ACA Implementation Adequacy and Sustainability of Coverage for

ACA Implementation: Adequacy and Sustainability of Coverage for Cancer Survivors Mark Mc. Clellan, MD Ph. D The Brookings Institution © The Brookings Institution. All rights reserved. No part of this presentation may be reproduced or transmitted in any form or by any means without permission in writing from the Brookings Institution, 1775 Massachusetts Avenue, N. W. , Washington, D. C. 20036 (Email: stetreault@brookings. edu).

Overview 1. Key Implementation Steps: What Happens When 2. Lessons from Part D Experience - Clear Policy Goals - Intense Education and Enrollment Support - Systems - Implementation Flexibility 1. Next Steps for Affordable, Innovative Cancer Care 2
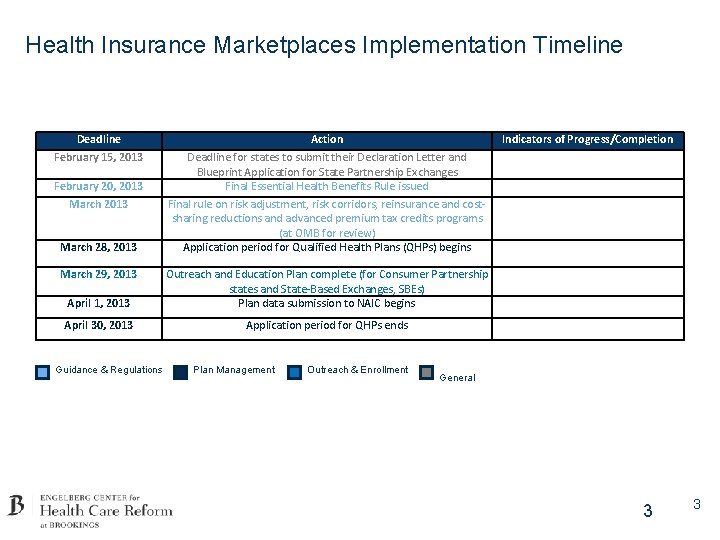
Health Insurance Marketplaces Implementation Timeline Deadline February 15, 2013 February 20, 2013 March 28, 2013 March 29, 2013 Action Deadline for states to submit their Declaration Letter and Blueprint Application for State Partnership Exchanges Final Essential Health Benefits Rule issued Final rule on risk adjustment, risk corridors, reinsurance and costsharing reductions and advanced premium tax credits programs (at OMB for review) Application period for Qualified Health Plans (QHPs) begins April 1, 2013 Outreach and Education Plan complete (for Consumer Partnership states and State-Based Exchanges, SBEs) Plan data submission to NAIC begins April 30, 2013 Application period for QHPs ends Guidance & Regulations Plan Management Outreach & Enrollment Indicators of Progress/Completion General 3 3
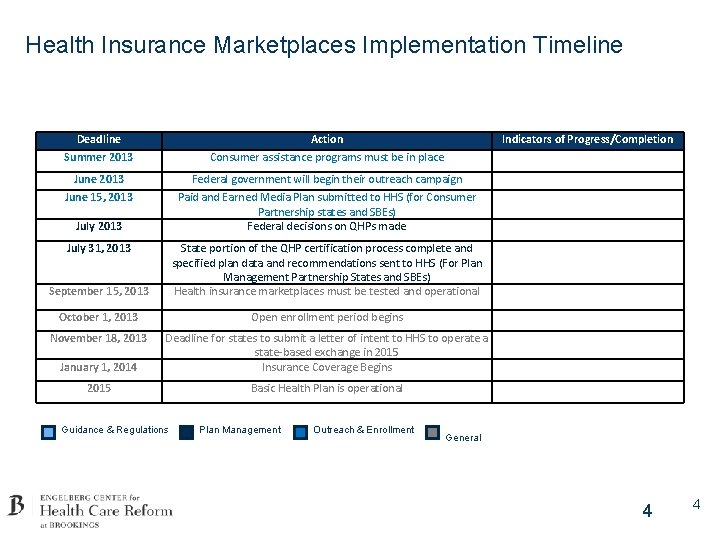
Health Insurance Marketplaces Implementation Timeline Deadline Summer 2013 Action Consumer assistance programs must be in place June 2013 June 15, 2013 Federal government will begin their outreach campaign Paid and Earned Media Plan submitted to HHS (for Consumer Partnership states and SBEs) Federal decisions on QHPs made July 2013 July 31, 2013 Indicators of Progress/Completion September 15, 2013 State portion of the QHP certification process complete and specified plan data and recommendations sent to HHS (For Plan Management Partnership States and SBEs) Health insurance marketplaces must be tested and operational October 1, 2013 Open enrollment period begins November 18, 2013 January 1, 2014 Deadline for states to submit a letter of intent to HHS to operate a state-based exchange in 2015 Insurance Coverage Begins 2015 Basic Health Plan is operational Guidance & Regulations Plan Management Outreach & Enrollment General 4 4

Lessons from Part D: Policy Decisions • Just because a market doesn’t exist, doesn’t mean the market can’t succeed – Have desired policy outcomes squarely in mind (requires dealing with tradeoffs) – Provide reliable information sufficient for decisionmaking by all major parties, particularly health plans and states – Convey confidence through step-by-step progress with milestones identified in advance – Ensure extensive communication for answering technical questions clearly and consistently: industry workshops, open door forums, FAQs, subregulatory guidances, etc. • Protect vulnerable populations – – Risk adjustment, reinsurance, risk corridors Meaningful but flexible coverage requirements (e. g. , oncology drugs) Auto-enrollment Take other reasonable policy steps to make potentially risky patients attractive to health plans 5

Lessons from Part D: Operations • Seek accurate and timely data flows – even the best laid plans and testing for systems won’t end up working without data – With any complex system involving multiple data feeds, there is the potential for problems – Pilot test systems with actual data to the extent time permits – Identify metrics to enable tracking of data availability and throughput (for example, individuals enrolled, prescriptions filled, measures of consumer experience) – Expect to devote teams to work proactively with states, health plans, and health care providers to address data flow problems • Make systems robust – do not depend on any single pathway for critical tasks to be accomplished • Identify best-practice solutions in plans, enrollment activities, states – cannot anticipate let alone figure them out centrally – and spread them 6

Lessons from Part D: Outreach and Collaboration • Find friends in unlikely places – build and leverage relationships with multiple stakeholders – Extensive effort to build broad-based local outreach efforts involving health plans, pharmacies, state agency officials, community organizations, and other stakeholders was crucial – Interagency cooperation in outreach and education also led to essential support – requires strong and ongoing support from the top • Overcoming awareness and enrollment inertia: free isn’t cheap enough in many cases – Multi-faceted outreach campaign enlisted the help of pharmacists and physicians to steadily address the “eligible but not enrolled” gap – Many mechanisms to find personalized information and enroll as easily as possible: web tools, phone customer service, community outreach events and enrollment hubs 7

Lessons from Part D: Maintain Flexibility to Ensure Successful Implementation • Mistakes will happen and problems will arise – allow for administrative flexibility and have contingency plans in place – Example: What if someone believes they are eligible for coverage and/or subsidies (and has some evidence for it) but their relevant electronic data cannot be found in coverage systems? • Assistance from plans and states can avoid frustrations from consumers – Make sure people who are counting on the program and need care can get it • Have metrics and support teams ready for potential problem areas • Expect the need for regular media updates and outreach about any problems and steps to correct them – nationally and especially state/local 8

Oncology Reform • Measures • Provider Payment • Benefit Design • Plan Choice 9
- Slides: 9