Acidbase Balance and its Disorders Prof Dr Meltem

Acid-base Balance and its Disorders Prof. Dr. Meltem Pekpak

For optimal functioning of cells. . • Acids and bases in the body must be in balance. • We all consume every day food and drinks which contain acids, metabolism produces also acids. . .

Body p. H Balance • • Chemical blood buffers: Lungs, Cells, Kidneys • Defences against changes in hydrogen concentration (getting acidotic. . )

You get acidotic every day ! • While living, eating and drinking. . . there is. . • Production of 1 mmol of fixed acid/kg body weight per day (60 kg=60 mmol/day)

Buffers • Extracellular: • Hemoglobin – (‘Chloride shift’-for each chloride leaving the cell-one bicarbonate ion enters) • Plasma protein – (with the liver, varying the amount of H-ions in the protein structure) • Bicarbonate system: – Normal acid to base ratio is 20: 1 – 20 parts bicarbonate to 1 part carbonic acid (H 2 CO 3=CO 2), – Neutralizing a strong acid bicarb. will be lost

Human Acid-base Homeostasis • Tight regulation: • CO 2 tension – by respiratory excretion (of volatile acids) • Plasma bicarbonate [HCO 3 -] – By renal HCO 3 - reabsorption and – Elimination of protons produced by metabolism • p. H is determined by CO 2 tension and [HCO 3 -]

Physiology of Buffering: • Ability of a solution containing a weak or poorly dissociated acid and its anion (a base) to resist change in p. H when strong acid or alkali is added • 1 ml of 0. 1 M HCl to 9 ml distilled water = • [H+] from 10 -7 M to 10 -2 M= p. H from 7 to 2 • 1 ml of 0. 1 M HCl to 9 ml of phosphate buffer: dissoc. H+ combines with [HPO 42 -] = (H 2 PO 4 -) • p. H fall of only 0. 1= to 6. 9

Bicarbonate Buffer • Extracellular most important buffer • Proteins and phosphate buffer less important • Intracellular phosphate- most important b. • Equilibrium conditions because abundant carbonic anhydrase in blood • H+ + HCO 3 - H 2 CO 3 H 2 O + CO 2 • [H+ ]= Keq x [H 2 CO 3 ]/[HCO 3 -]

Equations • H+ + HCO 3 - H 2 CO 3 H 2 O + CO 2 • Equilibrium • [H+ ]= Keq x [H 2 CO 3 ]/[HCO 3 -]
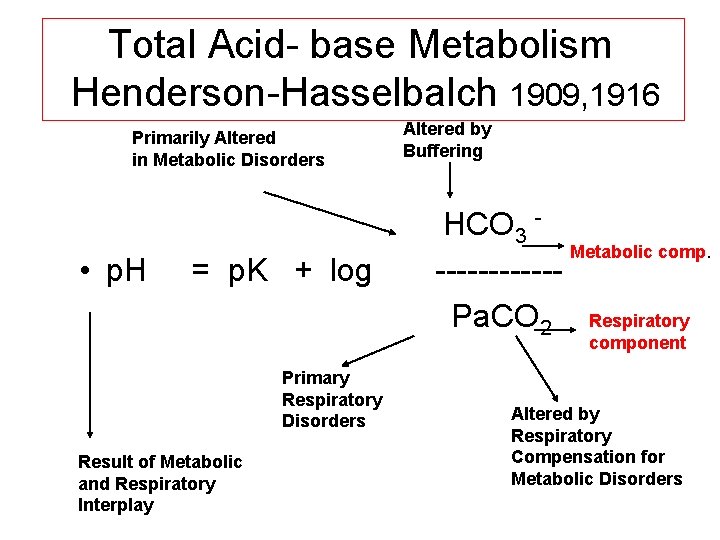
Total Acid- base Metabolism Henderson-Hasselbalch 1909, 1916 Primarily Altered in Metabolic Disorders • p. H = p. K + log Altered by Buffering HCO 3 Metabolic comp. ------Pa. CO 2 Respiratory component Primary Respiratory Disorders Result of Metabolic and Respiratory Interplay Altered by Respiratory Compensation for Metabolic Disorders
![Normal Values • • [HCO 3 -] ~ 24 m. M Pa. CO 2 Normal Values • • [HCO 3 -] ~ 24 m. M Pa. CO 2](http://slidetodoc.com/presentation_image_h/af92e880159995717e48068768685ae1/image-11.jpg)
Normal Values • • [HCO 3 -] ~ 24 m. M Pa. CO 2 = 38 torr p. H ~ 7. 42 Plasma HCO 3 - regulation by – reclaiming filtered HCO 3 - and – generating new HCO 3 - (carboanhydrase) – ( to replace the lost internally titrating metabolic acid and externally from the GI tract) • Production of 1 mmol of acid/kg body weight per day (60 kg=60 mmol/day)

Renal Acid -base Handling • Two seperate functions: • Bicarbonate reabsorption • Net acid secretion
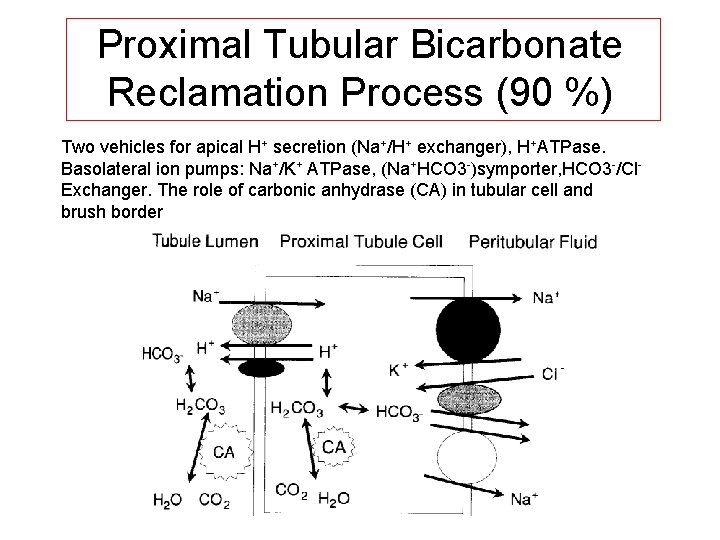
Proximal Tubular Bicarbonate Reclamation Process (90 %) Two vehicles for apical H+ secretion (Na+/H+ exchanger), H+ATPase. Basolateral ion pumps: Na+/K+ ATPase, (Na+HCO 3 -)symporter, HCO 3 -/Cl. Exchanger. The role of carbonic anhydrase (CA) in tubular cell and brush border

Net Acid Excretion • Urine is acid = p. H~ 4. 5 • Buffer salts are in the tubular fluid • Phosphate is the most important buffer in urine: HPO 42 - + H+ = H 2 PO 4 • Nonvolatile (fixed) acids (anions= sulfates, phosphates) must be accompanied in the urine by equivalent cations (Na +, K +, Ca + +) for maintenance of electrical neutrality • In acid urine ammonium helps to keep [H+ ] (ammonia NH 3+ to NH 4+)

Clinical Evaluation • • • Patient history Clinical presentation Acidemia Hyperventilation Alkalemia Paresthesias and Tetany Laboratory: Blood acid-base status: Blood p. H (4 º C, with anticoagulant, promptly), Urine p. H Plasma and urine electrolyte concentration Lactate concentration

Acidosis • • • Clinical effects of severe acidosis: p. H <7. 2 Cardiovascular system effects: Decreased myocardial contractility Decreased cardiac output Cardiac failure Hypotension Decreased hepatic and renal blood flow Centralization of effective blood volume Tissue hypoxia Pulmonary edema
![Metabolic acidosis • Hallmark is [HCO 3 -] • 1. Acid production net acid Metabolic acidosis • Hallmark is [HCO 3 -] • 1. Acid production net acid](http://slidetodoc.com/presentation_image_h/af92e880159995717e48068768685ae1/image-17.jpg)
Metabolic acidosis • Hallmark is [HCO 3 -] • 1. Acid production net acid intake above net renal excretion (ketoacidosis, lactic acidosis, ammonium chloride loading) • 2. failure of renal net excretion (chronic renal failure, renal tubular acidosis) • 3. Bicarbonate loss via the gastroinestinal tract (diarrhea, gastrointestinal fistula) • 4. Nonbicarbonate solutions added to ECF (dilutional acidosis)

Steps of evaluation • 1. Examine p. H= Reduction ( 7. 2) Acidosis • Increase (7. 5) Alkalosis • 2. Examine directional change of PCO 2 -] , and [HCO 3 • • p. H acid, HCO 3 - low Metabolic acidosis • p. H alkal. , HCO 3 - high Metabolic alkalosis • 3. Assess degree of compensation: Mixed acid-base disorder? • Metabolic acidosis PCO 2 • Metabolic alkalosis PCO 2 • Failure of respiratory compenstion= primary respiratory acid-base disorder • Never to initial p. H through compensation !!

Steps of evaluation • 4. Calculate the serum anion gap • Is the acid-base disorder organic or mineral in origin? ? • We use venous sample blood electrolytes: • Electroneutrality demands: • Serum anion gap, that means: • [Na+] + [UC]= [Cl-] +[Total CO 2] + [UA] • (U means: unmeasured)
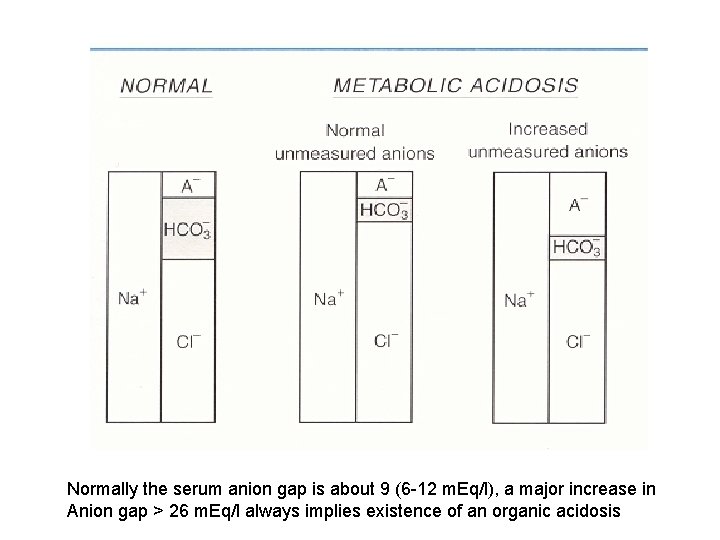
Normally the serum anion gap is about 9 (6 -12 m. Eq/l), a major increase in Anion gap > 26 m. Eq/l always implies existence of an organic acidosis

Differential Diagnosis of Metabolic Acidosis • Normal anion gap Increased anion gap • (hyperchloemic) (organic)_____ • GI loss of HCO 3 - acid production • • • Lactic acidosis Diab. Ketoacidosis Toxic alcohol, salicy. Acute renal failure Chronic renal failure Diarrhea Renal tub. Acidosis Parenteral alimentation Carbonic anhydr. İnh. K-sparing diuretics

Increased anion gap Metabolic acidosis • • Ketoacidosis (diabetic) Uremia (renal failure) Salicylate intoxication Starvation Methanol intoxication Alcohol ketoacidosis Unmeasured osmoles (intoxication) Lactic acidosis
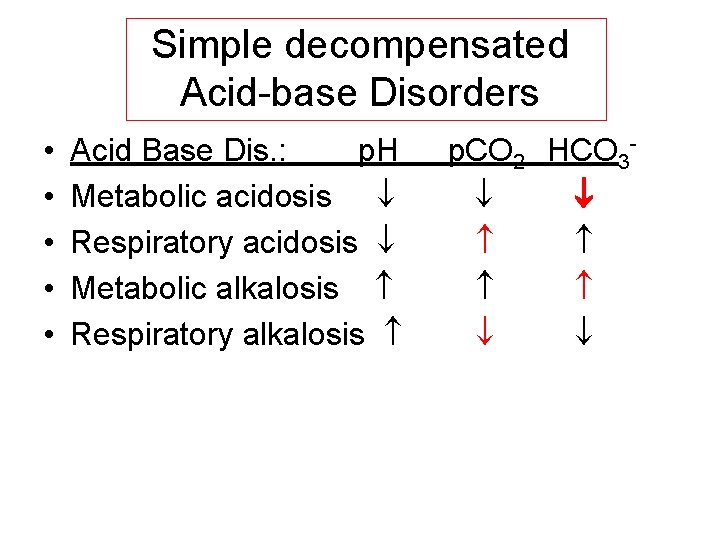
Simple decompensated Acid-base Disorders • • • Acid Base Dis. : p. H Metabolic acidosis Respiratory acidosis Metabolic alkalosis Respiratory alkalosis p. CO 2 HCO 3

Compensatory Response • • one half of acid load is buffered by nonbicarbonate buffers= Bone, protein, red cells. . PCO 2 (Kussmaul) compensatory response after 15 -30 minutes, 5 days up to maximal Kidney: Metabolic acidosis processing of glutamine into NH 4+ (ammonia to ammonium for better H-excretion) and Bicarbonate generation (and reclaiming)


Respiratory Acidosis • Acute increase in p. CO 2 • Buffered primarily by intracellular buffers • Chronic state: • Kidneys compensation: • Increase net acid excretion, • (48 hours for fully development) • • Underlying cause: Central nervous system disease, lung (COPD)and heart disease, sedatives and opiates depressing the respiratory center • Hypercapnic encephalopathy can develop
![Metabolic Alkalosis • Plasma bicarbonate [HCO 3 -] = p. H • 1) H+ Metabolic Alkalosis • Plasma bicarbonate [HCO 3 -] = p. H • 1) H+](http://slidetodoc.com/presentation_image_h/af92e880159995717e48068768685ae1/image-27.jpg)
Metabolic Alkalosis • Plasma bicarbonate [HCO 3 -] = p. H • 1) H+ GI loss or shift into cells • 2) Excess HCO 3 Administration of bicarbonate, or precursors: lactate, acetate, citrate or Failure to excrete: mineralocorticoid effect • 3) Loss of fluid with Diuretic therapy [Cl-], [K+] and [H+] loss from plasmaextracellular volume contraction

Alkalosis

Volume Depletion and Metabolic Alkalosis • Absolute volume depletion: • Loss of salt by bleeding or vomitting or • Effective volume depletion: • Heart failure, cirrhosis, nephrotic syndrome whenever • GFR • Tubular HCO 3 - reabsorption • Because proximal tubule reabsorption is enhanced for Na and water

Compensatory Respiratory Response • • Alveolar hypoventilation(hypercapnia) (limited p. CO 2 rise to 50 -60 mm Hg) Kidneys: Excretion of HCO 3 - proportional to GFR (excessive)
Respiratory Alkalosis p. CO 2 , p. H due to: Hypoxia (compensatory hyperventilation) • Acute: pulmonary edema or emboli, pneumonia, • Chronic: severe anemia, high altitude, hypotension Respiratory center stimulation • Pregnancy, Anxiety, Fever, heat stroke, sepsis, salisylate intox. , cerebral disease, hepatic cirrhosis, Increased mechanical ventilation

Respiratory Alkalosis • Most common acid-base disorder • Physiologic in pregnancy and high altitude • Bad prognosis in critically ill patients (the higher hypocapnia, the higher mortality) • Hyperventilation, • Perioral and extremity paresthesias, • Light-headedness, • Muscle cramps, • Hyperreflexia, seizures, ionized Ca tetany

Metabolic Alkalosis with and without Volume Depletion • Volume depleted- Chloride responsive metabolic acidosis: • Urine chloride is low (<10 mmol/l) • Due to: • Gastric fluid losses • Stool losses • Diuretic therapy

Metabolic Alkalosis Excessive Mineralocorticoids • Mineralocorticoids stimulate hydrogen ion secretion • And this bicarbonate reabsorption • Urinary chloride is normal (<20 mmol/l) • Hypokalemia • Primary aldosteronizm, • Bartter’s Syndrome, • Cushing Syndrome • Renovascular hypertension
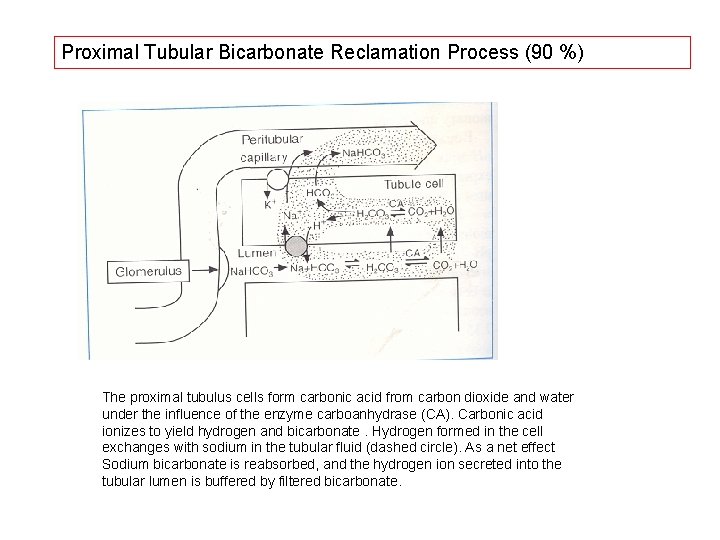
Proximal Tubular Bicarbonate Reclamation Process (90 %) The proximal tubulus cells form carbonic acid from carbon dioxide and water under the influence of the enzyme carboanhydrase (CA). Carbonic acid ionizes to yield hydrogen and bicarbonate. Hydrogen formed in the cell exchanges with sodium in the tubular fluid (dashed circle). As a net effect Sodium bicarbonate is reabsorbed, and the hydrogen ion secreted into the tubular lumen is buffered by filtered bicarbonate.

Henderson-Hasselbach 1909, 1916 • H 2 CO 3 = p CO 2 + solubility in physiol. Fluids • [H+ ]= K x [S x p. CO 2 ]/[HCO 3 -] Antilog of both sides: p. H= p. K + log 10 [HCO 3 -] / [S x PCO 2] In blood at 37º C, p. K =6. 1 and S is 0. 03 p. H= 6. 1+ log 10 [HCO 3 -] / [0. 03 x Pa. CO 2]
- Slides: 37