Acute Exacerbations of COPD Gareth Hynes Clinical Research

Acute Exacerbations of COPD Gareth Hynes Clinical Research Fellow University of Oxford

Introduction • Epidemiology • Causes • How to know who’s exacerbating • When to use antibiotics • When to use corticosteroids • When to admit patients • Summary

Background COPD Epidemiology • 115, 000 people are diagnosed with COPD each year – equivalent to a new diagnosis every 5 minutes • 9% in those over age 70 • Nearly 30, 000 people die from COPD each year, making it the second greatest cause of death from lung disease and the UK’s fifth biggest killer
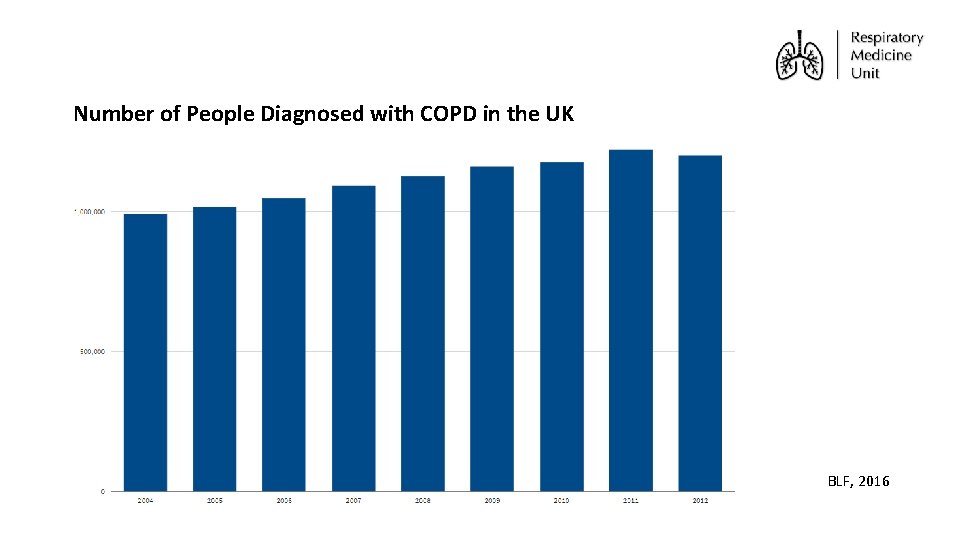
Number of People Diagnosed with COPD in the UK BLF, 2016

Background Exacerbations • Median number of exacerbations seen in primary care was two per year, with one in three suffering three or more exacerbations in 1 year • Frequent exacerbators (> 2 per year): • • • Chronic sputum producers Housebound Frequent colds Poor quality of life Raised inflammatory markers when stable
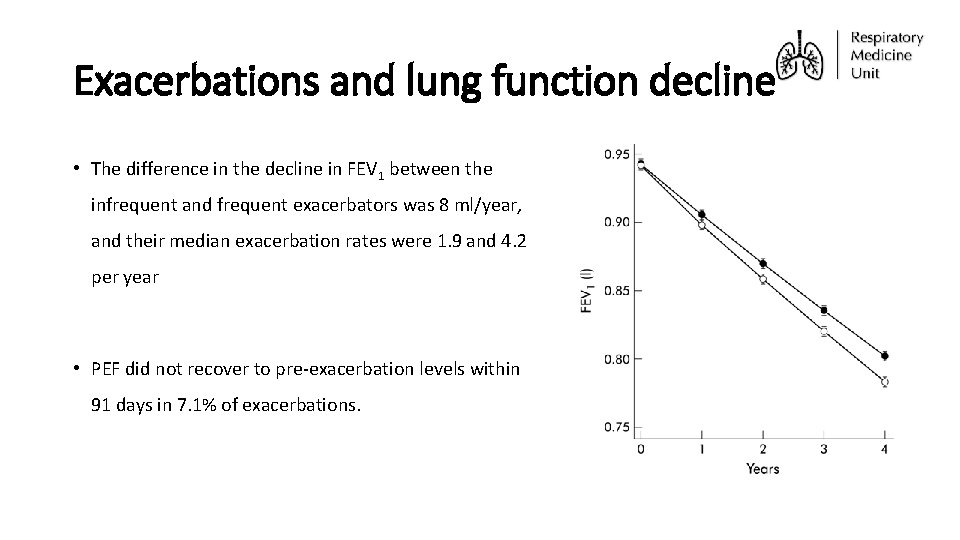
Exacerbations and lung function decline • The difference in the decline in FEV 1 between the infrequent and frequent exacerbators was 8 ml/year, and their median exacerbation rates were 1. 9 and 4. 2 per year • PEF did not recover to pre-exacerbation levels within 91 days in 7. 1% of exacerbations.
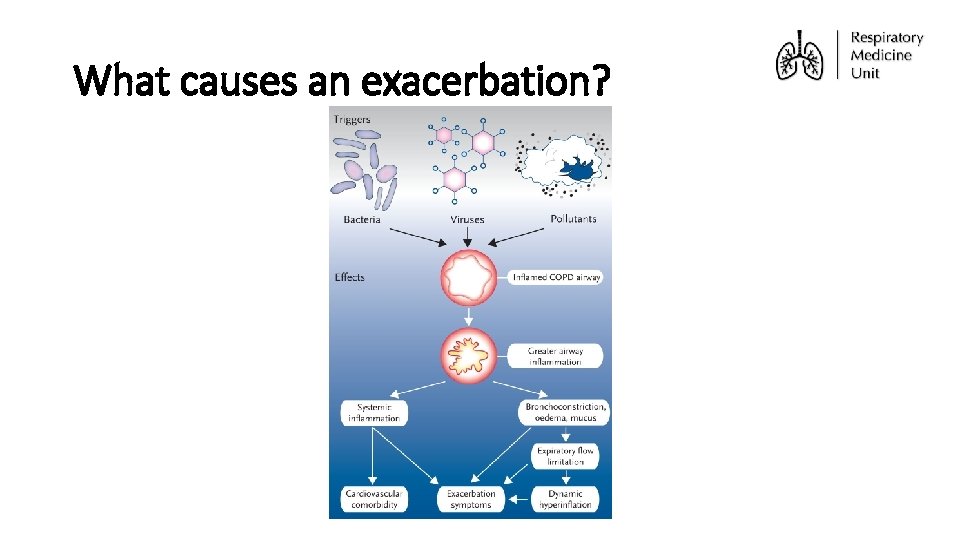
What causes an exacerbation?
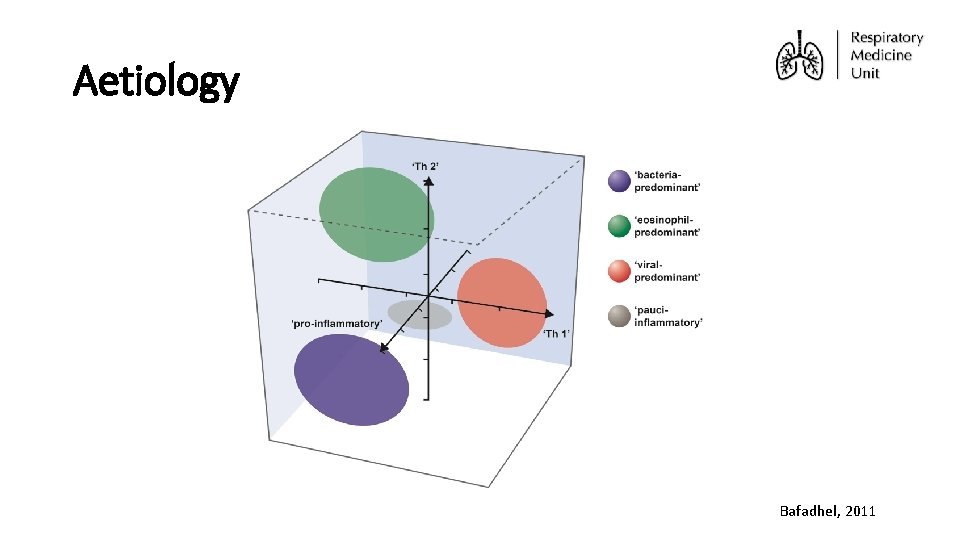
Aetiology Bafadhel, 2011
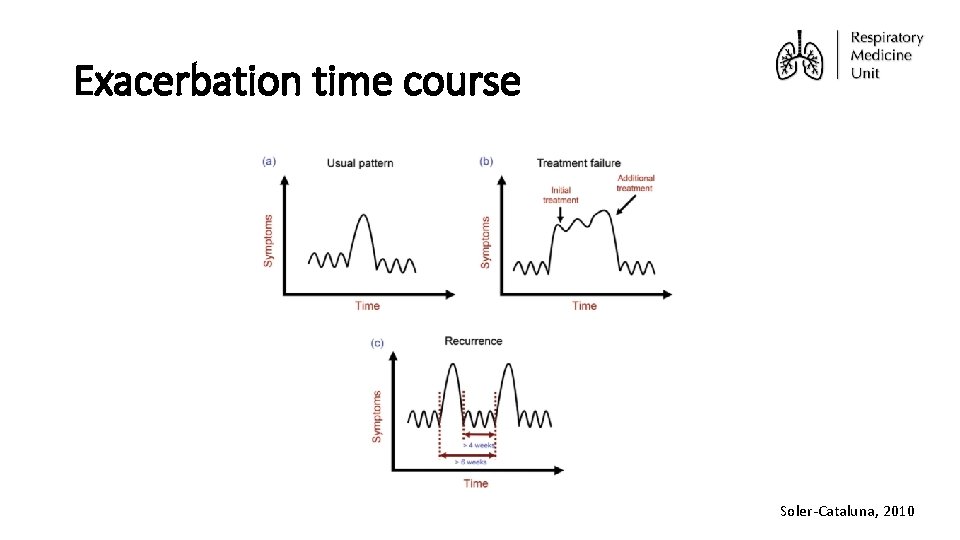
Exacerbation time course Soler-Cataluna, 2010

Diagnosing an Exacerbation An acute worsening of the patient’s usual pattern of respiratory symptoms beyond normal day-today variability: • Increased dyspnoea Dyspnoea: • Worsening cough • Airway narrowing • Increased sputum volume • Increased metabolic state • Sputum purulence No biomarkers of an exacerbation as yet • Increased ventilation–perfusion mismatch.
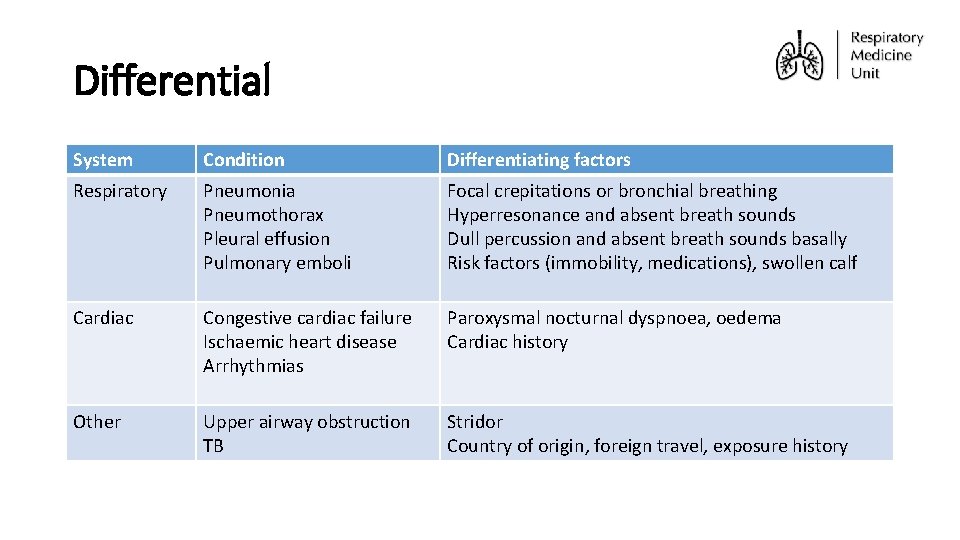
Differential System Condition Differentiating factors Respiratory Pneumonia Pneumothorax Pleural effusion Pulmonary emboli Focal crepitations or bronchial breathing Hyperresonance and absent breath sounds Dull percussion and absent breath sounds basally Risk factors (immobility, medications), swollen calf Cardiac Congestive cardiac failure Ischaemic heart disease Arrhythmias Paroxysmal nocturnal dyspnoea, oedema Cardiac history Other Upper airway obstruction TB Stridor Country of origin, foreign travel, exposure history

Antibiotics Anthonisen et al, 1979
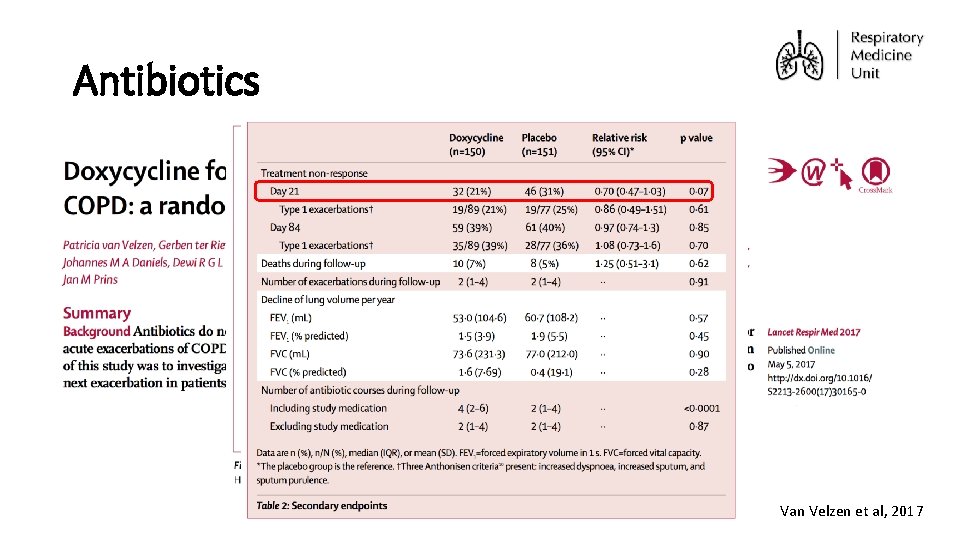
Antibiotics • Background Van Velzen et al, 2017

Antibiotics ERS/ATS Statement 2017 • Antibiotic therapy decreased treatment failure from 42% to 28% (RR 0. 67) - therefore NNT to prevent one treatment failure is 7 • The majority (58%) of patients improved without antibiotics, suggesting not all exacerbations require antibiotics

Antibiotics

Antibiotics Point of care CRP • In the placebo arm, 77% of CRP tests resulted in concentrations < 40 mg/L. • If CRP < 40, the failure rate was 12. 4% • If CRP > 40, the failure rate was 65. 5% (P < 0. 001) Miratvalles, 2013
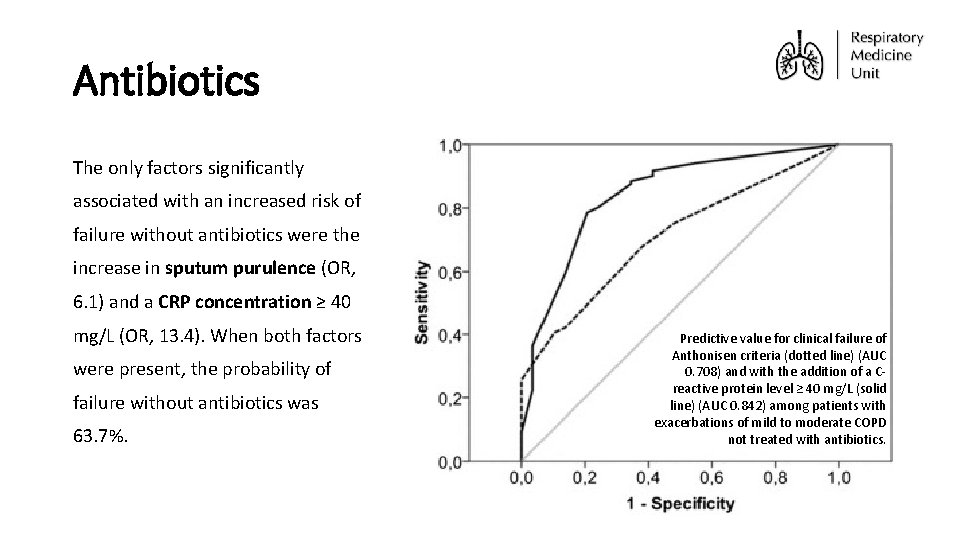
Antibiotics The only factors significantly associated with an increased risk of failure without antibiotics were the increase in sputum purulence (OR, 6. 1) and a CRP concentration ≥ 40 mg/L (OR, 13. 4). When both factors were present, the probability of failure without antibiotics was 63. 7%. Predictive value for clinical failure of Anthonisen criteria (dotted line) (AUC 0. 708) and with the addition of a Creactive protein level ≥ 40 mg/L (solid line) (AUC 0. 842) among patients with exacerbations of mild to moderate COPD not treated with antibiotics.

Antiobiotics Which antibiotics to use? • Targeted towards previous sputum results Moraxella commonly found, Haemophilus may need longer courses (2 weeks), if Pseudomonas isolated > 1 occasion seek respiratory advice • What the patient usually responds to • Otherwise: Amoxicillin 500 mg TDS, Co-Amoxiclav 625 mg TDS, Doxycyxline 100 mg OD, Clarithromycin 500 mg BD

Corticosteroids NICE 2017 In the absence of significant contraindications, oral corticosteroids should be considered in all patients with significant shortness of breath which interferes with day-to-day life Prednisolone 30 mg for 7 to 14 days ATS/ERS 2017 For patients with an exacerbation of COPD with suggest a short (≤ 14 days) course of prednisolone (conditional recommendation, very low quality of evidence)
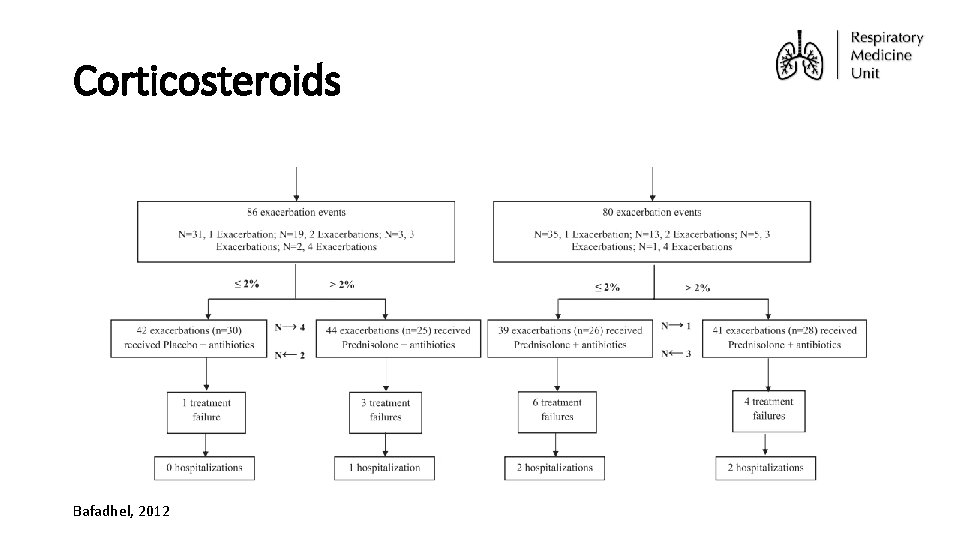
Corticosteroids Bafadhel, 2012
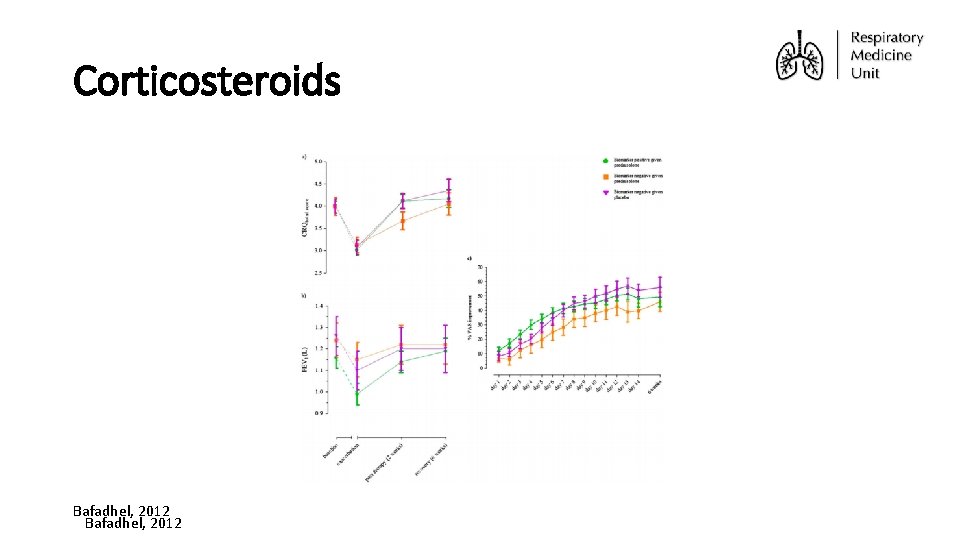
Corticosteroids Bafadhel, 2012

Admissions Major Criteria Minor Criteria • Ability to cope at home • Decreased level of activity • Hypoxia, saturations < 90% or > 5% drop on mild exertion • LTOT • Severe breathlessness • Poor general condition • Altered mental state • Rapid onset • Worsening peripheral oedema Suspicion of presence of differential such as pneumonia, pneumothorax, pulmonary emboli, myocardial infarction

Summary Who to give antibiotics to? Unwell, sputum purulence, CRP > 40 • Who to give corticosteroids to? Currently all In future ? high eosinophilics only Differential diagnoses • PTX • Pneumonia • Pulmonary emboli • Myocardial infarction and arrhythmia • Who to admit? Inability to manage at home, severe SOB, developing peripheral oedema, hypoxic Working towards biomarker-directed approach
- Slides: 23