Acute Demand an overview May 2011 Hospital beds

Acute Demand ……an overview May 2011
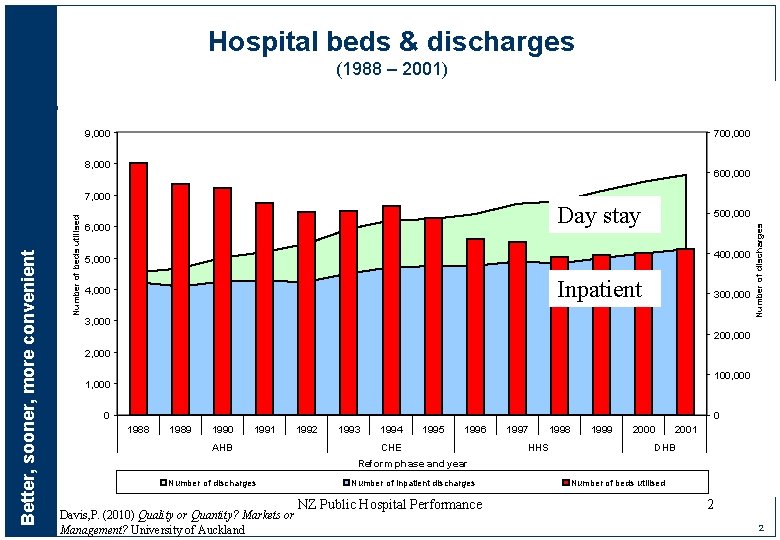
Hospital beds & discharges (1988 – 2001) 9, 000 700, 000 8, 000 600, 000 Day stay Day-stay 6, 000 500, 000 400, 000 5, 000 Inpatient 4, 000 300, 000 3, 000 Number of discharges Number of beds utilised Better, sooner, more convenient 7, 000 200, 000 2, 000 100, 000 1, 000 0 0 1988 1989 1990 1991 AHB 1992 1993 1994 1995 1996 CHE 1997 1998 HHS 1999 2000 2001 DHB Reform phase and year Number of discharges Davis, P. (2010) Quality or Quantity? Markets or Management? University of Auckland Number of inpatient discharges NZ Public Hospital Performance Number of beds utilised 2 2
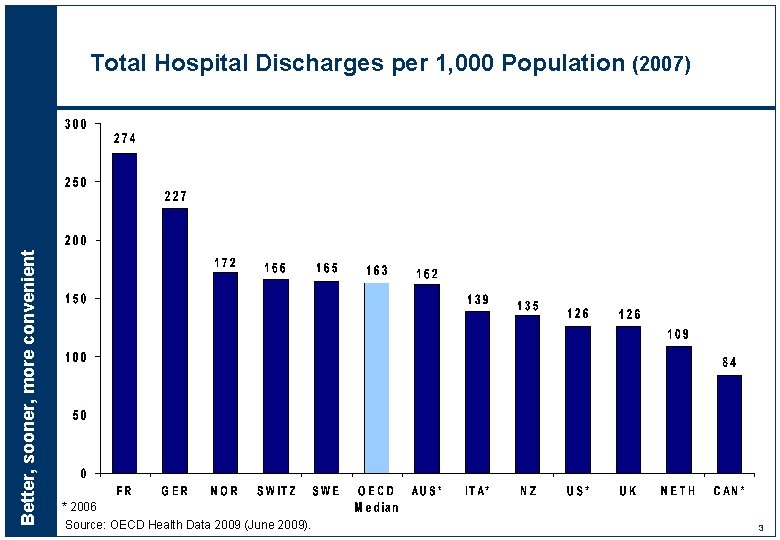
Better, sooner, more convenient Total Hospital Discharges per 1, 000 Population (2007) * 2006 Source: OECD Health Data 2009 (June 2009). 3
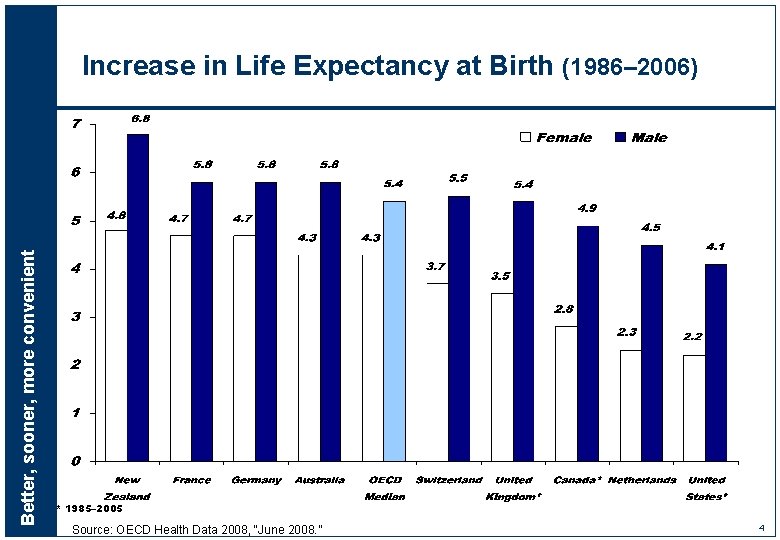
Better, sooner, more convenient Increase in Life Expectancy at Birth (1986– 2006) * 1985– 2005 Source: OECD Health Data 2008, “June 2008. ” 4

Better, sooner, more convenient Philosophy of Kaiser Permanente: “Unplanned hospital admissions are a sign of system failure” Ham, C. (2006), Developing Integrated Care in the NHS: adapting lessons from Kaiser, Health Services Management Centre, Birmingham University 5
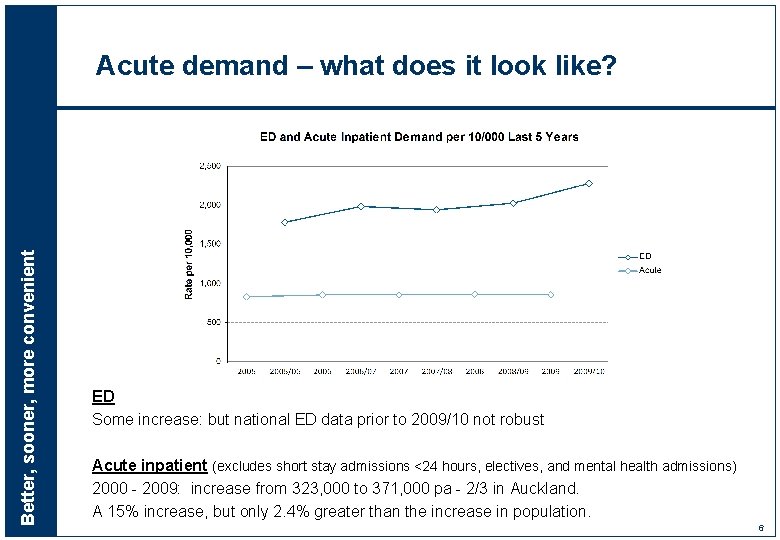
Better, sooner, more convenient Acute demand – what does it look like? ED Some increase: but national ED data prior to 2009/10 not robust Acute inpatient (excludes short stay admissions <24 hours, electives, and mental health admissions) 2000 - 2009: increase from 323, 000 to 371, 000 pa - 2/3 in Auckland. A 15% increase, but only 2. 4% greater than the increase in population. 6
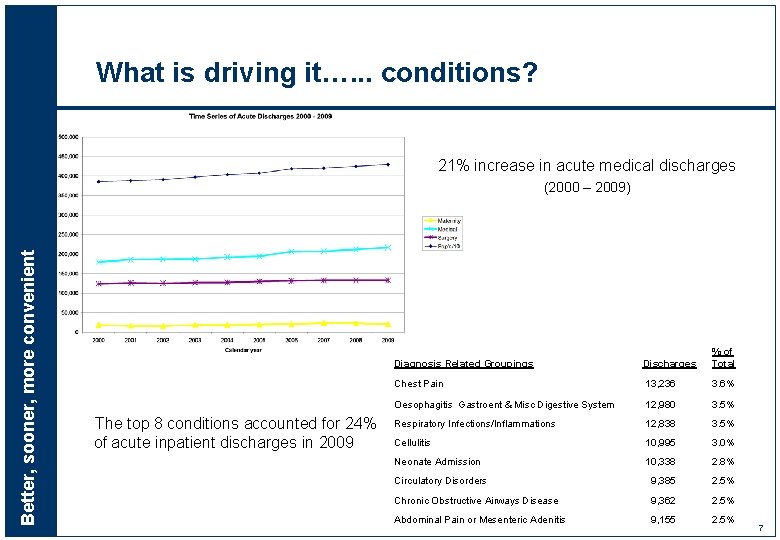
What is driving it…. . . conditions? 21% increase in acute medical discharges Better, sooner, more convenient (2000 – 2009) The top 8 conditions accounted for 24% of acute inpatient discharges in 2009 Diagnosis Related Groupings Discharges % of Total Chest Pain 13, 236 3. 6% Oesophagitis Gastroent & Misc Digestive System 12, 980 3. 5% Respiratory Infections/Inflammations 12, 838 3. 5% Cellulitis 10, 995 3. 0% Neonate Admission 10, 338 2. 8% Circulatory Disorders 9, 385 2. 5% Chronic Obstructive Airways Disease 9, 362 2. 5% Abdominal Pain or Mesenteric Adenitis 9, 155 2. 5% 7

Better, sooner, more convenient OECD Health Care Quality Indicators Database 2009 8
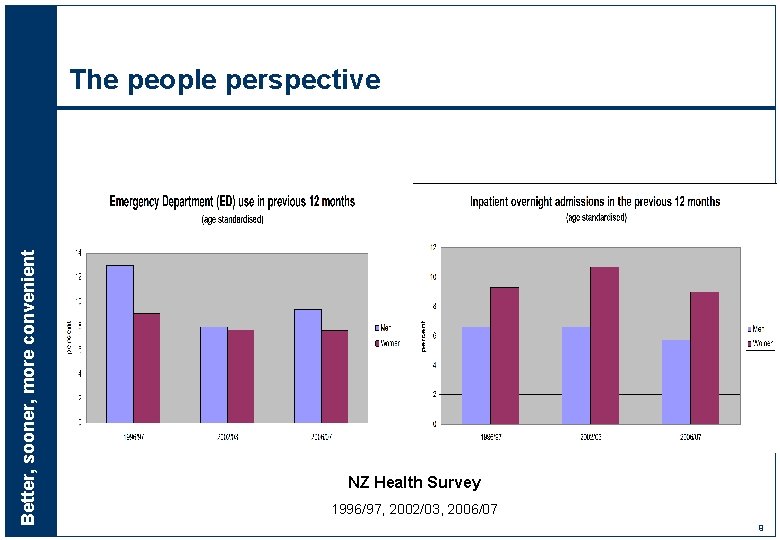
Better, sooner, more convenient The people perspective NZ Health Survey 1996/97, 2002/03, 2006/07 9
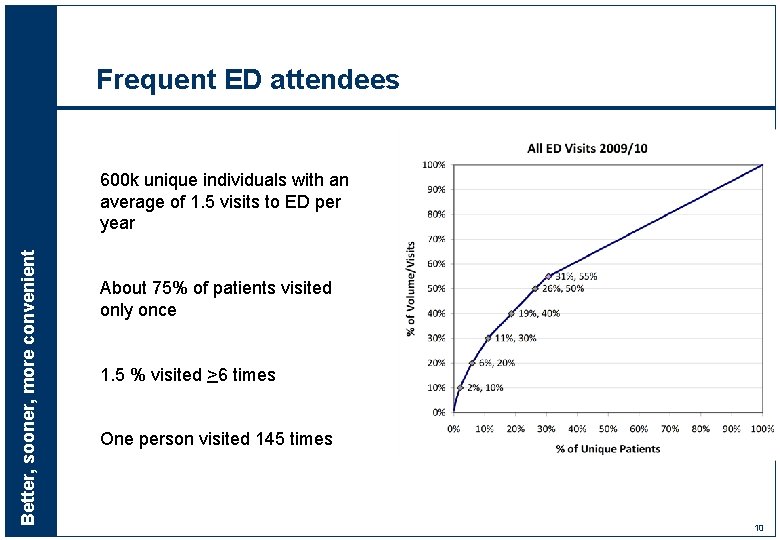
Frequent ED attendees Better, sooner, more convenient 600 k unique individuals with an average of 1. 5 visits to ED per year About 75% of patients visited only once 1. 5 % visited >6 times One person visited 145 times 10

Better, sooner, more convenient 11
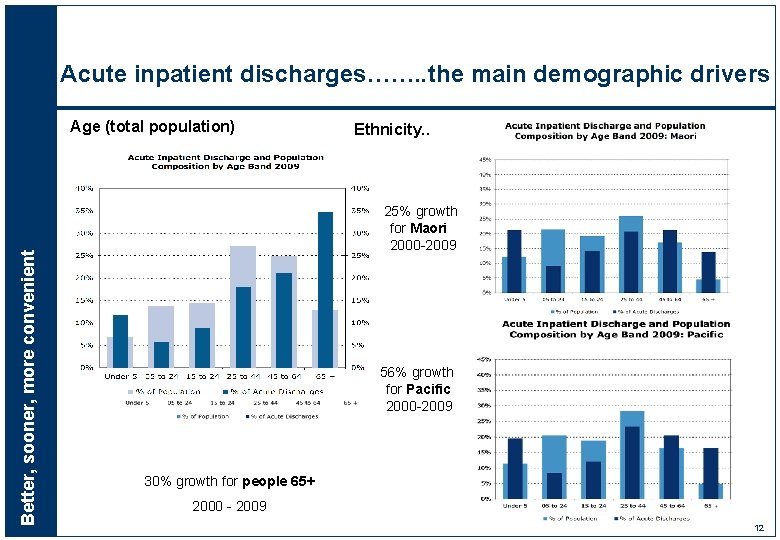
Acute inpatient discharges……. . the main demographic drivers Better, sooner, more convenient Age (total population) Ethnicity. . 25% growth for Maori 2000 -2009 56% growth for Pacific 2000 -2009 30% growth for people 65+ 2000 - 2009 12
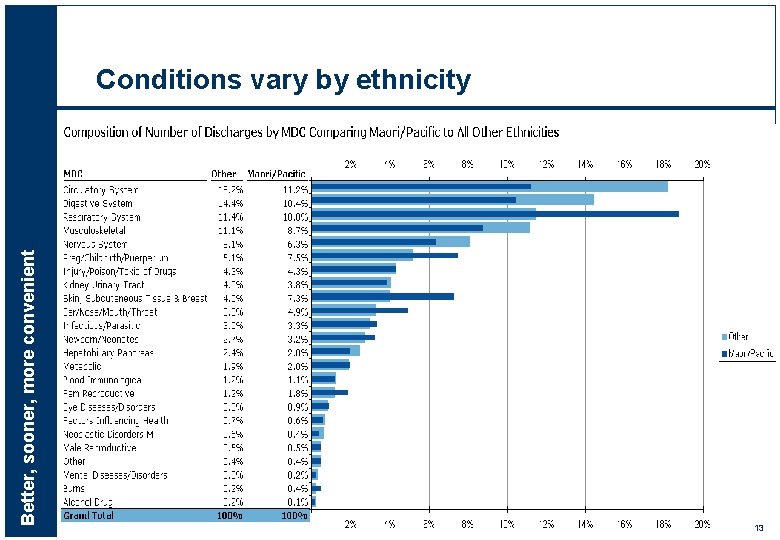
Better, sooner, more convenient Conditions vary by ethnicity 13
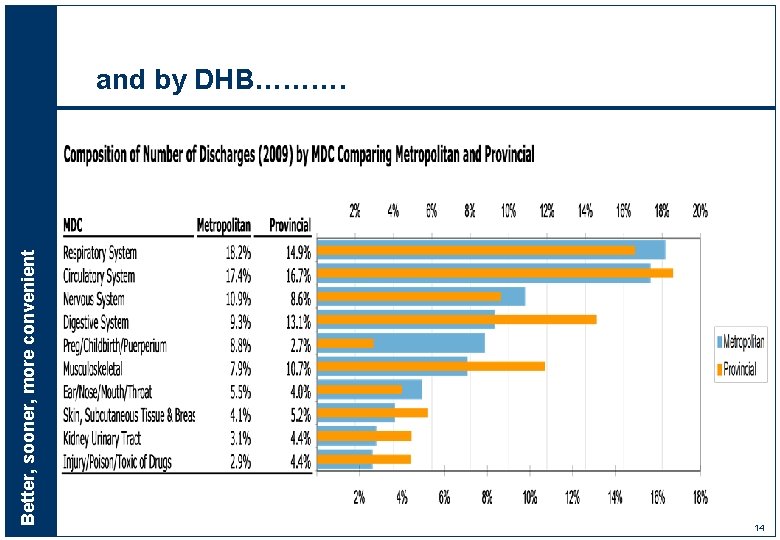
Better, sooner, more convenient and by DHB………. 14
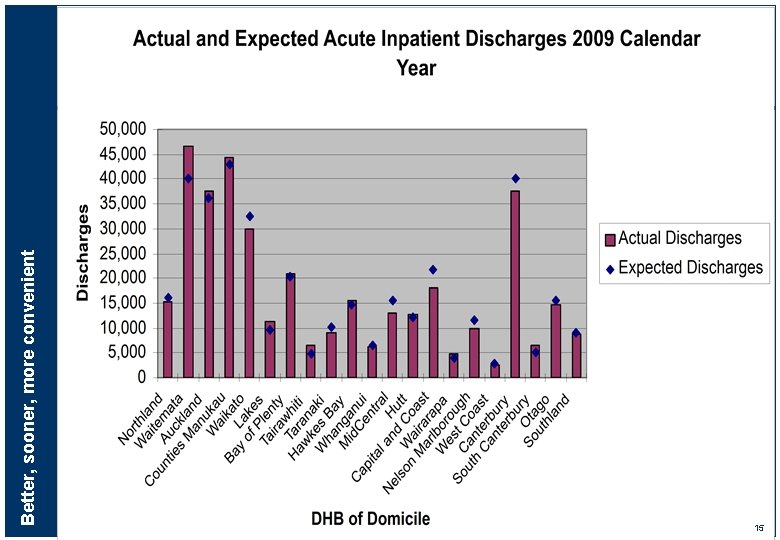
Better, sooner, more convenient 15
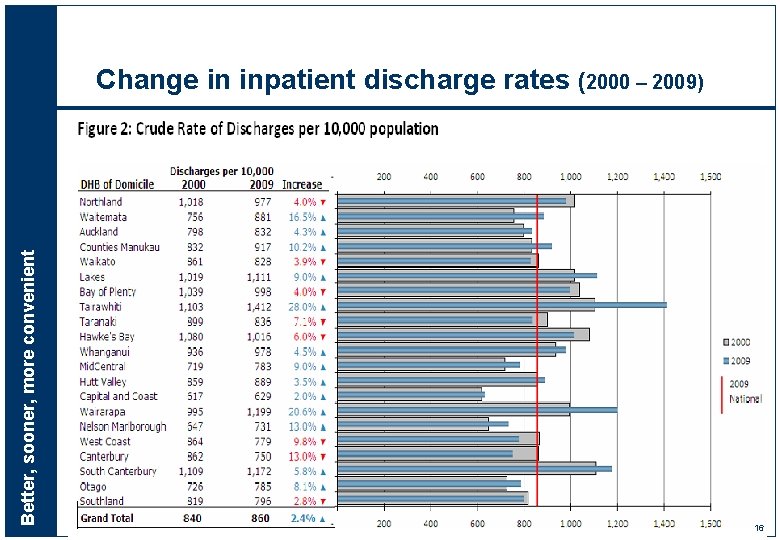
Better, sooner, more convenient Change in inpatient discharge rates (2000 – 2009) 16
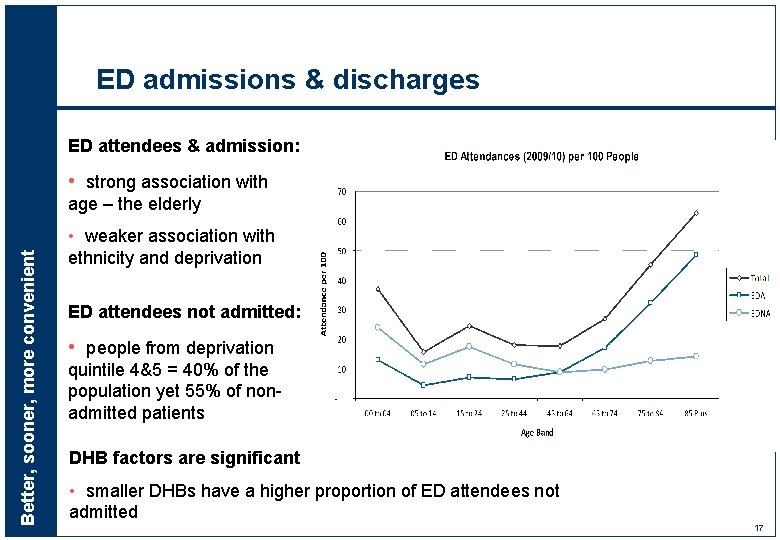
ED admissions & discharges ED attendees & admission: • strong association with Better, sooner, more convenient age – the elderly • weaker association with ethnicity and deprivation ED attendees not admitted: • people from deprivation quintile 4&5 = 40% of the population yet 55% of nonadmitted patients DHB factors are significant • smaller DHBs have a higher proportion of ED attendees not admitted 17

Relationships Better, sooner, more convenient There’s no statistical relationship between acute discharge rates and • the number of GPs • or GP/nurse consultation rates Preliminary analysis shows no relationship with the number of VLCA practices There’s a statistically significant inverse relationship between: • size of the DHB population and rates of ED attenders who are “not admitted” • GP/nurse consultation rates and rates of ED attenders who are “not admitted” (if West Coast and Wairarapa DHBs are excluded) 18
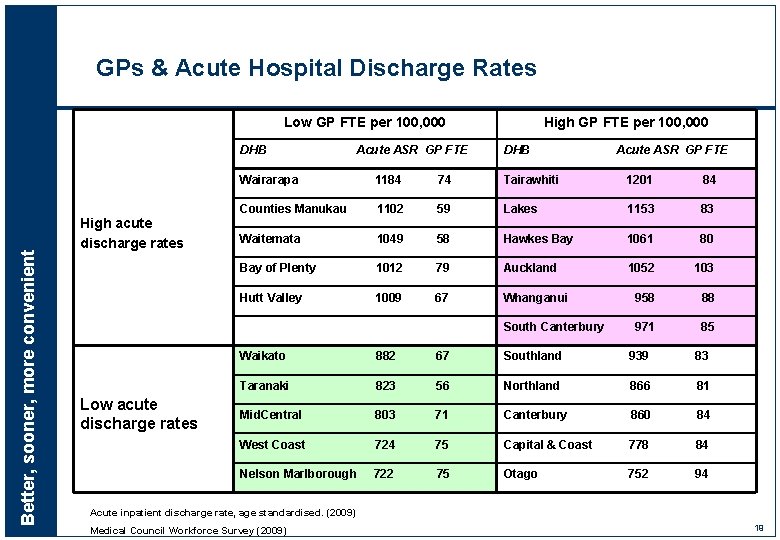
GPs & Acute Hospital Discharge Rates Low GP FTE per 100, 000 Better, sooner, more convenient DHB High acute discharge rates Low acute discharge rates Acute ASR GP FTE High GP FTE per 100, 000 DHB Acute ASR GP FTE Wairarapa 1184 74 Tairawhiti 1201 84 Counties Manukau 1102 59 Lakes 1153 83 Waitemata 1049 58 Hawkes Bay 1061 80 Bay of Plenty 1012 79 Auckland 1052 103 Hutt Valley 1009 67 Whanganui 958 88 South Canterbury 971 85 Waikato 882 67 Southland 939 83 Taranaki 823 56 Northland 866 81 Mid. Central 803 71 Canterbury 860 84 West Coast 724 75 Capital & Coast 778 84 Nelson Marlborough 722 75 Otago 752 94 Acute inpatient discharge rate, age standardised. (2009) Medical Council Workforce Survey (2009) 19
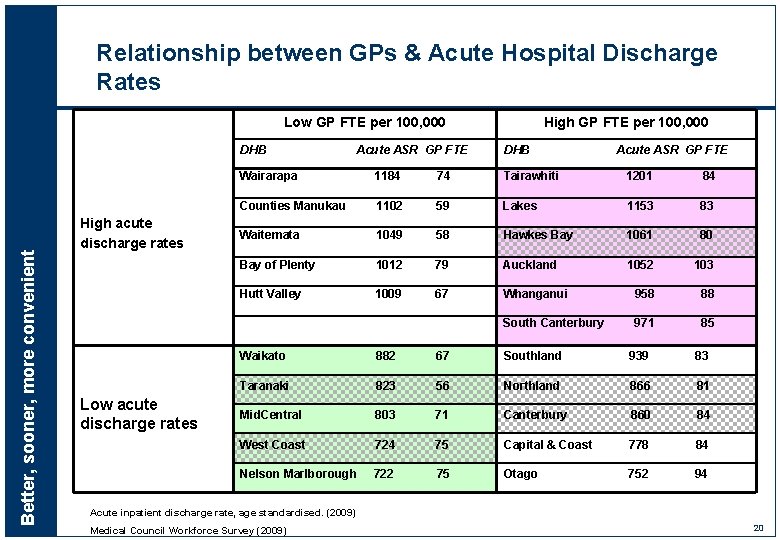
Relationship between GPs & Acute Hospital Discharge Rates Low GP FTE per 100, 000 Better, sooner, more convenient DHB High acute discharge rates Low acute discharge rates Acute ASR GP FTE High GP FTE per 100, 000 DHB Acute ASR GP FTE Wairarapa 1184 74 Tairawhiti 1201 84 Counties Manukau 1102 59 Lakes 1153 83 Waitemata 1049 58 Hawkes Bay 1061 80 Bay of Plenty 1012 79 Auckland 1052 103 Hutt Valley 1009 67 Whanganui 958 88 South Canterbury 971 85 Waikato 882 67 Southland 939 83 Taranaki 823 56 Northland 866 81 Mid. Central 803 71 Canterbury 860 84 West Coast 724 75 Capital & Coast 778 84 Nelson Marlborough 722 75 Otago 752 94 Acute inpatient discharge rate, age standardised. (2009) Medical Council Workforce Survey (2009) 20

Better, sooner, more convenient The system 21
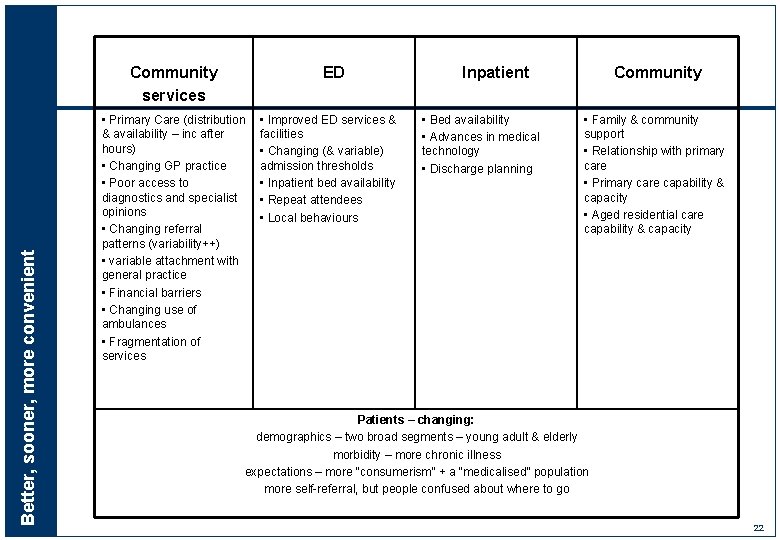
Better, sooner, more convenient Community services ED • Primary Care (distribution & availability – inc after hours) • Changing GP practice • Poor access to diagnostics and specialist opinions • Changing referral patterns (variability++) • variable attachment with general practice • Financial barriers • Changing use of ambulances • Fragmentation of services • Improved ED services & facilities • Changing (& variable) admission thresholds • Inpatient bed availability • Repeat attendees • Local behaviours Inpatient • Bed availability • Advances in medical technology • Discharge planning Community • Family & community support • Relationship with primary care • Primary care capability & capacity • Aged residential care capability & capacity Patients – changing: demographics – two broad segments – young adult & elderly morbidity – more chronic illness expectations – more “consumerism” + a “medicalised” population more self-referral, but people confused about where to go 22

Better, sooner, more convenient Through a consumer’s eyes……. . 23

Better, sooner, more convenient 24

Better, sooner, more convenient Do we have a problem? Growth - reducing the national growth will require a focus on • metropolitan Auckland, • the elderly, • Maori and Pacific populations Variation between DHBs = an improvement opportunity. Reducing this requires • good comparative data • clinical engagement • an understanding of local initiatives/patterns of behaviour/admission thresholds • capability & capacity – particularly in community settings ……and what about variation within DHBs? 25
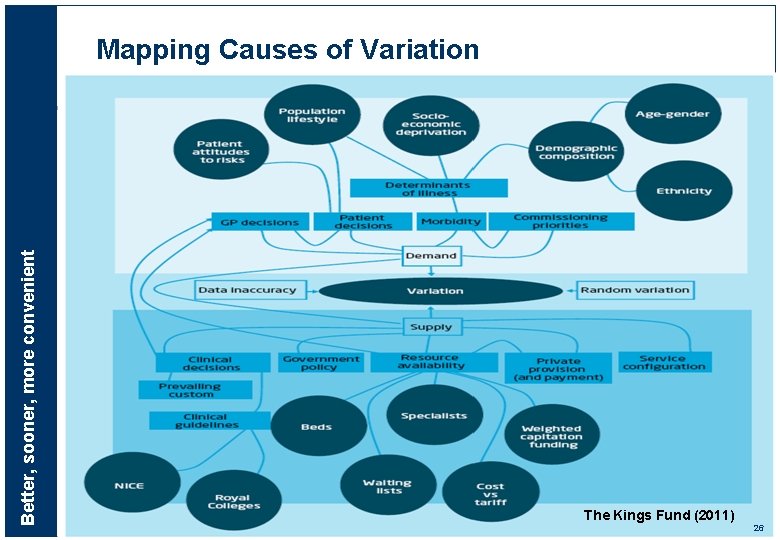
Better, sooner, more convenient Mapping Causes of Variation The Kings Fund (2011) 26

Useful resources Basu A, Brinson D (2008) The Effectiveness of Interventions for Reducing Ambulatory Sensitive Hospitalisations: A Systematic Review. HSAC Report Blunt I, Bardsley M, Dixon J (2010) Trends in Emergency Admissions in England 2004 – 2009. Nuffield Trust Better, sooner, more convenient Blunt I, Bardsley M, Dixon J (2010) Trends in Emergency Admissions in England 2004 – 2009: is greater efficiency breeding inefficiency? . Nuffield Trust Booz, Allen, Hamilton (2007) Key Drivers of Demand in the Emergency Department. NSW Department of Health Curry N, Ham C (2010) Clinical and Service Integration, the route to improved outcomes. The Kings Fund Ham C, Imison C, Jennings M (2010) Avoiding hospital admissions, lessons from evidence and experience. The Kings Fund NZHTA Report 8 (1998) Emergency Department Attendance a critical appraisal of the key literature. New Zealand Health Technology Assessment, University of Otago Purdy S (2010) Avoiding Hospital Admissions, what does the research evidence say? The Kings Fund Appleby J, Raleigh V, Frosini F, Bevan G, Gao H, Lyscom T (2011) Variations in Health Care, the good, the bad and the inexplicable. The Kings Fund 27

Better, sooner, more convenient Appendix 28
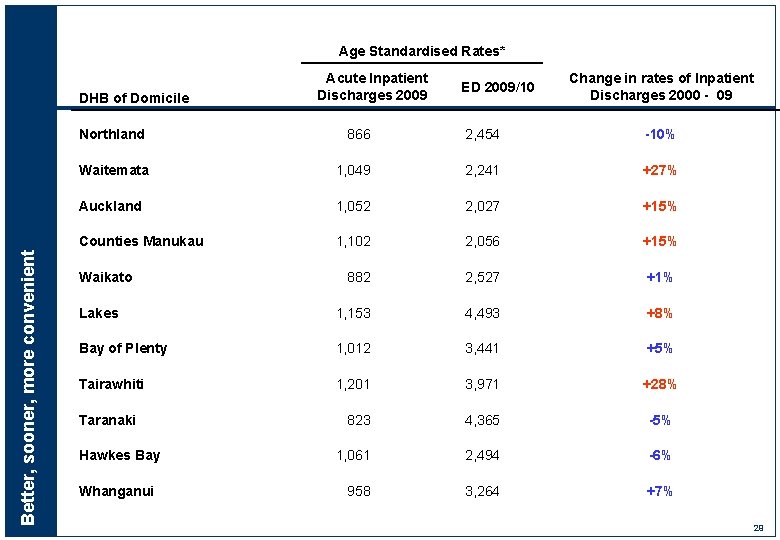
Age Standardised Rates* Better, sooner, more convenient DHB of Domicile Acute Inpatient Discharges 2009 ED 2009/10 Change in rates of Inpatient Discharges 2000 - 09 Northland 866 2, 454 -10% Waitemata 1, 049 2, 241 +27% Auckland 1, 052 2, 027 +15% Counties Manukau 1, 102 2, 056 +15% 882 2, 527 +1% Lakes 1, 153 4, 493 +8% Bay of Plenty 1, 012 3, 441 +5% Tairawhiti 1, 201 3, 971 +28% 823 4, 365 -5% 1, 061 2, 494 -6% 958 3, 264 +7% Waikato Taranaki Hawkes Bay Whanganui 29
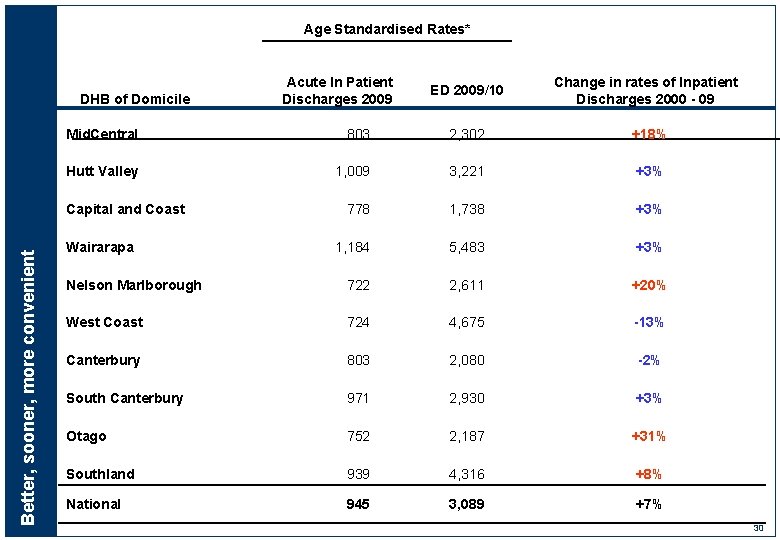
Age Standardised Rates* DHB of Domicile ED 2009/10 Change in rates of Inpatient Discharges 2000 - 09 Mid. Central 803 2, 302 +18% Hutt Valley 1, 009 3, 221 +3% 778 1, 738 +3% 1, 184 5, 483 +3% Nelson Marlborough 722 2, 611 +20% West Coast 724 4, 675 -13% Canterbury 803 2, 080 -2% South Canterbury 971 2, 930 +3% Otago 752 2, 187 +31% Southland 939 4, 316 +8% National 945 3, 089 +7% Capital and Coast Better, sooner, more convenient Acute In Patient Discharges 2009 Wairarapa 30
- Slides: 30