospitalisation and better patient outcome

HCSW/Nurses role in patient education 2 • (Awareness encourages patient to cooperate/ help collect urine samples) • (Patient awareness encourages effort to drink more fluid) • Inform patient of cause of AKI and management plan, how to prevent this in future • Drugs to withhold if dehydrated or sepsis- e. g ramipril, ibuprofen, metformin, furosemide etc. • Advice about making effort to increase fluid intake if unwell and seeking help early if reduced urine production, dark urine, +/-dizzy on standing

11. Summary • AKI is a common problem affecting 5 -15% of all hospitalised patients • AKI associated with 100, 000 inpatient deaths • AKI is easily reversible/preventable if identified early by assessing for risk factors, treating cause and monitoring frequently, especially urine output and vital signs • HCSW and nurses play a very important role in identifying, prevention and management of AKI

Management of AKI- summary 1 • Identify risk factors for AKI • Identify possible cause of AKI e. g dehydration, infection, medication, obstruction • Stage of AKI on e-alert ( or urine output) • Further investigations- bicarbonate, sepsis screen, USS as appropriate • Monitoring • Urinalysis- record result in notes, and appropriate action if abnormal • Urine output; Weigh patient, minimum urine output/h= 0. 5 ml x weight. • Assess urine output on admission and at least 4 hourly( 1 -2 hourly if AKI 2/3 or EWS>3, or inadequate urine output).

• Encourage hydration increased oral fluids or intravenous fluids • Monitor fluid balance at least 4 hourly or more often as above • Monitor EWS at least 4 hourly or 1 -2 hourly if AKI 2/3, poor urine output • Request help if persistent low urine output or high EWS>3 for over 4 hours Treatments • Rehydration- oral or i. v fluids- balanced crystalloids e. g. Hartman's or 0. 9% saline boluses to treat hypovolaemia till corrected signs and improved EWS. Maximum of 2 l in 2 -4 hours with doctor input. Otherwise maintenance fluids and extra to cover for excess loss

Management of AKI Summary 2 • Stop nephrotoxic drugs • Reduce dose of some drugs e. g. enoxaparin Augmentin, long acting opiates etc. • Treat precipitating cause e. g sepsis, hypovolaemia, obstruction • Blood transfusion if hypovolaemia due to bleed • Relief urinary obstruction with catheter • Repeat E&U at 6 -12 hr initially, then at least daily • Identify complications early and appropriate escalation • Patient/carers advice and information

Acknowledgement • http: //elearning. nice. org. uk/ National Institute for Health and Care Excellence (NICE) Acute Kidney injury An e-learning module for nonrenal registered nurses and Health Care Support workers in all settings March 2014 • NICE CG 169. National Institute for Health and Care Excellence. Clinical guideline 169: Acute kidney injury: prevention, detection and management of acute kidney injury up to the point of renal replacement therapy. 2013. • NCEPOD 2009. Stewart J et al (editors). Adding insult to injury: a review of the care of patients who died in hospital with a primary diagnosis of acute kidney injury (acute renal failure). The National Confidential Enquiry into Patient Outcome and Death. 2009 • www. thinkkidneys. nhs

Quiz • Q 1 - What is Acute Kidney Injury? • A) A sudden or rapid deterioration in renal function over hours or days • B) A rise in Creatinine of >26 mmol/l within 48 hours • C) Urine output <0. 5 ml/kg/h for over 6 hours • D) All of the above- definition of AKI
Q 2 How many stages of AKI are there? • A) 5 • B) 3 • C) 2

Q 3 How many people die from AKI in hospitals in the UK/ year • A) 10, 000 people • B) A million people • C) 100, 000 people

Q 4 Which of these are common causes of AKI • • • A) Sepsis B) Dehydration C) Myeloma- very rare cause D) Hypovolaemia E) Rhabdomyolysis- rare cause

Q 5 Which of these drugs can damage the kidney(nephrotoxic) • • • A) Ramipril B) Aspirin- safe C) Gentamicin D) Ibuprofen E) Gaviscon- safe

Q 6 Which of these measures are important in the management of AKI? • A) Important to stop nephrotoxic drugs • B) Record urinalysis results only if positive for blood and protein • C) Monitor urine output and EWS more frequently such as 1 -2 hourly in AKI 3 • D) Treat cause of AKI • E) New onset confusion, vomiting and shortness of breath in a patient with AKI 3 may indicate complication such as metabolic acidosis

Q 7 Which of these are complications of AKI? • A) Hyperkalaemia- True • B) Pulmonary oedema due to fluid overloadtrue • C) Uraemic Encephalitis- True • D) Death- True • E) Diabetes- False

Q 8 Which of these patients have got increased risk factors for AKI? • A) Known history of Chronic Kidney disease • B) Use of nephrotoxic drugs in past 7 days • C) 56 years old man attending eye clinic for cataract check( >65 years) • D) Patient admitted for emergency abdominal surgery • E) Acutely ill patient with EWS of 6
- Slides: 70