Accidental Ingestions Bindu Suresh PGY3 October 30 2015

Accidental Ingestions Bindu Suresh, PGY-3 October 30, 2015

Epidemiology 2 million exposures annually, 50% are accidental exposures in kids under 5 6 -12 year-olds account for only 6% of all pediatric exposures More than 90% of all pediatric exposures occur in the home, and most involve a single substance Ingestion 77%, dermal 7. 5%, inhalation 6%, ophthalmic 5% 50% are non-drug exposures: cosmetics, cleaning solutions, plants, foreign bodies, hydrocarbons 50% are drugs: analgesics, cough and cold products, antimicrobials, vitamins

Epidemiology 85% of pediatric cases can be managed without medical intervention (either because product not toxic or not enough of it taken); death is uncommon Fatalities most common in adolescents, usually with intentional exposures adolescents: 6. 1% of all fatal exposures children 6 -12: 1% of all fatal exposures children under 6: 1. 9% of all fatal exposures

History When What was ingested product name with ingredients and concentration, often discovered by the label, and, if not, by a poison centre to delineate which ingredients will be problematic and prioritize clinical effects

History How much better to overestimate than underestimate amount count remaining tablets, measure remaining liquid if bottle not full and exact level not known, assume bottle was full if multiple children, assume each had the maximum amount. Age and weight of the child is important in determining dose received
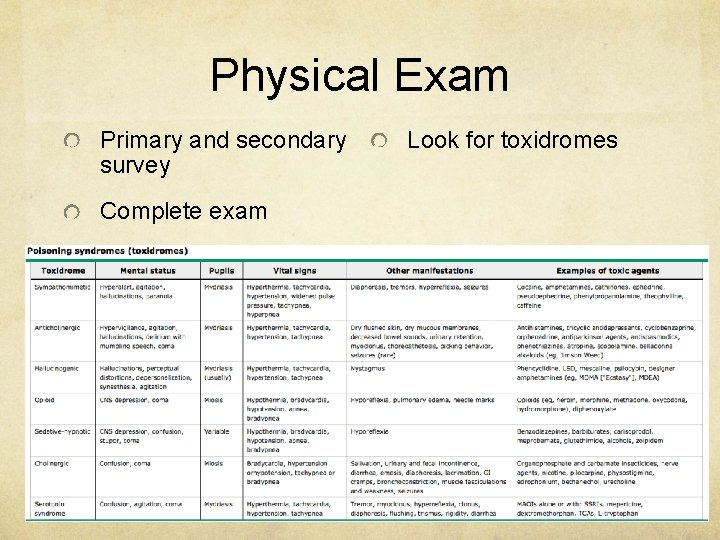
Physical Exam Primary and secondary survey Complete exam Look for toxidromes

Management: Preventing Absorption Toxins rapidly absorbed through the GI tract most liquids within 30 -45 minutes solids within 1 -2 hours exceptions: large ingestions may take 3 -6 hours, and anticholinergic ingestions can take 8 -12 hours (as they cause intestinal slowing) Rarely, ingestions can form into bezoars: suspect this when the patient continues to have symptoms days after apparent resolution of symptoms

Activated Charcoal How it works: has a very large adsorptive surface area; toxins get absorbed onto it rather than the GI tract only works for some ingestions; will not work for heavy metals, iron, lithium, hydrocarbons, cyanide, LMW alcohols. How it's prepared: prepared as a slurry or as a solution with sorbitol, a cathartic

Activated Charcoal Dose and route: given 1 g/kg for a child, 50 -100 g for an adult-sized adolescent can be given repeatedly q 2 -4 h at 0. 5 g/kg or 0. 25 g/kg for 24 h can be given PO or NG if won't tolerate orally, give through NG if giving through NG, confirm placement in stomach before giving charcoal

Activated Charcoal Special considerations: if patient not protecting airway, needs to be intubated before administration and charcoal given NG if giving repeated or continuous doses, watch for bowel sounds because of risk of impaction if can't tolerate repeated bolus dosages, give continuous only use cathartic with first charcoal dose, otherwise risk of dehydration Side effects: 25% of patients who receive charcoal vomit (can aspirate, but aspirating charcoal mixed with stomach contents not shown to be worse than aspirating gastric contents)

Cathartics Sorbitol, 1 g/kg; mag sulf, 250 mg/kg; mag citrate 250 m. L/kg No evidence for their use Can be used, but be wary of dehydration and electrolyte imbalances

Whole-Bowel Irrigation PEG 30 m. L/kg/hr Can use for slowly-absorbed substances like iron, sustained-release preparations, or foreign bodies Use with caution due to fluid and electrolyte imbalances

Emetics Syrup of ipeac Not routinely recommended Contraindicated in ingestion of caustics, hydrocarbons

Other Gastric Lavage Not routinely recommended Alkalization/Acidification of Urine Not routinely recommended Dialysis Rarely indicated Can be useful with toxic alcohols, methanol, ethylene glycol, large ingestions of salicylates, theophylline, lithium

Laboratory Investigations can order levels for salicylates, anticonvulsants, acetaminophen, iron, digoxin, methanol, lithium, theophylline, ethylene glycol, carbon monoxide for tox screens, best to use urine sample

Button Batteries: Pathophysiology become lodged in GI tract and cause caustic injury, mucosal ulceration, perforation esophagus most prone to impaction tend to halt at physiologic narrowings (UES, aortic arch, LES) damage is caused primarily by electrical discharge, but also by leakage of contents and pressure necrosis

Button Batteries: Pathophysiology severity of injury depends on: length of time (damage starts at 2 h, severe damage after 8 h) amount of electrical charge (lithium, >3 V, new batteries) size of battery (>20 mm) as length of time increases, edema increases and battery sticks to the mucosa low risk of damage once past the esophagus

Button Batteries: Symptoms usually asymptomatic can have CP, cough, N/V, diarrhea, abdo pain, fever, hematemesis, dysphagia, drooling if perforated, add shock, subcutaneous emphysema, tension pneumo
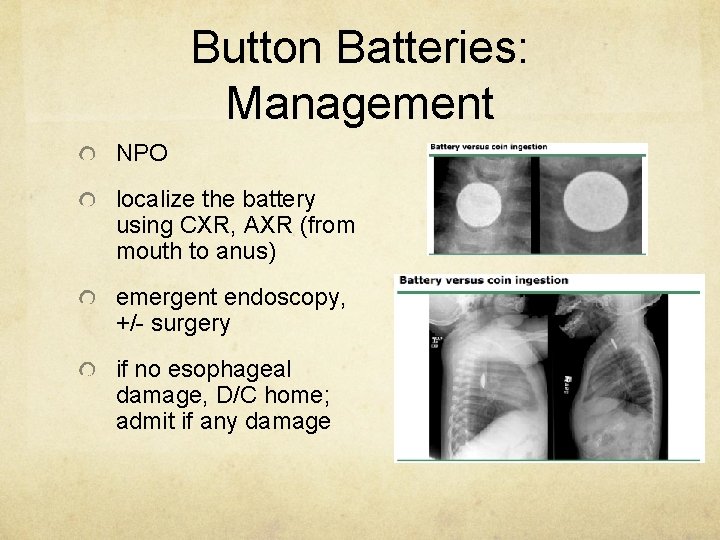
Button Batteries: Management NPO localize the battery using CXR, AXR (from mouth to anus) emergent endoscopy, +/- surgery if no esophageal damage, D/C home; admit if any damage

Button Batteries If patient asymptomatic, >12, battery <12 mm, no co-ingestion of magnet, can defer radiography and wait for battery to pass (if not passed in 2 weeks, repeat XR) do not use an emetic: battery unlikely to be expelled, and if in stomach could lodge in esophagus Long-Term Effects: TEF, vocal cord paralysis, perforation of esophagus, stomach, aortic arch, intestines (early) esophageal stenosis (late)

Caustics (Acids and Alkalis, Including Bleach) Pathophysiology: acids coagulate proteins, causing tissue necrosis, which limits tissue penetration alkalis cause liquefaction necrosis, which caries risk of perforation severity depends on p. H (worse if <2 or >12), concentration, length of contact time
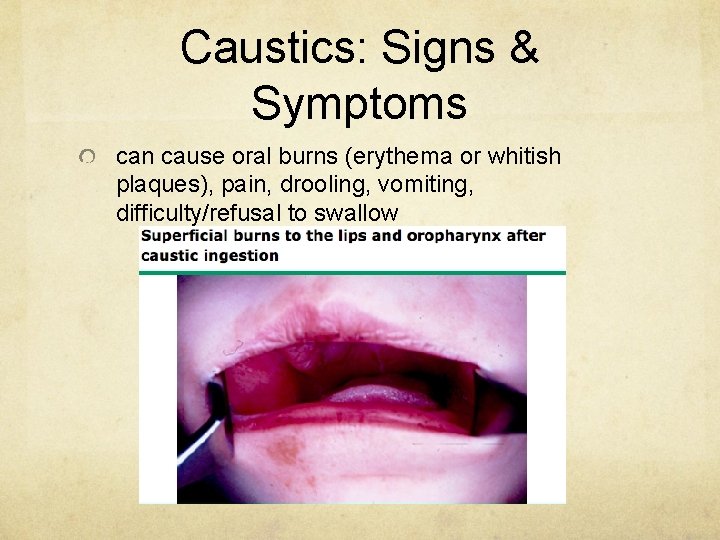
Caustics: Signs & Symptoms can cause oral burns (erythema or whitish plaques), pain, drooling, vomiting, difficulty/refusal to swallow

Caustics: Management rinse oral cavity evaluate for esophageal burns, and make NPO if there is damage endoscopy for those who are symptomatic or for whom the history suggests esophageal contact no emesis or gastric lavage (contraindicated) activated charcoal also contraindicated (does not bind these agents, and might just cause vomiting, which would cause further damage) prophylactic antibiotics not helpful

Caustics: Long-Term Effects circumferential burns of esophagus may cause strictures that will require dilatation or surgery acids can scar pylorus, causing delayed-onset gastric obstruction

Laundry Detergent Pods Pathophysiology alkali, ? ethoxylated alcohols, ? propylene glycol unclear why effects from pods worse than traditional detergent exposures Symptoms vomiting, 56%, coughing, 15%, lethargy or decreased LOC, 8%, nausea, 5% coma, seizures, gastric burns, respiratory arrest, hematemesis, pulmonary edema, bradycardia major effects in 8%, minor effects in 50% Management same as for caustics

NSAIDs Pathophysiology COX inhibitor Rarely cause toxicity at doses <100 mg/kg Symptoms Over 400 mg/kg can cause bradycardia, hepatic dysfunction, seizures and coma Symptoms usually develop within 4 -6 h of ingestion and resolve within 24 h Initial effects include N/V, epigastric pain, drowsiness, lethargy, ataxia Rarely, large ingestions can cause complications include anion gap metabolic acidosis, coma, apnea, renal failure, hypotension, seizures

NSAIDs: Management supportive care activated charcoal no antidote emesis not useful monitor renal function and acid-base balance after ingestion of large doses

TCAs Pathophysiology inhibit fast sodium channels in myocardium anticholinergic effect block reuptake of norepi, serotonin, dopamine peripherally and in CNS produce sedation, alpha blockade Symptoms can develop within 30 minutes, serious symptoms usually develop within 6 hours with large ingestions effects can be seen >8 hours, as has anticholinergic effects that slow gastric emptying/bowel motility for same blood level, adolescents > toxicity than children main effects are on CNS and CVS

TCAs: Symptoms CNS effects CNS>CVS effects in children drowiness, lethargy, or coma in 30%; coma usually resolves in a few hours but can last >24 h seizures in 15%, usually brief and self-resolving CVS effects tachycardia is most common cardiac effect (due to anticholinergic effect) hypertension soon after ingestion, but rarely requires treatment hypotension uncommon but is a poor prognostic sign also can get slowed conduction, PVCs, long QT, heart block, vtach, v-fib Other effects hypoventilation with respiratory arrest may occur anticholinergic syndrome may also occur

TCAs: Management monitor EKG plasma levels not helpful in determining course (though may aid in diagnosis) activated charcoal, can use repeated q 4 h doses sodium bicarbonate to maintain normal p. H to prevent dysrhythmias if sodium bicarbonate doesn't work, give lidocaine to control arrhythmia

TCAs: Management emesis contraindicated (risk of aspiration with decreased LOC, seizures) do not give quinine or procainamide as will further depress cardiac conduction do not use physostigmine (can cause seizures and dysrhythmias) if asymptomatic observe in ED on cardiac monitor for 6 h if any sign of QRS >100, conduction defects, altered LOC, hypotension or hypoventilation develop, monitor in ICU for 24 h

SSRIs Pathophysiology block re-uptake of serotonin in CNS wide therapeutic index, toxic effects usually mild Symptoms onset within 3 hours, resolution within 24 hours for treated patients most children asymptomatic most common symptoms are drowsiness or hyperactivity, agitation, tachycardia less commonly N/V, tremor, dizziness, abdominal pain rarely seizures, coma, hyperthermia serotonin syndrome adolescents > children
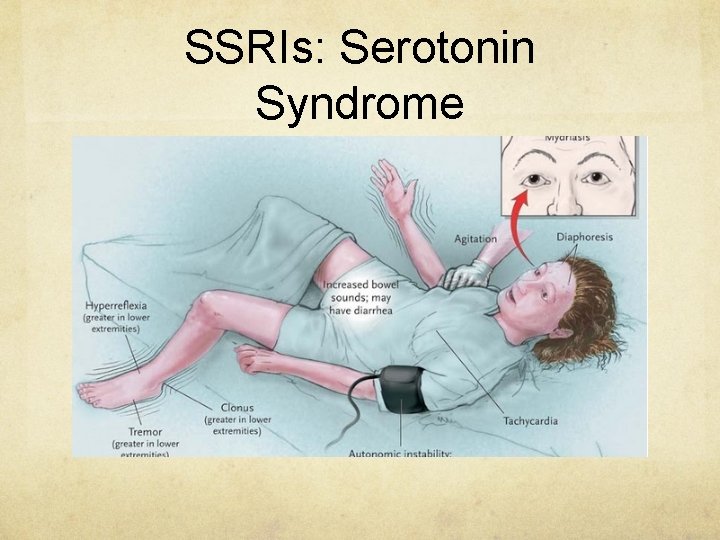
SSRIs: Serotonin Syndrome

SSRIs: Management severe symptoms: cardiac monitor, temperature monitoring activated charcoal benzos for agitation, hyperreflexia, tremors; if not responsive to this intubate and give paralytic antidotes: cyproheptadine or olanzapine (5 -HT 2 A antagonists) anti-pyretics not useful no emesis due to CNS depression

Clonidine Pathophysiology effects are due to alpha-2 adrenergic inhibition children very sensitive, with 0. 1 mg being toxic to young infants (toxicity even from used clonidine patches) Symptoms develop within 1 h of ingestion: lethargy, miosis, bradycardia, hypotension in younger children, apnea, respiratory depression, coma symptoms resolve after 24 h

Clonidine: Management monitor with EKG, vitals, blood gases aggressive supportive care can use naloxone in repeated doses (need to repeat them because duration of action shorter for naloxone than for clonidine) not helpful: levels, gastric decontamination (due to small quantities ingested, rapid onset of symptoms)

Iron: Pathophysiology amount of iron determined by # of tablets and % of elemental iron in each tablet ferrous sulfate, 20%; ferrous gluconate, 12%; ferrous fumarate, 33% iron usually listed as elemental iron toxic dose is >60 mg/kg Iron is corrosive and leads to ulceration and edema of GI tract, melena, hematemesis, perforation accumulates in mitochondria, causing cellular damage -> damage to mitochondria causes citric acidosis causes venodilation and hypotension -> decreased perfusion causes lactic acidosis causes hepatic necrosis

Iron Symptoms N/V/D, abdo pain, usually develop within 0. 5 -6 hours after ingestion; GI signs subside between 612 h Management cardiac monitor (possibility of cardiovascular collapse due to hypovolemia, acidosis) AXR to aid in diagnosis (iron is radio-opaque, but only undissolved tablets will be seen) repeat AXRs to monitor efficacy of decontamination treatment
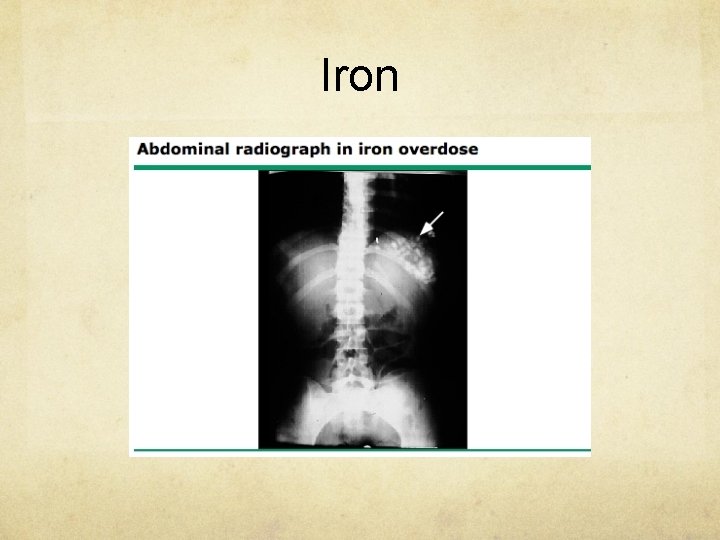
Iron

Iron: Management monitor serum iron levels, starting at 4 h: less than 500 = low risk more than 500 = high risk blood gas, glucose, liver enzymes, coagulation studies should be drawn if symptomatic or level >500 Useful: whole-bowel irrigation antidote: IV deferoxamine (indicated if iron level >500, or moderate to severe symptoms) as continuous infusion until patient symptom-free

Iron not useful activated charcoal as it does not absorb iron PO deferoxamine not as may increase iron absorption IM deferoxamine not as absorption erratic Long-term effects gastric scarring, pyloric stenosis, and intestinal strictures can develop 2 -4 weeks later

What Can Be Done? Poison prevention education how to poison-proof what to do if poisoning occurs (available from AAP, or Poison Control Centres) Batteries secure battery compartments with tape

References Boyer, et al. The Serotonin Syndrome. N Engl J Med 2005; 352: 1112 -1120. Fraser L, Wynne D, Clement WA, et al. Liquid detergent capsule ingestion in children: an increasing trend. Arch Dis Child 2012; 97: 1007. Valdez AL, Casavant MJ, Spiller HA, et al. Pediatric exposure to laundry detergent pods. Pediatrics 2014; 134: 1127. Caustic Esophageal Injury in Children, Upto. Date Button and Cylindrical Battery Ingestion, Upto. Date Nelson’s, pp 339 -357
- Slides: 43