Acute Community Acquired Pneumonia Babak Sayad Associate Professor

Acute Community Acquired Pneumonia Babak Sayad Associate Professor of Infectious Diseases Department of Infectious Diseases Kermanshah University of Medical Science (KUMS)

Introduction n n In 1901, Sir William Osler' noted in the fourth edition of his book, The Principles and Practice of Medicine, that "the most widespread and fatal of all acute diseases, pneumonia, is now Captain of the Men of Death“ Over a century later, the prominence of pneumonia a same clinical entity remains

Introduction n n It remains among the top 10 most common causes of death among all age groups in the United States It is the single most common cause of infection-related mortality

When we think about pneumonia ? n Respiratory finding: n n n Cough Sputum Dyspnea Takypnea Positive chest physical exam Non-Respiratory finding: n n n Fever Fatigue Sweating Headache Nausea Myalgia

Clinical evaluation n History n The history should attempt to define: (1) symptoms consistent with the diagnosis of pneumonia n (2) the clinical setting in which the pneumonia takes place n (3) defects in host defense that could predispose to the development of pneumonia n (4) possible exposures to specific pathogens n

Clinical evaluation n History n n n n Age Site of acquisition Season Geographic location Contact history Animal contact Travel history Occupational history Habits Drug history Socioeconomic status Concomitant diseases Rice Presentation of disease

Clinical evaluation n Physical Examination n n Vital signs Respiratory distress n n n Cyanosis Rapid respiratory rate Use of accessory muscles Sternal retraction Nasal flaring Chest exam n n n Splinting Rales Evidence of consolidation (dullness on percussion, bronchial breath sounds, and E to A changes)

Clinical evaluation n Physical Examination n Specific keys: Furuncle n Herpes labialis n Bullous myringitis n Splenomegaly n Track marks n Poor dentition n

Pneumonia syndromes n n Acute Community Acquired Pneumonia Nasocomial Pneumonia Aspiration Pneumonia …

Acute Community Acquired Pneumonia n Typical presentation: n n n Sudden fever Productive cough Chest pain Consolidation Atypical presentation: n n Slow manifestation Non-Productive cough Extrapulmonary manifestation CXR abnormality

Differential diagnosis n n n n Acute tracheobronchitis Exacerbation of COPD Pleurisy Lung abscess Malignancy Pulmonary emboli & infarction Systemic diseases: n n Wegner PAN SLE …

Diagnostic Testing n n n n Radiologic Examination Sputum Examination Blood Culture Examination of Pleural Effusions Serologic Studies Urine Studies, Including Antigen Detection Fiberoptic Bronchoscopy Lung Biopsy
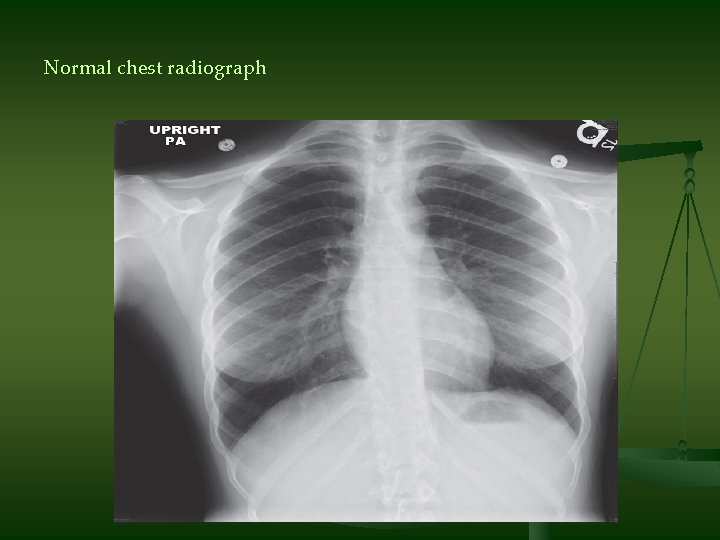
Normal chest radiograph
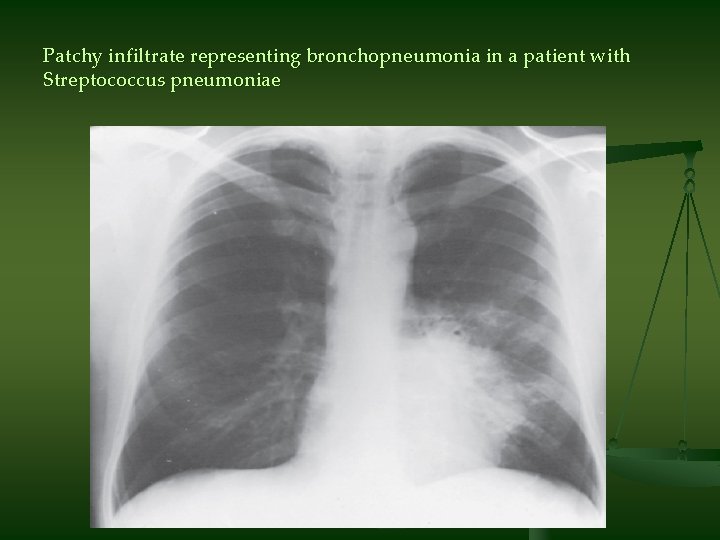
Patchy infiltrate representing bronchopneumonia in a patient with Streptococcus pneumoniae
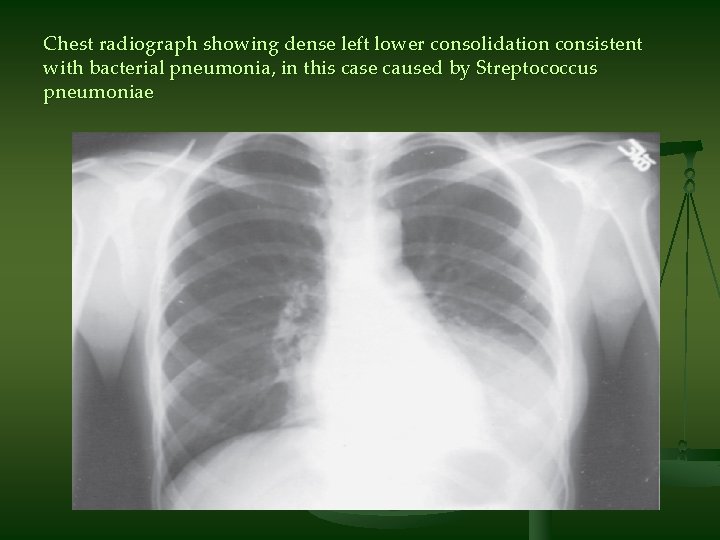
Chest radiograph showing dense left lower consolidation consistent with bacterial pneumonia, in this case caused by Streptococcus pneumoniae
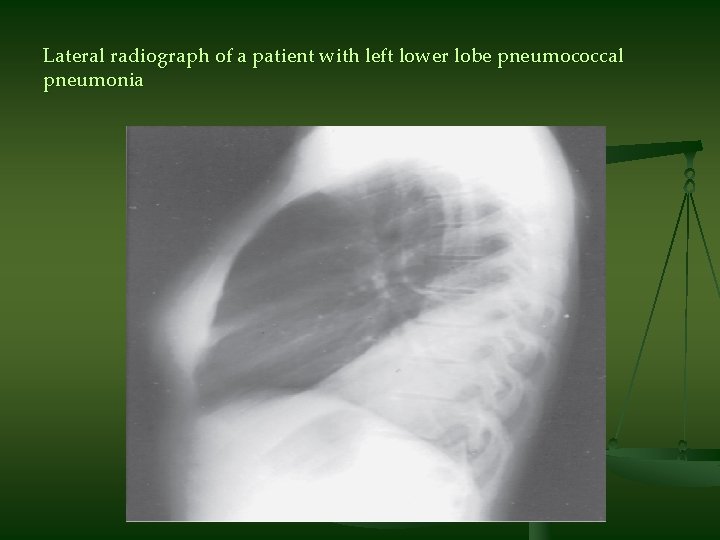
Lateral radiograph of a patient with left lower lobe pneumococcal pneumonia
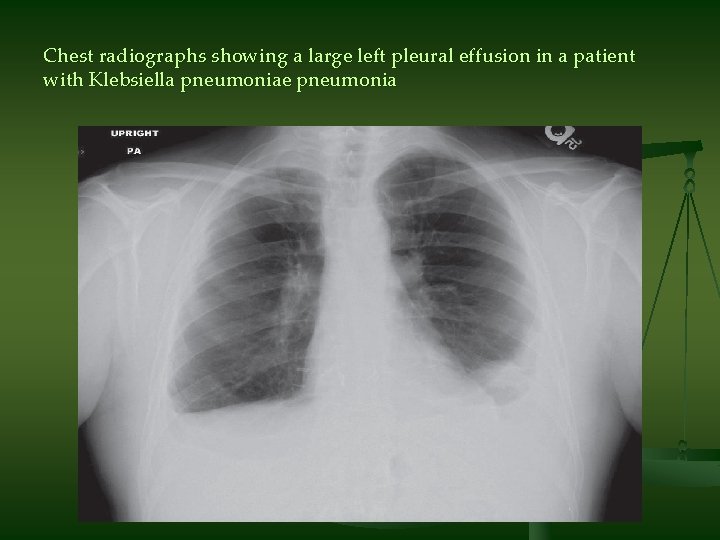
Chest radiographs showing a large left pleural effusion in a patient with Klebsiella pneumoniae pneumonia
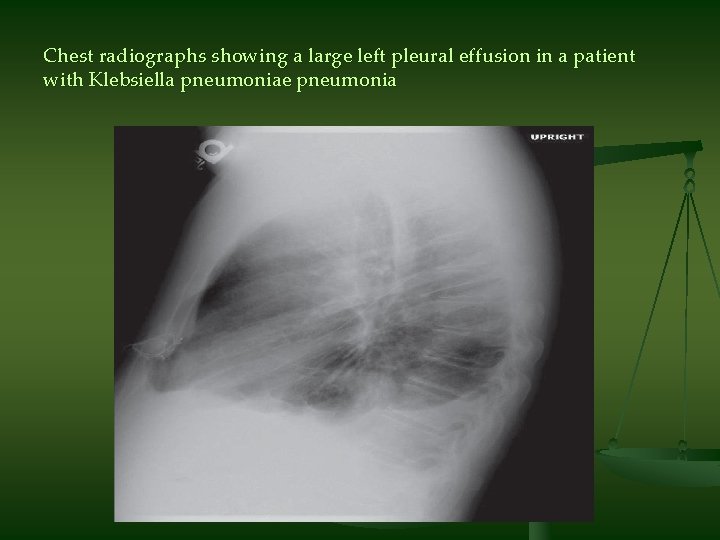
Chest radiographs showing a large left pleural effusion in a patient with Klebsiella pneumoniae pneumonia
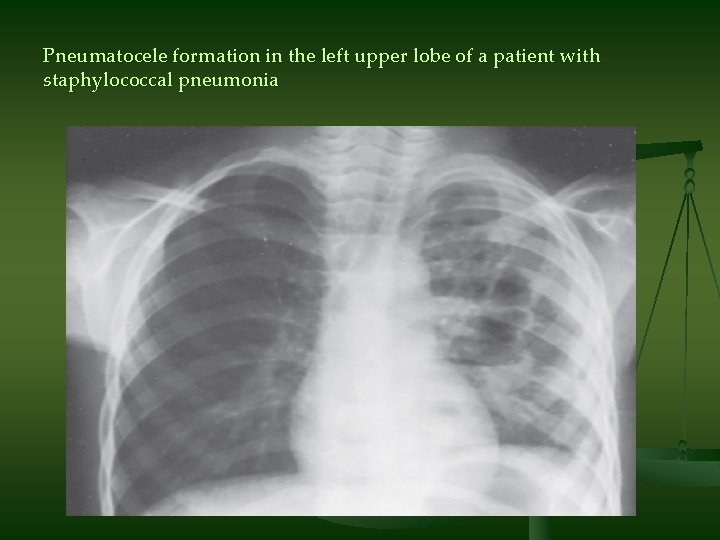
Pneumatocele formation in the left upper lobe of a patient with staphylococcal pneumonia
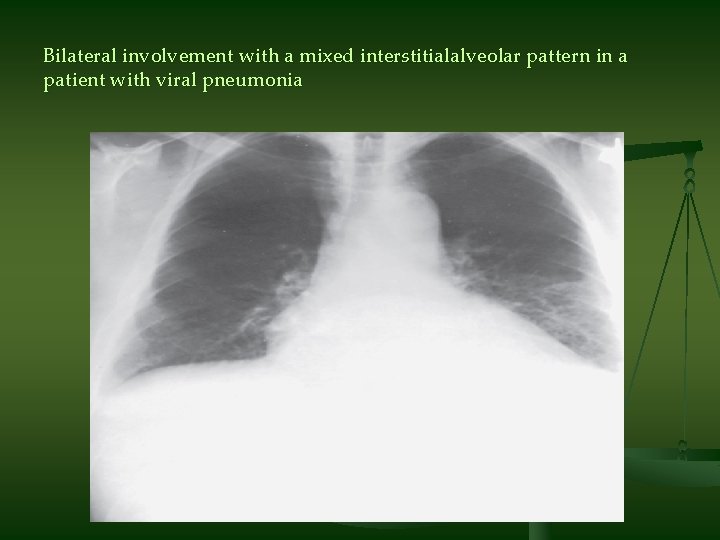
Bilateral involvement with a mixed interstitialalveolar pattern in a patient with viral pneumonia
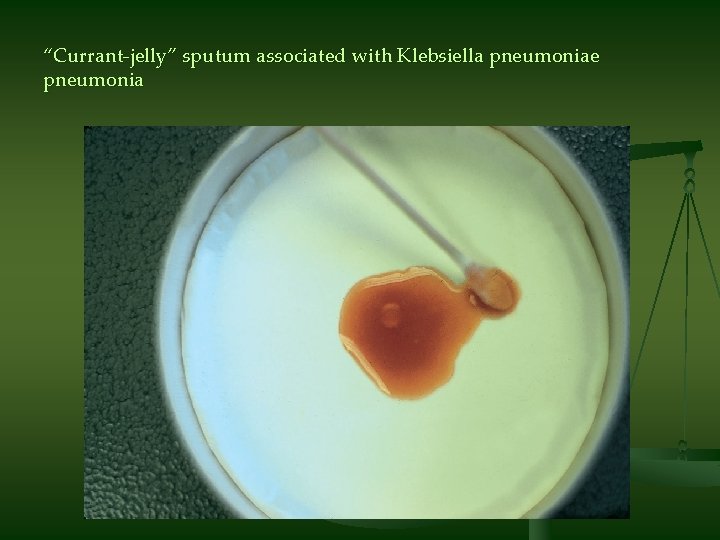
“Currant-jelly” sputum associated with Klebsiella pneumoniae pneumonia
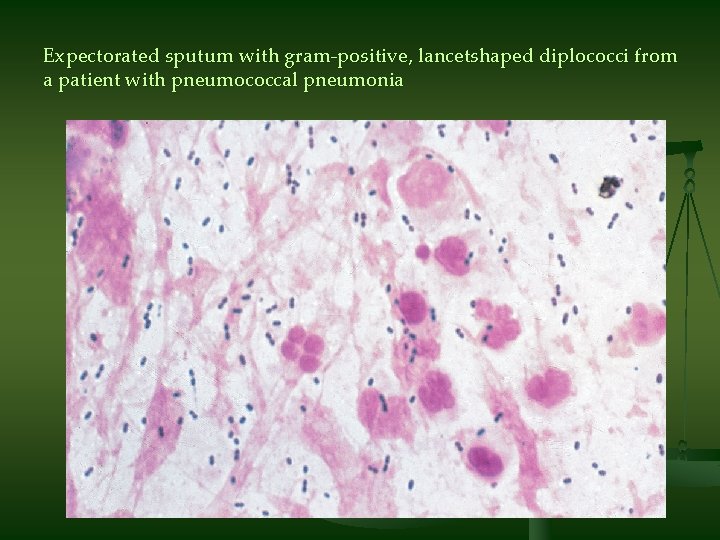
Expectorated sputum with gram-positive, lancetshaped diplococci from a patient with pneumococcal pneumonia
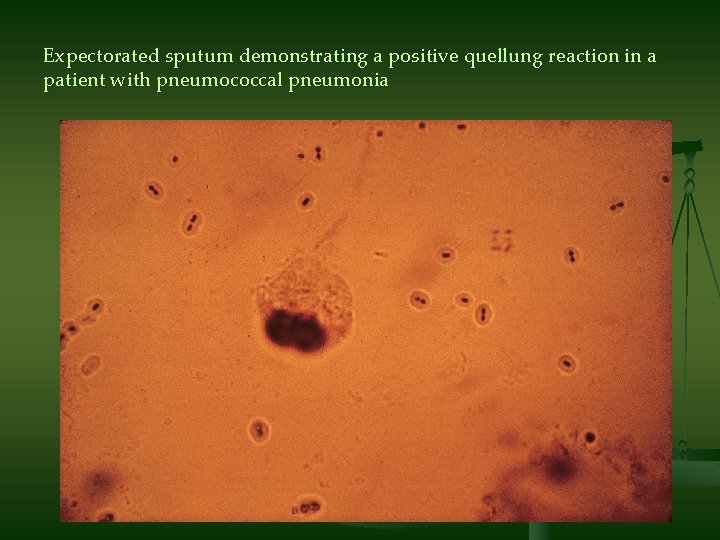
Expectorated sputum demonstrating a positive quellung reaction in a patient with pneumococcal pneumonia
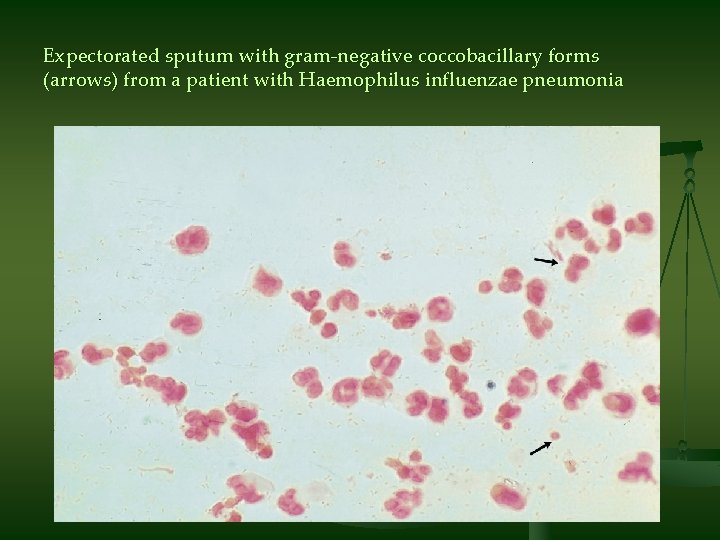
Expectorated sputum with gram-negative coccobacillary forms (arrows) from a patient with Haemophilus influenzae pneumonia
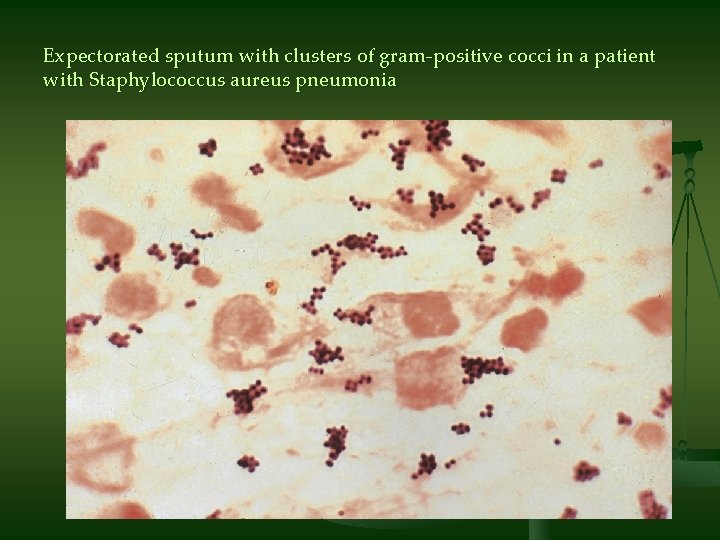
Expectorated sputum with clusters of gram-positive cocci in a patient with Staphylococcus aureus pneumonia
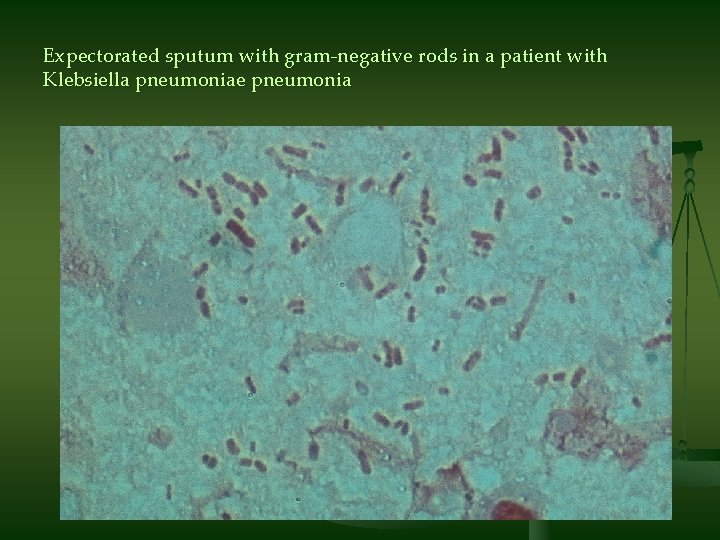
Expectorated sputum with gram-negative rods in a patient with Klebsiella pneumoniae pneumonia
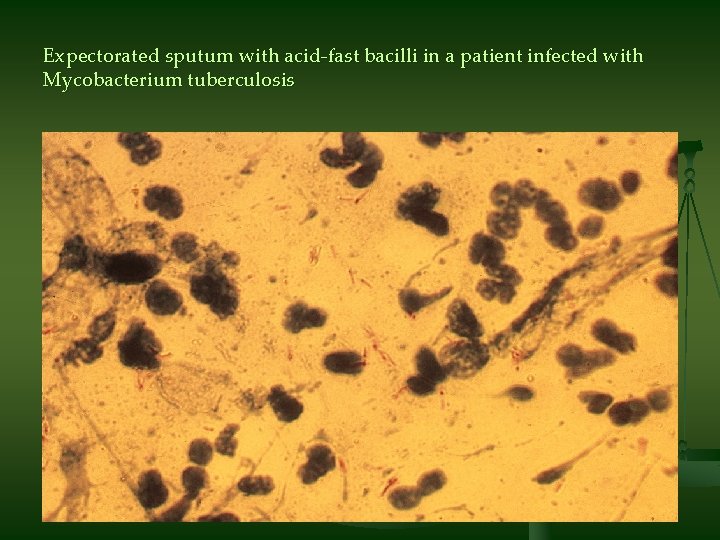
Expectorated sputum with acid-fast bacilli in a patient infected with Mycobacterium tuberculosis

Management n n 1 -The first decision confronting the clinician is whether the patient presenting with respiratory symptoms in fact has pneumonia. 2 -The next decision is whether the patient is to be hospitalized or out patient treatment 3 -The next problem is determining the most likely cause of pneumonia. 4 -Empirical Antibiotic Therapy

Management n The patient in fact has pneumonia: n Clinical evaluation History n Physical Examination n

Management n The patient is to be hospitalized or out patient treatment: n PORT score (Patient Outcome Research. Team) or Pneumonia Severity Index (PSI) n CURB, CURB-65, CRB-65 n n n C: Confusion U: Urea> 7 mmol/L R: RR>30/min B: BPs<90 mm Hg or BPd<60 mm Hg 65: Age>65 Y

Management n The most likely cause of pneumonia: n Diagnostic Testing Radiologic Examination n Sputum Examination n Blood Culture n Examination of Pleural Effusions n Serologic Studies n Urine Studies, Including Antigen Detection n Fiberoptic Bronchoscopy n Lung Biopsy n

Management n Empirical Antibiotic Therapy For most patients, a specific diagnosis cannot be established with certainty before the onset of therapy. Selecting an empirical antibiotic regimen is a continuing clinical challenge n Recent controversies and questions have included when antibiotics should be started, how to determine the most appropriate antibiotics to use, and how long therapy should continue n

Management n Empirical Antibiotic Therapy n When antibiotics should be started? n In 2007, the Joint Commission suggested that antibiotics be started within 6 hours, even though no other data had been presented. The joint IDSA & ATS guidelines have suggested a more common sense approach that antibiotic treatment for pneumonia be started “as soon as possible” after the diagnosis is considered likely

Management n Empirical Antibiotic Therapy n How to determine the most appropriate antibiotics to use? n Outpatient Therapy n n n Previously Healthy Comorbidities Inpatient Therapy n n n Medical Ward Intensive Care Unit (ICU) Health Care–Associated Pneumonia

Management n Empirical Antibiotic Therapy n Outpatient Therapy n Previously Healthy n No recent antibiotic therapy n n Macrolide or doxycycline Recent antibiotic therapy n A respiratory fluoroquinolone alone, an advanced macrolide plus oral β-lactam

Management n Empirical Antibiotic Therapy n Outpatient Therapy n Comorbidities n n No recent antibiotic therapy n An advanced macrolide plus oral β-lactam or a respiratory fluoroquinolone Recent antibiotic therapy n A respiratory fluoroquinolone alone or an advanced macrolide plus a β -lactam Suspected aspiration with infection n Amoxicillin-clavulanate or clindamycin Influenza with bacterial superinfection n Vancomycin, linezolid, or other coverage for MRSA or CA-MRSA

Management n Empirical Antibiotic Therapy n Inpatient Therapy n Medical Ward n n No recent antibiotic therapy n A respiratory fluoroquinolone alone or an advanced macrolide plus an IV β -lactam Recent antibiotic therapy n An advanced macrolide plus an IV β -lactam, or a respiratory fluoroquinolone alone (regimen selected will depend on nature of recent antibiotic therapy)

Management n Empirical Antibiotic Therapy n Inpatient Therapy n Intensive Care Unit (ICU) n n Pseudomonas infection is not a concern n A β -lactam plus either an advanced macrolide or a respiratory fluoroquinolone Pseudomonas infection is not a concern but patient has a β-lactam allergy n A respiratory fluoroquinolone, with or without clindamycin

Management n Empirical Antibiotic Therapy n Inpatient Therapy n Intensive Care Unit (ICU) n n n … Pseudomonas infection is a concern(cystic fibrosis, impaired host defenses) n Either (1) an antipseudomonal β -lactam plus ciprolloxacin, or (2) an antipseudomonal agent plus an aminoglycoside plus a respiratory fluoroquinolone or a macrolide Pseudomonas infection is a concern but the patient has a β -lactam allergy n Aztreonam plus aminoglycoside plus a respiratory fluoroquinolone

Management n Empirical Antibiotic Therapy n Inpatient Therapy n Health carc-associated pneumonia n Either (1) an antipseudomonal β-lactam plus ciprofloxacin or levofloxacin or (2) an antipseudomonal agent plus an aminoglycoside plus a respiratory fluoroquinolone or a macrolide plus vancomycin or linezolid (for MRSA coverage)

Management n Empirical Antibiotic Therapy n How long therapy should continue? The classic 10 to 14 days of care is unsupported by evidence n Recent data suggest that clinical stability occurs more quickly, and therefore antibiotic therapy may be safely discontinued earlier n Less than 7 days and as short as 3 days are just as effective as any longer durations of therapy for mild to moderate pneumonia. n Oral antibiotic therapy is safe after clinical stability has been reached n

Management n Empirical Antibiotic Therapy n Adjunctive Therapy Critical illness-related corticosteroid insufficiency (CIRCI) has been associated with communityacquired pneumonia n Statins also possess anti-inflammatory properties n
- Slides: 42