ACS and Acute MI Management How Did HORIZONS




![Primary Outcome Measures (ITT) Diff = -2. 9% [-4. 9, -0. 8] RR = Primary Outcome Measures (ITT) Diff = -2. 9% [-4. 9, -0. 8] RR =](https://slidetodoc.com/presentation_image_h/882b8165f01c472f1ac9da8c48652a1b/image-9.jpg)



- Slides: 27

ACS and Acute MI Management: How Did HORIZONS AMI Change MY Practice and Why? Roxana Mehran, MD Professor of Medicine (Cardiology), and Health Policy Director, Interventional Cardiovascular Research and Clinical Trials Mount Sinai School of Medicine

Roxana Mehran, MD §Institutional Grant/Research Support : § Bristol-Myers Squibb/Sanofi §The Medicines Company §Consulting Fees/Honoraria §Astra Zeneca, §Regado Biosciences, §Janssen

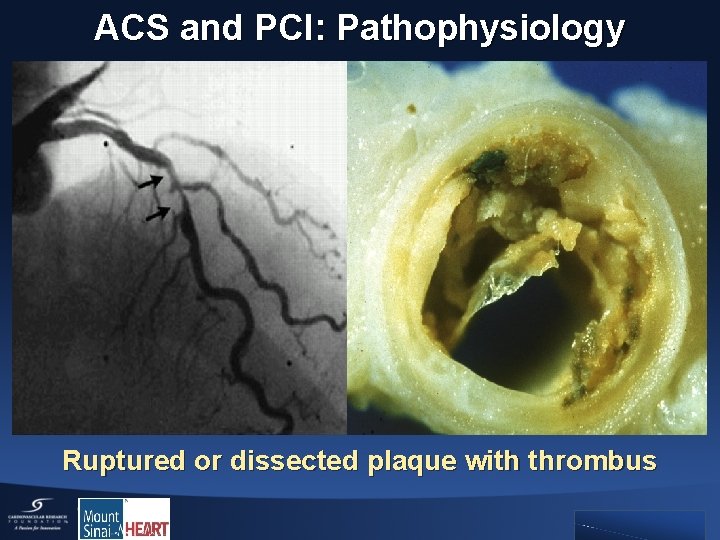
ACS and PCI: Pathophysiology Ruptured or dissected plaque with thrombus

STE/NSTE-ACS Primary PCI / Early Invasive Lytics / Early Conservative Aspirin loading Parenteral anticoagulant UFH Bolus / infusion LMWH Fondaparinux Bivalirudin Parenteral antiplatelet Abciximab Pre / post cath Eptifibatide Pre / post cath Tirofiban Pre / post cath Oral antiplatelet Clopidogrel 300 mg Pre / post cath Clopidogrel 600 mg Pre / post cath Prasugrel Pre / post cath ESC guidelines NSTE-ACS I-A, STE-ACS I-B Ticagrelor Pre / post cath 11 anti-thrombotic agents with 384 possible treatment combinations ESC = European Society of Cardiology, LMWH = low-molecular-weight heparin, UFH = unfractionated heparin. Bassand JP, et al. Eur Heart J. 2007; 28: 1598 -660. Van de Werf F, et al. Eur Heart J. 2008; 29: 2909 -45

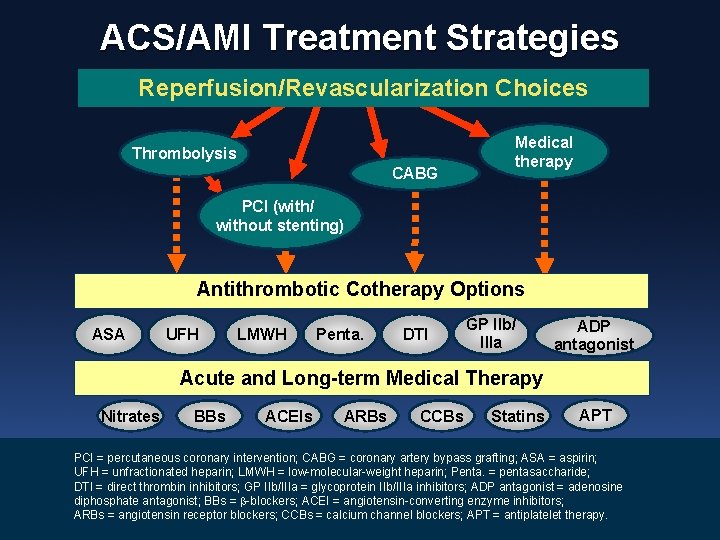
ACS/AMI Treatment Strategies Reperfusion/Revascularization Choices Thrombolysis CABG Medical therapy PCI (with/ without stenting) Antithrombotic Cotherapy Options ASA UFH LMWH Penta. DTI GP IIb/ IIIa ADP antagonist Acute and Long-term Medical Therapy Nitrates BBs ACEIs ARBs CCBs Statins APT PCI = percutaneous coronary intervention; CABG = coronary artery bypass grafting; ASA = aspirin; UFH = unfractionated heparin; LMWH = low-molecular-weight heparin; Penta. = pentasaccharide; DTI = direct thrombin inhibitors; GP IIb/IIIa = glycoprotein IIb/IIIa inhibitors; ADP antagonist = adenosine diphosphate antagonist; BBs = -blockers; ACEI = angiotensin-converting enzyme inhibitors; ARBs = angiotensin receptor blockers; CCBs = calcium channel blockers; APT = antiplatelet therapy.

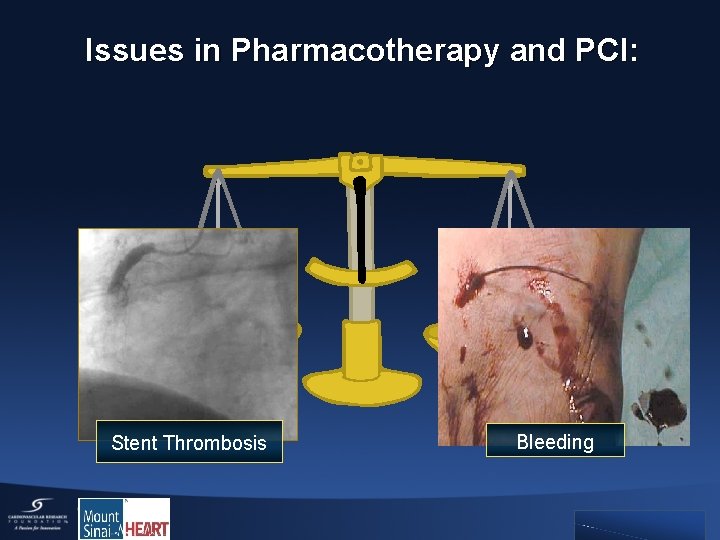
Issues in Pharmacotherapy and PCI: Stent Thrombosis bleeding Bleeding

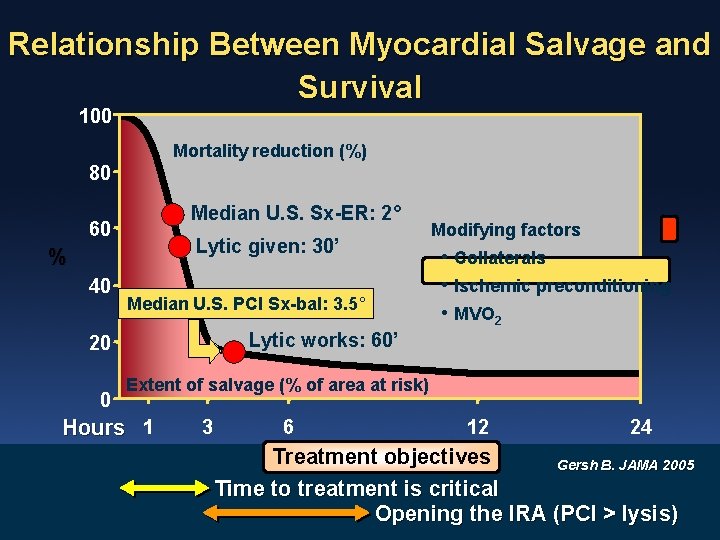
Relationship Between Myocardial Salvage and Survival 100 Mortality reduction (%) 80 Median U. S. Sx-ER: 2° 60 Lytic given: 30’ % 40 Median U. S. PCI Sx-bal: 3. 5° • Collaterals • Ischemic preconditioning • MVO 2 Lytic works: 60’ 20 0 Modifying factors Extent of salvage (% of area at risk) Hours 1 3 6 12 24 Treatment objectives Gersh B. JAMA 2005 Time to treatment is critical Opening the IRA (PCI > lysis)

Harmonizing Outcomes with Revascularization and Stents in AMI 3602 pts with STEMI with symptom onset ≤ 12 hours Aspirin, thienopyridine R 1: 1 UFH + GP IIb/IIIa inhibitor (abciximab or eptifibatide) Bivalirudin monotherapy (± provisional GP IIb/IIIa) Emergent angiography, followed by triage to… CABG – Primary PCI – Medical Rx 3006 pts eligible for stent randomization R 3: 1 Paclitaxel-eluting TAXUS stent Bare metal EXPRESS stent Clinical FU at 30 days, 6 months, 1 year, and then yearly through 5 years; angio FU at 13 months
![Primary Outcome Measures ITT Diff 2 9 4 9 0 8 RR Primary Outcome Measures (ITT) Diff = -2. 9% [-4. 9, -0. 8] RR =](https://slidetodoc.com/presentation_image_h/882b8165f01c472f1ac9da8c48652a1b/image-9.jpg)
Primary Outcome Measures (ITT) Diff = -2. 9% [-4. 9, -0. 8] RR = 0. 76 [0. 63, 0. 92] Diff = -3. 3% [-5. 0, -1. 6] RR = 0. 60 [0. 46, 0. 77] Diff = 0. 0% [-1. 6, 1. 5] RR = 0. 99 [0. 76, 1. 30] PNI ≤ 0. 0001 Psup = 0. 006 PNI ≤ 0. 0001 Psup = 1. 00 1 endpoint *Not related to CABG **MACE = All cause death, reinfarction, ischemic TVR or stroke

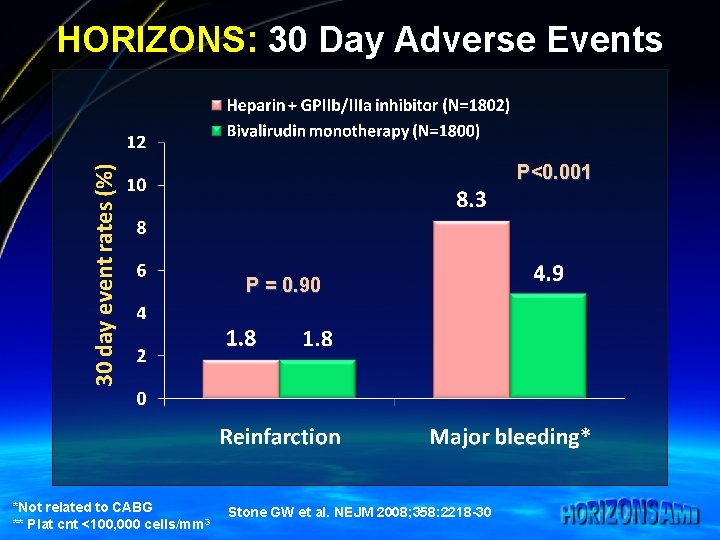
HORIZONS: 30 Day Adverse Events P<0. 001 P = 0. 90 *Not related to CABG ** Plat cnt <100, 000 cells/mm 3 Stone GW et al. NEJM 2008; 358: 2218 -30

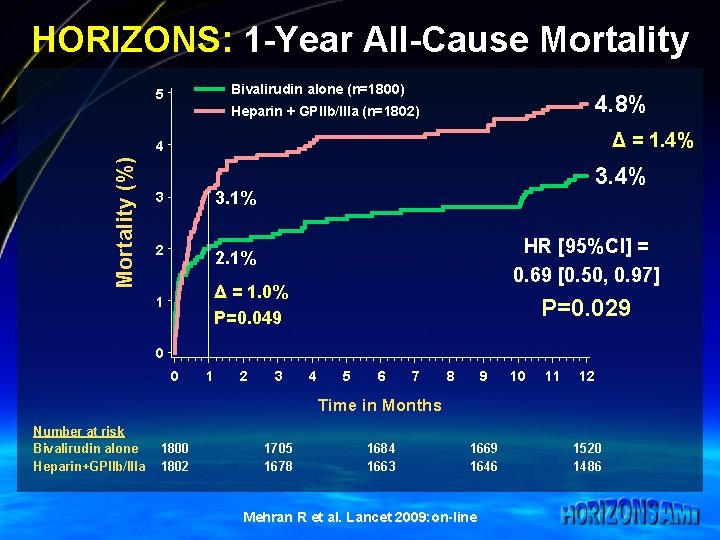
HORIZONS: 1 -Year All-Cause Mortality Bivalirudin alone (n=1800) 5 4. 8% Heparin + GPIIb/IIIa (n=1802) Δ = 1. 4% Mortality (%) 4 3 3. 1% 2 2. 1% 3. 4% HR [95%CI] = 0. 69 [0. 50, 0. 97] Δ = 1. 0% P=0. 049 1 P=0. 029 0 0 1 2 3 4 5 6 7 8 9 10 11 12 Time in Months Number at risk Bivalirudin alone Heparin+GPIIb/IIIa 1800 1802 1705 1678 1684 1663 1669 1646 Mehran R et al. Lancet 2009: on-line 1520 1486

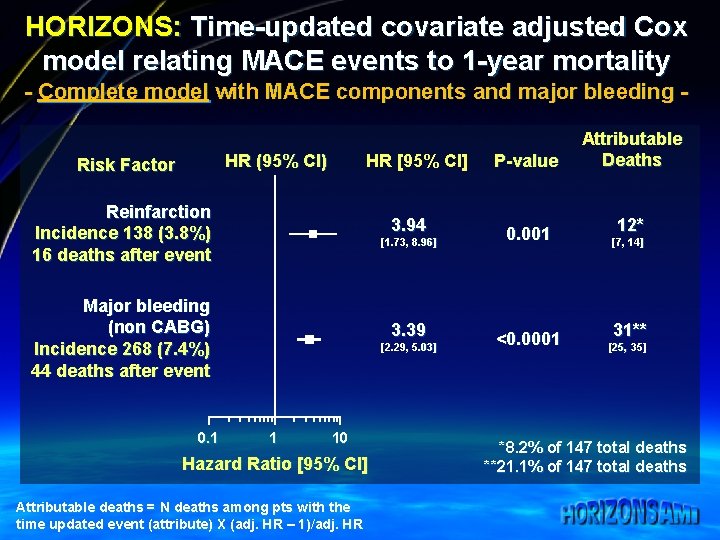
HORIZONS: Time-updated covariate adjusted Cox model relating MACE events to 1 -year mortality - Complete model with MACE components and major bleeding HR (95% CI) Risk Factor HR [95% CI] Reinfarction Incidence 138 (3. 8%) 16 deaths after event 3. 94 [1. 73, 8. 96] Major bleeding (non CABG) Incidence 268 (7. 4%) 44 deaths after event 0. 1 3. 39 [2. 29, 5. 03] 1 10 Hazard Ratio [95% CI] Attributable deaths = N deaths among pts with the time updated event (attribute) X (adj. HR – 1)/adj. HR P-value Attributable Deaths 0. 001 12* [7, 14] <0. 0001 [25, 35] 31** *8. 2% of 147 total deaths **21. 1% of 147 total deaths

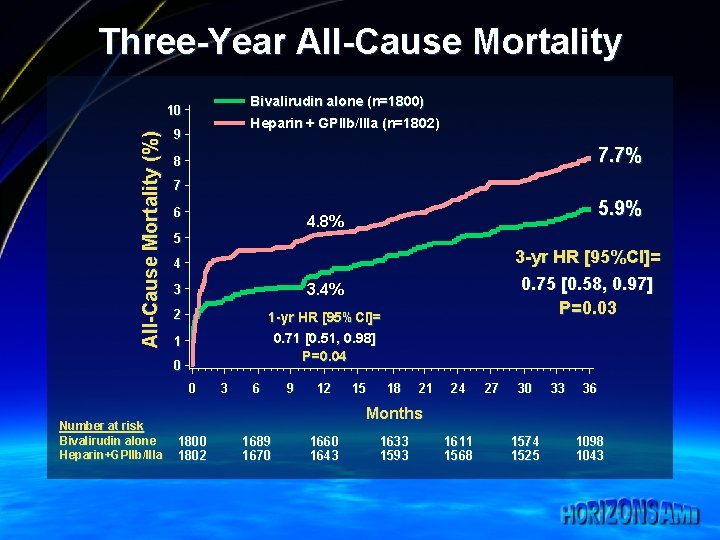
Three-Year All-Cause Mortality Bivalirudin alone (n=1800) All-Cause Mortality (%) 10 Heparin + GPIIb/IIIa (n=1802) 9 7. 7% 8 7 6 5 3 -yr HR [95%CI]= 0. 75 [0. 58, 0. 97] P=0. 03 4 3 3. 4% 2 1 -yr HR [95%CI]= 0. 71 [0. 51, 0. 98] P=0. 04 1 0 0 Number at risk Bivalirudin alone Heparin+GPIIb/IIIa 5. 9% 4. 8% 3 6 9 12 15 18 21 24 27 30 33 36 Months 1800 1802 1689 1670 1660 1643 1633 1593 1611 1568 1574 1525 1098 1043

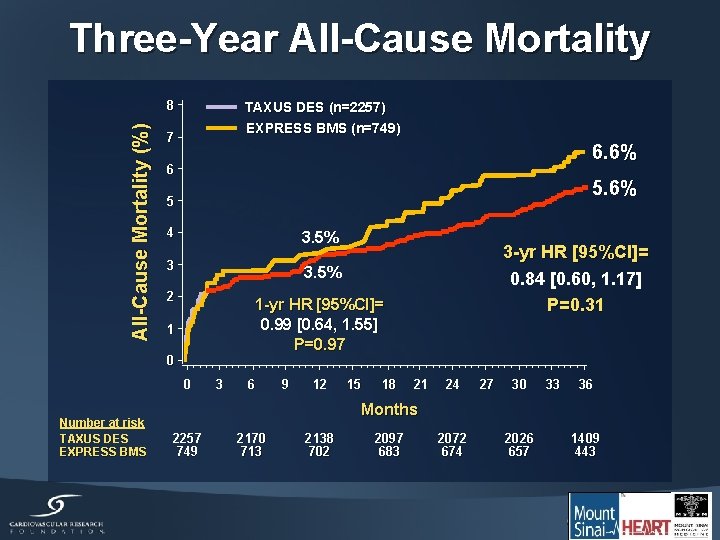
Three-Year All-Cause Mortality (%) 8 TAXUS DES (n=2257) EXPRESS BMS (n=749) 7 6. 6% 6 5. 6% 5 4 3. 5% 3 3. 5% 2 1 -yr HR [95%CI]= 0. 99 [0. 64, 1. 55] P=0. 97 1 0 0 Number at risk TAXUS DES EXPRESS BMS 3 6 9 12 15 18 3 -yr HR [95%CI]= 0. 84 [0. 60, 1. 17] P=0. 31 21 24 27 30 33 36 Months 2257 749 2170 713 2138 702 2097 683 2072 674 2026 657 1409 443

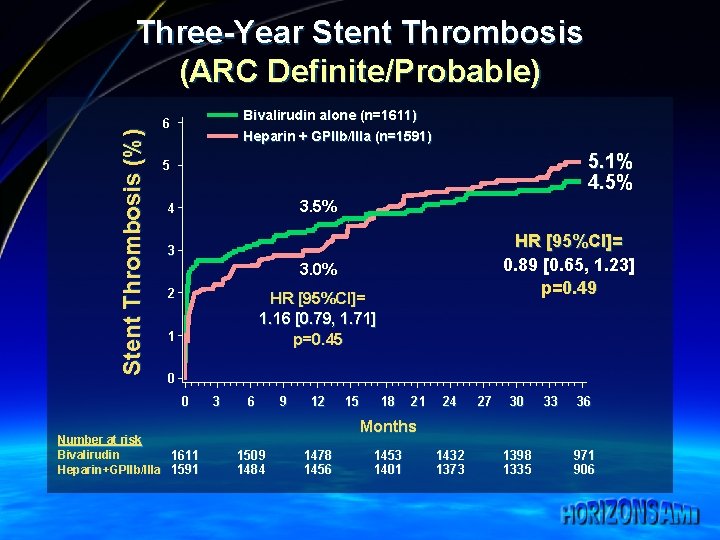
Stent Thrombosis (%) Three-Year Stent Thrombosis (ARC Definite/Probable) Bivalirudin alone (n=1611) 6 Heparin + GPIIb/IIIa (n=1591) 5. 1% 4. 5% 5 3. 5% 4 HR [95%CI]= 0. 89 [0. 65, 1. 23] p=0. 49 3 3. 0% 2 HR [95%CI]= 1. 16 [0. 79, 1. 71] p=0. 45 1 0 0 Number at risk Bivalirudin 1611 Heparin+GPIIb/IIIa 1591 3 6 9 12 15 18 21 24 27 30 33 36 Months 1509 1484 1478 1456 1453 1401 1432 1373 1398 1335 971 906

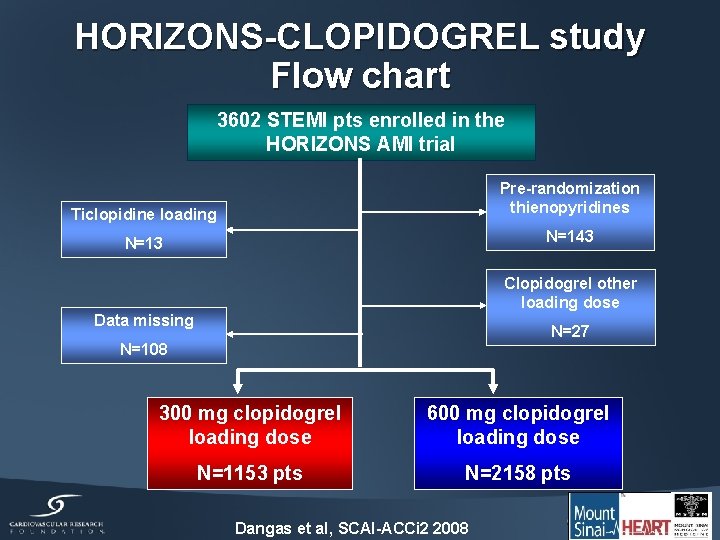
HORIZONS-CLOPIDOGREL study Flow chart 3602 STEMI pts enrolled in the HORIZONS AMI trial Ticlopidine loading Pre-randomization thienopyridines N=13 N=143 Clopidogrel other loading dose Data missing N=27 N=108 300 mg clopidogrel loading dose 600 mg clopidogrel loading dose N=1153 pts N=2158 pts Dangas et al, SCAI-ACCi 2 2008

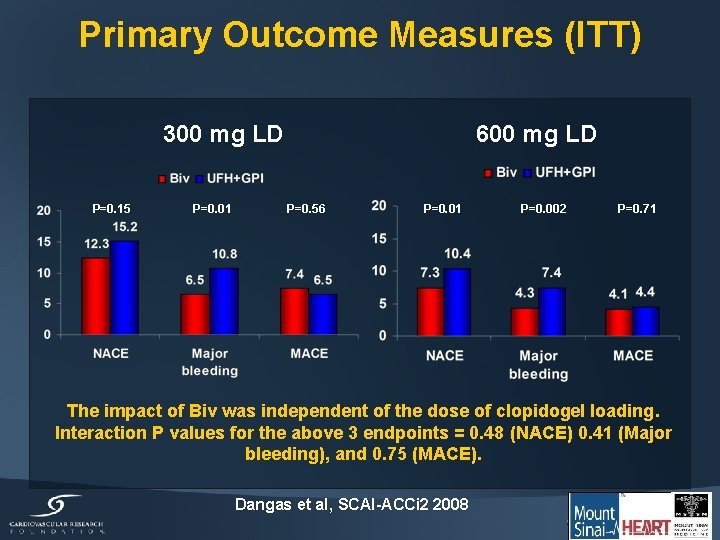
Primary Outcome Measures (ITT) 600 mg LD 300 mg LD P=0. 15 P=0. 01 P=0. 56 P=0. 01 P=0. 002 P=0. 71 The impact of Biv was independent of the dose of clopidogel loading. Interaction P values for the above 3 endpoints = 0. 48 (NACE) 0. 41 (Major bleeding), and 0. 75 (MACE). Dangas et al, SCAI-ACCi 2 2008

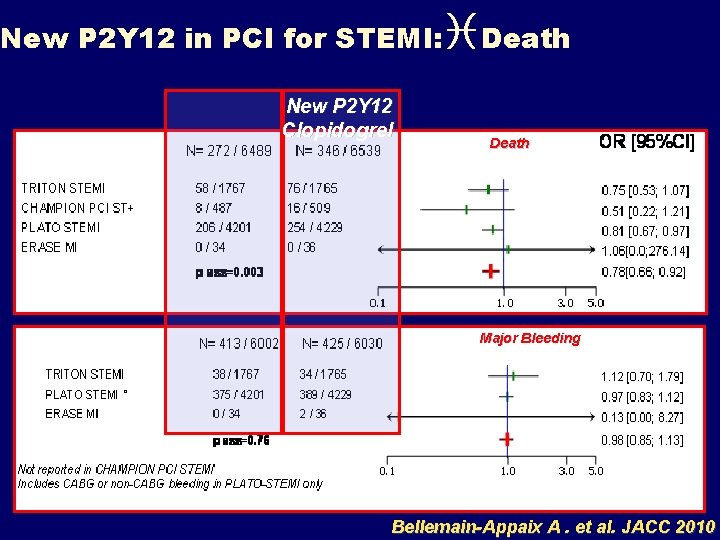
New P 2 Y 12 in PCI for STEMI: New P 2 Y 12 Clopidogrel i. Death Major Bleeding Bellemain-Appaix A. et al. JACC 2010

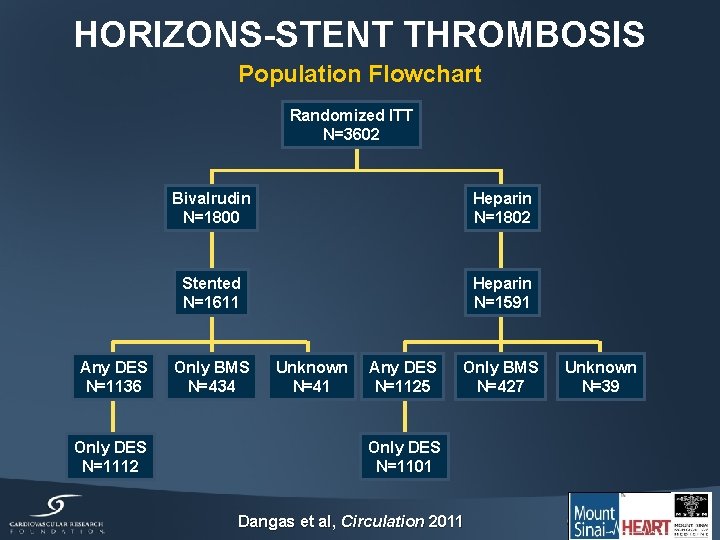
HORIZONS-STENT THROMBOSIS Population Flowchart Randomized ITT N=3602 Any DES N=1136 Only DES N=1112 Bivalrudin N=1800 Heparin N=1802 Stented N=1611 Heparin N=1591 Only BMS N=434 Unknown N=41 Any DES N=1125 Only BMS N=427 Only DES N=1101 Dangas et al, Circulation 2011 Unknown N=39

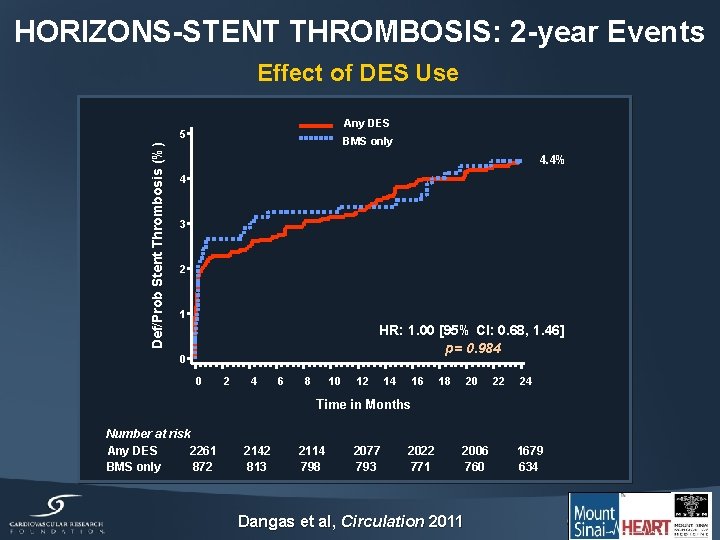
HORIZONS-STENT THROMBOSIS: 2 -year Events Effect of DES Use Any DES Def/Prob Stent Thrombosis (%) 5 BMS only 4. 4% 4 3 2 1 HR: 1. 00 [95% CI: 0. 68, 1. 46] p= 0. 984 0 0 2 4 6 8 10 12 14 16 18 20 22 24 Time in Months Number at risk Any DES 2261 BMS only 872 2142 813 2114 798 2077 793 2022 771 2006 760 Dangas et al, Circulation 2011 1679 634

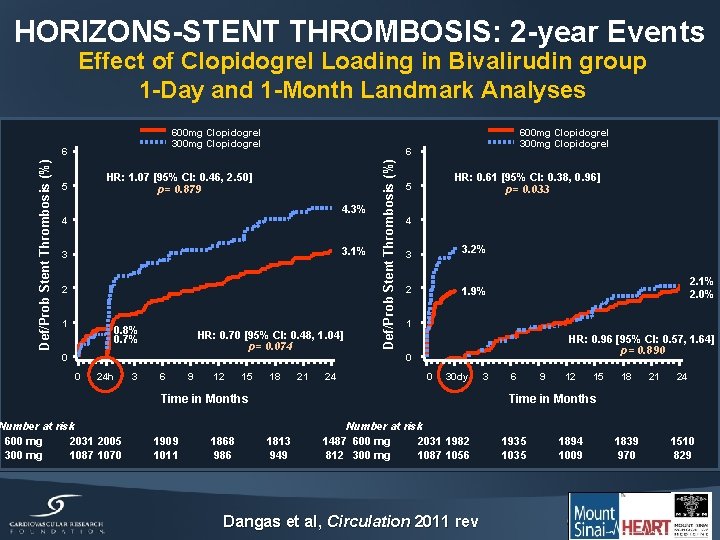
HORIZONS-STENT THROMBOSIS: 2 -year Events Effect of Clopidogrel Loading in Bivalirudin group 1 -Day and 1 -Month Landmark Analyses 600 mg Clopidogrel 300 mg Clopidogrel 6 HR: 1. 07 [95% CI: 0. 46, 2. 50] p= 0. 879 5 4. 3% 4 3. 1% 3 2 1 0. 8% 0. 7% HR: 0. 70 [95% CI: 0. 48, 1. 04] p= 0. 074 0 0 24 h Number at risk 600 mg 2031 2005 300 mg 1087 1070 3 6 9 12 15 18 21 24 Def/Prob Stent Thrombosis (%) 6 600 mg Clopidogrel 300 mg Clopidogrel HR: 0. 61 [95% CI: 0. 38, 0. 96] p= 0. 033 5 4 3. 2% 3 2 1 HR: 0. 96 [95% CI: 0. 57, 1. 64] p= 0. 890 0 0 30 dy Time in Months 1909 1011 1868 986 2. 1% 2. 0% 1. 9% 3 6 9 12 15 18 21 24 Time in Months 1813 949 Number at risk 1487 600 mg 2031 1982 812 300 mg 1087 1056 Dangas et al, Circulation 2011 rev 1935 1035 1894 1009 1839 970 1510 829

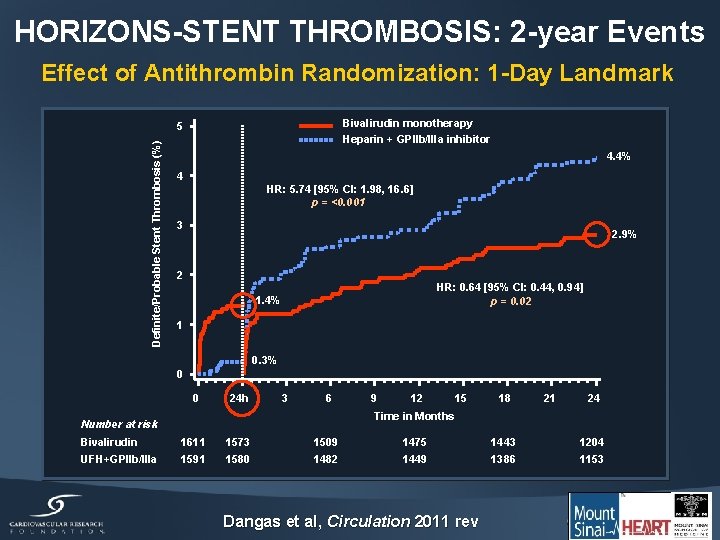
HORIZONS-STENT THROMBOSIS: 2 -year Events Effect of Antithrombin Randomization: 1 -Day Landmark Bivalirudin monotherapy Definite/Probable Stent Thrombosis (%) 5 Heparin + GPIIb/IIIa inhibitor 4. 4% 4 HR: 5. 74 [95% CI: 1. 98, 16. 6] p = <0. 001 3 2. 9% 2 HR: 0. 64 [95% CI: 0. 44, 0. 94] p = 0. 02 1. 4% 1 0. 3% 0 0 24 h 3 6 9 12 15 18 21 24 Time in Months Number at risk Bivalirudin 1611 1573 1509 1475 1443 1204 UFH+GPIIb/IIIa 1591 1580 1482 1449 1386 1153 Dangas et al, Circulation 2011 rev

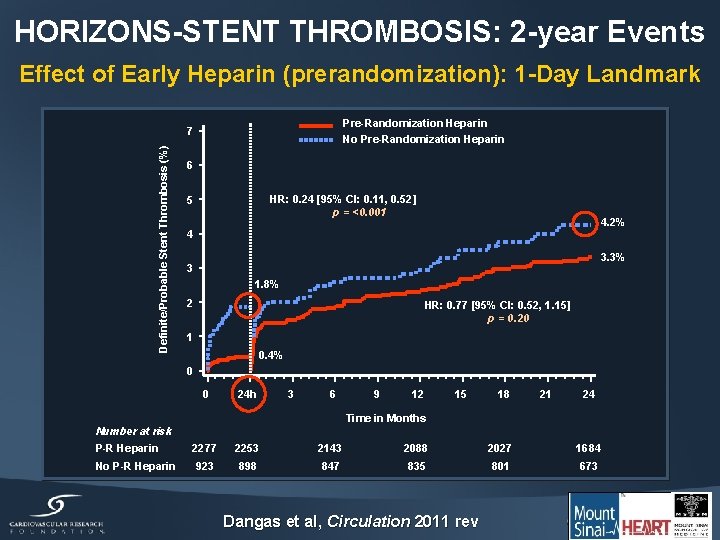
HORIZONS-STENT THROMBOSIS: 2 -year Events Effect of Early Heparin (prerandomization): 1 -Day Landmark Pre-Randomization Heparin Definite/Probable Stent Thrombosis (%) 7 No Pre-Randomization Heparin 6 HR: 0. 24 [95% CI: 0. 11, 0. 52] p = <0. 001 5 4. 2% 4 3. 3% 3 1. 8% 2 HR: 0. 77 [95% CI: 0. 52, 1. 15] p = 0. 20 1 0. 4% 0 0 24 h 3 6 9 12 15 18 21 24 Time in Months Number at risk P-R Heparin No P-R Heparin 2277 2253 2143 2088 2027 1684 923 898 847 835 801 673 Dangas et al, Circulation 2011 rev

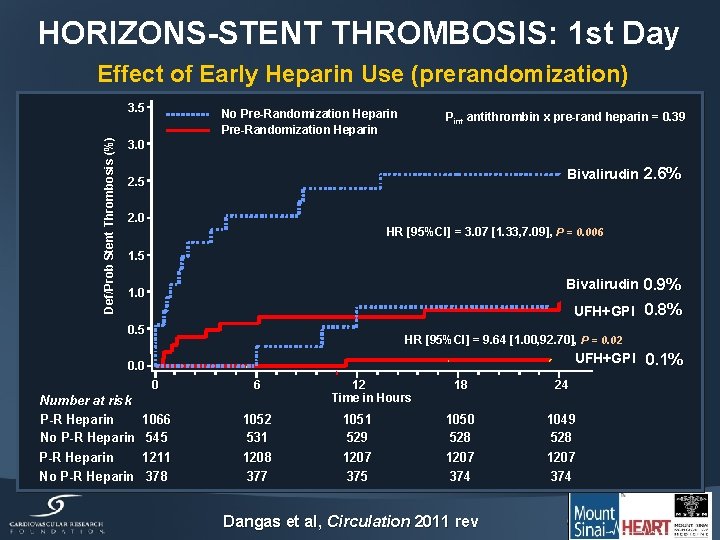
HORIZONS-STENT THROMBOSIS: 1 st Day Effect of Early Heparin Use (prerandomization) Def/Prob Stent Thrombosis (%) 3. 5 No Pre-Randomization Heparin Pint antithrombin x pre-rand heparin = 0. 39 3. 0 Bivalirudin 2. 6% 2. 5 2. 0 HR [95%CI] = 3. 07 [1. 33, 7. 09], P = 0. 006 1. 5 Bivalirudin 0. 9% 1. 0 UFH+GPI 0. 8% 0. 5 HR [95%CI] = 9. 64 [1. 00, 92. 70], P = 0. 02 UFH+GPI 0. 1% 0. 0 Number at risk P-R Heparin No P-R Heparin 0 6 1066 545 1211 378 1052 531 1208 377 12 Time in Hours 1051 529 1207 375 18 24 1050 528 1207 374 1049 528 1207 374 Dangas et al, Circulation 2011 rev

HORIZONS-STENT THROMBOSIS: 2 -Year Events Independent Predictors of ANY Definite/Probable ARC ST Variables H. R. (95% C. I. ) p Insulin-Treated Diabetes 2. 88 ( 1. 64, 5. 07) 0. 0002 Angiographic Aneurysm 2. 54 ( 1. 04, 6. 22) 0. 041 History of Previous PCI 2. 36 ( 1. 53, 3. 64) 0. 0001 Angiographic Ulceration 2. 25 ( 1. 04, 4. 86) 0. 039 Current Smoking 1. 66 ( 1. 16, 2. 38) 0. 006 Baseline flow grade TIMI 0/1 1. 59 ( 1. 07, 2. 36) 0. 021 1. 0041 ( 1. 0021, 1. 0060) <. 0001 0. 55 ( 0. 39, 0. 79) 0. 001 Baseline Platelet Count Pre-Randomization Heparin Dangas et al, Circulation 2011 rev

How has HORIZONS AMI changed my practice in AMI? ● Acute therapy in STEMI with complete focus on reperfusion and antithrombotic therapy: Time to reperfusion- Number one priority ● Reasonable options ¡ ¡ ¡ Good history to ascertain risk of bleeding in all pts Consider new antiplatelet agents (Prasugrel, Ticagrelor) in pts without overt risk of bleeding, in others 600 mg Clopid. Loading for all Bivalirudin in all pts, even if the pt received heparin prior to cath IIb IIIa reserved only in special situations- no reflow, giant thrombus Choice of BMS v. DES dependent of risk of RS and the pt.

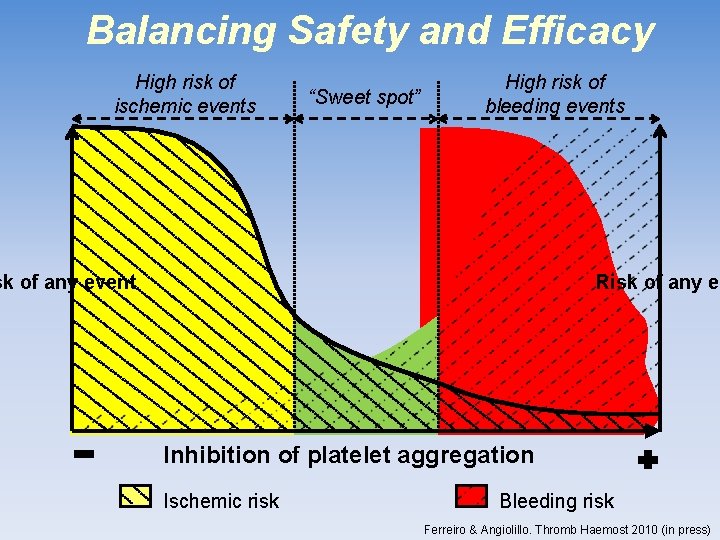
Balancing Safety and Efficacy High risk of ischemic events “Sweet spot” High risk of bleeding events sk of any event Risk of any ev Inhibition of platelet aggregation Ischemic risk Bleeding risk Ferreiro & Angiolillo. Thromb Haemost 2010 (in press)