ACROMEGALY Dr Zahra Ghasemzade Endocrine Fellow Shahid Beheshti

ACROMEGALY Dr Zahra Ghasemzade Endocrine Fellow Shahid Beheshti University Of Medical Science Mordad 1394 – August 2015

J Clin Endocrinol Metab, November 2014, 99(11): 3933– 3951

J Clin Endocrinol Metab, November 2014, 99(11): 3933– 3951
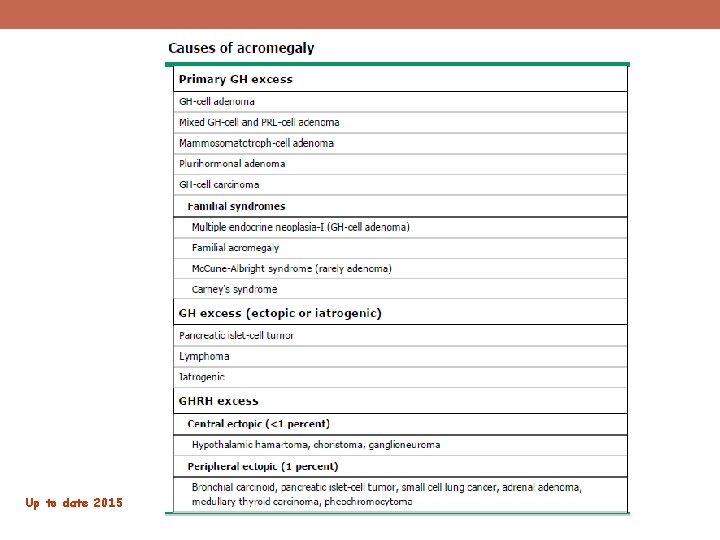
Up to date 2015
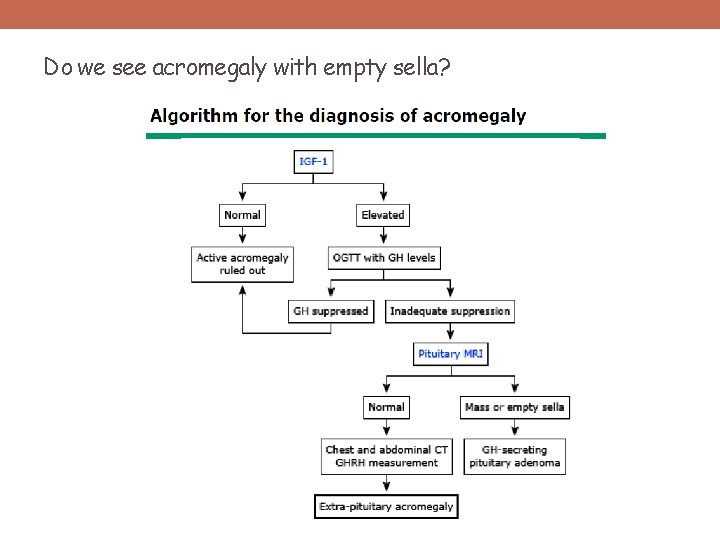
Do we see acromegaly with empty sella?

• Three criteria are mandatory for diagnosing ectopic GHRH secretion, • The confirmation of active GH hypersecretion, the unequivocal demonstration of GHRH production • And secretion from an extrapituitary tumor and the reversibility of acromegaly after tumor removal.

ü Overall standardized mortality rates are approximately two times higher than in the general population, relating to an average reduction in life expectancy of around 10 years. ü The excess deaths are due predominantly to cardiovascular, cerebrovascular and respiratory disease. ü Malignancy deaths have been high in some studies but not others; in the largest series looking at cancer mortality in acromegaly, overall cancer deaths were not increased, but colon cancer mortality was higher than expected. Rev Endocr Metab Disord (2008) 9: 33– 39
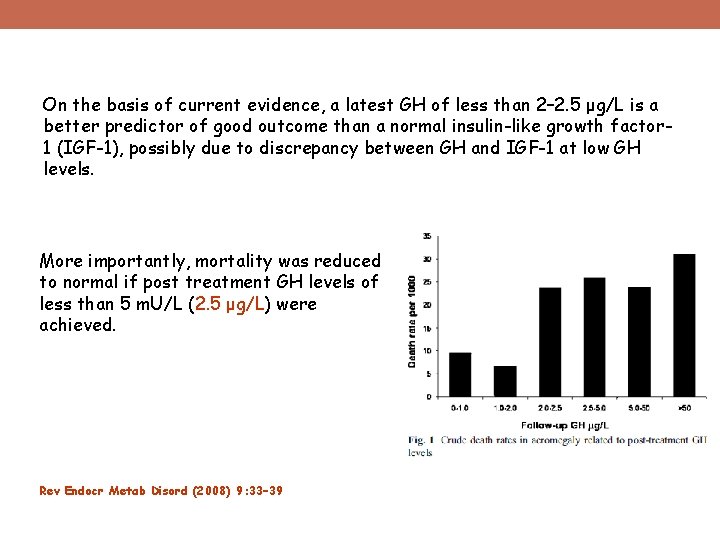
On the basis of current evidence, a latest GH of less than 2– 2. 5 μg/L is a better predictor of good outcome than a normal insulin-like growth factor 1 (IGF-1), possibly due to discrepancy between GH and IGF-1 at low GH levels. More importantly, mortality was reduced to normal if post treatment GH levels of less than 5 m. U/L (2. 5 μg/L) were achieved. Rev Endocr Metab Disord (2008) 9: 33– 39

ü No significant increase in mortality was identified in patients with a post-treatment GH less than 4 m. U/L (2 μg/L), but survival was reduced in the cohort failing to achieve this target, with an SMR of 1. 31. ü IGF-1 data was available in 360 patients representing 86% of the cohort. No effect of IGF-1 on outcome could be demonstrated, with the SMR for those patients achieving serum IGF-1 within the normal age-related range similar to those who did not. Rev Endocr Metab Disord (2008) 9: 33– 39

Thus the evidence linking GH excess to increased mortality in acromegaly is impressive and a reduction in values to less than 2. 5 μg/L and possibly even lower to less than 1 μg/L should be a fundamental aim of treatment in each case. However, some caution is needed here; it is established that non-acromegalic patients with hypopituitarism also have increased mortality. Rev Endocr Metab Disord (2008) 9: 33– 39

ü However the two larger studies, comprising a total of 151 deaths in 753 patients, have failed to demonstrate any relationship between posttreatment IGF-1 levels and mortality. On the basis of this data, serum IGF-1 does not appear to be a reliable marker of long-term risk. ü The reason for this discrepancy is unclear, but it is well known that not all actions of GH are mediated by IGF-1 and conversely, IGF-1 is not the only growth factor regulated by GH. ü IGF-1 is bound to specific serum binding proteins whose levels are influenced not only by GH but also by non-GH dependent mechanisms such as sex steroids, insulin secretion and nutrition. ü Other proposed mechanisms for this discrepancy include persistent GH dysregulation following “cure”, alteration of the normal IGF-1/GH relationship by somatostatin analogues and disruption ü of somatostatin tone due to radiotherapy. Rev Endocr Metab Disord (2008) 9: 33– 39
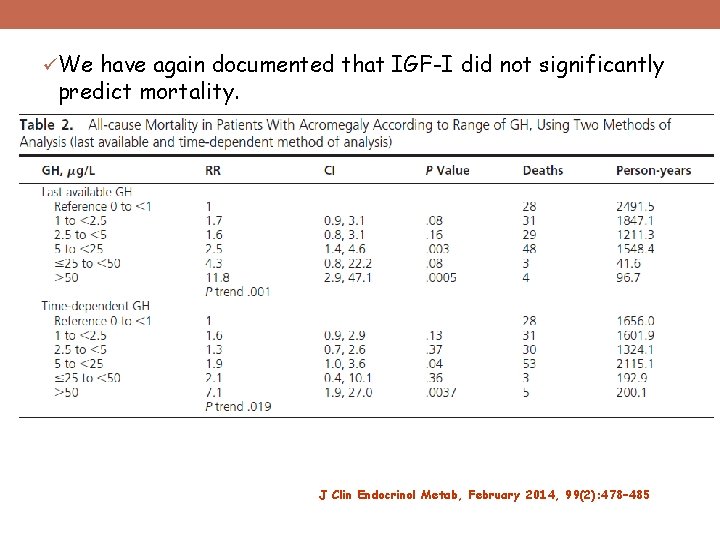
üWe have again documented that IGF-I did not significantly predict mortality. J Clin Endocrinol Metab, February 2014, 99(2): 478– 485
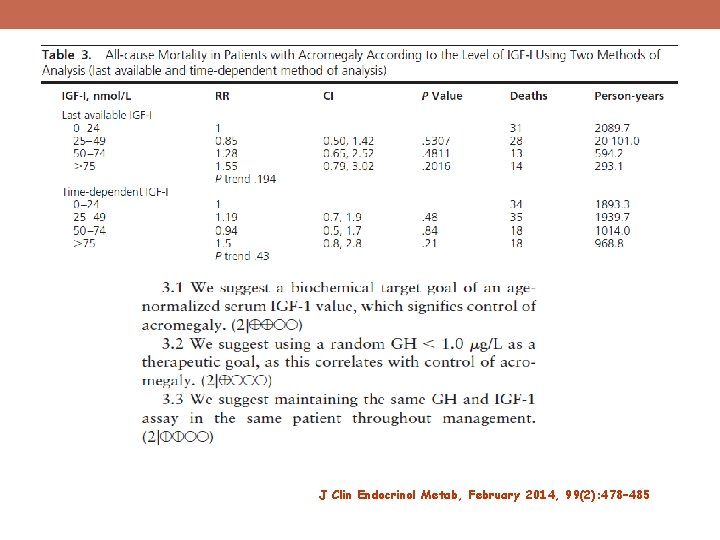
J Clin Endocrinol Metab, February 2014, 99(2): 478– 485

- Slides: 14