Acute Graft Versus Host Disease a GVHD Teaching























- Slides: 29

Acute Graft Versus Host Disease (a. GVHD) Teaching session 1 July, 2004 Meg Browning

Definition of terms v v v GVH(D): Graft-versus-host (disease). The set of symptoms that occur when the immune cells from a graft (marrow, organ, even transfusion) react against the recipient. MHC: major histocompatibility complex; the primary proteins that identify “self. ” We currently measure 10 genetic alleles for such proteins. These genes sort together, so you get them as sets from your parents, not as individual proteins. Syngeneic: matching exactly (e. g. , identical twins) Allogeneic: not matching at some level (a “matched sibling” is still allogeneic!) Autologous: (autogeneic, sadly, isn’t a word): from self

A brief note on “acute” and “chronic” The classic definition is whether or not the patient is within the first 100 days after transplant; thus, “acute” GVH occurs before day 100. v There are pathological differences, as seen on biopsy, between disease states that would be considered chronic vs. acute v The red skin rash we see is acute; the chronic skin disease is more like scleroderma v Profuse watery diarrhea is consistent with acute; wasting is more chronic v

Boring “historical perspective” slide v v v A fatal syndrome of skin abnormalities and diarrhea (or wasting, in newborns) given allogeneic spleen cells after irradiation (or in the newborns, at all). Primary disease was the same thing after irradiation itself. This was in the 1950’s, and in mice. Primary disease Secondary disease (GVHD)

1966 (original, Billingham) definition Criteria for the development of GVHD: v The graft must contain immunologically competent cells. v v v The host must possess alloantigens that are lacking in the graft (must appear foreign). v v Still true True in the parenthetical explanation The host must be incapable of mounting an effective anti-graft reaction, at least for a period of time. v True as long as you emphasize “effective. ”

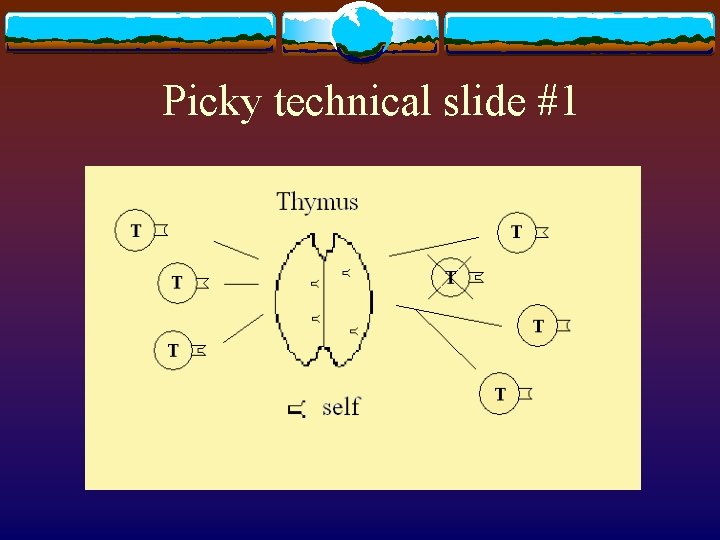
Picky technical slide #1

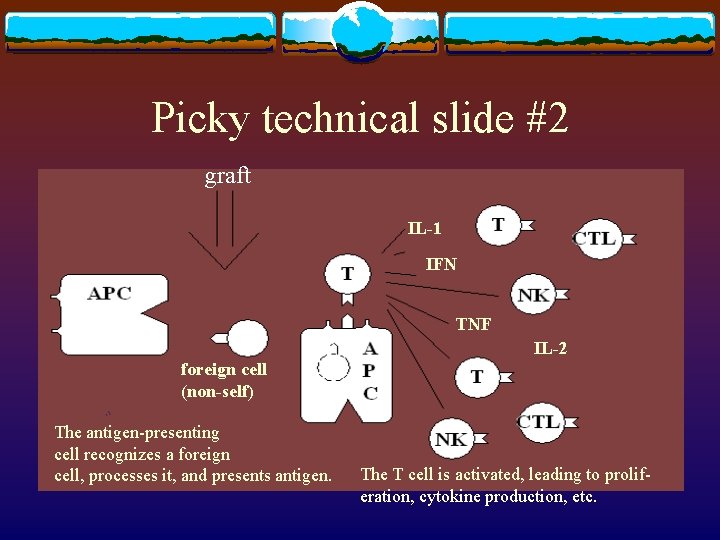
Picky technical slide #2 graft IL-1 IFN TNF IL-2 foreign cell (non-self) The antigen-presenting cell recognizes a foreign cell, processes it, and presents antigen. The T cell is activated, leading to proliferation, cytokine production, etc.

Trick Question v Can recipients of autologous (and/or syngeneic) transplants still get GVHD? v Yes. v (OK, so it loses something when I warn you it’s a trick. ) v How? v possibly thymic damage, and/or regulatory imbalance

What creates a GVHD set-up? (or lack thereof) v alloreactivity v v v recipient age v v v v particularly herpes family conditioning v v v cord: ? less marrow PBSC: more chronic whether T cell depleted microbes v 20%, 30%, and 80% at <20, 45 -50, and >50 donor age stem cell source v degree of mismatch strength of mismatch sex mismatch donor parity age v v immune suppression organ damage prophylaxis

Acute GVHD v v Occurs within the 1 st 100 days post-transplant; typically between days 4+ and 40. Triad of dermatitis, enteritis, and hepatitis v v v ocular symptoms, pneumonitis, and hemorrhagic cystitis may also occur acutely, as may thrombocytopenia and anemia. 40% of all HLA-matched recipients still get GVHD! GVHD increases the risk of sepsis and certain other complications a. GVHD patients are more likely to have c. GVHD There is no racial or gender predilection GVHD may decrease the likelihood of relapse

Skin is usually first v v Red to violet lesions, often starting on palms and soles. May hurt or itch. Becomes confluent over cheeks, ears, neck, trunk; papules may form. In severe cases, bullae and epidermal necrosis occur. DDx: scalded skin syndrome (infection), viral exanthem, chemo/radiation effects, drug allergy. Biopsy or serial biopsies are helpful in Dx. v Biopsy findings are graded, not staged Liver or GI involvement is unusual WITHOUT skin involvement

More skin GVH issues v Staging: 1: v 2: v 3: v 4: v < 25% of the BSA is involved 25 -50% BSA 50 -100%, as erythroderma vesicles and bullae Higher stages are more likely to develop chronic skin GVH v Hyperacute GVH: fever, erythroderma (may be pruritic), and desquamation prior to engraftement (before day 14). v

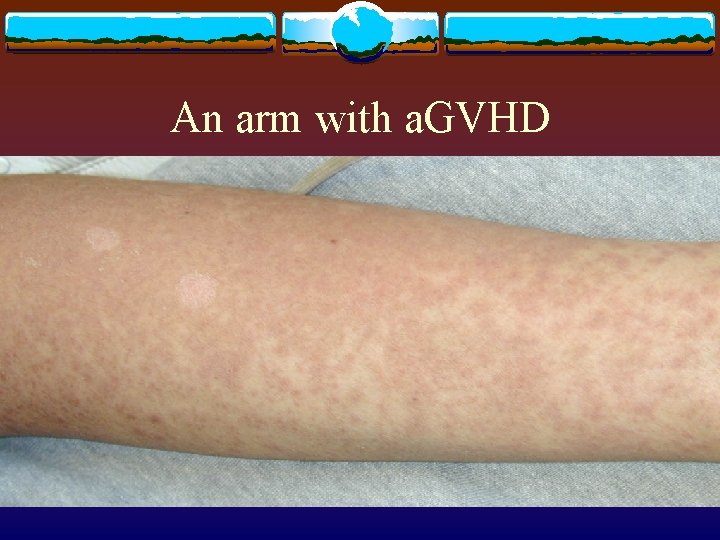
An arm with a. GVHD

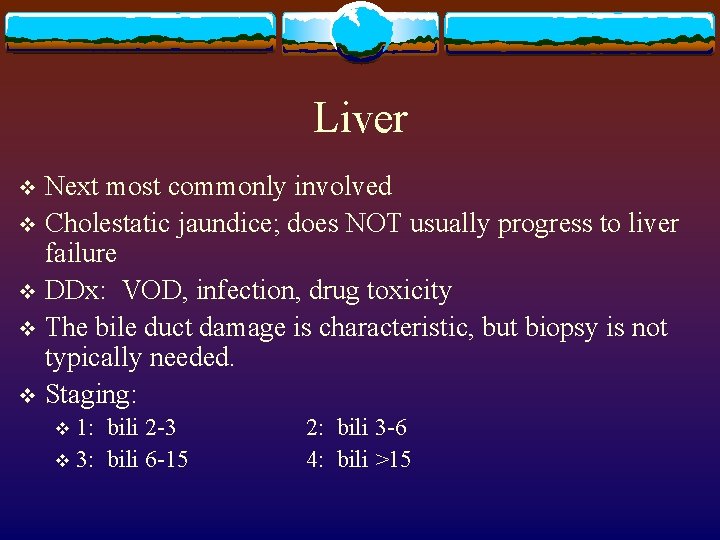
Liver Next most commonly involved v Cholestatic jaundice; does NOT usually progress to liver failure v DDx: VOD, infection, drug toxicity v The bile duct damage is characteristic, but biopsy is not typically needed. v Staging: v 1: bili 2 -3 v 3: bili 6 -15 v 2: bili 3 -6 4: bili >15

Gut v v v Diarrhea (green, water, mucoid; may contain cells and fecal casts), intestinal bleeding, crampy abdominal pain, ileus Upper tract disease is less common, and occurs in older patients. Requires Bx for diagnosis. Barium studies show increased transit time and loss of haustral folds Histology is quite variable. DDx: residual chemo effects, infection Staging: 1: diarrhea 500 -1000* cc of stool/day OR persistent nausea v 2: 1000 -1500* cc 3: >1500* cc 4: pain +/ileus *stool volumes were determined in adults. v

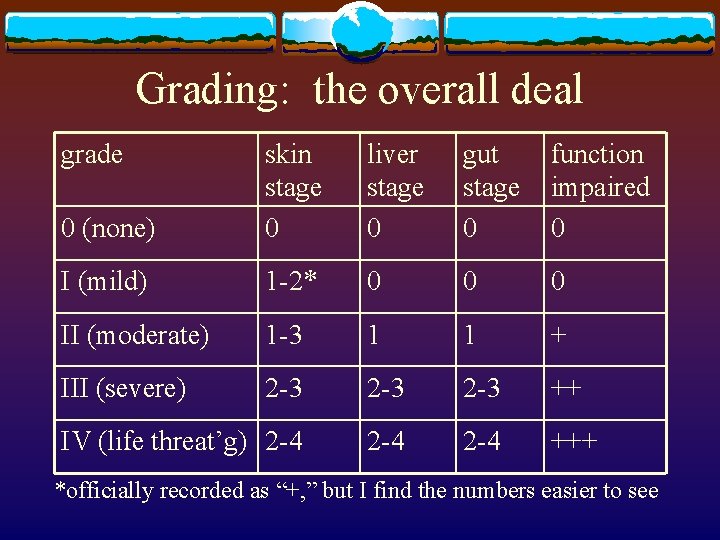
Grading: the overall deal grade 0 (none) skin stage 0 liver stage 0 gut stage 0 function impaired 0 I (mild) 1 -2* 0 0 0 II (moderate) 1 -3 1 1 + III (severe) 2 -3 2 -3 ++ IV (life threat’g) 2 -4 2 -4 +++ *officially recorded as “+, ” but I find the numbers easier to see

How do we treat GVHD? Prevent it!!

GVHD Prevention v To review briefly: match well (antigens, ? CMV), T-deplete (? ), condition less v These suggestions are all very well for GVHD, but have to be balanced with what is good (well, bad) for the underlying disease v Prevent infection v Immunosuppress post-transplant v Consider antibody prophylaxis

Antibody prophylaxis v IVIG helps on 2 fronts Prevents certain infections v Reduces the frequency of a. GVHD, at least in adults v v no, I don’t actually know how ATG has not yet been proven helpful on a sustained basis, but is sometimes used as part of immunosuppression v Other agents such as anti-cytokine products are now being used and tested – more on those if we have time. v

Immunosuppress v v v v MTX, the old standby MTX + CSA + PRED CSA FK 506 + CSA It’s difficult to interpret a lot of this data, as it is either very small numbers or compared across different prep regimens, types of transplant, ages, etc. Not only the agents, but the doses and length of therapy are all open to question.

What do we use? Aplastic anemia (non-TBIbased prep) v CSA/MTX Haploidentical donor – old protocol v Haplo, new protocol v CSA/ATG v Nothing! Unrelated donor, Tdepleted graft (with TBI) v CSA/MP taper v v v NOTE: Can substitute FK 506 (tacrolimus) for CSA in most cases

Prevent infection v v v v An area where the nursing staff has particularly great opportunity to make a difference BMT diet: NOT proven. SAA patients conditioned with CSA alone benefited from aseptic guts. Hand washing is well-proven, but not for GVH Limiting sick staff is a hot topic, again “just” for overall infection Surveillance cultures are still recommended, and antimicrobials Mouth cares: may actually be helpful, though it is unclear exactly how infectious mucositis and mucous membrane GVH involvement are related Matching for CMV: another hot topic, as it may be better from a relapse perspective NOT to.

OK, now what if we truly do have to treat it.

Initial therapy Treat all patients with grade II or greater. v Methylprednisolone (IV steroid) is the primary treatment of choice. Boluses may range from 1 -60 mg/kg/day. Taper based on response. v Continue GVH prophylaxis (such as CSA) during therapy, plus of course infection prophylaxis (especially TMP/SMX). v CSA is generally not a great treatment, nor ATG. However, some patients will respond, especially to CSA + methylpred. v

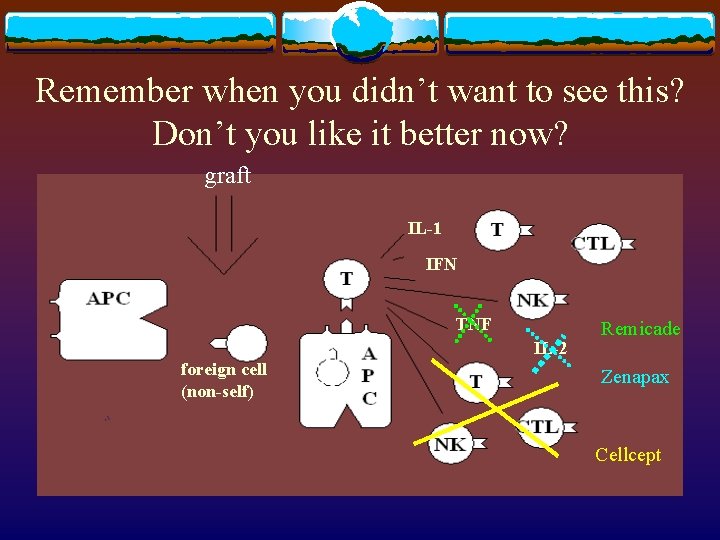
New kids on the block Mycophenolate mofetil (MMF, Cellcept) is becoming more established in the treatment of a. GVHD. It kills lymphocytes. v Newer on the block is anti-IL-2 R, aka anti-CD 25, or daclizumab (Zenapax). v

Salvage therapies v v v Anti-TNF-alpha, or infliximab (Remicade), which works for a. GVHD (especially gut) but leads to increased fungal infections. (We have mostly used it for c. GVHD, here. ) Anti-CD 25 (CD 25 is a surface marker for activated T cells), or daclizumab (Zenapax): a current NIH study Many others in adult patients, mostly with around 30% response rates and very poor “cure” rates Anti-CD 3 (anti-T cell) antibodies have been tried in various forms, but thus far with as many complications as successes (for this; they’re useful in solid tumor rejection) Ultraviolet radiation and psoralens are currently considered “salvage” as well.

Remember when you didn’t want to see this? Don’t you like it better now? graft IL-1 IFN TNF IL-2 foreign cell (non-self) Remicade Zenapax Cellcept

A few words about chronic GVHD By definition, occurs after day 100, but usually occurs between 3 and 18 mos post-BMT. v 30% of matched-sib transplants (all comers, not just peds) v Around 50% of those with > grade 1 acute GVH will go on to develop chronic GVHD; 10 -20% mortality. v In general, diagnosis and treatment are similar to acute; however, grading is usually as “limited” versus “extensive. ” v

What’s happening now FK 506 (tacrolimus, Prograf) is becoming more important in BMT, and may be particularly successful in steroidresistant patients. (Probably works by decreasing cytokine production and lymphocyte activation. ) v New antibodies and combinations of these newer therapies are keeping the basic science folks busy. Around our campus, cellular therapies are also being studied. v So, in 2 -3 years, the amount of information on GVH prevention and/or therapy may double. v