Acute Abdomen Acute Abdomen l Anatomy review l

Acute Abdomen

Acute Abdomen l Anatomy review l Non-hemorrhagic abdominal pain l Gastrointestinal hemorrhage l Assessment l Management

Abdominal Anatomy Review
Abdominal Cavity l Superior border = diaphragm l Inferior border = pelvis l Posterior border = lumbar spine l Anterior border = muscular abdominal wall

Peritoneum Abdominal cavity lining l Double-walled structure l » Visceral peritoneum » Parietal peritoneum l Separates abdominal cavity into two parts » Peritoneal cavity » Retroperitoneal space

Primary GI Structures l Mouth/oral cavity » Lips, cheeks, gums, teeth, tongue l Pharynx » Portion of airway between nasal cavity and larynx
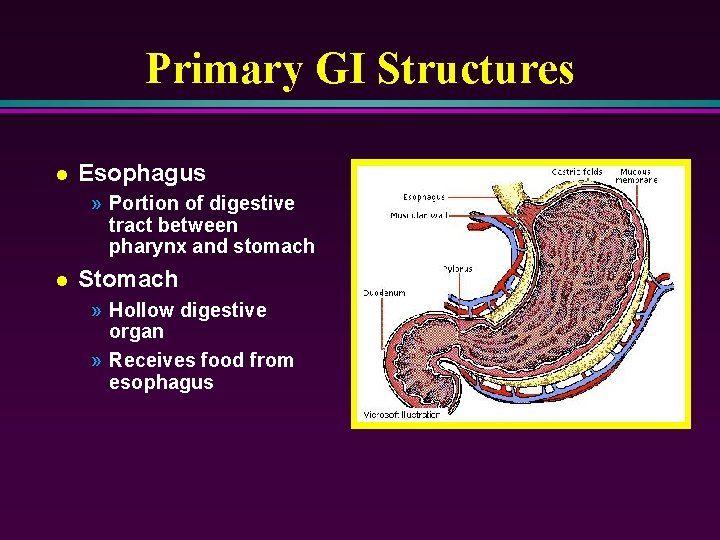
Primary GI Structures l Esophagus » Portion of digestive tract between pharynx and stomach l Stomach » Hollow digestive organ » Receives food from esophagus
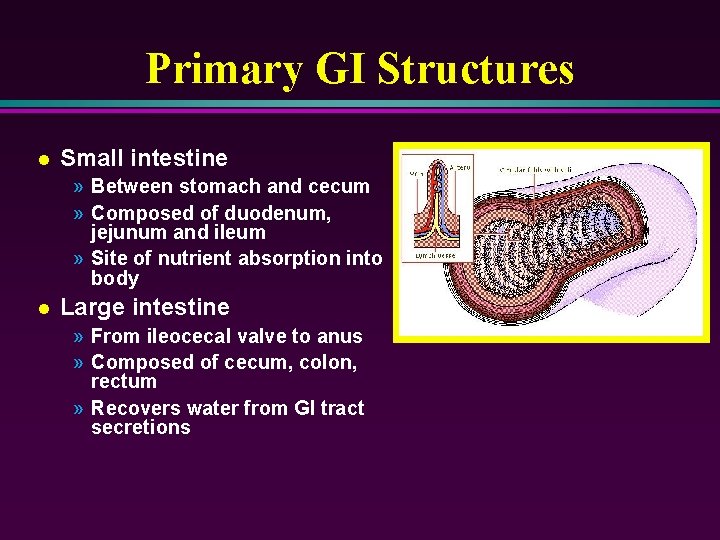
Primary GI Structures l Small intestine » Between stomach and cecum » Composed of duodenum, jejunum and ileum » Site of nutrient absorption into body l Large intestine » From ileocecal valve to anus » Composed of cecum, colon, rectum » Recovers water from GI tract secretions

Accessory GI Structures l Salivary glands » Produce, secrete saliva » Connect to mouth by ducts

Accessory GI Structures l Liver » Large solid organ in right upper quadrant » Produces, secretes bile » Produces essential proteins » Produces clotting factors » Detoxifies many substances » Stores glycogen l Gallbladder » Sac located beneath liver » Stores and concentrates bile

Accessory GI Structures l Pancreas » Endocrine pancreas secretes insulin into bloodstream » Exocrine pancreas secretes digestive enzymes, bicarbonate into gut l Vermiform appendix » Hollow appendage » Attached to large intestine » No physiologic function

Major Blood Vessels l Aorta l Inferior vena cava

Solid Organs l Liver l Spleen l Pancreas l Kidneys l Ovaries (female)

Hollow Organs l Stomach l Intestines l Gallbladder and bile ducts l Ureters l Urinary bladder l Uterus and Fallopian tubes (female)

Right Upper Quadrant l Liver l Gallbladder l Duodenum l Transverse colon (part) l Ascending colon (part)

Left Upper Quadrant: l Stomach l Liver (part) l Pancreas l Spleen l Transverse colon (part) l Descending colon (part)

Right Lower Quadrant l Ascending colon l Vermiform appendix l Ovary (female) l Fallopian tube (female)

Left Lower Quadrant l Descending colon l Sigmoid colon l Ovary (female) l Fallopian tube (female)

Acute Abdomen
Abdominal Pain l Visceral l Somatic l Referred
Abdominal Pain l Visceral pain » Stretching of peritoneum or organ capsules by distension or edema » Diffuse » Poorly localized » May be perceived at remote locations related to organ’s sensory innervation
Abdominal Pain l Somatic pain » Inflammation of parietal peritoneum or diaphragm » Sharp » Well-localized

Abdominal Pain l Referred pain » Perceived at distance from diseased organ » Pneumonia » Acute MI » Male GU problems

Non-hemorrhagic Abdominal Pain

Esophagitis l Inflammation of distal esophagus l Usually from gastric reflux, hiatal hernia

Esophagitis l Signs and Symptoms » Substernal burning pain, usually epigastric » Worsened by supine position » Usually without bleeding » Often temporarily relieved by nitroglycerin

Acute Gastroenteritis l Inflammation of stomach, intestine l May lead to bleeding, ulcers l Causes » acid secretion » Chronic Et. OH abuse » Biliary reflux » Medications (ASA, NSAIDS) » Infection

Acute Gastroenteritis l Signs and Symptoms » Epigastric pain, usually burning » Tenderness » Nausea, vomiting » Diarrhea » Possible bleeding

Chronic Infectious Gastroenteritis l l l Long-term mucosal changes or permanent damage Due primarily to microbial infections (bacterial, viral, protozoal) Fecal-oral transmission More common in underdeveloped countries Nausea, vomiting, fever, diarrhea, abdominal pain, cramping, anorexia, lethargy Handwashing, BSI
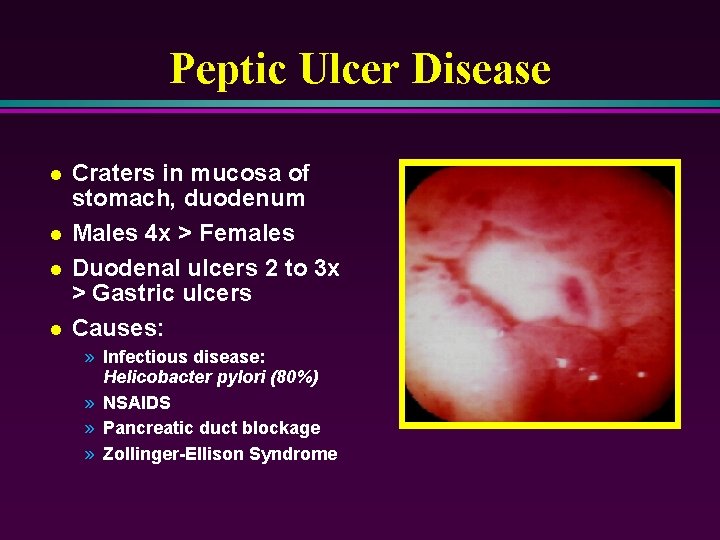
Peptic Ulcer Disease l l Craters in mucosa of stomach, duodenum Males 4 x > Females Duodenal ulcers 2 to 3 x > Gastric ulcers Causes: » Infectious disease: Helicobacter pylori (80%) » NSAIDS » Pancreatic duct blockage » Zollinger-Ellison Syndrome

Peptic Ulcer Disease l Duodenal Ulcers » 20 to 50 years old » High stress occupations » Genetic predisposition » Pain when stomach is empty » Pain at night l Gastric Ulcers » > 50 years old » Work at jobs requiring physical activity » Pain after eating or when stomach is full » Usually no pain at night

Peptic Ulcer Disease l Complications » Hemorrhage » Perforation, progressing to peritonitis » Scar tissue accumulation, progressing to obstruction

Peptic Ulcer Disease l Signs and Symptoms » Steady, well-localized pain » “Burning”, “gnawing”, “hot rock” » Relieved by bland, alkaline food/antacids » Worsened by smoking, coffee, stress, spicy foods » Stool changes, pallor associated with bleeding

Pancreatitis Inflammation of pancreas in which enzymes auto-digest gland l Causes include: l » Et. OH (80% of cases) » Gallstones obstructing ducts » Elevated serum triglycerides » Trauma » Viral, bacterial infections

Pancreatitis l May lead to: » Peritonitis » Pseudocyst formation » Hemorrhage » Necrosis » Secondary diabetes

Pancreatitis l Signs and Symptoms » Mid-epigastric pain radiating to back » Often worsened by food, Et. OH » Bluish flank discoloration (Grey-Turner Sign) » Bluish periumbilical discoloration (Cullen’s Sign) » Nausea, vomiting » Fever

Cholecystitis l l Gall bladder inflammation, usually 2 o to gallstones (90% of cases) Risk factors » Five Fs: Fat, Fertile, Febrile, Fortyish, Females » Heredity, diet, BCP use

Cholecystitis l Acalculus cholecystitis » Burns » Sepsis » Diabetes » Multiple organ systems failure l Chronic cholecystitis (bacterial infection)

Cholecystitis l Signs and Symptoms » Sudden pain, often severe, cramping » RUQ, radiating to right shoulder » Point tenderness under right costal margin (Murphy’s sign) » Nausea, vomiting » Often associated with fatty food intake » History of similar episodes in past » May be relieved by nitroglycerin
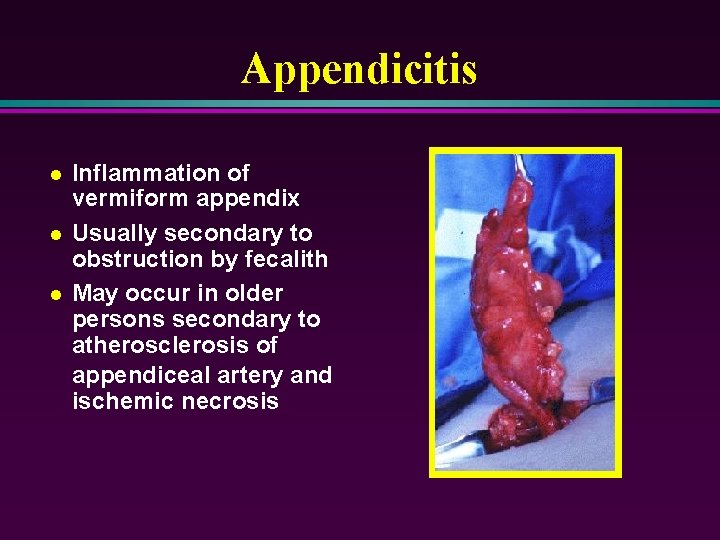
Appendicitis l l l Inflammation of vermiform appendix Usually secondary to obstruction by fecalith May occur in older persons secondary to atherosclerosis of appendiceal artery and ischemic necrosis

Appendicitis l Signs and Symptoms » Classic: Periumbilical pain RLQ pain/cramping » Nausea, vomiting, anorexia » Low-grade fever » Pain intensifies, localizes resulting in guarding » Patient on right side with right knee, hip flexed

Appendicitis l Signs and Symptoms » Mc. Burney’s Sign: Pain on palpation of RLQ » Aaron’s Sign: Epigastric pain on palpation of RLQ » Rovsing’s Sign: Pain in LLQ on palpation of RLQ » Psoas Sign: Pain when patient: – Extends right leg while lying on left side – Flexes legs while supine

Appendicitis l Signs and Symptoms » Unusual appendix position may lead to atypical presentations – Back pain – LLQ pain – “Cystitis” » Rupture: Temporary pain relief followed by peritonitis
Bowel Obstruction Blockage of intestine l Common Causes l » Adhesions (usually 2 o to surgery) » Hernias » Neoplasms » Volvulus » Intussuception » Impaction
Bowel Obstruction l Pathophysiology » Fluid, gas, air collect near obstruction site » Bowel distends, impeding blood flow/ halting absorption » Water, electrolytes collect in bowel lumen leading to hypovolemia » Bacteria form gas above obstruction further worsening distension » Distension extends proximally » Necrosis, perforation may occur
Bowel Obstruction l Signs and Symptoms » Severe, intermittent, “crampy” pain » High-pitched, “tinkling” bowel sounds » Abdominal distension » History of decreased frequency of bowel movements, semi-liquid stool, pencil-thin stools » Nausea, vomiting » ? Feces in vomitus

Hernia Protrusion of abdominal contents into groin (inguinal) or through diaphragm (hiatal) l Often secondary to intra-abdominal pressure (cough, lift, strain) l May progress to ischemic bowel (strangulated hernia) l

Hernia l Signs and Symptoms » Pain by abdominal pressure » Past history » Inguinal hernia may be palpable as mass in groin or scrotum

Crohn’s Disease Idiopathic inflammatory bowel disease l Occurs anywhere from mouth to rectum l 35 -45%: small intestine; 40%: colon l Runs in families l High risk groups l » White females » Jews » Persons under frequent stress

Crohn’s Disease l Pathophysiology » Mucosa of GI tract becomes inflamed » Granulomas form, invade submucosa » Muscular layer of bowel become fibrotic, hypertrophied » Increased risk develops for – Obstruction – Perforation – Hemorrhage

Ulcerative Colitis Idiopathic inflammatory bowel disease l Chronic ulcers develop in mucosal layer of colon l Spread to submucosal layer uncommon l 75% of cases involve rectum (proctitis) or rectosigmoid portion of large intestine l Inflammation can spread through entire large intestine (pancolitis) l

Ulcerative Colitis Severity of signs, symptoms depends on extent l Classic presentation l » Crampy abdominal pain » Nausea, vomiting » Blood diarrhea or stool containing mucus l Ischemic damage with perforation may occur
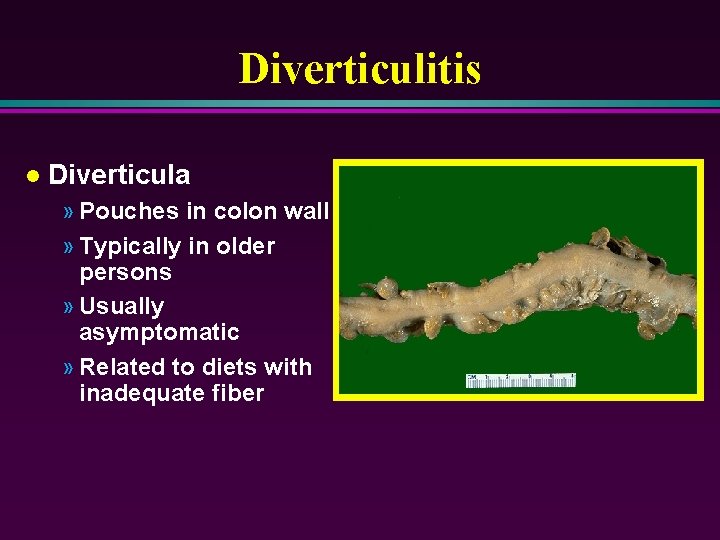
Diverticulitis l Diverticula » Pouches in colon wall » Typically in older persons » Usually asymptomatic » Related to diets with inadequate fiber

Diverticulitis Diverticula trap feces, become inflamed l Occasionally result in bright red rectal bleeding l Rupture may cause peritonitis, sepsis l

Diverticulitis l Signs and Symptoms » Usually left-sided pain » May localize to LLQ (“left-sided appendicitis”) » Alternating constipation, diarrhea » Bright red blood in stool

Hemorrhoids Small masses of veins in anus, rectum l Most frequently develop when patients are in 30 s or 40 s; common past 50 l Most are idiopathic, can be associated with pregnancy, portal hypertension l Cause bright red bleeding, pain on defecation l May become infected, inflamed l

Peritonitis l Inflammation of abdominal cavity lining l Signs and Symptoms » Generalized pain, tenderness » Abdominal rigidity » Nausea, vomiting » Absent bowel sounds » Patient resistant to movement

Hemorrhagic Abdominal Problems Gastrointestinal Hemorrhage Intraabdominal Hemorrhage
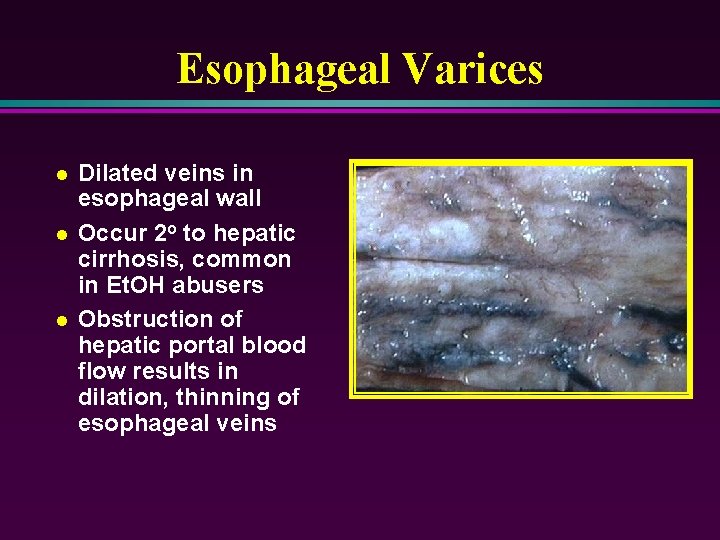
Esophageal Varices l l l Dilated veins in esophageal wall Occur 2 o to hepatic cirrhosis, common in Et. OH abusers Obstruction of hepatic portal blood flow results in dilation, thinning of esophageal veins
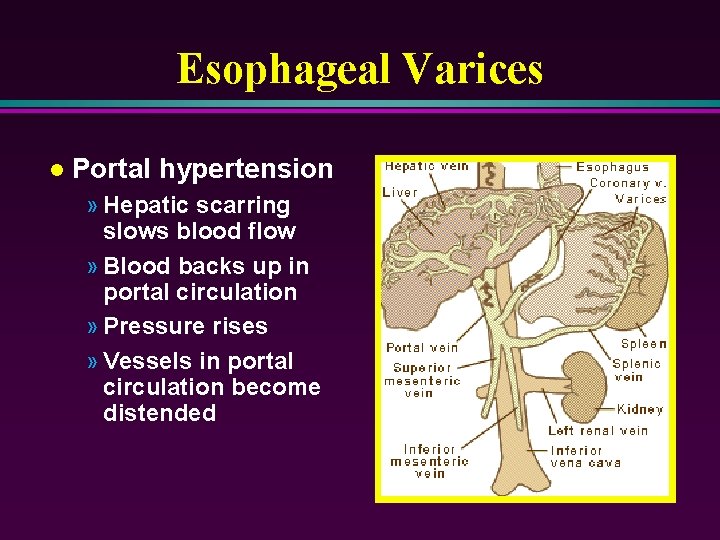
Esophageal Varices l Portal hypertension » Hepatic scarring slows blood flow » Blood backs up in portal circulation » Pressure rises » Vessels in portal circulation become distended

Esophageal Varices l Signs and Symptoms » Hematemesis (usually bright red) » Nausea, vomiting » Evidence of hypovolemia » Melena (uncommon)
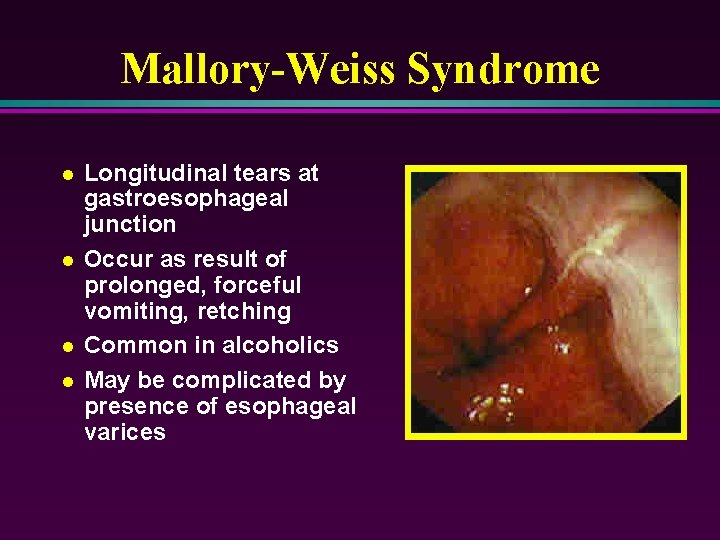
Mallory-Weiss Syndrome l l Longitudinal tears at gastroesophageal junction Occur as result of prolonged, forceful vomiting, retching Common in alcoholics May be complicated by presence of esophageal varices

Peptic Ulcer Disease l Ulcer erodes through blood vessel l Massive hematemesis l Melena may be present

Aortic Aneurysm Localized dilation due to weakening of aortic wall l Usually older patient with history of hypertension, atherosclerosis l May occur in younger patients secondary to » Trauma » Marfan’s syndrome l
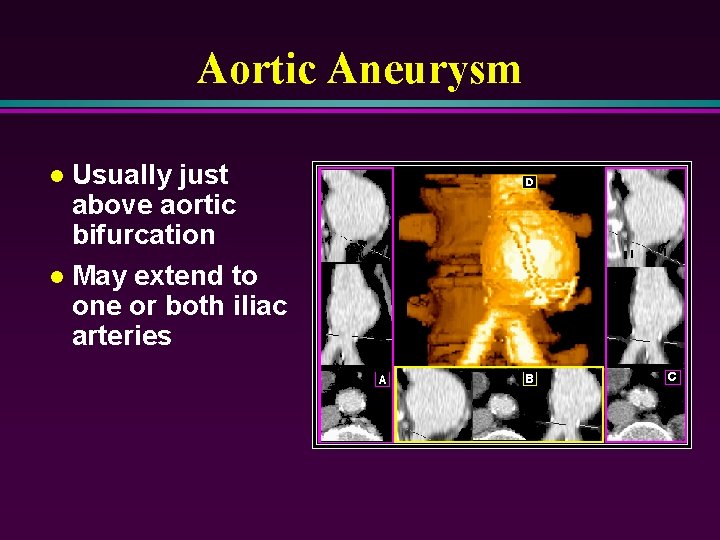
Aortic Aneurysm Usually just above aortic bifurcation l May extend to one or both iliac arteries l

Aortic Aneurysm l Signs and Symptoms » Unilateral lower quadrant pain; low back or leg pain » May be described as tearing or ripping » Pulsatile palpable mass usually above umbilicus » Diminished pulses in lower extremities » Unexplained syncope, often after BM » Evidence of hypovolemic shock
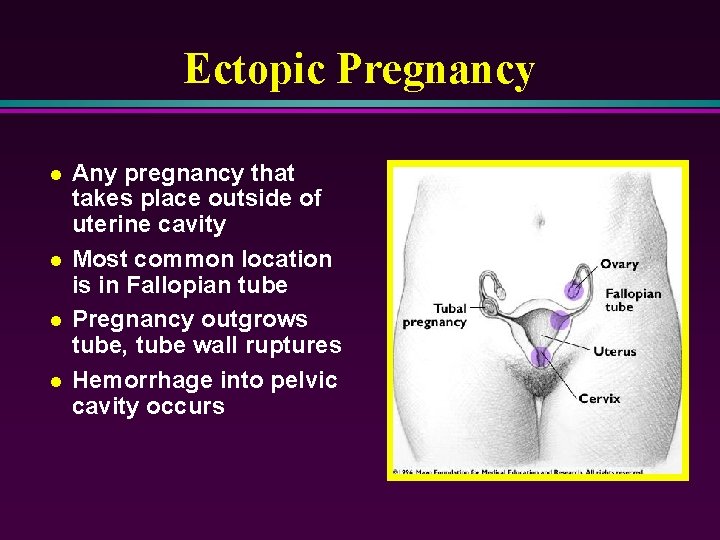
Ectopic Pregnancy l l Any pregnancy that takes place outside of uterine cavity Most common location is in Fallopian tube Pregnancy outgrows tube, tube wall ruptures Hemorrhage into pelvic cavity occurs

Ectopic Pregnancy l Suspect in females of child-bearing age with: » Abdominal pain, or » Unexplained shock l When was last normal menstrual period? Ectopic pregnancy does NOT necessarily cause missed period

Assessment of Acute Abdomen
History l Where do you hurt? » Try to point with one finger l What does pain feel like? » Steady pain = Inflammatory process » Cramping pain = Obstructive process l Onset of pain? » Sudden = Perforation or vascular occlusion » Gradual = Peritoneal irritation, distension of hollow organ

History l Does pain travel anywhere? » Gallbladder = Angle of right scapula » Pancreas = Straight through to back » Kidney/ureter = Around flank to groin » Heart = epigastrium, neck/jaw, shoulders, upper arms » Spleen = Left scapula, shoulder » Abdominal Aortic Aneurysm = low back radiating to one or both legs

History l How long have you been hurting? » >6 hours = increased probability of surgical significance l Nausea, vomiting » How much, How long? – Consider possible hypovolemia » Blood, coffee grounds? – Any blood in GI tract = emergency until proven otherwise

History l Urine » Change in urinary habits? – Frequency – Urgency » Color? » Odor?

History l Bowel movements » Change in bowel habits? Color? Odor? – Bright red blood – Melena = black, tarry, foul-smelling stool – Dark stool Suspect bleeding l Other causes possible (iron or bismuth containing materials) l

History l Last normal menstrual period? l Abnormal bleeding? l In females, lower abdominal pain = GYN problem until proven otherwise l In females of child-bearing age, lower abdominal pain = ectopic pregnancy until proven otherwise

Physical Exam l Position and General Appearance » Still, refusing to move = Inflammation, peritonitis » Extremely restless = Obstruction l Gross appearance of abdomen » Distended » Discolored » Consider possible third spacing of fluids

Physical Exam l Vital signs » Tachycardia = more important sign of volume loss than falling BP » Rapid, shallow breathing = possible peritonitis » Consider performing “tilt” test

Physical Exam l Bowel sounds » Auscultate BEFORE palpating » One minute in each abdominal quadrant » Absent sounds = possible peritonitis, shock » High-pitched, tinkling sounds = possible bowel obstruction

Physical Exam l Palpation » Palpate each quadrant » Palpate area of pain LAST » Do NOT check rebound tenderness in prehospital setting » ALL abdominal tenderness significant until proven otherwise

Management l Oxygen by non-rebreather mask l IV LR or NS l PASG (demonstrated benefit in intrabdominal hemorrhage) l Keep patient from losing body heat l Monitor vital signs

Management l Monitor EKG Consider possible MI with pain referred to abdomen in patients >30 years old Keep patient npo l Analgesia controversial l Demerol is preferred narcotic analgesic l
- Slides: 81