Acute inflammation 3 By Dr S Homathy This

Acute inflammation 3 By Dr. S. Homathy

• This is augmented by slowing of the blood flow and increased vascular permeability, • fluid leaves the vessel causing – leukocytes to settle-out of the central flow column – and “marginate” along the endothelial surface • Leucocytes accumulate at the periphery of vessels – Margination
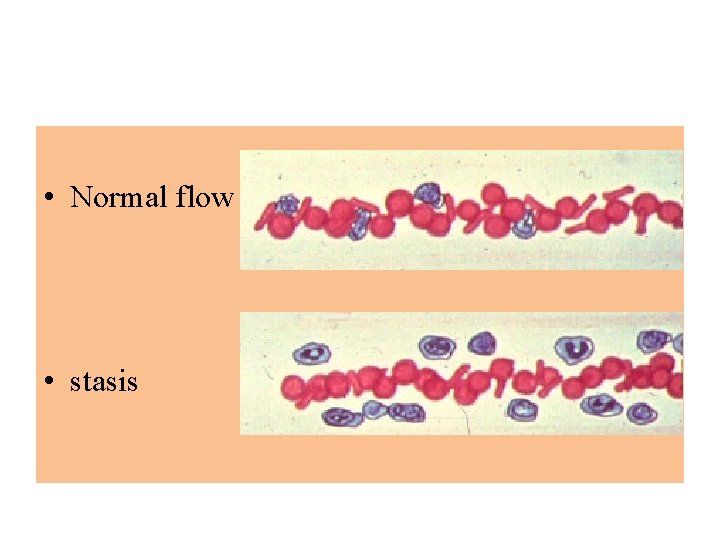
• Normal flow • stasis

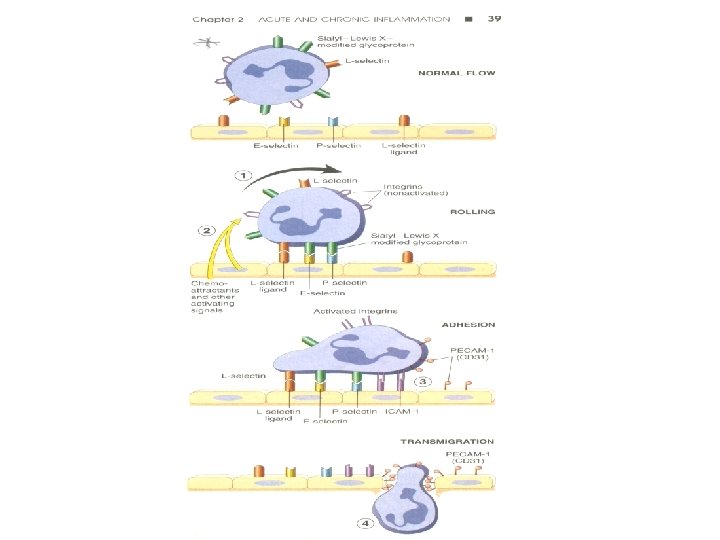
Rolling • Endothelial cells and leukocytes have complementary surface adhesion molecules • which briefly stick and release causing the leukocyte to roll along the endothelium – like a tumbleweed until – it eventually comes to a stop as mutual adhesion reaches a peak

Rolling • Then WBC tumble on the endothelial surface – Transiently sticking along the way- rolling • Lose and transient adhesions are mediated by the selectin family of molecules • Selectins are receptor expressed on leukocytes and endothelium – They bind to the selectin sugars v E-selectin - endothelium v P-selectin - endothelium and Platelets v L-selectin - leukocytes

• They are expressed at low level / absent on normal cells • They are up- regulated after stimulation by specific mediaters. • upregulated on endothelium by cytokines (TNF, IL-1) at injury sites
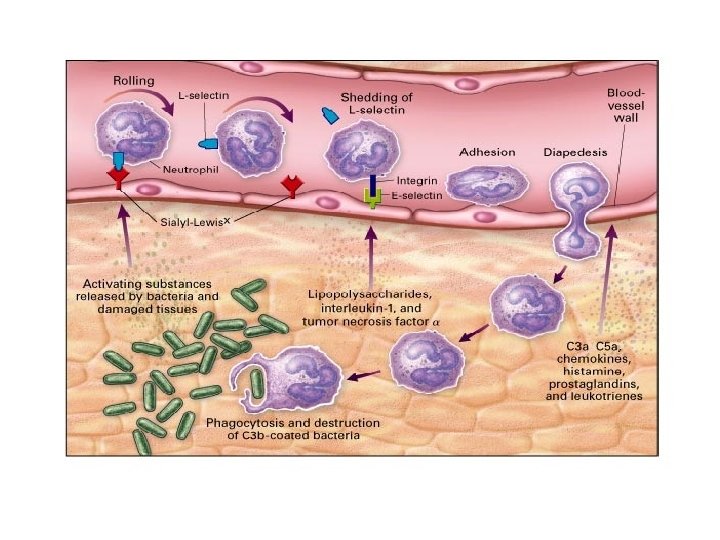
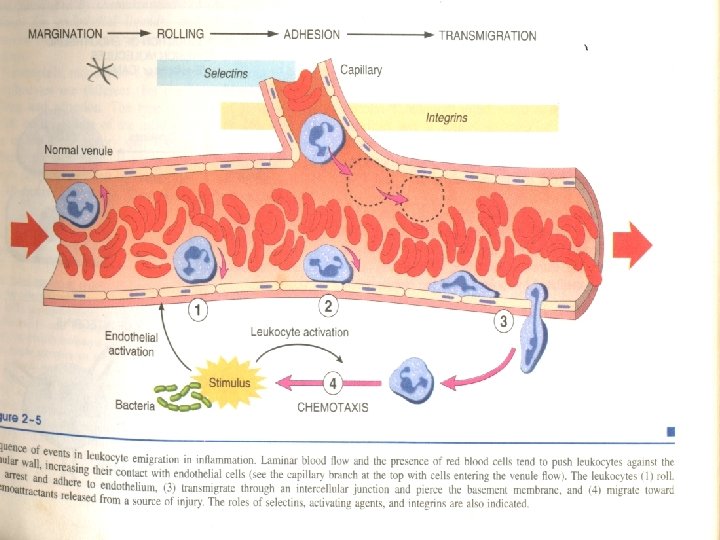

Adhesion • Rolling comes to a stop and adhesion results before leukocytes crawling between endothelial cells • The firm adhesionis mediated by molecules of immunoglobulin superfamily

• The molecules participate are: – Endothelial: ICAM-1, VCAM-1 – Leukocyte: LFA-1, Mac-1, VLA-4 (ICAM-1 binds LFA-1/Mac-1, VCAM-1 binds VLA-4) • Ordinarily down-regulated or in an inactive conformation, but inflammation alters this • Cytokines –TNF and IL-1 induce the expression of both ICAM-1 and VCAM-1
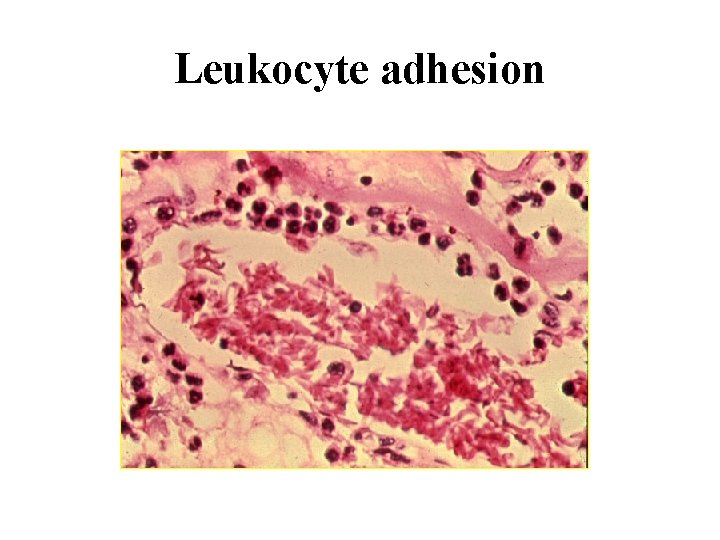
Leukocyte adhesion

Transmigration (Diapedesis) • Occurs after firm adhesion within the systemic venules and pulmonary capillaries via PECAM – 1 (CD 31) • Must then cross basement membrane • Leukocytes cross the BM by focally degrading them with secreted – Collagenases – Integrins

• Early in inflammatory response mostly PMNs, • but as cytokine and chemotactic signals change with progression of inflammatory response, • alteration of endothelial cell adhesion molecule expression – activates other populations of leukocytes to adhere (monocytes, lymphocytes, etc)

• In most acute inflammatory lesions PNL predominate in the first 6 -24 hrs • Then replaced by monocytes in 24 -48 hrs • Neutrophils undergo apoptosis within 24 -48 hrs of exiting the blood stream
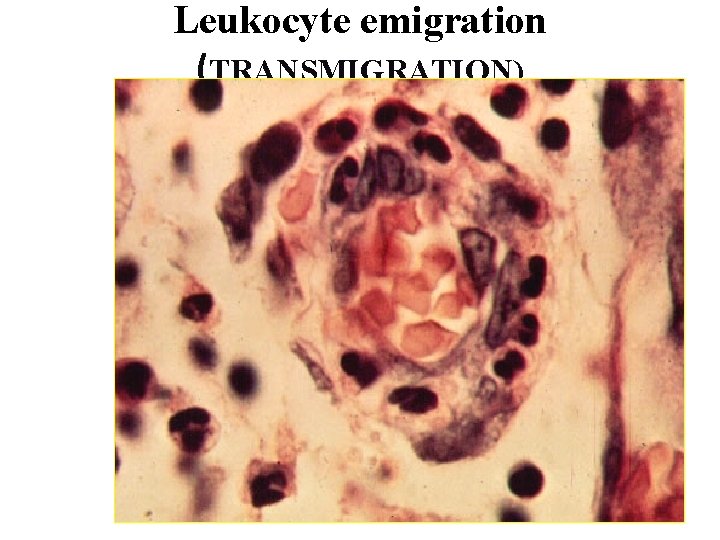
Leukocyte emigration (TRANSMIGRATION)

Chemotaxis and Activation • Leukocytes follow chemical gradient to site of injury (chemotaxis) • It is the unidirectional migration of cells towards an attractant – Soluble bacterial products – Complement components (C 5 a) – Cytokines (chemokine family e. g. , IL-8) – LTB 4 (AA metabolite)

• Chemotactic agents bind surface receptors • inducing calcium mobilization and assembly of cytoskeletal contractile elements

Leukocytes: • extend pseudopods with overlying surface adhesion molecules (integrins) that bind ECM during chemotaxis • undergo activation: – Prepare AA metabolites from phospholipids • Prostaglandin (and thromboxanes) • Leukotrienes • Lipoxins

• Prepare for degranulation and release of lysosomal enzymes (oxidative burst) • Regulate leukocyte adhesion molecule affinity as needed
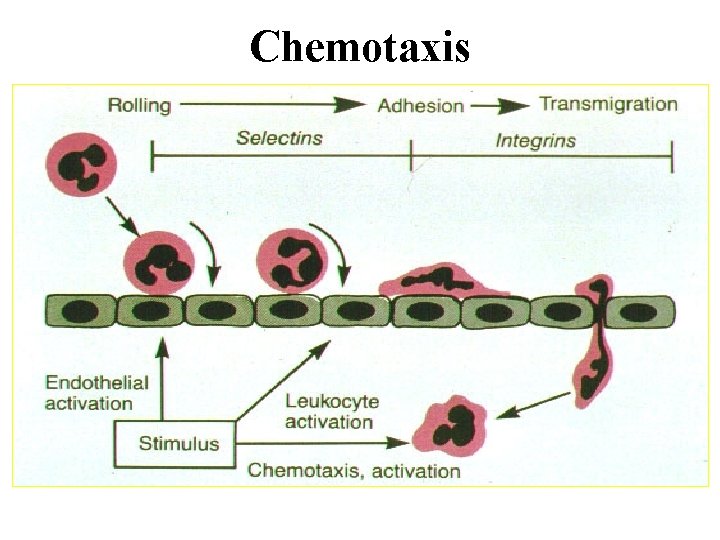
Chemotaxis

Phagocytosis and Degranulation • Once at site of injury, leukocytes involve several steps: – Recognize and attach – Engulf (form phagocytic vacuole) – Kill (degrade)

Recognition and Binding • Recognition and attachment of leukocytes is facilitated by serum protein- opsonins • Opsonized by serum complement, immunoglobulin (C 3 b, Fc portion of Ig. G) • Corresponding receptors on leukocytes (Fc. R, CR 1, 2, 3) leads to binding
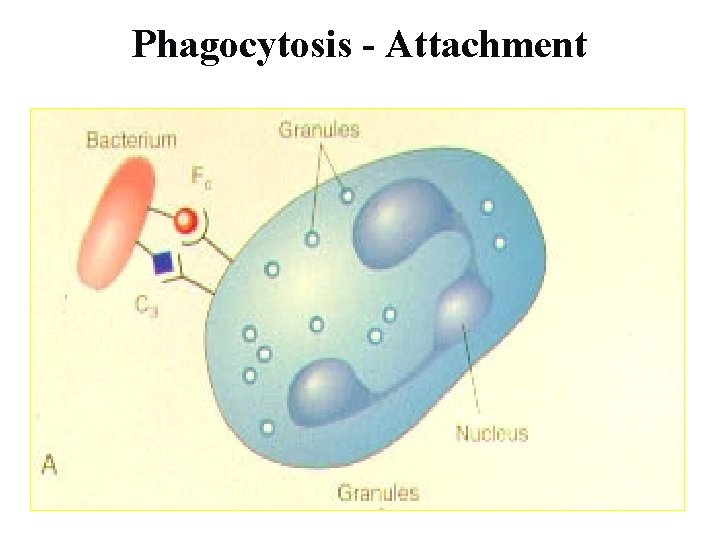
Phagocytosis - Attachment
- Slides: 24