AcidBase Interpretation Easy as 1 2 3 4

Acid-Base Interpretation: Easy as 1 -2 -3 -4 Eric Dryver Emergency Department, Skåne’s University Hospital, Lund

Normal Arterial Values p. H p. CO 2 HCO 3 Laktat 7. 38 7. 42 – 5. 0 5. 7 –k. Pa (37. 5 – 43 mm Hg( 22 26 –mmol/L < 2 mmol/L
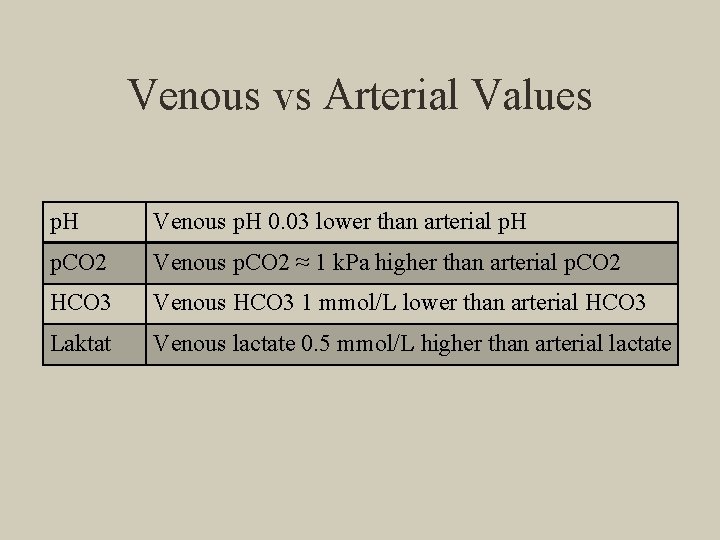
Venous vs Arterial Values p. H Venous p. H 0. 03 lower than arterial p. H p. CO 2 Venous p. CO 2 ≈ 1 k. Pa higher than arterial p. CO 2 HCO 3 Venous HCO 3 1 mmol/L lower than arterial HCO 3 Laktat Venous lactate 0. 5 mmol/L higher than arterial lactate

Terminology Acidemia: p. H < 7. 38 Alkalemia: p. H > 7. 42 Acidosis: process that decreases p. H Alkalosis: process that raises p. H

Step 1: Dominant Disorder? p. H < 7. 38 + – HCO 3 < 22 mmol/L: metabolic acidosis – p. CO 2 > 5. 7 k. Pa: respiratory acidosis p. H > 7. 42 + – HCO 3 > 26 mmol/L: metabolic alkalosis – p. CO 2 < 5. 0 k. Pa: respiratory alkalosis
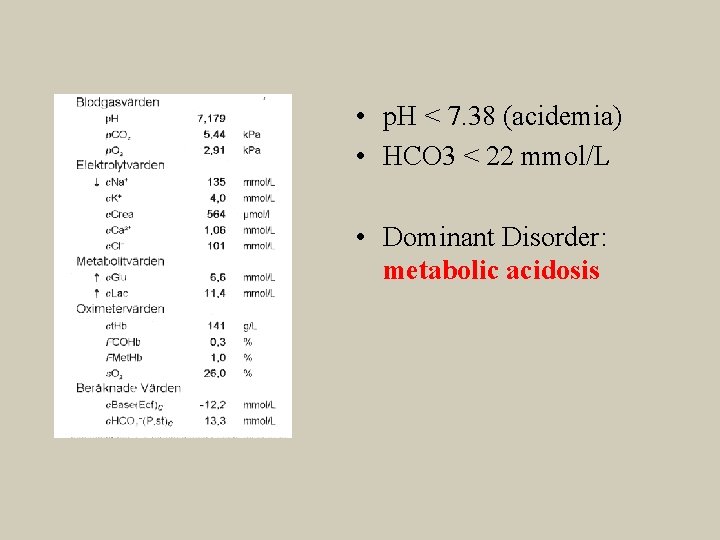
• p. H < 7. 38 (acidemia) • HCO 3 < 22 mmol/L • Dominant Disorder: metabolic acidosis
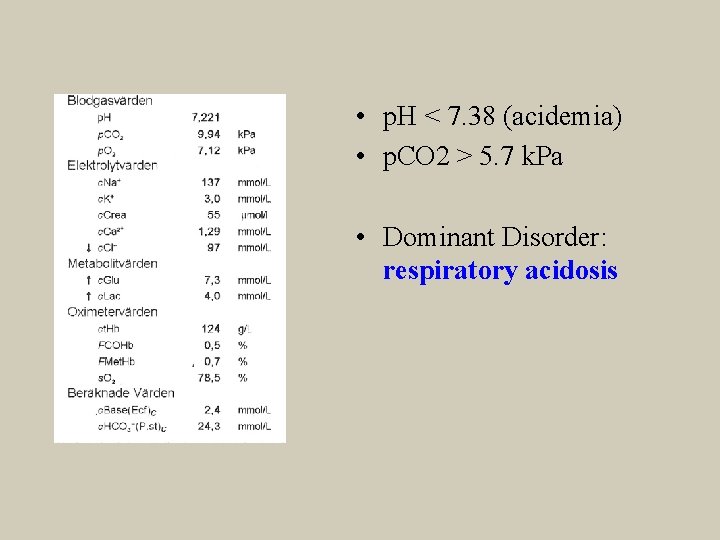

• p. H < 7. 38 (acidemia) • p. CO 2 > 5. 7 k. Pa • Dominant Disorder: respiratory acidosis
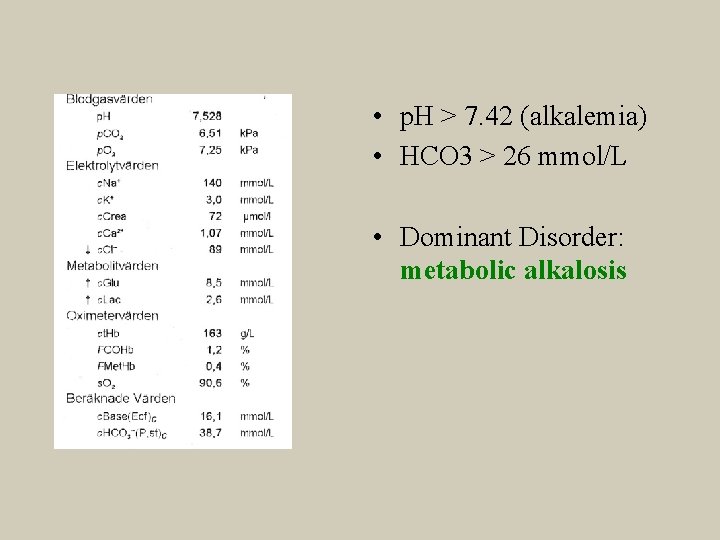
• p. H > 7. 42 (alkalemia) • HCO 3 > 26 mmol/L • Dominant Disorder: metabolic alkalosis
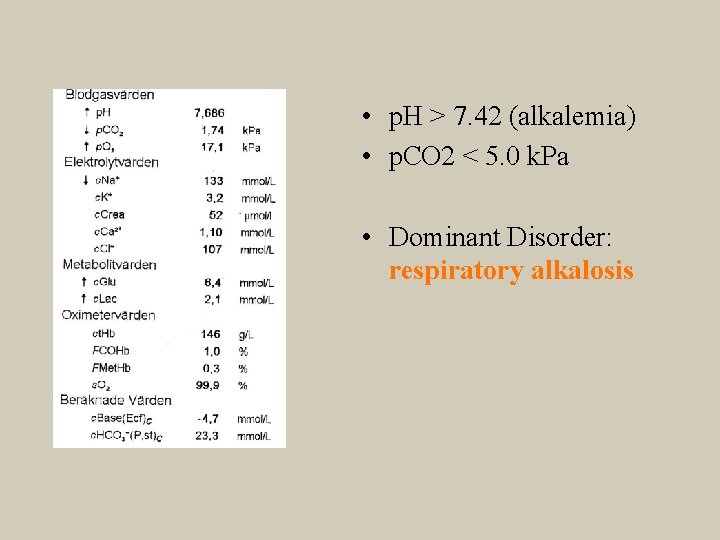

• p. H > 7. 42 (alkalemia) • p. CO 2 < 5. 0 k. Pa • Dominant Disorder: respiratory alkalosis
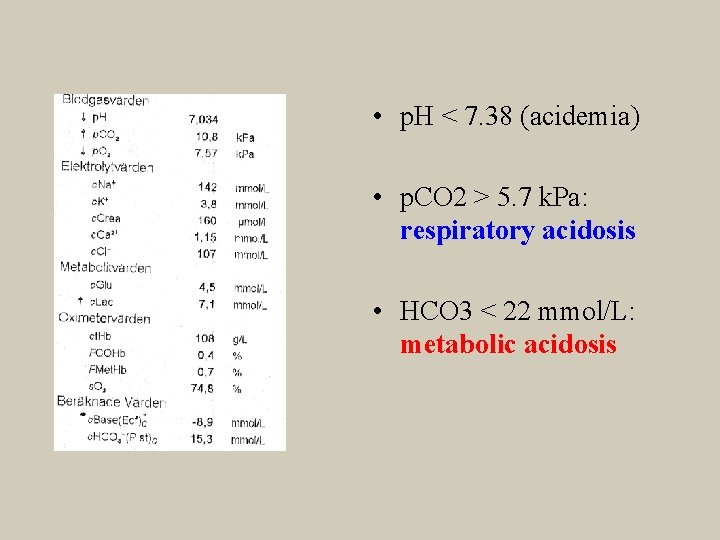

• p. H < 7. 38 (acidemia) • p. CO 2 > 5. 7 k. Pa: respiratory acidosis • HCO 3 < 22 mmol/L: metabolic acidosis

p. H Between 7. 38 and 7. 42 • If the p. H is normal, there are two possibilities: – No acid-base disturbances – ≥ 2 acid-base disturbances
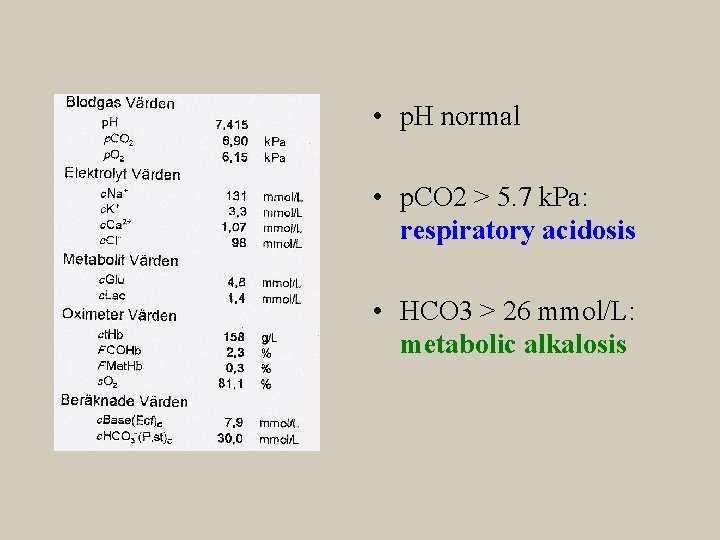
• p. H normal • p. CO 2 > 5. 7 k. Pa: respiratory acidosis • HCO 3 > 26 mmol/L: metabolic alkalosis
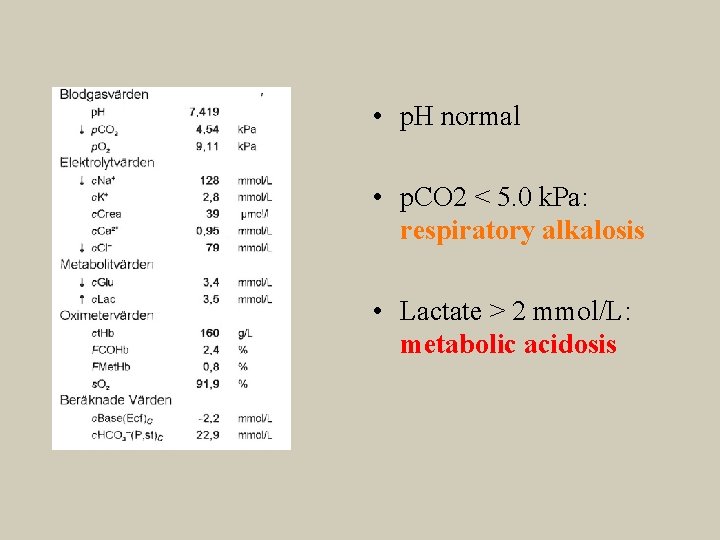

• p. H normal • p. CO 2 < 5. 0 k. Pa: respiratory alkalosis • Lactate > 2 mmol/L: metabolic acidosis
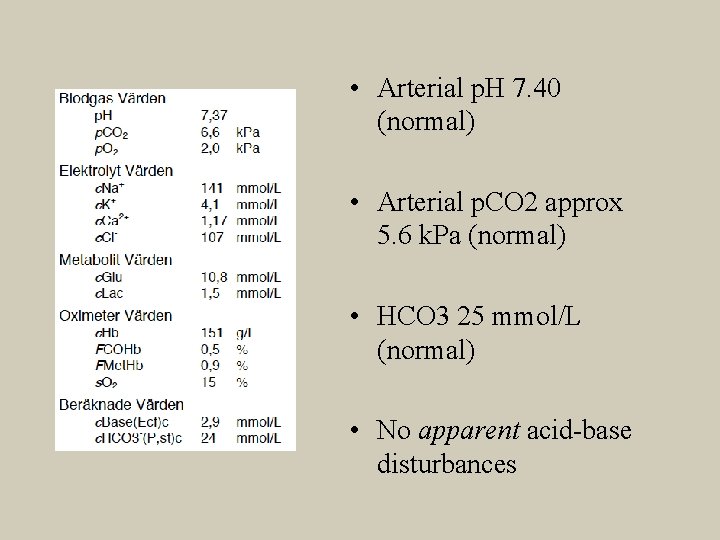
• Arterial p. H 7. 40 (normal) • Arterial p. CO 2 approx 5. 6 k. Pa (normal) • HCO 3 25 mmol/L (normal) • No apparent acid-base disturbances

Step 2: Compensation? • In the setting of a metabolic disorder, there should be a respiratory compensation • The respiratory compensation is immediate • The respiratory compensation is proportional to the metabolic disorder

Respiratory Compensation • You sprint over 100 m • You develop a metabolic acidosis (lactate) • You hyperventilate (not a disorder, rather a normal physiological response) • The degree of hyperventilation is proportional to the degree of acidosis Picture: https: //movietvtechgeeks. com/wp-content/uploads/2016/08/usain-bolt-at-rio-olympics. jpg

Expected Respiratory Compensation Metabolic acidosis Metabolic alkalosis ∆ p. CO 2 = ∆ HCO 3 x 0. 16 ∆ p. CO 2 = ∆ HCO 3 x 0. 09

Expected Compensation • ∆ HCO 3 = 24 - 4 = 20 • ∆ p. CO 2 = 20 x 0. 16 = 3. 2 • Expected p. CO 2 = 5. 3 – 3. 2 = 2. 1 • Actual p. CO 2 = 1. 9 Interpretation • Appropriate respiratory compensation: there are no apparent respiratory disorders
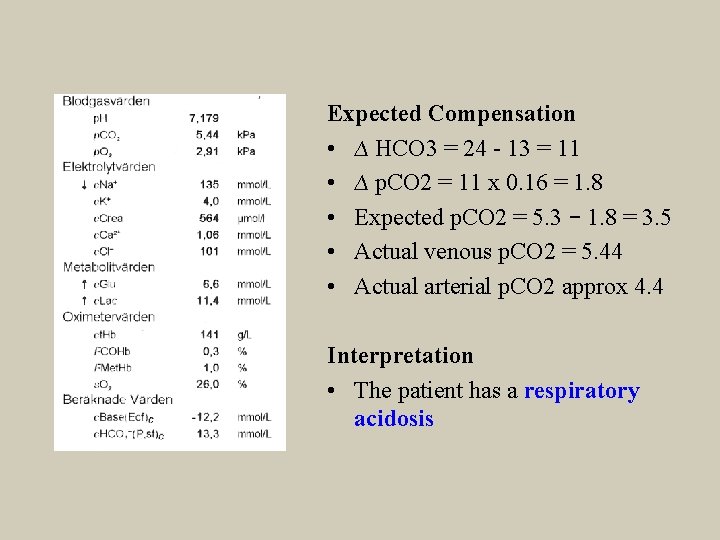
Expected Compensation • ∆ HCO 3 = 24 - 13 = 11 • ∆ p. CO 2 = 11 x 0. 16 = 1. 8 • Expected p. CO 2 = 5. 3 – 1. 8 = 3. 5 • Actual venous p. CO 2 = 5. 44 • Actual arterial p. CO 2 approx 4. 4 Interpretation • The patient has a respiratory acidosis
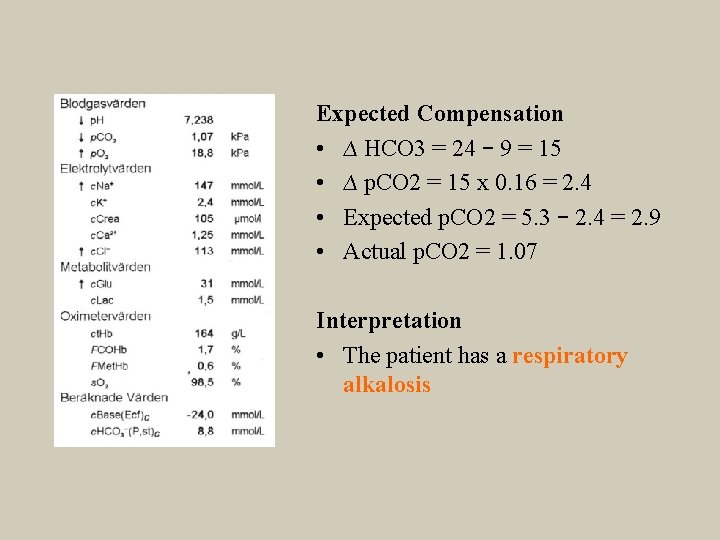

Expected Compensation • ∆ HCO 3 = 24 – 9 = 15 • ∆ p. CO 2 = 15 x 0. 16 = 2. 4 • Expected p. CO 2 = 5. 3 – 2. 4 = 2. 9 • Actual p. CO 2 = 1. 07 Interpretation • The patient has a respiratory alkalosis
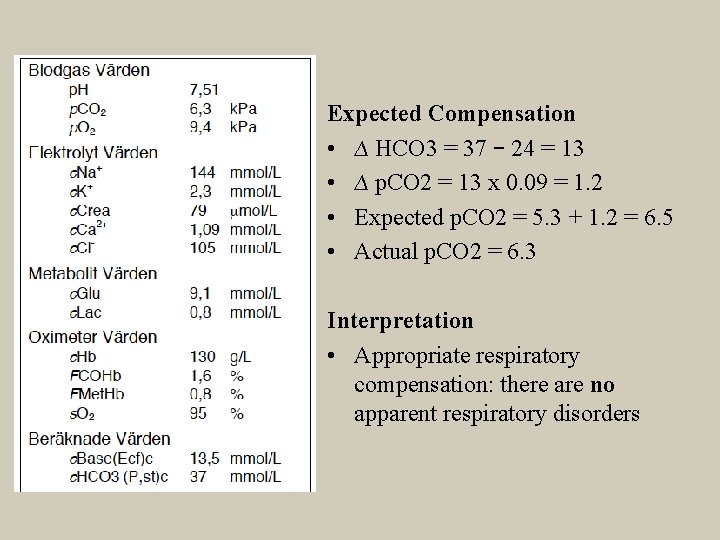
Expected Compensation • ∆ HCO 3 = 37 – 24 = 13 • ∆ p. CO 2 = 13 x 0. 09 = 1. 2 • Expected p. CO 2 = 5. 3 + 1. 2 = 6. 5 • Actual p. CO 2 = 6. 3 Interpretation • Appropriate respiratory compensation: there are no apparent respiratory disorders

Step 2: Compensation? • In the setting of a respiratory disorder, a metabolic compensation can occur • The metabolic compensationen takes 3 -5 days to fully develop • The metabolic compensation is proportional to the degree of the chronic respiratory disorder

Expected Metabolic Compensation to a Chronic Respiratory Disorder Respiratory acidosis ∆ HCO 3 = ∆ p. CO 2 x 2. 62 Respiratory alkalosis ∆ HCO 3 = ∆ p. CO 2 x 3. 0

Expected Chronic Compensation • ∆ p. CO 2 = 12. 1 – 5. 3 = 6. 8 • ∆ HCO 3 = 6. 8 x 2. 62 = 18 • Expected HCO 3 = 24 + 18 = 42 • Actual HCO 3 = 25 Interpretation • Acute respiratory acidosis
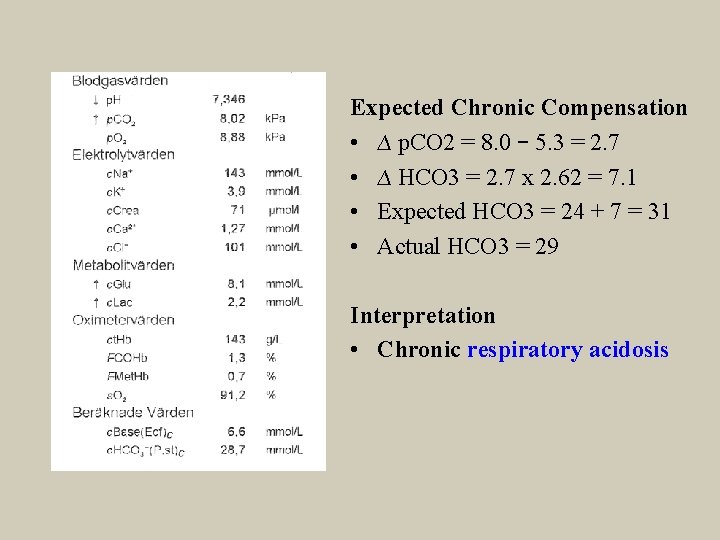
Expected Chronic Compensation • ∆ p. CO 2 = 8. 0 – 5. 3 = 2. 7 • ∆ HCO 3 = 2. 7 x 2. 62 = 7. 1 • Expected HCO 3 = 24 + 7 = 31 • Actual HCO 3 = 29 Interpretation • Chronic respiratory acidosis
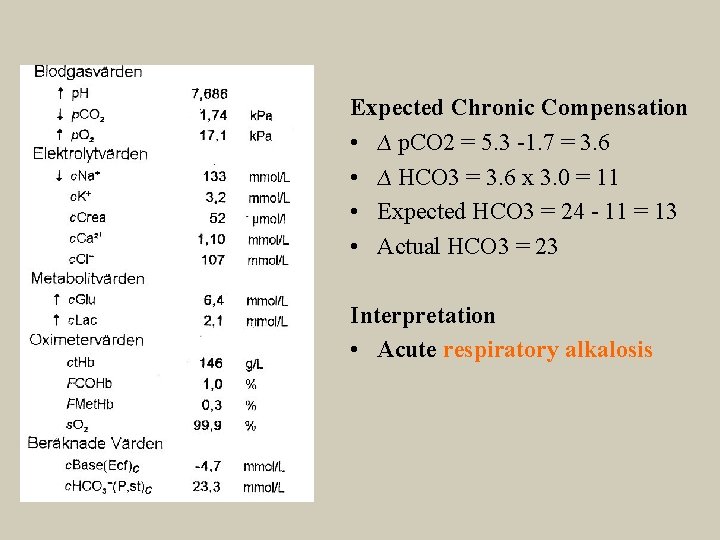
• Akut respiratorisk alkalos Expected Chronic Compensation • ∆ p. CO 2 = 5. 3 -1. 7 = 3. 6 • ∆ HCO 3 = 3. 6 x 3. 0 = 11 • Expected HCO 3 = 24 - 11 = 13 • Actual HCO 3 = 23 Interpretation • Acute respiratory alkalosis

Step 3: Ions 1. Calculate the Anion Gap (AG) 2. Estimate the Delta AG 3. Calculate Delta AG + HCO 3

Anion Gap • Total charge (cations) = total charge (anions) (electroneutrality) • The albumin present in blood is negatively charged • In order to preserve electroneutrality: Na+ > (Cl- + HCO 3 -)

Anion Gap & Electroneutrality Anion Gap: Na – Cl – HCO 3

Expected Anion Gap (AG) 6 -12 mmol/L Depends on how Na, Cl & HCO 3 are derived locally In my practice, my hunch is that • patients < 20 years have AG ≈ 6 mmol/L • patients > 60 years have AG ≈ 12 mmol/L

Delta Anion Gap • Delta AG = Actual AG –Expected AG • In the presence of a Delta AG, extra anions are present, i. e. the patient has a metabolic acidosis • It is the Delta AG that needs to be explained, not the Anion Gap per se

Anion Gap & Delta AG? 1. Reveals whether a metabolic acidosis is being concealed by a concurrent metabolic alkalosis

24 -Year-Old with Type 1 DM • p. H 7. 40 • p. CO 2 5. 3 • HCO 3 24 • Glucose 19 • Na 140 • Cl 98 • p. H, p. CO 2, HCO 3 are normal. • AG: 140 18 = 24 – 98 – • Expected AG ≈ 7 • Delta AG 11: metabolic acidosis likely DKA • A metabolic alkalosis must also be present (vomiting? )
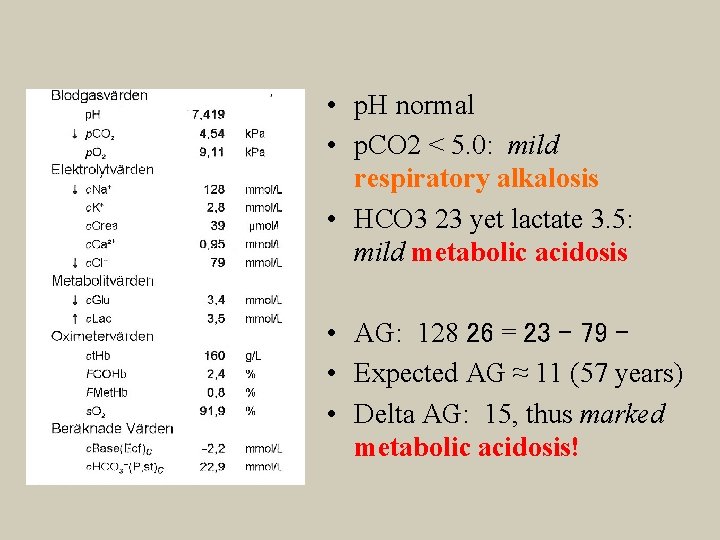

• p. H normal • p. CO 2 < 5. 0: mild respiratory alkalosis • HCO 3 23 yet lactate 3. 5: mild metabolic acidosis • AG: 128 26 = 23 – 79 – • Expected AG ≈ 11 (57 years) • Delta AG: 15, thus marked metabolic acidosis!

Anion Gap & Delta AG? 2. Narrows the differential diagnosis of the metabolic acidosis

Two Types of Metabolic Acidoses Increased AG Normal AG No metabolic acidosis Metabolic Acidosis Hyperchloremic Metabolic Acidosis

• p. H < 7. 38 & HCO 3 < 22: metabolic acidosis • AG: 135 21 = 13 – 101 – • Expected AG ≈ 9 (42 years) • Delta AG: 12 • Interpretation: increased AG metabolic acidosis (lactic)
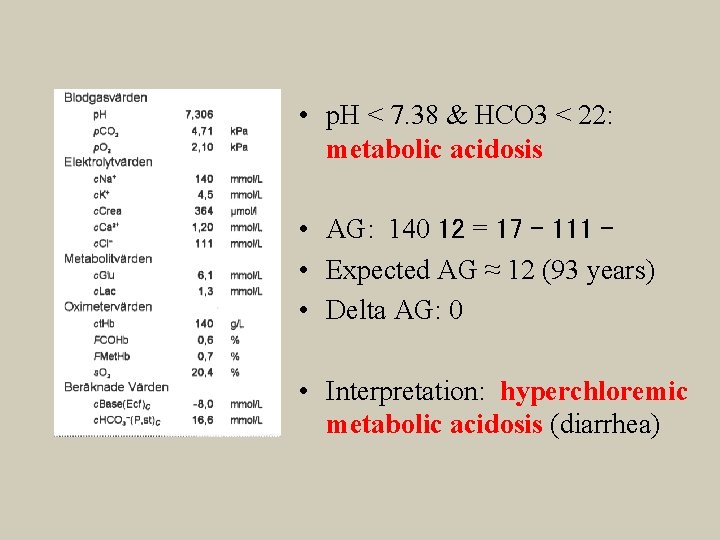

• p. H < 7. 38 & HCO 3 < 22: metabolic acidosis • AG: 140 12 = 17 – 111 – • Expected AG ≈ 12 (93 years) • Delta AG: 0 • Interpretation: hyperchloremic metabolic acidosis (diarrhea)

DDx Metabolic Acidosis Increased AG • • HCMA Methanol, Metformin Loss of HCO 3 from Uremia • Bowel (e. g. diarrhea) Diabetic ketoacidos • Kidney (e. g. RTA) Propylene glycol, Pyroglutamic acid Iron, Isoniazid Administration of ++ Na. Cl Lactate (L or D) Ethylene glycol, Ethanol ketoacidos Salicylates, solvents, starvation ketoacidosis

• AG: 135 21 = 13 – 101 – • Expected AG ≈ 9 (42 years) • Delta AG: 12 • Lactate accounts for Delta AG • There is no suspicion of an alternative explanation for the increased AG

• AG: 128 26 = 23 – 79 – • Expected AG ≈ 11 (57 years) • Delta AG: 15 • Lactate of 3. 5 mmol/L • 11. 5 mmol/L of anions remain to be accounted for

Anion Gap & Delta AG? 3. A low, even negative anion gap can reveal another disorder

DDx Low/Negative Anion Gap • • • Mnemonic LIMBS: Low albumin, Li 2+ Iodide Myeloma Bromide Salicylates

54 Year-Old Bipolar Unconscious Step 1 • p. H < 7. 38 & HCO 3 < 22: metabolic acidosis Step 2 • ∆ p. CO 2 = 6 x 0. 16 = 1 • Expected p. CO 2 = 4. 3: respiratory acidosis Step 3 • AG: 123 - 107 - 18 = - 2: lithium intoxication?

Anion Gap & Delta AG? 4. Reveal and quantify a background metabolic disorder by calculating Delta AG + HCO 3

Delta AG + HCO 3 • 1 mmol HCO 3 is consummed by 1 mmol of added anion. • If the patient has a Delta AG of 10 mmol/L, the HCO 3 has dropped by roughly 10 mmol/L • Actual HCO 3 + Delta AG can be thought of as HCO 3 ’prior’ to acquisition of extra anions

Delta AG + HCO 3 • Delta AG + HCO 3 ≈ 24 mmol/L: no sign of a metabolic disturbance • Delta AG + HCO 3 > 26 mmol/L: background metabolic alkalosis or compensation for a chronic respiratory acidosis • Delta AG + HCO 3 < 22 mmol/L: background hyperchloremic metabolic acidosis (HCMA)
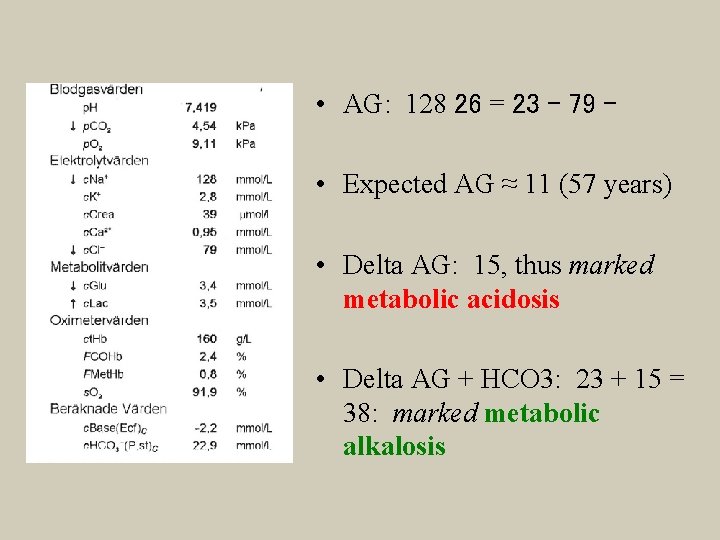

• AG: 128 26 = 23 – 79 – • Expected AG ≈ 11 (57 years) • Delta AG: 15, thus marked metabolic acidosis • Delta AG + HCO 3: 23 + 15 = 38: marked metabolic alkalosis

Step 4: Diagnosis Take into consideration all available information: • Backgrund: past medical history, medications. . . • History • Physical findings • Other bedside test results
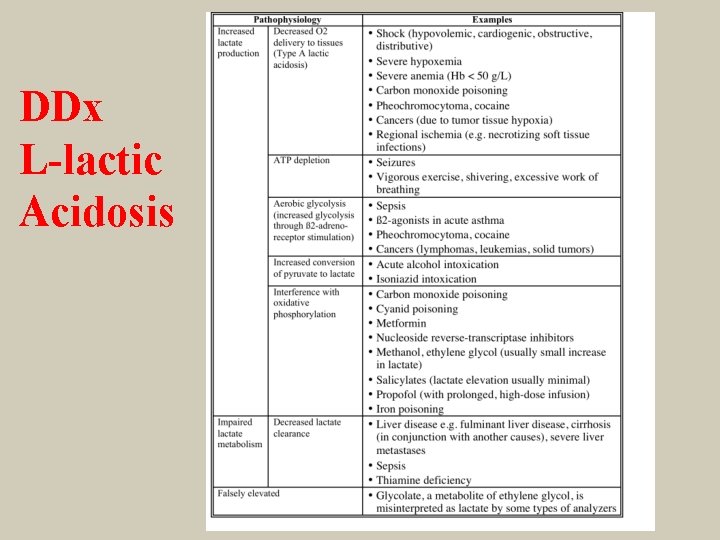
DDx L-lactic Acidosis

DDx Metabolic Alkalosis

DDx Respiratory Acidosis

DDx Respiratorisk Alkalosis
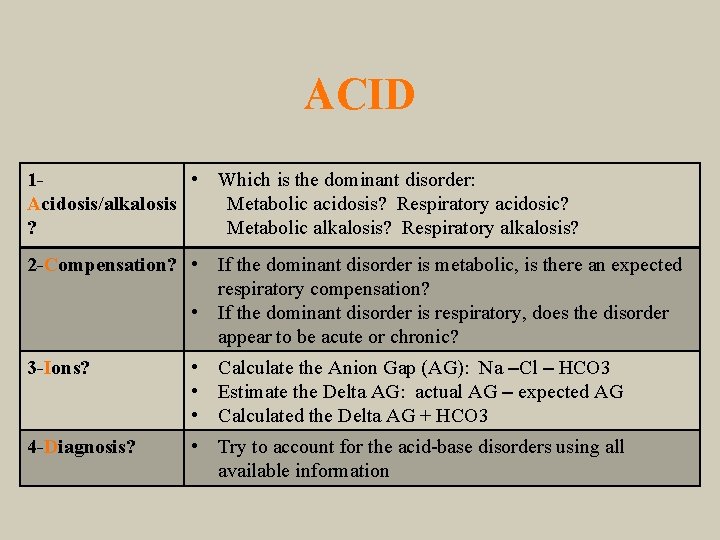

ACID 1 • Which is the dominant disorder: Acidosis/alkalosis Metabolic acidosis? Respiratory acidosic? ? Metabolic alkalosis? Respiratory alkalosis? 2 -Compensation? • If the dominant disorder is metabolic, is there an expected respiratory compensation? • If the dominant disorder is respiratory, does the disorder appear to be acute or chronic? 3 -Ions? • Calculate the Anion Gap (AG): Na –Cl – HCO 3 • Estimate the Delta AG: actual AG – expected AG • Calculated the Delta AG + HCO 3 4 -Diagnosis? • Try to account for the acid-base disorders using all available information

• KOL patient Step 1 • p. H < 7. 38 • p. CO 2 > 5. 7: respiratory acidosis • HCO 3 < 22: metabolic acidosis Step 3 • AG: 143 - 101 - 20 = 22 • DG: 10 (75 years) • Adjusted HCO 3: 20 + 10 = 30 Steg 4 (pat with severe COPD) • Chronic respiratory acidosis with metabolic compensation • Metabolic acidosis with elevated AG: uremia? • Acute respiratory acidosis (COPD exacerbation? )
- Slides: 55