Acetaminophen Toxicity Dr khodabandeh 1 OBJECTIVES Acetaminophen toxicity

Acetaminophen Toxicity Dr. khodabandeh 1

OBJECTIVES • Acetaminophen toxicity : a) Epidemiology b) Dosing c) Metabolism d) Diagnosis e) Treatment f) Prognosis 2

3

Epidemiology ¡ Most popular OTC analgesic ¡ Lay people commonly underestimate its toxicity 4

Epidemiology ¡ intentional (suicidal)=unintentional (chronic) poisonings ¡ ¡ is often thought to be benign, or is a “hidden ingredient” in other remedies. Accounts for more overdoses and overdose deaths each year in North America than any other pharmaceutical agent 5
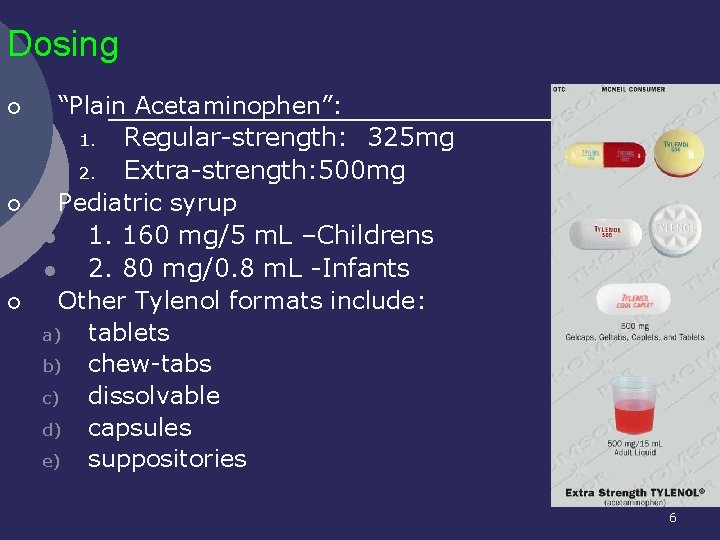
Dosing ¡ ¡ ¡ “Plain Acetaminophen”: 1. Regular-strength: 325 mg 2. Extra-strength: 500 mg Pediatric syrup l 1. 160 mg/5 m. L –Childrens l 2. 80 mg/0. 8 m. L -Infants Other Tylenol formats include: a) tablets b) chew-tabs c) dissolvable d) capsules e) suppositories 6

Dosing ¡ is also available as a co-ingredient in several combination medications: 7

Dosing ¡ Recommended Acetaminophen dosing is as follows: l l l Adult: 325 -650 mg every 4 -6 hours or 1000 mg 3 -4 times/day; do not exceed 4 g/day. 2. 5 mg in liver failure Peds: 10 -15 mg/kg/dose every 4 -6 hours as needed; do not exceed 5 doses (80 mg/kg) in 24 hours 8

Acute Toxic Dosing ¡ The minimum toxic dose for an acute ingestion of Acetaminophen (ie. occurring within a time frame of four hours) is: a) Adults: 7. 5 g b) Peds: 150 mg/kg It may be prudent to also use these levels as the minimum acute toxic dose per 24 hours. ¡ Ingestions occurring over a period of more than four hours are arbitrarily termed chronic ingestions. ¡ 9

Chronic Toxic Dosing The minimum toxic dose for chronic ingestions of Acetaminophen is less well defined. ¡ Rosen’s suggests: ¡ a) Adults: > 4 g/d if risk factors > 7. 5 g/d if no risk factors b) Peds: > 75 mg/kg/d if risk factors > 150 mg/kg/d if no risk factors 10

Metabolism ¡ ¡ Immediate-release is rapidly absorbed in the gut, with peak serum levels typically achieved in 30 m – 2 hr Peak serum levels can be delayed… 1. 2. 3. With sustained-release formulations. With combination formulations. In overdoses. a) peak levels not being achieved for up to 4 hrs following overdoses of immediate-release. b) peaks even >4 hrs following OD’s of extended-release 11

Metabolism ¡ Under normal circumstances, is metabolized in the following manner: 12
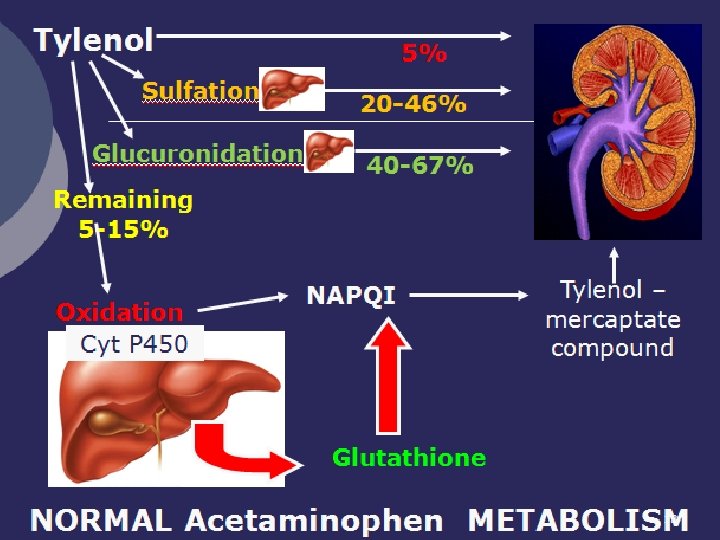
13
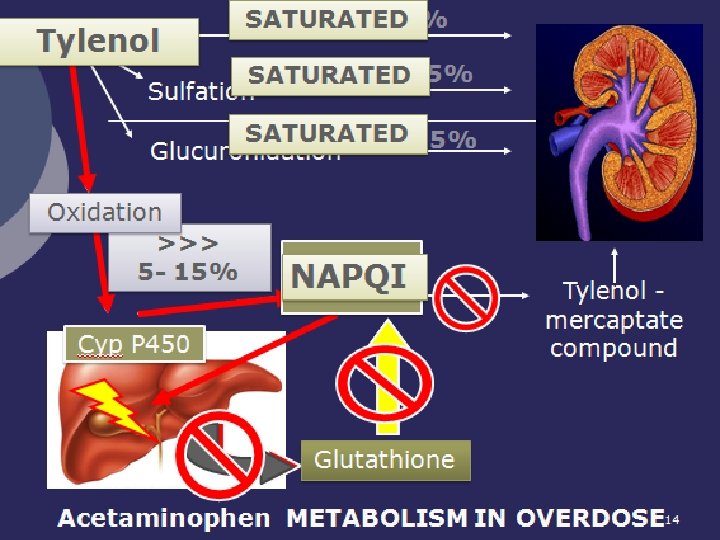
14

Risk Factors for Acetaminophen Toxicity ¡ An obvious corollary of the previous slide is that anything which potentiates the action of Cyp P 450 will accelerate the production of NAPQI. ¡ (And vice-versa. ) 15

Risk Factors Cyt P 450 Potentiators ( 1. 2. 3. 4. NAPQI): Chronic alcohol consumption Anticonvulsants: l Tegretol l Dilantin l Phenobarb Anti-tuberculosis medications: l Rifampin l INH Dexamethasone 16

(Not) Risk Factors Cyp P 450 Inhibitors ( Acute alcohol consumption Macrolides 1. 2. • 3. 4. 5. 6. 7. NAPQI): Erythromycin, Biaxin, Zithromax Antifungals Amiodarone HIV protease-inhibitors Cyclosporine Grapefruit juice 17

Quick note on the sauce… In practice, alcoholics tend not to be at increased risk for hepatotoxicity following an acute overdose of Tylenol. Practice matches theory more closely, however, in alcoholics with chronic Tylenol overdoses. ¡ ¡ l Even so, these pts are still unlikely to develop toxicity if they restrict their Tylenol use to <4 g/d. 18 *

Summary of Risk Factors 1. 2. 3. 4. 5. 6. 7. Induced Cyt-P 450 Chronic alcoholism Acute fasting (may include febrile peds) Chronic malnutrition Septra or AZT use Gilbert’s disease Elderly patients 19

Clinical Stages 1. Stage One (0 -24 hrs) • minimal clinical findings. • may be completely asymptomatic. • may have minor non-specific findings such as N/V, pallor, malaise. • liver panel unremarkable. 20
Clinical Stages 2. Stage Two (Day 2 -3) • clinical signs of hepatotoxicity. • RUQ pain, hepatomegaly, AST/ALT/bili/PT/lipase elevation. Most sensitive • patients may also develop early signs of renal failure or pancreatitis during this stage. 21

Clinical Stages 2. Stage Two continued… • From Stage 2, patients progress either to Stage 4 (with subsequent full recovery) or to Stage 3 (with subsequent probable death). 22

Clinical Stages 3. Stage Three (Day 3 -4) • Fulminant hepatic failure +/- death • Associated lactic acidosis, coagulopathy, encephalopathy; possible pancreatitis, hypoglycemia, ARF. • Marked elevation of liver enzymes (with AST typically >3, 000), • Elevation of NH 3, coags, lactate. 23

Clinical Stages 3. Stage Three continued… • Stage 3 will progress to: (a)death. (b)if lucky, a liver transplant. (c) if even luckier, Stage 4 and a full recovery. 24

Clinical Stages 4. Stage Four (Day 4 - 10) • If you do not die in Stage 3, you arrive at Stage 4 with rapid and complete hepatic recovery. • Clinical recovery usually begins by Day 4 and is complete by Day 7 -10. • Histological recovery may take up to 3 months. 25

Clinical Stages • Summary of stages: Days: 1. Minimal symptoms 1 2. Moderate symptoms 2 -3 3. Severe symptoms +/- death 3 -4 4. Complete recovery 4 -10 26

Treatment ¡ Early on in toxicity, NAC: 1. Acts as a glutathione precursor, increasing glutathione stores. 2. Binds NAPQI directly. 3. Enhances the sulfation pathway. 27

Treatment ¡ Later in toxicity… (when Tylenol levels are absent, but hepatotoxicity has begun) …NAC continues to offer benefit: 1. 2. 3. 4. 5. It has strong antiinflammatory effects. It has strong antioxidant effects. It scavenges free radicals. It modifies cytokine production. It increases inotropy and vasodilation, thereby improving microcirculation. 28

Treatment ¡ If NAC is initiated within 8 hours of (even a massive) acute overdose, the patient: 1. 2. ¡ Is very unlikely to suffer (even transient) serious hepatotoxicity. Essentially never dies from the overdose Beyond the 8 -hour point, NAC’s protective abilities steadily diminish. 29

Diagnosis 30

Diagnosis • history. • Sadly, with Acetaminophen toxicity, history can sometimes be a bit of a problem. 31

Diagnosis ¡ As such, the diagnosis of Acetaminophen toxicity rests on: 1. 2. 3. ¡ Acetaminophen levels AST/ALT (and other bloodwork) levels The Rumack-Matthew nomogram. The “other blood work” to consider drawing in Tylenol toxicity includes: 1. 2. PT, BUN/Cr, glucose, lipase, CK Medication levels (eg. ASA, Et. OH, etc. ) 32

Diagnosis There are some potential problems with the Rumack-Matthew nomogram. 1. 2. 3. What about chronic or multiple ingestions? What if the time of acute ingestion is not firmly established? What if the pt is lying to you? 4. What if the acute ingestion was <4 or >24 hours ago? 5. What about sustained-release drug? 33 #

Diagnosis What about chronic or multiple ingestions? 1. l It is generally accepted that the nomogram is not reliable in this situation. ¡ Drug levels could potentially be therapeutic (or, for that matter, undetectable) even in the face of significant hepatotoxicity. 34

Diagnosis 2. What if the time of acute ingestion is not firmly established? l l l In this instance (since the actual time of ingestion may well be >8 hrs ago), one would be wise to draw a Tylenol level at once and initiate NAC immediately. This is especially true for patients who have RUQ pain, are jaundiced, or look ill. When the acetaminophen (and other bloodwork) levels come back, one can decide whether or not to continue therapy. 35

Diagnosis 3. What if the pt is lying to you? l If you have these, then feel free to trust all your patients and follow the nomogram. – If you are not quite as trusting, then draw a Tylenol level at once and initiate NAC immediately. 36

Diagnosis 4. What if the ingestion was < 4 or >24 hours ago? l As already mentioned, the nomogram is unreliable outside of these timeframes. a) b) If <4 hrs from time of ingestion, Tylenol levels may still be increasing. If >24 hrs from time of ingestion, Tylenol levels may be undetectable, even in the face of significant hepatotoxicity. 37

Diagnosis 5. What about sustained-release Tylenol? ¡ “draw both a 4 - and 8 -hour Acetaminophen level, and initiate NAC if either level is potentially toxic. ” 38
And now… a return to Treatment 39

Treatment ¡ ¡ In the ED, the most difficult question to answer is not which therapy to use (psst… use NAC), but whether or not therapy is actually required. And this question will have to be answered at least twice: Once before the bloodwork is back. (b) Once after the bloodwork is back. (a) 40

Treatment 1. Hx of ingestion suggestive of toxicity. a) acute overdose (eg. >7. 5 g or >150 mg/kg). b) chronic supratherapeutic use (>4 g/d or >75 mg/kg). c) chronic therapeutic use in a patient with risk factors. d) chronic use or overuse of sustained-release or combined-ingredient. 41

Treatment 2. Hx of ingestion that is not suggestive of toxicity, but sounds like it is: a) inconsistent. b) incomplete. c) a big fat lie. 42

Treatment 3. Clinical findings suspicious of toxicity: a) RUQ pain b) jaundice c) N/V d) lethargy and malaise e) dehydration 43

Treatment ¡ So back to the original question: l When is therapy warranted? 44

Treatment before bloodwork ¡ Before bloodwork is back, initiate NAC if: 1. Clinical suspicion of Tylenol toxicity. ¡ ¡ ¡ Some will argue that if the bloodwork will be back within 8 hours of the time of ingestion, that you do not need to initiate empiric therapy. And, strictly speaking, this is true. So, by all means… 45

Treatment before bloodwork ¡ ¡ ¡ …if your patient took an : acute dose of immediate-release at an exact and known time, has no risk factors, and is not potentially lying to you, then go ahead and wait for the bloodwork to come back. 46 #

Treatment after bloodwork ¡ After bloodwork is back, initiate and/or continue NAC if: 1. 2. Nomogram indicates probable toxicity. In the setting of a unreliable nomogram* you have: a) b) clinical suspicion of toxicity and drug levels are even detectable. clinical suspicion of toxicity with undetectable drug levels, but AST or other bloodwork is abnormal. 47

Treatment after bloodwork What if you still have clinical suspicion of toxicity when all your bloodwork is back and it is all completely normal? ¡ l Chances are, you worry too much. 48

Treatment Protocols ¡ For uncomplicated Acetaminophen overdose, there are two types of NAC protocols: 1. Oral NAC ¡ ¡ ¡ 2. A 72 -hour course of therapy. 18 total doses (q 4 h dosing). Total dose = 1330 mg/kg of NAC. IV NAC 1. 2. 3. A 20 -hour course of therapy. Continuous IV infusion. Total dose = 300 mg/kg of NAC. 49 #

Treatment Protocols ¡ ¡ For overdose complicated by liver-failure, IV NAC is used but the infusion is not stopped at 20 hours. Instead, the NAC is continued until the patient: 1. 2. 3. Fully recovers. Dies. Receives a liver transplant. 50

Comparing Treatment Protocols 1. Oral NAC – 2. method of choice in the U. S. IV NAC – – – method of choice in Canada. typically better tolerated. major limitation is rate-related IV reactions (discussed next slide), which are typically nonserious and easily controlled. 51

Comparing Treatment Protocols • Adverse reactions with IV NAC: 1. 2. Reported frequency is 0. 2 – 21% Reported rxns (in order of increasing severity and decreasing frequency): ¡ ¡ ¡ nausea/flushing/chills/fever urticarial rash/hypotension bronchospasm/angioedema hemolysis cardiovascular collapse 52

Comparing Treatment Protocols • Adverse reactions with IV NAC: 3. These IV-related reactions: ¡ ¡ ¡ are dose- and rate-dependent usually occur in the first hour of Rx are usually easily controlled with: a) b) c) temporarily stopping the IV. treating with antihistamines. re-starting the IV at a (temporarily) lower-rate. 53

Comparing Treatment Protocols • Adverse reactions with IV NAC: 4. Continuation of IV therapy is the rule in all but life-threatening scenarios. 54

Comparing Treatment Protocols ¡ Effectiveness of IV vs. oral NAC. 1. 2. In an uncomplicated overdose at <8 hrs, IV NAC is as effective as oral. In an uncomplicated Tylenol overdose at >8 hrs, oral NAC may be superior to IV. l 3. Possibly secondary to the increased amount and duration of oral NAC. * In Tylenol-induced fulminant liver failure, only IV protocols have ever been formally used and studied. 55

Comparing Treatment Protocols 4. Tylenol toxicity in pregnancy has not been rigorously studied, but IV NAC is typically recommended: a) b) c) d) Fetal toxicity is rare, but has been reported at all stages of pregnancy. IV NAC is safe and effective in mom. Higher serum levels obtained with IV NAC (by avoiding hepatic first-pass metabolism in mom) may translate into higher serum levels in the fetus. Exact treatment guidelines are controversial, and require toxicological and/or obstetrical consultation. 56

Prognosis 57

Prognosis ¡ Although AST is the most sensitive marker for liver damage, it is a poor prognosticator. 58
Prognosis ¡ eligible for liver transplantation if: ** Arterial p. H < 7. 30 (following fluid resuscitation) ¡ prothrombin time (PT) >100 seconds, ¡ creatinine >3. 3 mg/d. L, ¡ grade III or IV encephalopathy, ¡ 59

Grades of Hepatic Encephalopathy * Clinical Stage Intellectual functioning Neuromuscular function Subclinical Normal exam Subtle changes only Grade I Decreased attention, personality changes Tremor, apraxia, incoordination, Grade II Drowsiness, behavioural Asterixis. slowed speech, changes ataxia Grade III Confusion, disorientation, amnesia Decreased reflexes, nystagmus, clonus, muscular rigidity Grade IV Stupor, coma Dilated pupils, decerebrate posturing 60

THE END 61

? 62
- Slides: 62