ACA Eligibility and Enrollment Changes Implications and Opportunities


ACA Eligibility and Enrollment Changes: Implications and Opportunities for Behavioral Health Providers Stephanie Mc. Claddie SAMHSA Regional Administrator DHHS Region IV FADAA Community Health and Wellness Conference April 22, 2013

Current Picture of Eligibility • Medicaid (as of January 1, 2013)* • Pregnant women (40 States at or above 185% FPL) • Disabled adults (11 States more restrictive than SSI) • Parents (1996 welfare income eligibility + waivers/state funds – benefit limits/cost sharing = mixed picture) (only 18 States offer full Medicaid at poverty level) • Low income, non-disabled, childless adults • 9 offer benefits equivalent to Medicaid (early ACA option/waivers/state funds) (AZ, CO, CT, DE, DC, HI, MN, NY, and VT) • 16 provide more limited benefits Source: “Getting into Gear for 2014: Findings from a 50 -State Survey of Eligibility, Enrollment, Renewal, and Cost-Sharing Policies in Medicaid and CHIP, 2012– 2013” available at: http: //www. kff. org/medicaid/upload/8401. pdf

Current Picture of Eligibility • CHIP/Children in Medicaid • All states have expanded coverage (26 have options at or above 250% FPL and only 4 less than 200% FPL) • CHIPRA allowed for significant improvements in eligibility determination processes (express lane/presumptive eligibility) • 25 have exemption from 5 -year lawfully-residing immigrant wait due to CHIPRA • Medicare • 65 years old or older or receiving SSI payments for 2 consecutive years • State Exchanges • Massachusetts (premium subsidized up to 300% FPL) • Utah (no subsidies)

Enrollment Assistance Efforts • 48 States offer in-person assistance in eligibility offices and/or toll-free hotline • 47 states offer toll-free hotline • 3 5 states have out-stationed state eligibility workers • 23 states have state-funded community-based application assisters • 37 states have electronic online application in Medicaid or CHIP • 28 states allow families to renew online (8 states added this capability in 2012) • 36 states provide on line accounts
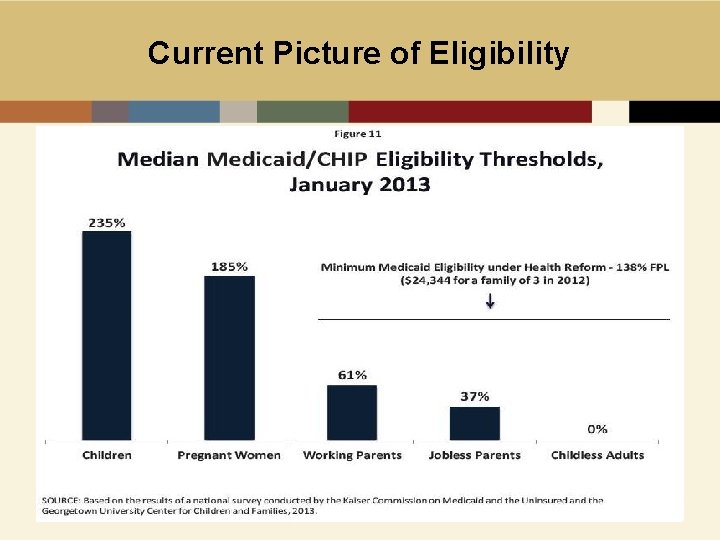
Current Picture of Eligibility
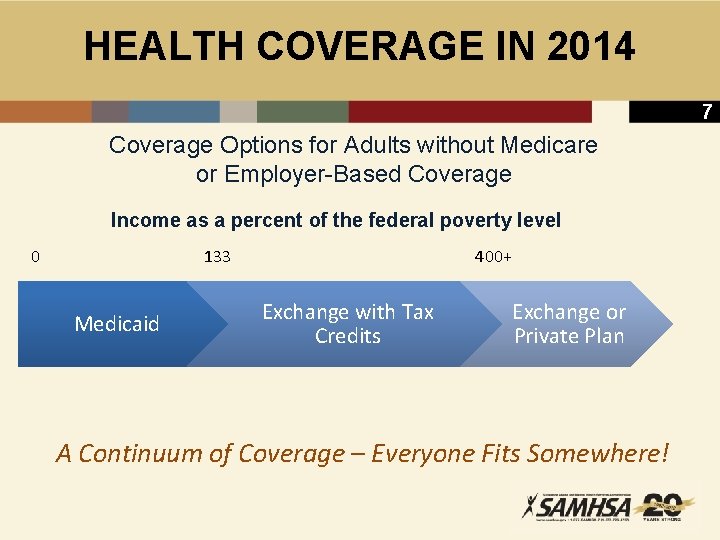
HEALTH COVERAGE IN 2014 7 Coverage Options for Adults without Medicare or Employer-Based Coverage Income as a percent of the federal poverty level 0 133 Medicaid 400+ Exchange with Tax Credits Exchange or Private Plan A Continuum of Coverage – Everyone Fits Somewhere!
A NEW WAY TO ENROLL IN COVERAGE 8 Simple, Streamlined Application “No Wrong Door” Eligibility and Enrollment Model Modern, Data-driven Verification Systems Online Tool for Consumers to Easily Compare and Enroll in Health Plans Data-driven Renewal for Continuous Coverage
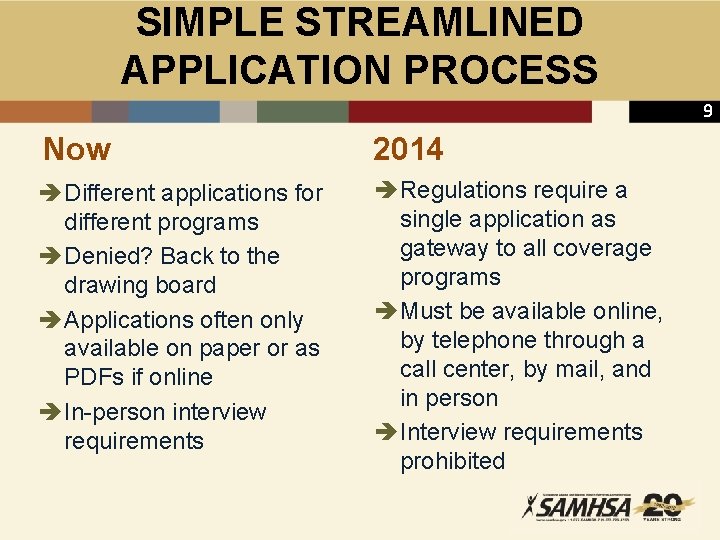
SIMPLE STREAMLINED APPLICATION PROCESS 9 Now 2014 è Different applications for different programs è Denied? Back to the drawing board è Applications often only available on paper or as PDFs if online è In-person interview requirements è Regulations require a single application as gateway to all coverage programs è Must be available online, by telephone through a call center, by mail, and in person è Interview requirements prohibited
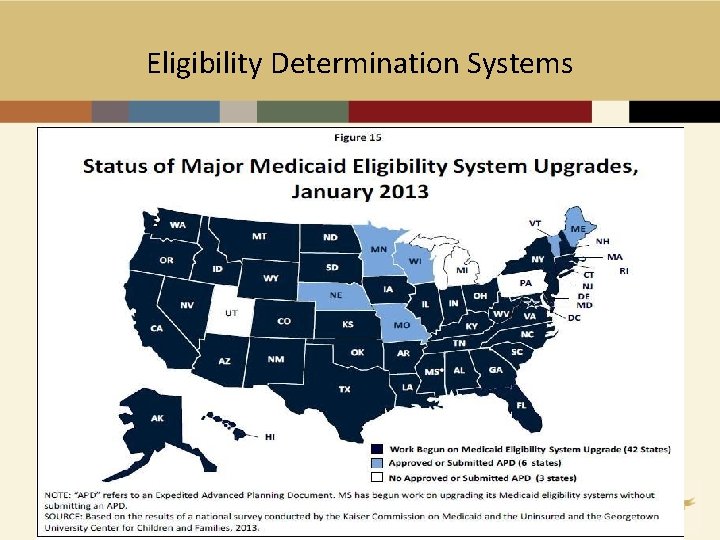
Eligibility Determination Systems

ACA Consumer/Enrollment Assistance Activities Consumer Assistance Grants • Employed directly by Medicaid agency or Exchange entity • Support state development of appeals assistance services and claims dispute processes • Hiring and training for enrollment assistance outreach workers • Public outreach • http: //www. healthcare. gov/news/factsheets/2010/10/capgrantsstates. html Marketplace Assisters • Employed directly by Medicaid agency or Exchange entity, or funded by grant or contract to fulfill additional non-navigator assistance requirement • Can be financed by consumer assistance or establishment grants • Cannot take the place of Navigator program

ACA Consumer/Enrollment Assistance Activities Navigator program (2014) • Conduct public education activities to raise awareness of the availability of qualified health plans • Distribute fair and impartial information about enrollment in qualified health plans and the availability of premium tax credits • Facilitate enrollment in qualified health plans • Provide referrals to an office of health insurance consumer assistance or ombudsman, or any other appropriate state agencies, for any enrollee with a grievance, complaint, or question regarding their health plan • Provide information in a manner that is culturally and linguistically appropriate to the needs of the population served by the Exchange

ACA Consumer/Enrollment Assistance Activities Navigator program (2014) • Required for and financed by each Exchange • Strong conflict of interest standards • Restrictions on producer/broker licensure requirements • Privacy and security standards • Training and credentialing will be necessary Implementation Update • FOA for FFE/SPE Navigators available NOW • At least 13 States engaged in public planning work (Feb. 27, 2013) – AR, WA, WV, CA, CO, CT, DC, HI, MN, NV, OR, VT • Some subsumed by broader assister program • Medicaid enrollment assistance questions raised
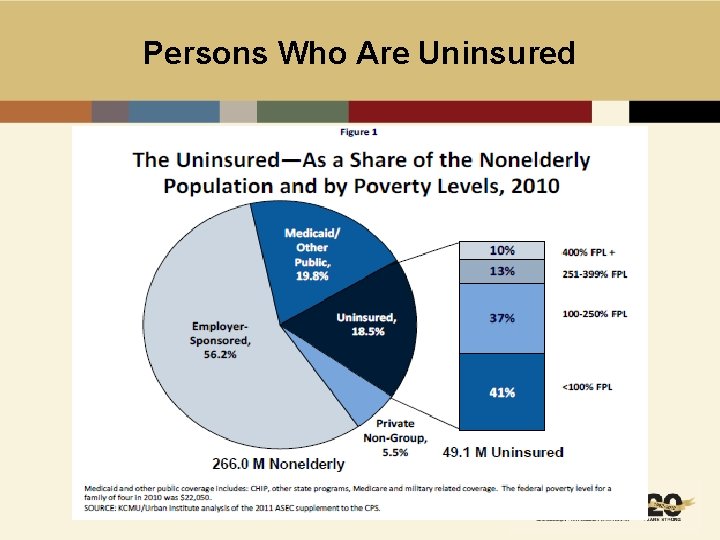
Persons Who Are Uninsured
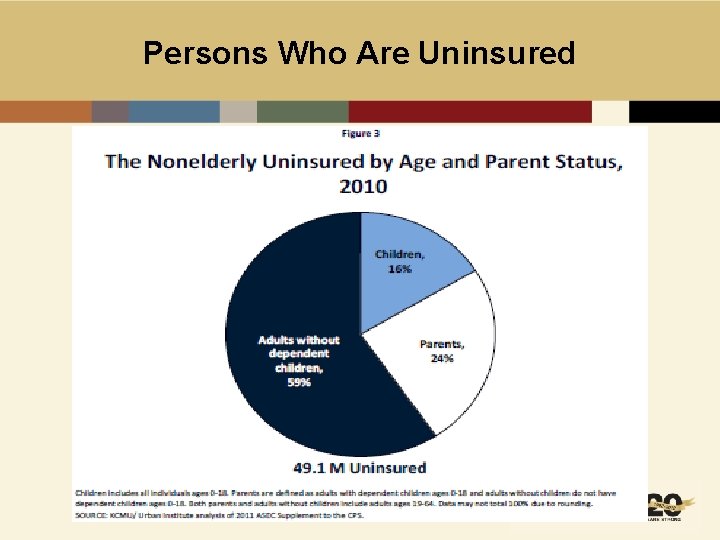
Persons Who Are Uninsured
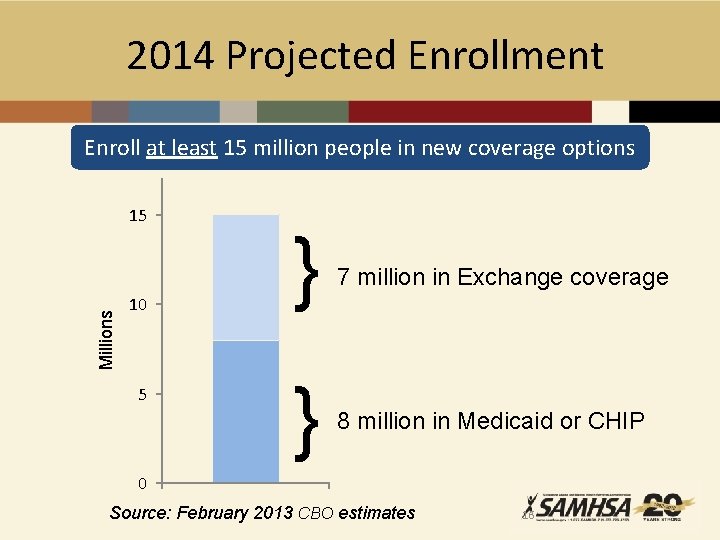
2014 Projected Enrollment Enroll at least 15 million people in new coverage options Millions 15 10 5 } 7 million in Exchange coverage } 8 million in Medicaid or CHIP 0 Source: February 2013 CBO estimates 16
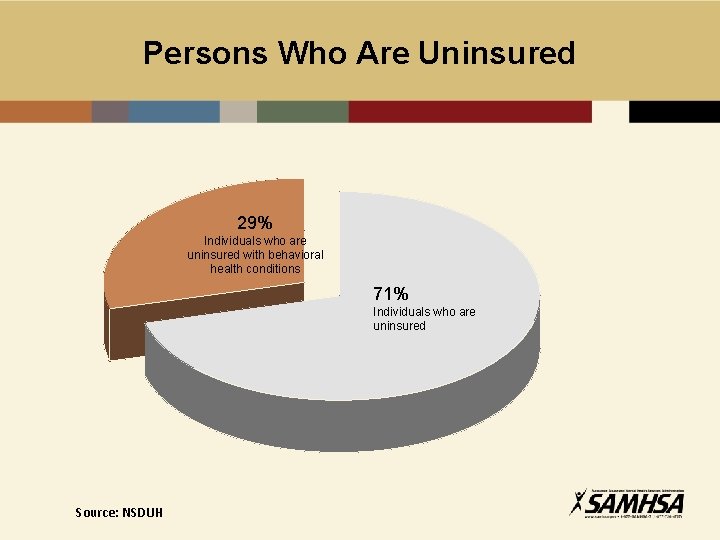
Persons Who Are Uninsured 29% Individuals who are uninsured with behavioral health conditions 71% Individuals who are uninsured Source: NSDUH

Data Sources • National Survey on Drug Use and Health - Sponsored by SAMHSA - National and state estimates on prevalence of behavioral health conditions and treatment - 2008 - 2010 data - Approximately 67, 500 interviews per year • American Community Survey - Sponsored by the U. S. Bureau of the Census - National and State population estimates, including counts of uninsured by income level - 2010 data - Approximately 1. 9 million persons in sample 18

Methods for Estimating Uninsured with M/SU Conditions by FPL • From NSDUH, identified by State the number of uninsured persons aged 18 -64 with income: - Between 133% and 400% of the Federal poverty level (FPL) eligible for health insurance exchanges - Less than 139% of the FPL eligible for Medicaid expansion • Calculated NSDUH prevalence rates for serious mental illness (SMI) and substance use disorder (SUD) by State, for the above groups • Applied SMI/SUD prevalence rates to American Community Survey counts of uninsured by State 19

Prevalence of Serious Mental Illness Among Adults Ages 18 – 64 by Current Medicaid Status and Eligibility for Medicaid Expansion or Health Insurance Exchanges: Florida, US 20 CI = Confidence Interval Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey

Prevalence of Serious Psychological Distress Among Adults Ages 18 – 64 by Current Medicaid Status and Eligibility for Medicaid Expansion or Health Insurance Exchanges: Florida, US 21 CI = Confidence Interval Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey

Prevalence of Substance Use Disorders Among Adults Ages 18 – 64 by Current Medicaid Status and Eligibility for Medicaid Expansion or Health Insurance Exchanges: Florida, US 22 CI = Confidence Interval Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey
Prevalence of Behavioral Conditions Among Health Insurance Exchange Population: Florida, US 23 CI = Confidence Interval Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey

Prevalence of Behavioral Conditions Among Medicaid Expansion Population: Florida, US 24 CI = Confidence Interval Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey

Methods for Estimating Population Characteristics • From NSDUH, calculated the national prevalence rates for SMI, serious psychological distress (SPD), and SUD by income group with demographic populations of interest (e. g. , uninsured non-Hispanic whites with income <138% FPL with SMI) • Multiplied national prevalence rate by the ACS’ State population by income group with this demographic characteristic (e. g. , national % of uninsured 18 -34 year olds with income <138% FPL with SMI * ACS State number of 18 -34 year olds with income <138% FPL) • Calculated the percent distribution with condition in the State across demographic groups such as race, age, and education (e. g. , percent with SMI with < high school, or college education) 25
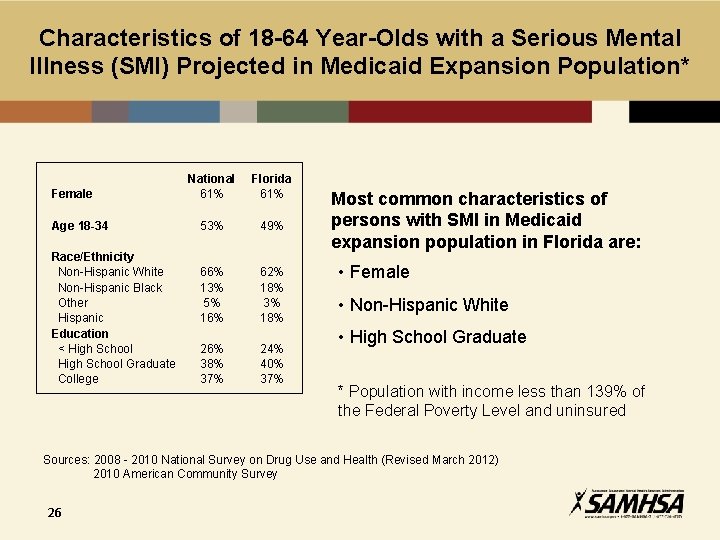
Characteristics of 18 -64 Year-Olds with a Serious Mental Illness (SMI) Projected in Medicaid Expansion Population* Female Age 18 -34 Race/Ethnicity Non-Hispanic White Non-Hispanic Black Other Hispanic Education < High School Graduate College National 61% Florida 61% 53% 49% 66% 13% 5% 16% 62% 18% 3% 18% 26% 38% 37% 24% 40% 37% Most common characteristics of persons with SMI in Medicaid expansion population in Florida are: • Female • Non-Hispanic White • High School Graduate * Population with income less than 139% of the Federal Poverty Level and uninsured Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey 26
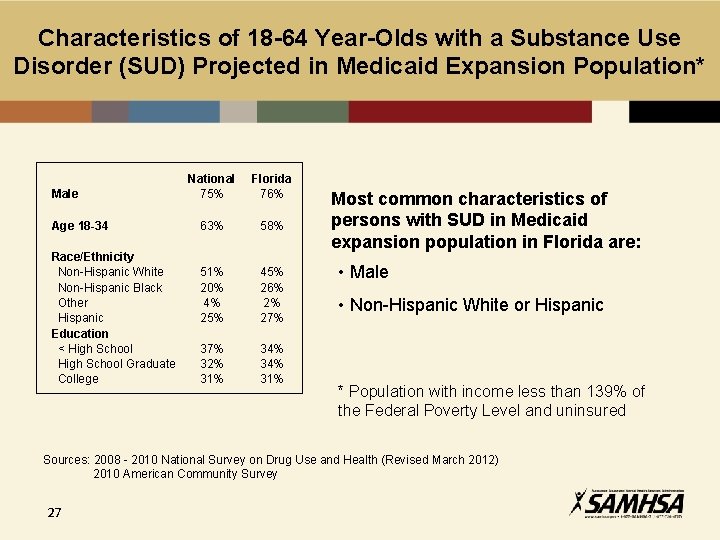
Characteristics of 18 -64 Year-Olds with a Substance Use Disorder (SUD) Projected in Medicaid Expansion Population* Male Age 18 -34 Race/Ethnicity Non-Hispanic White Non-Hispanic Black Other Hispanic Education < High School Graduate College National 75% Florida 76% 63% 58% 51% 20% 4% 25% 45% 26% 2% 27% 32% 31% 34% 31% Most common characteristics of persons with SUD in Medicaid expansion population in Florida are: • Male • Non-Hispanic White or Hispanic * Population with income less than 139% of the Federal Poverty Level and uninsured Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey 27
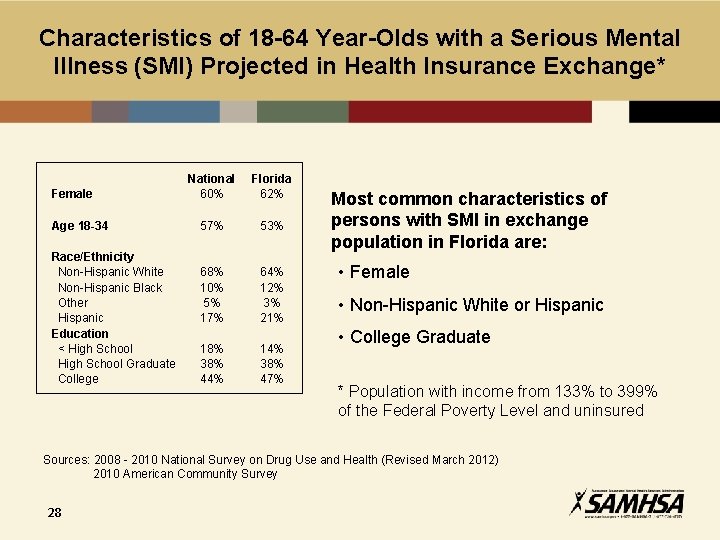
Characteristics of 18 -64 Year-Olds with a Serious Mental Illness (SMI) Projected in Health Insurance Exchange* Female Age 18 -34 Race/Ethnicity Non-Hispanic White Non-Hispanic Black Other Hispanic Education < High School Graduate College National 60% Florida 62% 57% 53% 68% 10% 5% 17% 64% 12% 3% 21% 18% 38% 44% 14% 38% 47% Most common characteristics of persons with SMI in exchange population in Florida are: • Female • Non-Hispanic White or Hispanic • College Graduate * Population with income from 133% to 399% of the Federal Poverty Level and uninsured Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey 28
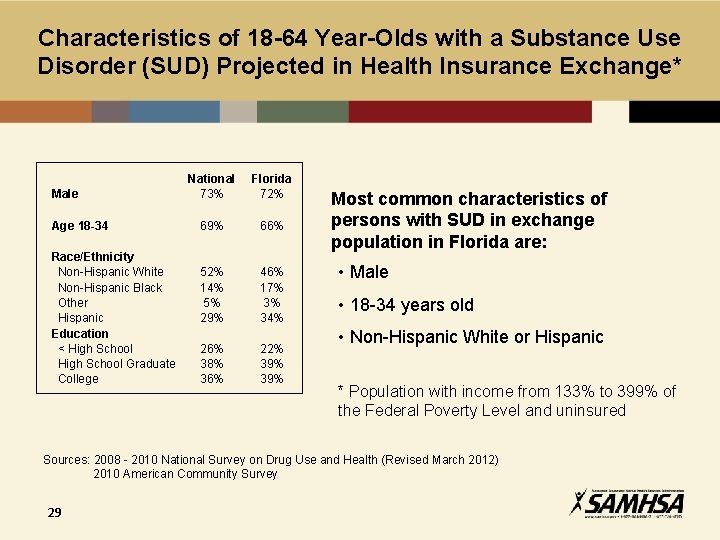
Characteristics of 18 -64 Year-Olds with a Substance Use Disorder (SUD) Projected in Health Insurance Exchange* Male Age 18 -34 Race/Ethnicity Non-Hispanic White Non-Hispanic Black Other Hispanic Education < High School Graduate College National 73% Florida 72% 69% 66% 52% 14% 5% 29% 46% 17% 3% 34% 26% 38% 36% 22% 39% Most common characteristics of persons with SUD in exchange population in Florida are: • Male • 18 -34 years old • Non-Hispanic White or Hispanic * Population with income from 133% to 399% of the Federal Poverty Level and uninsured Sources: 2008 - 2010 National Survey on Drug Use and Health (Revised March 2012) 2010 American Community Survey 29

Enrollment and Behavioral Health • In MA, 20 -30% of patients seeking acute services are uninsured (in a state where 97% of population as a whole is insured). * • In MA, 20 -25% of acute service presentations are uninsured and most of these are young men 18 -25 years old. * • In MA, half of patients with MH and SUD conditions in focus groups were avoidably disenrolled at least once from their health insurance in the past year. * • In ME, 10% of Maine residents but more than 31% of substance abuse treatment clients uninsured. ** *Source: Substance Abuse and Mental Health Services Administration. Enrollment and Disenrollment in Subsidized Health Insurance: Lessons Learned in Massachusetts. November 2011. ** Source: National Association of State Alcohol and Drug Abuse Directors, Inc. Effects of State Health Reform on Substance Abuse Services in Main, Massachusetts, and Vermont. Considerations for Implementation of the Patient Protection and Affordable Care Act (PPACA). June 2010. 3

SAMHSA Enrollment Coalitions Initiative • Collaborate with national organizations whose members/constituents interact regularly with individuals with mental health and/or substance use conditions to create and implement enrollment communication campaigns • Promote and encourage the use of CMS materials • Provide training and technical assistance in developing enrollment communication campaigns using these materials • Provide training to design and implement enrollment assistance activities • Channel feedback and evaluate success 31
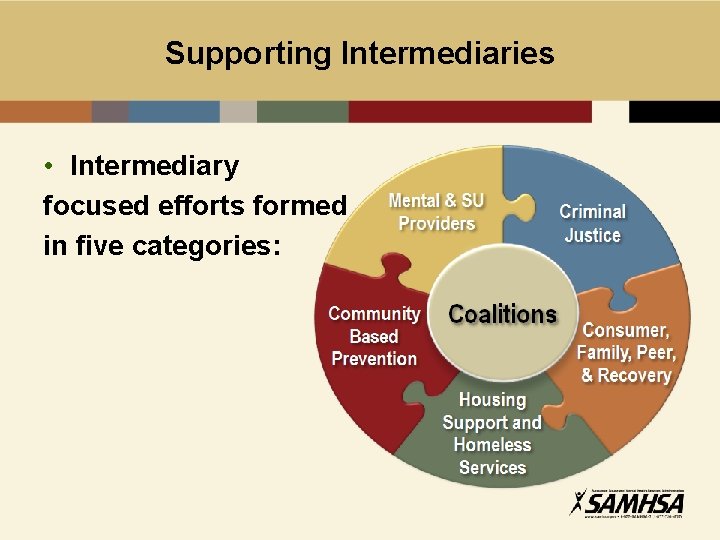
Supporting Intermediaries • Intermediary focused efforts formed in five categories:

SAMHSA Enrollment Coalitions Initiative • Supporting coalition groups in their commitment to promoting access to insurance for their constituents • Inviting coalition groups to shape enrollment support policy, planning, training and materials development • Providing leadership for other organizations 33
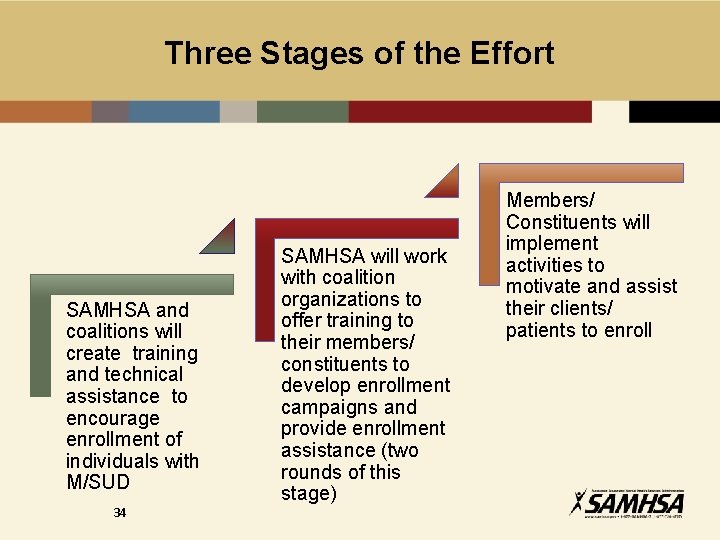
Three Stages of the Effort SAMHSA and coalitions will create training and technical assistance to encourage enrollment of individuals with M/SUD 34 SAMHSA will work with coalition organizations to offer training to their members/ constituents to develop enrollment campaigns and provide enrollment assistance (two rounds of this stage) Members/ Constituents will implement activities to motivate and assist their clients/ patients to enroll
Timeline Laying the Groundwork Preparing for Enrollment • Coalition formation • Health insurance literacy training and technical assistance • February –May 2013 • Enrollment campaign training • Enrollment assistance training • June – September 2013 35 Enrolling Eligible Individuals • Continuation of enrollment campaigns • Enrollment assistance • October 2013 - March 2014

Key Takeaways • High prevalence of substance abuse and mental health conditions among the uninsured • 2014 will potentially bring coverage to 11 million individuals with substance abuse and or mental health conditions • Significant changes are happening to eligibility and enrollment systems • Substance abuse and mental health peer organizations must play an active role in outreach and enrollment
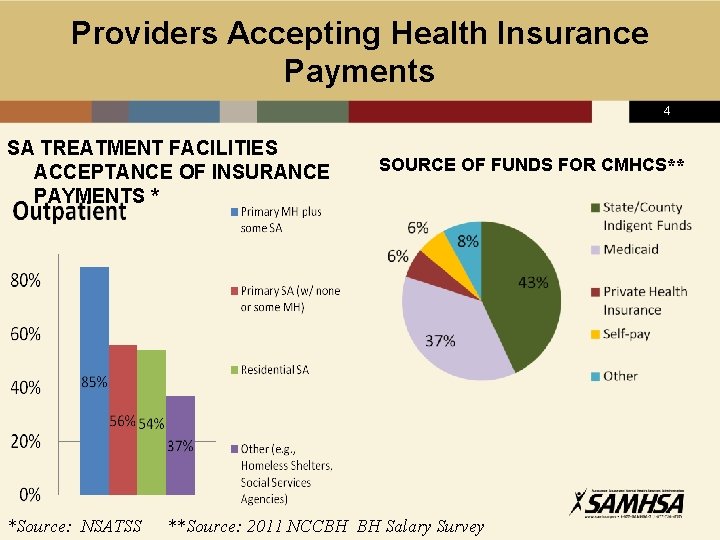
Providers Accepting Health Insurance Payments 4 SA TREATMENT FACILITIES ACCEPTANCE OF INSURANCE PAYMENTS * *Source: NSATSS SOURCE OF FUNDS FOR CMHCS** **Source: 2011 NCCBH BH Salary Survey

Provider Business Operations Learning Networks 38 • TA to help 900+ provider orgs/year in 5 areas of practice • Strategic business planning in an era of health reform • 3 rd-party contract negotiations • 3 rd-party billing and compliance • Health insurance eligibility determinations and enrollment • Health information technology adoption • Special focus on providers of peer & recovery support services & providers serving racial & ethnic minority and other vulnerable populations • http: //www. samhsa. gov/health. Reform/BHbusiness. a spx

Enrollment Resources • Healthcare. gov • http: //www. healthcare. gov/marketplace/index. html • HHS Partners Resources • http: //www. cms. gov/Outreach-and. Education/Outreach/HIMarketplace/index. html • SAMHSA Enrollment Webpage • http: //www. samhsa. gov/enrollment/ • State Refor(u)m Exchange Decisions • http: //www. statereforum. org/node/10222 • Enroll America Best Practices • http: //www. enrollamerica. org/best-practices-institute
- Slides: 39